Abstract
Data sources
A comprehensive literature search in all languages was carried out. Cochrane Oral Health's Information Specialist searched the following databases: Cochrane Oral Health's Trials Register (till 6 October 2016), the Cochrane Central Register of Controlled Trials (CENTRAL) (The Cochrane Library, 2016, Issue 9), MEDLINE Ovid (1946 till October 6th, 2016), Embase Ovid (1980 till October 6th, 2016) and EThOS (till October 6th, 2016). ClinicalTrials.gov and the World Health Organization International Clinical Trials Registry Platform. Authors were contacted to clarify study information.
Study selection
The inclusion criteria of studies were defined as patients undergoing orthodontic treatment, up to 18 years of age. Interventions: orthodontic treatment, exposure: non-pharmacological orthodontic pain intervention (low-level laser therapy, vibratory stimulation, chewing adjuncts, brain wave music or cognitive behavioral therapy and post-treatment communication ‘text message’). Outcome: pain.
Data extraction and synthesis
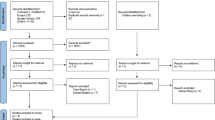
Two authors reviewed each study independently. A third author was used to resolve any disagreement on the eligibility of the included studies. The authors excluded papers that had unsuitable study design, and assessed the risk of bias on each paper they included. Data were combined using a random effect model and expressed results as mean differences (MD) with 95% confidence intervals (CIs).
Results
The authors included 14 randomised controlled trials (RCTs) that randomised 931 participants. Intervention modalities included: low-level laser therapy (LLLT) (four studies); vibratory devices (five reviews); chewing adjuncts (three studies); brainwave music or cognitive behavioral therapy (one study) and post-treatment communication in the form of a text message (one study). Twelve studies involved self-report assessment of pain on a continuous scale and two studies used questionnaires to assess the nature, intensity and location of pain. The combined data from two studies involving 118 participants provided low-quality evidence that LLLT reduced pain at 24 hours by 20.27 mm (95% CI −24.50 to −16.04, P < 0.001; I² = 0%). LLLT also appeared to reduce pain at six hours, three days and seven days. The results for the other comparisons are inconclusive due to low evidence quality.
Conclusions
The overall results of the current study are inconclusive. There is low quality evidence that non-pharmacological interventions reduce pain during orthodontic treatment.
Similar content being viewed by others
Commentary
Prevention of pain during orthodontic treatment is important to ensure patient compliance during the course of treatment. Pharmacological approaches are considered first-line therapy especially in the initial stages of treatment, particularly following initial orthodontic placement. Non-pharmacological measures (low-level laser therapy, vibratory stimulation, chewing adjuncts, brain wave music or cognitive behavioral therapy,and post-treatment communication ‘text message’) could be considered as an alternative to medication.
A Cochrane review was undertaken to assess the effects of non-pharmacological interventions to ease pain associated with orthodontic treatment. The current systematic review compared randomised controlled trials of a non-pharmacological pain intervention to a placebo or no intervention. Orthodontic and orthognathic procedures requiring analgesia or pharmacological pain relief following a surgical procedure were excluded, as were split-mouth trials and crossover trials.
Pain threshold differs from one person to another. Bartley1 for example concluded that increased pain sensitivity and risk for clinical pain are more common in women. A systematic review conducted by Wingfai Kwok et al.2 emphasised the cultural differences in pain perception for cancer patients. Asian patients normalised pain in comparison to Western patients who engage in active health-seeking behavior.2 According to El Tumi H. et al.3 old adults have lower pressure pain threshold in comparison with young adults.
Across the studies data were insufficient to consider the impact of different participant characteristics on the effectiveness of the interventions to reduce pain,4 for instance, investigating differential response between males and females.4 Information on the country where the study was carried out eg Japan, UK etc was provided within the tables, but no information was provided on ethnic groups. It may have been useful if the study's authors had attempted to include a more detailed description of the patient groups eg culture, ethnicity, gender and age. These variables may have been one of the reasons for the heterogeneity, or differences in pain perceptions and management across the different studies. However another reason is simply the differences between the contrasting non-pharmacological techniques.
The current study provides low quality of evidence due to lack of similar studies, small number of the included studies, variation among interventions and wide confidence intervals within the studies. There was no information about cost or side effects of these non-pharmacological interventions, which would have been useful. In addition, there was no prolonged follow-up to measure the effectiveness of treatment.
The review's authors assessed the quality of the included studies. Thirteen studies studies were assessed at unclear risk or high risk, with a lack of clarity about random sequence generation in six studies and questions regarding how the participants were allocated to the intervention group or control group (allocation concealment) being noted in five studies.
The wide diversity of non-pharmacological interventions can make it difficult to make an overall conclusion about the effectiveness of such a group. Due to the lack of reliable evidence and small number of studies concerning the effectiveness of a range of non-pharmacological interventions to manage orthodontic pain, the authors suggested more prospective research in the field.
References
Bartley EJ, Fillingim RB . Sex differences in pain: a brief review of clinical and experimental findings. B J Anaesth 2013; 111: 52–58.
Kwok W, Bhuvanakrishna T . The relationship between ethnicity and the pain experience of cancer patients: a systematic review. Indian J Palliat Care 2014; 20: 194–200.
El Tumi H, Johnson MI, Dantas PBF, Maynard MJ, Tashani OA . Age-related changes in pain sensitivity in healthy humans: A systematic review with meta-analysis. Eur J Pain 2017; 21: 955–964.
Fleming PS, Strydom H, Katsaros C, et al. Non-pharmacological interventions for alleviating pain during orthodontic treatment. Cochrane Database Syst Rev 2016; 12: CD010263
Author information
Authors and Affiliations
Additional information
Address for correspondence: Luisa Fernandez Mauleffinch, Managing Editor, Cochrane Oral Health Group, School of Dentistry, The University of Manchester, JR Moore Building, Oxford Road, Manchester, M13 9PL, UK. E-mail: luisa.fernandez@manchester.ac.uk
Fleming PS, Strydom H, Katsaros C, MacDonald L, Curatolo M, Fudalej P, Pandis N. Non-pharmacological interventions for alleviating pain during orthodontic treatment. Cochrane Database Syst Rev 2016; 12: CD010263. doi:10.1002/14651858.CD010263.pub2. Review. PubMed PMID: 28009052.
This paper is based on a Cochrane Review published in the Cochrane Library 2016, issue 12 (see www.thecochranelibrary.com for information). Cochrane Reviews are regularly updated as new evidence emerges and in response to feedback, and the Cochrane Library should be consulted for the most recent version of the review.
Rights and permissions
About this article
Cite this article
Aljudaibi, S., Duane, B. Non-pharmacological pain relief during orthodontic treatment. Evid Based Dent 19, 48–49 (2018). https://doi.org/10.1038/sj.ebd.6401305
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6401305