Abstract
Data sources
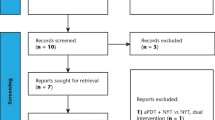
The Cochrane Oral Health Group Trials Register, Cochrane Central Register of Controlled Trials, Medline and Embase were searched to April 2006. Reference lists from relevant articles were scanned and the authors of eligible studies were contacted to identify trials and obtain additional information.
Study selection
For inclusion, an article had to satisfy the following criteria: document a randomised controlled trial (RCT); participants should be people receiving chemotherapy or radiotherapy treatment for cancer; prescribe agents to prevent oral mucositis; and have the primary outcome of preventing mucositis.
Data extraction and synthesis
Data were extracted independently and in duplicate. Authors were contacted for details of randomisation and withdrawals and a quality assessment was carried out. For dichotomous outcomes, risk ratios (RR) were calculated using a random-effects model.
Results
The search identified 202 articles, of which 71 studies had useable data comprising 5217 patients. Of the 29 interventions included in the trials, 10 studies showed some evidence of a weak benefit for preventing or reducing the severity of mucositis. Interventions where more than one trial in the meta-analysis found a significant difference compared with placebo/ no treatment were as follows:
-
amifostine: provided minimal benefit in preventing moderate and severe mucositis (RR, 0.84 and 0.60, respectively);
-
antibiotic paste or pastille: demonstrated moderate benefit in preventing mucositis (RR, 0.87);
-
hydrolytic enzymes: reduced moderate and severe mucositis (RR, 0.52 and 0.17, respectively); and
-
ice chips: prevented mucositis at all levels (RR, 0.63, 0.43 and 0.27).
Other interventions showing some benefit in only one study were benzydamine, calcium phosphate, honey, oral care protocols, povidone and zinc sulphate.
Conclusions
Several of the interventions were found to have some benefit at preventing or reducing the severity of mucositis associated with cancer treatment. The strength of the evidence was variable and implications for practice include consideration that benefits may be specific for certain cancer types and treatment. There is a need for well-designed RCT with sufficient numbers of participants to perform subgroup analyses by type of disease and chemotherapeutic agent.
Similar content being viewed by others
Commentary
The clinical question asked in this review is an important one. Oral mucositis (OM) occurs in up to 100% of patients undergoing bone marrow transplant, is associated with fever, infection and 100-day mortality,1 and is one of the most debilitating side effects of transplantation.2 In patients receiving radiotherapy for head and neck malignancies, OM is the major dose-limiting side effect and has the potential to cause significant treatment interruptions or premature termination of therapy, with resultant impact on local tumour control and patient survival. Quality of life may be greatly compromised because of severe pain and nutritional impairment. Treatment of the symptoms of OM may necessitate narcotic analgesics, enteral feeding and hospitalisation, adding significantly to the overall costs of treatment.1
This report uses the established, scientifically sound systematic review methods of the Cochrane Collaboration, and follows earlier work by the authors in the area of oral complications associated with cytotoxic cancer therapy. The authors report some benefit from several interventions, but the evidence is weak and is insufficient to guide practice. For instance, it is reported that amifostine, the intervention with the largest body of evidence in this review (five studies, comprising 446 patients) appears to have some, minimal, benefit for patients undergoing radiotherapy to the head and neck. It was reported that it did not affect survival at 24 months, recurrence at 18 months or incomplete response to radiation treatment, but there has been debate regarding theoretical concerns that amifostine may also protect tumour cells: long-term data are still unavailable to alleviate those concerns.
For another intervention, topical antibiotics, a large, multicentre RCT published in 20023 apparently was not identified by the search strategy. In that study of 137 patients, no difference was seen between the antibiotic lozenge and placebo control, data which may have affected the findings of the review.
Although ice chips were found to be beneficial, this finding is limited to the specific patient population undergoing 5FU (5 Flurouracil ) chemotherapy and is based on two trials, one of which was considered to be of medium risk and the other at high risk for bias.
As this review indicates, evidence remains elusive regarding the prevention and treatment of OM in people being treated for cancer, despite the fact that the current update has identified 19 more trials in less than 2 years. The authors point out significant flaws with past research in OM, common to many studies reported in the biomedical literature, although it is encouraging that several negative trials have been published. Study design and resulting useable data has been hampered by several factors, including lack of standardised outcome measures for OM, and intrastudy variability in disease types and sites and cytotoxic regimens.4–6
The biological complexities of OM at the molecular, cellular and tissue levels, as well as genetic influences and interaction with the local tissue environment, have only recently been understood,7,8 In this light, it is not surprising that past research, much of it based on empiricism rather than strong biological rationale, has failed to discover effective interventions. As our knowledge of the pathophysiology of OM advances, research targeting specific pathways, conducted in rigorous studies with adequate power to allow subgroup analyses, is needed. In parallel, new technology designed to more precisely target tumour while sparing normal mucosa (for example, intensity-modulated radiation therapy for head and neck cancer) should be pursued.
Practice points
Oral mucositis is a serious, pervasive and debilitating side effect of cytotoxic cancer therapy.
To date, there are few effective management strategies, other than palliative measures, including adequate pain control.
Despite a lack of evidence for oral care protocols, common sense dictates that good oral hygiene be maintained to the extent possible during therapy and that the dentist be aware of the possibility of pancytopenia or the presence of central venous access lines when contemplating dental procedures while a patient is under active treatment.
References
Sonis ST, Oster G, Fuchs H, et al. Oral mucositis and the clinical and economic outcomes of hematopoietic stem-cell transplantation. J Clin Oncol 2001; 19: 2201–2205.
Bellm LA, Epstein JB, Rose-Ped A, Martin P, Fuchs HJ . Patient reports of complications of bone marrow transplantation. Support Care Cancer 2000; 8:33–39.
El-Sayed S, Nabid A, Shelley W, et al. Prophylaxis of radiation-associated mucositis in conventionally treated patients with head and neck cancer: a double-blind, phase III, randomized, controlled trial evaluating the clinical efficacy of an antimicrobial lozenge using a validated mucositis scoring system. J Clin Oncol 2002; 20:3956–3963.
Sonis ST, Eilers JP, Epstein JB, et al. Validation of a new scoring system for the assessment of clinical trial research of oral mucositis induced by radiation or chemotherapy. Mucositis Study Group. Cancer 1999; 85:2103–2113.
Sutherland SE, Browman GP . Prophylaxis of oral mucositis in irradiated head-and-neck cancer patients: a proposed classification scheme of interventions and meta-analysis of randomized controlled trials. Int J Radiat Oncol Biol Phys 2001; 49:917–930.
Scully C, Epstein J, Sonis S . Oral mucositis: a challenging complication of radiotherapy, chemotherapy, and radiochemotherapy. Part 2: diagnosis and management of mucositis. Head Neck 2004; 26:77–84.
Sonis ST, Elting LS, Keefe D, et al. Perspectives on cancer therapy-induced mucosal injury: pathogenesis, measurement, epidemiology, and consequences for patients. Cancer 2004; 100 (suppl.):S1995–S2025.
Anthony L, Bowen J, Garden A, Hewson I, Sonis S . New thoughts on the pathobiology of regimen-related mucosal injury. Support Care Cancer 2006; 14:516–518.
Author information
Authors and Affiliations
Additional information
Address for correspondence: Professor Helen Worthington, Co-ordinating Editor, Cochrane Oral Health Group, MANDEC, School of Dentistry, University of Manchester, Higher Cambridge Street, Manchester M15 6FH, UK. Email: helen.worthington@manchester.ac.uk.
Worthington HV, Clarkson JE, Eden OB. Interventions for preventing oral mucositis for patients with cancer receiving treatment. Cochrane Database of Systematic Review 2006; issue 2
Rights and permissions
About this article
Cite this article
Sutherland, S. Several therapies may prevent or reduce the severity of oral mucositis associated with cancer treatment. Evid Based Dent 7, 104–105 (2006). https://doi.org/10.1038/sj.ebd.6400451
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6400451