Abstract
The importance of bone-morphogenetic proteins in prostate cancer is well recognized. Bone-morphogenetic protein-6 overexpression has been shown to increase the aggressiveness and invasiveness of prostate cancer cells. Recent studies on noggin and sclerostin, potent inhibitors of bone-morphogenetic protein signaling, have found that noggin also modifies the ability of prostate cancer cells to metastasize to bone. Taken together, these results suggest that bone-morphogenetic protein-6 signaling is important in prostate cancer progression. Our study investigated the expression of bone-morphogenetic protein-6, noggin and sclerostin in human prostate specimens (n=136) by immunohistochemical staining. We found that bone-morphogenetic protein-6 was increased (P<0.001), whereas sclerostin was decreased (P=0.004) in prostate cancer compared with nodular hyperplasia. In addition, significantly higher level of bone-morphogenetic protein-6 expression was observed in high-grade prostate cancer with Gleason score ≥7 (P=0.027). Bone-morphogenetic protein-6, noggin and sclerostin alone could not predict the development of distant metastasis in our patient cohort. However, high level of bone-morphogenetic protein-6 and low level of noggin, or high level of bone-morphogenetic protein-6 and low level of both noggin and sclerostin expression in primary prostate cancer significantly predicted development of distant metastasis. The predictive value was still valid when only high-grade prostate cancers were included or when patients with secondary lesion other than bone were excluded. Taken together, these results suggest that a high level of bone-morphogenetic protein-6 signaling, resulting from increased expression of bone-morphogenetic protein-6 and decreased expression of its inhibitors, might promote the development of prostate cancer metastases. Our results also imply the potential use of bone-morphogenetic protein-6, noggin and sclerostin expression together as a prognostic predictor for metastatic progression of prostate cancer.
Similar content being viewed by others
Main
Prostate cancer leads in cancer incidence and is the second leading cause of cancer-related death among American men.1 Patients with prostate cancer, differ from those with other aggressive cancers in having a relatively high 5-year survival rate. It follows that treatment directed against prostate cancer may not be beneficial in terms of the patients’ quality of living.2 However, once the patients develop clinically undetectable micrometastatic disease, the 5-year survival rate would be greatly reduced.3 As a result, reliable prognostic markers are required to distinguish indolent from aggressive prostate cancers for proper clinical management of the patients.
Bone-morphogenetic proteins (BMPs) play an important role in metastatic progression in prostate cancer. Among these BMPs, BMP-6 seems to play a central role in promoting prostate cancer metastasized to bone. BMP-6 expression is higher in prostate cancer compared with benign prostate specimens as well as in high-grade compared with low-grade prostate cancers.4, 5 Its expression is high in primary prostate cancer of patients with metastases, whereas is low or undetectable in non-metastatic prostate cancer and benign prostate specimens.1, 5 In addition, BMP-6 is also highly expressed in prostate cancer metastasized to bone.6 Recently, BMP-6 has been shown to promote prostate cancer metastasized to bone by enhancing the osteoblastic activity and the invasive ability of prostate cancer cells.7, 8
BMP signaling is tightly regulated. One way to control BMPs activity is to express BMPs antagonists, such as noggin and sclerostin.9 The expression of noggin and sclerostin is regulated by BMPs signaling,10, 11 forming a feedback loop, which is also observed in prostate cancer cells such that an increased expression of BMP-6 increases noggin expression,12 whereas decreased expression of BMP-7 decreases noggin expression.13 In addition, noggin and sclerostin also interact with each other to regulate BMPs activity.14
Noggin has been shown to modulate the invasiveness and the osteoblastic activity of prostate cancer cells.7, 15 Overexpression of noggin in prostate cancer cells results in decreased ability of the cells to form osteolytic or osteoblastic lesions in tibias of immunosuppressed mouse.16, 17 Another study has shown that expression of noggin is an important determinant to decide whether a metastatic lesion is osteoblastic or osteolytic in nature.18 In contrast, although the function of sclerostin in prostate cancer is still unknown, the mRNA of SOST, which encodes sclerostin, was not detected in several prostate cancer cell lines tested by Schwaninger et al.18
Noggin and sclerostin have both been shown to interact with and inhibit the activity of BMP-6.7, 19 Taken together, these lines of evidence suggest that BMP-6, noggin and sclerostin might be involved in a complex regulatory mechanism orchestrating the transformation, aggressiveness and bone metastatic ability of prostate cancer. In this study, we examined the expression level of BMP-6, noggin and sclerostin in 136 human prostate specimens by immunohistochemistry and investigated their prognostic significance in our prostate cancer patient cohort (n=95).
Materials and methods
Patients and Specimens
A total of 152 archival formalin-fixed paraffin-embedded prostate specimens were obtained from the Department of Pathology, The University of Hong Kong at Queen Mary Hospital. These specimens were either from transurethral resections (n=15) or radical prostatectomies (n=137), and were incorporated into tissue microarray as previously described.20 The prostate specimens include 41 nodular hyperplasia, 16 prostatic intraepithelial neoplasia and 95 prostate cancer specimens. The prostate cancer specimens were collected consecutively. Specimens from patients with prior treatment against prostate cancer or with insufficient tumor tissue for immunohistochemistry were excluded. Clinical data were retrieved from the computerized database of Queen Mary Hospital with the mean follow-up time of our prostate cancer patients being 23 months (ranged from at the time of diagnosis to 118.7 months). The median age of our cohort is 76 years (ranged from 56 to 94 years). Pretreatment prostate-specific antigen level was available in 71% (67 out of 95) of prostate cancer patients. Metastatic disease was established by clinical features, radiology (including computed tomography), radioisotopic bone scan and histological examination, either alone or in combination (Table 1).
Immunohistochemical Staining
Immunohistochemical staining was performed as previously described by using EnVision+ system-HRP (Dako).21 Polyclonal antibodies of BMP-6 (R&D System) and noggin (Abcam), and monoclonal antibody of sclerostin (R&D System) were applied at a concentration of 2.5, 2.5 and 5 μg/ml, respectively, for overnight at 4°C.
Evaluation of Immunohistochemical Staining Results
Evaluation was carried out as previously described.20 Briefly, the extent and intensity of the staining were graded by an arbitrary scale that ranged from 0 to 3 representing negative (0), weak (1), moderate (2) and strong (3) staining. Negative and weak staining were classified as low-level expression, whereas moderate and strong staining were classified as high-level expression.
Statistical Analysis
Statistical analysis was performed using SPSS 15.0 software. Differences in expression level among different clinicopathological stages were analyzed by χ2 or Mann–Whitney U tests where applicable. The association between the expression level and the risk to develop distant metastasis was estimated by Kaplan–Meier analysis and compared by log-rank test.
Results
BMP-6 was Upregulated While Sclerostin was Downregulated in Prostate Cancer
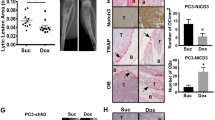
As shown in Figures 1 and 2a, significantly more prostate cancer specimens had a higher level of BMP-6 expression compared with nodular hyperplasia (P<0.001). The results obtained were similar to those of a previous study.5 They suggest that upregulation of BMP-6 is a common event in prostate cancer. Increased expression of BMP-6 was also observed in prostatic intraepithelial neoplasia compared with nodular hyperplasia specimens, but the difference did not reach statistical significance (P=0.059). Expression of noggin was not significantly different among these three types of prostate specimens, although a decreased expression of noggin was observed in prostate cancer specimens (Figures 1 and 2b). Significantly more nodular hyperplasia and prostatic intraepithelial neoplasia specimens had higher levels of sclerostin expression compared with prostate cancer (Figures 1 and 2c; P=0.004 and 0.032, respectively).
Representative results of immunohistochemical staining. High panels show tissue at × 100 magnification and lower panels show tissue at × 400 magnification. (a) BMP-6 expression was low in nodular hyperplasia and was higher in prostatic intraepithelial neoplasia and prostate cancer. The expression of BMP-6 was significantly higher in prostate cancer compared with nodular hyperplasia. (b) Noggin expression was very much similar among nodular hyperplasia, prostatic intraepithelial neoplasia and prostate cancer. The differences among the groups were not statistically significant. (c) Sclerostin expression was higher in nodular hyperplasia and prostatic intraepithelial neoplasia and was lower in prostate cancer. The expression of sclerostin was significantly higher in nodular hyperplasia compared with prostate cancer. (d, e) Two cases showing staining with relatively high level of BMP-6 and low levels of both noggin and sclerostin. These two patients developed distant metastasis in bone.
Summary of immunohistochemical staining results among different prostate specimens. (a) The expression level of BMP-6 was higher in prostate cancer compared with nodular hyperplasia (P<0.001). (b) The expression level of noggin was not significantly different among nodular hyperplasia, prostatic intraepithelial neoplasia and prostate cancer. (c) The expression level of sclerostin was lower in prostate cancer compared with nodular hyperplasia (P=0.004) and prostatic intraepithelial neoplasia (P=0.032).
BMP-6 Expression is Upregulated in High-Grade Prostate Cancer
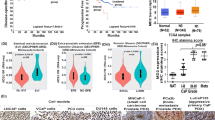
Gleason score has been widely used to indicate the aggressiveness of prostate cancer.22 We compared the expression levels of BMP-6, noggin and sclerostin between low-grade (Gleason score <7) and high-grade (Gleason score ≥7) prostate cancers. As shown in Figure 3, more than 46% of high-grade cancers expressed high level of BMP-6 but merely 21% low-grade cancers stained the same (P=0.027). This result was in line with other findings, suggesting that BMP-6 might play a role in prostate cancer progression.4 In contrast, we did not observe significant different noggin or sclerostin staining between high- and low-grade prostate cancers in our patient cohort. These results suggest that loss of BMPs inhibitors might not be a feature of high-grade prostate cancer.
Summary of immunohistochemical staining results in prostate cancer of different Gleason score and metastatic status. (a) The expression level of BMP-6 was significantly higher in high-grade compared with low-grade prostate cancer. The differences in noggin and sclerostin expression between high- and low-grade prostate cancers were not significant. (b) The three proteins, individually, confer no significant different between metastatic and non-metastatic prostate cancer. (c) Significantly more metastatic primary prostate cancer expressed high level of BMP-6 and low level of noggin compared with non-metastatic prostate cancer. Similarly, significantly more metastatic primary prostate cancer expressed high level of BMP-6 and low levels of both noggin and sclerostin compared with non-metastatic prostate cancer.
BMP-6, Noggin and Sclerostin Using Alone could not Predict Development of Distant Metastasis in Prostate Cancer
As shown in Figure 3b, although we observed that more metastatic prostate cancer specimens (42%, 16 out of 38) expressed a high level of BMP-6 compared with non-metastatic specimens (32%, 15 out of 47), the difference in the staining intensity between the two groups was not statistically significant. We also observed that more metastatic prostate cancer specimens (65%, 22 out of 34) had a lower level of sclerostin expression compared with non-metastatic specimens (45%, 19 out of 42). But the difference was again not statistically significant. The expression level of noggin is similar between metastatic and non-metastatic prostate cancer (Figure 3b). By Kaplan–Meier analysis, BMP-6 (P=0.152), noggin (P=0.642) and sclerostin (P=0.316) could not be used to predict development of distant metastasis in our patient cohort.
Primary Prostate Cancer with High Level of BMP-6 and Low Level of both Noggin and Sclerostin Predicted Development of Distant Metastasis
As noggin and sclerostin have been shown to inhibit BMP-6,7, 19 a high level of noggin or sclerostin might reduce the activity of BMP-6 and also mask the prognostic value of BMP-6 in our patient cohort. Therefore, we went on to analyze whether specimens with high level of BMP-6 and low level of noggin and/or sclerostin could predict development of distant metastasis. As shown in Figure 3c, significantly more metastatic prostate cancer specimens had a high level of BMP-6 and low level of noggin (24%, 9 out of 37) compared with non-metastatic specimens (P=0.042, 7.5%, 3 out of 37). In addition, we also observed significantly more metastatic prostate cancer specimens had a high level of BMP-6 and low level of both noggin and sclerostin (27%, 8 out of 30) compared with non-metastatic specimens (P=0.047, 8.3%, 3 out of 36). By Kaplan–Meier analysis, we found that primary prostate cancer specimens expressing high level of BMP-6 and low level of noggin significantly predicted development of distant metastasis (Figure 4a, P=0.021). Patients with primary prostate cancer, which stained high level of BMP-6 and low level of noggin, had an estimated median time for development of distant metastasis of only 9 months with 95% confidence interval of 0–18 months, whereas patients with other staining patterns had a median of 53 months with 95% confidence interval of 25–81 months. In addition, we also observed that primary prostate cancer specimens expressing high level of BMP-6 and low level of both noggin and sclerostin also significantly predicted development of distant metastasis (Figure 4b, P=0.018). Patients with primary prostate cancer, which stained high level of BMP-6 and low level of both noggin and sclerostin, had an estimated median time for development of distant metastasis of only 9 months with 95% confidence interval of 2–16 months, whereas patients with other staining patterns had a median of 53 months with 95% confidence interval of 21–85 months.
Kaplan–Meier analysis of increased BMP-6 activity in primary prostate cancer. (a) Patients with primary prostate cancer expressing high level of BMP-6 and low level of noggin were more likely to develop distant metastasis. (b) Patients with primary prostate cancer expressing high level of BMP-6 and low levels of both noggin and sclerostin were more likely to develop distant metastasis. (c) High Gleason score predicts development of distant metastasis in our patient cohort. (d, e) Of the high-grade prostate cancer, high activity of BMP-6 inferred a poor prognosis in our patient cohort. (f, g) As BMP-6 activity has been shown to promote prostate cancer metastasized to bone, we analyzed its effect on the timing for development of bony metastasis in prostate cancer. We found that high activity of BMP-6 in the primary prostate cancer infers a risk to earlier development of bone metastasis in our patient cohort.
Gleason score is a well-defined prognostic marker for prostate cancer. As shown in Figure 4c, by Kaplan–Meier analysis, we found that patients with high-grade tumor (Gleason score ≥7) are more likely to develop distant metastasis (P=0.001). To investigate whether increased BMP-6 activity could be of prognostic value in prostate cancer additional to Gleason score, we performed Kaplan–Meier analysis in a subgroup of patients who had primary prostate cancer of high Gleason scores (≥7). We found that BMP-6 activation had a predictive value for the development of distant metastasis in this subgroup (Figure 4d and e). We found that patients with primary prostate cancer expressing high level of BMP-6 and low level of noggin are more likely to develop distant metastasis (P=0.043), whereas patients with primary prostate cancer expressing high level of BMP-6 and low levels of both noggin and sclerostin are also more likely to develop distant metastasis (P=0.029).
In our patient cohort, 88% of the metastatic prostate cancer patients had their secondary lesion in bone. Because BMP-6 activity has been suggested to correlate with the ability of the prostate cancer to establish bone metastasis,6, 7, 12 we therefore analyzed our patient cohort, excluding those metastatic patients with their secondary lesion developed other than in bone, on whether increased BMP-6 activity could predict development of metastasis to bone. We found that, by Kaplan–Meier analysis, patients with primary prostate cancer expressing high level of BMP-6 and low level of noggin had a higher chance for the development of bone metastasis (Figure 4f, P=0.032), whereas patients with primary prostate cancer expressing high level of BMP-6 and low level of both noggin and sclerostin also had a higher chance for the development of bone metastasis (Figure 4g, P=0.028).
Discussion
BMP-6 is overexpressed in prostate cancer, especially in patients with skeletal metastases.5 The roles of BMP-6 in prostate cancer progression have been described as to increase the aggressiveness and bone metastatic ability of the prostate cancer cells.7, 8, 12 In this study, we obtained a similar result that BMP-6 was upregulated in prostate cancer compared with nodular hyperplasia (P<0.001) and in high-grade compared with low-grade prostate cancers (P=0.027). These results further suggest the importance of BMP-6 in prostate cancer progression.
Noggin has been shown to modify BMP signaling in prostate cancer.17, 18 Addition of noggin also results in decreased activity of BMP-6 signaling.12 However, prior to our study, the difference in the expression of noggin between different human prostate specimens has not been investigated. Sclerostin, another inhibitor of BMPs, has also been shown to have high affinity for and inhibit BMP-6.19 However, its function and expression in prostate cancer are largely unknown. In this study, we found that expression of sclerostin was significantly reduced in prostate cancer compared with nodular hyperplasia specimens (P=0.004), suggesting a negative role of sclerostin in prostate carcinogenesis.
Inhibitors of BMPs, such as noggin and sclerostin, have been shown to be upregulated by increased BMPs signaling.11, 12 This negative feedback regulatory mechanism might function to tightly control the extent of BMPs signaling. BMP-6 has been shown to upregulate both noggin and sclerostin,11, 12 whereas its activity is inhibited by noggin and sclerostin.7, 19 These results suggest that the activity of BMP-6 is regulated by this negative feedback loop. BMP-6 is important in prostate cancer carcinogenesis and progression, an upregulation of BMP-6 might not be enough to trigger the onset of these events if its upregulation is coupled by increased expression of its inhibitors, noggin or sclerostin. We speculated that the upregulation of BMP-6 and the uncoupling of this negative feedback loop might be important for the development of more aggressive phenotype of prostate cancer. In the present study, we found that the expression of BMP-6, noggin and sclerostin, used in isolation was not able to predict the development of distant metastasis in our patient cohort. However, we found that patients with primary prostate cancer expressing high level of BMP-6 and low level of noggin, or high level of BMP-6 and low level of noggin and sclerostin were at a higher risk for the development of distant metastasis. These results suggest that a measure of the activity of BMP-6 may be a prognostic marker for metastatic progression of prostate cancer.
Furthermore, we speculated that the use of BMPs activity as a prognostic marker might also apply to cancers other than that of prostate. BMP-6 has been shown to be upregulated in esophageal squamous cell carcinoma and correlate with patient survival.23 In another study, we found that although expression of BMP-6, noggin and sclerostin individually was not of prognostic value in an esophageal squamous cell carcinoma patient cohort, when used in combination, increased BMP-6 activity in primary esophageal squamous cell carcinoma was significantly associated with poor prognosis in the same patient cohort (Yuen HF et al, manuscript in preparation).
On the basis of our studies, we believe that the expression of BMP inhibitors should always be studied along with BMPs to reveal the true significance of expression of BMPs in cancers. Overexpression of BMPs has been described in other cancer types, such as osteosarcoma,24 breast cancer,25, 26 pancreatic cancer27 and malignant melanoma.28 The expression of BMPs has been shown not to confer prognostic value in predicting the outcome of patients with osteosarcoma.24 Further studies of BMP activity using a similar approach to ours might make clear the prognostic significance of BMP activity in other cancers.
In summary, we found that increased BMP-6 activity, denoted by high-level expression of BMP-6 and low-level expression of its inhibitors noggin and sclerostin, could be a useful prognostic marker for prostate cancer to predict development of distant metastasis.
References
Bentley H, Hamdy F, Hart K, et al. Expression of bone morphogenetic proteins in human prostatic adenocarcinoma and benign prostatic hyperplasia. Br J Cancer 1992;66:1159–1163.
van Tol-Geerdink J, Stalmeier P, van Lin E, et al. Do patients with localized prostate cancer treatment really want more aggressive treatment? J Clin Oncol 2006;24:4581–4586.
Loberg R, Gayed B, Olson K, et al. A paradigm for the treatment of prostate cancer bone metastases based on an understanding of tumor cell–microenvironment interactions. J Cell Biochem 2005;96:439–446.
Barnes J, Anthony C, Wall N, et al. Bone morphogenetic protein-6 expression in normal and malignant prostate. World J Urol 1995;13:337–343.
Hamdy F, Autzen P, Robinson M, et al. Immunolocalization and messenger RNA expression of bone morphogenetic protein-6 in human benign and malignant prostatic tissue. Cancer Res 1997;57:4427–4431.
Autzen P, Robson C, Bjartell A, et al. Bone morphogenetic protein 6 in skeletal metastases from prostate cancer and other common human malignancies. Br J Cancer 1998;78:1219–1223.
Dai J, Keller J, Zhang J, et al. Bone morphogenetic protein-6 promotes osteoblastic prostate cancer bone metastases through a dual mechanism. Cancer Res 2005;65:8274–8285.
Darby S, Cross S, Brown N, et al. BMP-6 over-expression in prostate cancer is associated with increased Id-1 protein and a more invasive phenotype. J Pathol 2008;214:394–404.
Yanagita M . BMP antagonists: their roles in development and involvement in pathophysiology. Cytokine Growth Factor Rev 2005;16:309–317.
Gazzerro E, Gangji V, Canalis E . Bone morphogenetic proteins induce the expression of noggin, which limits their activity in cultured rat osteoblasts. J Clin Invest 1998;102:2106–2114.
Sutherland M, Geoghegan J, Yu C, et al. Unique regulation of SOST, the sclerosteosis gene, by BMPs and steroid hormones in human osteoblasts. Bone 2004;35:448–454.
Haudenschild D, Palmer S, Moseley T, et al. Bone morphogenetic protein (BMP)-6 signaling and BMP antagonist noggin in prostate cancer. Cancer Res 2004;64:8276–8284.
Ye L, Lewis-Russell J, Kynaston H, et al. Endogenous bone morphogenetic protein-7 controls the motility of prostate cancer cells through regulation of bone morphogenetic protein antagonists. J Urol 2007;178:1086–1091.
Winkler D, Yu C, Geoghegan J, et al. Noggin and sclerostin bone morphogenetic protein antagonists form a mutually inhibitory complex. J Biol Chem 2004;279:36293–36298.
Dai J, Kitagawa Y, Zhang J, et al. Vascular endothelial growth factor contributes to the prostate cancer-induced osteoblast differentiation mediated by bone morphogenetic protein. Cancer Res 2004;64:994–999.
Feeley B, Gamradt S, Hsu W, et al. Influence of BMPs on the formation of osteoblastic lesions in metastatic prostate cancer. J Bone Miner Res 2005;20:2189–2199.
Feeley B, Krenek L, Liu N, et al. Overexpression of noggin inhibits BMP-mediated growth of osteolytic prostate cancer lesions. Bone 2006;38:154–166.
Schwaninger R, Rentsch C, Wetterwald A, et al. Lack of noggin expression by cancer cells is a determinant of the osteoblast response in bone metastases. Am J Pathol 2007;170:160–175.
Kusu N, Laurikkala J, Imanishi M, et al. Sclerostin is a novel secreted osteoclast-derived bone morphogenetic protein antagonist with unique ligand specificity. J Biol Chem 2003;278:24113–24117.
Yuen H, Chua C, Chan Y, et al. Id proteins expression in prostate cancer: high-level expression of Id-4 in primary prostate cancer is associated with development of metastases. Mod Pathol 2006;19:931–941.
Yuen H, Chan Y, Chan K, et al. Id-1 and Id-2 are markers for metastasis and prognosis in oesophageal squamous cell carcinoma. Br J Cancer 2007;97:1409–1415.
Harnden P, Shelley M, Coles B, et al. Should the Gleason grading system for prostate cancer be modified to account for high-grade tertiary components? A systematic review and meta-analysis. Lancet Oncol 2007;8:411–419.
Raida M, Sarbia M, Clement J, et al. Expression, regulation and clinical significance of bone morphogenetic protein 6 in esophageal squamous-cell carcinoma. Int J Cancer 1999;83:38–44.
Sulzbacher I, Birner P, Trieb K, et al. The expression of bone morphogenetic proteins in osteosarcoma and its relevance as a prognostic parameter. J Clin Pathol 2002;55:381–385.
Clement J, Sänger J, Höffken K . Expression of bone morphogenetic protein 6 in normal mammary tissue and breast cancer cell lines and its regulation by epidermal growth factor. Int J Cancer 1999;80:250–256.
Alarmo E, Rauta J, Kauraniemi P, et al. Bone morphogenetic protein 7 is widely overexpressed in primary breast cancer. Genes Chromosomes Cancer 2006;45:411–419.
Kleeff J, Maruyama H, Ishiwata T, et al. Bone morphogenetic protein 2 exerts diverse effects on cell growth in vitro and is expressed in human pancreatic cancer in vivo. Gastroenterology 1999;116:1202–1216.
Rothhammer T, Poser I, Soncin F, et al. Bone morphogenic proteins are overexpressed in malignant melanoma and promote cell invasion and migration. Cancer Res 2005;65:448–456.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yuen, HF., Chan, YP., Cheung, WL. et al. The prognostic significance of BMP-6 signaling in prostate cancer. Mod Pathol 21, 1436–1443 (2008). https://doi.org/10.1038/modpathol.2008.94
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/modpathol.2008.94
Keywords
This article is cited by
-
Chromatin conformation changes in peripheral blood can detect prostate cancer and stratify disease risk groups
Journal of Translational Medicine (2021)
-
Differential regulation of hepcidin in cancer and non-cancer tissues and its clinical implications
Experimental & Molecular Medicine (2018)
-
Serum sclerostin levels in renal cell carcinoma patients with bone metastases
Scientific Reports (2016)
-
Upregulation of Bone Morphogenetic Protein 4 is Associated with Poor Prognosis in Patients with Hepatocellular Carcinoma
Pathology & Oncology Research (2012)
-
Parallel inhibition of cell growth and induction of cell migration and invasion in breast cancer cells by bone morphogenetic protein 4
Breast Cancer Research and Treatment (2010)