Abstract
Aim:
Previous studies have shown that D(+)β-3,4-dihydroxyphenyl lactic acid (salvianic acid A, SAA) has anabolic effects on prednisone (GC)-induced osteoporosis in rats. The current study aims to investigate the molecular mechanism of SAA's impact on osteogenesis and adipogenesis in bone marrow stromal cells in intact and GC-treated rats.
Methods:
For in vitro study, newborn rat calvaria osteoblasts (rOBs) and rat bone marrow stromal cells (rMSCs) were isolated, identified and cultured with SAA at different concentrations to evaluate SAA's influence on osteogenesis and adipogenesis. In addition, 3-month-old Sprague-Dawley (SD) male rats were treated with distilled water, prednisone alone (3.0 mg·kg−1·d−1) or prednisone (3.0 mg·kg−1·d−1) and SAA (25 mg·kg−1·d−1) for 45 d. At the end point, the different groups of rMSCs were isolated by density-gradient centrifugation and cultured.
Results:
(1) At 0.1–10.0 mg/L, SAA increased ALP activity, type I collagen (Coll-I) mRNA and OPG mRNA expression and stimulated nodule mineralization of rOBs. SAA (0.5 mg/L) also significantly increased the ALP activity of rMSCs without a need for osteogenesis-inducing medium. At 5.0 mg/L, SAA decreased the number of adipocytes with less lipid droplet formation from the rMSCs, which typically undergo adipocyte induction. (2) Coll-I expression was markedly decreased, whereas lipoprotein lipase (LPL) mRNA expression increased by 98% when compared with the first generation of rMSCs in GC-treated rats. The SAA-treated rats demonstrated an over 2-fold increase in Coll-I expression when compared with intact rats and further showed a significant decrease in LPL expression when compared with GC-treated rats. When rMSCs were co-cultured with SAA (0.5 mg/L) in vitro, SAA did not affect Coll-I and LPL gene expression in intact rats but significantly increased Coll-I and decreased LPL gene expression in GC-treated rats.
Conclusion:
SAA protected bone from GC-induced bone marrow impairment by stimulating osteogenesis and depressing adipogenesis in bone marrow stromal cells both in vivo and in vitro. The data indicated that aqueous extract of Salvia miltiorrhiza, which include SAA, may serve as an active anabolic agent and a useful therapeutic strategy for the treatment of GC-associated osteoporosis.
Similar content being viewed by others
Introduction

Glucocorticoids (GCs) reduce bone formation and increase bone resorption. Consequently, individuals treated with GCs have a high incidence of osteoporotic fractures. Although the mechanism responsible for the GC-induced alterations in bone metabolism is not completely understood, multiple-etiologies are attributed to the GC-induced deterioration of skeletal micro-architecture1. Dysregulation of osteogenic growth factor synthesis2 and bone marrow osteogenic cell proliferation3 have been found to mediate excess GC suppression of metabolic activities in osteogenic cells. Furthermore, GC excess strongly increases adipocyte size and number in bone marrow, leading to impaired osteoblast linage recruitment and osteoblast apoptosis4, 5. Recently, attention has been focused on a potential therapeutic modality: controlling the balance between osteoblastogenesis and adipogenesis6. Although pharmacological and chemical treatments with anti-resorptive agents such as bisphosphonate have been reported to alleviate excess GC-suppressed bone mass in vivo, no beneficial candidate has been found to increase osteogenesis and alleviate adipogenesis in the treatment of GC-induced osteoporosis. We hypothesized that compounds with anti-lipid peroxidation and micro-circulation dilation functions would prevent or even reverse GC-induced osteopenia. D(+)β-3,4-dihydroxyphenyl lactic acid (salvianic acid A, SAA), the aqueous bioactive component from Salvia miltiorrhiza Bunge, is an example of this group of compounds. Its chemical structure is presented as follows.
Salvia miltiorrhiza Bunge is a well-known traditional Chinese medicine, which has been widely used in Eastern medicine for the treatment of heart and brain diseases7, hepatitis, hemorrhage, and menstrual abnormalities8. The current leading application of Salvia miltiorrhiza Bunge is in cardiovascular medicine. Phytochemical studies revealed multiple groups of compounds from Salvia miltiorrhiza Bunge extract, the main constituents of which include tanshinones (eg, diterpene chinolones, lipophilic) and phenolics (eg, protocatechuic aldehyde or salvianolic acid B, hydrophilic)9, 10. SAA is contained in lower quantities in the aqueous extract of Salvia miltiorrhiza, but can be derived and bio-transformed in vivo from salvianic acid B. SAA is the simplest structure and the most effective component of Salvia miltiorrhiza. Pharmacological studies have shown that the aqueous bioactive component of Salvia miltiorrhiza is an effective antioxidant and an inhibitor of lipid peroxidation11 and has the potential to improve hemorheology and microcirculation by inhibiting thrombocyte aggregation12 and improving angiogenesis13. Recent studies have found that the aqueous bioactive component from Salvia miltiorrhiza Bunge has additional important effects on osteopathies14, 15, 16. Our previous studies found that the aqueous extracts of Salvia miltiorrhiza and SAA effectively prevented bone loss from long-term administration of prednisone in rats through the stimulation of alkaline phosphatase (ALP) activity in osteoblasts17. On the other hand, Tanshinone IIA, one of the lipophilic components, reduced bone resorption by inhibiting osteoclast differentiation and activity16. It partially prevents ovariectomy-induced bone loss by suppressing bone turnover in vivo15 without stimulating osteoblast ALP activity18. These results indicated that SAA might target osteogenic and adipocyte differentiation in the bone marrow, and this mechanism may be linked directly to GC-mediated depression of bone formation.
In this study we seek to better understand the beneficial effects of SAA on GC-induced osteopenia using osteoblast and bone marrow stromal cell cultures.
Materials and methods
Isolation, proliferation and identification of rOBs
The isolation and proliferation of rOBs was performed according to the literature19. Briefly, the primary osteoblastic cells were isolated from newborn rat calvaria after the periosteum was removed, and the bones were then cut into small flaps of 1 mm3 and subjected to digestion with 0.25% trypsin (Life Technologies Gibco-BRL) for 20 min at 37 °C. The samples were then washed thoroughly with Dulbecco's modified Eagle's medium (DMEM, Gibco) to remove the fibroblast population. Then, the flaps were digested with 0.2% type I collagenase and 0.1% hyaluronidase (Life Technologies Gibco-BRL) for six 20-min intervals at 37 °C. Precipitate and bone flaps were collected after centrifugation, and the samples were transferred to 25 cm2 culture flasks and cultured in DMEM with 100 U/mL penicillin, 100 μg/mL streptomycin, and 10% fetal bovine serum (FBS, Gibco) at 37 °C in a humidified incubator with 5% CO2. The DMEM culture medium was changed every 3 d. To evaluate therapeutic effects, we sub-cultured the cells and expanded the cultures to >5×107 cells. To identify the mineralized function of rOBs, the cells were incubated further in DMEM medium with 10% fetal bovine serum (FBS) in the presence of 50 μg/mL ascorbic acid and 1 mmol/L β-glycerophosphate for 21 d. The cells were then washed with phosphate-buffered saline (PBS) twice, fixed in 95% ethanol for 15 min, and incubated with 1% Alizarin red-S (Sigma, St Louis, MO) for 5 min at room temperature. The mineralized nodules were stained red, and the number and area of nodules per well were counted using a digital imaging system (OM, OsteoMetric Inc, USA).
Isolation, proliferation and identification of rMSCs
The isolation and proliferation of rMSCs was performed according to previously described methods20. Briefly, 4-week-old Sprague-Dawley rats (100 g) (SPF grade, Laboratory Animal Center of Guangdong Medical College) were sacrificed and the bone marrow was harvested by flushing their femoral cavities with PBS. Bone marrow cells were prepared by gradient centrifugation at 900×g for 30 min on a Percoll-Paque gradient (Amersham Pharmacia, USA) at a specific gravity of 1.073 g/mL. The low-density mononuclear cells were washed twice in Hanks' balanced salt solution and cultured in DMEM supplemented with 10% FBS and 1% antibiotic (10 000 U/mL penicillin G sodium, 10 000 μg/mL streptomycin sulfate) at 37 °C in a humidified atmosphere containing 5% CO2. The medium was changed every 3 to 4 d to remove the non-adherent hematopoietic cells. The adherent cell population was expanded and passaged every 12 to 14 d. All cells used for the experiments have been through three passages. To identify the abilities of rMSCs with regard to osteogenesis and adipogenesis, the following studies were preformed.
Induction of osteogenesis and adipogenesis of rMSCs
When the rMSCs from passage number 2 became 80% confluent in the culture plates, the culture medium was changed to an osteoblast inducing medium containing 50 μg/mL L-ascorbic acid, 10−2 mol/L β-glycerophosphate, and 10−8 mol/L dexamethasone. This medium was changed every 3 to 4 d. When the cells became layered and confluent up to 100%, visible symmetric colonies were observed after osteoblast induction. We then tested the cells through a specific alkaline phosphatase (ALP) stain and compared the condition with a non-osteoblast induction condition. The modified Gomori calcium-cobalt method was used to examine intercellular ALP to identify the osteoblasts21. Briefly, the cells were fixed in 95% ethanol for 15 min and incubated at 37 °C for 2 h in a mixture of 3% disodium-β-glycerophosphate (5 mL), 2% barbital sodium (5 mL), 2% Ca(NO3)2 (10 mL), 2% MgSO4 (5 mL) and distilled water (25 mL). A 2% cobaltous nitrate solution was added for 2 min and the plates were washed with water. Then, 1% ammonium sulfate was added for 1 min and the plates were then rinsed with running water. Finally, the plates were dried and photographed. An ALP positive stain is dark brown.
On the other hand, when the rMSCs from passages 2 became 80% confluent, the culture medium was changed to an adipocyte inducing medium containing 5 μg/mL insulin (Sigma, St Louis, MO), 10−6 mol/L dexamethasone (Sigma, St Louis, MO), 6×10−7 mol/L indomethacin (Sigma, St Louis, MO) and 10−4 mol/L isobutylmethyl xanthine (IBMX, Sigma, St Louis, MO) for an additional 14 d. To identify adipocyte induction, we tested rMSCs by Oil red O (Sigma, St Louis, MO). Cells were washed twice with PBS and fixed with 10% formaldehyde for 10 min at room temperature. The cells were stained for 15 min at 37 °C with filtered Oil red O in 60% isopropanol solution. The cells were washed twice with distilled water and PBS, respectively. The positive adipocytes were stained red under a light microscope22.
Animal experimental protocols
Twenty SD male rats (2.5 months old, weighing 195±20 g) were acclimatized to local vivarium conditions (temperature 24−26 °C, humidity 67%) and allowed free access to water and normal diets. All animal experiments were conducted according to the SPF (special pathogen free) animal care-approved protocols at the Animal Center of Guangdong Medical College (Zhanjiang, China). Rats were divided into 4 groups with 5 rats per group. The rats received saline (control, Cont), glucocorticoid (prednisone, Guangdong Xianju Pharmacy Co) 3.0 mg·kg−1·d−1 by oral gavage (GC), glucocorticoid plus SAA (Hanfang Pharmaceutical Co, LTD, Guangzhou) at a dose of 25 mg·kg−1·d−1 oral gavage (SAA), or glucocorticoid plus simvastatin 2 mg·kg−1·d−1 oral gavage (Sim) for 45 d. At the end point, the rats were sacrificed under sterile conditions. The femoral bone marrow cells in one independent group with 5 rats were harvested together and seeded to a 25-mm2 plate and cultured in DMEM with 10% FBS, antibiotic and L-glutamine, as indicated above. The cells in the Cont and GC group were extended to >5×107, respectively, within 3 passages, followed by culturing in a 6-well plates. SAA (0.5 mg/L) was added to Cont and GC cells, respectively, and maintained for 72 h. The remaining bone marrow cells from Cont, GC, SAA and Sim groups were cultured for 7 d with 2 passages. All cells were harvested and total RNA was prepared for examination with Coll-I and LPL mRNA expression by a reverse transcription polymerase chain reaction (RT-PCR) assay.
Reverse transcription polymerase chain reaction (RT-PCR) assay
Total RNA from rOBs or rMSCs was extracted using TRIzol reagent (Invitrogen, Carlsbad, CA) and subjected to RT-PCR analysis using the 9600Gen Amp PCR system (PerkinElmer Applied Biosystems, USA) with PCR reagents from Invitrogen and primers, as shown in Table 1. For Coll-I and OPG, reactions were incubated for 30 min at 50 °C, denatured for 2 min at 94 °C, and subjected to 35 two-step amplification cycles with annealing at 54 °C for 30 s and extension at 70°C for 45 s, followed by denaturation at 94 °C for 30 s. For LPL, reactions were incubated for 30 min at 50 °C, denatured for 2 min at 94 °C, and subjected to 35 two-step amplification cycles with annealing at 51 °C for 30 s and extension at 70 °C for 45 s, followed by denaturation at 94 °C for 30 s. Amplified products were loaded on a 2% agarose gel and subjected to electrophoresis. Digital pictures were taken and analyzed using Bandscan analysis software. Each gene expression was normalized to β-actin. All PCR assays were performed in triplicate.
Determination of ALP and osteocalcin
rOBs in this study were at passage 2, whereas the rMSCs were at passage 3. The cells were divided into the normal control group, the PGE2 10−7 mol/L group, and the dose-dependent SAA groups at 0.01, 0.1, 0.5, 1.0, 5.0 and 10.0 mg/L. The PGE2 10−7 mol/L group was set up for comparison with the SAA groups in terms of mineralization function. A time course detection was performed at 2, 4, and 7 d for ALP activities and at 12, 24, 72, and 120 h for Coll-I mRNA expression after treating the cells with SAA at a concentration of 0.5 mg/L.
ALP activity assay Cells were seeded in 96-well plates at a seeding density of 2×104 cells/cm2 and further cultured in DMEM+10% FBS. Subsequently, the confluent cells were cultured for the indicated period with or without SAA treatment. Cells were washed with PBS and 150 μL of substrate buffer (6.7 mmol/L disodium p-nitrophenylphosphate hexahydrate, 25 mmol/L diethanolamine and 1 mmol/L MgCl2) was added in a 96-well plate. After the mixtures were incubated at 37 °C for 30 min, we measured the absorbance at 405 nm. ALP activity was assessed by reaction with 250 μL of p-nitrophenol solution for 30 min, followed by the appropriate measurements as determined with a standard curve. ALP activity was expressed as micromoles of p-nitrophenol.
Determination of osteocalcin secretion Cells were seeded in 6-well plates at a seeding density of 2×104 cells/cm2 and further cultured in DMEM+10% FBS. Cells were further cultured with or without SAA treatment for 14 d. At the end of the culture, the conditioned media were collected and stored at -20 °C until use. Six cultures from each treatment group were assessed. The concentration of free osteocalcin was measured by radioimmunoassay (RIA) according to the manufacturer's instructions (TianJin Nine Tripods Medical & Bioengineering Co, LTD). The intra-assay variance of the measurements of osteocalcin RIA was 1.26%.
Statistical analysis
The analyses were conducted using SPSS 12.0 software (SPSS Inc, Chicago, IL, USA). Statistical analysis was performed by ANOVA and Bonferroni examination between the two groups. Two-sided 5% and 1% levels of significance were chosen. A P-value<0.05 was considered statistically significant. Data for all parameters were presented as means±SEM (standard error of the mean).
Results
Characteristic for rOBs and the induction of osteogenesis and adipogenesis of rMSCs
To establish stable targeted cells for evaluating the effects of SAA, primary osteoblasts and bone marrow stromal cells were identified with morphology and functional assays. The primary osteoblasts were seen as round in shape, multiangular and comber-like cells after adherence for 2 d, and the population of cells quickly increased in 4 to 7 d. They became multilayered and condensed when cultured up to 14 d, and nodule bone formation was seen in 21 d. The calcified nodule bone was identified by Alizarin red stain (Figure 1).
The first generation rMSCs were polymorphisms, mostly of two types: fibroblast like and epithelia like. When being sub-cultured and induced to become osteoblasts from rMSCs, most of the cells became fibroblast-like and spindle-shaped. Moreover, the cells became corpulent and multiangular with increasing duration of osteoblast induction. The cells could be stained by ALP (a specific stain for osteoblasts) after osteoblast induction from rMSCs for 14 d (Figure 2). When undergoing induction into adipocytes from rMSCs, the cells became enlarged and obese, with some of them forming fat droplets that could be stained by Oil red O. These cells were identified as adipocytes (Figure 3).
Micrographs of bone marrow stromal cells from one month old rat (rMSCs) in different cultured periods. (A) Primary culture for 2 d without osteogenic inducement medium (indicated in Materials and Methods); (B) Subculture for 3 d; (C) Osteogenic inducement for 14 d from subculture rMSCs; (D) Identification of osteoblast by specific ALP stain after osteogenic inducement for 14 d from subculture rMSCs. (A–C: Magnification: ×200); (D: Magnification: ×100).
Effects of SAA on primary rOB activities in vitro
Upon osteoblast treatment, we examined the dose response and the treatment duration of SAA on the differentiation of rOBs. SAA at concentrations from 0.1 to 10.0 mg/L increased ALP activity of rOBs at 2, 4, and 7 d when compared with the control group (P<0.05). No effect on rOBs was observed with SAA at 0.01 mg/L. When the SAA concentration was over 10.0 mg/L, the ALP activity of rOBs was reduced (Figure 4). SAA (0.1 and 5.0 mg/L) also increased the mRNA expression of type I collagen in rOBs when compared with the control group (P<0.05). The strongest effect on type I collagen mRNA expression occurred after 72 h (Figure 5). SAA at concentrations of 0.1 and 0.5 mg/L significantly increased the mRNA level of OPG when compared with the control group (P<0.05). However, at a higher concentration (1.0 mg/L), SAA showed no effect (Figure 6). At concentrations of 0.1 and 0.5 mg/L, SAA also stimulated nodule mineralization in terms of both absolute number and area covered. Numerous bone formation nodules were observed in the six-well plate (Figure 7A). Quantification of this increase is shown in Table 2.
Effects of SAA on type I collagen(Coll-I) mRNA expression of calvarium osteoblast from new born rats (rOB). (A) rOB were treated with SAA in time-dependence, electrophoresis image of Coll-I was determined by RT-PCR. (B) Quantification of Coll-I expression (Coll-I/β-actin) treated by SAA for 12, 24, 72, and 120 h (blank: control, black: SAA). (C) rOB were treated with SAA in dose-dependence, activation of Coll-I was determined by RT-PCR. (D) Quantification of Coll-I expression (Coll-I/β-actin) treated with SAA at dose of 0.1, 0.5, 1.0, and 5.0 mg/L. Data shown are mean±SEM. bP<0.05, cP<0.01 vs SAA 0 mg/L.
Effects of SAA on osteoprotegerin (OPG) mRNA expression of calvarium osteoblast from new born rats (rOB). (A, C) rOB were treated with SAA in dose-dependence and by PGE2, activation of OPG was determined by RT-PCR (M: marker). (B, D) Quantification of OPG expression (OPG/β-actin) treated with SAA at dose of 0.1, 0.5, 1.0, 5.0, 10.0 mg/L and 10−7 mol/L of PGE2. Data shown are mean±SEM. bP<0.05, cP<0.01 vs control.
Effect of SAA on nodule bone formation at 21 d and the corresponding amount of osteocalcine (μg/L) secretion in the medium of rOB. (A) Nodule bone formation of rOB were seen (alizarin red stain) in six well plate (×100). Each well was in control (cont), treated with PGE2 1×10−7 mol/L, SAA 0.1 mg/L, SAA 0.5 mg/L, and SAA 5.0 mg/L. (B) Effects of SAA on the content of osteocalcine (μg/L) in the medium of nodule bone formation of rOB. Data shown are mean±SEM. cP<0.01 vs control.
The osteocalcine secretion in the corresponding medium showed significant increase after SAA treatment (0.5 mg/L, P<0.01, n=4). To compare its ability in stimulating osteoblast differentiation, we evaluated the effect of prostaglandin E2 (PGE2, 1×10−7 mol/L) on rOBs. PGE2 increased osteocalcin secretion but did not stimulate the formation of mineralized bone nodule when compared with the effect of SAA (Figure 7, Table 2).
Effects of SAA on rMSCs in vitro
The rMSCs could differentiate into either osteoblasts or adipocytes, as indicated by morphology changes. The ALP activity of rMSCs was significantly increased after the induction of osteogenesis for 14 d (P<0.01). SAA significantly increased ALP activity at a concentration of 0.5 mg/L in original rMSCs without osteogenic induction (P<0.01). However, SAA showed no effect with regard to ALP activity on rMSCs with osteogenic induction (Figure 8).
The rMSCs differentiated into adipocytes with abundant fat droplets after the induction of adipogenesis (Figure 9B). At concentrations of 0.1 and 1.0 mg/L, SAA did not affect the number of adipocytes under adipocyte induction. At 5.0 mg/L, however, SAA decreased the number of adipocytes (Figure 9). The quantification for adipocyte numbers from three independent experiments are summarized in Table 3.
Effects of SAA on morphology and numbers changes of rMSCs under the adipogenic inducement. (A) Primary rMSCs cultured without adipogenic inducement. (B) Adipogenic inducement of rMSCs for 7 d. Adipogenic inducement of rMSCs plus SAA treatment at concentration of 1.0 mg/L (C) and 5.0 mg/L (D). (Magnification: ×200).
Effects of SAA in vivo on rMSCs of intact and GC-treated rats
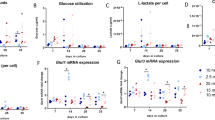
Ex vivo and in vivo studies were performed to evaluate the effects of SAA on rMSCs. Type I collagen (Coll-I) mRNA expression and lipoprotein lipase (LPL) mRNA expression were used to detect the function of osteogenesis and adipogenesis in different groups of rat MSCs. Compared with intact rats, the expression level of Coll-I mRNA was significantly decreased, whereas the LPL mRNA level was increased in the rMSCs of the GC-treated group (P<0.01). When SAA was co-cultured (0.5 mg/L) with rMSCs from intact or GC-treated rats, respectively, SAA did not affect Coll-I or LPL mRNA expression in the rMSCs of intact rats. However, SAA treatment significantly increased Coll-I mRNA expression (P<0.01) and appeared to also decrease LPL mRNA expression (P>0.05) in the rMSCs of GC-treated rats (Figure 10).
Effects of SAA on the Coll-I and lipoprotein lipase (LPL) mRNA expression in rMSCs of saline (Cont) and glucocorticoid treated rats (GC). SAA 0.5 mg/L was added to the rMSCs in vitro. (A) rMSCs electrophoresis image of Coll-I and LPL mRNA was determined by RT-PCR (M: marker). Cells were collected in total 5 rats per group. (B) Quantification of Coll-I expression (Coll-I/β-actin) on rMSCs from Cont and GC rats after treated with SAA (black) in vitro. (C) Quantification of LPL expression (LPL/β-actin) on rMSCs from Cont and GC rats after treated with SAA (black) in vitro. Data shown are mean±SEM. cP<0.01 vs Cont (without SAA). fP<0.01 vs Cont (with SAA). gP>0.05, iP<0.01 vs GC (without SAA).
To compare the effect of SAA with that of a HMG-CoA inhibitor, simvastatin was also tested in a control group (Sim). Rats that were administered SAA at a dose of 25 mg·kg−1·d−1 for 4 weeks showed an increase in Coll-I mRNA expression (P<0.01) and a decrease in LPL mRNA expression (P<0.05) in the rMSCs when compared with the corresponding mRNA expression levels in the GC treated group. At the same time, simvastatin treatment increased the Coll-I mRNA expression (P<0.05) and decreased the LPL mRNA expression (P<0.01) of rMSCs when compared with those in the GC treated group. A greater decrease in LPL mRNA expression was seen in the sim group than in the SAA treated group, whereas an increase in Coll-I mRNA expression was seen in SAA treated rats (Figure 11).
Effects of SAA on the Coll-I and LPL mRNA expression in rMSCs from different groups rats in vivo. (A) rMSCs electrophoresis image of Coll-I and LPL mRNA was determined by RT-PCR (M: marker) from rats treated with saline (Cont), glucocorticoid (GC), GC+salvianic acid A (SAA) and GC+simvastatin (Sim). Cells were collected in total 5 rats per group. (B) Quantification of Coll-I expression (Coll-I/β-actin) on rMSCs in different groups. (C) Quantification of LPL expression (LPL/β-actin) on MSCs in different groups. Data shown are mean±SEM. cP<0.01 vs Cont. eP<0.05, fP<0.01 vs GC.
Discussion
Our study demonstrated that SAA at a concentration range from 0.1 to 10.0 mg/L stimulated ALP activity and increased type I collagen mRNA expression of rOBs in vitro in a dose- and time-dependent manner. SAA at the same range of concentration up-regulated OPG mRNA expression level of rOBs in a dose- and time-dependent manner. SAA at a concentration of 0.5 mg/L increased the number and area of nodule mineralization. It also increased osteocalcin secretion in the rOB cultured medium. These results showed that a lower concentration of SAA not only increased osteoblast differentiation and active bone matrix formation, but also led to mineralization. As indicated in our results, prostaglandin E2 (PGE2) did not increase nodule mineralization of rOBs or decrease OPG mRNA expression (Table 2 & Figure 6). SAA treatment raised the osteocalcin content to 287% in cultured rOBs at 28 d, whereas PGE2 treatment only increased the same osteocalcin content to 72% (Figure 7). The number and area of nodule mineralization of rOBs that were cultured with SAA were higher than that in rOBs treated with PGE2 (Table 2). SAA promoted osteoblast functions by promoting bone mineralization rather than OB proliferation. This effect is beneficial to osteoblasts that conduct mature bone formation and therefore helps to improve bone quality. Currently studies have focused on the anabolic effects of parathyroid hormone (PTH) or growth hormone (GH) on bone. These hormones increase the bone mineral density of osteoporotic individuals but induce both osteoblast and osteoclast proliferation and differentiation, thereby leading to a high bone turnover rate23. Fluoride, an osseous cells stimulator and an effective bone forming agent, could postpone mineralization and induce the dysregulation of calcium distribution, which, in fact, does not decrease the incidence of osteoporotic fractures24. The effect of SAA on promoting osteoblast-mediated bone formation/mineralization may contribute significantly to the upregulation of OPG gene expression in OB. The OPG/RANKL/RANK system plays an important role in osteoclastogenesis and represents significant progress in bone biology. OPG, which is expressed by osteoblasts/stromal cells, strongly inhibits bone resorption by binding to its ligand RANKL and thereby blocks the interaction between BANKL and RANK. OPG especially regulates the later period of bone formation from preosteoblasts to mature osteoblast mineral25. A number of cytokines and hormones exert their effects on bone metabolism by regulating the OPG/RANKL ratio in the bone marrow microenvironment. GCs' impact on osteoblast-mediated bone formation has been attributed to a decrease in the release of OPG26. It was found in this study that SAA could cause nearly 50% more OPG gene expression in rOBs when compared with controls. The effect of mitotic activity of osteoblast by water soluble compounds (crude extracts) in Salvia miltiorrhiza Bunge was early observed by Hu27. Furthermore, SalB enhances angiogenesis processes on SVR cells through the up-regulation of vascular endothelial growth factor (VEGF) and its receptors genes. The present study observed the effects of dose and time of SAA administration on osteoblast mineral bone formation and OPG gene expression.
MSCs are undifferentiated multi-potent cells that predominantly reside in the bone marrow. They can be differentiated in vitro and in vivo into various cell types of mesenchymal origin. Although MSCs have been investigated widely in tissue engineering and gene therapy by multi-potential differentiation, scientists are interested in using MSCs as a model and potential target cells to identify the activators or suppressors of osteoporosis6. Our study isolated rat bone marrow stromal cells (rMSCs), which, although not well-defined, were isolated in this study with a population ratio of 1:100 000 to the mesenchymal stromal cell population by gradient centrifugation with a specific gravity of 1.073 g/mL. The adherent cell population was expanded and passaged 2–3 generations to increase the clonal density of MSCs20. To determine whether the harvested cells possess MSCs, the ability of rMSCs to differentiate in osteogenesis or adipogenesis was evaluated. Our study showed clear morphological changes in rMSCs from a fibroblast shape to a multiangular, osteoblast like structure with positive ALP expression after induction with osteogenic medium for 14 d. With adipocyte medium induction, the rMSCs became obese and were enriched with Oil red O stain-positive fat droplets in the cell plasma. The typical adipocytes were then finally differentiated from rMSCs. Therefore, the rMSCs gathered from our experimental protocols both in vitro and ex vivo were suitable models for investigating the osteogenic and anti-adipogenic potential of the compounds.
We cultured rMSCs in the presence of SAA at concentrations from 0.1 to 5.0 mg/L to determine whether SAA oriented the cells to osteogenesis or adipogenesis. The ALP activity was used as an indicator of early osteoblast differentiation. In our study, early rMSC treatment with osteoblast inducing medium led to barely detectable ALP activity levels. Increased levels of ALP observed at 7 d and stable secretion after 14 d were attributed to maturing osteoblasts from the new proliferation. Our results revealed a significant increase in ALP activity by rMSCs at 14 d without osteoblast induction. The effect of SAA on stimulating rMSC differentiation into osteoblasts was similar to that of the osteoblast induction medium. Moreover, the target cells treated with SAA became condensed and multi-layered and could be stained with ALP as dark spots (results not showed, morphological changes seen in Figure 2D) when compared with the control. Another hydrophilic component of Salvia miltiorrhiza Bunge, salvianic acid B, was reported to increase the total metabolic activity and ALP activity in bone marrow cells at lower concentrations (3–80 g/mL)28. The data demonstrated that SAA not only promoted osteoblast differentiation from marrow stromal cells, but also stimulated mature osteoblast activity in the secretion of bone matrix and the formation of bone minerals. For the effect on rMSCs differentiating into adipocytes, SAA at concentrations of 0.1 and 1.0 mg/L did not decrease the adipocyte number when cultured with rMSCs and adipocyte induction medium. However, 1.0 mg/L of SAA decreased the size of adipocytes and lessened the number of fat droplets (Figure 9C, 9D). In fact, 5.0 mg/L of SAA decreased the adipocyte number significantly (Table 3) when compared with the adipocyte induction control. These two concentrations of SAA could also stimulate ALP activity and increase type I collagen gene expression, as discussed before. No cell toxicity effect on rMSCs was observed at this typical concentration of SAA. For the first time, the inhibitory effects of pure SAA on rMSC differentiation into adipocytes in vitro were demonstrated in the present study.
The present study also provided significant results from both ex vivo and in vivo studies. Excess GC is related to osteoporosis in humans and rodents, where it mainly resulted in impaired osteoblast recruitment and adipogenesis29. Our results revealed that rats treated for long periods with GC (prednisone) exhibited significant decreases in type I collagen mRNA expression, around 97%. This was accompanied by a marked increase in lipoprotein lipase (LPL) mRNA expression (99%) in rMSCs compared with the vehicle control. The result showed a depression of mesenchymal stem cell differentiation to the osteoblast lineage and a preference for adipocyte differentiation in GC treated rats. When co-culturing the rMSCs with 0.5 mg/L of SAA from intact and GC-treated rats, the SAA dose did not significantly affect the type I collagen and LPL gene expression in intact rMSCs, although it did significantly increase type I collagen gene expression and decrease LPL gene expression in the rMSCs of GC-treated rats (Figure 10). Moreover, in vivo administration of SAA at 25 mg·kg−1·d−1 for 4 weeks to GC rats not only counteracted the decrease in type I collagen expression, but also elevated its expression in rMSCs by 2 fold compared with the intact control. However, simvastatin, a HMG-CoA inhibitor, could only recover the type I collagen expression to the control level (Figure 11). Although the HMG-CoA inhibitor lovastatin was able to increase the expression of Cbfa1/Runx2 and osteocalcin promoter activity on D1 cell line to prove its osteogenetic activity30, SAA has a more immediate effect on Coll-I mRNA expression than the HMG-CoA inhibitor. In addition, both SAA and simvastatin could decrease LPL mRNA expression in MSCs from the GC-treated group. A better effect of decreased LPL mRNA expression was seen in simvastatin treated rats (Figure 11). The results demonstrated that SAA has the potential to enhance osteogenesis and inhibit adipogenesis, both in vitro and in vivo.
Except for specific cytokines and some growth hormones with osteogenic and adipogenic effects in the bone marrow, other effective candidates for managing osteoporotic diseases targeted to the bone marrow have been rare. Minocycline was reported to stimulate the proliferation of bone marrow stromal cells31. Statins have been reported as the most effective agent in stimulating osteoblast-mediated bone formation. They promoted MSC differentiation to osteoblasts and inhibited adipogenic differentiation32. However, treatment of pluripotent mouse MSCs M2-10B4 with mevastatin or mevinolin inhibited the maturation of these cells into functional osteoblastic cells, and the effects of mevastatin were reversed by mevalonate33. The cholesterol biosynthetic pathway is needed for bone cell differentiation and maturation. Thus, statins may not be an osteogenic activator but rather an adipogenesis depressor, which may be attributed to their HMG-CoA inhibitory effect. Furthermore, recombinant leptin34, 35, prostaglandins36 and parathyroid hormone (PTH)37 have recently shown significant osteogenic effects on MSCs. However, these hormones may lead to systemic side effects and are expensive. Compared with the anabolic hormones, many compounds from traditional Chinese medicine, which consist of extracts from Salvia miltiorrhiza Bunge, possess potential osteogenic effects on MSCs28 and differentiation effects on other mesenchymal cell types38. Nevertheless, the results from these reports have been from in vitro studies, and the compounds used were crude extracts of herbal medicines. In the present study, our data demonstrated for the first time that SAA, a pure active compound from Salvia miltiorrhiza Bunge extract, could stimulate osteogenesis and inhibit adipogenic differentiation in both intact and impaired MSCs.
Aqueous extract of Salvia miltiorrhiza mainly includes hydrophilic phenolics, such as salvianolic acid B, SAA, and protocatechuic aldehyde. Our previous study showed that three of the compounds could stimulate ALP activity in rat primary osteoblasts, and among the three, SAA produced the most potent effect. The most effective effect on ALP secretion was seen when salvianolic acid B and SAA were in the ratio of 1:1 in the culture medium39, indicating that aqueous extracts of Salvia miltiorrhiza were the solid stimulator of the cells. The hydrophilic phenolics from Salvia miltiorrhiza are the main components in clinical preparations of Denshen injection, a well-known medication widely used in cardiovascular diseases. Denshen possesses pharmacological actions of vasodilation, anti-lipid peroxidation, improved hemorheology and bone marrow microcirculation. Therefore, we hypothesized that those actions were beneficial to the impaired bone marrow from GC associated osteoporosis. The present study supported the use of SAA in the prevention and treatment of different bone remodeling abnormalities, especially GC-induced osteoporosis.
Author contribution
Liao CUI, Tie WU, and Huai-qing CHEN designed research; Liao CUI, Yu-yu LIU and Chun-mei AI performed research; Yu-yu LIU and Tie WU contributed new analytical tools and reagents; Liao CUI and Yu-yu LIU analyzed data; Liao CUI and Yu-yu LIU wrote the paper.
References
Canalis E . Mechanisms of glucocorticoid action in bone. Curr Osteoporos Rep 2005; 3: 98–102.
Delany AM, Durant D, Canalis E . Glucocorticoid suppression of IGF-I transcription in osteoblasts. Mol Endocrinol 2001; 15: 1781–9.
Walsh S, Jordan GR, Jefferiss C, Stewart K, Beresford JN . High concentrations of dexamethasone suppress the proliferation but not differentiation or further maturation of human osteoblast precursors in vitro: relevance to glucocorticoid-induced osteoporosis. Rheumatology 2001; 40: 74–83.
Sher LB, Harrison JR, Adams DJ, Kream BE . Impaired corticalbone acquisition and osteoblast differentiation in mice with osteoblast-targeted disruption of glucocorticoid signaling. Calcif Tissue Int 2006; 79: 118–25.
Ito S, Suzuki N, Kato S, Takahashi T, Takagi M . Glucocorticoids induce the differentiation of a mesenchymal progenitor cell line, ROB-C26 into adipocytes and osteoblasts, but fail to induce terminal osteoblast differentiation. Bone 2007; 40: 84–92.
Nuttall ME, Gimble JM . Controlling the balance between osteoblastogenesis and adipogenesis and the consequent therapeutic implications. Curr Opin Pharmacol 2004; 4: 290–4.
Ghen W, Dong YL, Wang GG, Ting GS . Pharmacological studies of sodium tanshinone II-A sulfonate. Yao Xue Xue Bao 1979; 14: 277–83.
Yasumasa I, Izumi M, Yutaka T . Abietane type diterpenoids from Salvia miltiorrhiza. Phytochemistry 1989; 28: 3139–41.
Hu P, Liang QL, Luo GA, Zhao ZZ, Jiang ZH . Multi-component HPLC fingerprinting of Radix Salviae Miltiorrhizae and its LC-MS-MS identification. Chem Pharm Bull 2005; 53: 677–83.
Zhou L, Chow M, Zuo Z . Improved quality control method for Danshen products-consideration of both hydrophilic and lipophilic active components. J Pharm Biomed Anal 2006; 41: 744–50.
Zhao BL, Jing W, Zhao Y, Hou JW, Xin WJ . Scavenging effects of Salvia miltiorrhiza on free radical and its protection for myocardial mitochondrial membranes from ischemia-reperfusion injury. Biochem Mol Int 1996; 38: 1171–82.
Tang MK, Ren DC, Zhang JT, Du GH . Effect of salvianolic acids from Radix Salviae miltiorrhizae on regional cerebral blood flow and platelet aggregation in rats. Phytomedicine 2002; 9: 405–9.
Lay IS, Chiu JH, Shiao MS, Lui WY, Wu CW . Crude extract of Salvia miltiorrhiza and salvianolic acid B enhance in vitro angiogenesis in murine SVR endothelial cell line. Planta Med 2003; 69: 26–32.
Wang JG, Cao B . Progress of research on the promotion of bone union of fracture with Danshen. Chin J Orthop Traum 2003; 16: 637–8.
Cui L, Wu T, Liu YY, Deng YF, Ai CM, Chen HQ . Tanshinone prevents cancellous bone loss induced by ovariectomy in rats. Acta Pharmacol Sin 2004; 25: 678–84.
Lee SY, Choi DY, Woo ER . Inhibition of osteoclast differentiation by tanshinones from the root of Salvia Miltiorrhiza Bunge. Arch Pharmacol Res 2005; 28: 909–13.
Cui L, Zhou LY, Liu YY, Ai CM, Wu T, Wu Y . Preventing cancellous bone loss in steroid-treated rats and stimulating bone formation by water extract of Salvia miltiorrhiza and Danshensu. Chin Pharmacol Bull 2004; 20: 286–91.
Kwak HB, Sun HM, Ha H, Kim HN, Lee JH, Kim HH, et al. Thanshinone IIA suppresses inflammatory bone loss by inhibiting the synthesis of prostaglandin E2 in osteoblasts. Eur J Pharmacol 2008; 601: 30–7.
Tang LY, Kimmel DB, Jee WS, Yee JA . Functional characterization of prostaglandin e2 inducible osteogenic colony forming units in cultures of cells isolated from the neonatal rat calvarium. J Cell Physiol 1996; 166: 76–83.
Majumdar MK, Thiede MA, Mosca JD, Moorman M, Gerson SL . Phenotypic and functional comparison of cultures of marrow-derived mesenchymal stem cells (MSCs) and stromal cells. J Cell Physiol 1998; 176: 57–66.
Bernard GW . Ultrastructural localization of alkaline phosphatase in initial intramembranous osteogenesis. Clin Orthop Relat Res 1978; 135: 218–25.
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, et al. Multilineage potential of adult human mesenchymal stem cells. Science 1999; 284 (5411): 143–7.
Recker RR, Bare SP, Smith SY, Varela A, Miller MA, Morris SA, et al. Cancellous and cortical bone architecture and turnover at the iliac crest of postmenopausal osteoporotic women treated with parathyroid hormone 1–84. Bone 2009; 44: 113–9.
Haguenauer D, Welch V, Shea B, Tugwell P, Wells G . Fluoride for treating postmenopausal osteoporosis. Cochrane Database Syst Rev 2000; (4): CD002825.
Khosla S . Minireview: The OPG/RANKL/RANK system. Endocrinology 2001; 142: 5050–5.
Hofbauer LC, Kühne CA, Viereck V . The OPG/RANKL/RANK system in metabolic bone diseases. J Musculoskelet Neuronal Interact 2004; 4: 268–75.
Hu MZ . Effect of radix slaviae miltiorrhizae on the mitotic activity of osteoblast-like cells isolated from chicken embryo calvariae cultured in vitro. Chin J Surg 1993; 31: 251–3.
Liu YR, Qu SX, Maitz MF, Tan R, Weng J . The effect of the major components of Salvia miltiorrhiza Bunge on bone marrow cells. J Ethnopharmacol 2007; 111: 573–83.
Canalis E, Mazziotti G, Giustina A, Bilezikian JP . Glucocorticoid-induced osteoporosis: pathophysiology and therapy. Osteoporos Int 2007; 18: 1319–28.
Li X, Cui Q, Kao C, Wang GJ, Balian G . Lovastatin inhibits adipogenic and stimulates osteogenic differentiation by suppressing PPARgamma2 and increasing Cbfa1/Runx2 expression in bone marrow mesenchymal cell cultures. Bone 2003; 33: 652–9.
Williams S, Barnes J, Wakisaka A, Ogasa H, Liang CT . Treatment of osteoporosis with MMP inhibitors. Ann N Y Acad Sci 1999; 878: 191–200.
Tang QO, Tran GT, Gamie Z, Graham S, Tsialogiannis E . Statins: under investigation for increasing bone mineral density and augmenting fracture healing. Expert Opin Investig Drugs 2008; 17: 1435–63.
Parhami F, Mody N, Gharavi N, Ballard AJ, Tintut Y, Demer LL . Role of the cholesterol biosynthetic pathway in osteoblastic differentiation of marrow stromal cells. J Bone Miner Res 2002; 17: 1997–2003.
Reseland JE, Syversen U, Bakke I, Qvigstad G, Eide LG . Leptin is expressed in and secreted from primary cultures of human osteoblasts and promotes bone mineralization. J Bone Miner Res 2002; 17: 1135–40.
Astudillo P, Ríos S, Pastenes L, Pino AM, Rodríguez JP . Increased adipogenesis of osteoporotic human-mesenchymal stem cells (MSCs) characterizes by impaired leptin action. J Cell Biochem 2008; 103: 1054–65.
Ke HZ, Crawford DT, Qi H, Simmons HA, Owen TA, Paralkar VM, et al. A nonprostanoid EP4 receptor selective prostaglandin E2 agonist restores bone mass and strength in aged, ovariectomized rats. J Bone Miner Res 2006; 21: 565–75.
Kaback LA, Soung do Y, Naik A, Geneau G, Schwarz EM, Rosier RN, et al. Teriparatide (1–34 human PTH) regulation of osterix during fracture repair. J Cell Biochem 2008; 105: 219–26.
Wang XJ, Xu JX . Salvianic acid A protects human neuroblastoma SH-SY5Y cells against MPP+-induced cytotoxicity. Neurosci Res 2005; 51: 129–38.
Sun Y, Cui L, Wu T . Preparation of Salvia miltiorrhiza utility aqueous extract by hydrochloric acid method and evaluation on osteoblast. Chin Pharmacol Bull 2008; 24: 377–81.
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (No 30672470).
We wish to thank Dr Dong WANG at University of Nebraska for his contribution on reviewing and English polishing of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cui, L., Liu, Yy., Wu, T. et al. Osteogenic effects of D(+)β-3,4-dihydroxyphenyl lactic acid (salvianic acid A, SAA) on osteoblasts and bone marrow stromal cells of intact and prednisone-treated rats. Acta Pharmacol Sin 30, 321–332 (2009). https://doi.org/10.1038/aps.2009.9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2009.9
Keywords
This article is cited by
-
Tanshinol alleviates impaired bone formation by inhibiting adipogenesis via KLF15/PPARγ2 signaling in GIO rats
Acta Pharmacologica Sinica (2018)
-
Danshen (Salvia miltiorrhiza) protects ovariectomized rats fed with high-saturated fat-sucrose diet from bone loss
Osteoporosis International (2018)
-
Salvianolic acid B stimulates osteogenesis in dexamethasone-treated zebrafish larvae
Acta Pharmacologica Sinica (2016)