Abstract
Amphetamine (AMPH) increases adult rat 50-kHz ultrasonic vocalizations, preferentially promoting frequency-modulated (FM) calls that have been proposed to reflect positive affect. The main objective of this study was to investigate a possible noradrenergic contribution to AMPH-induced calling. Adult male Long-Evans rats were tested with AMPH (1 mg/kg intraperitoneal) or saline combined with various systemic pretreatments: clonidine (α2 adrenergic agonist), prazosin (α1 antagonist), atipamezole (α2 antagonist), propranolol, betaxolol, and/or ICI 118,551 (β1/β2, β1, and β2 antagonists, respectively), nadolol (β1/β2 antagonist, peripheral only), or NAD-299 (5HT1A antagonist). In addition, effects of cirazoline (α1 adrenergic agonist) and cocaine (0.25–1.5 mg/kg intravenous) were studied alone. AMPH-induced calling was suppressed by low-dose clonidine and prazosin. Cirazoline and atipamezole did not significantly affect calling rate. Propranolol, without affecting the call rate, dose dependently promoted ‘flat’ calls under AMPH while suppressing ‘trills,’ thus reversing the effects of AMPH on the ‘call subtype profile.’ This effect of propranolol seemed to be mediated by simultaneous inhibition of CNS β1 and β2 rather than by 5HT1A receptors. Finally, cocaine elicited fewer calls than did AMPH, but produced the same shift in the call subtype profile. Taken together, these results reveal differential drug effects on flat vs trill vs other FM 50-kHz calls. These findings highlight the value of detailed call subtype analyses, and show that 50-kHz calls are associated with adrenergic α1- and β-receptor mechanisms. These preclinical findings suggest that noradrenergic contributions to psychostimulant subjective effects may warrant further investigation.
Similar content being viewed by others
INTRODUCTION
Adult laboratory rats emit two main types of ultrasonic vocalizations (USVs), commonly termed ‘22-kHz calls’ and ‘50-kHz calls.’ Evidence suggests that USVs may have a communicative role (Brudzynski, 2005; Burgdorf et al, 2008a; Wohr and Schwarting, 2009). Vocalizations of the 22-kHz type serve as alarm or distress calls (Covington and Miczek, 2003; Litvin et al, 2007), whereas 50-kHz calls are frequently elicited by appetitive stimuli (Burgdorf et al, 2010; Knutson et al, 2002).
The 50-kHz class of adult rat USVs encompasses a wide frequency range (30–90 kHz) (Kaltwasser, 1990; Sales and Pye, 1974; Wright et al, 2010) and comprises two main subclasses: flat (ie, constant frequency) and frequency-modulated (FM) calls. These two subclasses seem to differ in their behavioral significance and neurochemical basis (Ahrens et al, 2009; Barker et al, 2010; Burgdorf et al, 2007, 2008a; Burgdorf and Panksepp, 2006; Ciucci et al, 2009; Meyer et al, 2011; Simola et al, 2009; Wohr et al, 2008, 2009). FM 50-kHz USVs are diverse, with at least 13 acoustic subtypes, and the prevalent ‘trill’ call subtype, in particular, consistently occurs in appetitive situations (Burgdorf et al, 2008a). On this basis, it has been proposed that FM calls (and especially trill calls) reflect an emotional state homologous to positive affect in humans (Burgdorf and Moskal, 2009; Burgdorf et al, 2010).
The prototypical euphoriant D-amphetamine (AMPH) (Foltin and Fischman, 1991) increases the rate of 50-kHz call production in adult rats, both after systemic and central administration (Ahrens et al, 2009; Burgdorf et al, 2001; Simola et al, 2009; Thompson et al, 2006; Wintink and Brudzynski, 2001; Wright et al, 2010). In addition, AMPH has been shown to modify the 50-kHz call ‘profile’ (ie, the relative proportion of different call subtypes), preferentially increasing trills and decreasing flat calls (Wright et al, 2010). Cocaine administration is also reported to promote 50-kHz calling (Barker et al, 2010; Browning et al, 2011; Ma et al, 2010; Maier et al, 2010; Mu et al, 2009; Williams and Undieh, 2010), and a recent report shows a preferential increase in FM 50-kHz calls in response to intraperitoneal (IP) cocaine (Meyer et al, 2011). However, whether intravenous (IV) cocaine mimics the AMPH-induced shift in the call profile has not been reported.
Dopaminergic transmission seems to have a key role in the production of 50-kHz USVs. In particular, dopaminergic manipulations are reported to affect calls elicited by AMPH (Thompson et al, 2006), sex-relevant odors (Ciucci et al, 2009), tickling (Burgdorf et al, 2007), and intracerebral glutamate (Wintink and Brudzynski, 2001). However, the observation that dopamine (DA)-depleting lesions inhibited FM but not flat 50-kHz calls (Burgdorf et al, 2007; Ciucci et al, 2009) indicates that not all 50-kHz calls are necessarily DA dependent.
AMPH and cocaine promote noradrenergic, as well as dopaminergic neurotransmission (McKittrick and Abercrombie, 2007; Segal and Kuczenski, 1997). However, a possible noradrenergic role in the production of adult rat 50-kHz USVs has not, to our knowledge, been investigated, except in the context of social stress (Tornatzky and Miczek, 1994). This issue is of interest for several reasons. First, recent evidence supports a noradrenergic contribution to conventional reward-related behaviors, notably conditioned place preference (CPP) and reinstatement of IV self-administration (for review, see Weinshenker and Schroeder (2007); also see the ‘Discussion’ section). Second, noradrenaline (NA) also seems to contribute to the discriminative stimulus effects of AMPH in several species (Snoddy and Tessel, 1983, 1985); these cues potentially model subjective drug effects in humans (Stolerman, 1992). Third, early studies indicated that AMPH euphoria in human subjects is critically dependent on catecholaminergic transmission (Jonsson et al, 1969, 1971), and in some studies, AMPH euphoria seemed to be DA independent, suggesting a possible role for NA (Brauer and de Wit, 1997; Rothman et al, 2001; Sofuoglu et al, 2009).
The main aim of this study was to test the hypothesis that NA (or adrenaline) contributes to the emission of spontaneous and AMPH-induced 50-kHz USVs, potentially in a call subtype-selective manner. To this end, we first examined whether 50-kHz USV emission under AMPH was altered by acute pretreatment with the α2 agonist clonidine, administered at doses that decrease NA release (Schoffelmeer and Mulder, 1984). We then tested the α1 adrenergic antagonist prazosin, the α1 agonist cirazoline, the α2 antagonist atipamezole, and the β1/β2 blocker propranolol. Propranolol produced a dose-dependent shift in the call profile under AMPH, and we subsequently investigated the pharmacological mechanism underlying this effect: (1) To test for peripheral mediation, we administered nadolol, a non-selective hydrophilic β-blocker, which does not readily cross the blood–brain barrier (Schiff and Saxey, 1984); (2) We evaluated the contribution of β1 vs β2 receptor blockade using selective antagonists (betaxolol and ICI 118,551); and (3) As propranolol is a weak 5HT1A receptor antagonist, we tested a selective antagonist of this receptor (NAD-299) (Ross et al, 1999). In a final experiment, we tested whether the call subtype-dependent effects produced by IP administration of AMPH would generalize to the IV route and also to cocaine.
MATERIALS AND METHODS
Subjects
Subjects were 77 male Long-Evans rats (Charles River Laboratories, St Constant, Quebec, Canada), weighing 307–425 g (ie, aged approximately 9–11 weeks) at the start of the experiment. They were housed 2 per cage (25 × 48 × 20 cm3) in a temperature- and humidity-controlled colony room (19–20°C, 50–60%) at the McGill University Animal Research Center. Rats were maintained on a reverse 12 : 12 light/dark cycle, with lights off at 0700 hours. All behavioral testing took place during the dark phase of the cycle. Food and water were available ad libitum, except during testing sessions. All procedures were approved by the McGill Animal Care Committee in accordance with the guidelines of the Canadian Council on Animal Care. In all experiments, rats were initially drug-naive and experimentally naive; Experiments 3 and 6 were each divided into two parts, with part b beginning within a week after the end of part a.
Overview of Experiments
Almost all experiments investigated the effects of various drug pretreatments on the USV response (ie, call rate and acoustic profile) to systemic (IP) AMPH. Exceptionally, Experiment 3a examined the acute USV response to cirazoline and atipamezole alone, and Experiment 7 comprised a dose-response study of IV cocaine given alone. Details of individual experiments are summarized in Table 1.
Protocol for Individual Experiments
AMPH screen
A significant minority of rats emit few USVs in response to systemic AMPH (Wright et al, 2010). To identify and exclude such subjects, rats were initially screened for AMPH-induced calling in three 20-min test sessions spaced 2 days apart. Immediately before each session, rats were administered AMPH (1 mg/kg, IP) and then placed in a test chamber. On the intervening days, rats remained in their home cages. Only the third AMPH test session was analyzed because the first two sessions are not necessarily indicative of a rat's subsequent USV response to AMPH (unpublished observation). USVs that were emitted 10–20 min after injection were counted; rats with the lowest rate of calling (ie, 20–43% of rats depending on the experiment) were excluded from subsequent testing. In total, 47 out of 124 rats were excluded on this basis.
Drug testing
Drug testing was initiated 2–5 days after the final AMPH screening session, with the exception of Experiment 7 (ie, 11 days) in which rats needed to recover from surgery before drug testing began. All experiments used a fully parametric within-subject design in which each rat was tested once under each drug condition (see Table 1 for details). Thus, in Experiments 1, 2, 3b, and 4–6, rats received all combinations of pretreatment and treatment drugs including vehicle controls. Similarly, in Experiments 3a and 7, rats received a test with each of the following: vehicle, AMPH, and each dose of the drug(s) being tested. Within each experiment, the order of testing was counterbalanced as far as possible. Test sessions were of 20 min duration except in Experiment 7; here, subjects were administered IV cocaine or AMPH and were tested only 0–10 min after injection, ie, during the period of drug onset. Test sessions were spaced 2 days apart to minimize possible carry-over effects of the drugs.
For Experiment 7 (IV cocaine and AMPH), rats first underwent IV catheterization surgery (see below). After recovery, the experiment comprised an initial habituation day, whereby rats were placed in the test chambers for 10 min, then removed and immediately injected with 0.1 ml heparin-Baytril-saline solution to maintain catheter patency. On the five test days that followed, each rat received a 10-s infusion of drug directly after they were placed in the test chamber. Immediately after drug infusion, the tubing was disconnected and the session started.
IV Catheterization Surgery
General anesthesia was provided by ketamine HCl (80 mg/kg IP) and xylazine HCl (16 mg/kg IP). A 5-mm incision was made on the right ventral surface of the neck. A chronic indwelling silastic catheter (0.5 mm I.D. and 0.9 mm O.D., Fisher Scientific, Montreal, Quebec, Canada) was inserted in the right jugular vein and secured using silk sutures. The catheter was passed subcutaneously to a 2-cm incision on the head, where it was connected to a modified plastic cannula (Plastics One, Roanoke, VA), which was then anchored to the top of the skull with stainless steel mounting screws (Plastics One) and dental cement (Stoelting, Wooddale, IL). The cannula was blocked using a plastic stopper made from Tygon tubing (Fisher Scientific), and shielded with an aluminum cap when not in use. The analgesic carprofen (5 mg/kg SC) was administered during surgery to alleviate post-surgical pain. In all, 4 rats out of 19 died from anesthetic overdose during surgery. To verify catheter patency, each rat received an infusion of Na methohexital (‘Brevital,’ 1 mg in 0.1 ml, 2-s infusion, IV) once in their home cage, 3–5 days after surgery; three rats failed to show the expected sedative response and were therefore excluded from the experiment. The remaining rats were allowed 7–9 days of recovery before experimental testing began. Immediately after the habituation session and after each test session, the catheters were flushed with 0.1 ml of a sterile 0.9% saline solution containing 0.2 mg/ml heparin (Sigma-Aldrich, Oakville, Ontario, Canada) and 17 mg/ml Baytril (ICN Biomedicals, Cleveland, OH).
Acquisition and Classification of USVs
Testing took place in clear Plexiglas experimental chambers (ENV-007CT, Med Associates, St Albans, VT), each of which was enclosed in a melamine compartment lined with sound-attenuating acoustic foam (Primacoustic, Port Coquitlam, British Columbia). Condenser ultrasound microphones (CM16/CMPA, Avisoft Bioacoustics, Berlin, Germany) were securely inserted through small (5-cm diameter) holes located centrally in the top panels of the experimental chambers. Consequently, the microphones were 15–30 cm from rats during testing. Microphone signals were fed into an UltraSoundGate 416H data acquisition device (Avisoft Bioacoustics) with a sampling rate of 250-kHz and a 16-bit resolution.
Acoustical analysis was performed using Avisoft SASLab Pro (version 4.2, Avisoft Bioacoustics). Spectrograms were generated with a fast Fourier transform length of 512 points and an overlap of 75% (FlatTop window, 100% frame size). Correspondingly, spectrograms had a frequency resolution of 490 Hz and a time resolution of 0.5 ms. Calls were selected manually from spectrograms by an individual who was masked to the treatment condition. Each identified 50-kHz call was classified into 1 of 14 distinct categories: complex, upward ramp, downward ramp, flat, short, split, step-up, step-down, multi-step, trill, flat–trill combination, trill with jumps, or composite (see Wright et al (2010) for criteria for call identification and classification, several examples of each call type, as well as descriptive statistics relating to acoustic parameters). This method of manual call selection has been validated by surgical devocalization, and classification is associated with high inter- and intra-rater reliability (Wright et al, 2010). Some representative 50-kHz USVs are shown in Figure 1. 22-KHz calls were rarely observed in this study and were not analyzed further.
Spectrographic display of individual 50-kHz calls, which are representative of the following subtypes (left to right): trill, step-up, flat, step-down, and trill with jumps. See Wright et al (2010) for additional examples of all fourteen 50-kHz call subtypes so far recognized.
Drugs
All test drugs, doses, and routes of administration are shown in Table 1. Drugs were: D-AMPH sulfate (Sigma-Aldrich, Poole, UK); cocaine HCl (Medisca, St-Laurent, Quebec, Canada); clonidine HCl, prazosin HCl, (±)-propranolol HCl, and nadolol (all from Sigma-Aldrich); NAD-299 HCl (ie, Robalzotan), betaxolol HCl, ICI 118,551 HCl, cirazoline HCl, and atipamezole HCl (all from Tocris Bioscience, Ellisville, MO). The doses of prazosin, propranolol, clonidine, and nadolol are expressed as the free base; all other drug doses are expressed as the salt. Drugs were dissolved in sterile 0.9% saline and administered in a volume of 1 ml/kg body weight with the following exceptions: (1) prazosin was dissolved in distilled water, (2) the combination of betaxolol and ICI 118,551 in Experiment 6 was administered in a volume of 4 ml/kg (divided into 2 separate injections), and (3) nadolol (Experiment 5), as well as betaxolol and ICI 118,551 in Experiment 5 were administered in a volume of 2 ml/kg. Control injections were of saline (Experiments 1 and 3–7) or water (for prazosin, Experiment 2) and administered in the same volume as the corresponding drug.
Data Analysis and Statistics
Data were analyzed using commercial software (Systat v11, SPSS, Chicago, IL; GraphPad Prism 4, GraphPad Software, La Jolla, CA). For the IV cocaine dose-response study (Experiment 7), only the USVs emitted during the first 30-s of each minute were analyzed. For Experiment 3a (effects of cirazoline and atipamezole), minutes 3, 8, 13, and 18 were analyzed. For all other experiments, analysis of USVs was restricted to minutes 12, 14, and 16 of the 20-min session to allow time for AMPH to take effect. In the analysis, ‘call rate’ was defined as the total number of 50-kHz calls (ie, calls of all categories) emitted per minute. ANOVA or Friedman's test was performed, where appropriate, to test the effects of the within-subject factors ‘pretreatment’ and ‘treatment’ (see Table 1), for both the call rate and for each call subtype expressed as a proportion of all calls. In addition, for Experiments 4, 6a, and 7, a post hoc analysis was performed on non-trill FM calls (ie, all call subtypes except trills, flats, and shorts). All ANOVA p-values were subject to the Huynh–Feldt correction. Multiple comparison tests were performed using Tukey's, Dunnett's, paired t-tests, or Wilcoxon's tests, depending on the type of comparisons to be made and the distribution of the data. For call rate, the latter two tests were subjected to the Holm–Bonferroni (H-B) correction. However, for call subtype analysis, pairwise comparisons were performed using unprotected tests to maintain statistical power. For all tests, a two-tailed p-value <5% was considered significant.
RESULTS
Experiments 1 and 2: Effects of Clonidine and Prazosin
As expected, AMPH administered alone (ie, with vehicle pretreatment) significantly increased the overall rate of calling (ie, sum of all 50-kHz call categories emitted per minute) (Figure 2a and b). This effect was significantly reduced by the lowest dose of the α2 adrenergic agonist clonidine (ie, 10 μg/kg) and abolished by the two higher doses (20 or 100 μg/kg; Figure 2a). Clonidine also seemed to decrease calls when administered alone (ie, under saline treatment; Friedman test, Q3=12.97, p<0.01; Figure 2a), but no individual dose of clonidine exerted a significant effect (Wilcoxon's tests with H-B correction, Z⩽2.37, NS). The α1 antagonist prazosin alone significantly inhibited calling (Friedman test, Q2=18.48, p<0.001; Figure 2b), and even the lower dose (0.3 mg/kg) of this drug virtually abolished AMPH-induced calling (Wilcoxon's test with H-B correction, Z=2.59, p<0.01).
Experiments 1 and 2: Clonidine and prazosin dose dependently decreased the 50-kHz call rate (ie, calls of all categories). The y axis represents mean+SEM calls/min. Each rat was tested under all conditions (clonidine group n=12, prazosin group n=12). AMPH administration only significantly increased the call rate when rats were pretreated with vehicle (a, b) or with the lowest dose of clonidine (panel a). Under AMPH treatment, clonidine (panel a) and prazosin pretreatment (panel b) dose dependently reduced the call rate. Prazosin alone (ie, with saline treatment) also decreased the call rate at both doses tested. Clonidine (ie, saline treatment) appeared to decrease calls when administered alone (Friedman test, p<0.01), but the trend did not reach statistical significance for any individual dose (p>0.05). All pairwise comparisons were made by Wilcoxon's tests with Holm–Bonferroni (H-B) correction, n=12 (per experiment). ^p<0.05, ^^p<0.01 vs the corresponding saline treatment (ie, same pretreatment), ##p<0.01 vs VEH+saline condition, *p<0.05, **p<0.01 vs corresponding VEH pretreatment condition.
Clonidine and prazosin also modified the call profile. As many rats failed to make any calls at higher doses of these drugs, analysis was restricted to the following low-dose conditions: (1) AMPH alone vs clonidine (10 μg/kg)+AMPH and (2) all four combinations of vehicle or prazosin (0.3 mg/kg) with saline or AMPH. In the presence of AMPH, clonidine increased the proportion of multi-step calls, while decreasing the proportion of flat–trill combination calls (paired t-tests, t8=2.74 and t8=2.83, respectively, both p<0.05; see Supplementary Figure S1). Prazosin (0.3 mg/kg) blocked the AMPH-induced increase in the proportion of ‘trills’ and ‘trills with jumps’ (Figure 3; ANOVA pretreatment × treatment interactions: trills: F1,7=6.74, p=0.036; trills with jumps: F1,7=23.31, p<0.01).
Experiment 2: Prazosin inhibited or blocked the AMPH-induced increase in the percentage of trills (a) and trills with jumps (b). The y axes represent mean+SEM percentage. Each rat was tested under all conditions (n=12). Both two-way ANOVA interactions were significant (see main text). *p<0.05, **p<0.01 vs corresponding vehicle/saline condition (paired t-tests).
Experiment 3: Effects of Atipamezole and Cirazoline
3a: Effect of atipamezole and cirazoline alone
Neither dose of the α2 antagonist atipamezole (0.3 and 1 mg/kg), administered alone, significantly altered the call rate (Figure 4a) or altered the call profile (data not shown). The α1 agonist cirazoline at both doses tested (0.5 and 1 mg/kg) produced observable changes in the behavior in all rats, such that they disengaged from their cage mate and reared in one corner of the cage. In the first three test days, two rats died shortly after receiving either 0.5 or 1 mg/kg cirazoline, possibly due to pulmonary edema (Micheletti et al, 1987). Consequently, saline injection was substituted for cirazoline for the remainder of the experiment. Among rats that received cirazoline (n=5), there was an apparent but non-significant decrease in the call rate (mean±SEM values for saline and 1 mg/kg cirazoline were 10.7±5.4 and 1.0±1.0 calls/min, respectively).
Experiment 3: (a) AMPH increased the call rate, whereas atipamezole (0.3 and 1 mg/kg ATI; n=10) administered alone had no significant effect. The y axis represents the mean+SEM call rate per minute. ***p<0.001 vs saline condition (paired t-test) (b) AMPH increased the call rate in rats pretreated with saline or atipamezole. Atipamezole alone did not significantly increase the call rate. The y axis represents the mean+SEM call rate per minute. Filled bars correspond to AMPH treatment and open bars correspond to saline treatment. Each rat was tested under all conditions (n=9). *p<0.05, ***p<0.001 compared with the same pretreatment with saline challenge (paired t-tests).
3b: Effect of atipamezole in combination with AMPH
Atipamezole (1 mg/kg) alone tended to increase the call rate in this experiment, but not significantly (Wilcoxon's test, Z=1.89, p=0.0584; Figure 4b). Atipamezole did not affect the call rate under AMPH (Wilcoxon's test, Z=0.41, NS; Figure 4b), and only had moderate effects on the AMPH call profile. In particular, the percentage of short calls, step-ups, and step-downs was increased by atipamezole (paired t-tests, t8=2.43–3.08, each p<0.05). Mean±SEM values in the presence vs absence of atipamezole were 17.4±3.1% vs 10.4±1.8% (short calls), 11.5±2.3% vs 6.5±2.3% (step-ups), and 4.1±0.9% vs 2.1±0.7% (step-downs), respectively.
Experiment 4: Effect of Propranolol
Propranolol failed to change the call rate significantly (Figure 5). Although propranolol seemed to depress calling when administered alone, no dose differed significantly from saline in this respect, even before correction for multiple comparisons (Wilcoxon's tests, Z⩽1.96, NS for each dose). Propranolol also failed to affect ‘AMPH-induced’ calls (ie, AMPH minus saline difference score; ANOVA F3,21=1.86, NS; uncorrected paired t-tests, t7=0.4–1.16, NS). In contrast, propranolol had a striking effect on the types of calls emitted (Supplementary Figure S2). In particular, under AMPH, propranolol dose dependently promoted flat calls while nearly abolishing trill calls (ANOVA: flat calls F3,21=23.9, p<0.0001; trills F3,21=5.66, p<0.05; see Table 2 for t-statistics comparing each propranolol dose with saline; Figure 6a). In contrast, all other non-trill FM calls collectively remained constant across propranolol doses (ANOVA F3,21=0.18, NS; Figure 6b). The absolute number of trills, flats, and non-trill FM calls are provided in Supplementary Table S1.
Experiment 4: AMPH-induced 50-kHz call rate was not altered by propranolol. The y axis shows mean+SEM calls/min (n=8). Each rat was tested under all conditions. AMPH increased the call rate at all doses of propranolol (Wilcoxon's tests: p<0.05). No dose of propranolol significantly altered the call rate under AMPH (paired t-tests, p>0.05) or when administered alone (Wilcoxon's tests, p>0.05). All other pairwise comparisons were subjected to H-B corrections.
Experiment 4: Propranolol promoted flat calls and inhibited trill calls under AMPH. Line graphs showing (a) the dose-dependent increase in flat calls and concomitant decrease in trills, and (b) no significant difference in non-trill frequency-modulated calls, expressed as mean±SEM percentage of total calls emitted (ie, calls of all 50-kHz categories). *p<0.05, **p<0.01, ***p<0.001 compared with vehicle (VEH) pretreatment (paired t-tests, n=8).
Experiment 5: Effects of Betaxolol, ICI 118,551, and Nadolol
In this experiment, the effects of the selective β1 adrenergic antagonist betaxolol, the selective β2 adrenergic antagonist ICI 118,551, and the hydrophilic β1/β2 blocker nadolol were examined. As with propranolol, none of these agents significantly affected the rate of calling after saline or AMPH treatment (Wilcoxon's tests; saline treatment: Z=0.62–0.89, NS; AMPH treatment: Z=0.53–1.95, NS; Figure 7). Analysis of individual call subtypes was restricted to AMPH treatment conditions, as saline test session yielded few calls (Figure 8). Propranolol again caused a highly significant shift in the call profile under AMPH (paired t-tests: proportion of (1) trills, t10=6.54, p<0.001; (2) flat calls, t10=4.45, p<0.01) (Figure 8a and b). Here, propranolol also had effects on other call subtypes: propranolol increased the proportion of flat–trill combinations (paired t-test, t10=2.4, p<0.05) and split calls (paired t-test, t10=2.47, p<0.05) (Figure 8c and d). However, betaxolol, ICI 118,551, and nadolol were all without effect on call profile (Figure 8). The absolute number of trills, flats, flat–trill combinations, and split calls are provided in Supplementary Table S2.
Experiment 5: AMPH-induced 50-kHz calling was not altered by propranolol (PRO; 10 mg/kg, IP), betaxolol (BET; 1 mg/kg, IP), ICI 118,551 (ICI; 0.2 mg/kg, IP), or nadolol (NDL; 5 mg/kg, IP). AMPH robustly increased the call rate under all pretreatment conditions (Wilcoxon's tests: p<0.05–0.003). No pretreatment affected the call rate when administered alone (Wilcoxon's tests: p>0.05) or when combined with AMPH (Wilcoxon's tests: p>0.05). The y axis represents mean+SEM calls/min. Each rat was tested under all conditions (n=11). All pairwise comparisons were subjected to H-B corrections.
Experiment 5: Propranolol decreased the percentage of trills (a) and increased the percentage of flats, flat–trill combinations, and splits (b–d) under AMPH. The y axis represents mean+SEM percentage of total calls (ie, all 50-kHz categories). Each rat was tested under all conditions (n=11). *p<0.05, **p<0.01, ***p<0.001 vs vehicle pretreatment condition (paired t-tests).
Given the possible sensitizing effects of AMPH on USVs (Ahrens et al, 2009), we assessed order effects by examining the call rate under AMPH as a function of the number of times the rat was exposed to AMPH. The call rate did not change significantly over multiple AMPH exposures in this experiment (Supplementary Figure S3).
Experiment 6: Effects of NAD-299 and Higher Doses of Betaxolol and ICI 118,551
The findings of Experiment 5 indicated that the observed effects of propranolol might require simultaneous β1/β2 receptor blockade, or might result from this drug's ability to antagonize 5HT1A receptors; alternatively, our doses of betaxolol and ICI 118,551, chosen to ensure β1 vs β2 selectivity in vivo (see ‘Notes’ in Supplementary Material), might have been insufficient. Therefore, Experiment 6 examined the effects of (1) higher doses of betaxolol and ICI 118,551 alone or in combination and (2) the selective 5HT1A antagonist NAD-299.
6a: Effects of betaxolol and ICI 118,551 in combination and NAD-299
AMPH treatment again produced a highly significant increase in call rate, and this effect was unaltered by pretreatment with either propranolol, the combination of betaxolol and ICI 118,551, or NAD-299 (Tukey's test: AMPH treatment conditions vs saline, q=9.07–11. 22, each p<0.001; AMPH treatment alone vs drug pretreatment+AMPH, q=0.35–1.80, NS; Supplementary Figure S4). As before, propranolol normalized the trill/flat profile shift induced by AMPH (Figure 9a and b; see Table 3 for statistical details), and in addition, it caused a significant decrease in the proportion of short calls (Figure 9c). The betaxolol/ICI 118,551 combination mimicked these effects of propranolol, whereas NAD-299 was without significant effect (Figure 9a–c). However, propranolol also caused an increase in the proportion of split calls, an effect not observed with the betaxolol/ICI 118,551 combination or with NAD-299 (Figure 9d). There was no significant change in the proportion of non-trill FM calls after any pretreatment in this experiment (Figure 9e).
Experiment 6a: Propranolol (PRO; 10 mg/kg, IP) and the combination of betaxolol and ICI 118,551 (BET/ICI; 2.5 and 1 mg/kg IP, respectively) increased the percentage of flat calls under AMPH (a) while decreasing the percentage of trills (b) and shorts (c). In this experiment, propranolol also significantly increased the percentage of split calls (d), an effect not observed with the betaxolol/ICI 118,551 combination. There was no significant effect of any pretreatment on non-trill frequency-modulated calls (e). All pairwise comparisons between the PRO vs BET/ICI conditions were non-significant (paired t-tests, p=0.07–0.81). NAD-299 failed to affect the percentage of any calls emitted. The y axis shows mean+SEM percent of total calls (ie, all subtypes) (n=12). Pretreatments are listed immediately below the x axes, and saline or AMPH treatment conditions are indicated underneath each graph. *p<0.05, **p<0.01, ***p<0.001 compared with the VEH/AMPH condition.
6b: Effect of betaxolol and ICI 118,551 alone at higher doses
Here, betaxolol or ICI 118,551 was tested individually at the same doses as used in Experiment 6a (2.5 and 1 mg/kg, respectively) in combination with AMPH (1 mg/kg, IP). Neither antagonist affected USV rate or profile (Supplementary Figures S5 and S6).
Experiment 7: Effect of IV Cocaine and AMPH on 50-kHz USVs
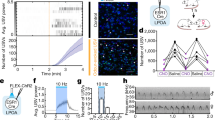
The dose of AMPH used in this experiment (0.5 mg/kg IV) was chosen based on a preliminary dose-response study (0.1, 0.5, 1, and 2 mg/kg, IV; Supplementary Figure S7). Only AMPH and the 0.75 mg/kg dose of cocaine significantly increased the call rate compared with saline treatment, and cocaine was less effective than AMPH in this regard (Tukey's test: AMPH vs saline, q=10.19, p<0.001; 0.75 mg/kg cocaine vs saline, q=4.08, p<0.05; AMPH vs each cocaine dose, q=6.11–8.66, all p<0.001; Figure 10a). Analysis restricted to FM calls showed the same pattern of effects (Supplementary Figure S8). Under AMPH, the call rate increased detectably within the first 30 s after infusion (paired t-test vs saline, t11=3.12, p<0.01), and this drug effect peaked between 180 and 210 s (Figure 10b). Cocaine (0.75 mg/kg) produced a significant increase in the call rate 60–90 s after the infusion (paired t-test vs saline, t11=2.27, p<0.05), and this effect peaked between 120 and 150 s (Figure 10b).
Experiment 7: Cocaine (0.25, 0.75, 1.5 mg/kg, IV) dose dependently increased the number of USVs emitted by rats, but significantly less so than amphetamine (0.5 mg/kg IV; AMPH). (a) The rate of 50-kHz calling was averaged 0–10 min after injection and is expressed as calls/min (mean+SEM). Each rat was tested under all conditions (n=12). Only AMPH and 0.75 mg/kg cocaine significantly increased the call rate. *p<0.05, ***p<0.001 vs corresponding saline (VEH) condition, #p<0.001 vs the corresponding AMPH condition (Tukey's test). (b) Time course of the call rate after AMPH (0.5 mg/kg, IV) or cocaine (0.25, 0.75, and 1.5 mg/kg, IV) administration. The x axis refers to the time after the end of the 10-s infusion. For visual clarity, only the VEH, AMPH, and the 0.75 mg/kg doses of cocaine (ie, the most effective dose of cocaine on the call rate) are illustrated.
Although cocaine only modestly affected call rate, it produced a highly significant shift in the call profile at all doses tested (Figure 11). In this respect, it closely mimicked the effect of AMPH, such that trill calls proportionally increased while flat calls decreased (Dunnett's tests vs saline: trills, q=2.67–4.35, p<0.01–0.05; flat calls, q=3.25–4.53, p<0.01 for each comparison). There was no change in the proportion of non-trill FM calls under AMPH or cocaine (Dunnett's test vs saline: q=0.35–2.05, NS).
Experiment 7: AMPH (0.5 mg/kg, IV) and all doses of cocaine (0.25, 0.75, and 1.5 mg/kg, IV) promoted trill calls while suppressing flat calls. The y axis represents the percentage of the total calls that were trills, flat calls, and non-trill frequency-modulated calls for each drug/dose condition (mean+SEM, n=12). *p<0.05, **p<0.01, ##p<0.01 vs corresponding VEH (ie, saline) condition (Dunnett's tests).
DISCUSSION
Previous investigations relating noradrenergic mechanisms to rat USV emission have almost exclusively focused on adult 22-kHz USVs (McIntosh and Barfield, 1984) or pup calls (Blumberg et al, 2005); both types of call appear to be functionally distinct from the 50-kHz calls emitted by adult rats (Portfors, 2007). To our knowledge, the only previous report of a potential noradrenergic contribution to adult rat 50-kHz USVs was in the context of social stress (Tornatzky and Miczek, 1994). Hence, this study is the first to examine the association between NA and 50-kHz USV production in unstressed adult rats.
Pharmacological Considerations
As discussed below, the effects of prazosin, clonidine, and propranolol observed in this study are likely mediated through α1, α2, and β1/β2 adrenergic receptors, respectively. Doses of prazosin were based on the drug's potency in the following in vivo assays: α1 radiotracer binding (Couch et al, 1988), antagonism of an α1 agonist cue (Schechter, 1991), and inhibition the psychomotor stimulant effects of AMPH (Selken and Nichols, 2007; Vanderschuren et al, 2003). Prazosin, at the doses used in this study, is highly α1-selective, with negligible affinity for α2 or β adrenergic, DA, and serotonin receptors (Balle et al, 2003; Clineschmidt et al, 1979; Miach et al, 1980; Sanger, 1989) or for imidazoline sites (Angel et al, 1995). However, prazosin also binds to melatonin MT3 receptors, although with significantly lower affinity than to α1 receptors (Doxey et al, 1984; Molinari et al, 1996; Pickering and Niles, 1990). The function of the MT3 receptor remains poorly characterized, except in the regulation of intraocular pressure (Pintor et al, 2001). Therefore, on present evidence it is not clear whether MT3 antagonism would produce detectable behavioral effects.
Clonidine acts as a potent agonist at both α2 adrenergic and I1-imidazoline receptors (Edwards et al, 2001). In the dose range administered (0.01–0.1 mg/kg), clonidine would be expected to dose dependently stimulate α2 autoreceptors (Drew et al, 1979), thereby inhibiting release and turnover of NA (Anden et al, 1970; Sacchetti et al, 2001). Moreover, within this dose range, clonidine (0.04 mg/kg) produced an α2 receptor-mediated drug cue without detectable α1- or β-receptor activity (Bennett and Lal, 1982). However, clonidine probably also activated I1-imidazoline receptors. These receptors have been proposed to contribute to the CNS control of blood pressure (Holt, 2003) and to modulate aversive effects of opiate withdrawal (Georges et al, 2005). As the neuropharmacological and behavioral consequences of I1-imidazoline receptor stimulation are largely unknown, we cannot exclude their possible role in USV inhibition by clonidine.
Propranolol selectively antagonizes β1, β2, and 5HT1A receptors (Middlemiss and Tricklebank, 1992), while possessing much lower affinity for β3 receptors (Baker, 2005). Several observations suggest that 5HT1A receptors did not contribute to the call profile-changing effect of propranolol under AMPH. First, the highly selective 5HT1A antagonist NAD-299 (Ross et al, 1999) failed to affect USVs in this study, even when administered in a dose (0.2 mg/kg) beyond that required to inhibit in vivo responses to the 5HT1A agonist 8-OH-DPAT (Arborelius et al, 1999; Johansson et al, 1997). Second, the highest dose of propranolol used here (ie, 10 mg/kg) did not inhibit 8-OH-DPAT effects on 5HT release (Sharp et al, 1989). Third, the effects of propranolol observed in this study were mimicked by co-administration of selective β1 and β2 antagonists (ie, betaxolol and ICI 118,551), neither of which interact significantly with the 5HT1A receptor (Middlemiss et al, 1985). Finally, our negative finding with nadolol, a non-CNS penetrant β-adrenergic antagonist (Schiff and Saxey, 1984), suggests that propranolol's effects on ultrasonic calling depend on central β1 and/or β2 receptors.
Behavioral Considerations
Clonidine and prazosin
Both clonidine and prazosin, when administered alone, inhibited USV emission. An inhibitory effect of high-dose clonidine (ie, 0.1 mg/kg) is consistent with its known sedative effects (Drew et al, 1979). The inhibitory effects of lower doses of clonidine (ie, 0.01 and 0.02 mg/kg IP) are perhaps attributable to mild sedation, which has been seen in some (Carey et al, 2008; Drew et al, 1979; Sara et al, 1995) but not in all (De Luca et al, 1999; Skolnick et al, 1978) studies. Prazosin, in contrast, inhibited 50-kHz calling at doses that are clearly non-sedative (Drouin et al, 2002; Vanderschuren et al, 2003).
Both clonidine and prazosin dose dependently inhibited AMPH-induced calling, with partial-to-complete block even at low doses. It is unlikely that these drugs produced aversive effects, which might have inhibited 50-kHz calling. Clonidine, for example, is self-administered IV (Davis and Smith, 1977) and induces CPP (Asin and Wirtshafter, 1985; Cervo et al, 1993) in rats, whereas prazosin seems motivationally neutral (Forget et al, 2009; Zarrindast et al, 2002). The inhibitory effect of prazosin is potentially interesting in view of its reported failure to block either the discriminative stimulus effects of AMPH in rats (Arnt, 1996; West et al, 1995) or the acquisition of AMPH CPP (Hoffman and Donovan, 1995).
Although clonidine and prazosin, at doses used here, also suppress AMPH-induced locomotion (Drouin et al, 2002; Vanderschuren et al, 2003), the act of locomotion per se does not seem to cause rats to emit ultrasonic calls (Knutson et al, 2002).
Cirazoline and atipamezole
The α1 agonist cirazoline failed to increase the call rate significantly or modify the call profile, when administered alone. However, cirazoline (0.5. and 1 mg/kg) produced major adverse side effects after injection, most likely due to its action on peripheral α1 receptors (Micheletti et al, 1987). Thus, it remains unclear whether activation of central α1 receptors without the peripheral side effects would elicit 50-kHz USVs. Surprisingly, comparable or even higher doses of cirazoline have been used in several other studies of conscious rats (Alsene et al, 2006; Sebban et al, 1999; Swerdlow et al, 2006).
In contrast, the highly selective α2 antagonist atipamezole (Virtanen et al, 1989) did not produce any observable changes in behavior. Doses of atipamezole were chosen based on previous studies showing increased extracellular NA levels in the brain (Bondi et al, 2010; Wortley et al, 1999). The lack of effect of atipamezole on call rate suggests that increased NA release resulting from α2 receptor antagonism is not sufficient to elicit USVs. Moreover, the effect of atipamezole on USVs under AMPH suggests that α2 receptor inhibition does not affect AMPH-induced call rate, but may modestly contribute to AMPH's ability to modify the call profile.
Propranolol
This study reveals potentially novel psychostimulant effects that are mediated by CNS β-receptors. Propranolol profoundly altered the call profile in rats that were acutely challenged with AMPH. Thus, propranolol suppressed trill calls and promoted flat calls, effectively countering the profile-altering effects exerted by AMPH alone. Additional tests with betaxolol, ICI 118,551, nadolol, and NAD-299 implicated centrally located β-receptors. In contrast, propranolol did not inhibit the AMPH-induced enhancement of call rate, a result that may possibly be related to propranolol's inability to inhibit behavioral stimulant effects of AMPH (Simon et al, 1972; Vanderschuren et al, 2003). As both USVs and discriminative stimulus (cue) properties have been proposed to model subjective effects of drugs, it is of interest that propranolol antagonized AMPH's effects on call profile (this study) at doses that failed to inhibit the AMPH cue (West et al, 1995).
Remarkably, the effects of β-blockers on conventional measures of psychostimulant reward or aversion have received little attention in animals. For example, there seem to be no reports of CPP/aversion testing using propranolol. In an initial study, acute propranolol administration inhibited IV self-administration of AMPH in rats (Yokel and Wise, 1976). In addition, propranolol substantially reduced cocaine IVSA (Harris et al, 1996). Thus, in light of these findings, CNS β-adrenergic receptors warrant further attention in the context of psychostimulant reward and aversion.
50-KHz USVs in Relation to Subjective Drug Effects in Humans
In human subjects, there is considerable debate as to the relative importance of dopaminergic and noradrenergic mechanisms in the positive subjective effects of AMPH (Abi-Dargham et al, 2003; Brauer and de Wit, 1997; Dlugos et al, 2007; Jonsson, 1972; Leyton et al, 2007; Lott et al, 2005; Nurnberger et al, 1984; Rothman et al, 2001; Sofuoglu et al, 2009). For example, dopaminergic antagonists have failed to reduce psychostimulant euphoria in most studies (Brauer and de Wit, 1995, 1996, 1997; Gawin, 1986; but see Gunne et al (1972) and Jonsson (1972)). Moreover, human and animal studies suggest that DA transmission does not contribute to the hedonic impact of psychostimulants, but rather to the incentive salience of reward-related cues (Berridge and Robinson, 1998; Leyton et al, 2005, 2007). In contrast, several observations point to possible noradrenergic mediation of AMPH euphoria (Dlugos et al, 2007; Rothman et al, 2001; Sofuoglu et al, 2009); although preliminary studies using α- or β-receptor antagonists have been largely negative, only low antagonist doses were used (Brauer and de Wit, 1995; Jonsson, 1972; Nurnberger et al, 1984).
FM 50-kHz calls have been proposed as an index of positive affect in rats (Burgdorf et al, 2010). Accordingly, this study confirmed that AMPH selectively promotes trill calls (this study; Wright et al, 2010) at doses that are comparable to euphorigenic doses in human studies (Grilly and Loveland, 2001). Propranolol countered this call profile shift. In humans, the impact of β-receptor blockade on the euphoric effect of AMPH has been investigated in only two studies (Jonsson, 1972; Nurnberger et al, 1984), to our knowledge. Both studies used propranolol and were ostensibly negative. However, in the first of these, an unusually high dose of AMPH (200 mg, ie, ∼3 mg/kg IV) was combined with only moderate doses of propranolol (20 and 40 mg PO). In the second, the dose of AMPH was lower (0.3 mg/kg IV), but subjective effects were inferred only from the subjects’ behavior; here, too, it is not clear whether propranolol (0.1 mg/kg IV) was administered in a sufficiently high dose. Therefore, our preclinical findings suggest that CNS β-receptor mechanisms would merit further study in humans under AMPH challenge.
Possible (Nor)Adrenaline–DA Interactions
USV emission by adult rats is not only influenced by (nor)adrenergic mechanisms (this study) but is also strongly DA dependent (see the ‘Introduction’ section). These neurotransmitter systems are extensively coupled (for review, see Weinshenker and Schroeder (2007)); for example, a number of studies have shown a critical role of noradrenergic transmission in AMPH-induced mesoaccumbens DA release (Darracq et al, 1998; Pan et al, 1996). However, it seems unlikely that clonidine, prazosin, or propranolol interfered with dopaminergic agonist actions of AMPH in this study. For example, prazosin (0.5 mg/kg IP) did not affect extracellular DA in the nucleus accumbens after systemic AMPH administration (Darracq et al, 1998). Similarly, clonidine failed to alter AMPH-induced extracellular DA levels (Florin et al, 1994; Tanda et al, 1996). Finally, propranolol administration did not inhibit several DA-dependent behavioral effects of AMPH, ie, locomotor stimulation (Simon et al, 1972; Vanderschuren et al, 2003), stereotypy (Simon et al, 1972), and cue properties (West et al, 1995).
Generalization to IV Cocaine and AMPH
Acute IP cocaine administration reportedly increases 50-kHz call rate (Williams and Undieh, 2010). Previous studies using IV cocaine have been performed in the context of self-administration (and its anticipation) and sensitization (Barker et al, 2010; Browning et al, 2011; Ma et al, 2010; Maier et al, 2010). Here, we provide the first report of the effects of non-contingent IV administration of cocaine on USVs. Cocaine increased the call rate at the 0.75 mg/kg dose, with a rapid onset (peak effect 120–150 s after infusion). Although this USV rate-enhancing effect of cocaine was less pronounced than that of AMPH, cocaine nevertheless produced a profound AMPH-like shift in the call profile at all doses tested (ie, 0.25–1.5 mg/kg). In this dose range, cocaine maintains self-administration (Roberts et al, 2007) and induces CPP (Nomikos and Spyraki, 1988; Sellings et al, 2006), but is also anxiogenic (Ettenberg, 2004); how these effects may relate to USV emission merits further investigation.
Information Gained from 50-kHz Call Subtype Analysis vs Call Rate
Several findings of this study highlight the importance of detailed call subtype analysis. First, both cocaine and propranolol changed the propensity to emit different call subtypes at doses that did not significantly change the call rate. These results add to evidence that call rate and profile can be manipulated independently by drugs or lesions (Ciucci et al, 2009, 2007). Moreover, although several groups currently distinguish between FM and flat 50-kHz calls (Ahrens et al, 2009; Burgdorf et al, 2007, 2008a; Burgdorf and Panksepp, 2006; Simola et al, 2009; Wohr et al, 2008), only a few investigators have extended their analysis beyond those two classes (Ciucci et al, 2009; Kaltwasser, 1990; Takahashi et al, 2010; Vivian and Miczek, 1993; White et al, 1990; Wright et al, 2010). Importantly, our detailed analysis reveals that the prevalent trill call subtype (Wright et al, 2010) is not representative of all FM calls.
Human psychostimulant abusers cannot readily discriminate between cocaine and AMPH (Fischman et al, 1976). In this study, cocaine affected the FM call rate less than AMPH, yet produced an equivalent shift in the call profile (ie, preferentially promoting trills over flat calls). Therefore, insofar as FM 50-kHz calls convey information about positive affect in rats (as proposed by Burgdorf et al (2010)), the call profile might be more pertinent than the absolute FM call rate.
Limitations and Methodological Considerations
Adult rats vary considerably in their USV response to various stimuli including systemic AMPH (Burgdorf and Panksepp, 2006; Schwarting et al, 2007; Wohr et al, 2008; Wright et al, 2010). To study the effects of drugs on AMPH-induced calling, it was necessary to exclude low responders based on an initial test screen. However, it is important to bear in mind that low- and high-calling rats may differ in other behavioral or neurochemical respects (Burgdorf et al, 2008b). The test screen likely explains why we did not subsequently observe sensitization with repeated exposure to AMPH during the experiment, as USV sensitization seems to occur mainly within the first three exposures to cocaine or AMPH (Ahrens et al, 2009; Meyer et al, 2011; Mu et al, 2009).
These findings strongly indicate a (nor)adrenergic role in AMPH-induced 50-kHz USVs. However, the evidence for α1 receptor mediation rests on the use of a single drug—prazosin. Although prazosin is a well-characterized and selective α1 receptor antagonist (see above), it would have been desirable to test other drugs of the same class. However, other currently available α1 antagonists are either less α1-selective (eg, phentolamine), α1 subtype selective (eg, tamsulosin), brain impenetrant (eg, doxazosin), or little characterized in the rat (eg, HEAT).
In this study, only prazosin significantly inhibited 50-kHz calling when administered alone. However, rates of spontaneous calling were generally low, making it hard to detect potential suppressive effects of other drugs. To determine whether noradrenergic transmission has a wider role in USV production, it would be informative to test these drugs in combination with non-pharmacological stimuli that evoke high rates of 50-kHz calling (Ciucci et al, 2007; Panksepp and Burgdorf, 2000).
Conclusions
These findings provide the first evidence of (nor)adrenergic involvement in the elicitation of adult rat 50-kHz USVs by AMPH. Furthermore, USV emission seems to be differentially associated with α1- vs β-receptor mechanisms, whereby (nor)adrenergic transmission through α1 receptors principally modulates the call rate, whereas NA (or adrenaline) acting on β-receptors affects the acoustic subtypes of 50-kHz calls emitted.
In the context of drug addiction, psychostimulants reinforce self-administration behavior and acutely promote positive affect. At present, it is not clear how these two effects are related. Dopaminergic transmission in the brain seems critical to motivation, but has not been convincingly linked to psychostimulant euphoria. Preliminary evidence points to a noradrenergic contribution to euphorigenic effects of AMPH, but receptor mechanisms have not been identified. These findings suggest that CNS β-adrenergic receptors merit further attention in this regard.
References
Abi-Dargham A, Kegeles LS, Martinez D, Innis RB, Laruelle M (2003). Dopamine mediation of positive reinforcing effects of amphetamine in stimulant naive healthy volunteers: results from a large cohort. Eur Neuropsychopharmacol 13: 459–468.
Ahrens AM, Ma ST, Maier EY, Duvauchelle CL, Schallert T (2009). Repeated intravenous amphetamine exposure: rapid and persistent sensitization of 50-kHz ultrasonic trill calls in rats. Behav Brain Res 197: 205–209.
Alsene KM, Carasso BS, Connors EE, Bakshi VP (2006). Disruption of prepulse inhibition after stimulation of central but not peripheral alpha-1 adrenergic receptors. Neuropsychopharmacology 31: 2150–2161.
Anden NE, Corrodi H, Fuxe K, Hokfelt B, Hokfelt T, Rydin C et al (1970). Evidence for a central noradrenaline receptor stimulation by clonidine. Life Sci 9: 513–523.
Angel I, Le RM, Pimoule C, Graham D, Arbilla S (1995). [3H]cirazoline as a tool for the characterization of imidazoline sites. Ann N Y Acad Sci 763: 112–124.
Arborelius L, Wallsten C, Ahlenius S, Svensson TH (1999). The 5-HT(1A) receptor antagonist robalzotan completely reverses citalopram-induced inhibition of serotonergic cell firing. Eur J Pharmacol 382: 133–138.
Arnt J (1996). Inhibitory effects on the discriminative stimulus properties of D-amphetamine by classical and newer antipsychotics do not correlate with antipsychotic activity. Relation to effects on the reward system? Psychopharmacology (Berl) 124: 117–125.
Asin KE, Wirtshafter D (1985). Clonidine produces a conditioned place preference in rats. Psychopharmacology (Berl) 85: 383–385.
Baker JG (2005). The selectivity of beta-adrenoceptor antagonists at the human beta1, beta2 and beta3 adrenoceptors. Br J Pharmacol 144: 317–322.
Balle T, Perregaard J, Ramirez MT, Larsen AK, Soby KK, Liljefors T et al (2003). Synthesis and structure-affinity relationship investigations of 5-heteroaryl-substituted analogues of the antipsychotic sertindole. A new class of highly selective alpha(1) adrenoceptor antagonists. J Med Chem 46: 265–283.
Barker DJ, Root DH, Ma S, Jha S, Megehee L, Pawlak AP et al (2010). Dose-dependent differences in short ultrasonic vocalizations emitted by rats during cocaine self-administration. Psychopharmacology (Berl) 211: 435–442.
Bennett DA, Lal H (1982). Discriminative stimuli produced by clonidine: an investigation of the possible relationship to adrenoceptor stimulation and hypotension. J Pharmacol Exp Ther 223: 642–648.
Berridge KC, Robinson TE (1998). What is the role of dopamine in reward: hedonic impact, reward learning, or incentive salience? Brain Res Brain Res Rev 28: 309–369.
Blumberg MS, Johnson ED, Middlemis-Brown JE (2005). Inhibition of ultrasonic vocalizations by beta-adrenoceptor agonists. Dev Psychobiol 47: 66–76.
Bondi CO, Jett JD, Morilak DA (2010). Beneficial effects of desipramine on cognitive function of chronically stressed rats are mediated by alpha1-adrenergic receptors in medial prefrontal cortex. Prog Neuropsychopharmacol Biol Psychiatry 34: 913–923.
Brauer LH, de Wit H (1995). Role of dopamine in d-amphetamine-induced euphoria in normal, healthy volunteers. Exp Clin Psychopharmacol 3: 371–381.
Brauer LH, de Wit H (1996). Subjective responses to d-amphetamine alone and after pimozide pretreatment in normal, healthy volunteers. Biol Psychiatry 39: 26–32.
Brauer LH, de Wit H (1997). High dose pimozide does not block amphetamine-induced euphoria in normal volunteers. Pharmacol Biochem Behav 56: 265–272.
Browning JR, Browning DA, Maxwell AO, Dong Y, Jansen HT, Panksepp J et al (2011). Positive affective vocalizations during cocaine and sucrose self-administration: A model for spontaneous drug desire in rats. Neuropharmacology 61: 268–275.
Brudzynski SM (2005). Principles of rat communication: quantitative parameters of ultrasonic calls in rats. Behav Genet 35: 85–92.
Burgdorf J, Knutson B, Panksepp J, Ikemoto S (2001). Nucleus accumbens amphetamine microinjections unconditionally elicit 50-kHz ultrasonic vocalizations in rats. Behav Neurosci 115: 940–944.
Burgdorf J, Kroes RA, Moskal JR, Pfaus JG, Brudzynski SM, Panksepp J (2008a). Ultrasonic vocalizations of rats (Rattus norvegicus) during mating, play, and aggression: behavioral concomitants, relationship to reward, and self-administration of playback. J Comp Psychol 122: 357–367.
Burgdorf J, Moskal JR (2009). Frequency modulated 50 kHz ultrasonic vocalizations reflect a positive emotional state in the rat: neural substrates and therapeutic implications. In: Brudzynski SM (ed). Handbook of Mammalian Vocalization. Academic Press: Oxford. pp 209–214.
Burgdorf J, Panksepp J (2006). The neurobiology of positive emotions. Neurosci Biobehav Rev 30: 173–187.
Burgdorf J, Panksepp J, Brudzynski SM, Beinfeld MC, Cromwell HC, Kroes RA et al (2008b). The effects of selective breeding for differential rates of 50-kHz ultrasonic vocalizations on emotional behavior in rats. Dev Psychobiol 51: 34–46.
Burgdorf J, Panksepp J, Moskal JR (2010). Frequency-modulated 50 kHz ultrasonic vocalizations: a tool for uncovering the molecular substrates of positive affect. Neurosci Biobehav Rev 9: 1831–1836.
Burgdorf J, Wood PL, Kroes RA, Moskal JR, Panksepp J (2007). Neurobiology of 50-kHz ultrasonic vocalizations in rats: electrode mapping, lesion, and pharmacology studies. Behav Brain Res 182: 274–283.
Carey RJ, DePalma G, Shanahan A, Damianopoulos EN, Muller CP, Huston JP (2008). Effects on spontaneous and cocaine-induced behavior of pharmacological inhibition of noradrenergic and serotonergic systems. Pharmacol Biochem Behav 89: 54–63.
Cervo L, Rossi C, Samanin R (1993). Clonidine-induced place preference is mediated by alpha 2-adrenoceptors outside the locus coeruleus. Eur J Pharmacol 238: 201–207.
Ciucci MR, Ahrens AM, Ma ST, Kane JR, Windham EB, Woodlee MT et al (2009). Reduction of dopamine synaptic activity: degradation of 50-kHz ultrasonic vocalization in rats. Behav Neurosci 123: 328–336.
Ciucci MR, Ma ST, Fox C, Kane JR, Ramig LO, Schallert T (2007). Qualitative changes in ultrasonic vocalization in rats after unilateral dopamine depletion or haloperidol: a preliminary study. Behav Brain Res 182: 284–289.
Clineschmidt BV, Flataker LM, Faison E, Holmes R (1979). An in vivo model for investigating alpha 1- and alpha 2-receptors in the CNS: studies with mianserin. Arch Int Pharmacodyn Ther 242: 59–76.
Couch MW, Greer DM, Thonoor CM, Williams CM (1988). In vivo binding in rat brain and radiopharmaceutical preparation of radioiodinated HEAT, an alpha-1 adrenoceptor ligand. J Nucl Med 29: 356–362.
Covington HEI, Miczek KA (2003). Vocalizations during withdrawal from opiates and cocaine: possible expressions of affective distress. Eur J Pharmacol 467: 1–13.
Darracq L, Blanc G, Glowinski J, Tassin JP (1998). Importance of the noradrenaline-dopamine coupling in the locomotor activating effects of D-amphetamine. J Neurosci 18: 2729–2739.
Davis WM, Smith SG (1977). Catecholaminergic mechanisms of reinforcement: direct assessment by drug-self-administration. Life Sci 20: 483–492.
De Luca LAJ, Nunes de Souza RL, Yada MM, Meyer EW (1999). Sedation and need-free salt intake in rats treated with clonidine. Pharmacol Biochem Behav 62: 585–589.
Dlugos A, Freitag C, Hohoff C, McDonald J, Cook EH, Deckert J et al (2007). Norepinephrine transporter gene variation modulates acute response to D-amphetamine. Biol Psychiatry 61: 1296–1305.
Doxey JC, Lane AC, Roach AG, Virdee NK (1984). Comparison of the alpha-adrenoceptor antagonist profiles of idazoxan (RX 781094), yohimbine, rauwolscine and corynanthine. Naunyn Schmiedebergs Arch Pharmacol 325: 136–144.
Drew GM, Gower AJ, Marriott AS (1979). Alpha 2-adrenoceptors mediate clonidine-induced sedation in the rat. Br J Pharmacol 67: 133–141.
Drouin C, Blanc G, Villegier AS, Glowinski J, Tassin JP (2002). Critical role of alpha1-adrenergic receptors in acute and sensitized locomotor effects of D-amphetamine, cocaine, and GBR 12783: influence of preexposure conditions and pharmacological characteristics. Synapse 43: 51–61.
Edwards L, Fishman D, Horowitz P, Bourbon N, Kester M, Ernsberger P (2001). The I1-imidazoline receptor in PC12 pheochromocytoma cells activates protein kinases C, extracellular signal-regulated kinase (ERK) and c-jun N-terminal kinase (JNK). J Neurochem 79: 931–940.
Ettenberg A (2004). Opponent process properties of self-administered cocaine. Neurosci Biobehav Rev 27: 721–728.
Fischman MW, Schuster CR, Resnekov L, Shick JF, Krasnegor NA, Fennell W et al (1976). Cardiovascular and subjective effects of intravenous cocaine administration in humans. Arch Gen Psychiatry 33: 983–989.
Florin SM, Kuczenski R, Segal DS (1994). Regional extracellular norepinephrine responses to amphetamine and cocaine and effects of clonidine pretreatment. Brain Res 654: 53–62.
Foltin RW, Fischman MW (1991). Assessment of abuse liability of stimulant drugs in humans: a methodological survey. Drug Alcohol Depend 28: 3–48.
Forget B, Hamon M, Thiebot MH (2009). Involvement of alpha1-adrenoceptors in conditioned place preference supported by nicotine in rats. Psychopharmacology (Berl) 205: 503–515.
Gawin FH (1986). Neuroleptic reduction of cocaine-induced paranoia but not euphoria? Psychopharmacology (Berl) 90: 142–143.
Georges F, Caille S, Vouillac C, Le MC, Stinus L (2005). Role of imidazoline receptors in the anti-aversive properties of clonidine during opiate withdrawal in rats. Eur J Neurosci 22: 1812–1816.
Grilly DM, Loveland A (2001). What is a ‘low dose’ of d-amphetamine for inducing behavioral effects in laboratory rats? Psychopharmacology (Berl) 153: 155–169.
Gunne LM, Anggard E, Jonsson LE (1972). Clinical trials with amphetamine-blocking drugs. Psychiatr Neurol Neurochir 75: 225–226.
Harris GC, Hedaya MA, Pan WJ, Kalivas P (1996). beta-adrenergic antagonism alters the behavioral and neurochemical responses to cocaine. Neuropsychopharmacology 14: 195–204.
Hoffman DC, Donovan H (1995). Effects of typical, atypical, and novel antipsychotic drugs on amphetamine-induced place conditioning in rats. Drug Dev Res 36: 193–198.
Holt A (2003). Imidazoline binding sites on receptors and enzymes: emerging targets for novel antidepressant drugs? J Psychiatry Neurosci 28: 409–414.
Johansson L, Sohn D, Thorberg SO, Jackson DM, Kelder D, Larsson LG et al (1997). The pharmacological characterization of a novel selective 5-hydroxytryptamine1A receptor antagonist, NAD-299. J Pharmacol Exp Ther 283: 216–225.
Jonsson L-E (1972). Pharmacological blockade of amphetamine effects in amphetamine dependent subjects. Eur J Clin Pharmacol 4: 206–211.
Jonsson LE, Anggard E, Gunne LM (1971). Blockade of intravenous amphetamine euphoria in man. Clin Pharmacol Ther 12: 889–896.
Jonsson LE, Gunne LM, Anggard E (1969). Effects of alpha-methyltyrosine in amphetamine-dependent subjects. Eur J Clin Pharmacol 2: 27–29.
Kaltwasser MT (1990). Acoustic signaling in the black rat (Rattus rattus). J Comp Psychol 104: 227–232.
Knutson B, Burgdorf J, Panksepp J (2002). Ultrasonic vocalizations as indices of affective states in rats. Psychol Bull 128: 961–977.
Leyton M, aan het Rot M, Booij L, Baker GB, Young SN, Benkelfat C (2007). Mood-elevating effects of d-amphetamine and incentive salience: the effect of acute dopamine precursor depletion. J Psychiatry Neurosci 32: 129–136.
Leyton M, Casey KF, Delaney JS, Kolivakis T, Benkelfat C (2005). Cocaine craving, euphoria, and self-administration: a preliminary study of the effect of catecholamine precursor depletion. Behav Neurosci 119: 1619–1627.
Litvin Y, Blanchard DC, Blanchard RJ (2007). Rat 22 kHz ultrasonic vocalizations as alarm cries. Behav Brain Res 182: 166–172.
Lott DC, Kim SJ, Cook Jr EH, de WH (2005). Dopamine transporter gene associated with diminished subjective response to amphetamine. Neuropsychopharmacology 30: 602–609.
Ma ST, Maier EY, Ahrens AM, Schallert T, Duvauchelle CL (2010). Repeated intravenous cocaine experience: development and escalation of pre-drug anticipatory 50-kHz ultrasonic vocalizations in rats. Behav Brain Res 212: 109–114.
Maier EY, Ahrens AM, Ma ST, Schallert T, Duvauchelle CL (2010). Cocaine deprivation effect: cue abstinence over weekends boosts anticipatory 50-kHz ultrasonic vocalizations in rats. Behav Brain Res 214: 75–79.
McIntosh TK, Barfield RJ (1984). Brain monoaminergic control of male reproductive behavior. III. Norepinephrine and the post-ejaculatory refractory period. Behav Brain Res 12: 275–281.
McKittrick CR, Abercrombie ED (2007). Catecholamine mapping within nucleus accumbens: differences in basal and amphetamine-stimulated efflux of norepinephrine and dopamine in shell and core. J Neurochem 100: 1247–1256.
Meyer PJ, Ma ST, Robinson TE (2011). A cocaine cue is more preferred and evokes more frequency-modulated 50-kHz ultrasonic vocalizations in rats prone to attribute incentive salience to a food cue. Psychopharmacology (Berl) (in press).
Miach PJ, Dausse JP, Cardot A, Meyer P (1980). 3H-Prazosin binds specifically to ‘alpha 1’-adrenoceptors in rat brain. Naunyn Schmiedebergs Arch Pharmacol 312: 23–26.
Micheletti G, Warter JM, Marescaux C, Depaulis A, Tranchant C, Rumbach L et al (1987). Effects of drugs affecting noradrenergic neurotransmission in rats with spontaneous petit mal-like seizures. Eur J Pharmacol 135: 397–402.
Middlemiss DN, Neill J, Tricklebank MD (1985). Subtypes of the 5-HT receptor involved in hypothermia and forepaw treading induced by 8-OH-DPAT. Br J Pharmacol 85: 251P.
Middlemiss DN, Tricklebank MD (1992). Centrally active 5-HT receptor agonists and antagonists. Neurosci Biobehav Rev 16: 75–82.
Molinari EJ, North PC, Dubocovich ML (1996). 2-[125I]iodo-5-methoxycarbonylamino-N-acetyltryptamine: a selective radioligand for the characterization of melatonin ML2 binding sites. Eur J Pharmacol 301: 159–168.
Mu P, Fuchs T, Saal DB, Sorg BA, Dong Y, Panksepp J (2009). Repeated cocaine exposure induces sensitization of ultrasonic vocalization in rats. Neurosci Lett 453: 31–35.
Nomikos GG, Spyraki C (1988). Cocaine-induced place conditioning: importance of route of administration and other procedural variables. Psychopharmacology (Berl) 94: 119–125.
Nurnberger JI, Simmons-Alling S, Kessler L, Jimerson S, Schreiber J, Hollander E et al (1984). Separate mechanisms for behavioral, cardiovascular, and hormonal responses to dextroamphetamine in man. Psychopharmacology (Berl) 84: 200–204.
Pan WH, Sung JC, Fuh SM (1996). Locally application of amphetamine into the ventral tegmental area enhances dopamine release in the nucleus accumbens and the medial prefrontal cortex through noradrenergic neurotransmission. J Pharmacol Exp Ther 278: 725–731.
Panksepp J, Burgdorf J (2000). 50-kHz chirping (laughter?) in response to conditioned and unconditioned tickle-induced reward in rats: effects of social housing and genetic variables. Behav Brain Res 115: 25–38.
Pickering DS, Niles LP (1990). Pharmacological characterization of melatonin binding sites in Syrian hamster hypothalamus. Eur J Pharmacol 175: 71–77.
Pintor J, Martin L, Pelaez T, Hoyle CH, Peral A (2001). Involvement of melatonin MT(3) receptors in the regulation of intraocular pressure in rabbits. Eur J Pharmacol 416: 251–254.
Portfors CV (2007). Types and functions of ultrasonic vocalizations in laboratory rats and mice. J Am Assoc Lab Anim Sci 46: 28–34.
Roberts DC, Morgan D, Liu Y (2007). How to make a rat addicted to cocaine. Prog Neuropsychopharmacol Biol Psychiatry 31: 1614–1624.
Ross SB, Thorberg S, Jerning E, Mohell N, Stenfors C, Wallsten C et al (1999). Robalzotan (NAD-299), a novel selective 5-HT1A receptor antagonist. CNS Drug Rev 5: 213–232.
Rothman RB, Baumann MH, Dersch CM, Romero DV, Rice KC, Carroll FI et al (2001). Amphetamine-type central nervous system stimulants release norepinephrine more potently than they release dopamine and serotonin. Synapse 39: 32–41.
Sacchetti G, Bernini M, Gobbi M, Parini S, Pirona L, Mennini T et al (2001). Chronic treatment with desipramine facilitates its effect on extracellular noradrenaline in the rat hippocampus: studies on the role of presynaptic alpha2-adrenoceptors. Naunyn Schmiedebergs Arch Pharmacol 363: 66–72.
Sales GD, Pye D (1974). Ultrasonic Communication by Animals. Chapman and Hall: London.
Sanger DJ (1989). Discriminative stimulus effects of the alpha 2-adrenoceptor antagonist idazoxan. Psychopharmacology (Berl) 99: 117–121.
Sara SJ, Dyon-Laurent C, Herve A (1995). Novelty seeking behavior in the rat is dependent upon the integrity of the noradrenergic system. Brain Res Cogn Brain Res 2: 181–187.
Schechter MD (1991). Discriminative stimulus effect of phenylephrine. Arch Int Pharmacodyn Ther 309: 20–31.
Schiff AA, Saxey A (1984). Autoradiography of nadolol and propranolol in the rat. Xenobiotica 14: 687–691.
Schoffelmeer AN, Mulder AH (1984). Presynaptic opiate receptor- and alpha 2-adrenoceptor-mediated inhibition of noradrenaline release in the rat brain: role of hyperpolarization? Eur J Pharmacol 105: 129–135.
Schwarting RK, Jegan N, Wohr M (2007). Situational factors, conditions and individual variables which can determine ultrasonic vocalizations in male adult Wistar rats. Behav Brain Res 182: 208–222.
Sebban C, Zhang XQ, Tesolin-Decros B, Millan MJ, Spedding M (1999). Changes in EEG spectral power in the prefrontal cortex of conscious rats elicited by drugs interacting with dopaminergic and noradrenergic transmission. Br J Pharmacol 128: 1045–1054.
Segal DS, Kuczenski R (1997). An escalating dose ‘binge’ model of amphetamine psychosis: behavioral and neurochemical characteristics. J Neurosci 17: 2551–2566.
Selken J, Nichols DE (2007). Alpha1-adrenergic receptors mediate the locomotor response to systemic administration of (+/−)-3,4-methylenedioxymethamphetamine (MDMA) in rats. Pharmacol Biochem Behav 86: 622–630.
Sellings LH, McQuade LE, Clarke PB (2006). Evidence for multiple sites within rat ventral striatum mediating cocaine-conditioned place preference and locomotor activation. J Pharmacol Exp Ther 317: 1178–1187.
Sharp T, Bramwell SR, Hjorth S, Grahame-Smith DG (1989). Pharmacological characterization of 8-OH-DPAT-induced inhibition of rat hippocampal 5-HT release in vivo as measured by microdialysis. Br J Pharmacol 98: 989–997.
Simola N, Ma ST, Schallert T (2009). Influence of acute caffeine on 50-kHz ultrasonic vocalizations in male adult rats and relevance to caffeine-mediated psychopharmacological effects. Int J Neuropsychopharmacol 13: 123–132.
Simon P, Chermat R, Fosset MT, Boissier JR (1972). [Adrenergic blocking agents and amphetamine or apomorphine induced stereotyped behavior in rats]. Psychopharmacologia 23: 357–364.
Skolnick P, Daly JW, Segal DS (1978). Neurochemical and behavioral effects of clonidine and related imidazolines: interaction with alpha-adrenoceptors. Eur J Pharmacol 47: 451–455.
Snoddy AM, Tessel RE (1983). Nisoxetine and amphetamine share discriminative stimulus properties in mice. Pharmacol Biochem Behav 19: 205–210.
Snoddy AM, Tessel RE (1985). Prazosin: effect on psychomotor-stimulant cues and locomotor activity in mice. Eur J Pharmacol 116: 221–228.
Sofuoglu M, Poling J, Hill K, Kosten T (2009). Atomoxetine attenuates dextroamphetamine effects in humans. Am J Drug Alcohol Abuse 35: 412–416.
Stolerman I (1992). Drugs of abuse: behavioural principles, methods and terms. Trends Pharmacol Sci 13: 170–176.
Swerdlow NR, Bongiovanni MJ, Tochen L, Shoemaker JM (2006). Separable noradrenergic and dopaminergic regulation of prepulse inhibition in rats: implications for predictive validity and Tourette syndrome. Psychopharmacology (Berl) 186: 246–254.
Takahashi N, Kashino M, Hironaka N (2010). Structure of rat ultrasonic vocalizations and its relevance to behavior. PLoS ONE 5: e14115.
Tanda G, Bassareo V, Di CG (1996). Mianserin markedly and selectively increases extracellular dopamine in the prefrontal cortex as compared to the nucleus accumbens of the rat. Psychopharmacology (Berl) 123: 127–130.
Thompson B, Leonard KC, Brudzynski SM (2006). Amphetamine-induced 50 kHz calls from rat nucleus accumbens: a quantitative mapping study and acoustic analysis. Behav Brain Res 168: 64–73.
Tornatzky W, Miczek KA (1994). Behavioral and autonomic responses to intermittent social stress: differential protection by clonidine and metoprolol. Psychopharmacology (Berl) 116: 346–356.
Vanderschuren LJ, Beemster P, Schoffelmeer AN (2003). On the role of noradrenaline in psychostimulant-induced psychomotor activity and sensitization. Psychopharmacology (Berl) 169: 176–185.
Virtanen R, Savola JM, Saano V (1989). Highly selective and specific antagonism of central and peripheral alpha 2-adrenoceptors by atipamezole. Arch Int Pharmacodyn Ther 297: 190–204.
Vivian JA, Miczek KA (1993). Morphine attenuates ultrasonic vocalization during agonistic encounters in adult male rats. Psychopharmacology (Berl) 111: 367–375.
Weinshenker D, Schroeder JP (2007). There and back again: a tale of norepinephrine and drug addiction. Neuropsychopharmacology 32: 1433–1451.
West WB, Van Groll BJ, Appel JB (1995). Stimulus effects of d-amphetamine II: DA, NE, and 5-HT mechanisms. Pharmacol Biochem Behav 51: 69–76.
White NR, Cagiano R, Moises AU, Barfield RJ (1990). Changes in mating vocalizations over the ejaculatory series in rats (Rattus norvegicus). J Comp Psychol 104: 255–262.
Williams SN, Undieh AS (2010). Brain-derived neurotrophic factor signaling modulates cocaine induction of reward-associated ultrasonic vocalization in rats. J Pharmacol Exp Ther 332: 463–468.
Wintink AJ, Brudzynski SM (2001). The related roles of dopamine and glutamate in the initiation of 50-kHz ultrasonic calls in adult rats. Pharmacol Biochem Behav 70: 317–323.
Wohr M, Houx B, Schwarting RK, Spruijt B (2008). Effects of experience and context on 50-kHz vocalizations in rats. Physiol Behav 93: 766–776.
Wohr M, Kehl M, Borta A, Schanzer A, Schwarting RK, Hoglinger GU (2009). New insights into the relationship of neurogenesis and affect: tickling induces hippocampal cell proliferation in rats emitting appetitive 50-kHz ultrasonic vocalizations. Neuroscience 163: 1024–1030.
Wohr M, Schwarting RKW (2009). Activation of limbic system structures by replay of ultrasonic vocalization in rats. In: Brudzynski SM (ed). Handbook of Mammalian Vocalization: An Integratice Neuroscience Approach pp 113–124, Academic Press: Oxford.
Wortley KE, Heal DJ, Stanford SC (1999). Modulation of sibutramine-induced increases in extracellular noradrenaline concentration in rat frontal cortex and hypothalamus by alpha2-adrenoceptors. Br J Pharmacol 128: 659–666.
Wright JM, Gourdon JC, Clarke PB (2010). Identification of multiple call categories within the rich repertoire of adult rat 50-kHz ultrasonic vocalizations: effects of amphetamine and social context. Psychopharmacology (Berl) 211: 1–13.
Yokel RA, Wise RA (1976). Attenuation of intravenous amphetamine reinforcement by central dopamine blockade in rats. Psychopharmacology (Berl) 48: 311–318.
Zarrindast MR, Bahreini T, Adl M (2002). Effect of imipramine on the expression and acquisition of morphine-induced conditioned place preference in mice. Pharmacol Biochem Behav 73: 941–949.
Acknowledgements
This research was supported by a Natural Science and Engineering Research Council of Canada discovery grant (155055 to PBSC) and a Canadian Institutes of Health Research of Canada operating grant (MOP-10516 to PBSC). We thank Annie Constantin for performing IV catheterization surgeries and Tina Scardochio for constructive comments on the manuscript. JMW holds a NSERC PGSD.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Neuropsychopharmacology website
Supplementary information
PowerPoint slides
Rights and permissions
About this article
Cite this article
Wright, J., Dobosiewicz, M. & Clarke, P. α- and β-Adrenergic Receptors Differentially Modulate the Emission of Spontaneous and Amphetamine-Induced 50-kHz Ultrasonic Vocalizations in Adult Rats. Neuropsychopharmacol 37, 808–821 (2012). https://doi.org/10.1038/npp.2011.258
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2011.258
Keywords
This article is cited by
-
Effects of nicotine, nornicotine and cotinine, alone or in combination, on locomotor activity and ultrasonic vocalization emission in adult rats
Psychopharmacology (2020)
-
Effects of acute morphine withdrawal on ultrasonic vocalizations in adult rats: unchanged 50-kHz call rate and altered subtype profile
Psychopharmacology (2018)
-
Inter-individual differences in serotonin and glutamate co-transmission reflect differentiation in context-induced conditioned 50-kHz USVs response after morphine withdrawal
Brain Structure and Function (2018)
-
Effects of anxiogenic drugs on the emission of 22- and 50-kHz ultrasonic vocalizations in adult rats
Psychopharmacology (2018)
-
Effects of repeated morphine on ultrasonic vocalizations in adult rats: increased 50-kHz call rate and altered subtype profile
Psychopharmacology (2017)