Abstract
Purpose To assess whether the issuing of local guidelines for glaucoma detection including a protocol for the referral of suspects can improve the quality and accuracy of referrals from optometrists.
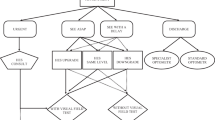
Methods Universally agreed guidelines, which included a protocol for referring glaucoma suspects, were circulated to all optometrists in the catchment area of a major teaching hospital ophthalmic unit. Data on 207 new patients referred to one glaucoma clinic were collected from GOS18 forms and hospital records covering two 12 month periods spanning the guideline dissemination. Referral accuracy was calculated and the reasons for protocol violations and referral of normal individuals were determined. Where possible, data were compared with a similar study relating to referrals made to the same clinic in 1988 and 1993.
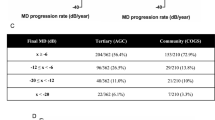
Results The mean (SD) intraocular pressure (IOP) at which optometrists referred patients was 22.5 (6.6) in 1997 and 21.9 mmHg (6.6) in 1998/9, both significantly less than in 1988. A statistically significant upward trend with time was found in the number of patients referred with an assessment of cup/disc ratio and in those with details of a visual field assessment. The overall ‘true positive diagnosis’ was 40% (42/105) in 1997 and 32.3% (33/102) in 1998/9 after the guidelines (p = 0.32), both of which were significantly lower than the 1988 rate of 56% (34/75) (p = 0.03 and 0.003). Fifty per cent of false positive referrals in both 1997 and 1998/9 were associated with an assessment by the optometrist of the optic disc(s) that was at variance with the ophthalmologist's. False positive visual fields were associated with 22% and 35% of non-true positive referrals in 1997 and 1998/9. Protocol violations were observed in 48% of referrals after the guidelines had been disseminated. When the referral was both a false positive and the guideline protocol was not followed, 88% of violations were associated with IOP measurement in 1997 and 73% in 1998/9. The equivalent figures for visual field violations were 70% in 1997 and 76% in 1998/9. Normal individuals referred as suspects were significantly (p = 0.001) less likely to be referred on IOP grounds if their optometrist followed the referral protocol.
Conclusion Local dissemination of glaucoma screening guidelines with a protocol for referral did not appear to improve the diagnostic accuracy of optometrists in our area Optometrists who follow the guidelines refer fewer normal individuals on IOP grounds, but false positive visual fields and optic disc interpretation difficulties remain a factor in such referrals. Additional strategies will be necessary to improve the quality and accuracy of referrals for suspect glaucoma by optometrists.
Similar content being viewed by others
Article PDF
References
Harrison RJ, Wild JM, Hobley AJ . Referral patterns to an ophthalmic outpatient clinic by general practitioners and ophthalmic optometrists and the role of these professionals screening for ocular disease. BMJ 1988;297:1162–7.
Vernon SA . The changing pattern of glaucoma referrals by optometrists. Eye 1998;12:854–7.
Sheldrick JH, Ng C, Austin DJ, et al. An analysis of referral routes and diagnostic accuracy in cases of suspected glaucoma. Ophthalmic Epidemiol 1994;1:31–9.
Newman DK, Anwar S, Jordan K . Glaucoma screening by optometrists: positive predictive value of visual field testing. Eye 1998;12:921–4.
Brittain GPH, Austin DJ, Kelly SP . A prospective survey to determine sources and diagnostic accuracy of glaucoma referrals. Health Trends 1988;20:43–4.
Tuck M, Crick RP . Efficacy of referral for suspected glaucoma. BMJ 1991;302:998–1000.
The routine eye examination. Guideline advice on best practice. London: College of Optometrists, 1997.
Vernon SA, Henry DJ . Do optometrists screen for glaucoma? Eye 1989;3:131–4.
Clearkin L, Harcourt B . Referral pattern of true and suspected glaucoma to an adult ophthalmic outpatient clinic. Trans Ophthalmol Soc UK 1983;103:284–7.
Strong NP . How optometrists screen for glaucoma: a survey. Ophthalmic. Physiol Optics 1992;12:3–7.
Tuck WM, Crick RP . Use of visual field tests in glaucoma detection by optometrists in England and Wales. Ophthalmic Physiol Optics 1994;14:227–31.
Vernon SA . Intraeye pressure range and pulse profiles in normals with the Pulsair Noncontact Tonometer. Eye 1993;7:134–7.
Vernon SA . Reproducibility with the Keeler Pulsair 2000 noncontact tonometer. Br J Ophthalmol 1995;79:544–7.
Vernon SA, Henry DJ, Cater L, et al. Screening for glaucoma in the community by non-ophthalmically trained staff using semi-automated equipment. Eye 1990;4:89–97.
Harper R, Reeves B, Smith G . Observer variability in optic disc assessment: implications for glaucoma shared care. Ophthalmic Physiol Opt 2000;20:265–73.
Tuck MW, Crick RP . The cost-effectiveness of various modes of screening for primary open angle glaucoma. Ophthal Epidemiol 1997;4:3–17.
Vernon SA . Shared care in glaucoma. Glaucoma Forum, spring 2000, issue 5 12-13. London: IGA.
Author information
Authors and Affiliations
Corresponding author
Additional information
Presented in part to the 1999 meeting of the UK and Eire Glaucoma Society and at the 2000 Annual Congress of the Royal College of Ophthalmologists, Harrogate
Proprietary interests: None
Grant support: None
Rights and permissions
About this article
Cite this article
Vernon, S., Ghosh, G. Do locally agreed guidelines for optometrists concerning the referral of glaucoma suspects influence referral practice?. Eye 15, 458–463 (2001). https://doi.org/10.1038/eye.2001.155
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/eye.2001.155
Keywords
This article is cited by
-
Outcomes of newly referred patients with suspected angle closure: do we need to redefine the clinical pathways?
Eye (2024)
-
Referrals from community optometrists to the hospital eye service in Scotland and England
Eye (2022)
-
Care pathways for glaucoma detection and monitoring in the UK
Eye (2020)
-
The Portsmouth-based glaucoma refinement scheme: a role for virtual clinics in the future?
Eye (2012)
-
Patterns of adherence to NICE Glaucoma Guidance in two different service delivery models
Eye (2012)