Abstract
The clinical spectrum of preeclampsia (PE) ranges from mild hypertension to severe vasospasm associated with convulsions and multiple organ damage. The biological factors that determine the progression of PE to eclampsia (E) are unknown. Endothelial cell activation seems related to an impaired maternal immune response. The production of cytokines, IL-10 and TGF-β1, is apparently suppressed, and altered IL-2/IL-10 and TNF-α/IL-10 ratios have been reported in preeclamptic cases. The relationship between PE and cytokine gene polymorphism has been studied, but there are few studies that include eclamptic patients. This study aimed at investigating whether polymorphisms in genes, TNF-α promoter (−308 G>A), IL6 promoter (−174 G>C), IFN-γ intron 1 (+874 A>T), IL10 promoters (−1082 A>G), (−819 C>T) and (−592 C>A) and TGF-β1 codon 10 (+869 T>C) and codon 25 (+915 G>C) are associated with E and/or PE. Genotyping was carried out in 266 Mulatto women from the northeastern region of Brazil who were referred to a single maternity hospital: 92 with PE, 73 with E and 101 normotensive controls. The χ2 or Fisher's exact tests were used to compare genotype frequencies. Among the six single-nucleotide polymorphisms (SNPs) studied, we found no difference in genotype frequencies between the groups. There was a higher frequency of IFN-γ (+874 A) in eclamptic patients in comparison with that in controls. (70.3 vs. 57.8%, respectively; P=0.02). There were no other significant differences in allelic frequencies between eclamptic, preeclamptic and control groups We found no independent association between any single SNP and PE or E risk in this population of Mulatto women from the northeastern region of Brazil.
Similar content being viewed by others
Introduction
Preeclampsia (PE) is a common systemic obstetric disorder and a major cause of maternal and neonatal morbidity and mortality. The clinical spectrum of PE is large, ranging from mild hypertension with minimal proteinuria to severe hypertension associated with convulsions and multiple end-organ damage that can lead to maternal demise.1 Current knowledge suggests that the underlying physiopathology for eclampsia (E) is a posterior reversible encephalopathy syndrome with vasogenic edema because of hyperfusion rather than vasospasms.2 The biological factors that determine the progression of PE to E are unknown. General endothelial cell activation is present in both conditions, and seems to be related to an impaired maternal immune response.3
Excessive innate activity and a shift toward an inflammatory cytokine profile have been reported in PE.4, 5 Elevated levels of Th-1 cytokines, such as tumor necrosis factor TNF-α, IFN-γ and low IL-4 production by phytohemagglutinin-stimulated peripheral blood mononuclear cells have been identified in preeclamptic patients. The production of immunoregulatory cytokines, IL-10 and TGF-β1, is apparently suppressed, and altered IL-2/IL-10 and TNF-α/IL-10 ratios have been reported in placental tissue from preeclamptic cases.6
Cytokine gene polymorphisms have been associated with certain inflammatory and infectious diseases, including some obstetric disorders.7, 8, 9, 10 The relationship between PE and single-nucleotide polymorphisms (SNPs) in cytokine genes has been investigated, but is still unclear.11, 12, 13, 14, 15
The controversial results reported by different investigators may in part be because of selection criteria. Genotype frequencies of SNPs and linkage disequilibrium patterns can differ among ethnic groups, leading to different results.16 Moreover, distinct clinical patterns may involve different pathological mechanisms.17, 18 Few studies have evaluated patients with E.
Considering that cytokine gene polymorphism may influence disease susceptibility, severity and outcome,7, 19, 20 our purpose was to investigate whether polymorphisms in genes, TNF-α promoter (−308 G>A), IL6 promoter (−174 G>C), IFN-γ intron 1 (+874 A>T), IL10 promoters (−1082 A>G), (−819 C>T) and (−592 C>A) and TGF-β1 codon 10 (+869 T>C) and codon 25 (+915 G>C) are associated with E and/or PE in a northeastern Brazilian population.
Methods
All patients were Mulatto (of mixed white and black ancestry) and lived in the same geographical location (Maceio, Alagoas, Brazil). All women with a single live pregnancy and who were referred to a single hospital (Santa Monica Obstetric Clinic) were eligible.
This case–control study included 92 women with PE, 73 patients with E and 101 healthy women (control). The control women had to be normotensive in the index pregnancy, with a history of at least one previous normal pregnancy, without any maternal or fetal disorder.
The diagnoses of PE and E were based on the criteria of the Report of the ‘National High Blood Pressure Education Program.’21
Exclusion criteria were multiple gestation, fetal death, autoimmune disease, diabetes, uterine malformation, in vitro fertilization treatment, placental abruption, any infection, cancer or any other systemic disease, including preexisting hypertension.
On admission, 5 ml of venous blood was drawn from each participant. The samples were collected in tubes containing ethylenediamine tetraacetic acid (Sigma-Aldrich Corp., St Louis, MO, USA), immediately centrifuged to separate the buffy coat containing polymorphonuclear cells and frozen at −20°C for later DNA extraction.
The study protocol was approved by the ethics committee of Alagoas State University. Written informed consent was obtained from each participant. Experimental procedures on humans followed the ethical standards for human experimentation that were established by the Declaration of Helsinki of 1975, revised in 1983.
Genotyping
DNA was extracted from whole blood by the dodecyl trimethyl-ammonium bromide/cetyl trimethyl-ammonium bromide (DTAB/CTAB, Sigma-Aldrich Corp.) technique.22 Cytokine genotyping was carried out by the PCR sequence-specific primer method, using the ‘Cytokine Genotyping Tray’ (One Lambda Inc., Canoga Park, CA, USA), according to the manufacturer's instructions. The polymorphisms analyzed in this study were TNF-α promoter (−308 G>A), IL6 promoter (−174 G>C), IFN-γ intron 1 (+874 A>T), IL10 promoters (−1082 A>G), (−819 C>T) and (−592 C>A) and TGF-β1 codon 10 (+869 T>C) and codon 25 (+915 G>C).
Following the kit's manufacturer's suggestion and literature recommendations,23, 24, 25 cytokine genotype and phenotype were grouped as follows: for the TNF-α gene, the alleles were distributed as A/A and A/G (high) and G/G (low); for the IL-6 gene, the groups were G/G and G/C (high) and C/C (low); for the IL-10 gene, the alleles for each polymorphism were grouped as GCC/GCC (high), GCC/ATA and GCC/ACC (intermediate) and ACC/ACC and ACC/ATA (low); for the IFN-γ gene, the alleles were distributed as T/T (high), T/A (intermediate) and A/A (low); and for the TGF-β1 gene, the groups were T/T G/G and T/C G/G (high), T/C G/C and C/C G/G (intermediate) and C/C G/C, C/C C/C, T/T C/C and T/C C/C (low).
Statistical analysis
Sample size estimates were based on a reported 67% frequency of TNF-α (308G) in the general population and a 43% frequency of TNF-α (−308G) in patients with increased susceptibility to E.26 Assuming a similar difference in TNF-α (−308G) frequencies between patients and controls, a two-tailed-α of 0.05 and 80% power, a sample size of 67 per group would be sufficient to detect an association between this allele and E/PE. We selected this specific TNF-α SNP for sample size calculation as it is the most frequently assessed in PE studies.12, 13, 14, 26, 27
Hardy–Weinberg equilibrium tests were carried out by calculating the expected frequencies of each genotype and comparing them with the observed values. Arlequin software (Geneva, Switzerland) was used for these analyses.28 Single allelic and single genotype frequencies (obtained by direct count) were analyzed by Fisher's exact or χ2 tests, with the level of significance set at P⩽0.05. Odds ratios and 95% confidence intervals were calculated.
Results
The clinical characteristics of preeclamptic, eclamptic and control women are presented in Table 1.
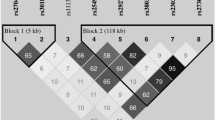
Linkage disequilibrium was detected between the three alleles of the IL10 promoter, (−1082 A>G), (−819 C>T) and (−592 C>A), and between the two alleles of TGF-β1, codon 10 (+869 T>C) and codon 25 (+915 G>C) in all patient and control groups, confirming the earlier findings.29
All SNPs in PE, E and in control patients were in Hardy–Weinberg equilibrium. Genotyping data are presented in Table 2. Among the six SNPs studied, we found no difference in genotype frequencies between the groups.
We detected a higher frequency of IFN-γ (+874 A) in eclamptic patients in comparison with that in controls. (Fisher's exact test: 70.3 vs. 57.8%, respectively; P=0.02). There were no other significant differences in allelic frequencies between eclamptic, preeclamptic and control groups (Table 3).
Discussion
We did not find an association between polymorphisms in genes, TNF-α promoter (−308 G>A), IL6 promoter (−174 G>C), IFN-γ intron 1 (+874 A>T), IL10 promoters (−1082 A>G), (−819 C>T) and (−592 C>A) and TGF-β1 codon 10 (+869 T>C) and codon 25 (+915 G>C) and E or PE.
These results are in line with other publications,12, 13, 30, 31, 32, 33 including our earlier investigation.11 In that study, we evaluated cytokine gene polymorphisms in preeclamptic and control women of three different ethnic groups, and there was a significant association between PE and IL-10 (−1082-G/G) in white women.
The significantly higher frequency of IFN-γ (+874 A) in eclamptic patients in comparison with that in controls was unexpected and could be because of chance. We did not detect a corresponding expression in genotype frequency. This finding should be interpreted with caution as it is the first time that this SNP is being investigated in patients with E. This finding needs to be further investigated.
We selected SNPs in cytokine genes that are known to influence cytokine production.23, 24 However, the protocol used to measure cytokine, the interactions between genes and environmental factors involved in the activation of these genes may also affect cytokine production. Therefore, the relationship between genotype and phenotype cannot always be clearly demonstrated.25
PE and E are considered as expressions of the same syndrome, with E being the most severe form of PE. Although other studies have investigated the relationship between PE and cytokine gene polymorphism, few have evaluated eclamptic patients. The PE syndrome is a state of excessive inflammatory response. However, both excessive Th1 (pro-inflammatory) and Th2 (anti-inflammatory) cytokine productions have been associated with PE.3, 4, 5, 34, 35 Hence, although we selected only patients with PE, we may have evaluated a heterogeneous population, including women with different cytokine and genetic profiles.
Polymorphisms in IL6, IL10, IFN-γ and TGF-β1 genes in preeclamptic patients have been investigated earlier, but most of these studies involved the analysis of SNPs in the TNF-α gene. Several polymorphisms in the promoter region of the TNF-α gene have been described. Specifically, the TNF-α −308 G>A polymorphism has been extensively evaluated because of functional significance, and discordant results have been reported.11, 12, 13, 14, 27, 36, 37, 38
Similarly, there is no consensus regarding cytokine production and PE/E. There are studies indicating a consistent increase in TNF-α production,39 others reporting that a part of these patients exhibit high TNF levels,40 whereas some investigators did not detect any change in cytokine levels.41 These discrepancies have been reported for almost all cytokines.42
These several conflicting findings could be because of heterogeneity in study designs, definition of phenotype, SNP selection, population diversity and sample size. These factors interfere with the interpretation of the results, especially in a complex disease such as PE.
Multiple mechanisms and mediators are involved in the development of PE; therefore, this disorder can be associated with more than one cytokine and with other non-cytokine genes.43, 44 Moreover, gene–gene interaction and environmental factors are likely to play a role in determining an individual's risk for a disease.29, 45, 46, 47 These interactions can be so important that they can obscure eventual associations between gene polymorphisms and the disease and lead to discordant results in different studies involving the same disorder.
To circumvent possible ethnic interference, we included only Mulatto women from a single geographical location. This is the first study that evaluates the relationship between six different cytokine polymorphisms in preeclamptic and eclamptic patients and healthy women without any obstetric or systemic disease. One of the limitations of this study is the small sample size. However, the size was sufficient to detect (with an 80% power) a possible association between cytokine gene polymorphism and E/PE, in accordance with earlier studies.26, 27, 48
These findings need to be replicated in future studies. The role of these cytokine gene SNPs in PE/E has to be further investigated, because they may be involved with etiology and not with susceptibility to disease.
Conflict of interest
The authors declare no conflict of interest.
References
Sibai BM, Dekker G, Kupferminc M . Preeclampsia. Lancet 2005; 365: 785–799.
Wasseff S . Mechanisms of convulsions in eclampsia. Med Hypotheses 2009; 72: 49–51.
Wilczyñski JR . Immunological analogy between allograft rejection, recurrent abortion and pre-eclampsia—the same basic mechanism? Hum Immunol 2006; 67: 492–511.
Saito S, Sakai M . Th1/Th2 balance in preeclampsia. J Reprod Immunol 2003; 59: 161–173.
Saito S, Shiozaki A, Nakashima A, Sakai M, Sasaki Y . The role of the immune system in preeclampsia. Mol Aspects Med 2007; 28: 192–209.
Dong M, Zhengping JH, Xie X, Wang H . Placental imbalance of Th-1 and Th-2-type cytokines in preeclampsia. Acta Obstet Gynecol Scand 2005; 84: 788–793.
Bidwell J, Keen L, Gallagher G, Kimberly R, Huizinga T, McDermott MF, Oksenberg J, McNicholl J, Pociot F, Hardt C, D’Alfonso S . Cytokine gene polymorphism in human disease: on line databases. Genes Immun 2001; 1: 3–19.
Daher S, Shulzhenko N, Morgun A, Mattar R, Rampim GF, Camano L, DeLima MG . Associations between cytokine gene polymorphisms and recurrent pregnancy loss. J Reprod Immunol 2003; 58: 69–77.
Speer EM, Gentile DA, Zeevi A, Pillage G, Huo D, Skoner DP . Role of single nucleotide polymorphisms of cytokine genes in spontaneous preterm delivery. Hum Immunol 2006; 67: 915–923.
Choi YK, Kwak-kim J . Cytokine gene polymorphisms in recurrent spontaneous abortions: a comprehensive review. Am J Reprod Immunol 2008; 60: 91–110.
Daher S, Sass N, Oliveira LG, Mattar R . Cytokine genotyping in preeclampsia. Am J Reprod Immunol 2006; 55: 130–135.
Canto-Cetina T, Canizales-Quinteros S, Méndez R, Patricia C . Analysis of C-850T and G-308A polymorphisms of the tumor necrosis factor-α gene in maya-mestizo women with preeclampsia. Hypertens Pregnancy 2007; 26: 283–291.
Stonek F, Hafner E, Metzenbauer M, Katharina S, Stümpflen I, Schneeberger C, Zeisler H, Husslein P, Philipp K . Absence of an association of tumor necrosis factor (TNF)-alpha G308A, interleukin-6 (IL-6) G174C and interleukin-10 (IL-10)G1082A polymorphism in women with preeclampsia. Am J Reprod Immunol 2008; 77: 85–90.
Mirahmadian M, Kalantar F, Heidari G, Safadarin L, Mansouri R, Amirzargar AA . Association of tumor necrosis factor-alfa and interleukin-10 gene polymorphisms in Iranian patients with pre-eclampsia. Am J Reprod Immunol 2008; 60: 179–185.
Molvarec A, Jermendy A, Kovács M, Prohászka Z, Rigó Jr J . Toll-like receptor 4 gene polymorphisms and preeclampsia: lack of association in a Caucasian population. Hypertens Res 2008; 31: 859–864.
Hassan MI, Aschner Y, Manning CH, Xu J, Aschner JL . Racial differences in selected cytokine allelic and genotypic frequencies among healthy, pregnant women in North Carolina. Cytokine 2003; 21: 10–16.
Hirashima C, Ohkuchi A, Matsubara S, Suzuki H, Takahashi K, Usui R, Suzuki M . Alteration of serum soluble endoglin levels after the onset of preeclampsia is more pronounced in women with early-onset. Hypertens Res 2008; 31: 1541–1548.
Ohkuchi A, Hirashima C, Matsubara S, Suzuki H, Takahashi K, Arai F, Watanabe T, Kario K, Suzuki M . Alterations in placental growth factor levels before and after the onset of preeclampsia are more pronounced in women with early onset severe preeclampsia. Hypertens Res 2007; 30: 151–159.
Chen YP, Pfab T, Slowinski T, Richter CM, Godes M, Hocher B . Impact of genetic variation of tumor necrosis factor-alpha on gestational hypertension. Chin Med J 2006; 119: 719–724.
Molvarec A, Vér A, Fekete A, Rosta K, Derzbach L, Derzsy Z, Karádi I, Rigó Jr J . Association between estrogen receptor alpha (ESR1) gene polymorphisms and severe preeclampsia. Hypertens Res 2007; 30: 205–211.
National High Blood pressure Education Program Working Group on High Blood Pressure in Pregnancy. Am J Obstet Gynecol 2000; 183: 1–22.
Gustincich S, Manfioletti G, Del Sal G, Schneider C, Carninci P . A fast method for high-quality genomic DNA extraction from whole human blood. Biotechniques 1991; 11: 298–300.
Hoffmann SC, Stanley EM, Darrin Cox E, Craighead N, DiMercurio BS, Koziol DE, Harlan DM, Kirk AD, Blair PJ . Association of cytokine polymorphic inheritance and in vitro cytokine production in anti-CD3/CD28 stimulated peripheral blood lymphocytes. Transplantation 2001; 72: 1444–1450.
Pravica V, Asderakis A, Perrey C, Hajeer A, Sinnott PJ, Hutchinson IV . In vitro production of IFN-γ correlates with CA repeat polymorphism in the human IFN-γ gene. Eur J Immunogenetics 1999; 26: 1–3.
Warlé MC, Farhan A, Metselaar HJ, Hop WC, Perrey C, Zondervan PE, Kap M, Kwekkeboom J, Ijzermans JN, Tilanus HW, Pravica V, Hutchinson IV, Bouma GJ . Are cytokine gene polymorphisms related to in vitro cytokine production profiles? Liver Transpl 2003; 9: 170–181.
Kaiser T, Grehan M, Brennecke SP, Moses EK . Association of the TNF2 allele with eclampsia. Gynecol Obstet Invest 2004; 57: 204–209.
Molvarec A, Jermendy A, Nagy B, Kovács M, Várkonyi T, Hupuczi P, Prohászka Z, Rigó Jr J . Association between tumor necrosis factor (TNF)-alpha G-308A gene polymorphism and preeclampsia complicated by severe fetal growth restriction. Clin Chim Acta 2008; 392: 52–57.
Excoffier L, Laval G, Schneider S . Arlequin ver. 3.0: An integrated software package for population genetics data analysis. Mol Bio Evol 2005; 1: 47–50.
Guzman VB, Yambartsev A, Goncalves-Primo A, Silva ID, Carvalho CR, Ribalta JC, Goulart LR, Shulzhenko N, Gerbase-Delima M, Morgun A . New approach reveals CD28 and IFNG gene interaction in the susceptibility to cervical cancer. Hum Mol Genet 2008; 17: 1838–1844.
Freeman DJ, McManus F, Brown EA, Cherry L, Norrie J, Ramsay JE, Clark P, Walker ID, Sattar N, Greer IA . Short-and long-term changes in plasma inflammatory markers associated with preeclampsia. Hypertension 2004; 4: 708–714.
de Groot CJ, Jansen MW, Bertina RM, Schonkeren JJ, Helmerhorst FM, Huizinga TW . Interleukin 10-2849AA genotype protects against pre-eclampsia. Genes Immun 2004; 5: 313–314.
Kamali-Sarvestani E, Kiany S, Gharesi-Fard B, Robati M . Association study of IL-10 and IFN-gamma gene polymorphisms in Iranian women with preeclampsia. J Reprod Immunol 2006; 72: 118–126.
Saarela T, Hiltunen M, Helisalmi S, Heinonen S, Laakso M . Polymorphisms of interleukin 6, hepatic lipase and calpain—10 genes, and preeclampsia. Eur J Obstet Gynecol Reprod Biol 2006; 128: 175–179.
Omu AE, Al-Azemi MK, Al-Qattan F, Al-Yatama M . Connection between human leucocyte antigens D region and T helper cytokines in preeclampsia. Arch Gynecol Obstet 2004; 269: 79–84.
Ligam P, Manuelpillai U, Wallace EM, Walker D . Localization of indoleamine 2,3-dioxygenase and kynurenine hydroxylase in the human placenta and decidua: implications for role of the kynurenine pathway in pregnancy. Placenta 2005; 26: 498–504.
Chen G, Wilson R, Wang SH, Zheng HZ, Walker JJ, McKillop JH . Tumour necrosis factor-alpha (TNF-alpha) gene polymorphism and expression in preeclampsia. Clin Exp Immunol 1996; 104: 154–159.
Heiskanen J, Romppanen E, Livonen MHS, Mannermaa A, Punnonen K, Heinonen S . Polymorphism in the tumor necrosis factor—alfa gene in women with preeclampsia. J Assist Reprod Genet 2002; 19: 220–223.
Haggerty CL, Ferrell RE, Hubel CA, Markovic N, Harger G, Ness RB . Association between allelic variants in cytokine genes and preeclampsia. Am J Obstet Gynecol 2005; 193: 209–215.
Saito S, Umekage H, Sakamoto Y, Sakai M, Tanebe K, Sasaki Y, Morikawa H . Increased T-Helper-1-type immunity and decreased T-Helper-2-type immunity in patients with preeclampsia. Am J Reprod Immunol 1999; 41: 297–306.
Meekins JW, Pijnenborg R, Hanssens M, McFadyen IR, van Asshe A . A study of placental bed spiral arteries and trophoblast invasion in normal and severe pre-eclamptic pregnancies. Br J Obstet Gynecol 1994; 101: 669–674.
Munno I, Chiechi LM, Lacedra G, Berardesca C, Patimo C, Marcuccio L, Nardelli; P, Loizzi P . Evaluation of nonspecific immunity and plasma levels of interferon-gamma, interleukin-6 and tumor necrosis factor-alpha in preeclampsia. Immunopharmacol Immunotoxicol 1999; 21: 551–564.
Jonsson Y, Matthiesen L, Berg G, Ernerudh J, Nieminen K, Ekerfelt C . Indications of an altered immune balance in preeclampsia: a decrease in vitro secretion of IL-5 and IL-10 from blood mononuclear cells and in blood basophil counts compared with normal pregnancy. J Reprod Immunol 2005; 66: 69–84.
Zafarmand MH, Franx A, Sabour S, van der Schouw YT, Grobbee DE, de Leeuw PW, Bots ML . The M235T variant of the angiotensinogen gene is related to development of self-reported hypertension during pregnancy: the Prospect-EPIC cohort study. Hypertens Res 2008; 31: 1299–1305.
Canto P, Canto-Cetina T, Juárez-Velázquez R, Rosas-Vargas H, Rangel-Villalobos H, Canizales-Quinteros S, Velázquez-Wong AC, Villarreal-Molina MT, Fernández G, Coral-Vázquez R . Methylenetetrahydrofolate reductase C677T and glutathione S-transferase P1 A313G are associated with a reduced risk of preeclampsia in Maya-Mestizo women. Hypertens Res 2008; 31: 1015–1019.
Hoffjan S, Nicolae D, Ostrovnaya I, Roberg K, Evans M, Mirel DB, Steiner L, Walker K, Shult P, Gangnon RE, Gern JE, Martinez FD, Lemanske RF, Ober C . Gene-environment interaction effects on the development of immune responses in the 1st year of life. Am J Hum Genet 2005; 76: 696–704.
Engel SA, Erichsen HC, Savitz DA, Thorp J, Chanock SJ, Olshan AF . Risk of spontaneous preterm birth is associated with common proinflammatory cytokine polymorphisms. Epidemiology 2005; 16: 469–477.
Kerk J, Dördelmann M, Bartels DB, Brinkhaus MJ, Dammann CE, Dörk T, Dammann O . Multiplex measurement of cytokine/receptor gene polymorphisms and interaction between interleukin-10 (−1082) genotype and chorioamnionitis in extreme preterm delivery. J Soc Gynecol Investig 2006; 13: 350–356.
Saarela T, Hiltunen M, Helisalmi S, Heinonen S, Laakso M . Tumour necrosis factor-alpha gene haplotype is associated with pre-eclampsia. Mol Hum Reprod 2005; 11: 437–440.
Acknowledgements
This work was supported by Fundação de Amparo à Pesquisa do Estado de Alagoas (FAPEAL).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Lima, T., Sass, N., Mattar, R. et al. Cytokine gene polymorphisms in preeclampsia and eclampsia. Hypertens Res 32, 565–569 (2009). https://doi.org/10.1038/hr.2009.58
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2009.58
Keywords
This article is cited by
-
Highlighting allelic variations at the interleukin-19 locus in term of preeclampsia predisposing factors and access to an accurate diagnostic/screening option
BMC Pregnancy and Childbirth (2023)
-
IL-27 variants might be genetic risk factors for preeclampsia: based on genetic polymorphisms, haplotypes and in silico approach
Molecular Biology Reports (2020)
-
Interleukin-23 receptor (IL-23R) gene polymorphisms and haplotypes associated with the risk of preeclampsia: evidence from cross-sectional and in silico studies
Journal of Assisted Reproduction and Genetics (2019)
-
Candidate Gene, Genome-Wide Association and Bioinformatic Studies in Pre-eclampsia: a Review
Current Hypertension Reports (2018)
-
Polymorphisms of the IL27 gene in a Chinese Han population complicated with pre-eclampsia
Scientific Reports (2016)