Abstract
In previous studies, we have demonstrated that human heparanase (endo-β-D-glucuronidase) is localized primarily in a perinuclear pattern within lysosomes and late endosomes, and occasionally may be surface associated and secreted. The presence of two potential nuclear localization sequences in human heparanase, led us to investigate heparanase translocation into the nucleus and subsequent degradation of nuclear heparan sulfate. Applying cell fractionation, Western blot analysis, determination of heparanase activity and confocal microscopy, we identified heparanase within the nuclei of human glioma and breast carcinoma cells and estimated its amount to be about 7% of the cytosolic enzyme. Our results indicate that nuclear heparanase colocalizes with nuclear heparan sulfate and is enzymaticaly active. Moreover, following uptake of latent 65 kDa heparanase by cells that do not express the enzyme, an active 50 kDa heparanase was detected in the cell nucleus, capable of degrading both nuclear and extracellular matrix-derived heparan sulfate. Immunohistochemical examination of human squamous cell carcinoma specimens revealed a prominent granular staining of heparanase within the nuclei of the epithelial tumor cells vs no nuclear staining in the adjacent stromal cells. Taken together, it appears that heparanase is translocated into the cell nucleus where it may degrade the nuclear heparan sulfate and thereby affect nuclear functions that are thought to be regulated by heparan sulfate. Nuclear localization of heparanase suggests that the enzyme may fulfill nontraditional functions (ie, regulation of gene expression and signal transduction) apart of its well-documented involvement in cancer metastasis, angiogenesis and inflammation.
Similar content being viewed by others
Main
Heparan sulfate proteoglycans (HSPGs) in the basement membrane (BM), extracellular matrix (ECM) and cell surfaces affect biological processes by interacting with various ECM constituents and a large number of biologically active molecules.1, 2 HSPGs thus influence a variety of normal and pathological processes involving cell adhesion, migration and invasion.1, 2, 3, 4 Although presence of HSPGs in the cell nucleus has long been reported,5, 6, 7 their biological significance was not clearly elucidated. Several studies have demonstrated the involvement of HS in internalization and nuclear uptake of FGF-1 and FGF-2.7, 8, 9 In view of their abundance and importance in cell and tissue physiology, enzymatic degradation of HS is likely to be involved in fundamental biological processes ranging from pregnancy, morphogenesis and normal development to inflammation, angiogenesis and cancer metastasis.10, 11, 12, 13, 14
Mammalian endoglycosidase (heparanase), capable of partially depolymerizing HS chains, has been identified in highly invasive normal and malignant cells, including cytotrophoblasts, activated cells of the immune system, lymphoma, melanoma and carcinoma cells.12, 13, 14, 15, 16 The full-length 65 kDa heparanase proenzyme undergoes proteolytic processing, yielding an active heterodimer enzyme composed of 50 and 8 kDa polypeptides.17, 18 Expression of heparanase has been correlated with the metastatic potential of tumor cells, and treatment with heparanase inhibitors markedly reduced the incidence of experimental metastasis and autoimmunity.12, 13, 14, 16, 19, 20 Moreover, enhanced heparanase expression correlates with shorter postoperative survival of cancer patients.21, 22, 23 Apart from its involvement in the egress of cells from the vasculature, heparanase is tightly involved in normal and pathological angiogenesis, primarily by means of releasing heparin-binding angiogenic factors sequestered by HS in the BM and ECM.13, 24, 25, 26, 27
In previous studies, we have demonstrated that human heparanase is localized primarily in a perinuclear pattern within lysosomes and late endosomes.28, 29 and occasionally may be surface associated and secreted.27, 30, 31, 32 In view of the accumulating data on the occurrence of nuclear HSPGs and the presence of two potential nuclear localization signals (residues 271–277; PRRKTAK, and 427–430; KRRK) in human heparanase (H-hpa), we investigated whether endogenous or exogenously added heparanase is translocated into the nucleus and whether nuclear HS is accessible to degradation by the enzyme. Applying cell fractionation, Western blot analysis and confocal microscopy, we have identified heparanase within the cell nucleus and demonstrated that the enzyme is capable of degrading nuclear HS. Moreover, following uptake of latent 65 kDa heparanase by heparanase negative rat or human glioma cells, both the latent and active 50 kDa enzymes were detected in the cell cytoplasm and nucleus. Heparanase activity was readily observed in the nuclear fraction of cells that internalized the enzyme, but not of control cells. Nuclear heparanase was also detected in specimens of human squamous cell carcinoma. Taken together, we propose that following uptake and translocation, heparanase resides in the cell nucleus where it may degrade nuclear HS and affect nuclear functions (ie, gene transcription), independent of its well-established involvement in ECM degradation and related effects on cell invasion and response to changes in the extracellular microenvironment.
Materials and methods
Cells
MDA-435 human breast carcinoma, U87 human glioma, and C6 rat glioma cells were cultured in DMEM (4.5 g glucose/l) supplemented with 10% FCS and antibiotics. Cultures of bovine corneal endothelial cells were established from steer eyes and maintained in DMEM (1 g glucose/l) supplemented with 5% newborn calf serum, 10% FCS and 1 ng/ml bFGF, as described.33 Confluent cells were dissociated with 0.05% trypsin and 0.02% EDTA and subcultured at a split ratio of 1:10.33
Antibodies
Monoclonal mouse anti-human heparanase antibodies (mAb 130), kindly provided by InSight Ltd. (Rehovot, Israel), were prepared as previously described.10 These antibodies recognize both the latent 65 kDa and processed 50 kDa heparanase enzymes. Polyclonal rabbit anti-human heparanase antibodies (pAb 733) were raised against a peptide (KKFKNSTYSRSSVDC) located in the 50 kDa active human heparanase enzyme. These antibodies recognize primarily the 50 kDa heparanase subunit. Secondary Cy2-conjugated goat anti-mouse antibodies, Cy3-conjugated goat anti-rabbit antibodies, and HRP-conjugated goat anti-mouse, or goat anti-rabbit antibodies were from Jackson Immunoresearch Laboratories (Bar Harbor, MA, USA). 3G10 anti-HS antibodies34 were kindly provided by the late Dr M Bernfield (Division of Newborn Medicine, Children's Hospital, Boston, MA, USA).
Preparation of Cellular Extracts and Western Blot Analysis
U87 human glioma and C6 rat glioma cells (1 × 107) were washed (× 3) with PBS containing 1 mM Na3VO4, harvested (scraping) and lysed in lysis buffer (20 mM Tris, pH 7.5, 150 mM NaCl, 1 mM Na3VO4, 5 mM EDTA, 0.4% NP40, 10% glycerol, 1 mM DTT, 1 mM PMSF, 1 μg/ml leupeptin). Cytosolic and nuclear fractions of cells were prepared as previously described.35 For heparanase detection, cell extracts (100 μg total protein) were first incubated (1 h, 4°C) with ConA-Sepharose beads (Amersham Pharmacia, Uppsala, Sweden), washed (× 3) with PBS and eluted with Laemmli's sample buffer. Equal amounts of protein from cytosolic, nuclear, or whole cell extracts were subjected to 10% SDS-PAGE and Western blot analysis. Immunoblotting was performed with the designated primary antibodies, followed by secondary HRP-conjugated goat anti-mouse or goat anti-rabbit antibodies (Jackson Immunoresearch Laboratories, Bar Harbor, MA, USA). Immunoreactive bands were detected by enhanced chemiluminescence (ECL) using SuperSignal West Pico chemiluminescent substrate (Pierce, Rockford, IL, USA). The light emitted by the chemical reaction was detected by exposure to Hyperfilm ECL (Amersham Pharmacia) for 3–10 s. For verification of fraction purity, same protein amounts from the respective nuclear and cytosolic fractions were separated on 10% SDS-PAGE and immunoblotted with monoclonal anti-integrin β1 antibodies (Sigma Chemical Co., St Louis, MO, USA), detecting cell membranes, or polyclonal rabbit anti-SC35 antibodies (Santa Cruz Biotechnology, Santa Cruz, CA, USA), detecting cell nuclei, followed by secondary HRP-conjugated goat anti-mouse, or goat anti-rabbit antibodies (Jackson Immunoresearch Laboratories) and visualized by ECL. Fraction purity control was applied in each experiment.
Preparation of Sulfate Labeled Nuclear Fraction
Bovine corneal endothelial cells, or C6-glioma cells were plated on tissue culture dishes at an initial density of 2 × 105 cells/ml and cultured in Fischer's medium (sulfate low) supplemented with 10% FCS and 5% newborn calf serum. Na235SO4 (25 μCi/ml) (Amersham, Buckinghamshire, UK) was added on days 2 and 4 after seeding and the cultures were incubated with the label without medium change.33 On day 12, the cells were washed (× 3) free of unincorporated sulfate, scraped off the plate, washed (× 5) with PBS, lysed in lysis buffer, and the intact nuclear fraction was separated from the cytosol, as described.35 Nuclei were washed (× 3) with PBS and lysed by 3 cycles of freezing and thawing in heparanase reaction mixture (20 × mM phosphate citrate, pH 5.8, 150 mM NaCl, 1 mM CaCl2, 1 mM DTT), containing a cocktail of protease inhibitors (Roche Diagnostics, Mannheim, Germany).
Preparation of Sulfate Labeled ECM
Bovine corneal endothelial cells were plated into 35-mm tissue culture dishes and cultured as described above, except that 4% dextran T-40 was included in the growth medium.33, 36 Na235SO4 (25 μCi/ml) (Amersham) was added as described above and the subendothelial ECM was exposed by dissolving the cell layer with PBS containing 0.5% Triton X-100 and 20 mM NH4OH, followed by four washes with PBS.33, 36 The ECM remained intact, free of cellular debris and firmly attached to the entire area of the tissue culture dish. Nearly 80% of the radioactivity was incorporated into HSPGs.33, 36
Heparanase Activity
Cytosolic or nuclear or nuclear fractions prepared from 2 × 106 cells were incubated (16 h, 37°C, pH 5.8) with sulfate-labeled ECM, as described.33, 36 The incubation medium was centrifuged and the supernatant containing sulfate-labeled degradation products were analyzed by gel filtration on Sepharose CL-6B columns (0.9 × 30 cm). Fractions (0.2 ml) were eluted with PBS and their radioactivity counted in a β-scintillation counter. Heparanase-produced degradation fragments of HS were eluted from Sepharose 6B at 0.5<Kav< 0.8 (peak II). Nearly intact HSPGs were eluted just after the V0 (Kav<0.2, peak I).10, 33 To evaluate whether nuclear HS is degraded by heparanase, soluble sulfate (Na235SO4) labeled material extracted from the nuclear fraction of metabolically labeled corneal endothelial cells were incubated (pH 5.8, 37oC, 15 h) with recombinant heparanase (0.5 μg/ml), centrifuged and subjected to gel filtration analysis, as described above. Each determination was performed at least 3 times and the variation in elution positions (Kav values) did not exceed ±15%.
Indirect Immunofluorescence
Cells (U87 human glioma, C6 rat glioma, MDA-435 human breast carcinoma) were seeded on glass coverslides and subjected to indirect immunofluorescence, as previously described.29, 37 Cells were fixed with ice-cold methanol (5 min) and intrinsic fluorescence was blocked with 50 mM NH4Cl (30 min, 24oC). The cells were then incubated with blocking solution (10% goat serum in PBS, 30 min, 24oC) followed by incubation (2 h, 24oC) with the indicated antibodies (anti-HS G310, anti heparanase mAb 130, or pAb 733). Following washes (× 5) with PBS, cells were incubated (1 h, 24°C) with secondary Cy2 (green)- or Cy3 (red)- conjugated goat anti-mouse or goat anti-rabbit antibodies.
Immunohistochemistry
Immunostaining was performed as previously described with minor modifications.27 Briefly, paraffin-embedded 5-μm sections were deparaffinized, rehydrated and denatured for 3 min in a microwave oven in citrate buffer (10 mM, pH 6.0). Blocking steps included successive incubations in 3% H2O2 in methanol (30 min, 24°C) and blocking solution (10% goat serum, 0.2% Triton X-100 in PBS, 1 h, 24oC). Slides were then incubated (overnight, 4°C) with polyclonal (pAb 733) anti-human heparanase antibodies, diluted 1:150 in blocking solution. Following several washes with PBS, slides were incubated with secondary HRP-conjugated goat anti-rabbit antibodies (EnVision, DAKO Corporation, Carpinteria, CA, USA). Color reaction was obtained using Zymed aminoethyl carbozole (AEC, red staining) single solution (Zymed, South San-Francisco, CA, USA). Cell nuclei were counterstained with Mayer's hematoxylin (Sigma). Staining of the same tissue for P53 and Tunnel was performed, as described.38
Results
Localization of Human Heparanase in the Cell Nucleus of Transfected Cells
To study heparanase nuclear localization in transfected cells, nonmetastatic C6 rat glioma and U87 human glioma cells were stable transfected with the full-length human heparanase (H-hpa) cDNA, as described.30 Cultures were harvested and cytosolic and nuclear fractions were prepared and analyzed for the presence of heparanase. Briefly, following concentration of each fraction on ConA-Sepharose beads, bound proteins were subjected to 10% SDS-PAGE and Western immunoblot analysis, utilizing anti-heparanase mAb 130 recognizing both the latent 65 kDa and active 50 kDa heparanase forms (Figure 1). Purity of the nuclear and cytosolic fractions was verified by Western blot analysis, applying antibodies directed against the nuclear protein SC35 and the β1 cell membrane integrin, respectively (Figure 1). As demonstrated in Figure 1, both heparanase forms were present in the cytosolic fraction of H-hpa transfected U87 cells, whereas, the nuclear fraction of the same cells exhibited, predominantly, the 50 kDa active heparanase. A similar distribution pattern was obtained with H-hpa transfected C6 rat glioma cells (not shown). U87 cells transfected with insert free pcDNA3 plasmid were used as control. Immunoblot analysis of nuclear and cytosolic fractions prepared from mock-transfected cells, failed to detect the heparanase protein in both fractions (Figure 1, lanes #2).
Heparanase nuclear localization in transfected U87 glioma cells. Nuclear and cytosolic fractions from pooled populations of U87 human glioma cells, stable transfected with H-hpa cDNA (lanes #1), or mock transfected (lanes #2), were subjected to western immunoblotting applying antiheparanase mAb 130, recognizing both the latent (65 kDa) and active (50 kDa) heparanase forms. Purity of fractions was verified utilizing nuclear specific (anti-SC35), or cell membrane specific (anti-integrin β1) antibodies.
Nuclear Localization of Exogenously Added Recombinant Heparanase Following Uptake
Previously, we described the processing and trafficking events associated with cellular activation and uptake of exogenously added heparanase.28 We have demonstrated that primary human fibroblasts are capable of binding and converting the 65 kDa heparanase precursor into its highly active 50 kDa form, concomitantly with its cytoplasmic accumulation, mainly within endosomal structures.28 These results and the observed localization of heparanase within the nucleus of transfected glioma cells (Figure 1) led us to investigate whether uptake of exogenous heparanase is associated with translocation of the enzyme into the cell nucleus. For this purpose, nontransfected U87 glioma cells were incubated (DMEM, 1% FCS, 37oC, 0–60 min) with recombinant 65 kDa latent heparanase (4 μg/ml). Cells were then washed (PBS) and their nuclear (Figure 2a) and cytosolic (Figure 2b) fractions were subjected to Western blot analysis using monoclonal anti-heparanase antibodies. As demonstrated in Figure 2, the 65 kDa latent enzyme appeared both in the cytosol and nucleus already 30 min after incubation. Apparently, processing of the 65 kDa latent enzyme occurred both in the cytosol and nucleus, resulting in accumulation of the 50 kDa active heparanase, in both the nuclear and cytosolic fractions already at 1 h of incubation. Following 2 h incubation, only the 50 kDa form of heparanase was detected, most likely due to a complete conversion of the internalized 65 kDa latent enzyme into its active form (Figure 2a, b). It should be noted that the anti-heparanase mAb 130 used for the Western immunoblots recognizes both the latent 65 kDa and active 50 kDa heparanase forms. β-Actin levels were used as control to assure equal protein loading (Figure 2b, lower panel).
Nuclear translocation of exogenously added heparanase. Human glioma (U87) cells were incubated (DMEM, 1% FCS, 37°C) with recombinant 65 kDa heparanase (4 μg/ml) for 0–60 min. Following washes (PBS) to remove unbound heparanase, cells were lysed, fractionated to nuclear and cytosolic fractions and analyzed (10% SDS-PAGE followed by Western immunoblotting) for heparanase uptake and localization. Cells that were not exposed to heparanase were used as zero time control. (a) nuclear, or (b) cytosolic fractions of cells that were incubated with exogenous heparanase were subjected to immunoblotting with antiheparanase mAb-130. Lower panel: β-actin levels were used as a control for equal protein loading. (c) Rat C6 glioma cells that do not produce heparanase were incubated (RPMI, 0.5% FCS, 2 h, 37°C) with latent heparanase (4 μg/ml) in the absence (lanes #1), or presence (lanes #2) of heparin (10 μg/ml), as described above. Immunoblotting was performed with anti-heparanase pAb 733.
Heparanase Nuclear Translocation is Inhibited by Heparin
In a previous study it was demonstrated that excess heparin inhibited the uptake of exogenous heparanase into the cytoplasm.28 To study the effect of heparin on heparanase uptake and trafficking into the nucleus, cells (C6 glioma) that do not express heparanase30 were incubated (RPMI, 0.5% FCS, 2 h, 37oC) with recombinant 65 kDa heparanase in the absence (Figure 2c, lanes #1), or presence (Figure 2c, lanes #2) of 10 μg/ml heparin. Following washes (× 3) in cold PBS, the cells were lysed, fractionated to nuclear and cytosolic fractions, and subjected to 10% SDS-PAGE and Western immunoblotting, utilizing anti-heparanase pAb 733 antibodies. As demonstrated in Figure 2c, heparin markedly reduced heparanase uptake into the cytoplasm and completely abolished the enzyme’ translocation into the nucleus. The absence of the 65 kDa band (Figure 2c) is due to the relatively long incubation time (2 h) of the cells with the 65 kDa recombinant heparanase, as also demonstrated in Figure 2a and b. This result suggests that heparanase uptake into the nucleus is mediated through binding to cellular HSPGs, and that excess heparin competes with this binding and thereby inhibits heparanase cellular uptake and nuclear translocation.
Nuclear Heparanase is Enzymaticaly Active
Heparanase nuclear localization and in particular the presence of the active 50 kDa enzyme in the nuclear fraction, led us to investigate whether nuclear heparanase is capable of HS degradation. For this purpose, nuclear and cytoplasmic extracts of hpa-, or mock-transfected U87 human glioma cells, were assayed for their ability to degrade biosynthetically 35S-labeled ECM. Briefly, cell lysates (1 × 107 cells/ml) were fractioned to cytosolic and nuclear fractions, and incubated (pH 5.8, 37°C, 15 h) on sulfate-labeled ECM. Labeled material released into the incubation medium was analyzed by gel filtration on Sepharose CL-6B, as described.36 As demonstrated in Figure 3a, both nuclear and cytosolic fractions of hpa-transfected U87 cells degraded the ECM’ HSPGs into low molecular weight labeled fragments that eluted toward the Vt of the column (fractions 20–35, 0.5<Kav<0.75). Labeled fragments eluted in peak II were previously shown to be degradation products of HS, as they were five–six fold smaller than intact HS side chains, resistant to further digestion with papain and chondroitinase ABC and susceptible to deamination by nitrous acid.36 No heparanase activity was detected in nuclear or cytosolic fractions prepared from control mock-transfected U87 cells (Figure 3b). Nuclear heparanase activity was also evaluated in nontransfected MDA-435 human breast carcinoma cells that endogenously express the heparanase protein. As demonstrated in Figure 3c, both cytosolic and nuclear extracts of MDA-435 cells exhibited a high heparanase enzymatic activity. Moreover, exogenous recombinant latent heparanase that was added to U87 cells (Figure 2a), was found to be enzymatically active in both the nuclear and cytosolic fractions derived from these cells (Figure 3d). This result suggests that cellular binding and uptake of extracellular latent heparanase is associated with its activation and translocation into the cytoplasm and cell nucleus.
Enzymatic activity of nuclear-heparanase. (a) U87 glioma cells transfected with human heparanase (H-hpa), or (b) mock transfected, were lysed and fractionated to nuclear (•) and cytosolic (□) fractions and incubated (16 h, pH 5.8, 2 × 106 cells) on 35S-labeled ECM. Labeled degradation fragments released into the incubation medium were analyzed by gel filtration on Sepharose 6B, as described in ‘Materials and Methods’. (c) Nuclear-heparanase activity in cells expressing endogenous heparanase. Nuclear (•), or cytosolic (□) fractions of human breast carcinoma cells (MDA-435) expressing endogenous human heparanase were fractionated and tested for nuclear and cytosolic heparanase enzymatic activity, as described in a. (d), Nuclear-heparanase activity following cellular uptake of recombinant heparanase. U87 glioma cells (1 × 107) were incubated (DMEM, 1% FCS, 37°C, 1 h) with recombinant (65 kDa) heparanase (4 μg/ml), lysed and fractionated to nuclear (▴) and cytosolic (□) fractions, as described in ‘Materials and methods’. Following extensive washes to remove any free enzyme, fractions were incubated (pH 5.8, 37°C, 15 h) with 35S-labeled ECM. The incubation medium was subjected to gel filtration on Sepharose CL-6B, as described in ‘Materials and methods’.
Nuclear Heparan Sulfate is a Substrate for Nuclear Heparanase
Nuclear localization of both HS5, 6, 7, 39, 40, 41 and heparanase led us to investigate whether nuclear HS may serve as a substrate for heparanase activity. To examine this possibility, primary bovine corneal endothelial cells, were cultured in medium supplemented with Na235SO4 to label the cellular HS moieties. Cells were then washed (× 4) to remove unincorporated labeled material, lysed and fractionated to nuclear and cytosolic fractions. Following extensive washes, the nuclear fraction was incubated (pH 5.8, 37°C, 15 h) with active recombinant heparanase and assayed for HS degradation. The incubation medium was analyzed by gel filtration on Sepharose CL-6B, as described.36 Labeled nuclear fraction alone was used as control. As demonstrated in Figure 4, nuclear HSPGs were effectively degraded by recombinant heparanase, as indicated by generation of characteristic low molecular weight sulfate-labeled degradation fragments eluted toward the Vt of the column (peak II). Labeled material derived from a nuclear fraction that was not incubated with recombinant heparanase was eluted just after the void volume (V0) (peak I, Figure 4) of the column and consisted almost entirely of nearly intact, high molecular weight HSPGs. Similar results were obtained with sulfate-labeled nuclear preparation of C6 rat glioma cells (not shown). Laminaran sulfate (5 μg/ml), a potent inhibitor of heparanase activity and experimental metastasis,42 inhibited the degradation of nuclear HS by heparanase (Figure 4), as previously demonstrated for HS in the ECM.42
Nuclear HS is a substrate for heparanase activity. Bovine corneal endothelial cells were cultured in the presence of Na235SO4 (25 μCi/ml) added on days 2 and 5 after seeding, as described in ‘Materials and methods’. Following extensive washes to remove unincorporated labeled material, cells were lysed and fractionated to nuclear and cytosolic fractions, as described in ‘Materials and methods’. The sulfate-labeled nuclear fraction was then incubated (pH 5.8, 37°C, 15 h) with recombinant 50 kDa heparanase (0.5 μg/ml) in the absence (▪) or presence (×) of 5 μg/ml laminaran sulfate. Control nuclear fraction alone was incubated under the same conditions (□). The incubation medium was then centrifuged and the supernatant analyzed by gel filtration on Sepharose CL-6B.
Nuclear Colocalization of Heparanase and Heparan Sulfate
In order to study whether heparanase and HS colocalize within the cell nucleus, U87 hpa- and mock-transfected cells were double stained for heparanase and HS. Briefly, cells were seeded on glass cover slides, fixed, permeabllized and stained with anti-HS mAb 3G10 and anti-heparanase pAb 733. Following co-incubation with these antibodies, cells were washed and incubated with secondary Cy2 anti-mouse (Figure 5a, green) and Cy3 anti-rabbit (Figure 5b, red)-conjugated antibodies, respectively, and subjected to confocal microscopy. Granular staining of heparan sulfate (Figure 5a) and heparanase (Figure 5b) was noted in the cell nucleus. As shown in Figure 5c, heparanase and HS co-localized, in part, in the nucleus of hpa-transfected glioma cells, as indicated by the yellow nuclear staining observed in the double-stained cells (Figure 5c and d). In contrast, no such staining was detected when the same antibodies were applied to mock-transfected U87 cells (not shown). In a subsequent experiment, human-hpa-transfected C6 glioma cells (Figure 6b) and nontransfected MDA-435 breast carcinoma cells (Figure 6a), expressing endogenous heparanase, were subjected to immunostaining with anti-heparanase mAb 130. Specific heparanase labeling was readily detected within the cell nuclei, adjacent to the nucleoli (Figure 6b). Mock-transfected C6 glioma cells were used as control and exhibited no heparanase staining (Figure 6b, inset). These results indicate that nuclear localization of heparanase is not cell specific, occurring in both native and transfected heparanase expressing cells. In addition, staining with both monoclonal (mAb 130, Figure 6) and polyclonal (pAb 733, Figure 5) anti-heparanase antibodies yielded a similar staining pattern.
Nuclear colocalization of heparanase and heparan sulfate. Stable H-hpa-transfected U87 glioma cells (pooled population) were subjected to indirect immunofluorescence staining with (a) monoclonal anti-HS antibodies (mAb 3G10) followed by Cy2-conjugated goat anti-mouse antibody (green), and (b) polyclonal antiheparanase antibodies (733) followed by Cy3-conjugated goat anti-rabbit antibodies (red), as described in ‘Materials and methods’, (c and d) Colocalization of nuclear HS and heparanase (yellow, arrows). Immunofluorescent staining was analyzed by confocal microscopy. Images were obtained at an original objective magnification of × 60. There was no staining of cells exposed to Cy2- or Cy3-conjugated antibodies alone.
Nuclear localization of heparanase in nontransfected and hpa-transfected cells. (a) Nuclear heparanase in nontransfected human breast carcinoma cells. MDA-435 cells endogenously expressing heparanase were subjected to indirect immunoflorescent staining applying anti-heparanase mAb 130 and secondary anti-mouse Cy3-conjugated antibodies. (b) Nuclear heparanase in H-hpa transfected glioma cells. Stable H-hpa-transfected C6-rat glioma cells (pooled population) were subjected to indirect immunoflorescent staining as described in (a) Inset: mock-transfected C6 glioma cells. Cells were analyzed by confocal microscopy. Images were taken at an original objective magnification of X60.
Heparanase Nuclear Localization in Human Tumor Cells In Vivo
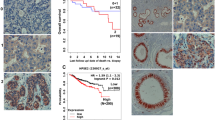
We investigated whether heparanase nuclear localization is limited to cultured cells, or is a general property of cancer cells in vivo. For this purpose, tissue sections of moderately differentiated squamous cell carcinoma (SCC) specimens from human oral cavity were subjected to immunostaining, utilizing anti-heparanase polyclonal antibodies (pAb 733). As demonstrated in Figure 7, a prominent granular heparanase staining (red-brown) is seen in the nuclei of a large proportion of the epithelial tumor cells (Figure 7a), vs no nuclear staining in the adjacent stromal cells (Figure 7b, arrows). It should be noted that less than 20% of the cells in the same specimens exhibited p53 staining, and that the apoptotic rate calculated from positive Tunnel staining of cells was less than 1% in the same specimens (not shown).
Nuclear localization of heparanase in human oral squamous cell carcinoma. Paraffin-embedded tissue sections from human oral SCC were subjected to immunostaining with anti-heparanase antibodies (pAb 733), as described in ‘ Materials and methods’. (a) Intense, nuclear granular staining of heparanase is seen in most salivary gland tumor cells, with only scant cytoplasmic staining. (b) Nuclear staining of heparanase in the mucosal epithelial tumor cells. Nuclear staining is not detected in the adjacent stromal cells (arrows). Mayer's hematoxylin was used for counterstaining of the cell nuclei (Blue). Images were taken at an original objective magnification of X60.
Discussion
In the present study we investigated heparanase nuclear localization and activity in hpa-transfected glioma (U87-human, C6-rat) and nontransfected human breast carcinoma (MDA-435) cells. Our results clearly indicate that in addition to heparanase granular localization in the cell cytoplasm,29 both the latent (65 kDa) and active (50 kDa) heparanase forms are found in the cell nucleus. Interestingly, the nuclei of the examined cells contained predominantly the 50 kDa active heparanase, as demonstrated by subcellular fractionation and Western blot analysis, applying anti-heparanase monoclonal antibodies recognizing both the latent and active enzymes. Moreover, incubation of cells with recombinant latent heparanase resulted in internalization of the enzyme and subsequent translocation into the cell nucleus. While mostly the 65 kDa enzyme was found in the nucleus at 30 min following uptake, the 50 kDa enzyme was the predominant form at 60 min and was no longer detected at 2 h. Although the exact location and mode of heparanase processing has not been fully characterized, it may well be that conversion of latent heparanase into its active form occurs, in several compartments,28 including the cell nucleus. Since the protease responsible for processing of the latent enzyme has not been identified, it is not certain whether heparanase is processed in the nucleus in the same manner as in the cytosol.
To evaluate whether nuclear heparanase is enzymaticaly active, nuclear fractions from hpa-transfected human and rat glioma cells, and nontransfected human breast carcinoma cells (MDA-435), were assayed for heparanase activity. All nuclear preparations exhibited a high HS degrading activity, similar to the cytoplasmic enzyme. It should be noted, however, that the cytosolic and nuclear fractions were incubated with the ECM for 15 h, allowing the enzymatic reaction to proceed beyond the linear phase. Under these conditions, more than 80% of the total labeled substrate was degraded, precluding quantitative estimation of the actual amount of cytosolic vs nuclear heparanase. The relative amount of cytosolic vs nuclear heparanase can be estimated, however, based on the Western blot presented in Figure 1. It appears that the cytosolic fraction contains approximately four-fold more heparanase than the nuclear fraction. Taking into account that in the hpa-transfected glioma cells the total amount of protein extracted from the cytosol vs the nucleus was 3.6-fold higher, it is estimated that the total amount of nuclear heparanase is about 7% of that found in the cytosol. This estimation was confirmed by performing the heparanase activity assay applying equal amounts of glioma cytosolic and nuclear protein, incubated with the ECM for 4 rather than 15 h. A similar result was obtained with MDA-435 cells, expressing high levels of endogenous heparanase (not shown).
Recombinant exogenously added latent heparanase that was translocated into the nucleus was found to be enzymatically active, similar to the endogenous nuclear heparanase. These results suggest that cellular binding and uptake of extracellular heparanase secreted, for example, by activated platelets and neutrophils,16, 43 or by astrocytes32 may result in the uptake and storage of the enzyme in lysosomal28, 29 and nuclear cellular compartments.
Several groups have reported the presence of HS chains in the nucleus of various cell types5, 6, 7, 39, 40, 41 and demonstrated that HSPGs may regulate the internalization and nuclear uptake of FGF-1 and FGF-2.7, 8, 9 It was also suggested that a correlation exists between nuclear localization of HS and the growth rate of hepatoma cells, and that both glypican and biglycan participate in the regulation of C6 glioma cell proliferation and survival through a direct involvement of HSPGs in nuclear processes.44 These reports emphasize the catabolism of HSPGs to free HS chains and their regulated nuclear uptake and potential participation in nuclear processes. In view of these results, we investigated whether nuclear heparanase is capable of degrading nuclear HS and thus play a role in HS turnover and nuclear functions. Our results clearly indicate that nuclear HSPGs are readily degraded by recombinant and nuclear heparanases. Immunofluorescent staining, utilizing anti-heparanase and anti-HS antibodies (3G10), clearly demonstrated that heparanase colocalizes with HSPGs within the cell nucleus, suggesting a possible formation of a complex between the two. The exact nuclear localization of heparanase was not characterized. Confocal microscopy indicated that in cultured glioma cells the enzyme is localized in close proximity to the nucleoli.
Although the exact mode of heparanase translocation into the nucleus requires further investigation, at least two putative mechanisms for heparanase nuclear localization are feasible. First, the human heparanase sequence contains two potential nuclear localization signals (residues 271–277; PRRKTAK and residues 427–430; KRRK) that can mediate the enzyme’ nuclear localization. Second, nuclear translocation of heparanase may be facilitated by its heparin binding domain, utilizing HS as its vehicle. In fact, as was previously suggested28 and as demonstrated in the present study, heparin inhibited the uptake of extracellular recombinant heparanase and thereby its nuclear translocation, supporting a role for HS in heparanase cellular translocation and nuclear localization. In fact, nuclear translocation of HSPGs is well documented and has been shown to involve a nuclear localization sequence in the core protein of glypicans.44 Our preliminary results indicate that cell surface HS plays a role in heparanase cellular binding and uptake. The internalized HS-bound enzyme may then be translocated into the nucleus utilizing its own and/or the HSPG nuclear localization signal. β- and γ-catenins may also function as vehicles for heparanase nuclear internalization, or vise versa. In fact, our preliminary results indicate that heparanase specifically interacts with β- and γ-catenins in the cell cytoplasm, followed by translocation into the nucleus (Schubert et al, unpublished results).
Although the exact function played by heparanase in the nucleus requires further investigation, several potential activities of nuclear heparanase can be hypothesized. For example, heparin binding proteins such as FGF-1 and FGF-2 depend on HS for translocation into the nucleus.45, 46 Also, HSPGs were demonstrated to play a fundamental role in the regulation of topoisomerase-I mediated DNA relaxation.47 Degradation of HS by nuclear heparanase may thus contribute to the malignant phenotype of cells by liberating the inhibitory effect of HS on topoisomerase-I DNA relaxation. Likewise, heparanase cleavage of nuclear HS may affect the transcriptional activity associated with nuclear FGF-2.48, 49 Our preliminary experiments suggest a potential role for heparanase in nuclear translocation of β- and γ-catenins and their subsequent involvement in Lef/Tcf-mediated transcriptional activity and control of cell proliferation (Schubert et al, unpublished results). Similarly, it has been demonstrated that FGF-2 may augment nuclear levels of β-catenin and promote Lef/Tcf-dependent transcription of a cyclin D1-luciferase construct.49
It should be emphasized that heparanase nuclear localization is not restricted to cancer cell lines maintained in culture and, as demonstrated in the present study, was also found in human primary tumors of the oral cavity and salivary glands. In these specimens, a granular distribution of heparanase was noted in the nucleus and was not restricted to areas adjacent to the nucleoli. Nuclear immunostaining of heparanase was recently demonstrated in human gastric and esophagus cancers,21 supporting our observations in vitro and in vivo.
References
Bernfield M, Gotte M, Park PW, et al. Functions of cell surface heparan sulfate proteoglycans. Annu Rev Biochem 1999;68:729–777.
Vlodavsky I, Bar-Shavit R, Korner G, et al. Extracellular matrix-bound growth factors, enzymes and plasma proteins. In: Rohrbach DH, Timpl R (eds). The Basement Membranes: Cellular and Molecular Aspects. Academic Press Inc.: Orlando, FL, 1993;pp:327–343.
Iozzo RV . Matrix proteoglycans: from molecular design to cellular function. Annu Rev Biochem 1998;67:609–652.
Kjellen L, Lindahl U . Proteoglycans: structures and interactions. Annu Rev Biochem 1991;60:443–475.
Ishihara M, Fedarko NS, Conrad HE . Transport of heparan sulfate into the nuclei of hepatocytes. J Biol Chem 1986;261:13575–13580.
Fedarko NS, Conrad HE . A unique heparan sulfate in the nuclei of hepatocytes: structural changes with the growth state of the cells. J Cell Biol 1986;102:587–599.
Tumova S, Hatch BA, Law DJ, et al. Basic fibroblast growth factor does not prevent heparan sulphate proteoglycan catabolism in intact cells, but it alters the distribution of the glycosaminoglycan degradation products. Biochem J 1999;337:471–481.
Sperinde GV, Nugent MA . Heparan sulfate proteoglycans control intracellular processing of bFGF in vascular smooth muscle cells. Biochemistry 1998;37: 13153–13164.
Sperinde GV, Nugent MA . Mechanisms of fibroblast growth factor 2 intracellular processing: a kinetic analysis of the role of heparan sulfate proteoglycans. Biochemistry 2000;39:3788–3796.
Vlodavsky I, Freidmann Y, Elkin M, et al. Mammalian heparanase: gene cloning, expression and function in tumor progression and metastasis. Nat Med 1999;5: 793–802.
Dempsey LA, Plummer TB, Coombes SL, et al. Heparanase expression in invasive trophoblasts and acute vascular damage. Glycobiology 2000;10:467–475.
Nakajima M, Irimura T, Nicolson GL . Heparanases and tumor metastasis. J Cell Biochem 1988;36:157–167.
Vlodavsky I, Friedmann Y . Molecular properties and involvement of heparanase in cancer metastasis and angiogenesis. J Clin Invest 2001;108:341–347.
Parish CR, Freeman C, Hulett MD . Heparanase: a key enzyme involved in cell invasion. Biochim Biophys Acta 2001;1471:M99–M108.
Dempsey LA, Brunn GJ, Platt JL . Heparanase, a potential regulator of cell–matrix interactions. Trends Biochem Sci 2000;25:349–351.
Vlodavsky I, Eldor A, Haimovitz-Friedman A, et al. Expression of heparanase by platelets and circulating cells of the immune system: possible involvement in diapedesis and extravasation. Invasion Metast 1992;12:112–127.
McKenzie E, Young K, Hircock M, et al. Biochemical characterisation of the active heterodimer form of human Heparanase (Hpa1) protein expressed in insect cells. Biochem J 2003;373:423–435.
Levy-Adam F, Miao HQ, Heinrikson RL, et al. Heterodimer formation is essential for heparanase enzymatic activity. Biochim Biophys Res Comm 2003;308:885–891.
Vlodavsky I, Mohsen M, Lider O, et al. Inhibition of tumor metastasis by heparanase inhibiting species of heparin. Invasion Metast 1994;14:290–302.
Parish CR, Freeman C, Brown KJ, et al. Identification of sulfated oligosaccharide-based inhibitors of tumor growth and metastasis using novel in vitro assays for angiogenesis and heparanase activity. Cancer Res 1999;59:3433–3441.
Takaoka M, Naomoto Y, Ohkawa T, et al. Heparanase expression correlates with invasion and poor prognosis in gastric cancers. Lab Invest 2003;83:613–622.
Koliopanos A, Friess H, Kleeff J, et al. Heparanase expression in primary and metastatic pancreatic cancer. Cancer Res 2001;61:4655–4659.
Gohji K, Hirano H, Okamoto M, et al. Expression of three extracellular matrix degradative enzymes in bladder cancer. Int J Cancer 2001;95:295–301.
Myler HA, West JL . Heparanase and platelet factor-4 induce smooth muscle cell proliferation and migration via bFGF release from the ECM. J Biochem (Tokyo) 2002;131:913–922.
Elkin M, Ilan N, Ishai-Michaeli R, et al. Heparanase as mediator of angiogenesis: mode of action. FASEB J 2001;15:1661–1663.
Folkman J, Klagsbrun M, Sasse J, et al. A heparin-binding angiogenic protein–basic fibroblast growth factor—is stored within basement membrane. Am J Pathol 1988;130:393–400.
Goldshmidt O, Zcharia E, Abramovitch R, et al. Cell surface expression and secretion of heparanase markedly promote tumor angiogenesis and metastasis. Proc Natl Acad Sci USA 2002;3:10031–10036.
Nadav L, Eldor A, Yacoby-Zeevi O, et al. Activation, processing and trafficking of extracellular heparanase by primary human fibroblasts. J Cell Sci 2002;115: 2179–2187.
Goldshmidt O, Nadav L, Aingorn H, et al. Human heparanase is localized within lysosomes in a stable form. Exp Cell Res 2002;281:50–62.
Goldshmidt O, Zcharia E, Aingorn H, et al. Expression pattern and secretion of human and chicken heparanase are determined by their signal peptide sequence. J Biol Chem 2001;276:29178–29187.
Goldshmidt O, Zcharia E, Cohen M, et al. Heparanase mediates cell adhesion independent of its enzymatic activity. FASEB J 2003;17:1015–1025.
Marchetti D, Li J, Shen R . Astrocytes contribute to the brain-metastatic specificity of melanoma cells by producing heparanase. Cancer Res 2000;60:4767–4770.
Vlodavsky I . Preparation of extracellular matrices produced by cultured corneal endothelial and PF-HR9 endodermal cells. In: Current Protocols in Cell Biology. John Wiley & Sons: New York, 1999, pp. 10.14.11–10.14.14.
David G, Bai XM, Van der Schueren B, et al. Developmental changes in heparan sulfate expression: in situ detection with mAbs. J Cell Biol 1992;119:961–975.
Molitor JA, Walker WH, Doerre S, et al. NF-kappa B: a family of inducible and differentially expressed enhancer—binding proteins in human T cells. Proc Natl Acad Sci USA 1990;87:10028–10032.
Vlodavsky I, Fuks Z, Bar-Ner M, et al. Lymphoma cell-mediated degradation of sulfated proteoglycans in the subendothelial extracellular matrix: relationship to tumor cell metastasis. Cancer Res 1983;43:2704–2711.
Katz BZ, Levenberg S, Yamada KM, et al. Modulation of cell–cell adherens junctions by surface clustering of the N-cadherin cytoplasmic tail. Exp Cell Res 1998;243:415–424.
Nagler RM, Kerner H, Laufer D, et al. Squamous cell carcinoma of the tongue: the prevalence and prognostic roles of p53, Bcl-2, c-erbB-2 and apoptotic rate as related to clinical and pathological characteristics in a retrospective study. Cancer Lett 2002;186:137–150.
Fedarko NS, Ishihara M, Conrad HE . Control of cell division in hepatoma cells by exogenous heparan sulfate proteoglycan. J Cell Physiol 1989;139:287–294.
Ishihara M, Conrad HE . Correlations between heparan sulfate metabolism and hepatoma growth. J Cell Physiol 1989;138:467–476.
Ishihara M, Fedarko NS, Conrad HE . Involvement of phosphatidylinositol and insulin in the coordinate regulation of proteoheparan sulfate metabolism and hepatocyte growth. J Biol Chem 1987;262:4708–4716.
Miao HQ, Elkin M, Aingorn H, et al. Inhibition of heparanase activity and tumor metastasis by laminarin sulfate and synthetic phosphorothioate oligodeoxynucleotides. Int J Cancer 1999;83:424–431.
Ishai-Michaeli R, Eldor A, Vlodavsky I . Heparanase activity expressed by platelets, neutrophils, and lymphoma cells releases active fibroblast growth factor from extracellular matrix. Cell Regul 1990;1:833–842.
Liang Y, Haring M, Roughley PJ, et al. Glypican and biglycan in the nuclei of neurons and glioma cells: presence of functional nuclear localization signals and dynamic changes in glypican during the cell cycle. J Cell Biol 1997;139:851–864.
Gabriel B, Baldin V, Roman AM, et al. Localization of peptide growth factors in the nucleus. Methods Enzymol 1991;198:480–494.
Amalric F, Baldin V, Bosc-Bierne I, et al. Nuclear translocation of basic fibroblast growth factor. Ann N Y Acad Sci 1991;638:127–138.
Kovalszky I, Dudas J, Olah-Nagy J, et al. Inhibition of DNA topoisomerase I activity by heparan sulfate and modulation by basic fibroblast growth factor. Mol Cell Biochem 1998;183:11–23.
Riedel F, Gotte K, Oulmi Y, et al. Immunocytochemical localization of basic fibroblast growth factor in squamous cell carcinomas of the head and neck. Anticancer Res 2001;21:1873–1878.
Holnthoner W, Pillinger M, Groger M, et al. Fibroblast growth factor-2 induces Lef/Tcf-dependent transcription in human endothelial cells. J Biol Chem 2002;277:45847–45853.
Acknowledgements
We are thankful to Insight Ltd. (Rehovot, Israel) for providing the anti-human heparanase antibodies (mAb 130). This work was supported by the Israel Science Foundation (Grant # 503/98). The Israel Cancer Research Fund (ICRF) and the Prostate Cancer Foundation Israel awarded to IV.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schubert, S., Ilan, N., Shushy, M. et al. Human heparanase nuclear localization and enzymatic activity. Lab Invest 84, 535–544 (2004). https://doi.org/10.1038/labinvest.3700084
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3700084
Keywords
This article is cited by
-
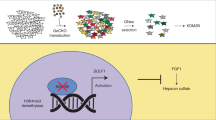
Upregulation of ERK-EGR1-heparanase axis by HDAC inhibitors provides targets for rational therapeutic intervention in synovial sarcoma
Journal of Experimental & Clinical Cancer Research (2021)
-
Heparanase and the hallmarks of cancer
Journal of Translational Medicine (2020)
-
Nuclear heparanase-1 activity suppresses melanoma progression via its DNA-binding affinity
Oncogene (2015)
-
Significance of Heparanase in Cancer and Inflammation
Cancer Microenvironment (2012)