Abstract
A previous study has shown that the stress responsive neurohormone arginine vasopressin (AVP) is activated in the amygdala during early withdrawal from cocaine. The present studies were undertaken to determine whether (1) AVP mRNA levels in the amygdala or hypothalamus, as well as hypothalamic–pituitary–adrenal (HPA) activity, would be altered during chronic intermittent escalating heroin administration (10 days; 7.5–60 mg/kg/day) or during early (12 h) and late (10 days) spontaneous withdrawal; (2) foot shock stress would alter AVP mRNA levels in the amygdala or hypothalamus in rats withdrawn from heroin self-administration (7 days, 3 h/day, 0.05 mg/kg/infusion); and (3) the selective V1b receptor antagonist SSR149415 (1 and 30 mg/kg, intraperitoneal) would alter heroin seeking during tests of reinstatement induced by foot shock stress and by heroin primes (0.25 mg/kg), as well as HPA hormonal responses to foot shock. We found that AVP mRNA levels were increased during early spontaneous withdrawal in the amygdala only. This amygdalar AVP mRNA increase was no longer observed at the later stage of heroin withdrawal. Foot shock stress increased AVP mRNA levels in the amygdala of rats withdrawn from heroin self-administration, but not in heroin naïve rats. Behaviorally, SSR149415 dose-dependently attenuated foot shock-induced reinstatement and blocked heroin-induced reinstatement. Finally, SSR149415 blunted the HPA activation by foot shock. Together, these data in rats suggest that stress responsive AVP/V1b receptor systems (including the amygdala) may be critical components of the neural circuitry underlying the aversive emotional consequences of drug withdrawal, as well as the effect of negative emotional states on drug-seeking behavior.
Similar content being viewed by others
INTRODUCTION
In humans, stress has long been recognized as a major factor contributing to the development and perpetuation of drug addiction. For example, psychological stress elevates drug cravings (Sinha et al, 1999), and stress-induced hypothalamic-pituitary-adrenal (HPA) axis responses predict amounts of subsequent drug use (Sinha et al, 2006). Drugs of abuse themselves, and withdrawal from such drugs, can act as stressors promoting persistent and compulsive drug abuse (see reviews by Kreek and Koob, 1998; Stewart, 2000; Sinha, 2001). Furthermore, stress-related anxiety and depression are major psychiatric consequences of chronic drug abuse, especially during withdrawal (Koob and le Moal, 1997; Markou et al, 1998). A growing body of evidence suggests that vasopressinergic neuronal activity in the amygdala and hypothalamus represents an important element in the neurobiology of stress-related behaviors. In fact, acute stress increases extracellular levels of arginine vasopressin (AVP) in the rat amygdala and hypothalamus (Ebner et al, 2002; Wigger et al, 2004), and activation of V1b receptors by AVP modulates anxiogenic and depressive behaviors in rats (Griebel et al, 2002; Wigger et al, 2004).
During the 1980s, evidence emerged implicating AVP in the motivational properties of heroin and cocaine. In fact, systemic administration of desglycinamide-(Arg8)-vasopressin decreased heroin and cocaine self-administration (van Ree et al, 1988), and intracerebroventricular (i.c.v.) administration of AVP antiserum increased cocaine self-administration (De Vry et al, 1988). Furthermore, in studies exploring the role of AVP in cocaine-induced locomotion sensitization, Brattleboro homozygote rats lacking vasopressin showed deficient onset and persistence of cocaine-induced sensitization (Post et al, 1982).
Our laboratory has recently begun to explore the role of AVP in drug addiction. We have found that acute cocaine withdrawal increases AVP gene expression in the amygdala through an opioid receptor activation-mediated mechanism (Zhou et al, 2005). On the basis of these results, we designed a set of novel experiments addressing two research questions. The first was to determine whether chronic heroin exposure and spontaneous heroin withdrawal would alter AVP gene expression. To answer this question, we employed an administration regimen of chronic intermittent escalating-dose heroin, which mimics the multiple and escalating doses taken by heroin-dependent individuals to prevent symptoms of withdrawal (Kreek et al, 2002). Using this regimen, we assessed the effects of chronic (10 days) intermittent escalating-dose heroin administration, and early (12 h) and late (10 days) spontaneous withdrawal on AVP mRNA levels in the amygdala. We also examined the effects of heroin withdrawal (both early and late) on several components of HPA axis activity, including mRNA levels of AVP, its V1b receptor (V1b) and proopiomelanocortin (POMC) in the hypothalamus and anterior pituitary, and HPA hormonal levels in plasma.
The second research question was whether AVP could modulate heroin-seeking behavior. To this end, we tested the effects of SSR149415 on heroin seeking, using the reinstatement model (Shaham et al, 2000a, 2003; Stewart, 2003; Bossert et al, 2005). This compound was selected because of its ability to antagonize the V1b receptor; the receptor type involved in the modulation of ACTH release by endogenous vasopressin and of other brain functions (De Wied et al, 1993; Aguilera and Rabadan-Diehl, 2000). SSR149415 is a non-peptide antagonist highly selective for the V1b receptor (60- to 800-fold more than for the V1a receptor) (Serradeil-Le et al, 2003; Guillon et al, 2004), and shown to possess both anxiolytic and antidepressant properties, as well as to block several neuroendocrine (ACTH release), neurochemical (noradrenaline release), and autonomic (hyperthermia) responses to various stressors in rodents (Griebel et al, 2002, 2005; Serradeil-Le et al, 2003; Overstreet and Griebel, 2005).
We assessed the effect of SSR149415 pretreatment on two operant tests of drug seeking carried out 6 and 8 days after the last day of heroin self-administration; one occurred following exposure to foot shock stress, and the other test occurred following priming injections of heroin, two manipulations well known to reinstate responding in rats trained to self-administer a variety of drugs (Erb et al, 1996; Shaham et al, 2000a; Stewart, 2003; McFarland et al, 2004). On the basis of evidence implicating central corticotropin-releasing factor (CRF) activity on stress-induced, but not heroin-induced relapse to heroin seeking (Shaham et al, 1997; Erb et al, 1998; Erb and Stewart, 1999; Stewart, 2000), we anticipated an effect of pretreatment with the V1b antagonists primarily on stress-induced reinstatement. SSR149415 was also injected before the first session of extinction in order to uncover possible effects on lever pressing per se.
Finally, we assessed the AVP mRNA levels in the amygdala and hypothalamus in response to foot shock stress in rats withdrawn from heroin self-administration, and the effects of pretreatment with the SSR149415 on HPA responses to foot shock stress.
MATERIALS AND METHODS
Effects of Chronic Heroin Exposure and its Spontaneous Withdrawal on mRNA Levels of AVP, V1b, and POMC, and on Plasma Levels of ACTH and Corticosterone
Subjects
Forty-four male Fischer rats (250–275 g, Charles River Labs, Kingston, NY) were housed individually in a stress-minimized facility with free access to water and food. Animals were adapted to a standard 12-h light/dark cycle (lights off from 0700–1900 hours) for 7 days before the beginning of the experiment. We followed the Principles of Laboratory Animal Care (NIH publication no. 86-23, 1996). The specific protocol was approved by the Rockefeller University Animal Care and Use Committee. During all experimental procedures, the number of animals and potential suffering by treatments were minimized.
Drug treatment
The regimen of chronic drug exposure (saline or heroin) consisted of intraperitoneal (i.p.) injections in the home cage three times daily with two 6-h intervals and one 12-h interval, beginning 4 h after the beginning of the dark cycle (1100, 1700, and 2300 hours) for 10 days. For animals treated with heroin (Sigma Chemical Co., St Louis, MO), doses were increased every second day. Therefore, the heroin-treated rats received initial dosing at 7.5 (3 × 2.5) mg/kg/day on days 1–2, 15 (3 × 5.0) mg/kg/day on days 3–4, 30 (3 × 10) mg/kg/day on days 5 and 6, 45 (3 × 15) mg/kg/day on days 7–8, and then 60 (3 × 20) mg/kg/day on days 9–10.
In order to assess neurochemical and hormonal changes associated with chronic heroin exposure and different stages of withdrawal, two experiments were performed involving five separate groups of rats. Experiment 1. Chronic heroin with early withdrawal—included three groups: (1) control group I (n=8): chronic intermittent saline injections, and one injection of saline at 1100 hours of day 11; (2) chronic heroin (n=8): chronic intermittent escalating-dose heroin, and one injection of heroin (20 mg/kg) at 1100 hours of day 11; and (3) early heroin withdrawal (n=8): chronic intermittent escalating-dose heroin, and one injection of saline (instead of heroin) at 1100 hours of day 11. Experiment 2. Late withdrawal—included two groups: (1) control group II (n=10): chronic intermittent saline injections, and one injection of saline at 1100 hours of the 10th day following chronic saline injections (ie, day 20); and (2) late heroin withdrawal (n=10): chronic intermittent escalating-dose heroin, and one injection of saline (instead of heroin) at 1100 hours of the 10th day following chronic heroin injections (ie, day 20). At 1130 hours (30 min after the last injection), all rats were briefly exposed to CO2 (within 15 s) and killed by decapitation.
As 20 mg/kg is a relatively high dose of heroin in opiate-naïve animals, possibly leading to symptoms of heroin overdose, including respiratory depression and lethality, we could not examine the effects of acute heroin treatment at 20 mg/kg. Instead, we examined the effects of a single 5 mg/kg dose of heroin and observed an increase of ACTH and corticosterone levels in heroin naïve rats 30 min after the injection (unpublished data). However, this acute heroin treatment had no effect on AVP mRNA levels in either the amygdala or hypothalamus (data not shown).
Preparation of RNA extracts
Each rat brain was removed from the skull and placed in a chilled rat brain matrix (Electron Microscopy Sciences, Ft. Washington, PA). Coronal slices containing the brain regions of interest were removed from the matrix and placed on a chilled Petri dish. Dissection was carried out under a dissecting microscope using razor blades and forceps. The brain regions of interest were identified according to the Rat Brain in Stereotaxic Coordinates (Paxinos and Watson, 1986), as we described in detail in our early publication (Zhou et al, 1996). Brain regions and pituitary, including the anterior pituitary, neurointermediate lobe/posterior lobe (NIL/PL) of the pituitary, hypothalamus (the paraventricular nucleus-rich dissection), and amygdala (including the medial nucleus and basolateral nucleus) were dissected on ice, homogenized in guanidinium thiocyanate buffer, and extracted with acidic phenol and chloroform as described previously (Branch et al, 1992). After the final ethanol precipitation step, each extract was resuspended in H2O and stored at −80°C.
Solution hybridization ribonuclease (RNase) protection-trichloroacetic acid precipitation assay
The solution hybridization RNase protection-trichloroacetic acid (TCA) precipitation protocol has been described in detail in earlier reports (Branch et al, 1992; Zhou et al, 1996). A 502 bp fragment from the rat AVP cDNA and a 1201 bp fragment from the rat V1b cDNA were cloned into the polylinker region of pCR II (Invitrogen, Carlsbad, CA). A 538 bp fragment from the rat POMC cDNA was cloned into the polylinker region of pSP64 (Promega, Madison, WI) in both the sense and antisense orientations. The plasmid pS/E (a pSP65 derivative) was used to synthesize riboprobe for the 18S rRNA to determine total RNA. 33P-labeled cRNA antisense probes and unlabeled RNA sense standards were synthesized using an SP6 transcription system. A denaturing agarose gel containing 1.0 M formaldehyde showed that a single full-length transcript had been synthesized from each plasmid.
RNA extracts were dried in 1.5 ml Eppendorf tubes and resuspended in 30 μl that contained 150 000–300 000 c.p.m. of a probe in 2 × TESS (10 mM N-Tris[hydroxy-methyl]methyl-2-aminoethane sulfonic acid, pH 7.4; 10 mM ethylenediaminetetraacetic acid (EDTA); 0.3 M NaCl; 0.5% sodium dodecyl sulfate (SDS)). Samples were covered with mineral oil and hybridized overnight at 75°C. For RNase treatment, 250 μl of a buffer that contained 0.3 M NaCl, 5 mM EDTA, 10 mM Tris-HCl (pH 7.5), 40 μg/ml RNase A (Worthington, Biochemicals, Freehold, NJ), and 2 μg/ml RNase T1 (Calbiochem, San Diego, CA) were added and each sample was incubated at 30°C for 1 h. TCA precipitation was effected by the addition of 1 ml of a solution that contained 5% TCA and 0.75% sodium pyrophosphate. Precipitates were collected onto a filter in sets of 24 by using a cell harvester (Brandel, Gaithersburg, MD) and were measured in a scintillation counter with liquid scintillant (Beckman Instruments, Palo Alto, CA).
The procedure to measure mRNA levels involved comparison of values obtained from experimental samples (brain extracts) to those obtained for a set of calibration standards. The calibration standards had known amounts of an in vitro sense transcript whose concentration was determined by optical absorbance at 260 nm. The set of calibration standards included those with no added sense transcript and those that contained between 1.25 and 80 pg of the sense transcript (Zhou et al, 1996). A new standard curve was generated each time experimental samples were analyzed and all extracts of a particular tissue were assayed for each mRNA as a group in a single assay.
Total cellular RNA concentrations were measured by hybridization of diluted extracts to a 33P-labeled probe complementary to 18S rRNA at 75°C. The calibration standards for this curve contained 10 μg of Escherichia coli tRNA plus either 0.0, or from 2.5 to 40 ng of total RNA from rat brain whose concentration was determined by optical absorbance at 260 nm.
Radioimmunoassays
At the time of decapitation, blood from each rat was collected in tubes, placed on ice, and was spun in a refrigerated centrifuge. Plasma was separated and stored at 40°C for hormonal measurements by radioimmunoassay. Corticosterone levels were assayed using a rat corticosterone 125I kit from MP Biomedicals (Costa Mesa, CA). ACTH immunoreactivity levels were assayed from unextracted plasma by using a kit from DiaSorin Inc. (Stillwater, MN). All values were determined in duplicate in a single assay.
Statistical analyses
In Experiment 1, group differences in mRNA levels of the AVP, V1b, and POMC, and plasma levels of ACTH and corticosterone were analyzed using one-way analysis of variance (ANOVA) for all three groups followed by Newman–Keuls post hoc tests or planned comparisons (α=0.05). In Experiment 2, differences between two groups were analyzed using t-test (α=0.05). All statistical analyses were performed using SigmaStat (version 3.0 for Windows, SPSS Inc.).
Effects of Selective V1b Receptor Antagonist on Heroin Seeking
Subjects
Thirty-six adult male Sprague–Dawley rats (Charles River, QC), weighing 225–250 g at the beginning of the experiment, were singly housed and maintained on a reverse light/dark cycle (0800 hours lights off; 2000 hours lights on) with free access to food and water except during behavioral testing, which always occurred during the dark cycle. All experiments were approved by the Animal Care Committee of the University of Guelph and were carried out in accordance with the recommendations of the Canadian Council on Animal Care.
Surgery
Rats were surgically implanted with intravenous silastic catheters (Dow Corning, Midland, MI) in the right jugular vein, under general anesthesia induced by a combination of sodium pentobarbital (18.5 mg/kg i.p., MTC Pharmaceutical, Cambridge, ON), morphine (5 mg/kg subcutaneously (s.c.), Ontario Veterinary College, Guelph, ON), and diazepam (1 mg/kg s.c., Sabex Inc., Boucherville, QC). Rats were given atropine sulfate (4.5 mg/kg s.c., Ontario Veterinary College, Guelph, ON) just before surgery and Depocillin (300 000 IU, 0.1 ml/rat i.m., Intervet Canada, Whitby, ON) immediately following surgery. The catheter was secured to the vein with silk sutures and was passed s.c. to the top of the skull where it exited into a connector (a modified 22 G cannula; Plastics One, Roanoke, VA) mounted to the skull with jeweler's screws and dental cement. A plastic blocker was placed over the opening of the connector during the recovery period and at all other times when the rats were not in a self-administration session. To prevent clogging, catheters were flushed daily with saline and every day with 0.1 ml of a saline–heparin solution (0.2 mg/ml Hepalean 1.000 IU, Organon, Toronto, ON). Behavioral testing began after 8 days of recovery from surgery.
Apparatus
Twenty-six Plexiglas operant chambers (model ENV-008CT, Med Associates, Georgia, VT) were each enclosed in larger sound-attenuating plywood chambers (model ENV-018M, Med Associates). Each operant box had a house light (28 V) and two levers, one retractable and one stationary, located 10 cm apart and 8 cm above the floor of the box. The retractable lever (active lever) was connected to an infusion pump positioned outside the sound-insulating chamber for the delivery of drugs (Razel Scientific Instruments, Stamford, CT). The stationary lever served to control for baseline, non-reinforced operant behavior; pressing this lever had no consequence (inactive lever), but all presses were recorded. A white light (28 V) stimulus located 3 cm above the active lever was illuminated for 30 s at the beginning of the session, and for the duration of each drug infusion (5 s), serving as a discrete cue or conditioned stimulus for drug delivery. Each self-administration chamber was fitted to deliver constant-current, intermittent, inescapable, electric foot shock through a scrambler (model ENV-414, Med Associates) to the grid floor.
Procedure
The experiment consisted of three phases: self-administration, extinction, and reinstatement.
Self-administration: One 3-h self-administration session occurred every day for 7 consecutive days. Rats were transferred from their home cages to the operant chambers and their cannulas were attached to infusion lines. Each session began with the activation of the house light, the entry of the retractable lever and the illumination of the light cue for 30 s. If the rat pressed the active lever during this first 30-s presentation of the light cue, it received an infusion of heroin followed by termination of the light. Subsequently, lever-presses led to drug infusions, and activation of the light CS, according to a continuous schedule of reinforcement. Drug was infused in a volume of 150 μl over a 5-s period, and responses during this 5-s period were recorded, but did not lead to additional infusion. On the basis of number of responses emitted on the last session of self-administration, animals were assigned to three groups (n=12 each) to receive: the vehicle, 1–30 mg/kg SSR149415, and administered i.p. 30 min before behavioral testing. These routes of administration and time intervals between administration and testing were selected on the basis of previous reports on the effects of this antagonist on hormonal and behavioral responses to stressors (Griebel et al, 2002).
Extinction: The final five sessions of the experiment were all conducted in extinction conditions. These sessions were identical to the self-administration sessions except that heroin was substituted with saline. Before the first session of extinction, which occurred 48 h after the last day of self-administration, rats were pretreated with vehicle or SSR149415 in their housing colony, and 30 min later transported to the operant chambers where responding in the absence of heroin was monitored for 3 h.
Reinstatement: Following three additional extinction sessions with no pretesting injections, rats received the same treatment used in the extinction test and then were tested for stress-induced reinstatement. Forty-eight hours later, they received again the same treatment and then were tested for heroin-induced reinstatement. No extra extinction was given between the two tests. For the stress-induced reinstatement, rats were exposed to 15 min of intermittent foot shock stress (0.5 mA, 0.5 s ON, a mean OFF period of 40 s) and, immediately after this period, chambers were activated and responding was monitoring for 3 h. For heroin-induced reinstatement, rats received an injection of heroin (0.25 mg/kg s.c.), followed by a 10 min interval after which the chambers were activated and responding was monitored for 3 h.
Two days following the reinstatement session, the experiment was concluded by challenging the rats with a final injection of vehicle or SSR149415, and by exposing them to 15 min of intermittent foot shock stress (0.5 mA, 0.5 s ON, a mean OFF period of 40 s) in the operant chambers. Immediately following foot shock stress, rats were briefly exposed to CO2 (within 15 s) and killed by decapitation, and plasma obtained to measure levels of ACTH and corticosterone. Additionally, the brains of rats not exposed to AVP antagonists were extracted to measure levels of amygdalar and hypothalamic AVP mRNA expression.
Drugs and doses
For the self-administration experiments, diacetylmorphine HCl (heroin) was obtained from Almat Pharmachem (Concord, ON, Canada), and was dissolved in 0.9% physiological saline and self-administered at a dose of 0.05 mg/kg/infusion. In our laboratory, this dose has been shown to induce reliable acquisition of self-administration behavior within 7 days (Leri and Stewart, 2001). The V1b AVP receptor antagonist SSR149415 was generously donated by Sanofi-Synthélabo Recherche (Sanofi Aventis, Montpellier Cedex, France) and was suspended in physiological saline containing DMSO (5%) and Cremophor EL (5%). The two doses of SSR149415 used in this experiment are at the extreme ends of a dose-range found to be effective in producing anxiolytic-like effects in rats (Griebel et al, 2002). We selected these extreme doses because SSR149415 has never been tested in animals with a history of heroin exposure, and this treatment is likely to alter the endogenous AVP system.
Statistical analyses
One- and two-way ANOVAs with independent and repeated measures, as well as planned comparisons or t-tests, were used as appropriate for the experimental design. In case of significant interactions or significant main effects, multiple comparisons were performed using Newman–Keuls post hoc method to identify individual mean differences (α=0.05). The values on nonsignificant analyses are not reported. All statistical analyses were performed using SigmaStat (version 3.0 for Windows, SPSS Inc.).
RESULTS
Effects of Chronic Heroin Exposure and Spontaneous Heroin Withdrawal on mRNA Levels of AVP, V1b, and POMC, and on Plasma Levels of ACTH and Corticosterone
AVP mRNA levels in the amygdala and hypothalamus
In Experiment 1 (chronic heroin with early withdrawal) (Figure 1), one-way ANOVA revealed a marginally significant effect for treatment on the amygdalar AVP mRNA levels (F(2,18)=3.44, p=0.051). The rationale for post hoc tests was based on a pilot study on morphine withdrawal from chronic (10 days) intermittent escalating-does morphine (from 7.5 mg/kg/day on day 1 up to 120 mg/kg/day on day 10): the AVP mRNA levels in the amygdala were significantly higher in 12-h withdrawn rats (0.64±0.21 pg AVP mRNA/μg total RNA, n=6), than in saline controls (0.22±0.04 pg AVP mRNA/μg total RNA, n=6) (Mann–Whitney U=2.00, p<0.05). Newman–Keuls post hoc tests of Experiment 1 showed that the AVP mRNA levels in the rats withdrawn from chronic heroin for 12 h were significantly higher than those of saline controls (p<0.05).
Effects of chronic (10-day) intermittent escalating-dose heroin administration, early (12-h) and late (10-day) spontaneous heroin withdrawal on AVP mRNA levels (pg/μg RNA) in the amygdala. Data shown in graphs are treatment group mean+SEM. Significant differences are indicated: *p<0.05 vs control I.
The AVP mRNA was not altered during chronic heroin exposure (control I vs chronic heroin), nor after 10 days of withdrawal from heroin (control II vs late withdrawal).
In the hypothalamus, no significant group differences in the AVP mRNA expression were found (Table 1).
AVP V1b receptor and POMC mRNAs in the anterior pituitary or NIL/PL
In the anterior pituitary, no significant group differences in the AVP V1b receptor mRNA expression were found (Table 1).
However, one-way ANOVA revealed a significant effect for the treatment on the POMC mRNA levels (F(2,17)=11.1, p<0.001) (Figure 2). In comparison to controls, POMC mRNA levels were found to be significantly elevated in animals chronically exposed to heroin (p<0.01) and in rats in early heroin withdrawal (p<0.01). POMC mRNA levels in rats in late heroin withdrawal were similar to control animals.
Effects of chronic (10-day) intermittent escalating-dose heroin administration, early (12-h) and late (10-day) spontaneous heroin withdrawal on POMC mRNA levels (pg/μg RNA) in the anterior pituitary. Data shown in graphs are treatment group mean+SEM. Significant differences are indicated: **p<0.01 vs control I.
In the NIL/PL of the pituitary, no significant group differences in the POMC mRNA expression were found (data not shown).
Plasma levels of ACTH and corticosterone
In Experiment 1 (chronic heroin with early withdrawal), one-way ANOVA did not reveal any significant effects on plasma ACTH levels (Figure 3a). As there was a significant increase in plasma corticosterone levels during early withdrawal (see below and Figure 3b), we used a planned comparison to examine the effects on plasma ACTH during early withdrawal. There was a tendency toward an elevated level of plasma ACTH during early withdrawal (F(1,22)=3.81, p=0.06). Plasma ACTH levels in rats in late heroin withdrawal were similar to control animals.
Effects of chronic (10-day) intermittent escalating-dose heroin administration, early (12-h) and late (10-day) spontaneous heroin withdrawal on plasma hormonal levels of ACTH (pg/ml) (a) and corticosterone (ng/ml) (b). Data shown in graphs are treatment group mean+SEM. Significant differences are indicated: *p<0.05 vs control I.
As shown in Figure 3b, corticosterone levels showed a similar pattern of variation. In Experiment 1 (chronic heroin with early withdrawal), one-way ANOVA showed a significant effect for the treatment (F(2,18)=4.49, p<0.05). Multiple Newman–Keuls post hoc tests showed that plasma corticosterone was significantly elevated over control levels in animals in early withdrawal from heroin (control I vs early withdrawal, p<0.05), but not during chronic heroin exposure (control I vs chronic heroin). Plasma corticosterone levels in rats in late heroin withdrawal were similar to control animals (control II vs late withdrawal).
Effects of the Selective V1b Receptor Antagonist SSR149415 on Heroin Seeking
Behavior
A total of three animals had to be removed from the experiment because of catheter leakage or systemic infection; the data from these animals were completely eliminated from the following behavioral analyses.
Over the seven sessions of heroin self-administration, rats displayed significant increases in responding on the active lever in parallel with significant decreases in responding on the inactive lever (Figure 4; session by lever interaction: (F(6,192)=20.5, p<0.001); main effect of session: (F(6,192)=11.6, p<0.001); main effect of lever: (F(1,32)=25.1, p<0.001)). Along with increases in responding on the active lever, heroin intake significantly increased over the course of the self-administration period (Figure4; (F(6,192)=18.0, p<0.001)).
The main panel of Figure 5 represents responding on the active lever on the last session of heroin self-administration and on the first session of extinction. Just before this extinction session, rats were pretreated with different doses of SSR149415. A two-way mixed-design ANOVA comparing responding on these two sessions revealed only a significant main effect of session (F(1,30)=12.3, p<0.001). Thus, although rats injected with 30 mg/kg SSR149415 showed the lowest level of extinction responding, there was no statistically significant group difference. Similarly, a one-way independent group ANOVA revealed no significant group differences in responding on the inactive lever during the first extinction session (see smaller panel of Figure 5).
Mean (SEM) responses on the active lever and on the inactive lever during the last day of heroin self-administration and the first session of extinction given 48 h later. Thirty minutes before this extinction session, rats received injections of vehicle (n=12), SSR149415 at 1 mg/kg (n=12), and SSR149415 at 30 mg/kg (n=9). Significant difference between the last self-administration and the first extinction sessions.
To ascertain the effect of SSR149415 on heroin-seeking, we performed two separate mixed-design ANOVAs comparing responding emitted during the first hour of the last extinction session (ie, session 4) to responding emitted during the first hour following exposure to foot shock stress, and to responding emitted during the first hour following the heroin prime. As illustrated by the graphs in the left column of Figure 6, both foot shock and heroin injections induced significant reinstatement in vehicle-treated rats, but not in rats pretreated with either doses of SSR149415 (foot shock—group by session interaction: (F(2,30)=4.9, p<0.05); heroin prime—group by session interaction: (F(2,30)=3.54, p<0.05); main effect of group: (F(2,30)=3.93, p<0.05)). No significant differences in responding on the inactive lever were observed on either test of reinstatement (graphs in the right column of Figure 6).
Left column: mean (SEM) responses on the active lever during the first hour of the last day of extinction and the first hour following exposure to foot shock and to heroin during the reinstatement tests. Thirty minutes before these test sessions, rats were injected with SSR149415. No injections were given before the last session of extinction. *p<0.05 vs last day of extinction. Right column: mean (SEM) responses on the inactive lever during the same tests.
Plasma levels of ACTH and corticosterone
The three animals removed from the behavioral analyses above were also excluded from the following plasma hormonal analyses.
Basal levels of plasma ACTH and corticosterone used to establish the effects of SSR149415 on HPA axis reactivity to foot shock stress were obtained from plasma ACTH and corticosterone values observed in rats not exposed to foot shock and previously employed as control rats in a self-administration experiment performed in our laboratory. This control group (n=8) had never been exposed to drugs, but was allowed to lever press. For plasma ACTH levels, one-way ANOVA just failed to reveal a significant main effect of group (F(3,37)=2.75, p=0.056). As an increased corticosterone level after foot shock was observed (see below and Figure 7b), we used a planned comparison to examine the effects on plasma ACTH levels after foot shock stress. A planned comparison indicated that foot shock induced a significant increase in plasma ACTH levels (F(1,37)=6.41, p<0.05) and that this response was attenuated, dose-dependently, by SSR149415 (Figure 7a).
Plasma hormonal levels of ACTH (pg/ml) (a) and corticosterone (ng/ml) (b) in heroin naïve rats or heroin self-administered rats after foot shock stress with SSR149415 pretreatment. Data shown in graphs are treatment group mean+SEM. Significant differences are indicated: *p<0.05 or **p<0.01 vs basal level; ##p<0.01 vs vehicle+foot shock group.
For plasma corticosterone levels, one-way ANOVA revealed a significant main effect of group (F(3,37)=7.37, p<0.001). Multiple comparisons further found that foot shock induced a significant increase in plasma corticosterone levels (p<0.01) and that both doses of SSR149415 reduced this increase (both p<0.01) (Figure 7b).
AVP mRNA levels in the amygdala and hypothalamus
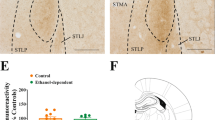
The final analysis of AVP mRNA expression in the amygdala and hypothalamus after foot shock stress included three groups: (1) the same control rats (n=8) employed in the previous analysis (ie, never exposed to drugs or foot shock); (2) foot shock control, a small group of rats (n=4) allowed to lever press for saline and then exposed to foot shock; and (3) rats (n=9) in the vehicle pretreatment group used in the present heroin self-administration experiment. As shown in Figure 8, the ANOVA revealed a significant main effect of group (F(2,18)=7.83, p<0.01), and foot shock induced a significant increase in AVP mRNA levels in the amygdala (p<0.01) in rats withdrawn from heroin self-administration, but not in heroin naïve rats. There was no change in the hypothalamus (Figure 8).
DISCUSSION
The first objective of these experiments was to investigate the effects of chronic intermittent escalating-dose heroin administration, early spontaneous withdrawal (12 h), and late spontaneous withdrawal (10 days) on two stress responsive systems: AVP in the amygdala and the HPA axis. AVP mRNA levels in the amygdala were not altered during chronic heroin exposure. However, we found that early spontaneous withdrawal was associated with increases in amygdalar AVP mRNA level, which were found to be nearly 2.5 times higher than levels observed in control rats. This effect occurred primarily during early withdrawal, because we noted no significant increases in AVP mRNA levels in animals after 10 days following the last heroin injection. Furthermore, this effect was tissue-specific, as we observed no effect of early heroin withdrawal in the hypothalamus, where AVP mRNA is constitutively expressed. The increase in amygdalar AVP mRNA levels during early heroin withdrawal suggests an enhanced AVP biosynthesis. It has been demonstrated that acute stress stimulates AVP release in the amygdala (Ebner et al, 2002). Although the stimulatory factors influencing elevation of AVP mRNA levels are not yet fully elucidated, it is possible that an augmented AVP release is responsible for the increase in AVP mRNA to compensate for early heroin withdrawal-induced peptide depletion. Nevertheless, this novel finding in heroin-treated rats parallels our recent studies demonstrating an increased AVP mRNA level in the amygdala during early cocaine withdrawal (Zhou et al, 2005).
Acute opiate exposure to opiate naïve rats stimulates HPA activity, as reflected by a significant elevation of plasma ACTH and corticosterone levels (Buckingham and Cooper, 1984; Ignar and Kuhn, 1990; Zhou et al, 2006). In this study, after 10 days of chronic intermittent escalating-dose heroin administration, however, the HPA hormonal levels did not show responses to heroin, indicating adaptation or tolerance of HPA activity to chronic heroin. In early withdrawal phase (12 h after the last heroin injection), plasma corticosterone levels were significantly elevated. These results are in line with earlier findings of HPA axis activation by opiate withdrawal, after tolerance has developed following chronic morphine exposure (Ignar and Kuhn, 1990; Zhou et al, 2006). As reported before, a blunting of HPA axis activity in response to chronic opiates is associated with an opiate-induced reduction of CRF gene expression in the hypothalamus (Milanes et al, 2002). Chronic intermittent exposure to opiates is a chronic stressor (Houshyar et al, 2003), and it may modulate the responsivity of the HPA axis at the corticotrope level, as do many other stressors (Shiomi et al, 1986; Zhou et al, 2003). In the present study, there was a significant increase of POMC mRNA levels in the anterior pituitary after chronic heroin. Our study on heroin withdrawal further showed that the POMC mRNA increase induced by chronic heroin persisted 12 h into acute withdrawal, and was coupled with an activation of the HPA axis by early withdrawal. Taken together, our results suggest that chronic heroin may modulate corticotrope responsivity to hypothalamic CRF and/or AVP input through the induction of POMC gene expression in the anterior pituitary, with resultant increases of the HPA activity in early withdrawal.
The second objective of these experiments was to investigate the potential of the V1b receptor blockade in reducing heroin seeking in tests for reinstatement induced by foot shock stress and heroin priming in rats trained to self-administer heroin. SSR149415, a systemically active, selective, non-peptide V1b receptor antagonist, significantly reduced foot shock-induced reinstatement and blocked heroin-induced reinstatement in dose-dependent manners. It is unlikely that this resulted from a suppression of general mobility by SSR149415 because, even at the highest dose tested during the first extinction session, the 12 rats still emitted a total of 614 responses in 3 h, with a range between 15 and 123 responses. Furthermore, the well-established anxiolytic profile of SSR149415 (Griebel et al, 2002) is based on performance on tests whereby reductions in anxiety are indexed by enhanced motor activity. These results suggest that stress responsive AVP activation on V1b receptors plays a critical role in modulating the effects of stress on reinstatement of heroin seeking.
This modulation may occur in the amygdala, and may involve an interaction with local noradrenergic (NA) systems. In fact, infusions of noradrenaline in the amygdala have been found to increase local AVP release (Raber and Bloom, 1996). In addition, both the basolateral and central nucleus of the amygdala receive NA projections that are sensitive to stress and to adrenergic manipulations (Quirarte et al, 1998). Exposure to foot shock, for example, increases NA release in these regions (Quirarte et al, 1998; Hatfield et al, 1999; Erb et al, 2000). Also, partial 6-hydroxydopamine lesions of the ventral NA bundle projecting to the amygdala attenuate foot shock-induced reinstatement of heroin seeking (Shaham et al, 2000b), and blockade of beta-NA receptors within the central amygdala block the stress-induced reinstatement (Leri et al, 2002). In the present studies, we found that the AVP mRNA levels were enhanced by foot shock in the amygdala of rats withdrawn from heroin self-administration but not in the amygdala of the heroin naïve rats. Thus, although this is a tentative interpretation, which requires additional investigation, our data suggest that the NA–AVP interaction within the amygdala may be involved in heroin-seeking behaviors precipitated by stress.
Opioid receptors within the amygdala may also be involved in drug seeking, especially as a result of heroin priming. In fact, it is well known that the effect of heroin primes on reinstatement is dependent on activation of mu-opioid receptor (MOP-r) (de Wit and Stewart, 1983; Shaham et al, 1996; Leri et al, 2004). In the paraventricular nucleus of the hypothalamus, AVP-producing parvocellular cells express MOP-rs, and activity of these cells is under tonic inhibition by endogenous opioids (Nikolarakis et al, 1987). In the amygdala, it is not clear whether there is a direct interaction between AVP-producing cells and MOP-r activity. Despite an increased MOP-r binding density, earlier studies have found a decrease in MOP-r-stimulated G-protein (as reflected by GTPγS binding) in the rat amygdala after chronic heroin self-administration (Sim-Selley et al, 2000; Kruzich et al, 2003), suggesting involvement of amygdalar MOP-r desensitization in heroin dependence. Our recent finding that cocaine withdrawal stress increases the AVP mRNA in the amygdala through opioid receptors, suggests a functional interaction between the opioidergic and AVPergic systems in the amygdala (Zhou et al, 2005). However, in the present study, we found that amygdalar MOP-r mRNA levels were not affected by either chronic heroin or heroin withdrawal (data not shown). Therefore, further time-course studies are necessary before alternative explanations, such as indirect amygdalar activation due to extra-amygdalar opioid action can be ruled out (eg, in the nucleus accumbens core during opiate or cocaine withdrawal) (Yao et al, 2005; Leri et al, 2006; Zhou et al, 2006).
Interestingly, earlier studies have found that another neuropeptide related to the stress hormone, that is, oxytocin, had an effect opposite to that of AVP on heroin self-administration behavior (van Ree and De Wied, 1977; see review by van Ree et al, 1999). The central amygdala expresses relatively high levels of receptors for both AVP and oxytocin (Huber et al, 2005; Stemmelin et al, 2005). Activation of AVP and oxytocin receptors has opposite effects on anxiety-related behaviors, fear- and stress-related responses (Landgraf and Neumann, 2004; Huber et al, 2005). Whether oxytocin and its receptor are involved in modulating drug-seeking behaviors, with a potential interaction with AVP/V1b receptor systems, is under investigation in our laboratories.
In summary, these studies in rats demonstrated that early heroin withdrawal is associated with a significant increase in amygdalar AVP mRNA levels. In line with this finding, we have recently found increases in amygdalar AVP mRNA levels during early cocaine withdrawal as well (Zhou et al, 2005). Furthermore, the selective V1b receptor antagonist SSR149415 attenuated heroin seeking during stress- and heroin-induced reinstatement. Because activation of the HPA activity stimulated by foot shock was blunted by SSR149415 in a dose-dependent manner, and because AVP gene expression was increased by foot shock in the amygdala of rats that had self-administered heroin only, we suggest that AVP-V1b systems may be a critical component of a neural circuitry underlying the aversive emotional consequences of drug withdrawal, as well as the effect of negative emotional states on drug-seeking behavior. To our best knowledge, SSR149415 is the only systemically available compound identified in reinstatement studies to reduce stress- and drug-induced reinstatement of heroin seeking. Such latter finding suggests that it may be worthwhile to explore the usefulness of systemically effective V1b receptor antagonists for the management of withdrawal and for the prevention of relapse.
References
Aguilera G, Rabadan-Diehl C (2000). Vasopressinergic regulation of the hypothalamic-pituitary-adrenal axis: implications for stress adaptation. Regul Pept 96: 23–29.
Bossert JM, Ghitza UE, Lu L, Epstein DH, Shaham Y (2005). Neurobiology of relapse to heroin and cocaine seeking: an update and clinical implications. Eur J Pharmacol 526: 36–50.
Branch A, Unterwald E, Lee S, Kreek MJ (1992). Quantitation of preproenkephalin mRNA levels in brain regions from male Fischer rats following chronic cocaine treatment using a recently developed solution hybridization assay. Mol Brain Res 14: 231–238.
Buckingham JC, Cooper TA (1984). Differences in hypothalamo-pituitary-adrenocortical activity in the rat after acute and prolonged treatment with morphine. Neuroendocrinology 38: 411–417.
De Vry J, Donselaar I, van Ree JM (1988). Effects of desglycinamide9, (Arg8) vasopressin and vasopressin antiserum on the acquisition of intravenous cocaine self-administration in the rat. Life Sci 42: 2709–2715.
De Wied D, Diamant M, Fodor M (1993). Central nervous system effects of the neurohypophyseal hormones and related peptides. Front Neuroendocrinol 14: 251–302.
De Wit H, Stewart J (1983). Drug reinstatement of heroin-reinforced responding in the rat. Psychopharmacology 79: 29–31.
Ebner K, Wotjak C, Landgraf R, Engelmann M (2002). Forced swimming triggers vasopressin release within the amygdala to modulate stress-coping strategies in rats. Eur J Neurosci 15: 384–388.
Erb S, Hitchcott PK, Rajabi H, Mueller D, Shaham Y, Stewart J (2000). Alpha-2 adrenergic receptor agonists block stress-induced reinstatement of cocaine seeking. Neuropsychopharmacology 23: 138–150.
Erb S, Shaham Y, Stewart J (1996). Stress reinstates cocaine-seeking behavior after prolonged extinction and a drug-free period. Psychopharmacology 128: 408–412.
Erb S, Shaham Y, Stewart J (1998). The role of corticotropin-releasing factor and corticosterone in stress- and cocaine-induced relapse to cocaine seeking in rats. J Neurosci 18: 5529–5536.
Erb S, Stewart J (1999). A role for the bed nucleus of the stria terminalis, but not the amygdala, in the effects of corticotropin-releasing factor on stress-induced reinstatement of cocaine seeking. J Neurosci 19: RC35.
Griebel G, Simiand J, Serradeil-Le Gal C, Wagnon J, Pascal M, Scatton B et al. (2002). Anxiolytic- and antidepressant-like effects of the non-peptide vasopressin V1b receptor antagonist, SSR149415, suggest an innovative approach for the treatment of stress-related disorders. Proc Natl Acad Sci USA 99: 6370–6375.
Griebel G, Stemmelin J, Gal CS, Soubrie P (2005). Non-peptide vasopressin V1b receptor antagonists as potential drugs for the treatment of stress-related disorders. Curr Pharm Des 11: 1549–1559.
Guillon G, Derick S, Pena A, Cheng LL, Stoev S, Seyer R et al. (2004). The discovery of novel vasopressin V1b receptor ligands for pharmacological, functional and structural investigations. J Neuroendocrinol 16: 356–361.
Hatfield T, Spanis C, McGaugh JL (1999). Response of amygdalar norepinephrine to footshock and GABAergic drugs using in vivo microdialysis and HPLC. Brain Res 835: 340–345.
Houshyar H, Gomez F, Manalo S, Bhargava A, Dallman MF (2003). Intermittent morphine administration induces dependence and is a chronic stressor in rats. Neuropsychopharmacology 28: 1960–1971.
Huber D, Veinante P, Stoop R (2005). Vasopressin and oxytocin excite distinct neuronal populations in the central amygdala. Science 308: 245–248.
Ignar DM, Kuhn CM (1990). Effects of specific mu and kappa opiate tolerance and abstinence on hypothalamo-pituitary-adrenal axis secretion in the rat. J Pharmacol Exp Ther 225: 1287–1295.
Koob GF, Le Moal M (1997). Drug abuse: hedonic homeostatic dysregulation. Science 278: 52–58.
Kreek MJ, Borg L, Zhou Y, Schluger J (2002). Relationships between endocrine functions and substance abuse syndromes: heroin and related short-acting opiates in addiction contrasted with methadone and other long-acting opioid agonists used in pharmacotherapy of addiction. In: Pfaff DW (eds). Hormones, Brain and Behavior. Academic Press: San Diego. pp 781–830.
Kreek MJ, Koob GF (1998). Drug dependence: stress and dysregulation of brain reward pathways. Drug Alcohol Depend 51: 23–47.
Kruzich PJ, Chen AC, Unterwald EM, Kreek MJ (2003). Subject-regulated dosing alters morphine self-administration behavior and morphine-stimulated [35S]GTPgammaS binding. Synapse 47: 243–249.
Landgraf R, Neumann ID (2004). Vasopressin and oxytocin release within the brain: a dynamic concept of multiple and variable modes of neuropeptide communication. Front Neuroendocrinol 25: 150–176.
Leri F, Flores J, Rodaros D, Stewart J (2002). Blockade of stress-induced but not cocaine-induced reinstatement by infusion of noradrenergic antagonists into the bed nucleus of the stria terminalis or the central nucleus of the amygdala. J Neurosci 22: 5713–5718.
Leri F, Stewart J (2001). Drug-induced reinstatement to heroin and cocaine seeking: a rodent model of relapse in poly-drug use. Exp Clin Psychopharmacol 9: 297–306.
Leri F, Tremblay A, Sorge RE, Stewart J (2004). Methadone maintenance reduces heroin- and cocaine-induced relapse without affecting stress-induced relapse in a rodent model of poly-drug use. Neuropsychopharmacology 29: 1312–1320.
Leri F, Zhou Y, Goddard B, Cummins E, Kreek MJ (2006). Effects of high dose methadone maintenance on cocaine place conditioning, cocaine self-administration, and mu-opioid receptor mRNA expression in the rat brain. Neuropsychopharmacology 31: 1462–1474.
Markou A, Kosten TR, Koob GF (1998). Neurobiological similarities in depression and drug dependence: a self-medication hypothesis. Neuropsychopharmacology 18: 135–174.
McFarland K, Davidge SB, Lapish CC, Kalivas PW (2004). Limbic and motor circuitry underlying footshock-induced reinstatement of cocaine-seeking behavior. J Neurosci 24: 1551–1560.
Milanes MV, Laorden ML, Angel E, Tankosic P, Burlet A (2002). Effect of naloxone-precipitated morphine withdrawal on CRH and vasopressin mRNA expression in the rat hypothalamic paraventricular nucleus. Neurosci Lett 15: 586–591.
Nikolarakis KE, Almeida OFX, Herz A (1987). Feedback inhibition of opioid peptide release in the hypothalamus of the rat. Neuroscience 23: 143–148.
Overstreet DH, Griebel G (2005). Antidepressant-like effects of the vasopressin V1b receptor antagonist SSR149415 in the Flinders Sensitive Line rat. Pharmacol Biochem Behav 82: 223–227.
Paxinos G, Watson C (1986). The Rat Brain in Stereotaxic Coordinates. 2nd edn. Academic Press: New York, NY.
Post RM, Contel NR, Gold P (1982). Impaired behavioral sensitization to cocaine in vasopressin deficient rats. Life Sci 31: 2745–2750.
Quirarte GL, Galvez R, Roozendaal B, McGaugh JL (1998). Norepinephrine release in the amygdala in response to footshock and opioid peptidergic drugs. Brain Res 808: 134–140.
Raber J, Bloom FE (1996). Arginine vasopressin release by acetylcholine or norepinephrine: region-specific and cytokine-specific regulation. Neuroscience 71: 747–759.
Serradeil-Le GC, Derick S, Brossard G, Manning M, Simiand J, Gaillard R et al. (2003). Functional and pharmacological characterization of the first specific agonist and antagonist for the V1b receptor in mammals. Stress 6: 199–206.
Shaham Y, Erb S, Stewart J (2000a). Stress-induced relapse to heroin and cocaine seeking in rats: a review. Brain Res Rev 33: 13–33.
Shaham Y, Funk D, Erb S, Brown TJ, Walker CD, Stewart J (1997). Corticotropin-releasing factor, but not corticosterone, is involved in stress-induced relapse to heroin seeking in rats. J Neurosci 17: 2605–2614.
Shaham Y, Highfield D, Delfs J, Leung S, Stewart J (2000b). Clonidine blocks stress-induced reinstatement of heroin seeking in rats: an effect independent of locus coeruleus noradrenergic neurons. Eur J Neurosci 12: 292–302.
Shaham Y, Rajabi H, Stewart J (1996). Relapse to heroin-seeking in rats under opioid maintenance: the effects of stress, heroin, priming and withdrawal. J Neurosci 16: 1957–1963.
Shaham Y, Shalev U, Lu L, de Wit H, Stewart J (2003). The reinstatement model of drug relapse: history, methodology and major findings. Psychopharmacology 168: 3–20.
Shiomi H, Watson SJ, Kelsey JE, Akil H (1986). Pretranslational and posttranslational mechanisms for regulation beta-endorphin-adrenocorticotropin of the anterior pituitary lobe. Endocrinology 119: 1793–1799.
Sim-Selley LJ, Selley DE, Vogt LJ, Childers SR, Martin TJ (2000). Chronic heroin self-administration desensitizes mu opioid receptor-activated G-proteins in specific regions of rat brain. J Neurosci 20: 4555–4562.
Sinha R (2001). How does stress increase risk of drug abuse and relapse? Psychopharmacology 158: 343–359.
Sinha R, Catapano D, O'Malley S (1999). Stress-induced craving and stress response in cocaine dependent individuals. Psychopharmacology 142: 343–351.
Sinha R, Garcia M, Paliwal P, Kreek MJ, Rounsaville BJ (2006). Stress-induced cocaine craving and hypothalamic–pituitary–adrenal responses are predictive of cocaine relapse outcomes. Arch Gen Psychiatry 63: 324–331.
Stemmelin J, Lukovic L, Salome N, Griebel G (2005). Evidence that the lateral septum is involved in the antidepressant-like effects of the vasopressin V1b receptor antagonist, SSR149415. Neuropsychopharmacology 30: 35–42.
Stewart J (2000). Pathways to relapse: the neurobiology of drug- and stress-induced relapse to drug-taking. J Psychiatry Neurosci 25: 125–136.
Stewart J (2003). Stress and relapse to drug seeking: studies in laboratory animals shed light on mechanisms and sources of long-term vulnerability. Am J Addict 12: 1–17.
van Ree JM, Burbach-Bloemarts EM, Wallace M (1988). Vasopressin neuropeptides and acquisition of heroin and cocaine self-administration in rats. Life Sci 42: 1091–1099.
van Ree JM, De Wied D (1977). Modulation of heroin self-administration by neurohypophyseal principles. Eur J Pharmacol 43: 199–202.
van Ree JM, Gerrits MAFM, Vanderschuren LJMJ (1999). Opioids, reward and addiction: an encounter of biology, psychology, and medicine. Pharmacol Rev 51: 341–396.
Wigger A, Sánchez MM, Mathys KC, Ebner K, Frank E, Liu D et al. (2004). Alterations in central neuropeptide expression, release, and receptor binding in rats bred for high anxiety: critical role of vasopressin. Neuropsychopharmacology 29: 1–14.
Yao L, McFarland K, Fan P, Jiang Z, Inoue Y, Diamond I (2005). Activator of G protein signaling 3 regulates opiate activation of protein kinase A signaling and relapse of heroin-seeking behavior. Proc Natl Acad Sci USA 102: 8746–8751.
Zhou Y, Bendor JT, Hofmann L, Randesi M, Ho A, Kreek MJ (2006). Mu opioid receptor and orexin/hypocretin mRNA levels in the lateral hypothalamus and striatum are enhanced by morphine withdrawal. J Endocrinol 191: 137–145.
Zhou Y, Bendor JT, Yuferov V, Schlussman SD, Ho A, Kreek MJ (2005). Amygdalar vasopressin mRNA increases in acute cocaine withdrawal: evidence for opioid receptor modulation. Neuroscience 134: 1391–1397.
Zhou Y, Spangler R, LaForge KS, Maggos CE, Ho A, Kreek MJ (1996). Corticotropin-releasing factor and type 1 corticotropin-releasing factor receptor messenger RNAs in rat brain and pituitary during ‘binge’ pattern cocaine administration and chronic withdrawal. J Pharmacol Exp Ther 279: 351–358.
Zhou Y, Spangler R, Schlussman SD, Ho A, Kreek MJ (2003). Alterations in hypothalamic–pituitary–adrenal axis activity and in levels of proopiomelanocortin and corticotrophin-releasing hormone receptor 1 mRNAs in the pituitary and hypothalamus of the rat during chronic ‘binge’ cocaine and withdrawal. Brain Res 964: 187–199.
Acknowledgements
We thank Dr G Aguilera for providing the AVP and V1b receptor cDNAs; Dr J Roberts for the POMC cDNA; Drs T Nilsen and P Maroney for the 18S DNA. The work was supported by NIDA Center Grant DA-P60-05130, DA-00049 (MJK) and the Natural Sciences and Engineering Research Council of Canada (NSERC) (FL).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhou, Y., Leri, F., Cummins, E. et al. Involvement of Arginine Vasopressin and V1b Receptor in Heroin Withdrawal and Heroin Seeking Precipitated by Stress and by Heroin. Neuropsychopharmacol 33, 226–236 (2008). https://doi.org/10.1038/sj.npp.1301419
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1301419
Keywords
This article is cited by
-
Complex formation between the vasopressin 1b receptor, β-arrestin-2, and the μ-opioid receptor underlies morphine tolerance
Nature Neuroscience (2018)
-
Oprm1 A112G, a single nucleotide polymorphism, alters expression of stress-responsive genes in multiple brain regions in male and female mice
Psychopharmacology (2018)
-
NF-κB signaling and vesicle transport are correlated with the reactivation of the memory trace of morphine dependence
Diagnostic Pathology (2014)
-
Chronic psychosocial stress causes delayed extinction and exacerbates reinstatement of ethanol-induced conditioned place preference in mice
Psychopharmacology (2014)
-
Tolerance and sensitization to chronic escalating dose heroin following extended withdrawal in Fischer rats: possible role of mu-opioid receptors
Psychopharmacology (2013)