Abstract
In Duchenne muscular dystrophy patients, the pathological hallmark of the disease, namely, the chronic accumulation of sclerotic scar tissue in the interstitial space of skeletal muscle is attributed to manifestation of secondary pathological processes. Such anomalous generation of matrix protein is thought to be driven by the continuous degeneration and regeneration of muscle both in Duchenne Muscular Dystrophy and in the mdx mouse homolog. We examined mdx and the control strain C57bl/10 mice over a range of ages with respect to the amounts of collagen present in muscles and other organs, finding that the mdx have significantly higher collagen content at later time points in their kidney and lung as well as their muscles. Surprisingly, when we bred the mdx mice on the nu/nu background, the time course of fibrogenesis was modified depending on the tissue and the collagen content was significantly different in age-matched mice. Transplantation of normal thymic tissue into the mdx-nu/nu mice replenished their T-cells and concomitantly altered the collagen content in their tissues to levels comparable with those in immunocompetent mdx mice. This suggests that T-cells play a role in the onset of the fibrotic events that undermines the ability of dystrophic muscle to regenerate.
Similar content being viewed by others
Introduction
Duchenne muscular dystrophy (DMD) was originally described as a myosclerosis (Duchenne, 1868), in recognition of the conspicuous deposition of collagenous scar tissue within the muscles. Fibrosis entails the excessive and inappropriate deposition of collagenous extracellular matrix. It is a central feature of many chronic diseases because it tends to disrupt and destroy the function of tissue, irrespective of the organ involved, be it kidney, heart, skin or skeletal muscle and is a major cause of suffering and death. It has also been suggested that this connective tissue proliferation may be important in the pathogenesis of the disease (Ionasecu and Ionasecu, 1982). Certainly, in primary myopathies such as Duchenne and congenital muscular dystrophies, striking increases in the levels of matrix proteins are a major histopathological feature (Stephens et al, 1982). In skeletal muscle, in addition to its obvious impact on the mechanical function of the tissue, progressive fibrosis may have widespread effects on a variety of mechanisms, which are crucial to the proper function of this tissue. Thus, the mechanisms of vascular and extravascular perfusion, which are critical for the supply of nutrients and removal of waste products in this metabolically active tissue, are likely to be compromised by the accumulation of dense, sclerotic scar tissue in the interfibre spaces. It has also been suggested that this scar tissue may itself assume a pathogenic role and contribute to the disease progression by interfering with effective muscle regeneration and re-innervation (Lipton, 1979).
Experimental investigation of dystrophinopathies has been rendered possible by the advent of authentic animal models of DMD, of which the mdx mouse is the most convenient and available. There has been much debate as to its faithfulness as a model of the human disease, largely around the point that the mouse is not notably clinically affected during the first 18 months of its life, although the same is true of DMD boys and it is not clear that such processes should be proportionalized to life span. Nonetheless, the lack of dystrophin in the mdx mouse leads to persistent necrosis of muscle fibres (Pagel and Partridge, 1999) much as in DMD with eventual onset of fibrosis, first in the diaphragm (Stedman et al, 1991) and, towards the end of the second year, in the limb muscles (Pastoret and Sebille, 1995).
Although little is known about the factors controlling the development and maintenance of muscle connective tissue, it has been suggested that the instability of dystrophic muscle due to the loss of dystrophin leads to the degeneration of muscle fibres with an invasion of inflammatory cells (Arahata and Engel, 1988) such as macrophages and T-lymphocytes. CD8+ cells are major constituents of the inflammatory cell population of dystrophic muscle (Emslie-Smith et al, 1989; McDouall et al, 1990) and these cells have been shown to be activated (Engel and Arahata, 1986). In dystrophic muscle, the finding of conserved amino acid sequence in the T-cell receptor (Gussoni et al, 1994), and increased expression of extracellular matrix ligands and receptors in the muscular tissue as well as draining lymph nodes (Lagrota-Candido et al, 1999) suggests an important role of T-cells in the pathophysiology of muscular dystrophy.
Although cytotoxic lymphocytes have been shown to contribute significantly to apoptosis and regeneration in the mdx mouse (Lagrota-Candido et al, 1999; Spencer et al, 1997), little is known about the contribution of T-lymphocytes to the progressive fibrogenesis that occurs during the repeated degeneration and regeneration of the mdx muscle.
Here, we report our finding on fibrogenesis over much of the lifespan of mdx and mdx bred onto the nu/nu background. We find that the absence of T-lymphocytes markedly delayed the onset of collagen deposition in skeletal muscles and some visceral organs of the mdx mouse.
Results
Effect of Age on the Hydroxyproline Levels on mdx and C57bl/10 Mice
Four muscles: diaphragm, heart, tibialis anterior (TA) and soleus, as well as two visceral organs; lung and kidney were selected for measurement of the accumulation of collagen with increasing age in mdx compared with C57bl/10 control mice. The hydroxyproline content normalized against total protein content showed an overall tendency to increase with age, in the mdx tissues (Figure 1). The diaphragm showed a consistent and progressive increase with age, reaching significance at 24 and 88 weeks (p < 0.001 and p < 0.02, respectively). In contrast, the heart, soleus and TA showed a dramatic rise at 88 weeks compared to earlier time points. However, the mdx soleus at early age, 3 and 12 weeks contained a significantly lower level of hydroxyproline when compared with control muscle (p < 0.02 for both points).
Histogram demonstrating the levels of hydroxyproline with increasing age in mdx compared with C57bl/10 control mice. Most tissues assayed showed a significant increase by 88 weeks in mdx compared to control mice. The diaphragm results illustrate the build up of matrix protein compared to other muscles. In contrast, the soleus shows a significant decrease in hydroxyproline content at the early ages when compared with control mice. However, this finding is reversed in later months (Nine mdx mice were used for each time point except for 24 and 88 weeks, where 12 and 6 mice were used, respectively. Six C57bl/10 mice were used for each time point except for 88 weeks, where 3 mice were used). Data is expressed as means and sem. *denotes significance between mdx and control C57bl/10.
A surprising finding was the tendency for higher hydroxyproline content in mdx lung and kidney compared with control C57bl/10. The lung showed a general steady increase with age in both mdx and control mice but tended to be higher in mdx and was significantly so at 24 weeks (p < 0.04). The kidney mirrored the levels in the heart and limb muscles with a sudden increase at 88 weeks compared to control (p < 0.02).
Immunolabelling of Matrix Proteins in Diaphragms of Old Mice
Since the diaphragm was found to be the most affected organ with the highest level of hydroxyproline, we carried out an immunolabelling study to identify the common components of the matrix present in the fibrosing muscle. This is shown in Figure 2 using van Gieson staining of frozen sections at 88 weeks. mdx diaphragm reveals the extensive loss of fibers and the accumulation of matrix compared with control. Further immunolabelling of matrix proteins reveals that the interstitial space is filled with fibronectin, collagens type I and III.
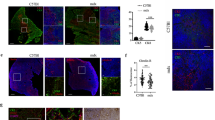
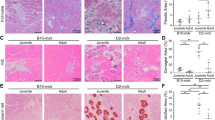
Photomicrographs illustrating the deposition of matrix proteins in diaphragms of 88 week old mdx (a, c, e and g) and C57bl/10 (b, d, f and h) mouse. The Verhoeff/van Gieson staining (a and b) demonstrating the fibre loss and extracellular matrix build up (pink/red)in the mdx, compared with C57bl/10. Specific immunoperoxidase labeling reveals the presence of substantially higher levels of collagen type I (c and d), type III (e and f), and fibronectin (g and h) staining in the old mdx compared with C57bl/10. Original Magnification × 200.
Difference in Hydroxyproline Levels Between mdx and mdx-nu/nu Mice
Organs were removed from mdx-nu/nu mice as outlined in the previous experiment for mdx and C57bl/10 mice except for the 88 weeks time point because the mdx-nu/nu mice are severely ill at that stage.
The hydroxyproline content measured in the mdx-nu/nu diaphragm and heart did not mimic the results obtained in the equivalent mdx muscle. On the contrary, there was a significantly less hydroxyproline content at 24 weeks compared with mdx (p < 0.04, p < 0.007, respectively; Figure 3). In contrast, the hydroxyproline content at three weeks of age in the soleus and TA of mdx-nu/nu were significantly increased compared with mdx, p < 0.0001 and p < 0.001, respectively. This latter result was surprising and was repeated and confirmed in a further 7 animals. No difference was seen between the mdx-nu/nu lung and kidney compared with mdx tissues.
Histogram demonstrating the levels of hydroxyproline with increasing age in mdx compared with mdx-nu/nu mice. Differences can be seen between the tissues assayed. Significant decrease in the hydroxyproline content is found in the diaphragm and heart of mdx–nu/nu compared with mdx. Of equal interest is the dramatic increase of hydroxyproline in the soleus and TA of the mdx-nu/nu at the earlier ages when compared with mdx. No significant change was seen in lung and kidney. (Nine mdx-nu/nu were used for each time point except for 3 weeks, where 16 mice were used to the soleus and TA samples. The numbers of mdx mice used was the same as in Figure 1) Data is expressed as means and sem. *denotes significance between mdx and mdx-nu/nu
Histological Analysis of mdx, mdx-nu/nu, and C57bl/10 Mice
Frozen sections of diaphragm from 24 week old mdx, mdx-nu/nu and control mice were stained with Verhoeff’s and van Gieson showing a notable increase in matrix deposition in mdx tissue compared to mdx-nu/nu and C57bl/10 control mice (Figure 4).
Photomicrographs showing the difference in matrix build up at 24 weeks old mdx compared with mdx-nu/nu and control C57bl/10. Note the substantial increase in van Gieson stain (pink/red) in the diaphragm of the mdx mouse compared with age-matched mdx-nu/nu and C57bl/10 mice. Original Magnification × 100.
Increased Hydroxyproline Levels in the T-cell Reconstituted mdx-nu/nude Mice
FACS analysis showed that mdx-nu/nu mice have neither CD4 nor CD8 cell populations (Figure 5). However, the thymus- transplanted mdx-nu/nu mice, examined at nine weeks after transplantation, showed a T-cell profile similar to that of immunocompetent mice. Similar results were obtained 21 weeks after thymus transplantation (data not shown).
Tissues from the reconstituted mice were removed and assayed for hydroxyproline content and compared with similarly aged mdx and mdx-nu/nu. The results were compared to 12 and 24 week old mdx and mdx-nu/nu. Interestingly, the hydroxyproline content of T-cell reconstituted mdx-nu/nu was comparable to that in mdx by 12 weeks in the diaphragm and the TA but declined by 24 weeks to become indistinguishable from the content in muscles of non-reconstituted mdx-nu/nu mice (Figure 6). By contrast, the heart and the soleus muscles showed an inverse pattern, being unaffected in the T-cell reconstituted muscles at 12 weeks but raised to the same levels as mdx mice by 24 weeks, where the heart in the T-cell reconstituted mice showed a significant increase compared with mdx-nu/nu (p < 0.05). The lung and the kidney showed no significant difference in the reconstituted animals at either 12 or 24 weeks of age.
Histogram demonstrating the effect of restoring T-cells to the mdx-nu/nu mice on the hydroxyproline content of the diaphragm, TA, soleus, heart, lung and kidney at twelve (n = 3) and at twenty-four weeks (n = 3). Data is expressed as means and sem showing a general increase in hydroxyproline specific activity between T cell reconstituted and mdx-nu/nu mice. The level of significance is noted in the heart at 24 weeks (*p < 0.05).
Discussion
In this study, we examined the extent of fibrosis in the mdx mouse in both muscle and other tissues and compared them with control C57b/l10 as well as with mdx mice bred onto a nude background (mdx-nu/nu).
Three main points of interest emerge from this study:
More Collagenous Extracellular Matrix is Deposited in mdx Tissues than Control C57Bl/10 Mice, Including Nonmuscle Tissues
A progressive increase was noted in hydroxyproline levels in mdx diaphragm and to a lesser extent in kidney and lung, compared with control mice. Immunostaining of the old mdx diaphragm showed more fibronectin and collagens type I and III, but no difference was noted for type iv collagen (data not shown). Early changes in the diaphragm were first reported by Stedman (Stedman et al, 1991), but the accumulation of collagen in the heart, although reported histologically has not previously been measured. The early appearance of pathological changes in these tissues in the mdx mouse may parallel the failure in respiratory function that is a frequent cause of death in DMD.
Not all skeletal muscles exhibited this rapid accumulation of hydroxyproline. In the heart and skeletal muscles of the limbs such as the soleus and TA, no difference in amounts of hydroxyproline were seen until 88 weeks, at which time a sudden increase was noted. We were surprised to find that the hydroxyproline content of the soleus muscle in all strains was, on average, two to three times higher than other skeletal muscle, in the same mouse. Why this should be the case is not known and this finding, to our knowledge, has not been reported before. This fibrotic aspect of the disease has been alluded to in several publications (Grounds, 1991; Stephens et al, 1982) but forgotten in the search for therapeutic strategies over recent years. Instead, identification of the dystrophin gene as the site of the primary genetic defect (Hoffman et al, 1987) has concentrated efforts on correction or compensation of the biochemical defect in the muscle fibre, largely to the neglect of possibilities for intervention at points further down the pathological cascade.
The high level of hydroxyproline in kidney and lung of the mdx mice compared to control mice is of particular interest. Increased collagen accumulation in a tissue that does not contain significant amounts of skeletal muscle points to a systemic stimulus to fibrosis, which may be triggered in the muscle but may be cytokine driven and spread via the vasculature.
Mdx-nu/nu Tissues Show Different Patterns of Collagen Deposition from the Equivalent Tissue in mdx Mice
Lack of a functional T cell repertoire in the nude mouse is due to abnormal development of the thymic stroma that is essential for T cell development and education (Nehls et al, 1994). We had not anticipated that mdx on the nude background would exhibit major differences in the production of fibrous tissue. However, our data clearly show two significant effects of the nude background on the hydroxyproline content of tissues. The more explicable of these is a marked reduction or delay in the deposition of matrix in the diaphragm and heart of mdx-nu/nu by comparison with mdx mice.
This finding is consistent with some previous studies using congenitally T-cell deficient mice as models to address the role of cell mediated immunity in other fibrotic diseases. For example, in a model of pulmonary fibrosis induced by bleomycin, lungs of nude or T lymphocyte-depleted rats, contained less hydroxyproline than those of normal bleomycin-treated rats (Schrier et al, 1983; Thrall et al, 1980). Similar results were obtained with silica-induced pulmonary fibrosis (Suzuki et al, 1996). However, other investigations show great variability between experimental models (Corsini et al, 1994; Hyde et al, 1988; Schrier and Phan, 1984) depending on the animal species, strain, tissue examined and fibrogenic agent used. Even within a single experimental model, the ‘tight skin’ mouse, skin fibrosis was reduced when it was bred onto a CD4-/- background but the lung pathology was not affected (Wallace et al, 1994), suggesting that the T cell contribution to fibrogenesis is pleiotropic.
Running against the general trend of our observations, was the 3-fold higher hydroxyproline content of TA and soleus seen in the young (3 weeks) mdx-nu/nu mice than in either C57 or mdx mice. This was a most surprising result, which we have confirmed in 18 day old mice, but for which we currently have no explanation. It is limited to the limb muscles, not appearing in the diaphragm, and occurs at or before the onset of the dystrophinopathy in these animals, making it difficult to explain in terms of the disease. Furthermore, we see no conspicuous histological correlate of the biochemical measures. This phenomenon is phasic, returning to normal levels by 3 and 6 months of age, at which times the diaphragm shows marked elevations in hydroxyproline levels. Because these observations appear to be quite unrelated to the increased fibrosis in immunocompetent mdx mice seen in diaphragm and heart at 6 months and, in the limb muscles, by 22 months, it is the subject of further investigation.
Repopulation of mdx-nu/nude Mice with T-cells Restores Excessive Accumulation of Collagen
In order to evaluate the direct role of T-cells in matrix deposition, we grafted mdx-nu/nu mice with thymi from their non-nude littermates. This resulted in the generation of approximately normal numbers of T cells in the circulation of these mice (Figure 5), perhaps by expansion of lymphocytes from the graft, perhaps by re-education of the population of naïve endogenous lymphocytes. When T-cells were reconstituted in the mdx-nu/nu, the results showed a trend of increased matrix accumulation in different muscles, at different time after transplantation, but not in lung and kidney (Figure 6). This suggests that T-cells have a direct role in the development of fibrosis in the mdx mouse.
In vitro, T cells have been shown to modulate fibroblast proliferation and secretion of matrix proteins (Postlethwaite, 1995). Soluble factors have been implicated the promotion of collagen gene expression in some studies (Ichiki et al, 1997; Kovacs and Dipetro, 1994; Postlethwaite et al, 1992; Wahl and Gately, 1983) however, direct contact between lymphocytes and fibroblasts has also been shown to suppress collagen production (Chizzolini et al, 1998; Rezzonico et al, 1998).
In vivo, the major phase of inflammation in dystrophic mdx muscle occurs prior to the detection of increases in collagen content. Numerous T-cells invade the mdx muscle during the first few weeks of the myopathy but return to normal by three months of age (Spencer et al, 1997). By contrast, we find a progressive increase in collagen with age in the majority of muscles, extending well beyond this 3 months period, most of it occurring in the second year. This suggests that activation of the matrix-producing cells in the muscle is not dependent on continuous contact with lymphocytes. Support for the idea of a soluble fibrogenic stimulus is the finding that non-muscle organs such as kidney and lung show an increased level of collagen with age. The simplest explanation is that the inflammatory cells invading dystrophic skeletal muscle during degeneration, secrete soluble factors which influence the local environment and also have a systemic effect as shown here in the mdx mouse.
Whether a certain sub-set of T-cells is involved in this increase in fibrosis, and whether the T-cells produced are derived from the host animal or are due to the transfer of lymphocytes during the thymus transplantation require further investigation and are subjects of our current investigation. Furthermore, the inverse relationship between the diaphragm and the TA, on one hand, and the heart and soleus, on the other, may reflect differences in accessibility of these muscles to T-cells or cytokines, or to intrinsic differences in the mechanism driving fibrogenesis in these muscles. We and others have shown that collagen genes contain tissue-specific elements that regulate expression during development and in response to injury (Bou-Gharios et al, 1996; Braghetta et al, 1996; Rossert et al, 1995), it is likely that cis–acting elements will vary between muscles. Moreover, these genes are also regulated by the response to various cytokines, including those secreted by T-cells such as TGFβ (Inagaki et al, 1994), TNF-α (Inagaki et al, 1995; Solis-Herruzo et al, 1988), IL-1 (Goldring and Krane, 1987) and IL-4 (Postlethwaite et al, 1992) etc. These may be differentially expressed, at different times, and in different muscles.
The cellular mechanisms and the cascade of events leading to fibroblast differentiation in fibrosis and the subsequent overproduction of matrix proteins are still poorly defined. In man, fibrosis poses clinical problems mainly in association with chronic disease, whereas the general run of animal models of fibrosis are driven by acute stimuli. It is important, therefore, that the mdx mouse exhibits an endogenously evoked chronic degeneration that drives a complex pattern of fibrosis, making it of particular value as a model system. Our findings that the excessive accumulation of collagen involves interactions between T-cells and this chronic disease, further raises its status as a model relevant to human disease, for in the mouse, subtle experimental manipulation of the immune system and of associated cytokine production should permit intricate dissection of the role of these mechanisms in skeletal muscle fibrosis.
Materials and Methods
Animals and Processing of Samples
Mdx and C57bl/10 mice were used at three, twelve, twenty-four and eighty eight weeks of age. Mdx-nu/nu mice were used at three, twelve and twenty four weeks of age but not eighty-eight weeks because these animals do not remain healthy beyond a year of age.
At least three mice were examined from each strain of mice, at any time point but the total number varied as indicated in the results. At each time point, the mice were humanely killed by cervical dislocation. The heart, diaphragm, soleus, TA, lung and kidney were quickly dissected, weighed and placed into 3 ml of 0.1M KCl/0.02M Tris (pH 7.6) buffer and kept on ice. The samples were homogenized, divided into 1 ml aliquots and stored at −80° C until measurement of the hydroxyproline and protein content. The contralateral muscle or a piece of the organ taken was mounted on cork using Gum Tragacanth (Sigma G-1128) and snap frozen in isopentane, cooled to freezing point in liquid nitrogen. The blocks were stored at −80° C, prior to sectioning.
Determination of Hydroxyproline Level
The method described by Woessner (Woessner, 1961) as modified by the Clinical Chemistry Department at Hammersmith Hospital, London (unpublished) was used. Briefly, 1 ml of homogenate obtained above was added to 2 ml of Amberlite resin suspension (Sigma I-6641) which had been previously treated with 2M HCl and dried overnight at 50° C. The resin was washed with 7 ml of water and vortexed for ten seconds. The samples were centrifuged at 270g. for five minutes. The supernatant was discarded and tubes were capped tightly and placed in an oven at 105–110° C overnight. After allowing the tubes to cool to room temperature, 5 ml of elution buffer pH 6.0 (34.4g sodium acetate anhydrous (Sigma S-2889), 37.5g trisodium citrate dihydrate (Sigma C-8532) and 5.5g citric acid monohydrate (Sigma C-7129) dissolved in one litre of distilled water and the pH adjusted to 6.0, was added to the tubes, vortexed for fifteen seconds and centrifuged at 270g. for ten minutes.
An aliquot of the supernatant (0.5 ml) was added to 1 ml of isopropanol (Sigma I-9516) in a test tube and 0.5 ml of freshly prepared 1.4% chloramine-T (Sigma C9887-made up in 35 ml elution buffer and 15 ml isopropanol) was added and left for 5 minutes before the addition of 5 ml of color reagent (5% 4-dimethylaminobenzaldehyde (Sigma D2004) dissolved in 50 ml of 18.9% perchloric acid (Fluka 77230) and 450 ml isopropanol). After vigorous mixing between all additions, the tubes were heated at 60° C for twenty minutes and then allowed to cool at room temperature. The samples absorbance were then read at 560 nm. A standard curve was run along side the samples using trans-4-HYDROXY-l-PROLINE (Sigma H-6002 Poole, UK) to determine hydroxyproline concentration.
Determination of Protein Content
Protein content was determined using a BCA Assay Kit (PIERCE 23225) and carried out according to the instruction leaflet with the reagents. The samples were diluted accordingly in order to fit within the range of an albumin standard curve.
Immunolabelling of Tissues with Antibodies Against Matrix Proteins
Immunolabelling for matrix proteins was carried out on 8-μm thick unfixed cryostat sections, which were initially blocked for one hour with 10% Normal Swine Serum (Dako × 0901). The sections were incubated for two hours with primary antisera; Rabbit anti- murine fibronectin (Biogenesis 4470–4304), Rabbit anti -mouse collagen type I and rabbit anti- collagen type III (TCS biological, UK). The sections were washed three times with Tris buffered saline, followed by a forty-five minutes incubation with the secondary biotinylated swine anti-Rabbit IgG (Dako E0353). The sections were then washed in Tris buffered saline containing 2.5% Hydrogen Peroxide (30% w/v) to remove any endogenous peroxidase and incubated with streptavidin Horseradish Peroxidase (Dako P0397) for forty-five minutes. Color was developed with Diaminobenzidine and hydrogen peroxide tablets (Sigma D4293). Incubations were performed in a humid chamber at room temperature. Sections were mounted and observed with a light microscope. Adjacent sections were also stained with Verhoeff’s and van Gieson stain (Dubowitz, 1985), which colours the collagen red, nuclei brown, nerves in black and the surrounding tissue green-brown.
Grafting of Thymi into mdx-nu/nu Mice
Three week old mdx-nu/nu mice were anaesthetized with 50 μl Hypnorm (Janssen Animal Health): Hypnovel (Roche): Water; 1:1:2. Hairy mdx littermates were humanely killed by cervical dislocation and the thymi were carefully dissected, cut into several pieces and placed in 5 ml of Dulbeccos Modified Eagles Medium (DMEM). Mdx-nu/nu mice were anaesthetized using a combination of hypnorm and hypnovel (Gross and Morgan, 1999), and the body wall was cut to expose the kidney. A small incision was made in the kidney capsule and several small pieces of thymus were placed under the kidney capsule. Larger pieces were placed between the skin and body wall musculature. The mice were sutured and allowed to recover on a warm pad. Three mice were taken at two time points, twelve and twenty-four weeks, and their muscles and other organs were analyzed for hydroxyproline content.
FACS Analysis of T Lymphocytes
The thymus transplanted mdx/nude mice were bled from the tail tip into an eppendorf containing 0.5 ml PBS, 20U heparin and 2% fetal calf serum (approximately 4–5 drops per mouse). The suspension was underlayed with 0.3 ml of ficoll-paque (Pharmacia Biotech 17–0840-02) and spun at 400g for fifteen minutes at room temperature. The lymphocytes were removed from the interface and placed into an allocated well of a 96-well microtitre plate. The cells were centrifuged and washed with 0.2 ml of PBS with 2% fetal calf serum. The antibody solution containing two directly labeled antibodies against anti-mouse CD8a (Ly-2) R-PE (PharMingen 01045B) and anti-mouse CD4 (L3T4) FITC (PharMingen 01064A) was added to the cells and incubated at room temperature for fifteen minutes. The cells were washed several times, resuspended in approximately 25 μl of buffer and analyzed on a flow cytometer.
Spleen lymphocytes were harvested by sieving through a 40 μm nylon mesh with 20% fetal calf serum. The cell suspension was centrifuged at 350 xg for ten minutes at 4° C. The cells were resuspended in 20 ml of 20% fetal calf serum and counted. A cell suspension of 5 × 105 was centrifuged as described above to isolate T cells which were immunolabelled and analyzed using a flow cytometer.
References
Arahata K and Engel AG (1988). Monoclonal antibody analysis of mononuclear cells in myopathies IV. Cell mediated cytotoxicity and muscle fiber necrosis. Ann Neurol 23:168–173.
Bou-Gharios G, Garrett L-A, Rossert J, Niederreither K, Eberspeacher H, Smith C, Black C, and De Crombrugghe B (1996). A potent far-upstream enhancer in the mouse pro-α2(1) collagen gene regulates expression of reporter genes in transgenic mice. J Cell Biol 134:1333–1344.
Braghetta P, Fabbro C, Piccolo S, Marvulli D, Bonaldo P, Volpin D, and Bressan GM (1996). Distinct regions control transcriptional activation of the α1(V1) collagen promoter in different tissue of transgenic mice. J Cell Biol 135:1163–1177.
Chizzolini C, Rezzonico R, Ribbens C, Burger D, Wollheim FA, and Dayer J-M (1998). Inhibition of type 1 collagen production by dermal fibroblasts upon contact with activated T cells. Arth & Rheum 41:2039–2047.
Corsini E, Luster MI, Mahler J, Craig WA, Blazka ME, and Rosenthal GJ (1994). A protective role for T lymphocytes in asbestos-induced pulmonary inflammtion and collagen deposition. J Respir Cell Mol Biol 11:531–539.
Dubowitz V (1985). Muscle Biopsy: A practical approach. London:Eastbourne Bailliere Tindall.
Duchenne GB (1868). Recherches sur la paralysie musculaire pseudohypertrophique ou la paralysie myo-sclerotique. Archives Generales de Medicine 11:5–25.
Emslie-Smith AM, Arahata K, and Engel A (1989). Major histocompatibility complex class I antigen expression, immunolocalization of interferon subtypes and t cell-mediated cytotoxicity in myopathies. Hum Pathol 20:224–231.
Engel AG and Arahata K (1986). Mononuclear cells in myopathies. Hum Pathol 17:704–721.
Goldring M and Krane S (1987). Modulation by recombinant interleukin 1 of synthesis of types I and III collagens and associated procollagen mRNA levels in cultured human cells. J Biol Chem 262:16724–16729.
Gross JG and Morgan JE (1999). Muscle precursor cells injected into irradiated mdx mouse muscle persist after serial injury. Muscle & Nerve 22:174–185.
Grounds MD (1991). Towards understanding skeletal-muscle regeneration. Pathol Res Pract 187:1–22.
Gussoni E, Pavlath GK, Miller RG, Panzara MA, Powell M, Blau HM, and Steinman L (1994). Specific T cell receptor gene rearrangements at the site of muscle degeneration in Duchenne muscular dystrophy. J Immunol 153:4798–4805.
Hoffman EP, Brown RJ, and Kunkel LM (1987). Dystrophin: The protein product of the Duchenne muscular dystrophy locus. Cell 51:919–928.
Hyde DM, Henderson TS, Giri SN, Tyler NK, and Stovall MY (1988). Effect of murine gamma interferon on the cellular response to bleomycin in mice. Exp Lung Res 14:687–704.
Ichiki Y, Smith EA, Leroy EC, and Trojanowska M (1997). Basic fibroblast growth factor inhibits basal and transforming growth factor-β induced collagen α 2 (I) gene expression in scleroderma and normal fibroblasts. J Rheumatol 24:90–95.
Inagaki Y, Truter S, and Ramirez F (1994). Transforming growth factor-beta stimulates alpha 2(I) collagen gene expression through a cis-acting element that contains an Sp1-binding site. J Biol Chem 263:5841–5845.
Inagaki Y, Truter S, Tanaka S, Di Liberto M, and Ramirez F (1995). Overlapping pathways mediate the opposing actions of tumor necrosis factor-alpha and transforming growth factor-beta on alpha 2 (I) collagen gene transcription. J Biol Chem 262:3353–3358.
Ionasecu V and Ionasecu R (1982). Increased collagen synthesis by Duchenne myogenic clones. J Neurol Sci 54:79–87.
Kovacs EJ and Dipetro LA (1994). Fibrogenic cytokines and connective tissue production. FASEB J 8:854–861.
Lagrota-Candido J, Canella I, Savino W, and Quirico-Santos T (1999). Expression of extracellular matrix ligands and receptors in the muscular tissue and draining lymph nodes of mdx dystrophic mice. Clin Immunol 93:143–151.
Lipton BH (1979). Skeletal muscle regeneration in muscular dystrophy. In: Mauro A, editor. Muscle Regeneration. New York:Raven Press, 31–40.
McDouall RM, Dunn M, and Dubowitz V (1990). Nature of the mononuclear infiltrate and the mechanism of muscle damage in juvenile desmatonyositis and Duchenne muscular dystrophy. J Neurol Sci 99:199–217.
Nehls M, Pfeifer D, Schorpp M, Hedrich H, and Boehm T (1994). New members of the winged-helix protein family disrupted in mouse and rat nude mutations. Nature 372:103–107.
Pagel C and Partridge TA (1999). Covert persistence of mdx mouse myopathy is revealed by acute and chronic effects of irradiation. J Neurol Sci 164:103–116.
Pastoret C and Sebille A (1995). mdx mice show progressive weakness and muscle deterioration with age. J Neurol Sci 129:97–105.
Postlethwaite AE (1995). Role of T cells and cytokines in effecting fibrosis. Intern Rev Immunol 12:247–258.
Postlethwaite AE, Holness MA, Katai H, and Raghow R (1992). Human fibroblasts synthesize elevated levels of extracellular matrix proteins in response to Interleukin 4. J Clin Invest 90:1479–1485.
Rezzonico R, Burger D, and Dayer J-M (1998). Direct contact between T lymphocytes and human dermal fibroblasts or synoviocytes down-regulates types I and III collagen production via cell-associated cytokines. J Bio Chem 273:18720–18728.
Rossert J, Eberspaecher H, and de Crombrugghe B (1995). Separate cis-acting DNA elements of the mouse pro-α1(I) collagen promotor direct expression of reporter genes to different type I collagen-producing cells in transgenic mice. J Cell Biol 129:1421–1432.
Schrier DJ and Phan SH (1984). Modulation of bleomycin-induced pulmonary fibrosis in the BALB/c mouse by cyclophosphamide-sensitive T cells. Am J Pathol 116:270–278.
Schrier DJ, Phan SH, and McGarry BM (1983). The effects of the nude (nu/nu) mutation on bleomycin-induced pulmonary fibrosis. A biochemical evaluation. Am Rev Respir Dis 127:614–617.
Solis-Herruzo JA, Brenner DA, and Chojkier M (1988). Tumor necrosis factor alpha inhibits collagen gene transcription and collagen synthesis in cultured human fibroblasts. J Biol Chem 263:5841–5845.
Spencer M, Walsh C, Dorshkind K, Rodriguez E, and Tidball J (1997). Myonuclear apoptosis in dystrophic MDX muscle occurs by perforin-mediated cytotoxicity. J Clin Invest 99:2745–2751.
Stedman HH, Sweeney HL, Shrager JB, Maguire HC, Panettieri RA, Petrof B, Narusawa M, Leferovich JM, Sladky JT, and Kelly AM (1991). The mdx mouse diaphragm reproduces the degenerative changes of Duchenne muscular dystrophy. Nature 352:536–539.
Stephens HR, Duance VC, Dunn MJ, Bailey AJ, and Dubowitz V (1982). Collagen types in neuromuscular diseases. J Neurol Sci 53:45–62.
Suzuki N, Ohta K, Horiuchi H, Ueda T, Kuwabara M, Shiga J, and Ito K (1996). T lymphocytes and silica-induced pulmonary inflammation and fibrosis in mice. Thorax 51:1036–1042.
Thrall RS, Lovett EJ, Barton RW, McCornick JR, Phan SH, and Ward PA (1980). The effect of T-cell depletion on the development of bleomycin-induced pulmonary fibrosis in the rat. Am Rev Respir Dis 121:99–101.
Wahl SM and Gately CL (1983). Modulation of fibroblast growth by a lymphokine of human T cell continuous T cell line origin. J Immunol 130:1226–1230.
Wallace VA, Kondo S, Kono T, Xing Z, Timms E, Furlonger C, Keystone E, Gauldie J, Saunder DN, Mak TW, and Paige CJ (1994). A role for CD4+ cells in the pathogenesis of skin fibrosis in tight skin mice. Eur J Immunol 24:1463–1466.
Woessner JF (1961). The determination of hydroxyproline in tissue and protein samples containing small proportions of this amino acid. Arch Biochem Biophys 93:440–447.
Acknowledgements
This work was supported by the Medical Research Council of Great Britain and a grant from Muscular Dystrophy Campaign. The authors are grateful to Dr Matthias Merkenschlager for FACS and helpful discussions and Graham Reed for photographic reproduction.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morrison, J., Lu, Q., Pastoret, C. et al. T-Cell-Dependent Fibrosis in the mdx Dystrophic Mouse. Lab Invest 80, 881–891 (2000). https://doi.org/10.1038/labinvest.3780092
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3780092
This article is cited by
-
Origins, potency, and heterogeneity of skeletal muscle fibro-adipogenic progenitors—time for new definitions
Skeletal Muscle (2021)
-
Defective dystrophic thymus determines degenerative changes in skeletal muscle
Nature Communications (2021)
-
The linkage between inflammation and fibrosis in muscular dystrophies: The axis autotaxin–lysophosphatidic acid as a new therapeutic target?
Journal of Cell Communication and Signaling (2021)
-
Skeletal muscle cell transplantation: models and methods
Journal of Muscle Research and Cell Motility (2020)
-
Glycine administration attenuates progression of dystrophic pathology in prednisolone-treated dystrophin/utrophin null mice
Scientific Reports (2019)