Abstract
In Nepal, we tested 300 males for glucose-6-phosphate dehydrogenase (G6PD) activity. Two subjects were G6PD deficient (0.67%). Compared with normal controls, G6PD activity was 12% and 26%, respectively. The hemoglobin concentration of these two subjects was normal. We extracted genomic DNA from whole blood and read all sequences of G6PD. Both subjects had the same replacement of 563C>T, which was classified as G6PD Mediterranean. The amino acid might change from Ser to Phe at codon 188. These subjects also had a replacement of 1311C>T, which caused no replacement of an amino acid. A similar replacement pattern of G6PD Mediterranean is described from persons living in Mediterranean countries and Middle East countries. However, G6PD Mediterranean found in India and Pakistan has no replacement at nucleotide 1311. Thus, these two subjects in Kathmandu, Nepal, would be closer to people in Middle East countries than people in India. This is the first study of molecular analysis for G6PD deficiency in Nepal.
Similar content being viewed by others
Introduction
Glucose-6-phosphate dehydrogenase (G6PD) deficiency is one of the most frequent hereditary abnormalities. G6PD is located on the X chromosome, and is composed of 13 exons (Chen et al. 1991). Almost all G6PD deficiencies are caused by one amino-acid change, resulting from a point mutation of the genomic DNA, and greater than 100 molecular abnormalities of the G6PD genotype have been identified (Fujii and Miwa 1998). We have described ten molecular abnormalities of the G6PD genotype in Southeast Asian countries (Iwai et al. 2001).
We have introduced rapid diagnosis methods of malaria, which kills more than two million people in the world every year, and G6PD deficiency test in malaria endemic areas. With these methods, patients are notified of the results of blood examination within 30 min and are able to receive anti-malaria medicine, including primaquine (Tantular et al. 1999). Primaquine can kill gametocytes, the sexual stage of malaria parasites, which are the cause of malaria transmission via mosquitoes. However, once G6PD-deficient persons take primaquine, a hemolysis attack can follow. Without G6PD, erythrocytes cannot prepare a sufficient amount of reduced pyridine nucleotide and reduced glutathione, and cannot prevent oxidant attack by primaquine. Thus, primaquine should not be administered to malaria patients before confirming their G6PD condition.
In Nepal, malaria endemic areas distribute along the India-Nepal border where the altitude is less than 1,000 meters above sea level and malaria transmittable vector mosquitoes, Anopheles species, survive. We intended to introduce rapid diagnosis methods for malaria and G6PD activity in rural areas in Nepal. Prior to starting the project, we conducted a small investigation for G6PD deficiency, because, for Nepalese, only one study has reported the prevalence of G6PD deficiency (Henderson and Baronne 1987), and there has been no molecular analysis study of G6PD.
Materials and methods
In the National College for Advanced Learning, Kathmandu, Nepal, we collected 10 µl of blood from 270 male students and 30 male staff members on cation exchange cellulose paper (Whatman, P81). In total 300 samples were examined. The age of students was 16–22 years old, and the age of staff members was 21–51 years old. We received informed consent from each person before collecting blood. The blood spots were punched out in a 6-mm diameter disk, put on an agar plate for the G6PD test, and incubated at 37 °C for 8 h (Fujii et al. 1984). If G6PD activity was normal, blue formazan ring (greater than 10 mm in diameter) appeared around the filter sheet. If G6PD was not normal, the formazan ring appeared small (less than 8 mm). G6PD activity was estimated by measuring the area of blue formazan spot (Fujii et al. 1984).
When a G6PD-deficient person was found, we received additional informed consent and took 0.5 ml of peripheral blood. To evaluate the anemic state, hemoglobin concentration was measured by the oxyhemoglobin method. Genomic DNA was extracted from 0.1 ml of whole blood and purified with a DNA purification kit (Amersham Pharmacia Biotech, Buckinghamshire, UK). Since genomic G6PD consists of 13 exons, we prepared primers for each exon (Iwai et al. 2001), amplified the exon by PCR, and read the DNA sequence (ABI PRISM 310; PE Biosystems, Conn., USA). Both strands of each exon were sequenced.
Results and discussion
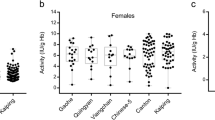
Among 300 Nepalese males, two subjects were G6PD-deficient (0.67%). They were not related to each other. They did not have a history of malaria infection or hemolytic attack. The hemoglobin concentrations of these two subjects were normal. When compared with normal control, their G6PD activity was estimated as 26% and 12%, respectively (Fig. 1).
In Asian countries, the prevalence of G6PD deficiency is different in each country or each ethnic group (Panich 1986). In our previous studies, the prevalence of G6PD deficiency in Southeast Asian countries was 0–14.1% in male populations (Matsuoka et al. 1986; Tantular et al. 1999; Iwai et al. 2001). In Nepalese, only one study on G6PD deficiency was reported by Henderson and Baronne (1987). They used the Sigma Diagnostics G6PD Kit, tested 441 healthy subjects that immigrated to Hong Kong but originally lived in mid-hill areas in Nepal, where malaria transmission had not occurred, and found one G6PD deficiency case. The prevalence was accordingly calculated as 0.23%. They did not add further molecular analysis on this case.
We collected blood samples in Kathmandu, where the altitude was 1,300–1,400 m above sea level and malaria transmission had not occurred. Malaria appears to exert a selection pressure in favor of G6PD deficiency, since deficiency confers relative protection against Plasmodium falciparum (Ruwende et al. 1995). The present result, that the prevalence of G6PD deficient was 0.67%, would be reasonable, because in the mid-hills (e.g., Kathmandu) selection pressure was absent, and the prevalence of G6PD had not increased.
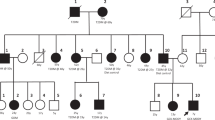
We read all 1,545 bp of G6PD of the two persons and found that both had the same mutation, a replacement of 563C>T in exon 6 (Fig. 2). This variant was previously reported as G6PD Mediterranean. Serine (TCC) at codon 188 might be substituted by phenylalanine (TTC). From both subjects, another replacement 1311C>T was found in exon 11. This replacement 1311C>T was a silent mutation, because both TAC and TAT coded tyrosine.
We have described ten molecular abnormalities of G6PD genotype in Southeast Asian countries (Iwai et al. 2001), but we have not found G6PD Mediterranean (563C>T). According to previous studies, G6PD Mediterranean cases are found from Mediterranean countries, Middle East countries, Pakistan and India (Luzzatto and Notaro 2001). Among G6PD Mediterranean cases, people in Mediterranean countries and Middle East countries have a silent mutation (1311C>T) (Kurdi-Haidar et al. 1990; Samilchuk et al. 1999), and people in Pakistan and India show wild type (1311C) (Beutler and Kuhl 1990; Kaeda et al. 1995). The two cases of G6PD Mediterranean in Nepal in the present study showed the silent mutation (1311C>T). From the view of G6PD, Nepalese appear to be closer to the population in the Middle East countries than Indian populations. Nepalese consist of many ethnic groups, and we only investigated a small population in Kathmandu in the present study. We should study larger populations and more ethnic groups. Since we are going to start rapid diagnosis methods of malaria and G6PD in rural areas at India-Nepal border, we may be able to analyze this issue in the near future.
References
Beutler E, Kuhl W (1990) The NT 1311 polymorphism of G6PD: G6PD Mediterranean mutation may have originated independently in Europe and Asia. Am J Hum Genet 47:1008–1012
Chen EY, Cheng A, Lee A, Kuang WJ, Hillier L, Green P, Schlessinger D, Ciccodicola A, D'Urso M (1991) Sequence of human glucose-6-phosphate dehydrogenase cloned in plasmids and a yeast artificial chromosome. Genomics 10:792–800
Fujii H, Miwa S (1998) Red blood cell enzymes and their clinical application. Adv Clin Chem 33:1-54
Fujii H, Takahashi K, Miwa S (1984) A new simple screening method for glucose 6-phosphate dehydrogenase deficiency. Acta Haematol Jpn 47:185–188
Henderson A, Baronne A (1987) Glucose-6-phosphate dehydrogenase deficiency in healthy Nepalese patients. Trans Roy Soc Trop Med Hyg 81:543
Iwai K, Hirono A, Matsuoka H, Kawamoto F, Horie T, Lin K, Tantular IS, Dachlan YP, Notopuro H, Hidayah NI, Salim A M, Fujii H, Miwa S, Ishii A (2001) Distribution of glucose-6-phosphate dehydrogenase mutations in Southeast Asia. Human Genetics 108:445–449
Kaeda JS, Chhotray GP, Ranjit MR, Bautista JM, Reddy PH, Stevens D, Naidu JM, Britt RP, Vulliamy TJ, Luzzatto L, Mason PJ (1995) A new glucose-6-phosphate dehydrogenase variant, G6PD Orissa (44 Ala→Gly), is the major polymorphic variant in tribal populations in India. Am J Hum Genet 57:1335–1341
Kurdi-Haidar B, Mason PJ, Berrebi A, Ankra-Badu G, al-Ali A, Oppenheim A, Luzzatto L (1990) Origin and spread of the glucose-6-phosphate dehydrogenase variant (G6PD-Mediterranean) in the Middle East. Am J Hum Genet 47:1013–1019
Luzzatto L, Notaro R (2001) Malaria. Protecting against bad air. Science 20:442–443
Matsuoka H, Ishii A, Panjaitan W, Sudiranto R (1986) Malaria and glucose-6-phosphate dehydrogenase deficiency in North Sumatra, Indonesia. Southeast Asian J Trop Med Public Health 17:530-536
Panich V (1986) G6PD Variants in southern Asian populations. In: Yoshida A, Beutler E (eds) Glucose-6-phosphate dehydrogenase deficiency. Academic Press, London, pp 195–241
Ruwende C, Khoo SC, Snow RW, Yates SN, Kwiatkowski D, Gupta S, Warn P, Allsopp CE, Gilbert SC, Peschu N, Newbold CI, Greenwood BM, Marsh K, Hill AVS (1995) Natural selection of hemi- and heterozygotes for G6PD deficiency in Africa by resistance to severe malaria. Nature 376:246–249
Samilchuk E, D'Souza B, Al-Awadi S (1999) Population study of common glucose-6-phosphate dehydrogenase mutations in Kuwait. Hum Hered 49:41–44
Tantular IS, Iwai K, Khin-Lin, Basuki S, Horie T, Htay HH, Matsuoka H, Marwoto H, Wongsrichanalai C, Dachlan Y P, Kojima S, Ishii A, Kawamoto F (1999) Field trials of a rapid test for G6PD deficiency in combination with a rapid diagnosis of malaria. Trop Med Int Health 4:245–250
Acknowledgements
This work was supported by a grant-in-aid from the Japanese Ministry of Education, Science, Culture and Sports (12576019 to H.M.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Matsuoka, H., Jichun, W., Hirai, M. et al. Two cases of glucose-6-phophate dehydrogenase-deficient Nepalese belonging to the G6PD Mediterranean-type, not India-Pakistan sub-type but Mediterranean-Middle East sub-type. J Hum Genet 48, 275–277 (2003). https://doi.org/10.1007/s10038-003-0018-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10038-003-0018-2
Keywords
This article is cited by
-
G6PD deficiency in malaria endemic areas of Nepal
Malaria Journal (2020)
-
Glucose-6-phosphate dehydrogenase deficiency in people living in malaria endemic districts of Nepal
Malaria Journal (2017)
-
Prevention of Kernicterus in South Asia: Role of Neonatal G6PD Deficiency and its Identification
The Indian Journal of Pediatrics (2014)
-
Glucose-6-phosphate dehydrogenase (G6PD) mutations in Cambodia: G6PD Viangchan (871G>A) is the most common variant in the Cambodian population
Journal of Human Genetics (2005)
-
Five different glucose-6-phophate dehydrogenase (G6PD) variants found among 11 G6PD-deficient persons in Flores Island, Indonesia
Journal of Human Genetics (2003)