Abstract
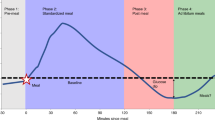
More than 50 years ago, Jean Mayer proposed that changes in blood glucose concentrations or arteriovenous glucose differences are detected by glucoreceptors that affect energy intake. According to this theory, an increase in blood glucose concentrations results in increased feelings of satiety whereas a drop in blood glucose concentrations has the opposite effect. The pioneering work of Mayer has recently received support from our group as low glycemia has been shown to be linked with body weight gain prospectively and has been considered as a strong predictor of the amount of weight regained after weight loss. This state of mild hypoglycemia also predicts the increase in depressive symptoms with weight loss and a greater propensity to glucose intolerance and type 2 diabetes, particularly for individuals having short sleep durations. Furthermore, knowledge-based work has been shown to induce a significant increase in spontaneous energy intake being related to changes in glycemic control. In accordance with the glucostatic theory, this oriented review suggests that factors favoring a trend toward hypoglycemia and/or glucose instability might induce excess energy intake, overweight and impaired glucose tolerance. Data also raise the possibility that fat gain might be protective against mild hypoglycemia by providing compensation to the stimuli promoted by a modern environment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Kennedy GC . The hypothalamic control of food intake in rats. Proc R Soc Lond B Biol Sci 1950; 889: 535–549.
Mellinkoff SM, Frankland M, Boyle D, Greipel M . Relationship between serum amino acid concentration and fluctuations in appetite. J Appl Physiol 1956; 8: 535–538.
Brobeck JR . Food intake as a mechanism of temperature regulation. Yale J Biol Med 1948; 20: 545–552.
Bray GA, Campfield LA . Metabolic factors in the control of energy stores. Metabolism 1975; 24: 99–117.
Schwartz MW, Woods SC, Porte Jr D, Seely RJ, Baskin DG . Central nervous system control of food intake. Nature 2000; 404: 661–671.
Campfield LA, Smith FJ . Blood glucose dynamics and control of meal initiation: a pattern detection and recognition theory. Physiol Rev 2003; 83: 25–58.
Carlson AJ (ed). The Control of Hunger in Health and Disease. University of Chicago Press: Chicago IL, 1916.
Mayer J . Glucostatic mechanism of regulation of food intake. N Engl J Med 1953; 249: 13–16.
Mayer J . Regulation of energy intake and the body weight, the glucostatic theory and the lipostatic hypothesis. Ann NY Acad Sci 1955; 63: 15–43.
Stunkard AJ, Van Italie TB, Reiss BB . Effect of glucagon on gastric hunger contractions in man. Proc Soc Exp Biol Med 1955; 89: 258–261.
Van Itallie TB, Beaudoin R, Mayer J . Arteriovenous glucose differences, metabolic hypoglycemia and food intake in man. J Clin Nutr 1953; 1: 208–216.
Bernstein LM, Grossman MI . An experimental test of the glucostatic theory of the regulation of food intake. J Clin Invest 1956; 35: 627–633.
Van Itallie TB, Hashim SA . Biochemical concomitants of hunger and satiety in man. Am J Clin Nutr 1960; 8: 587–594.
Booth DA, Campbell AT, Chase A . Temporal bounds of post-ingestive glucose induced satiety in man. Nature 1970; 228: 1104–1105.
Stunkard AJ, Wolff HG . Studies on the physiology of hunger. I. The effect of intravenous administration of glucose on gastric hunger contractions in man. J Clin Invest 1956; 35: 954–963.
Van Itallie TB . The glucostatic theory 1953–1988: roots and branches. Int J Obes 1990; 14: 1–10.
Grinker J, Cohn CK, Hirsch J . The effects of intravenous administration of glucose, saline, and mannitol on meal regulation in normal-weight human subjects. Behav Biol 1971; 6: 203–208.
Woo R, Kissileff H, Pi-Sunyer XF . Elevated post-prandial insulin levels do not induce satiety in normal-weight humans. Am J Physiol Regul Integr Comp Physiol 1984; 247: R-475–R-479.
Louis-Sylvestre J, Le Magnen J . A fall in blood glucose level precedes meal onset in free-feeding rats. Neurosci Biobehav Rev 1980; 4: 13–15.
Campfield LA, Smith FJ . Functional coupling between transient declines in blood glucose and feeding behavior: temporal relationships. Brain Res Bull 1986; 17: 427–433.
Campfield LA, Smith FJ . Transient declines in blood glucose signal meal initiation. Int J Obes 1990; 14: 15–31.
Campfield LA, Smith FJ, Rosenbaum M, Hirsch J . Human eating: evidence for a physiological basis using a modified paradigm. Neurosci Biobehav Rev 1996; 20: 133–137.
Melanson KJ, Westerterp-Plantenga MS, Campfield LA, Saris WH . Blood glucose and meal patterns in time-blinded males, after aspartame, carbohydrate, and fat consumption, in relation to sweetness perception. Br J Nutr 1999; 82: 437–446.
Melanson KJ, Westerterp-Plantenga MS, Saris WH, Smith FJ, Campfield LA . Blood glucose patterns and appetite in time-blinded humans: carbohydrate versus fat. Am J Physiol 1999; 277: R337–R345.
Louis-Sylvestre J . Glucose utilization dynamics and food intake. Brit J Nutr 1999; 82: 427–429.
Bray GA . Static theories in a dynamic world: a glucodynamic theory of food intake. Obes Res 1996; 4: 489–492.
Boulé NG, Chaput JP, Doucet E, Richard D, Després JP, Bouchard C et al. Glucose homeostasis predicts weight gain: prospective and clinical evidence. Diabetes Metab Res Rev 2008; 24: 123–129.
Halverson JD, Kramer J, Cave A, Permutt A, Santiago J . Altered glucose tolerance, insulin response, and insulin sensitivity after massive weight reduction subsequent to gastric bypass. Surgery 1982; 92: 235–240.
Marsoobian V, Grosvenor M, Jacob M, Ipp E . Very-low-energy diets alter the counterregulatory response to falling plasma glucose concentrations. Am J Clin Nutr 1995; 61: 373–378.
Permutt MA, Delmez J, Stenson W . Effects of carbohydrate restriction on the hypoglycemic phase of the glucose tolerance test. J Clin Endocrinol Metab 1976; 43: 1088–1093.
Tremblay A, Doucet E, Imbeault P, Mauriège P, Després JP, Richard D . Metabolic fitness in active reduced-obese individuals. Obes Res 1999; 7: 556–563.
Leblanc J, Nadeau A, Richard D, Tremblay A . Variations in plasma glucose, insulin, growth hormone and catecholamines in response to insulin in trained and non-trained subjects. Metabolism 1982; 31: 453–456.
Tremblay A, Sauvé L, Després JP, Nadeau A, Thériault G, Bouchard C . Metabolic characteristics of postobese individuals. Int J Obes 1989; 13: 357–366.
Chaput JP, Drapeau V, Hetherington M, Lemieux S, Provencher V, Tremblay A . Psychobiological impact of a progressive weight loss program in obese men. Physiol Behav 2005; 86: 224–232.
Chaput JP, Drapeau V, Hetherington M, Lemieux S, Provencher V, Tremblay A . Psychological effects observed in obese men experiencing body weight loss plateau. Depress Anxiety 2007; 24: 518–521.
Chaput JP, Arguin H, Gagnon C, Tremblay A . Increase in depression symptoms with body weight loss: association with glucose homeostasis and thyroid function. Appl Physiol Nutr Metab 2008; 33: 86–92.
Goldstein DJ . Beneficial health effects of modest weight loss. Int J Obes 1992; 16: 397–415.
Tremblay A, Després JP, Maheux J, Pouliot MC, Nadeau A, Moorjani S et al. Normalization of the metabolic profile in obese women by exercise and a low fat diet. Med Sci Sports Exerc 1991; 23: 1326–1331.
Tremblay A, Therrien F . Physical activity and body functionality: implications for obesity prevention and treatment. Can J Physiol Pharmacol 2006; 84: 149–156.
Boulé NG, Weisnagel SJ, Lakka TA, Tremblay A, Bergman RN, Rankinen T et al. Effects of exercise training on glucose homeostasis: the HERITAGE Family Study. Diabetes Care 2005; 28: 108–114.
Frese M . The changing nature of work. In: Chmiel N (ed). An Introduction to Work and Organisational Psychology. Blackwell Publishing: Oxford, 2000, pp 424–439.
Stubbs RJ, Murgatroyd PR, Goldberg GR, Prentice AM . Carbohydrate balance and the regulation of day-to-day food intake in humans. Am J Clin Nutr 1993; 57: 897–903.
Campfield AL, Smith JF . Systemic factors in the control of food intake. Evidence for patterns as signals. In: Stricker EM (ed). Handbook of Behavioral Neurobiology. Plenum Press: New York, 1990, pp 183–206.
Mayer J, Thomas DW . Regulation of food intake and obesity. Science 1967; 156: 328–337.
Flatt JP . Dietary fat, carbohydrate balance, and weight maintenance: effects of exercise. Am J Clin Nutr 1987; 45: 296–306.
Russek M . Current status of the hepatostatic theory of food intake control. Appetite 1981; 2: 137–143.
Chaput JP, Tremblay A . Acute effects of knowledge-based work on feeding behavior and energy intake. Physiol Behav 2007; 90: 66–72.
McCann BS, Warnick GR, Knopp RH . Changes in plasma lipids and dietary intake accompanying shifts in perceived workload and stress. Psychosom Med 1990; 52: 97–108.
Chaput JP, Drapeau V, Poirier P, Teasdale N, Tremblay A . Glycemic instability and spontaneous energy intake: association with knowledge-based work. Psychosom Med 2008; 70: 797–804.
Humphrey DG, Kramer AF . Toward a psychophysiological assessment of dynamic changes in mental workload. Hum Factors 1994; 36: 3–26.
Humphrey DG, Kramer AF . Auditory probe sensitivity to mental workload changes–an event-related potential study. Int J Psychophysiol 2001; 40: 201–209.
Bonnet MH, Arand DL . We are chronically sleep deprived. Sleep 1995; 18: 908–911.
Chokroverty S (ed). Sleep Disorders Medicine: Basic Science, Technical Considerations, and Clinical Aspects, 2nd edn. Butterworth and Heinemann: Boston, MA, 1999, pp 14–16.
Kripke DF, Simons RN, Garfinkel L, Hammond EC . Short and long sleep and sleeping pills. Is increased mortality associated? Arch Gen Psychiatry 1979; 36: 103–116.
Amos AF, McCarty DJ, Zimmet P . The rising global burden of diabetes and its complications: estimates and projections to the year 2010. Diabet Med 1997; 14 (Suppl 5): S1–S85.
National Sleep Foundation. 2002 ‘Sleep in America’ Poll. National Sleep Foundation: Washington, DC, 2002. Available at http://www.sleepfoundation.org/site/c.huIXKjM0IxF/b.2417141/k.2E30/The_National_Sleep_Foundation.htm.
Taheri S, Lin L, Austin D, Young T, Mignot E . Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS Med 2004; 1: 210–217.
Gangwisch JE, Malaspina D, Boden-Albala B, Heymsfield SB . Inadequate sleep as a risk factor for obesity: analyses of the NHANES I. Sleep 2005; 28: 1289–1296.
Chaput JP, Brunet M, Tremblay A . Relationship between short sleeping hours and childhood overweight/obesity: results from the ‘Québec en Forme’ Project. Int J Obes 2006; 30: 1080–1085.
Patel SR, Malhotra A, White DP, Gottlieb DJ, Hu FB . Association between reduced sleep and weight gain in women. Am J Epidemiol 2006; 164: 947–954.
Chaput JP, Després JP, Bouchard C, Tremblay A . The association between sleep duration and weight gain in adults: a 6-year prospective study from the Quebec Family Study. Sleep 2008; 31: 517–523.
Ayas NT, White DP, Al-Delaimy WK, Manson JE, Stampfer MJ, Speizer FE et al. A prospective study of self-reported sleep duration and incident diabetes in women. Diabetes Care 2003; 26: 380–384.
Nilsson PM, Roost M, Engstrom G, Hedblad B, Berglund G . Incidence of diabetes in middle-aged men is related to sleep disturbances. Diabetes Care 2004; 27: 2464–2469.
Mallon L, Broman JE, Hetta J . High incidence of diabetes in men with sleep complaints or short sleep duration: a 12-year follow-up study of a middle-aged population. Diabetes Care 2005; 28: 2762–2767.
Yaggi HK, Araujo AB, McKinlay JB . Sleep duration as a risk factor for the development of type 2 diabetes. Diabetes Care 2006; 29: 657–661.
Chaput JP, Després JP, Bouchard C, Tremblay A . Association of sleep duration with type 2 diabetes and impaired glucose tolerance. Diabetologia 2007; 50: 2298–2304.
Patel SR, Hu FB . Short sleep duration and weight gain: a systematic review. Obesity (Silver Spring) 2008; 16: 643–653.
Spiegel K, Leproult R, Van Cauter E . Impact of sleep debt on metabolic and endocrine function. Lancet 1999; 354: 1435–1439.
Spiegel K, Knutson K, Leproult R, Tasali E, Van Cauter E . Sleep loss: a novel risk factor for insulin resistance and type 2 diabetes. J Appl Physiol 2005; 99: 2008–2019.
Tremblay A, Doucet E . Obesity: a disease or a biological adaptation? Obes Rev 2000; 1: 27–35.
Zhang Y, Proenca R, Maffei M, Barone M, Leopold L, Friedman JM . Positional cloning of the mouse obese gene and its human homologue. Nature 1994; 372: 425–432.
Tremblay A, Boulé N, Doucet E, Woods SC . Is the insulin resistance syndrome the price to be paid to achieve body weight stability? Int J Obes 2005; 29: 1295–1298.
Groop LC, Bonadonna RC, Simonson DC, Petrides AS, Shank M, DeFronzo RA . Effect of insulin on oxidative and nonoxidative pathways of free fatty acid metabolism in human obesity. Am J Physiol 1992; 263: E79–E84.
Astrup A, Buemann B, Western P, Toubro S, Raben A, Christensen NJ . Obesity as an adaptation to high-fat diet: evidence from a cross-sectional study. Am J Clin Nutr 1994; 59: 350–355.
Schutz Y, Tremblay A, Weinsier RL, Nelson KM . Role of fat oxidation in the long-term stabilization of body weight in obese women. Am J Clin Nutr 1992; 55: 670–674.
O’Dea K, Esler M, Leonard P, Stockigt JR, Nestel P . Noradrenaline turnover during under- and over-training in normal weight subjects. Metabolism 1982; 31: 896–899.
Aronne LJ, Mackintosh R, Rosenbaum M, Leibel RL, Hirsch J . Autonomic nervous system activity in weight gain and weight loss. Am J Physiol 1995; 269: R222–R225.
Tremblay A, Nadeau A, Després JP, Bouchard C . Hyperinsulinemia and regulation of energy balance. Am J Clin Nutr 1995; 61: 827–830.
Considine RV, Sinha MK, Heiman ML, Kriauciunas A, Stephens TW, Nyce MR et al. Serum immunoreactive-leptin concentrations in normal-weight and obese subjects. N Engl J Med 1996; 334: 292–295.
Acknowledgements
JPC is supported by a studentship from the Hôpital Laval Research Center and AT is partly funded by the Canada Research Chair in Environment and Energy Balance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflicts of interest
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Chaput, JP., Tremblay, A. The glucostatic theory of appetite control and the risk of obesity and diabetes. Int J Obes 33, 46–53 (2009). https://doi.org/10.1038/ijo.2008.221
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2008.221
Keywords
This article is cited by
-
Increased plasma asprosin levels are associated with overeating and loss of control in drug-free bulimia nervosa
Eating and Weight Disorders - Studies on Anorexia, Bulimia and Obesity (2022)
-
Increased plasma asprosin levels in patients with drug-naive anorexia nervosa
Eating and Weight Disorders - Studies on Anorexia, Bulimia and Obesity (2021)
-
The novel GCK variant p.Val455Leu associated with hyperinsulinism is susceptible to allosteric activation and is conducive to weight gain and the development of diabetes
Diabetologia (2021)
-
Increased oral processing and a slower eating rate increase glycaemic, insulin and satiety responses to a mixed meal tolerance test
European Journal of Nutrition (2021)
-
Contribution of macronutrients to obesity: implications for precision nutrition
Nature Reviews Endocrinology (2020)