Abstract
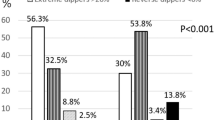
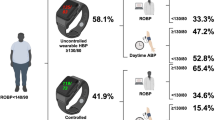
Blood pressure (BP) exhibits a circadian variation characterized by a morning increase, followed by a small postprandial valley and a deeper descent during nocturnal rest. Although abnormal 24-h variability (abnormal circadian variability (ACV)) predicts adverse cardiovascular disease (CVD) outcomes, a 7-day automatic ambulatory BP monitoring (ABPM) and subsequent chronobiologic analysis of the gathered data, permits identification of consistency of any abnormal circadian variation. To test whether normal overweight healthy men and women with prediabetes differed from subjects with normoglycemia in having ACV with a 7-day ABPM. Consent for a 7-day ABPM was obtained from subjects with family history of diabetes mellitus, who were participating in the screening phase for a randomized, double blind, placebo-controlled weight loss trial in prediabetics to prevent progression to diabetes mellitus. The automatic 7-day ABPM device recorded BP and heart rate every 30 min during the day and every 60 min during the night. Normoglycemic and prediabetic subjects matched for age, sex, race, BP, BMI, waist circumference and glycemic control, differed statistically significantly only in their fasting and/or 2-h postprandial serum glucose concentrations. Chronobiologically-interpreted 7-day ABPM uncovered no abnormalities in normoglycemics, whereas prediabetics had a statistically significantly higher incidence of high mean BP (MESOR-hypertension), excessive pulse pressure and/or circadian hyper-amplitude-tension (CHAT) (P<0.001). ACV detected with 7-day ABPM may account for the enhanced CVD risk in prediabetes. These findings provide a basis for larger-scale studies to assess the predictive value of 7-day ABPM over the long term.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Halberg F, Conner RL . Circadian organization and microbiology: variance spectra and a periodogram on behavior of Escherichia coli growing in fluid culture. Proc Minn Acad Sci 1961; 29: 227–239.
Halberg F, Cornélissen G, Katinas G, Tvildiani L, Gigolashvili M, Janashia K et al. International BIOCOS Group. Chronobiology's progress: season's appreciations 2004-2005. Time, frequency, phase, variable, individual, age- and site-specific chronomics. J Appl Biomed 2006; 4: 1–38.
Halberg F, Cornélissen G, Katinas G, Tvildiani L, Gigolashvili M, Janashia K et al. International BIOCOS Group. Chronobiology's progress: part II, chronomics for an immediately applicable biomedicine. J Appl Biomed 2006; 4: 73–86.
Yamamoto T, Nakahata Y, Soma H, Akashi M, Mamine T, Takumi T . Transcriptional oscillation of canonical clock genes in mouse peripheral tissues. BMC Mol Biol 2004; 5: 18. doi:10.1186/1471-2199-5-18.
Haus E . Chronobiology in the endocrine system. Adv Drug Deliv Rev 2007; 59: 985–1014.
O'Brien E . Ambulatory blood pressure measurement: a trove of hidden gems? Hypertension 2006; 48: 364–365.
Staessen JA, Thijs L, Fagard R, O′Brien ET, Clement D, de Leeuw PW et al. Predicting cardiovascular risk using conventional vs ambulatory blood pressure in older patients with systolic hypertension. Systolic Hypertension in Europe Trial Investigators. JAMA 1999; 282: 539–546.
White WB . How well does ambulatory blood pressure predict target-organ disease and clinical outcome in patients with hypertension? Blood Press Monit 1999; 4 (Suppl 2): S17–S21 (review).
Juutilainen A, Lehto S, Ronnemaa T, Pyorala K, Laakso M . Type 2 diabetes as a ‘coronary heart disease equivalent’: an 18-year prospective population-based study in Finnish subjects. Diabetes Care 2005; 28: 2901–2907.
Whiteley L, Padmanabhan S, Hole D, Isles C . Should diabetes be considered a coronary heart disease risk equivalent?: results from 25 years of follow-up in the Renfrew and Paisley survey. Diabetes Care 2005; 28: 1588–1593.
The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long term complications in the diabetes control in insulin dependent diabetes mellitus. N Engl J Med 329: 977–986.
Nielson C, Lange T, Hadjokas N . Blood glucose and coronary artery disease in nondiabetic patients. Diabetes Care 2006; 29: 998–1001.
Schnell O, Standl E . Impaired glucose tolerance, diabetes, and cardiovascular disease. Endocr Pract 2006; 12 (Suppl 1): 16–19.
Barr EL, Zimmet PZ, Welborn TA, Jolley D, Magliano DJ, Dunstan DW et al. Risk of cardiovascular and all-cause mortality in individuals with diabetes mellitus, impaired fasting glucose, and impaired glucose tolerance: the Australian Diabetes, Obesity, and Lifestyle Study (AusDiab). Circulation 2007; 116: 151–157.
Diamantopoulos EJ, Andreadis EA, Tsourous GI, Katsanou PM, Georgiopoulos DX, Nestora KC et al. Early vascular lesions in subjects with metabolic syndrome and prediabetes. Int Angiol 2006; 25: 179–183.
Meigs JB, Larson MG, D′Agostino RB, Levy D, Clouse ME, Nathan DM et al. Coronary artery calcification in type 2 diabetes and insulin resistance: the Framingham offspring study. Diabetes Care 2002; 25: 1313–1319.
Kim SH, Reaven GM . The metabolic syndrome: one step forward, two steps back. Diab Vasc Dis Res 2004; 1: 68–75.
Reaven GM . Insulin resistance, the insulin resistance syndrome, and cardiovascular disease. Panminerva Med 2005; 47: 201–210.
Ninomiya JK, L′Italien G, Criqui MH, Whyte JL, Gamst A, Chen RS . Association of the metabolic syndrome with history of myocardial infarction and stroke in the Third National Health and Nutrition Examination Survey. Circulation 2004; 109: 42–46.
Bingham C, Arbogast B, Guillaume GC, Lee JK, Halberg F . Inferential statistical methods for estimating and comparing cosinor parameters. Chronobiologia 1982; 9: 397–439.
Zaslavskaya RM . Chronodiagnosis and chronotherapy of cardiovascular diseases, 2nd edn. Translation into English from Russian Medicina: Moscow, 1993, pp 397.
Katinas GS, Cornélissen G, Otsuka K, Haus E, Bakken EE, Halberg F . Why continued surveillance? Intermittent blood pressure and heart rate abnormality under treatment. Biomed Pharmacother 2005; 59 (Suppl 1): S141–S151. Diabetes Care. 1999; 22:233-40.
Coutinho M, Gerstein HC, Wang Y, Yusuf S . The relationship between glucose and incident cardiovascular events. A meta regression analysis of published data from 20 studies of 95 783 individuals followed for 12.4 years. Diabetes Care 1999; 22: 1385–1387.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo Jr JL et al. National Heart, Lung, and Blood Institute Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure; National High Blood Pressure Education Program Coordinating Committee. The Seventh Report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Stolarz K, Staessen JA, O′Brien ET . Night-time blood pressure: dipping into the future? J Hypertens 2002; 20: 2131–2133 (review).
Giles TD . Circadian rhythm of blood pressure and the relation to cardiovascular events. J Hypertens Suppl 2006; 24: S11–S16 (review).
Jerrard-Dunne P, Mahmud A, Feely J . Circadian blood pressure variation: relationship between dipper status and measures of arterial stiffness. J Hypertens 2007; 25: 1233–1239.
Hermida RC, Ayala DE, Portaluppi F . Circadian variation of blood pressure: the basis for the chronotherapy of hypertension. Adv Drug Deliv Rev 2007; 59: 904–922.
Dolan E, Stanton A, Thijs L, Hinedi K, Atkins N, McClory S et al. Superiority of ambulatory over clinic blood pressure measurement in predicting mortality: the Dublin outcome study. Hypertension 2005; 46: 156–161.
Dolan E, Li Y, Thijs L, McCormack P, Staessen JA, O'Brien E et al. Ambulatory arterial stiffness index: rationale and methodology. Blood Press Monit 2006; 11: 103–105.
Li Y, Dolan E, Wang JG, Thijs L, Zhu DL, Staessen JA et al. Ambulatory arterial stiffness index: determinants and outcome. Blood Press Monit 2006; 11: 107–110.
Kikuya M, Staessen JA, Ohkubo T, Thijs L, Metoki H, Asayama K et al. Ambulatory arterial stiffness index and 24-h ambulatory pulse pressure as predictors of mortality in Ohasama, Japan. Stroke 2007; 38: 1161–1166.
Mayer B, Lieb W, Radke PW, Götz A, Fischer M, Bässler A et al. Association between arterial pressure and coronary artery calcification. J Hypertens 2007; 25: 1731–1738.
O′Brien E . Sleepers versus nonsleepers: another twist to the dipper/nondipper concept. Hypertension 2007; 49: 769–770.
Schwartzkopff O, Halberg F, Katinas G, Cornélissen G, Otsuka K, Watanabe Y et al. Strain tests: gauging variability in a day, week, year or decade. In: Proceedings 59th Annual Meeting Japan Society of Neurovegetative Research, Tokyo, November 1–3, 2006, pp 64–68.
Cornélissen G, Halberg F, Bakken EE, Singh RB, Otsuka K, Tomlinson B et al. 100 or 30 years after Janeway or Bartter, Healthwatch helps avoid ‘flying blind’. Biomed Pharmacother 2004; 58(Suppl 1): S69–S86.
De La Pena SS, Gonzalez C, Cornelissen G, Halberg F . Blood Pressure (BP), Heart Rate (HR) and Non-Insulin-Dependent Diabetes Mellitus (NIDDM) Chronobiology. Int J Cardiol 2004; 97 (Suppl 2): S14.
Cornélissen G, Halberg F, Otsuka K, Singh RB, Chen CH . Chronobiology predicts actual and proxy outcomes when dipping fails. Hypertension 2007; 49: 237–239.
Halberg F, Cornélissen G, Halberg J, Schwartzkopff O . Pre-hypertensive and other variabilities also await treatment. Am J Med 2007; 120: e19–e20.
Després JP . Cardiovascular disease under the influence of excess visceral fat. Crit Pathw Cardiol 2007; 6: 51–59 (review).
Rajala MW, Scherer PE . Minireview: the adipocyte—at the crossroads of energy homeostasis, inflammation, and atherosclerosis. Endocrinology 2003; 144: 3765–3773.
Moreno-Aliaga MJ, Campion J, Milagro FI, Berjon A, Martinez JA . Adiposity and proinflammatory state: the chicken or the egg. Adipocytes 2005; 1: 1–16.
Fantuzzi G . Adipose tissue, adipokines, and inflammation. J Allergy Clin Immunol 2005; 115: 911–919; quiz 920.
Vettor R, Milan G, Rossato M, Federspil G . Review article: adipocytokines and insulin resistance. Aliment Pharmacol Ther 2005; 22 (Suppl 2): 3–10 (review).
Xu H, Barnes GT, Yang Q, Tan G, Yang D, Chou CJ et al. Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 2003; 112: 1785–1788.
Kougias P, Chai H, Lin PH, Yao Q, Lumsden AB, Chen C . Effects of adipocyte-derived cytokines on endothelial functions: implication of vascular disease. J Surg Res 2005; 126: 121–129.
Acknowledgements
This study was supported by grants from NIH (GM-13981) (FH) and University of Minnesota Supercomputing Institute (GC and FH).
Author information
Authors and Affiliations
Corresponding author
Additional information
Presented at The Obesity Society 2007.
Rights and permissions
About this article
Cite this article
Gupta, A., Greenway, F., Cornelissen, G. et al. Prediabetes is associated with abnormal circadian blood pressure variability. J Hum Hypertens 22, 627–633 (2008). https://doi.org/10.1038/jhh.2008.32
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2008.32
Keywords
This article is cited by
-
Prevalence of prediabetes and associated factors among community members in rural Isingiro district
BMC Public Health (2023)
-
Cardiac magnetic resonance assessment of aortic distensibility in prediabetic patients
The Egyptian Heart Journal (2020)
-
The prevalence of prediabetes and associated conditions in Ahmedabad population
International Journal of Diabetes in Developing Countries (2020)
-
Within-visit blood pressure variability is associated with prediabetes and diabetes
Scientific Reports (2015)
-
Prediabetes and associated disorders
Endocrine (2015)