Abstract
Barrett's esophagus is diagnosed when goblet cells are found in the lower esophageal mucosa. However, the distribution of these cells is patchy and they may not represent the earliest marker of intestinal metaplasia. Cdx2 is a transcription factor whose expression in normal tissues is restricted to intestinal-type epithelium. Its distribution in the columnar-lined esophagus with and without intestinal metaplasia has been seldom studied. We evaluated Cdx2 expression in lower esophageal biopsies from 90 patients with endoscopic diagnosis of short segment Barrett's esophagus, including 45 consecutive cases showing intestinal metaplasia (goblet cells present in hematoxylin eosin and/or Alcian blue stains) and 45 consecutive cases without goblet cells. 25 samples of cardiac-type mucosa without intestinal metaplasia biopsied from the stomach served as controls. All cases with intestinal metaplasia revealed Cdx2 reactivity in goblet cells and adjacent nongoblet columnar cells. Dysplastic foci, seen in five cases from this group, were Cdx2 positive. In the group without goblet cells, Cdx2 was focally expressed by columnar cells in 17 (38%) cases. All control cases were Cdx2 negative. Strips of Alcian blue-positive nongoblet columnar cells (‘columnar blues’) were observed in 11 (24%) of the cases without intestinal metaplasia. All these foci were Cdx2 negative. In conclusion, Cdx2 is a highly sensitive marker for Barrett's esophagus. It is also expressed in a significant minority of cases of columnar-lined esophagus without goblet cells, suggesting that it may detect intestinal phenotypic modifications in the absence of goblet cells. Accordingly, Cdx2 immunostaining could help identify patients with Barrett's metaplasia in cases where no goblet cells are visible in biopsies from the columnar-lined esophagus. Finally, lack of Cdx2 expression in the ‘columnar blues’ suggests that these cells are not diagnostic of intestinal metaplasia.
Similar content being viewed by others
Main
Barrett's esophagus is the premalignant lesion for adenocarcinoma of the esophagus.1, 2, 3 It is characterized by a columnar change in the distal esophageal squamous epithelium that can be recognized at endoscopy, and is confirmed to have intestinal (specialized) metaplasia by biopsy.4 Although the specialized columnar epithelium is composed of both goblet and columnar non goblet cells, only the former are considered as the hallmark of Barrett's esophagus.4, 5, 6, 7 The rapidly rising incidence of esophageal adenocarcinoma over the past two decades has driven efforts to identify patients with Barrett's esophagus.8, 9, 10 Currently, endoscopy with biopsies is the gold standard in making a diagnosis of this entity. The sensitivity and positive predictive values of standard upper endoscopy for diagnosing Barrett's esophagus have, however, been reported as 82 and 34%, respectively.11 This is secondary to the patchy and mosaic distribution of intestinal metaplasia within the columnar-lined esophagus.4, 11, 12 Thus, the diagnosis may be missed when goblet cells are inconspicuous or when small biopsies with crush artifact are sent for examination. In addition, it has been recently suggested that during the reflux–metaplasia–dysplasia–adenocarcinoma sequence, goblet cell development is preceeded by the development of columnar ‘cardiac-type’ metaplastic cells.13, 14 Accordingly, the availability of a marker capable of detecting intestinal differentiation in the absence of goblet cells could be of clinical importance.
The caudal-related Cdx2 gene encodes an intestine-specific transcription factor belonging to the homeobox family of genes that has been reported to regulate both proliferation and differentiation in intestinal epithelial cells.15, 16, 17, 18, 19 The expression of Cdx2 in adult non-neoplastic tissues has been shown to be restricted to normal intestinal epithelium, normal pancreatic epithelial cells, and gastric and esophageal intestinal metaplasia.20, 21, 22, 23, 24, 25, 26, 27 In the gastrointestinal tract, Cdx2 is strongly and diffusely expressed in the nuclei of normal small and large intestinal epithelial cells, including absorptive, goblet, endocrine and Paneth cells; in the pancreatic epithelium its expression is focal and patchy.22, 24, 27 Normal esophageal and gastric epithelial cells are Cdx2 negative.22, 24, 27 In contrast, esophageal and gastric intestinal metaplastic cells are Cdx2 positive.20, 21, 23, 25, 26 Further studies will help to confirm or refute Cdx2 as a sensitive and specific marker of intestinal differentiation.
The purposes of this study were to assess Cdx2 immunoreactivity in the columnar-lined esophagus with and without intestinal metaplasia and to determine the potential utility of this marker in detecting intestinal differentiation of the columnar-lined esophagus in the absence of goblet cells.
Materials and methods
We prospectively analyzed lower esophageal biopsies from 45 consecutive patients with endoscopically recognized columnar-lined esophagus in which intestinal metaplasia was demonstrated histologically (Barrett's esophagus) and from 45 consecutive patients with endoscopically recognized columnar-lined esophagus in which no goblet cells were found. All cases consisted of formalin-fixed paraffin-embedded, randomly taken lower esophageal biopsies containing columnar and squamous epithelium. They were obtained from 90 patients with symptoms related to reflux and an endoscopic diagnosis of short-segment Barrett's esophagus (columnar-lined esophagus <3 cm in length). Clinical and endoscopic data were obtained from the patients' hospital charts and/or by contacting the patients' physician when necessary. Specimens were stained with hematoxylin–eosin and Alcian blue (pH 2.5) stains, and later subdivided into those with or without goblet cells. Positive Alcian blue staining of columnar cells without unequivocal features of goblet cells (‘columnar blue cells’) was not regarded as intestinal metaplasia.
For controls, 25 samples of gastric cardiac-type mucosa without intestinal metaplasia biopsied from the stomach were used. The gastroesophageal junction corresponded to the location of the squamocolumnar junction in all these cases. Sections were prepared and evaluated in the same way as the study specimens.
For Cdx2 immunohistochemistry, sections were placed on positively charged glass slides, deparaffinized and subjected to high-temperature antigen unmasking in Tris-buffer, pH 9.5 (NUCLEAR Decloaker, BiocareMedical Walnut Creek, CA, USA) using an electric pressure cooker set at 118° for 4 min. Endogenous peroxidase activity was quenched with hydrogen peroxide. Detection of Cdx2 binding (clone Cdx2-88; dilution 1:25; Biogenex, San Ramon, CA, USA) was achieved using the Picture-Plus polymer kit (Zymed, South San Francisco, CA, USA). The formed complexes were visualized with aminoethyl carbazole chromogen/substrate. Sections were then counterstained with hematoxylin, dehydrated, cleared and permanently mounted. Normal colonic mucosa was used as positive control. In the negative control, the primary antibody was discarded. Only nuclear staining was considered as positive.
Results
There were no significant clinical differences between the two groups. The 45 cases that showed goblet cells included a total of 162 biopsies (mean: 3.6 biopsies per block, range: 1–5) belonging to 32 males and 18 females with a mean age of 58 years (range: 19–85 years). In the group without goblet cells, there was a total of 153 biopsies (mean: 3.4 biopsies per block, range: 1–5) taken from 29 males and 21 females with a mean age of 54 years (range: 20–79 years).
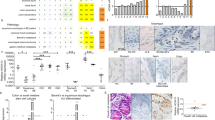
All 45 cases of Barrett's esophagus revealed nuclear Cdx2 reactivity in areas of intestinal metaplasia. The staining was strong and clearly seen in both goblet and adjacent nongoblet columnar cells (Figure 1). Five (11%) cases had foci of dysplasia (low grade in four cases and high grade in one case). All dysplastic cells revealed strong nuclear reactivity for Cdx2 (Figure 2). Overall, 22 cases from this group included tissue fragments devoid of goblet cells; in five (23%) of them there was focal Cdx2 expression in columnar cells that were negative or weakly positive for Alcian blue stain.
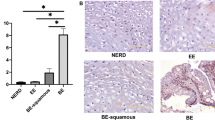
In the group without goblet cells, 17 of 45 (38%) cases demonstrated focal nuclear Cdx2 expression of variable intensity (Figure 3). In most cases, Cdx2-positive cells were located at the surface or in the upper portion of cardiac or oxyntocardiac-type glands and adjacent or at a short distance from the squamocolumnar junction. All the Cdx2-positive columnar cells were negative or weakly positive for Alcian blue stain (Figure 3). No dysplasia was found in this group. None of the cases from the control group expressed Cdx2.
Strips of superficial Alcian blue-positive columnar mucous cells devoid of goblet cells (‘columnar blues’) were identified in 11 (24%) cases from the group without intestinal metaplasia. None of these foci expressed Cdx2 (Figure 4). Diffuse cytoplasmic or granular perinuclear reactivity for Cdx2 was observed in superficial and deep columnar cells in 10 (22%) of the cases with intestinal metaplasia and in 16 (35%) of the cases without intestinal metaplasia. As previously stated, this staining pattern was disregarded. The squamous epithelium was consistently Cdx2 negative.
Discussion
Our study showed that the intestinal marker Cdx2 is consistently expressed in esophageal intestinal metaplasia. In addition, it was found to be reactive in a significant minority of biopsies taken from patients with an endoscopic diagnosis of columnar-lined esophagus in which no goblet cells were found. Human Cdx2 is a member of the caudal-related homeobox gene family that activates an intestinal-specific gene transcription, which regulates normal intestinal development and differentiation and plays an important role in triggering cells towards the phenotype of differentiated enterocytes as well as in the maintenance of the phenotype.15, 16, 17, 18, 19 Cdx2 expression in normal adult tissues is restricted to intestinal and colonic epithelium and a subset of pancreatic acinar and ductal cells.22, 24, 27 In neoplasms, it is expressed by small and large intestinal epithelial tumors, by esophageal, urinary bladder and ovarian mucinous adenocarcinomas, and by a subset of pancreatobiliary adenocarcinomas.20, 21, 22, 24, 25, 26, 27, 28, 29 In addition, Cdx2 is consistently expressed in gastric intestinal metaplasia and gastric adenocarcinomas with an intestinal phenotype.20, 21, 26, 29 Accordingly, it was suggested that Cdx2 may be involved in intestinal differentiation along the gastric carcinogenesis pathway.20
Cdx2 reactivity in Barrett's esophagus has been seldom evaluated. Eda et al23 studied three cases of Barrett's esophagus and found Cdx2 expression in all of them. In a larger series, Phillips et al25 analyzed 134 esophageal biopsy and resection specimens and found Cdx2 expression in goblet and nongoblet columnar cells in 100% (72 of 72) of the slides with intestinal metaplasia. Our study yielded identical results in the group with goblet cells, confirming the exquisite sensitivity of this marker in detecting intestinal metaplasia of the columnar-lined esophagus. Five of our cases from the group with goblet cells had areas of Barrett's-related dysplasia and all of them expressed Cdx2. Likewise, in the study of Phillips et al25 Cdx2 was heterogeneously expressed in each of 38 slides from 21 patients with Barrett's-related dysplasia or adenocarcinoma. This finding was not unexpected since dysplasia and adenocarcinoma are invariably associated with intestinal metaplasia of the columnar-lined esophagus.1, 2, 3
We found strips of Alcian blue-positive superficial columnar cells in 24% of cases from the group without goblet cells; all of which were Cdx2 negative. Some authors have suggested that these cells, known as ‘columnar blues’, represent an indicator of intestinal metaplasia and Barrett's esophagus.30, 31 However, other studies questioned this view.7, 32, 33 The absence of Cdx2 expression in these cells suggests that they are not diagnostic of intestinal metaplasia in the columnar-lined esophagus. It can be argued that the ‘columnar blues’ represent an incomplete or early form of intestinal metaplasia being Cdx2 produced at later stages. However, it has been demonstrated that Cdx2 expression constitutes a very early event during intestinal development, as its presence is necessary for embryonic intestinal proliferation and differentiation.15, 17, 19
The most interesting finding of this study was the presence of Cdx2-positive columnar cells in a substantial minority (38%) of cases lacking histological or histochemical features of intestinal metaplasia. The same feature was observed in five of the 22 (23%) cases from the group with intestinal metaplasia that included tissue samples devoid of goblet cells. In contrast, all our control cases were Cdx2 negative. These results validate the findings of Phillips et al,25 who reported Cdx2 reactivity in 30% (20 of 62) of cases of columnar-lined esophagus without definitive histologic evidence of intestinal metaplasia. Although it can be argued that Cdx2 expression in the columnar-lined esophagus without goblet cells indicates lack of specificity, we agree with Phillips et al25 in that it rather reflects the ability of Cdx2 to detect early intestinal phenotypic features prior to morphologic and histochemical changes identified by conventional histological and histochemical methods.
Previous studies have demonstrated that Cdx2 plays an important role in the development of gastric intestinal metaplasia21, 34 and in the activation of the intestinal mucin gene MUC2 in gastric cells leading to goblet cell differentiation.35, 36 Cdx2 reactivity in the nongoblet cell population of the columnar esophagus may be an early event in intestinal differentiation, and its presence would indicate that the molecular machinery for intestinal differentiation is in place, even when histologic evidence of such differentiation is lacking.25 In fact, it has been proposed that the first step in the reflux–adenocarcinoma sequence of the columnar-lined esophagus is the development of columnar nongoblet epithelium of ‘cardiac-type’ which may evolve either to oxynto-cardiac mucosa, with no risk of malignant transformation, or to intestinal-type epithelium, with risk for adenocarcinoma.13, 14 We do not know from our study how many of the Cdx2-positive cases from the group without goblet cells were truly negative for these cells and how many represented underdiagnosis of the lesion because of insufficient sampling. Nevertheless, it is tempting to speculate that the ability of Cdx2 immunostaining in detecting intestinal differentiation in samples of columnar-lined esophagus devoid of goblet cells may alert us to the existence of Barrett's metaplasia in patients that otherwise would have been dismissed.
Intestinal differentiation of the nongoblet columnar cell population in the columnar-lined esophagus has been previously demonstrated using other antibodies. Chaves et al37 assessed the immunoreactivity for sucrase–isomaltase (SI) and dipeptidylpeptidase (DPP), two markers of enterocytic differentiation that are not expressed by goblet cells, in the columnar-lined esophagus. SI was positive in 67% of cases with goblet cells and in the same percentage of cases without goblet cells, whereas DPP was identified in 50% of cases with and in 75% of cases without goblet cells. They also found expression of both markers in esophageal adenocarcinoma and suggested that, in addition to goblet cells, the nongoblet cells may be involved in the malignant transformation of Barrett's esophagus.37 Griffel et al38 evaluated Das1, a murine monoclonal antibody that reacts with colonic but not jejunal, ileal, gastric or esophageal epithelium, in 29 samples of columnar-lined esophagus and found immunoexpression in 10 of 10 (100%) cases showing intestinal metaplasia and in five of 19 (26%) cases without goblet cells. They suggested that the phenotypic change of the columnar-lined esophagus to a colonic cell type precedes the morphologic changes identified by routine histology.38 It should be noted that SI, DPP and Das1 display a membranous or cytoplasmic staining pattern, whereas Cdx2 is characterized by a strong and high-quality nuclear localization, which is regarded as more reliable and easier to interpret.
In summary, this study showed that Cdx2 is a highly sensitive marker of intestinal (Barrett's) metaplasia of the esophagus and that it is expressed in a significant minority of cases of columnar-lined esophagus without goblet cells, suggesting that it may detect intestinal phenotypic modifications in the absence of goblet cells. Accordingly, Cdx2 immunostaining could be of value in identifying patients with Barrett's metaplasia when no goblet cells are found in biopsies from the columnar-lined esophagus. In addition, our study further confirmed that Barrett's-associated dysplasia has an intestinal phenotype and suggested that the ‘columnar blue cells’ are not diagnostic of intestinal metaplasia.
References
Hameeteman W, Tytgat GN, Houthoff HJ, et al. Barrett's esophagus: development of dysplasia and adenocarcinoma. Gastroenterology 1989;96:1249–1256.
McArdle JE, Lewin KJ, Randall G, et al. Distribution of dysplasias and early invasive carcinoma in Barrett's esophagus. Hum Pathol 1992;23:479–482.
Smith RR, Hamilton SR, Boitnott JK, et al. The spectrum of carcinoma arising in Barrett's esophagus. A clinicopathologic study of 26 patients. Am J Surg Pathol 1984;8:563–573.
Sampliner RE . Practice guidelines on the diagnosis, surveillance and therapy of Barrett's esophagus. Am J Gastroenterol 1998;93:1028–1031.
Weinstein WM, Ippoliti AF . The diagnosis of Barrett's esophagus: goblets, goblets, goblets. Gastrointest Endosc 1996;44:91–95.
Batts KP . Barrett's esophagus. More steps forward. Hum Pathol 2001;32:357–359.
Goldblum JR . Barrett's esophagus and Barrett's-related dysplasia. Mod Pathol 2003;16:316–324.
Blot WJ, Devesa SS, Kneller RW, et al. Rising incidence of adenocarcinoma of the esophagus and gastric cardia. JAMA 1991;265:1287–1289.
Devesa SS, Blot WJ, Fraumeni JF . Changing patterns in the incidence of esophageal and gastric carcinoma in the United States. Cancer 1988;83:2049–2053.
Vizcaino AP, Moreno V, Lambert R, et al. Time trends incidence of both major histologic types of esophageal carcinomas in selected countries. Int J Cancer 2002; 99:860–868.
Eloubeidi MA, Provenzale D . Does this patient have Barrett's esophagus? The utility of predicting Barrett's esophagus at the index endoscopy. Am J Gastroenterol 1999;94:937–943.
Coad RA, Shepherd NA . Barrett's oesophagus: definition, diagnosis and pathogenesis. Curr Diagn Pathol 2003;9:218–227.
Oberg S, Peters JH, DeMeester TR, et al. Inflammation and specialized intestinal metaplasia of cardiac mucosa: a manifestation of gastroesophageal reflux disease. Ann Surg 1997;226:522–532.
Chandrasoma PT, Der R, Dalton P, et al. Distribution and significance of epithelial types in columnar-lined esophagus. Am J Surg Pathol 2001;25:1188–1193.
Freund JN, Domon-Dell C, Kedinger M, et al. The Cdx-1 and Cdx-2 homeobox genes in the intestine. Biochem Cell Biol 1998;76:957–969.
James R, Erler T, Kazenwadel J . Structure of the murine homeobox gene cdx-2. Expression in embryonic and adult intestinal epithelium. J Biol Chem 1994;269:15229–15237.
Silberg DJ, Swain GP, Suth ER, et al. Cdx1 and Cdx2 expression during intestinal development. Gastroenterology 2000;119:961–971.
Suh E, Chen L, Taylor J, et al. A homeodomain protein related to caudal regulates intestine-specific gene transcription. Mol Cell Biol 1994;14:7340–7351.
Suh E, Traber PG . An intestine-specific homeobox gene regulates proliferation and differentiation. Mol Cell Biol 1996;16:619–625.
Almeida R, Silva E, Santos-Silva F, et al. Expression of intestine-specific transcription factors, CDX1 and CDX2, in intestinal metaplasia and gastric carcinomas. J Pathol 2003;199:36–40.
Bai Y-Q, Yamamoto H, Akiyama Y, et al. Ectopic expression of homeodomain protein CDX2 in intestinal metaplasia and carcinomas of the stomach. Cancer Lett 2002;176:147–155.
Barbareschi M, Murer B, Colby TV, et al. CDX-2 homeobox gene expression is a reliable marker of colorectal metastases to the lungs. Am J Surg Pathol 2003;27:141–149.
Eda A, Osawa H, Satoh K, et al. Aberrant expression of Cdx2 in Barrett's epithelium and inflammatory esophageal mucosa. J Gastroenterol 2003;38:14–22.
Moskaluk CA, Zhang H, Powell SM . Cdx2 protein expression in normal and malignant human tissues: an immunohistochemical survey using tissue microarrays. Mod Pathol 2003;16:913–919.
Phillips RW, Frierson HF, Moskaluk CA . Cdx2 as a marker of epithelial intestinal differentiation in the esophagus. Am J Surg Pathol 2003;27:1442–1447.
Seno H, Oshima M, Taniguchi MA, et al. CDX2 expression in the stomach with intestinal metaplasia and intestinal-type cancer: prognostic implications. Int J Oncol 2002;21:769–774.
Werling RW, Yaziji H, Bacchi CE, et al. CDX2, a highly sensitive and specific marker of adenocarcinomas of intestinal origin. An immunohistochemical survey of 476 primary and metastatic carcinomas. Am J Surg Pathol 2003;27:303–310.
Groisman GM, Meir A, Sabo E . The value of Cdx2 in differentiating primary ovarian carcinomas from colonic carcinomas metastatic to the ovaries. Int J Gynecol Pathol 2004;23:52–57.
Mizoshita T, Inada K, Tsukamoto T, et al. Expression of the intestine-specific transcription factors, Cdx1 and Cdx2, correlates shift to an intestinal phenotype in gastric cancer cells. J Cancer Res Clin Oncol 2004; 130:29–36.
Lee RG . Mucins in Barrett's esophagus: a histochemical study. Am J Clin Pathol 1984;81:500–503.
Peuchmaur M, Potet F, Goldfain D . Mucin histochemistry of the columnar epithelium of the esophagus (Barrett's esophagus): a prospective biopsy study. J Clin Pathol 1984;37:607–610.
Gottfried MR, McClave SA, Boyce HW . Incomplete intestinal metaplasia in the diagnosis of columnar lined esophagus. Am J Clin Pathol 1989;92:741–746.
Haggitt RC . Barrett's esophagus, dysplasia and adenocarcinoma. Hum Pathol 1994;25:982–993.
Silberg DB, Sullivan J, Kang E, et al. Cdx2 ectopic expression induces gastric intestinal metaplasia in transgenic mice. Gastroenterology 2002;122:689–696.
Mesquita P, Jonckheere N, Almeida R, et al. Human MUC2 mucin gene is transcriptionally regulated by Cdx homeodomain proteins in gastrointestinal carcinoma cells. J Biol Chem 2003;278:51549–51556.
Yamamoto H, Bai YQ, Yuasa Y . Homeodomain protein Cdx2 regulates goblet-specific MUC2 gene expression. Biochem Biophys Res Commun 2003;300:813–818.
Chaves P, Cardoso P, Mendes de Almeida JC, et al. Nongoblet cell population of Barrett's esophagus: an immunohistochemical demonstration of intestinal differentiation. Hum Pathol 1999;30:1291–1295.
Griffel LH, Amenta PS, Das KM . Use of a novel monoclonal antibody in diagnosis of Barrett's esophagus. Dig Dis Sci 2000;45:40–48.
Acknowledgements
We thank S Younes and A Atamna for technical assistance and E Eshkol and A Ehrlich for editing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was published in Abstract form in Mod Pathol 2004;17:116A, and presented in part at the Annual Meeting of the United States and Canadian Academy of Pathology, March 6–12, 2004, Vancouver, BC, Canada.
Rights and permissions
About this article
Cite this article
Groisman, G., Amar, M. & Meir, A. Expression of the intestinal marker Cdx2 in the columnar-lined esophagus with and without intestinal (Barrett's) metaplasia. Mod Pathol 17, 1282–1288 (2004). https://doi.org/10.1038/modpathol.3800182
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/modpathol.3800182
Keywords
This article is cited by
-
P63 Deficiency and CDX2 Overexpression Lead to Barrett’s-Like Metaplasia in Mouse Esophageal Epithelium
Digestive Diseases and Sciences (2021)
-
CDX-2 Expression in Esophageal Biopsies Without Goblet Cell Intestinal Metaplasia May Be Predictive of Barrett’s Esophagus
Digestive Diseases and Sciences (2020)
-
Histology of Barrett’s Metaplasia: Do Goblet Cells Matter?
Digestive Diseases and Sciences (2018)
-
Are Gastric and Esophageal Metaplasia Relatives? The Case for Barrett’s Stemming from SPEM
Digestive Diseases and Sciences (2018)
-
Reflux esophagitis and its role in the pathogenesis of Barrett’s metaplasia
Journal of Gastroenterology (2017)