Abstract
It has been suggested that losses of twin conceptuses in very early pregnancy are high, and that for every liveborn twin pair there are a further 10–12 twin pregnancies that end up as a singleton birth1. Here we show that in a group of women who had double-ovulated and conceived, the probability of the second egg also becoming fertilized and developing is 20–30% — which is comparable to the probability of conception and survival of a single conceptus2. We conclude that the presence of one embryo does not affect the development of its twin.
Similar content being viewed by others
Main
So far, no direct measure has been available of the proportion of double ovulations that lead to twins. We have obtained this information by using ultrasound to identify pregnant women with two corpora lutea, and correlating these with the number who had one or two fetuses (dizygotic twins) in early pregnancy. The corpus luteum is an endocrine organ that develops in the ovary at the site at which the egg was released, and can therefore act as an indicator of the number of ovulation events.
As only two small ultrasound studies have identified the corpus luteum in early pregnancy3,4, we confirmed these findings in a larger series at our centre, where the ovaries of all pregnant women are routinely examined. We scan mainly low-risk pregnancies, as well as women who had assistance in conceiving. In scans of 504 women where both ovaries were seen in early pregnancy (5–9 weeks gestation), the corpus luteum could be identified in 94.6% of cases. Its mean diameter was 19.6 mm (± 5.28 standard deviation). Single ovulations were distributed equally between the two ovaries, occurring on the left in 49.3% of cases.
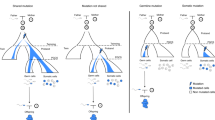
There were 48 cases of double ovulation identified by these ultrasound scans (Fig. 1). Of these (Table 1), 27 were spontaneous, with 9 among this group conceiving twin pairs (30%) and the remainder singletons. Fifteen double ovulations were induced by clomiphene citrate, and among these there were three sets of twins (20%). We were unable to determine whether the dual ovulation was spontaneous or induced in the remaining six cases, of which three were twin pregnancies. Maternal age among those who had double-ovulated (32.5 years) was not significantly different from those who had had a single ovulation (30.7 years; P = 0.07, t-test). All sets of twins were of dichorionic and diamniotic placentation on ultrasound examination, which is consistent with dizygotic twinning.
We conclude that the presumption of huge losses of dizygotic twins in early pregnancy1 is unfounded, as we would then have seen many more double ovulations with a singleton-pregnancy outcome (signifying an aborted twin). The probability of the second egg also becoming fertilized seems to be similar to that of one egg becoming fertilized in a singleton pregnancy2. The presence of one embryo therefore does not impede the development of its twin.
Our study does not, of course, eliminate the possibility that both twins might be lost at a higher rate than singletons. However, we do not believe that this would fit with our finding that the second egg has the same chance of developing as a singleton pregnancy once the first egg is fertilized.
The distribution of spontaneous double ovulations is consistent with a random spread of ovulation between left and right ovaries (Table 1). This suggests that the mechanism responsible for dual ovulation involves signalling from outside the ovary, rather than local intra-ovarian control5, as we would then have seen more double ovulations from the same ovary.
We have confirmed that the corpus luteum can be readily identified in an early-pregnancy scan, enabling us to characterize a significant number of double ovulations in the human. To our knowledge the last attempt to do this was in 1794, when William Hunter observed after 400 dissections of pregnant uteri: “When there is one child, there is only one corpus luteum; and two in the case of twins. ...In some of these cases, there were two distinct corpus lutea in one ovarium.”6.
References
Boklage, C. E. in Multiple Pregnancy. Epidemiology, Gestation and Perinatal Outcome (eds Keith, L. G., Papiernik, E., Keith, D. M. & Luke, B.) 41–50 (Parthenon, New York, 1995).
Short, R. V. Ciba Found. Symp. 64, 377–394 (1978).
Frates, M. C. et al. J. Ultrasound Med. 20, 821–827 (2001).
Durfee, S. M. & Frates, M. C. J. Clin. Ultrasound 27, 55–59 (1999).
Gilfillan, C. P. et al. J. Clin. Endocrinol. Metab. 81, 1557–1562 (1996).
Short, R. V. in The Ovary (eds Zuckerman, L. & Weir, B. J.) 1–39 (Academic, New York, 1977).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
brief communications is intended to provide a forum for both brief, topical reports of general scientific interest and technical discussion of recently published material of particular interest to non-specialist readers. Priority will be given to contributions that have fewer than 500 words, 10 references and only one figure. Detailed guidelines are available on Nature's website (http://www.nature.com) or on request from nature@nature.com
Rights and permissions
About this article
Cite this article
Tong, S., Meagher, S. & Vollenhoven, B. Dizygotic twin survival in early pregnancy. Nature 416, 142 (2002). https://doi.org/10.1038/416142a
Issue Date:
DOI: https://doi.org/10.1038/416142a
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.