Abstract
The fact that the complement system is activated during immune-complex glomerular disease has been known for nearly 50 years. Detection of complement deposition in the glomerulus using immunochemistry has become an important element of the histological analysis of renal biopsies, and is key to the diagnosis of many types of glomerulonephritis. In recent years it has become evident that complement activation is involved in the pathogenesis of other types of renal disease; complement activation is implicated in transplant injury, atypical hemolytic uremic syndrome and progressive tubulointerstitial fibrosis. Emergence of this evidence has provided insight into how these diseases develop, and has yielded useful diagnostic tools and potential targets for therapeutic intervention. Clinicians have, by using plasma-based therapies, unknowingly treated abnormalities of the complement system in renal patients for many years. Advances in antibody and protein technologies have led to the development of complement inhibitors that have been used in phase III clinical studies. More-specific agents and applications are likely to be developed over the coming years and are discussed in this Review.
Key Points
-
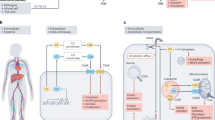
The majority of circulating complement is produced by the liver; complement synthesized in the kidney is likely to have an important role in local injury
-
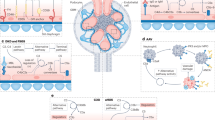
Different pathways of complement activation are involved in different forms of renal disease, such as the alternative pathway in atypical hemolytic uremic syndrome and the classical pathway in lupus nephritis
-
Mutations of, deficiencies in, or autoantibodies against, complement proteins and their regulators have been detected in patients with, for example, atypical hemolytic uremic syndrome, lupus nephritis or membranoproliferative glomerulonephritis
-
Advances in antibody and protein technologies have led to the development of complement inhibitors that have been used in phase III clinical studies
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Walport MJ (2001) Complement. Second of two parts. N Engl J Med 344: 1140–1144
Walport MJ (2001) Complement. First of two parts. N Engl J Med 344: 1058–1066
Carroll MC (2004) The complement system in regulation of adaptive immunity. Nat Immunol 5: 981–986
Thurman JM and Holers VM (2006) Complement deficient mice as model systems for kidney diseases. In Complement and Kidney Disease, 49–63 (Ed Zipfel PF) Basel: Birkhauser
Gasser C et al. (1955) Hemolytic-uremic syndrome: bilateral necrosis of the renal cortex in acute acquired hemolytic anemia. [German]. Schweiz Med Wochenschr 85: 905–909
Constantinescu AR et al. (2004) Non-enteropathic hemolytic uremic syndrome: causes and short-term course. Am J Kidney Dis 43: 976–982
Noris M et al. (1999) Hypocomplementemia discloses genetic predisposition to hemolytic uremic syndrome and thrombotic thrombocytopenic purpura: role of factor H abnormalities. Italian Registry of Familial and Recurrent Hemolytic Uremic Syndrome/Thrombotic Thrombocytopenic Purpura. J Am Soc Nephrol 10: 281–293
Stuhlinger W et al. (1974) Letter: Haemolytic-uraemic syndrome: evidence for intravascular C3 activation. Lancet 2: 788–789
Warwicker P et al. (1997) Three new polymorphisms in the human complement factor H gene and promoter region. Immunogenetics 46: 437–438
Warwicker P et al. (1998) Genetic studies into inherited and sporadic hemolytic uremic syndrome. Kidney Int 53: 836–844
Rodriguez de Cordoba S et al. (2004) The human complement factor H: functional roles, genetic variations and disease associations. Mol Immunol 41: 355–367
Caprioli J et al. (2006) Genetics of HUS: the impact of MCP, CFH, and IF mutations on clinical presentation, response to treatment, and outcome. Blood 108: 1267–1279
Jokiranta TS et al. (2005) Binding of complement factor H to endothelial cells is mediated by the carboxy-terminal glycosaminoglycan binding site. Am J Pathol 167: 1173–1181
Manuelian T et al. (2003) Mutations in factor H reduce binding affinity to C3b and heparin and surface attachment to endothelial cells in hemolytic uremic syndrome. J Clin Invest 111: 1181–1190
Jozsi M et al. (2006) Factor H and atypical hemolytic uremic syndrome: mutations in the C-terminus cause structural changes and defective recognition functions. J Am Soc Nephrol 17: 170–177
Fremeaux-Bacchi V et al. (2004) Complement factor I: a susceptibility gene for atypical haemolytic uraemic syndrome. J Med Genet 41: e84
Kavanagh D et al. (2005) Mutations in complement factor I predispose to development of atypical hemolytic uremic syndrome. J Am Soc Nephrol 16: 2150–2155
Richards A et al. (2003) Mutations in human complement regulator, membrane cofactor protein (CD46), predispose to development of familial hemolytic uremic syndrome. Proc Natl Acad Sci USA 100: 12966–12971
Noris M et al. (2003) Familial haemolytic uraemic syndrome and an MCP mutation. Lancet 362: 1542–1547
Dragon-Durey MA et al. (2005) Anti-Factor H autoantibodies associated with atypical hemolytic uremic syndrome. J Am Soc Nephrol 16: 555–563
Noris M and Remuzzi G (2005) Genetic abnormalities of complement regulators in hemolytic uremic syndrome: how do they affect patient management? Nat Clin Pract Nephrol 1: 2–3
Stratton JD and Warwicker P (2002) Successful treatment of factor H-related haemolytic uraemic syndrome. Nephrol Dial Transplant 17: 684–685
Manderson AP et al. (2004) The role of complement in the development of systemic lupus erythematosus. Annu Rev Immunol 22: 431–456
Bao L et al. (2002) Transgenic expression of a soluble complement inhibitor protects against renal disease and promotes survival in MRL/lpr mice. J Immunol 168: 3601–3607
Bao L et al. (2003) Administration of a soluble recombinant complement C3 inhibitor protects against renal disease in MRL/lpr mice. J Am Soc Nephrol 14: 670–679
Botto M et al. (1998) Homozygous C1q deficiency causes glomerulonephritis associated with multiple apoptotic bodies. Nat Genet 19: 56–59
Mitchell DA et al. (1999) Cutting edge: C1q protects against the development of glomerulonephritis independently of C3 activation. J Immunol 162: 5676–5679
Taylor PR et al. (2000) A hierarchical role for classical pathway complement proteins in the clearance of apoptotic cells in vivo. J Exp Med 192: 359–366
Nauta AJ et al. (2004) Opsonization with C1q and mannose-binding lectin targets apoptotic cells to dendritic cells. J Immunol 173: 3044–3050
Nauta AJ et al. (2003) Mannose-binding lectin engagement with late apoptotic and necrotic cells. Eur J Immunol 33: 2853–2863
Garred P et al. (2001) Association of mannose-binding lectin gene variation with disease severity and infections in a population-based cohort of systemic lupus erythematosus patients. Genes Immun 2: 442–450
Mosca M et al. (2006) Prevalence and clinico-serological correlations of anti-alpha-enolase, anti-C1q, and anti-dsDNA antibodies in patients with systemic lupus erythematosus. J Rheumatol 33: 695–697
Seelen MA et al. (2003) Autoantibodies against mannose-binding lectin in systemic lupus erythematosus. Clin Exp Immunol 134: 335–343
Trouw LA et al. (2004) Anti-C1q autoantibodies in murine lupus nephritis. Clin Exp Immunol 135: 41–48
Trouw LA et al. (2004) Anti-C1q autoantibodies deposit in glomeruli but are only pathogenic in combination with glomerular C1q-containing immune complexes. J Clin Invest 114: 679–688
Appel GB et al. (2005) Membranoproliferative glomerulonephritis type II (dense deposit disease): an update. J Am Soc Nephrol 16: 1392–1403
Hogasen K et al. (1995) Hereditary porcine membranoproliferative glomerulonephritis type II is caused by factor H deficiency. J Clin Invest 95: 1054–1061
Pickering MC et al. (2002) Uncontrolled C3 activation causes membranoproliferative glomerulonephritis in mice deficient in complement factor H. Nat Genet 31: 424–428
Licht C et al. (2006) Deletion of Lys224 in regulatory domain 4 of Factor H reveals a novel pathomechanism for dense deposit disease (MPGN II). Kidney Int 70: 42–50
Saland JM et al. (2006) Favorable long-term outcome after liver–kidney transplant for recurrent hemolytic uremic syndrome associated with a factor H mutation. Am J Transplant 6: 1948–1952
Acosta J et al. (2004) Complement and complement regulatory proteins as potential molecular targets for vascular diseases. Curr Pharm Des 10: 203–211
Qin X et al. (2004) Glycation inactivation of the complement regulatory protein CD59: a possible role in the pathogenesis of the vascular complications of human diabetes. Diabetes 53: 2653–2661
Mackensen-Haen S et al. (1992) The consequences for renal function of widening of the interstitium and changes in the tubular epithelium of the renal cortex and outer medulla in various renal diseases. Clin Nephrol 37: 70–77
Morita Y et al. (2000) Complement activation products in the urine from proteinuric patients. J Am Soc Nephrol 11: 700–707
Camussi G et al. (1982) In vitro alternative pathway activation of complement by the brush border of proximal tubules of normal rat kidney. J Immunol 128: 1659–1663
Nath KA et al. (1991) Increased ammoniagenesis as a determinant of progressive renal injury. Am J Kidney Dis 17: 654–657
Ichida S et al. (1994) Localization of the complement regulatory proteins in the normal human kidney. Kidney Int 46: 89–96
Mosolits S et al. (1997) Membrane attack complex and membrane cofactor protein are related to tubulointerstitial inflammation in various human glomerulopathies. Nephron 75: 179–187
Nangaku M et al. (2002) C6 mediates chronic progression of tubulointerstitial damage in rats with remnant kidneys. J Am Soc Nephrol 13: 928–936
Nangaku M et al. (1999) Complement membrane attack complex (C5b-9) mediates interstitial disease in experimental nephrotic syndrome. J Am Soc Nephrol 10: 2323–2331
Nomura A et al. (1997) Role of complement in acute tubulointerstitial injury of rats with aminonucleoside nephrosis. Am J Pathol 151: 539–547
Nomura A et al. (1997) Role of complement in acute tubulointerstitial injury of rats with aminonucleoside nephrosis. Am J Pathol 151: 539–547
Morita Y et al. (1997) The role of complement in the pathogenesis of tubulointerstitial lesions in rat mesangial proliferative glomerulonephritis. J Am Soc Nephrol 8: 1363–1372
Welch TR and Blystone LW (2005) C3 is central to the interstitial component of experimental immune complex glomerulonephritis. Clin Immunol 115: 80–84
Turnberg D et al. (2006) Complement activation contributes to both glomerular and tubulointerstitial damage in adriamycin nephropathy in mice. J Immunol 177: 4094–4102
He C et al. (2005) Complement inhibitors targeted to the proximal tubule prevent injury in experimental nephrotic syndrome and demonstrate a key role for C5b-9. J Immunol 174: 5750–5757
Welch TR et al. (2002) C5a is important in the tubulointerstitial component of experimental immune complex glomerulonephritis. Clin Exp Immunol 130: 43–48
de Vries B et al. (2004) The mannose-binding lectin-pathway is involved in complement activation in the course of renal ischemia-reperfusion injury. Am J Pathol 165: 1677–1688
Zhang M et al. (2006) Identification of the target self-antigens in reperfusion injury. J Exp Med 203: 141–152
Farrar CA et al. (2004) Independent pathways of P-selectin and complement-mediated renal ischemia/reperfusion injury. Am J Pathol 164: 133–141
Zhou W et al. (2000) Predominant role for C5b-9 in renal ischemia/reperfusion injury. J Clin Invest 105: 1363–1371
Granger CB et al. (2003) Pexelizumab, an anti-C5 complement antibody, as adjunctive therapy to primary percutaneous coronary intervention in acute myocardial infarction: the COMplement inhibition in Myocardial infarction treated with Angioplasty (COMMA) trial. Circulation 108: 1184–1190
Mahaffey KW et al. (2003) Effect of pexelizumab, an anti-C5 complement antibody, as adjunctive therapy to fibrinolysis in acute myocardial infarction: the COMPlement inhibition in myocardial infarction treated with thromboLYtics (COMPLY) trial. Circulation 108: 1176–1183
Nickeleit V et al. (2002) Detection of the complement degradation product C4d in renal allografts: diagnostic and therapeutic implications. J Am Soc Nephrol 13: 242–251
Feucht HE et al. (1991) Vascular deposition of complement-split products in kidney allografts with cell-mediated rejection. Clin Exp Immunol 86: 464–470
Feucht HE et al. (1993) Capillary deposition of C4d complement fragment and early renal graft loss. Kidney Int 43: 1333–1338
Collins AB et al. (1999) Complement activation in acute humoral renal allograft rejection: diagnostic significance of C4d deposits in peritubular capillaries. J Am Soc Nephrol 10: 2208–2214
Herzenberg AM et al. (2002) C4d deposition in acute rejection: an independent long-term prognostic factor. J Am Soc Nephrol 13: 234–241
Bohmig GA et al. (2002) Capillary C4d deposition in kidney allografts: a specific marker of alloantibody-dependent graft injury. J Am Soc Nephrol 13: 1091–1099
Racusen LC et al. (2003) Antibody-mediated rejection criteria—an addition to the Banff 97 classification of renal allograft rejection. Am J Transplant 3: 708–714
Mauiyyedi S et al. (2001) Chronic humoral rejection: identification of antibody-mediated chronic renal allograft rejection by C4d deposits in peritubular capillaries. J Am Soc Nephrol 12: 574–582
Berger SP et al. (2005) Association between mannose-binding lectin levels and graft survival in kidney transplantation. Am J Transplant 5: 1361–1366
Tang S et al. (1999) Contribution of renal secreted complement C3 to the circulating pool in humans. J Immunol 162: 4336–4341
Pratt JR et al. (2002) Local synthesis of complement component C3 regulates acute renal transplant rejection. Nat Med 8: 582–587
Farrar CA et al. (2006) Local extravascular pool of C3 is a determinant of postischemic acute renal failure. FASEB J 20: 217–226
Brown KM et al. (2006) Influence of donor C3 allotype on late renal-transplantation outcome. N Engl J Med 354: 2014–2023
Sheerin NS et al. (2006) Accumulation of immune complexes in glomerular disease is independent of locally synthesized c3. J Am Soc Nephrol 17: 686–696
Springall T et al. (2001) Epithelial secretion of C3 promotes colonization of the upper urinary tract by Escherichia coli. Nat Med 7: 801–806
Li K et al. (2006) CD46 (membrane cofactor protein) acts as a human epithelial cell receptor for internalization of opsonized uropathogenic Escherichia coli. J Immunol 177: 2543–2551
Weisman HF et al. (1990) Soluble human complement receptor type 1: in vivo inhibitor of complement suppressing post-ischemic myocardial inflammation and necrosis. Science 249: 146–151
Mollnes TE and Kirschfink M (2006) Strategies of therapeutic complement inhibition. Mol Immunol 43: 107–121
Keshavjee S et al. (2005) A randomized, placebo-controlled trial of complement inhibition in ischemia-reperfusion injury after lung transplantation in human beings. J Thorac Cardiovasc Surg 129: 423–428
Li JS et al. (2004) Pharmacokinetics and safety of TP10, soluble complement receptor 1, in infants undergoing cardiopulmonary bypass. Am Heart J 147: 173–180
Zimmerman JL et al. (2000) Phase I trial of the recombinant soluble complement receptor 1 in acute lung injury and acute respiratory distress syndrome. Crit Care Med 28: 3149–3154
Smith GP and Smith RA (2001) Membrane-targeted complement inhibitors. Mol Immunol 38: 249–255
Fitch JC et al. (1999) Pharmacology and biological efficacy of a recombinant, humanized, single-chain antibody C5 complement inhibitor in patients undergoing coronary artery bypass graft surgery with cardiopulmonary bypass. Circulation 100: 2499–2506
Bao L et al. (2005) C5a promotes development of experimental lupus nephritis which can be blocked with a specific receptor antagonist. Eur J Immunol 35: 2496–2506
Bao L et al. (2005) Signaling through up-regulated C3a receptor is key to the development of experimental lupus nephritis. J Immunol 175: 1947–1955
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Brown, K., Sacks, S. & Sheerin, N. Mechanisms of Disease: the complement system in renal injury—new ways of looking at an old foe. Nat Rev Nephrol 3, 277–286 (2007). https://doi.org/10.1038/ncpneph0465
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpneph0465
This article is cited by
-
Tissue-specific deletion of Crry from mouse proximal tubular epithelial cells increases susceptibility to renal ischemia–reperfusion injury
Kidney International (2014)
-
Discovering hidden relationships between renal diseases and regulated genes through 3D network visualizations
BMC Research Notes (2010)
-
Current status and issues of C1q nephropathy
Clinical and Experimental Nephrology (2009)
-
Complement: coming full circle
Archivum Immunologiae et Therapiae Experimentalis (2009)
-
Complement and the atypical hemolytic uremic syndrome in children
Pediatric Nephrology (2008)