Abstract
N-acetylglutamate synthase (NAGS) deficiency is a rare inborn error regarding the urea cycle, however, its diagnosis is important as it can be effectively treated by N-carbamylglutamate. We evaluated a patient with NAGS deficiency who harbored two novel NAGS mutations and who showed excellent responsiveness during 1 year of N-carbamylglutamate treatment.
Similar content being viewed by others
Introduction
N-acetylglutamate synthase (NAGS) is a liver enzyme producing N-acetylglutamate from glutamate and acetyl coenzyme A. N-acetylglutamate is an essential cofactor for the first urea-cycle enzyme, carbamyl phosphate synthase I (CPS I). NAGS deficiency is an extremely rare autosomal recessive urea-cycle disorder (UCD).1 NAGS deficiency presents as an acute hyperammonemic crisis, in most patients during the newborn period. N-carbamylglutamate, a synthetic derivative of glutamic acid, is a stable structural analog of human N-acetylglutamate.2 N-carbamylglutamate is the treatment of choice for NAGS deficiency, as it thus ameliorates hyperammonemia and enhances ureagenesis.3, 4
We present a case of NAGS deficiency described with two novel NAGS mutations. One year of N-carbamylglutamate treatment improved the patient’s hyperammonemic episodes, which were formerly observed frequently. Nitrogen scavenging medication and a low-protein diet was discontinued with this treatment.
Case report
Our study patient was the first baby born to non-consanguineous Korean parents. He was born after 40 weeks of gestation after an uneventful pregnancy and delivery and weighed 3400 g. On the eighth day after birth, he showed poor feeding, vomiting and lethargy. Hyperammonemia (800 μmol l−1; normal range, 11–32 μmol l−1) was detected and was treated using i.v. fluids, protein restriction and peritoneal dialysis. His plasma glutamine was 1117 μmol l−1 (376–709 μmol l−1), and the arginine and citrulline were 51 μmol l−1 (6–140 μmol l−1) and 7 μmol l−1 (10–45 μmol l−1), respectively. His urine orotic acid level was 1.77 μmol per mol Cr (0.2–6 μmol per mol Cr). After the emergency management, he was given a low-protein diet with sodium benzoate (250 mg kg−1 per day). L-carnitine (100 mg kg−1 per day) and citrulline (100 mg kg−1 per day) were used as supplements.
At 2 years of age, he was referred to our medical institution for further evaluation and management. Molecular analysis for the CPS1 gene was normal, whereas two novel variants, c.[929T>C];[1464_1465del] and (p.[V310A];[H488Qfs*2]), were found in the NAGS gene (Figure 1). The former mutation was inherited from his mother, while the latter from his father. Treatments for the patient were low-protein diet (1.0 g kg−1 per day) with essential amino acid supplementation, sodium benzoate, L-carnitine and citrulline. The daily amount of protein intake could not be increased due to frequent episodes of hyperammonemia. After 2 years of age, medications were changed into sodium benzoate, sodium phenylbutyrate (250 mg kg−1 per day), L-carnitine and arginine (100 mg kg−1 per day) according to domestic availability of the medications.
Despite the treatment, hyperammonemia (112–357 μmol l−1) recurred every 3 to 4 months, provoked by viral infection, starvation or intake of protein-rich foods. Whenever hyperammonemic episode develops, protein intake was temporarily minimized to 0–0.5 g kg−1 per day with high glucose (7–10 mg kg−1 per min) and lipid (1 g kg−1 per day) supplementation, and increment of dosage of sodium benzoate (250–500 mg kg−1 per day) and sodium phenylbutyrate (350–400 mg kg−1 per day). The patient subsequently suffered from neuropsychological problems including seizures, mild mental retardation and attention-deficit/hyperactivity disorder. His growth velocity was decelerated with poor weight gain. At 7.6 years of age, his height and weight were −0.33 and the −2.59 of the standard deviation score, respectively.
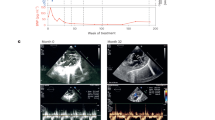
At 8.1 years of age, oral N-carbamylglutamate (Carbaglu; Orphan Europe, Paris, France; 100 mg kg−1 per day in four divided doses) was begun with the discontinuation of sodium benzoate, sodium phenylbutyrate and arginine (Figure 2a). During the first 4 months of this therapy, the hyperammonemic episodes were absent and subsequently daily protein intake was increased to 2 g kg−1 per day without any protein restriction. At age 9 years (after 1 year of treatment with N-carbamylglutamate), his plasma ammonia levels remained within the normal range (10–14 μmol l−1) with increased body mass index and growth velocity (Figure 2b). Subsequently, the dose of N-carbamylglutamate reduced to 75 mg kg−1 per day with no metabolic crisis during the next 5 months.
(a) Graph of the patient’s ammonia level. The patient presented with recurrent hyperammonemic events despite protein restriction and nitrogen scavenger treatment. After replacement of N-carbamylglutamate, the ammonia levels were in a normal range without a special diet, protein restriction or nitrogen scavenger treatment. (b) Growth curve of the patient showing stunted height and poor weight gain. The asterisk indicates the commencement of N-carbamylglutamate. A full color version of this figure is available at the Journal of Human Genetics journal online.
Discussion
NAGS deficiency is an extremely rare UCD, and only ~35 cases have been reported since the first report by Bachmann et al.1, 5 Patients with this condition usually manifest hyperammonemic encephalopathy during the first few days of life, although late-onset presentation has been reported in some patients.5, 6 The hepatic enzymatic test or molecular analysis is required for the confirmatory diagnosis of NAGS deficiency as it shows similar clinical and biochemical features as those seen in the more common UCD, CPS I deficiency, that is, hyperammonemia, high glutaminemia, low citrullinemia, and low or normal orotic aciduria.6 The patient reported here was also diagnosed following identification of the two novel NAGS mutations. p.V310A is a missense mutation and is located on a highly conserved residue in various species. The two web-based software programs, SIFT (http://sift.jcvi.org) and polyphen-2 (http://genetics.bwh.harvard.edu/pph2/), predicted that this mutation significantly alters the protein function. The other variant, p.H488Qfs*2 caused by small deletion, produces premature truncated protein, which lacks the C-terminal region (residue 488–534), and thus lacking its appropriate function.
In patients with UCD, as the neurodevelopmental prognosis is influenced by the duration of hyperammonemia and the peak ammonia levels, acute management should be done immediately in case of a hyperammonemic crisis.2, 7 In addition, long-term management, including a low-protein diet, nitrogen scavengers and liver transplantation for selected patients, and regular monitoring of biochemical parameters, physical growth and development are needed to prevent hyperammonemia and to achieve normal growth and development.2 On the other hand, in patients with NAGS deficiency, N-carbamylglutamate is the most efficacious therapy and early treatment of N-carbamylglutamate without any other interventions can predict a good prognosis.2, 8, 9 This drug is approved by the European Medicines Agency (EMA) and the Food and Drug Administration in the US for the treatment of NAGS deficiency.2 In addition, N-carbamylglutamate is licensed by the EMA for the treatment of some types of organic acidemia as it enhances ureagenesis.2 Previous studies have reported normal neurodevelopment in patients who received N-carbamylglutamate since the neonatal or infantile period. N-carbamylglutamate has maintained a stable metabolic status regardless of the onset timing.5, 8, 9 However, in some acute hyperammonemic crises, N-carbamylglutamate alone may not be sufficient, and nitrogen scavengers and extracorporeal detoxification should be considered due to their prompt effect. Our patient is the first case of NAGS deficiency in Korea. Since N-carbamylglutamate has not been made commercially available in Korea, N-carbamylglutamate could be prescribed only after he reached 8 years of age and could be provided by a compassionate program. Since then, our patient has showed a marked response to this drug and has an improved quality of life, although after only short-term observation. Gastrointestinal symptoms, such as vomiting, abdominal pain and diarrhea, have been reported as common adverse reactions, although the drug administration has been tolerable in our patient.4 A few long-term follow-up studies have shown that N-carbamylglutamate has beneficial effects including a stable metabolic status and improvement in growth and neurodevelopment without serious safety issues.10, 11
In conclusion, this case report provides yet more evidence of the N-carbamylglutamate efficacy in NAGS deficiency and underscores the importance of early identification and treatment for optimizing the patient prognosis.
References
Bachmann, C., Krahenbuhl, S., Colombo, J. P., Schubiger, G., Jaggi, K. H. & Tonz, O. N-acetylglutamate synthetase deficiency: a disorder of ammonia detoxication. N. Engl. J. Med. 304, 543 (1981).
Haberle, J., Boddaert, N., Burlina, A., Chakrapani, A., Dixon, M. & Huemer, M. et al. Suggested guidelines for the diagnosis and management of urea cycle disorders. Orphanet J. Rare Dis 7, 32 (2012).
Tuchman, M., Caldovic, L., Daikhin, Y., Horyn, O., Nissim, I. & Korson, M. et al. N-carbamylglutamate markedly enhances ureagenesis in N-acetylglutamate deficiency and propionic acidemia as measured by isotopic incorporation and blood biomarkers. Pediatr. Res. 64, 213–217 (2008).
Daniotti, M., la Marca, G., Fiorini, P. & Filippi, L. New developments in the treatment of hyperammonemia: emerging use of carglumic acid. Int. J. Gen. Med. 4, 21–28 (2011).
Cartagena, A., Prasad, A. N., Rupar, C. A., Strong, M., Tuchman, M. & Ah Mew, N. et al. Recurrent encephalopathy: NAGS (N-acetylglutamate synthase) deficiency in adults. Can. J. Neurol. Sci. 40, 3–9 (2013).
Caldovic, L., Ah Mew, N., Shi, D., Morizono, H., Yudkoff, M. & Tuchman, M. N-acetylglutamate synthase: structure, function and defects. Mol. Genet. Metab. 100 (Suppl 1), S13–S19 (2010).
Lee, B. H., Kim, Y. M., Heo, S. H., Kim, G. H., Choi, I. H. & Lee, B. S. et al. High prevalence of neonatal presentation in Korean patients with citrullinemia type 1, and their shared mutations. Mol. Genet. Metab. 108, 18–24 (2013).
Van Leynseele, A., Jansen, A., Goyens, P., Martens, G., Peeters, S. & Jonckheere, A. et al. Early treatment of a child with NAGS deficiency using N-carbamyl glutamate results in a normal neurological outcome. Eur. J. Pediatr. 173, 1635–1638 (2013).
Gessler, P., Buchal, P., Schwenk, H. U. & Wermuth, B. Favourable long-term outcome after immediate treatment of neonatal hyperammonemia due to N-acetylglutamate synthase deficiency. Eur. J. Pediatr. 169, 197–199 (2010).
Guffon, N., Gessler, P., Galloway, P., Martinez-Pardo, M., Meli, C. & Mulder, M. et al. Treatment of NAGS deficiency: retrospective data on 23 patients treated with carglumic acid over 16 years. Mol. Genet. Metab. 102, 286–287 (2011).
Christelle, C., Alain, F., Cécile, A. & Gerard, B. First French case of NAGS deficiency. 20 years of follow up. Mol. Genet. Metab. 102, 275 (2011).
Acknowledgements
This study was supported by a grant from the National Research Foundation of Korea funded by the Ministry of Education, Science, and Technology (Grant No. 2011-0019674). We thank SAMOH PHARM for providing their compassionate use program.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kim, J., Kim, YM., Lee, B. et al. Short-term efficacy of N-carbamylglutamate in a patient with N-acetylglutamate synthase deficiency. J Hum Genet 60, 395–397 (2015). https://doi.org/10.1038/jhg.2015.30
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2015.30
This article is cited by
-
The efficacy of Carbamylglutamate impacts the nutritional management of patients with N-Acetylglutamate synthase deficiency
Orphanet Journal of Rare Diseases (2024)
-
Presentation and management of N-acetylglutamate synthase deficiency: a review of the literature
Orphanet Journal of Rare Diseases (2020)
-
Low prevalence of argininosuccinate lyase deficiency among inherited urea cycle disorders in Korea
Journal of Human Genetics (2018)
-
Aminoacidopathies: Prevalence, Etiology, Screening, and Treatment Options
Biochemical Genetics (2018)
-
A commentary on short-term efficacy of N-carbamylglutamate in a patient with N-acetylglutamate synthase deficiency
Journal of Human Genetics (2015)