Abstract
Aim:
To develop a population pharmacokinetic (PopPK) model of tacrolimus in healthy Chinese volunteers and liver transplant recipients for investigating the difference between the populations, and for potential individualized medication.
Methods:
A set of 1100 sparse trough concentration data points from 112 orthotopic liver transplant recipients, as well as 851 dense data points from 40 healthy volunteers receiving a single dose of tacrolimus (2 mg, po) were collected. PopPK model of tacrolimus was constructed using the program NONMEM. Related covariates such as age, hepatic and renal functions that were potentially associated with tacrolimus disposition were evaluated. The final model was validated using bootstrapping and a visual predictive check.
Results:
A two-compartment model of tacrolimus could best describe the data from the two populations. The final model including two covariates, population (liver transplant recipients or volunteers) and serum ALT (alanine aminotransferase) level, was verified and adequately described the pharmacokinetic characteristics of tacrolimus. The estimates of V2/F, Q/F and V3/F were 22.7 L, 76.3 L/h and 916 L, respectively. The estimated CL/F in the volunteers and liver transplant recipients was 32.8 and 18.4 L/h, respectively. Serum ALT level was inversely related to CL/F, whereas age did not influence CL/F. Thus, the elderly (≥65 years) and adult (<65 years) groups in the liver transplant recipients showed no significant difference in the clearance of tacrolimus.
Conclusion:
Compared with using the sparse data only, the integrating modeling technique combining sparse data from the patients and dense data from the healthy volunteers improved the PopPK analysis of tacrolimus.
Similar content being viewed by others
Introduction
Liver transplant (LT)1 technology was initiated in the 1950s and was primarily performed in the patients with end-stage liver disease caused by a variety of liver diseases, such as hepatocellular carcinoma (HCC), liver cirrhosis, chronic severe hepatitis, biliary atresia (which was common in children), and congenital metabolic diseases. HCC accounts for approximately 40% of the liver transplantation surgeries. The liver transplant is the only effective radical cure for all types of end-stage liver diseases and provides new technology, new ideas and new hope for patients. Meanwhile, immunosuppressants are the main preventive and treatment measures for organ transplant rejections. The appropriate use of immunosuppressants is directly related to the survival of the liver transplant recipients.
After liver transplantation, a triple immunosuppressive regimen2 centered on tacrolimus is usually adopted. Tacrolimus (Prograf®, FK506) is a potent macrocycliclactone immune inhibitor3,4 that was isolated from the soil by the Fujisawa Pharmaceutical Company in 1984. It is widely used to prevent immune rejection caused by the liver, pancreas, kidneys, heart, lungs and other solid organ transplantations and to treat some autoimmune diseases2,5,6,7,8,9,10. Tacrolimus has a clear First pass effect and incomplete oral absorption in the gastrointestinal tract, with an absolute oral bioavailability of 10%–17% in adult kidney transplant patients, 6%–22% in adult liver transplant patients and 5%–18% in healthy subjects11,12. Its binding rate with protein is approximately 99%, primarily binding with α1-acid glycoprotein and albumin, and it has a high affinity with red blood cells13,14.
Tacrolimus is widely metabolized by a variety of mixed function oxidases15,16, primarily the cytochrome P450 3A enzymes (CYP3A4 or CYP3A5) of the liver and intestine. It is biotransformed through demethylation and hydroxylation, with a primary metabolite of 13-demethyl tacrolimus. Tacrolimus is excreted at 30.7%–92.6% and 1.10%–2.30% from the bile and urine, respectively.
The therapeutic window of tacrolimus is relatively narrow and has a significant individual variability17,18 in its pharmacokinetics and toxicology. Too high of a trough concentration can lead to side effects19,20, and too low of a concentration may result in rejection21. Thus, it is particularly important to develop an individualized immunosuppressive therapy regimen through therapeutic drug monitoring. Although monitoring blood concentrations is an effective way to regulate the immunosuppressant dosages, clinical studies have found large differences in the desired dosages among different individuals to achieve and maintain the same immune inhibitor concentration22. Currently, immunosuppressive effects are empirically assessed by monitoring the whole blood trough concentration and the indexes of liver and kidney function. Thus, a certain amount of uncertainty exists in using immunosuppressant medications.
In recent years, compared with a large number of reports about the population pharmacokinetics (PopPK) of tacrolimus in other countries23,24,25,26,27, reports in China are still limited. The published research has focused on liver and kidney transplantation, and the majority of studies were performed in renal transplant patients, motivating us to perform this PopPK study in liver transplant patients. Moreover, PopPK studies of tacrolimus have usually been conducted in healthy subjects and patients of adult or children, but relevant studies of tacrolimus in the elderly have been rare. As a result, it is important to discover the disposition characteristics of tacrolimus in elderly liver transplant patients.
In this study, we retrospectively collected routinely monitored tacrolimus trough blood concentrations from 112 orthotopic liver transplant patients during their early postoperative days, as well as the rich concentration data from 40 healthy volunteers. These data were used to develop a PopPK model and explore the key covariates that affect the PK of tacrolimus. This study may potentially individualize therapy in Chinese liver transplant recipients, particularly for elderly patients. We also developed an integrative modeling strategy by combing the sparse data from patients and the rich data from healthy volunteers. We hypothesized that our method may facilitate a better understanding of the pharmacokinetic profiles of tacrolimus and other medicines for which only sparse data are available from patients.
Materials and methods
One hundred and twelve liver transplant patients receiving allograft orthotopic liver transplantation for the first time were enrolled from March 2004 to August 2012 in the Organ Transplant Center of the General Hospital of the Armed Police Forces. Forty healthy volunteers were from the PLA Second Artillery General Hospital. All subjects including liver transplant recipients and healthy volunteers provided informed consent, and all treatment was performed in accordance with the ethical standards of the Declaration of Helsinki and approved by the Hospital Ethics Committee.
The inclusion criteria for liver transplant patients were as follows: 1) no major existing primary diseases in preoperative days and a good recovery in postoperative period; 2) no serious complications during the surgery; 3) did not take any food or medicine, which may potentially affect the pharmacokinetics of tacrolimus; and 4) survived more than one year. The exclusion criteria for liver transplant patients included subjects with a rejection reaction, a primary graft failure or severe complications, such as an infection or even death after transplantation. All of the healthy volunteers in this study were male, and all of their examinations were normal.
The individual information for each subject was carefully recorded, including gender, age, body weight (BW), white blood cells (WBC), hemoglobin (HGB), hematocrit (HCT), platelet (PLT), alanine aminotransferase (ALT), aspartate aminotransferase (AST), and total bilirubin (TBIL). If the subjects were healthy volunteers, the value of the SubPop was 0; otherwise, the value was 1.
Drugs and software
Tacrolimus (Prograf®, FK506) capsules 0.5 mg or 1 mg (Astellas Pharma China, Inc), mycophenolate mofetil (MMF) dispersible tablets 0.25 g, (Hangzhou ZhongMeiHua Co, China), methylprednisolone injection 40 mg/bottle or 500 mg/bottle (Pfizer), and methylprednisolone tablet 4 mg (Tianjin TianYao Pharmaceuticals) were used. NONMEM Software: Version 7.2 (ICON, MD, USA), Perl-speaks-NONMEM (PsN, version 3.4.2) and R 2.15.3 (R-project.org) were used.
Dosage regimen
All liver transplant recipients were given 500–1000 mg of a methylprednisolone injection during surgery. Patients initiated a triple immunosuppressive regimen of FK506, MMF and corticosteroids on the day following the surgery. The drugs were initially administered by nasal feeding and were gradually replaced by oral administration. The initial dose of tacrolimus was 0.05 mg·kg−1·d−1 (twice daily). The dose was adjusted when necessary based on the results of therapeutic drug monitoring (TDM), biochemical parameters and physical conditions. The MMF dispersible tablets were administered as 750 mg bid after meals from the following day after surgery. A methylprednisolone injection was given simultaneously at a dose of 80 mg and was gradually decreased to 20 mg/d at a rate of 20 mg/d. Finally, oral methylprednisolone tablets were given at 16 mg/d to replace the injections and were gradually decreased to 4 mg/d at a rate of 4 mg/d. All healthy volunteers were given a single dose of tacrolimus (2 mg orally) in a randomized, two-formulation, double-cycle, cross-over design experiment.
Blood sample collecting and analysis
A peripheral venous blood sample (1–2 mL) was collected from the liver transplant recipients before taking tacrolimus on the morning of their third day after surgery. The samples were measured using a monoclonal antibody-based microparticle enzyme immunoassay (MEIA). The calibration curve was linear over a range of 1.5–30 μg/L, and the accuracy and precision met the requirements. For healthy volunteers, whole blood samples were intensively drawn at 0 h prior to drug administration and 0.5, 1, 1.5, 2, 3, 4, 6, 12, 24, 48, and 72 h after drug administration. The concentrations of tacrolimus in these samples were determined using HPLC-MS. The assay was assessed to be linear over the range of 0.1–25 μg/L, and the accuracy and precision met the requirements28.
Population pharmacokinetic model development
First-order conditional estimation with interaction (FOCEI) estimation29,30,31 of the NONMEM (ADVAN4 module) was used to develop the model. Both a one- and two-compartment model with first-order absorption were used to describe our data. The random effects of the population pharmacokinetic study were composed of inter-individual variability and residual random effects. Random effects between individuals are expressed exponentially or additively, whereas residual random effects refer to the difference between the observed values and the predicted ones caused by unknown factors and are expressed additively, proportionally, or by a combination of the two. The volume of distribution in the peripheral compartment (V3/F) was fixed as the estimate from the healthy Chinese volunteer group.
Covariates were investigated based on diagnostic plots and the value of the objective function (OFV). When introducing a covariate into the model, if the change in the OFV (ΔOFV) was greater than 3.84, the factor was indicated to significantly improve the model (P<0.05) and thus be included. All of the covariates were introduced individually to examine their effects on the model. At the end, all of the factors that significantly impacted the model were retained, and the full model was established.
The effect of the covariates in the full model was further evaluated using more stringent criteria (ΔOFV>7.88, P<0.005). The covariates were excluded from the full regression model one by one to confirm their significance in the model. An increase of more than 7.88 in OFV indicated that the factor had a significant effect on the model and should thus be retained in the model; otherwise, the factor should be excluded from the model. The final model was eventually developed after excluding the unnecessary covariates.
In this study, the continuous covariates were included by using Eqs 1 or 2:


where i, Pi, θTV [or θ*EXP(θcov)] and θcov were the individual's ID, individual parameter, typical value of the corresponding parameter and the correlation coefficient for the relevant covariate, respectively.
For the categorical covariates, such as gender and SubPop, they were evaluated using Eq 3:

where θ was the estimate of the parameter for the reference group. θcov describes the effect contributed by the other group.
Eventually, the robustness, reliability and prediction performance of the final model were evaluated by bootstrapping and a visual predictive check (VPC). Through the bootstrap analysis, resampling was performed 1000 times. The median and 95% confidence interval of the parameters were obtained and compared with the estimates of the final model from the NONMEM. For the VPC, the concentration vs the time curve of tacrolimus was simulated 1000 times using the final model. Consequently, the median and 90th percentile interval of the simulation were graphically compared with the observed values to evaluate the model's predictive performance.
Results
A total of 1100 routinely monitored tacrolimus whole blood trough concentration data were retrospectively collected from 112 liver transplant patients, in which 36 patients were older than 65 years. A total of 851 tacrolimus whole blood concentration data were collected from 40 healthy Chinese male volunteers in a bioequivalent study. The demographic and biological characteristics of the two populations in this study are summarized in Table 1.
A two-compartment model with first-order absorption described our data better. The inter-individual variability was evaluated exponentially, and the residual error was estimated proportionally. The parameter estimates obtained using NONMEM are shown in Table 2.
The regression equations of the population pharmacokinetic base model of tacrolimus follow below.






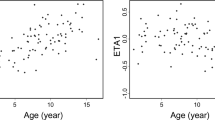
All of the covariates listed in Table 1 were investigated in this study. The results of stepwise forward addition and backward elimination are shown in Table 3. The SubPop and ALT were found to significantly improve the fitting of our model and were included. The effect of other covariates was also evaluated on the base model, including age, gender, BW, HGB, HCT, and TBIL on the parameter of apparent clearance (CL/F), but no significant improvement was observed. The estimates of the final model are listed in Table 2, and the basic goodness-of-fit plots are shown in Figure 1. The typical values of the volume of distribution in the central compartment (V2/F), the inter-compartmental clearance (Q/F), the volume of distribution in peripheral compartment (V3/F), the constant of absorption (Kα) and the time lag (ALAG1) derived from the final model were 22.7 L, 76.3 L/h, 916 L, 0.419 h−1 and 0.404 h, respectively. Unsurprisingly, the estimate of CL/F was different between the groups, with values of 32.8 L/h (healthy volunteers) and 18.4 L/h (patients). ALT was inversely related to CL/F in the patient group. In Figure 1, the plots of observations vs population predictions and observations vs individual predictions show a symmetric distribution around the identity line. The conditional weighted residuals (CWRES) vs the predictions plot suggested an appropriate error model. The CWRES distributed evenly around the zero line.
Basic goodness-of-fit plots of the final model. The grey circles represent observations from healthy volunteers and the black dots represent observations from liver transplant subjects. (A) The plot of observations (LNDV, natural log of data) vs population predictions. (B) The plot of observations (LNDV) vs individual predictions. (C) The plot of conditional weighted residuals (CWRES) vs predictions. (D) The plots of conditional weighted residuals (CWRES) vs time. The solid lines in A and B are identity lines. The solid lines in C and D are zero lines. The dashed lines represent regression lines by using locally-weighted polynomial regression. DV, PRED, and IPRED values had been log-transformed.
The regression equations of the final model were obtained after backward elimination as follows:






The robustness of the final model was validated using a bootstrap method. The percentage of successful minimizations and covariance was 81.9%. The median and 95% CI of the parameters from the bootstrap analysis were in good agreement with the estimates from the final model obtained using NONMEM (Table 2). The graphical results of VPC are presented in Figure 2, which shows the predictive property of the model was good with most of the observation points falling in the 90% prediction interval. Because there were limited observations after approximately 1500 h, the VPC plot of the liver transplant patients was cut off at 1500 h.
Visual predictive check (VPC) for the final model. Circles are the observations. The solid line represents the medians of the simulation values, the shaded area represents the 90% predictive interval. (A) The VPC plot for the healthy Chinese volunteers; (B) The VPC plot for the liver transplant patients (time <1500 h).
Discussion
China has one of the highest incidences of end-stage liver disease across countries, and new cases of hepatic cancers account for approximately 55% of all cases worldwide. Many people died of various types of liver disease such as liver cirrhosis and hepatic cancer. Male accounted for 76.79%, and female accounted for 23.21% of the 112 cases of orthotropic liver transplant patients in this study. Primary hepatic cancer, liver cirrhosis and chronic severe hepatitis, hepatic cancer recurrence after resection or interventional treatment, and alcoholic cirrhosis in this study accounted for 50.9%, 30.6%, 6.48%, 4.63%, and 2.70% of the diseases in this study, respectively, whereas the other liver diseases accounted for less than 5%. Primary hepatic cancer accounted for half of these cases, and liver transplantation is the only effective method to treat hepatic cancer and other end-stage liver diseases. Thus, early diagnosis and early treatment for hepatic cancer are particularly important.
Tacrolimus is metabolized in the liver and primarily excreted by bile. Renal tacrolimus clearance only accounted for 1.1%–2.3%. Therefore, the status of the patient's liver and biliary tract plays a very important role on its pharmacokinetics. Of the seven biochemical factors in the patient group (Table 1), only WBC and PLT remained in the normal range within the early postoperative period, whereas HGB and HCT were lower and the rest of the values were higher than normal. In previous studies, covariates including HCT, ALT (or AST) were added to the final model32,33,34. In this study, ALT was added to the model and showed a significant influence on the elimination of tacrolimus for the liver transplant patient group. No influence of ALT on CL/F was included in the final model for the healthy volunteer group because no evident relationship between them was observed based on graphic evaluation. HCT was also evaluated in the model, but it was not significantly influential. Moreover, POD was excluded from our model because of its high correlation with the hepatic biochemical parameters (ALT in our model).
Most of the previously reported population pharmacokinetic models of tacrolimus for the transplant patients were one-compartment models26,35,36,37. Limited by the sparse data from this population, the reliability, prediction performance and robustness in these models could hardly be expected to be high. Tacrolimus is a fat-soluble drug and can easily distribute to the peripheral compartment. Therefore, a two-compartment model (as demonstrated in this study) was more reasonable to describe tacrolimus pharmacokinetic behavior. The volume of distribution in the peripheral compartment for tacrolimus between the healthy volunteers and the liver transplant patients can be reasonably assumed to be similar based on previous publications38,39,40. A two-compartment model of tacrolimus was developed by combining the dense data from the healthy volunteers and the sparse data from the liver transplant patients, which allowed us to capture more information on pharmacokinetic behaviors, especially in the patients.
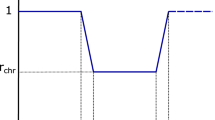
Nearly one-third of the subjects from this liver transplant population were over 65 years old. As a covariate, age showed a non-significant effect on CL/F in the liver transplant patient population. CL/F from the elderly (≥65 years) and adult patient (<65 years) groups in the final model are compared in Figure 3. No significant difference exists between the elderly and adult groups for tacrolimus pharmacokinetics among liver transplant patients. Compared with other studies, the model developed may be more representative, relatively stable and suitable for a wider population range of liver transplant patients.
The comparison between the adult (<65 yr) and elderly (≥65 yr) patient groups in apparent clearance (CL/F).
In conclusion, we developed a PopPK model of tacrolimus, in which we retrospectively collected trough concentrations from 112 orthotopic liver transplantation patients and rich concentration data from 40 healthy volunteers. The pharmacokinetics of tacrolimus between the healthy subjects and the liver transplant patients were revealed to be different in CL/F, whereas the pharmacokinetics between the elderly and adult patient groups was shown to be similar within the patient population. More importantly, compared with using the sparse data only, the integrating modeling technique combining sparse data from the patients and rich data from the healthy volunteers improved the PopPK analysis of tacrolimus. This method could be potentially expanded to other similar medications that could only be sparsely monitored in the clinic.
Author contribution
Wei LU, Yan-xia LU, and Qing-hong SU designed the research and wrote the paper; Qing-hong SU, Ke-hua WU, and Yu-peng REN analyzed data and plotted figures; Liang LI and Tian-yan ZHOU provided technical assistance.
References
Walia A, Schumann R . The evolution of liver transplantation practices. Curr Opin Organ Transplant 2008; 13: 275–9.
Shapiro R . Low toxicity immunosuppressive protocols in renal transplantation. Keio J Med 2004; 53: 18–22.
Goto T, Kino T, Hatanaka H, Okuhara M, Kohsaka M, Aoki H, et al. Tacrolimus: historical perspectives. Transplant Proc 1991; 23: 2713–7.
Kelly PA, Burckart GJ, Venkataramanan R . Tacrolimus: a new immunosuppressive agent. Am J Health Syst Pharm 1995; 52: 1521–35.
Fung JJ, Starzl TE . FK506 in solid organ transplantation. Ther Drug Monit 1995; 17: 592–5.
Spada M, Corno V, Colledan M, Segalin A, Lucianetti A, Torre G, et al. Rejection and tacrolimus conversion therapy in pediatric liver transplantation. Transpl Int 2000; 13: S341–4.
VanHooff JP, Christiaans MH . Use of tacrolimus in renal transplantation. Transplant Proc 1999; 31: 3298–9.
Crespo-Leiro MG . Tacrolimus in heart transplantation. Transplant Proc 2003; 35: 1981–3.
Espinosa M, Rodi R, Goikoetxea MJ, Zulueta J, Seijo LM . Lung Transplant. An Sist Sanit Navar 2006; 29: Suppl 2N: 105–12.
Lam VW, Pleass HC, Hawthorne W, Allen RD . Evolution of pancreas transplant sur-gery. ANZ J Surg 2010; 80: 411–8.
Neuhaus P, Blumhardt G, Bechstein WO . Comparison of FK506 and cyclosporine-based immuno suppression. In primary orthotopic liver transplantation. A single center experience. Transplantation 1995; 59: 31–40.
Flanagan WM, Corthésy B, Bram RJ, Crabtree GR . Nuclear association of a T-cell transcription factor blocked by FK506 and cyclosporin A. Nature 1991; 352: 803–7.
Nagase K, Iwasaki K, Nozaki K, Noda K . Distribution and protein binding of FK506, a potent immunosuppressive macrolide lactone in human blood and its uptake by erythrocytes. J Pharm Pharmacol 1994; 46: 113–7.
Zahir H, Nand RA, Brown KF, Tattam BN, McLachlan AJ . Validation of methods to study the distribution and protein binding of tacrolimus in human blood. J Pharmacol Toxicol Methods 2001; 46: 27–35.
Sattler M, Guengerich FP, Yun CH . Cytochrome P-450 3A enzymes are responsible for biotransformation of FK506 and rapamycin in man and rat. Drug Metab Dispos 1992; 20: 753–61.
Alak AM, Cook M, Bekersky I . Measurement of tacrolimus (FK506) and its metabolites: a review of assay development and application in therapeutic drug monitoring and pharmacokinetic studies. Ther Drug Monit 1997; 19: 338–51.
Ihara H, Shinkuma D, Ichikawa Y, Nojima M, Nagano S, Ikoma F . Intra- and inter-individual variation in the pharmacokinetics of tacrolimus (FK506) in kidney transplant recipients–importance of trough level as a practical indicator. Int J Urol 1995; 2: 151–5.
Yasuda SU, Zhang L, Huang SM . The role of ethnicity in variability in response to drugs: focus on clinical pharmacology studies. Clin Pharmacol Ther 2008; 84: 417–23.
Shaw LM, Kaplan B, Kaufman D . Toxic effects of immunosuppressive drugs: mechanisms and strategies for controlling them. Clin Chem 1996; 42: Pt 2: 1316–21.
Ishikawa M, Abo K, Nanba A, Satoh S, Mikawa Y, Higashi T, et al. Blood concentrations and side effects of tacrolimus in a living renal transplantation. Masui 2001; 50: 246–50.
Encke J, Uhl W, Stremmel W, Sauer P . Immunosuppression and modulation in liver transplantation. Nephrol Dial Transplant 2004; 19: iv22–5.
Venkataramanan R, Swaminathan A, Prasad T, Jain A, Zuckerman S, Warty V, et al. Clinical pharmacokinetics of tacrolimus. Clin Pharmacokinet 1995; 29: 404–30.
Antignac M, Barrou B, Farinotti R, Lechat P, Urien S . Population pharmacokinetics and bioavailability of tacrolimus in kidney transplant patients. Br J Clin Pharmacol 2007; 64: 750–7.
Zhao W, Fakhoury M, Baudouin V, Storme T, Maisin A, Deschenes G . Population pharmacokinetics and pharmacogenetics of once daily prolonged-release formulation of tacrolimus in pediatric and adolescent kidney transplant recipients. Eur J Clin Pharmacol 2013; 69: 189–95.
Zuo XC, Ng CM, Barrett JS, Luo AJ, Zhang BK, Deng CH, et al. Effects of CYP3A4 and CYP3A5 polymorphisms on tacrolimus pharmacokinetics in Chinese adult renal trans-plant recipients: a population pharmacokinetic analysis. Pharmacogenet Genomics 2013; 23: 251–61.
Antignac M, Hulot JS, Boleslawski E, Hannoun L, Touitou Y, Farinotti R . Population pharmacokinetics of tacrolimus in full liver transplant patients: modelling of the post-operative clearance. Eur J Clin Pharmacol 2005; 61: 409–16.
Suzuki Y, Homma M, Doki K, Itagaki F, Kohda Y . Impact of CYP3A5 genetic polymorphism on pharmacokinetics of tacrolimus in healthy Japanese subjects. Br J Clin Pharmacol 2008; 66: 154–5.
Li PF, Liu LH, Ma P . LC-MS/MS determination of tacrolimus in human blood and application in its bioequivalence study. Chin J Pharm Anal 2009; 29: 237–42. Chinese.
Beal S, Sheiner L, Boeckmann A . NONMEM user's guide. San Francisco: Division of Pharmacology, University of California; 1999.
Lars L, Jakob R, Jonsson EN . Perl-speaks-NONMEM (PsN)–a Perl module for NONMEM related programming. Comput Methods Programs Biomed 2004; 75: 85–94.
Jonsson E, Karlsson M . Xpose-an S-PLUS based population pharmacokinetic pharmacodynamics model building aid for NONMEM. Comput Methods Programs Biomed 1998; 58: 51–64.
Guy-Viterbo V, Scohy A, Verbeeck RK, Reding R, Wallemacq P, Musuamba FT . Population pharmacokinetic analysis of tacrolimus in the first year after pediatric liver transplantation. Eur J Clin Pharmacol 2013; 69: 1533–42.
Fukudo M, Yano I, Masuda S, Goto M, Uesugi M, Katsura T, et al. Population pharmacokinetic and pharmacogenomic analysis of tacrolimus in pediatric living-donor liver transplant recipients. Clin Pharmacol Ther 2006; 80: 331–45.
Staatz CE, Taylor PJ, Lynch SV, Willis C, Charles BG, Tett SE . Population pharmacokinetics of tacrolimus in children who receive cut-down or full liver transplants. Transplantation 2001; 72: 1056–61.
Zhang GM, Li L, Chen WQ, Bi SS, Liu X, Zhang XL . Population pharmacokinetics of tacrolimus in Chinese renal transplant patients. Acta Pharm Sin 2008; 43: 695–701.
Antignac M, Barrou B, Farinotti R, Lechat P, Urien S . Population pharmacokinetics and bioavailability of tacrolimus in kidney transplant patients. Br J Clin Pharmacol 2007; 64: 750–7.
Fukatsu S, Yano I, Igarashi T, Hashida T, Takayanagi K, Saito H . Population pharmacokinetics of tacrolimus in adult recipients receiving living-donor liver trans-plantation. Eur J Clin Pharmacol 2001; 57: 479–84.
Zhu L, Wang H, Sun X, Rao W, Qu W, Zhang Y, et al. The population pharmacokinetic models of tacrolimus in Chinese adult liver transplantation patients. J Pharm 2014. doi:10.1155/2014/713650
Qiu XH, Zhang Y, Shen ZY, Rui JZ, Li JH . Population pharmacokinetics of tacrolimus in 22 Chinese recipients of liver transplantation. J Med Postgrad 2008; 21: 915–9. Chinese.
Xue L, Zhang H, Ma S, Rui JZ, Miao LY . Population pharmacokinetics and pharmacogenetics of tacrolimus in healthy Chinese volunteers. Pharmacology 2011; 88: 288–94.
Acknowledgements
We thank Li CHEN and Xiao-ping YAN for collecting data for this study. We also thank doctor Yang YANG and nurse Li-yan FEN for providing advice for the liver transplantation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lu, Yx., Su, Qh., Wu, Kh. et al. A population pharmacokinetic study of tacrolimus in healthy Chinese volunteers and liver transplant patients. Acta Pharmacol Sin 36, 281–288 (2015). https://doi.org/10.1038/aps.2014.110
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2014.110
Keywords
This article is cited by
-
Population pharmacokinetic analyses of tacrolimus in non-transplant patients: a systematic review
European Journal of Clinical Pharmacology (2023)
-
Population Pharmacokinetic Analysis for Model-Based Therapeutic Drug Monitoring of Tacrolimus in Chinese Han Heart Transplant Patients
European Journal of Drug Metabolism and Pharmacokinetics (2023)
-
Physiologically based pharmacokinetic model combined with reverse dose method to study the nephrotoxic tolerance dose of tacrolimus
Archives of Toxicology (2023)
-
Clinical utility of ABCB1 single nucleotide polymorphism on tacrolimus dose requirements in Egyptian liver transplant patients
Egyptian Liver Journal (2021)
-
Effects of red blood cell concentrate transfusion on blood tacrolimus concentration
International Journal of Clinical Pharmacy (2020)