Abstract
Objective:
The objective of this study was to investigate the association between interdelivery interval (IDI) and subsequent perinatal outcomes in a large population-based cohort.
Study Design:
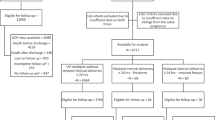
Retrospective cohort study of primiparous women with singleton gestations giving birth in the US in 2011 to 2012. IDI was defined as the time between last live birth and index live birth. IDI was categorized as 4 to 17 months, 18 to 36 months (referent), 37 to 60 months and >60 months. Statistical comparisons were made using chi-square tests and multivariable logistic regression models to control for confounding. Covariates included maternal age, prior preterm birth, prior cesarean and medical comorbidities.
Results:
Of the 1 964 523 women meeting study criteria, 9.0% had an IDI of 4 to 17 months, 39.7% 18 to 36 months, 26.8% 37 to 60 months and 24.5% >60 months. Short IDI was associated with preterm delivery (<37 weeks; 13.8 vs 8.8%, (adjusted odds ratio (aOR) 1.51, 95% confidence interval (CI) 1.48 to 1.53)) and adverse perinatal outcomes including low 5-min Apgar, small for gestational age (SGA) status and neonatal intensive care unit (NICU) admission. Women with long IDI had a higher risk of induction of labor, cesarean delivery, chorioamnionitis, maternal ICU admission, preterm delivery and SGA status, 5-min Apgar score <4, and NICU admission.
Conclusions:
Compared with women with 18 to 36 month IDIs, women with either shorter or very long IDIs were at an increased risk of adverse maternal and neonatal outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Copen CE, Thoma M, Kimeyer S . Interpregnancy intervals in the United States: Data from the Birth Certificate and the National Survey of Family Growth. Natl Vital Stat Rep 2015; 64 (3):1–10.
Shachar B, Lyell D . Interpregnancy interval and obstetrical complications. Obstet Gynecol Surv 2012; 67 (9): 584–596.
Conde-Agudelo A, Rosas-Bermudez A, Kafury-Goeta A . Birth spacing and risk of adverse perinatal outcomes: a meta-analysis. JAMA 2006; 295 (15): 1809–1823.
Conde-Agudelo A, Rosas-Bermudez A, Kafury-Goeta A . Effects of birth spacing on maternal health: a systematic review. Am J Obstet Gynecol 2007; 196 (4): 297–308.
Zhu B, Rolfs R, Nangle B, Horan J . Effect of the interval between pregnancies on perinatal outcomes. N Engl J Med 1999; 340 (8): 589–594.
de Weger F, Hukkelhoven C, Serroyen J, te Velde E, Smits L . Advanced maternal age, short interpregnancy interval, and perinatal outcome. Am J Obstet Gynecol 2011; 204 (5): 421.e1–9.
DeFranco EA, Seske LM, Greenberg JM, Muglia LJ . Influence of interpregnancy interval on neonatal morbidity. Am J Obstet Gynecol 2015; 212 (386): e1–e9.
Centers for Disease Control and Prevention. User Guide to the 2011 Natality Public Use File. Available from: http://www.cdc.gov/nchs/nvss.htm.
Centers for Disease Control and Prevention. User Guide to the 2008 Natality Public Use File. Available from: http://www.cdc.gov/nchs/nvss.htm.
Executive summary: neonatal encephalopathy and neurologic outcome, second edition. Report of the American College of Obstetricians and Gynecologists' Task Force on Neonatal Encephalopathy. Obstet Gynecol 2014; 123 (4): 896–901.
Conde-Agudelo A, Belizan J . Maternal morbidity and mortality associated with interpregnancy interval: cross sectional study. BMJ 2000; 321 (7271): 1255–1259.
Bogaerts A, Van den Bergh B, Ameye L, Witters I, Martens E, Timmerman D et al. Interpregnancy weight change and risk for adverse perinatal outcomes. Obstet Gynecol 2013; 122 (5): 999–1009.
Whiteman V, McIntosh C, Rao K, Mbah A, Salihu H . Interpregnancy BMI change and risk of primary caesarean delivery. J Obstet Gynaecol 2011; 31 (7):589–593.
Thiel de Bocanegra H, Chang R, Howell M, Darney P . Interpregnancy intervals: impact of postpartum contraceptive effectiveness and coverage. Am J Obstet Gynecol 2014; 210 (4): 311.e1–8.
White K, Teal S, Potter J . Contraception after delivery and short interpregnancy intervals among women in the United States. Obstet Gynecol 2015; 125 (6): 1471–1477.
Secura G, Madden T, McNicholas C, Mullersman J, Buckel C, Zhao Q et al. Provision of no-cost, long-acting contraception and teenage pregnancy. N Engl J Med 2014; 371 (14): 1316–1323.
Peipert J, Madden T, Allsworth J, Secura G . Preventing unintended pregnancies by providing no-cost contraception. Obstet Gynecol 2012; 120 (6): 1291–1297.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This abstract was presented as a poster presentation at the 2015 Society of Reproductive Investigation 62nd Annual Scientific Meeting in San Francisco, CA, USA (25–28 March 2015).
Rights and permissions
About this article
Cite this article
Yee, L., Truong, Y., Caughey, A. et al. The association between interdelivery interval and adverse perinatal outcomes in a diverse US population. J Perinatol 36, 593–597 (2016). https://doi.org/10.1038/jp.2016.54
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.54