Abstract
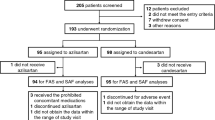
Adenosine is known as an endogenous cardioprotectant. We previously reported that plasma adenosine levels increase in patients with chronic heart failure (CHF), and that a treatment that further elevates plasma adenosine levels may improve the pathophysiology of CHF. Therefore, we performed a prospective, open-randomized clinical trial to determine whether or not exposure to dipyridamole for 1 year improves CHF pathophysiology compared with conventional treatments. The study enrolled 28 patients (mean±SEM: 66±4 years of age) attending specialized CHF outpatient clinics with New York Heart Association (NYHA) class II or III, no major complications, and stable CHF status during the most recent 6 months under fixed medications. They were randomized into three groups with or without dipyridamole (Control: n=9; 75 mg/day: n=9; 300 mg/day: n=10) in addition to their original medications and were followed up for 1 year. The other drugs were not altered. Among the enrolled patients, 100%, 4%, 100%, and 79% received angiotensin-converting enzyme inhibitors, aldosterone analogue, loop diuretics, and β-adrenoceptor blocker, respectively. Fifteen patients suffered from dilated cardiomyopathy, and 7/3/3 patients suffered from ischemic/valvular/hypertensive heart diseases, respectively. Mean blood pressure was comparable among the groups. While the baseline conditions were comparable, we found that echocardiographic ejection fraction (p<0.01 vs. baseline, p<0.01 vs. Control), left ventricular systolic diameter (p<0.05, p<0.05), Specific Activity Scale (SAS) score (p<0.05, p<0.01), maximal oxygen consumption (p<0.05, p<0.05) and plasma B-type natriuretic peptide level (p<0.01, p<0.01) were significantly improved in patients with dipyridamole after 1 year, generally in a dose-dependent manner. Therefore, we suggest that an additional administration of dipyridamole further improves CHF pathophysiology.
Similar content being viewed by others
Article PDF
References
Packer M : Evolution of the neurohormonal hypothesis to explain the progression of chronic heart failure. Eur Heart J 1995; 16 ( Suppl F): 4–6.
Vatner DE, Asai K, Iwase M, et al: Beta-adrenergic receptor-G protein-adenylyl cyclase signal transduction in the failing heart. Am J Cardiol 1999; 83: 80H–85H.
Mehra MR, Uber PA, Potluri S : Renin-angiotensin-aldosterone and adrenergic modulation in chronic heart failure: contemporary concepts. Am J Med Sci 2002; 324: 267–275.
Cicoira M, Kalra PR, Anker SD : Growth hormone resistance in chronic heart failure and its therapeutic implications. J Card Fail 2003; 9: 219–226.
Aukrust P, Gullestad L, Ueland T, Damas JK, Yndestad A : Inflammatory and anti-inflammatory cytokines in chronic heart failure: potential therapeutic implications. Ann Med 2005; 37: 74–85.
Packer M : Current role of beta-adrenergic blockers in the management of chronic heart failure. Am J Med 2001; 110 ( Suppl 7A): 81S–94S.
Yan AT, Yan RT, Liu PP : Narrative review: pharmacotherapy for chronic heart failure: evidence from recent clinical trials. Ann Intern Med 2005; 142: 132–145.
Funaya H, Kitakaze M, Node K, Minamino T, Komamura K, Hori M : Plasma adenosine levels increase in patients with chronic heart failure. Circulation 1997; 95: 1363–1365.
Hori M, Kitakaze M : Adenosine, the heart, and coronary circulation. Hypertension 1991; 18: 565–574.
Lagerkranser N, Sollevi A, Irestedt L, Tidgren B, Andreen M : Renin release during controlled hypotension with sodium nitroprusside, nitroglycerin and adenosine: a comparative study in the dog. Acta Anaesthesiol Scand 1985; 29: 45–49.
Bouma MG, Wildenberg FAJM, Buurman WA : Adenosine inhibits cytokine release and expression adhesion molecules by activated human endothelial cells. Am J Physiol 1996; 270: C522–C529.
Kitakaze M, Minamino T, Node K, et al: Elevation of plasma adenosine levels may attenuate the severity of chronic heart failure. Cardiovasc Drugs Ther 1998; 12: 307–309.
Richards AM, Lainchbury JG, Nicholls MG, Troughton RW, Yandle TG : BNP in hormone-guided treatment of heart failure. Trends Endocrinol Metab 2002; 13: 151–155.
Tsutamoto T, Wada A, Maeda K, et al: Attenuation of compensation of endogenous cardiac natriuretic peptide system in chronic heart failure: prognostic role of plasma brain natriuretic peptide concentration in patients with chronic symptomatic left ventricular dysfunction. Circulation 1997; 96: 509–516.
Omland T, Aakvaag A, Bonarjee VV, et al: Plasma brain natriuretic peptide as an indicator of left ventricular systolic function and long-term survival after acute myocardial infarction. Comparison with plasma atrial natriuretic peptide and N-terminal proatrial natriuretic peptide. Circulation 1996; 93: 1963–1969.
Koitabashi T, Inomata T, Niwano S, et al: Distinguishable optimal levels of plasma B-type natriuretic peptide in heart failure management based on complicated atrial fibrillation. Int Heart J 2005; 46: 453–464.
Berger R, Huelsman M, Strecker K, et al: B-type natriuretic peptide predicts sudden death in patients with chronic heart failure. Circulation 2002; 105: 2392–2397.
Yazaki Y, Muhlestein JB, Carlquist JF, et al: A common variant of the AMPD1 gene predicts improved survival in patients with ischemic left ventricular dysfunction. J Card Fail 2004; 10: 316–320.
Loh E, Rebbeck TR, Mahoney PD, DeNofrio D, Swain JL, Holmes EW : Common variant in AMPD1 gene predicts improved clinical outcome in patients with heart failure. Circulation 1999; 99: 1422–1425.
Kalsi KK, Yuen AH, Rybakowska IM, et al: Decreased cardiac activity of AMP deaminase in subjects with the AMPD1 mutation—a potential mechanism of protection in heart failure. Cardiovasc Res 2003; 59: 678–684.
Liao Y, Takashima S, Asano Y, et al: Activation of adenosine A1 receptor attenuates cardiac hypertrophy and prevents heart failure in murine left ventricular pressure-overload model. Circ Res 2003; 93: 759–766.
Zhang Q, Moalem J, Tse J, Scholz PM, Weiss HR : Effects of natriuretic peptides on ventricular myocyte contraction and role of cyclic GMP signaling. Eur J Pharmacol 2005; 510: 209–215.
Imaizumi S, Miura S, Nishikawa H, et al: Angiotensin II type 1 receptor blockers do not promote coronary collateral circulation in patients with coronary artery disease. Hypertens Res 2006; 29: 135–141.
Laghi-Pasini F, Guideri F, Petersen C, et al: Blunted increase in plasma adenosine levels following dipyridamole stress in dilated cardiomyopathy patients. J Intern Med 2003; 254: 591–596.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sanada, S., Asanuma, H., Koretsune, Y. et al. Long-Term Oral Administration of Dipyridamole Improves Both Cardiac and Physical Status in Patients with Mild to Moderate Chronic Heart Failure: A Prospective Open-Randomized Study. Hypertens Res 30, 913–919 (2007). https://doi.org/10.1291/hypres.30.913
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.30.913
Keywords
This article is cited by
-
Why Not Dipyridamole: a Review of Current Guidelines and Re-evaluation of Utility in the Modern Era
Cardiovascular Drugs and Therapy (2022)
-
Cardiac purinergic signalling in health and disease
Purinergic Signalling (2015)
-
Role of Antithrombotic Agents in Heart Failure
Current Cardiology Reports (2012)