Abstract
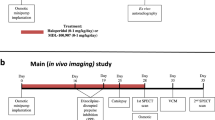
SSR181507 ((3-exo)-8-benzoyl-N-[[(2S)7-chloro-2,3-dihydro-1,4-benzodioxin-1-yl]methyl]-8-azabicyclo[3.2.1]octane-3-methanamine monohydrochloride) is a novel tropanemethanamine benzodioxane derivative that possesses high and selective affinities for D2-like and 5-HT1A receptors (KI=0.8, 0.2, and 0.2 nM for human D2, D3, and 5-HT1A, respectively). In vivo, SSR181507 inhibited [3H]raclopride binding to D2 receptors in the rat (ID50=0.9 and 1 mg/kg, i.p. in limbic system and striatum, respectively). It displayed D2 antagonist and 5-HT1A agonist properties in the same concentration range in vitro (IC50=5.3 nM and EC50=2.3 nM, respectively, in the GTPγS model) and in the same dose range in vivo (ED50=1.6 and 0.7 mg/kg, i.p. on striatal DA and 5-HT synthesis, respectively, and 0.03–0.3 mg/kg, i.v. on dorsal raphe nucleus firing rate). It selectively enhanced Fos immunoreactivity in mesocorticolimbic areas as compared to the striatum. This regional selectivity was confirmed in electrophysiological studies where SSR181507, given acutely (0.1–3 mg/kg, i.p.) or chronically (3 mg/kg, i.p., o.d., 22 days), increased or decreased, respectively, the number of spontaneous active DA cells in the ventral tegmental area, but not in the substantia nigra. Moreover, SSR181507 increased both basal and phasic DA efflux (as assessed by microdialysis and electrochemistry) in the medial prefrontal cortex and nucleus accumbens, but not in the striatum. This study shows that the combination of D2 receptor antagonism and 5-HT1A agonism, in the same dose range, confers on SSR181507 a unique neurochemical and electrophysiological profile and suggests the potential of this compound for the treatment of the main dimensions of schizophrenia.
Similar content being viewed by others
INTRODUCTION
Schizophrenia is a devastating psychiatric disorder characterized by a diversity of symptoms: the so-called positive symptoms (such as delusions and hallucinations), negative symptoms (such as blunted affect and social withdrawal), as well as cognitive-attentional deficits. While classical antipsychotics do show efficacy against the positive symptoms of schizophrenia, negative symptoms and cognitive defects are clearly less responsive to therapeutic intervention. The main limit to their clinical use, however, resides in their side effects, such as extrapyramidal signs (EPS), neuroendocrine disturbances, sexual dysfunction, orthostatic hypotension, weight gain, and excessive sedation. A second generation of antipsychotics, commonly referred to as ‘atypical antipsychotics’, is characterized by a modest progress in effect on positive symptoms of schizophrenia, but by an improved separation of efficacy against the positive symptoms and the induction of EPS, and by some efficiency on the cognitive symptoms of schizophrenia (Meltzer and McGurk, 1999). Conceptually, their putative mechanisms are related to a limbic selectivity characterized by a selective blockade of limbic dopaminergic neurotransmission. The predominant profile of these atypical antipsychotics appears to be blockade of both 5-HT2A and DA D2 receptors (multireceptor concept). Indeed, although activity at 5-HT2A receptors is not essential for antipsychotic efficacy, it has been proposed that the atypical clinical profile of several antipsychotics could be related to their ratio of affinities for 5-HT2A and DA D2 receptors (Meltzer, 1999; Scatton and Sanger, 2000). Some of them also interact with additional receptors such as α-adrenergic receptor subtypes, histamine H1, or muscarinic receptors (Miyamoto et al, 2000). The multiplicity of pharmacological targets for these atypical antipsychotics not only fuels the debate about the therapeutically relevant mechanism for such drugs, but also leads to a side-effect profile, besides EPS, that remains open for improvement. That highly selective DA D2 and D3 receptor blockade is sufficient to reveal limbic selectivity is demonstrated by amisulpride, which shows atypical antipsychotic activity and also an improved efficacy against the primary negative symptoms of schizophrenia (Boyer et al, 1995).
Although atypical antipsychotics have been a major advance in the treatment of schizophrenia, there is still a need for improvement, as a significant proportion of patients remain refractory to treatment, and negative and cognitive symptoms are little improved by current treatment. Recent preclinical and clinical data have suggested that combining antagonist activity at DA D2 receptors with agonist activity at 5-HT1A receptors might offer a promising alternative to schizophrenia treatment (see Meltzer and McGurk, 1999; Millan, 2000; Ichikawa et al, 2001; Bantick et al, 2001 for reviews).
Autoradiographic studies in post-mortem schizophrenic patients have shown that 5-HT1A binding site densities are increased in the dorsolateral prefrontal cortex and orbital frontal cortex (Burnet et al, 1996; Simpson et al, 1996) and PET studies recently revealed an increase in cortical 5-HT1A receptor binding in schizophrenia (Kasper et al, 2002), thus suggesting that the 5-HT1A receptor may indeed be implicated in this disease or its manifestations. Furthermore, 5-HT1A agonists attenuate certain DA D2 receptor-mediated motor side effects: 8-OH-DPAT and ipsapirone, two prototypical 5-HT1A receptor agonists, prevent or reduce haloperidol-induced catalepsy in rodents (Wadenberg and Ahlenius, 1991). In clinical studies, signs of Parkinsonism were improved by the addition of buspirone (Goff et al, 1991) to neuroleptic-treated schizophrenic patients. Thus, DA D2 receptor antagonists with high affinity and agonist properties at the 5-HT1A receptor should have a low incidence of EPS. Moreover, recent work with tandospirone (Sumiyoshi et al, 2000, 2001) have suggested the usefulness of 5-HT1A agonists for improving cognition in patients with schizophrenia. It has also been proposed that the ability of atypical antipsychotics to alleviate the negative and cognitive symptoms of schizophrenia is related to the fact that they enhance DA release in the medial prefrontal cortex (Kapur and Remington, 1996). As selective 5-HT1A agonists increase DA release in this structure (Arborelius et al, 1993), this property may lead to efficacy against the negative-cognitive symptomatology in schizophrenia. Finally, since stress and anxiety are often associated with schizophrenic episodes (Liberman and Corrigan, 1992) and because up to 75% of first diagnosed schizophrenics are depressed (Koreen et al, 1993), relief of these symptoms is also a desirable property. Along with anxiolysis (Borison et al, 1990), antidepressant activity has also been associated with 5-HT1A agonism (Robinson et al, 1989), thus suggesting that compounds with this activity should have additional advantages on schizophrenia-associated mood disorders.
We have recently synthesized a compound, SSR181507 (Figure 1), which combines DA D2 antagonism and 5-HT1A agonism in the same concentration and dose range. In the present study, we report on the binding profile of this compound and its intrinsic and functional activity at these two receptors, on its electrophysiological (firing of serotonergic cell bodies of dorsal raphe nucleus (DRN), number of active cells in DA cell bodies) and neurochemical (Fos expression, basal and evoked DA efflux) profile in support of the above-mentioned hypothesis. A companion paper (Depoortere et al, 2003) provides further psychopharmacological evidence to this end.
MATERIALS AND METHODS
Animals
Unless otherwise indicated, adult male Sprague–Dawley rats (OFA from Iffa Credo, Les Oncins, France or COBS from Charles River, St Aubin-les-Elbeuf, France) and Dunkin Hartley guinea-pigs (Iffa Credo) were used. All experiments were performed in accordance with the ‘Guide and Care and Use of Laboratory Animals’ (National Institutes of Health) and were approved by the in-house Animal Ethics Committee.
Material and Drugs
SSR181507 ((3-exo)-8-benzoyl-N-[[(2S)7-chloro-2,3-dihydro-1,4-benzodioxin-1-yl]methyl]-8-azabicyclo[3.2.1]octane- 3-methanamine monohydrochloride), WAY100635, amisulpride, clozapine, olanzapine, haloperidol, eliprodil, paroxetine, NAN-190, and 8-OH-DPAT were synthesized by the Chemistry Department of Sanofi-Synthelabo Recherche. Other chemicals (apomorphine, pargyline) were obtained commercially at the highest purity available.
Drugs were administered by the i.p. route, except when indicated otherwise; control groups received an equal volume of the corresponding vehicle. Doses refer to the free base equivalent. Pargyline, clozapine, and haloperidol were dissolved in saline (0.9% NaCl). SSR181507 and WAY100635 were suspended with Tween 80 (0.1%) in saline vehicle.
Radioligand-Binding Studies In Vitro
Studies of radioligand binding to animal receptors were performed essentially as described by the authors indicated: the DA D2 receptor in rat striatum (0.3 nM [3H]spiperone, Briley and Langer, 1978), the DA D3 receptor in bovine caudate nucleus (0.8 nM [3H]7-OH-DPAT in the presence of 0.2 μM eliprodil, Schoemaker, 1993), the serotonin 5-HT1A receptor in rat hippocampus (1 nM [3H]8-OH-DPAT in the presence of 3 μM paroxetine, Sanger and Schoemaker, 1992; Schoemaker and Langer, 1986). Assay conditions and references for competition binding studies at human receptor subtypes are summarized in Table 2. Results were evaluated as the drug concentration required to inhibit 50% of specific radioligand binding and converted to KI values as described by Cheng and Prusoff (1973).
Radioligand Binding Studies In Vivo
[3H]raclopride selectively recognizes DA D2-like receptors in vitro and was used to label these receptors in vivo (Köhler et al, 1985). [3H]raclopride (60–87 Ci/mmol, NEN Life Science Products, Boston, MA, USA) was injected (9 μCi/200 μl) into the tail vein of rats, 45 min before being killed. Test drugs or vehicle were administered in a final volume of 550 μl, either 45 min (SSR181507) or 75 min (haloperidol, amisulpride) before [3H]raclopride. The striatum and the limbic system (nucleus accumbens, septum, and olfactory tubercle) were dissected by hand, and tissue radioactivity was measured after overnight digestion in 0.5 ml Soluene. Nonspecific binding for the fitting of the competition curves was defined in the presence of haloperidol (1 mg/kg, i.p.).
[35S]GTPγS Binding at Human D2 and 5-HT1A Receptors
Functional activity at D2 and 5-HT1A receptors was evaluated using [35S]GTPγS binding. Assays were carried out essentially as described by Newman-Tancredi et al (1999) with some minor modifications. Briefly, membranes (7–11 μg protein) from CHO cells recombinantly expressing the human D2 (2 pmol/mg membrane protein, Receptor Biology, Baltimore, MD, USA) or 5-HT1A receptor (1.2 pmol/mg membrane protein, CRM-0.35, NEN Life Science Products) were incubated at room temperature (75 and 40 min, respectively) with agonists and/or antagonists and 0.1 nM [35S]GTPγS (1065 Ci/mmol; Amersham Pharmacia Biotech, England) in a final volume of 100 μl of 20 mM HEPES buffer (pH 7.4), containing 3 mM MgSO4, 3 μM GDP, 1 mM dithiothreitol, and 150 mM NaCl. Nonspecific binding was determined with 20 μM unlabeled GTPγS. Results were expressed as EC50 (concentration of the compound producing 50% effect) and IC50 (concentration of the compound producing 50% inhibition of the dopamine response) and were obtained by nonlinear regression analysis.
In Vitro Dopamine Release
The modulation of electrically evoked [3H]dopamine release from slices of rat striatum was performed essentially as described by Schoemaker et al (1997). Briefly, slices were incubated with 0.1 μM [3H]dopamine for 30 min at 37°C in Krebs buffer (mM: NaCl, 118; KCl, 4.7; CaCl2, 1.3; MgCl2, 1.2; NaH2PO4, 1.0; NaHCO3, 25.0; glucose, 11.1; EDTA, 0.004, equilibrated with 5% CO2/95% O2), washed, and superfused with Krebs buffer for 90 min at a flow rate of 0.7 ml/min. After this period, fractions (5 ml) were collected until the end of the experiment. Two 2-min periods of electrical field stimulation (rectangular pulses of 2 ms and 16 mA; 3 Hz) were applied to each slice 110 and 160 min after the beginning of superfusion. Apomorphine was added to the superfusion buffer starting 20 min before the second stimulation period. When the interaction between SSR181507 and apomorphine was studied, SSR181507 was present in the superfusion buffer 20 min before the first stimulation period. The stimulation-evoked [3H]dopamine overflow (S1 and S2, respectively) was calculated with respect to the spontaneous outflow (sp1 and sp2, respectively) in the fractions immediately before the stimulation. Apparent pA2 values were determined as pA2=log ([E′]/[E]−1)−log [B]), where [E′] and [E] are the concentrations of the agonist producing the half-maximal effect in the presence and the absence of the antagonist, respectively, and [B] the concentration of the antagonist (Furchgott, 1972).
Measurement of Dopamine and Serotonin Synthesis Rates
The rate of DA and serotonin (5-HT) synthesis was estimated by measuring the accumulation of dihydroxyphenylalanine (L-DOPA) and 5-hydroxytryptophane (5-HTP), respectively, after administration of 100 mg/kg, i.p. of the aromatic L-amino acid decarboxylase inhibitor NSD-1015 (Schoemaker et al, 1997). At 1 h after administration of SSR181507 (0.3–10 mg/kg, i.p.) and 30 min after the administration of NSD-1015, rats were killed by decapitation and different brain structures (striatum, hippocampus, limbic system (nucleus accumbens, septum, and olfactory tubercle), cortex) were dissected on ice. Brain structures were then weighed, homogenized in 20 volumes of 0.1 N HClO4 and centrifuged at 10 000 g for 10 min. L-DOPA and 5-HTP levels were measured in the supernatant by HPLC with electrochemical detection as described previously (Schoemaker et al, 1997).
Identical procedures were used in rats chronically treated with SSR181507 (3 or 10 mg/kg, i.p, b.i.d. for 20 days). In this case, SSR181507 was administered acutely at the dose of 3 mg/kg, i.p., 72 h after the last injection of the repeated treatment of vehicle control or SSR181507.
In Vivo Recording of Dorsal Raphe Neuronal Firing
Rats were anesthetized with chloral hydrate (400 mg/kg, i.p.) and were mounted in a stereotaxic frame after femoral vein cannulation. Additional doses of chloral hydrate were administered to maintain surgical anesthesia throughout the experiment. A burr hole was drilled into the skull over the DRN and tungsten electrodes were lowered (0.5–1 mm anterior to lambda, on the midline, 4.5–5.5 mm under the cortical surface, according to the atlas of Paxinos and Watson (1998)) for recording spontaneous cell unit activity. Action potentials were amplified and counted by 10-s periods with a spike discriminator connected to a computer driven by the software (Haigler and Aghajanian, 1974). SSR181507 (0.01–0.3 mg/kg, i.v.) was injected and its effect expressed as percentage of baseline firing rate. For antagonist studies, vehicle or WAY100635 (0.1 mg/kg, i.v.) was administered 5 min later.
In Vivo Recording of the Number of Spontaneously Active DA Cells
Rats were anesthetized with chloral hydrate (400 mg/kg, i.p.) and were mounted in a stereotaxic frame after cannulation of the lateral vein of the tail in order to allow both the i.v. injection of drugs and the continuous infusion of chloral hydrate (120 mg/kg/h). A burr hole was drilled into the skull above the area to be recorded. The micropipettes (glass tubing of 1.5 mm outer diameter that was heated, pulled, and broken under microscopic control to obtain a tip of 2.5 μm diameter) were filled with 0.9% saline and stereotaxically aimed at the vicinity of DA cells in the substantia nigra (SN: A9) or the ventral tegmental area (VTA: A10). The spikes recorded from the micropipette were amplified, filtered (0.1–2 kHz), and visualized on an oscilloscope.
In all, 12 electrode tracks were defined on a 12-box, 240 000 μm2 grid within the A9 or A10 area, according to the following coordinates: A9 (5.8–5.2 mm anterior to bregma, 1.8–2.2 mm lateral to bregma, 6.5–8.0 mm under the cortical surface), A10 (6.0–5.4 mm anterior to bregma, 0.4–0.8 mm lateral to bregma, 7.0–8.5 mm under the cortical surface). The number of spontaneously active DA cells was counted for each track until the grid was completed. The DA cells were identified and the number of spontaneously firing neurons per electrode track was determined according to Grace and Bunney (1983). The effects of SSR181507 on population response were investigated in an acute and a repeated treatment procedure (3 mg/kg, i.p. once daily for a period of 22 days). On the day of the experiment, SSR181507 or vehicle was administered 45–60 min before initiation of the first electrode track. WAY100635 (0.1 mg/kg, i.v) or apomorphine (0.063 mg/kg, i.v.) was administered after completion of the last electrode track, and cell counting was restarted for an additional five tracks, according to White and Wang (1983).
In Vivo Measurement of Basal Dopamine Efflux
Basal DA efflux was monitored in the medial prefrontal cortex, nucleus accumbens, or striatum by microdialysis. Adult male Sprague–Dawley rats were anesthetized with chloral hydrate (400 mg/kg, i.p.) and guide cannulae were stereotaxically implanted onto the dura mater above the medial prefrontal cortex (3.2 mm anterior to bregma, 0.6 mm lateral to bregma), the nucleus accumbens (1.7 mm anterior to bregma, 1.0 mm lateral to bregma), and the striatum (0.7 mm anterior to bregma, 3.0 mm lateral to bregma) (Paxinos and Watson, 1998). At least 5 days after surgery, microdialysis probes (Carnegie Medicine, Stockholm, Sweden), 250 μm in diameter with an exposed membrane length of 3 mm (medial prefrontal cortex) and 2 mm (nucleus accumbens and striatum), were positioned within the guide cannulae (vertical coordinates: 4.5, 8.0, and 8.0 mm, respectively, under the cortical surface) and perfused with artificial cerebrospinal fluid (mM: NaCl, 147; KCl, 4; CaCl2, 1.2; MgCl2, 1.0) using a CMA/100 pump (Carnegie Medicine) at a flow rate of 2 μl/min. Dialysate samples were collected every 20 min and analyzed using HPLC with electrochemical detection. The average concentration of five stable fractions immediately preceding drug administration was defined as the 100% control value. The area under the curve was expressed relative to these values and was calculated for 120 min after drug administration.
In Vivo Measurement of Evoked Catecholamine Efflux
Rats were anesthetized with urethane (1.15–1.4 g/kg, i.p.), treated with pargyline (75 mg/kg, s.c.), and placed in a stereotaxic frame. Evoked catecholamine (CA) efflux was monitored in the nucleus accumbens or medial prefrontal cortex by electrochemically treated carbon fiber electrodes combined with differential pulse amperometry (DPA). The sensitivity of the treated electrode for CA vs metabolites (<10 vs 100 nM) and the use of pargyline to prevent CA catabolism allow a selective measurement of DA levels in the nucleus accumbens (Suaud-Chagny et al, 1992). In the medial prefrontal cortex, DA is probably the main source of the CA signal variations induced by the electrical stimulation of the dopaminergic pathway, although a participation of noradrenaline to the evoked CA efflux measured in the medial prefrontal cortex cannot be excluded.
Carbon fiber electrodes (250 μm long and 8 μm in diameter) were electrochemically treated in phosphate-buffered saline (PBS) as previously described (Brun et al, 1995). Electrodes were then implanted in the nucleus accumbens or the medial prefrontal cortex at the following coordinates: 2.0–2.2 mm anterior to bregma, 1.3 mm lateral to bregma and from 6.5 to 7.0 mm below the cortical surface and 2.7–3.0 mm anterior to bregma, 0.5–0.7 mm lateral to bregma and from 4.0 to 4.5 mm below the cortical surface, respectively (Paxinos and Watson, 1998). They were connected to a voltammetric recorder (Biopulse; Radiometer Analytical, France). Electrically evoked changes in CA efflux were monitored every second using DPA with the final potential adjusted at +80 mV vs the Ag/AgCl reference electrode (Suaud-Chagny et al, 1992; Brun et al, 1995). All results were expressed as percentages of the mean of the three effects recorded before drug injection.
Electrical Stimulation of the Dopaminergic Pathway
Electrical stimulation of the ascending dopaminergic pathway was used to evoke short-lasting increases in the extracellular DA concentration. A bipolar stimulating electrode (SNEX-200, Rhodes Medical Instruments, USA) was positioned in the ascending dopaminergic pathway at the following coordinates: 4.0 mm posterior to bregma and 1.0 mm lateral to bregma. The depth (8.2–8.6 mm below the cortical surface) was adjusted for each experiment so that the response was maximal. Electrical stimulations consisted of square current pulses (300 μA, 0.5 ms) and were applied by an isolated stimulator (DS2, Digitimer, USA) every 10 min and for 10 s at the frequency of 20 Hz (nucleus accumbens) or 40 Hz (medial prefrontal cortex).
Fos Immunochemistry
Experiments were performed as described previously (Alonso et al, 1999). Briefly, rats were anesthetized with sodium pentobarbital (75 mg/kg, i.p.) and perfused transcardially with saline, followed by 4% paraformaldehyde. Brains were postfixed overnight and 50 μm coronal sections were cut using a vibratome. Immunohistochemistry was performed on free-floating tissue sections according to a standard avidin–biotin–peroxidase procedure using an anti-Fos rabbit polyclonal antibody directed against residues 3–16 of the N-terminal region of the Fos protein (sc-52, Santa Cruz Biotechnologies Inc., CA, USA). Sections were imaged through a Leica DMRX microscope, and the Fos-like immunoreactive signal was quantified with an image analysis system (Samba Technologies, Meylan, France) by counting the number of Fos-positive cells.
Statistical Analyses
Statistical differences between groups were assessed using ANOVA tests, followed by Dunnett's post hoc tests.
In DPA experiments, comparisons between treatments were performed using a one-way ANOVA with repeated measures, followed by a Fisher's PLSD post hoc test.
RESULTS
In Vitro Radioligand-Binding Studies
SSR181507 showed high affinity for animal DA D2, DA D3, and 5-HT1A receptors (KI=7.5, 3.6, and 4.5 nM, respectively, Table 1). Clozapine had a lower affinity for these receptors. Olanzapine, as well as amisulpride and haloperidol, had almost a similar affinity for DA D2 and DA D3 receptors, but in contrast to SSR181507, they were devoid of significant affinity for the 5-HT1A receptor (Table 1). SSR181507 displayed high affinity for cloned human (h) DA D2, DA D3, and 5-HT1A receptor subtypes (KI=0.8, 0.2, and 0.2 nM, respectively, Table 2). It had no affinity for hDA D1 and hDA D5 receptor subtypes and had only a modest affinity for hDA D4 receptor, h5-HT2A, h5-HT2C, h5-HT6, and h5-HT7 receptor subtypes, for hα1D and hα2A adrenoceptors, and for all five human muscarinic receptor subtypes (selectivity ratio >60-fold, Table 2).
In Vivo Radioligand-Binding Studies
In vivo [3H]raclopride-binding studies in rats revealed occupancy of DA D2 receptors by SSR181507 with similar ID50 values in the limbic system and in the striatum (0.9±0.2 and 1.0±0.2 mg/kg, i.p., respectively, Table 3). In this test, SSR181507 behaved like haloperidol, which showed similar affinity in both brain regions, but different from amisulpride, which was more potent at competing with [3H]raclopride binding in the limbic system than in the striatum (Table 3).
[35S]GTPγS Binding to the Human DA D2 Receptor
Dopamine induced a concentration-dependent increase in [35S]GTPγS binding to recombinantly expressed DA D2 receptors (EC50=3.1 μM). SSR181507, up to 100 nM, failed to stimulate [35S]GTPγS binding to the DA D2 receptor, but antagonized DA (3 μM)-stimulated [35S]GTPγS binding with an IC50=5.3±1.0 nM (Figure 2a). Under the same experimental conditions, haloperidol had an IC50=3.9±0.8 nM.
Effects of SSR181507 (a) alone and on dopamine-stimulated [35S]GTPγS binding in CHO cells expressing the human recombinant DA D2 receptor and (b) on the [35S]GTPγS binding in CHO cells expressing the human recombinant 5-HT1A receptor. (a) Binding of [35S]GTPγS (0.1 nM) to CHO cell membranes was measured after incubation with different concentrations of SSR181507 in the presence of 3 μM GDP (▴) and 3 μM dopamine (•). Data are representative results from four independent experiments. (b) Binding of [35S]GTPγS (0.1 nM) to CHO cell membranes was measured after incubation with different concentrations of compounds. Data are representative results from four independent experiments.
[35S]GTPγS Binding to the Human 5-HT1A Receptor
5-HT concentration-dependently increased [35S]GTPγS binding to the recombinant 5-HT1A receptor with an EC50 of 7.1±2.6 nM. SSR181507 stimulated [35S]GTPγS binding (EC50=2.3±1.2 nM) with a maximal efficacy (Emax) of 85% as compared to that of 5-HT (defined as 100%). The corresponding values for the full 5-HT1A agonist 8-OH-DPAT and the partial 5-HT1A agonist NAN-190 were: EC50=2.8±1.5 nM and Emax=79%, and EC50=0.8± 0.2 nM and Emax=56%, respectively. The maximal efficacy of the 5-HT1A antagonist WAY100635 was 10% (Figure 2b).
In Vitro Dopamine Release
The electrically evoked [3H]dopamine release from slices of rat striatum is subject to an inhibitory modulation mediated by DA D2-like terminal autoreceptors as shown by the inhibitory effect of the DA agonist, apomorphine (IC50=23 nM). SSR181507 (30 and 100 nM) produced a rightward shift of the apomorphine dose–response curve with an apparent pA2=7.94 (Figure 3).
Effect of SSR181507 on the apomorphine-induced inhibition of electrically evoked [3H]dopamine release from the rat striatum in vitro. The effect of two concentrations of SSR181507 on electrically evoked [3H]dopamine release was studied using slices from rat striatum. Slices were initially stimulated in the absence of apomorphine and SSR181507 and 40 min thereafter in their presence. Apparent pA2 values were determined for each concentration of SSR181507 (30 and 100 nM) according to Furchgott (1972) as detailed in Materials and methods (average pA2=7.94). Data shown are means with SEM of 3–13 replicates for each point on the curves.
In Vivo Dopamine and Serotonin Synthesis
SSR181507 (0.3–10 mg/kg, i.p.) dose-dependently increased (322% of controls) the synthesis of DA, as measured by the accumulation of L-DOPA, in rat striatum (ED50=1.6±0.1 mg/kg, i.p.). In the same dose range, it decreased the synthesis of 5-HT (maximal effect: 42% of controls at 10 mg/kg, i.p.), as measured by the accumulation of 5-HTP in this same structure (ED50=0.7±0.3 mg/kg, i.p., Figure 4). Likewise, SSR181507 increased DA synthesis in the limbic system (ED50=1.1±0.1 mg/kg, i.p.) and decreased 5-HT synthesis in the hippocampus and cortex (ED50=4.1±3.1 and 1.1±0.6 mg/kg, i.p, respectively). Under the same experimental conditions (results not shown), the 5-HT1A agonist 8-OH-DPAT (0.3 mg/kg, i.p.) decreased striatal 5-HT synthesis (47% of controls) without modifying DA synthesis (96% of controls) and the selective DA D2 antagonist amisulpride (100 mg/kg, i.p.) only affected striatal DA synthesis (363% of controls vs 98% of controls for 5-HT synthesis). After repeated treatment (20 days at 3 or 10 mg/kg, i.p., b.i.d., followed by 72 h of withdrawal), SSR181507 (3 mg/kg, i.p.) induced changes in DA and 5-HT synthesis similar to those observed in animals who received vehicle chronically (Figure 5).
Effect of SSR181507 on DA and 5-HT synthesis in the rat striatum. Rats received NSD-1015 (100 mg/kg, i.p.) 30 min after the administration of SSR181507 (0.3–10 mg/kg, i.p.) or its vehicle control, and were killed 30 min thereafter. Results are expressed as percentage over the control group for L-DOPA and of the control group for 5-HTP and are the mean with SEM of data obtained from six animals per group. ED50 values represent the estimated doses required to produce a half-maximal effect. (▪) L-DOPA (ED50=1.6 mg/kg; control value: 1008±50 ng/g), (•) 5-HTP (ED50=0.7 mg/kg; control value: 219±10 ng/g). L-DOPA, F(4,25)=47.7; 5-HTP, F(4,25)=34.2, *p<0.05 compared with the respective control group (Dunnett's test following ANOVA).
Effect of repeated treatment with SSR181507 on DA and 5-HT synthesis in the rat striatum. Rats received NSD-1015 (100 mg/kg, i.p.) 30 min after the administration of SSR181507 or its vehicle control and were killed 30 min thereafter. SSR181507 was administered at a dose of 3 mg.kg, i.p. 72 h after the last chronic injection of vehicle control or SSR181507 (3 or 10 mg/kg, i.p., b.i.d. for 20 days). Results are expressed as percentage of the respective control group and are means with SEM of data obtained from eight animals per group. (a) L-DOPA (control value: 964±80 ng/g), (b) 5-HTP (control value: 268±17 ng/g); L-DOPA, F(3,27)=14.2, 5-HTP, F(3,27)=37.1, *p<0.05 compared with the respective control group (Dunnett's test following ANOVA).
Number of Spontaneously Active DA Cells
In the rat, acute administration of SSR181507 (0.1–3 mg/kg, i.p.) increased the number of spontaneously active DA cells per track in the A10 area but, up to 10 mg/kg, i.p., failed to affect this parameter in the A9 area. In this latter area, when WAY100635 (0.1 mg/kg, i.v.) was administered with an inactive dose of SSR181507 (3 mg/kg, i.p.), the number of active DA cells was increased (Figure 6a).
Effect of acute and repeated treatment with SSR181507 on the number of spontaneously active DA cells in the A9 and A10 areas. The number of spontaneously active DA cells in the VTA (A10) and the SN (A9) was measured as described in Materials and methods. (a) Acute treatment: SSR181507 (0.1–10 mg/kg, i.p.) or vehicle were administered 45–60 min before initiation of the first electrode track. Results are mean with SEM of four to six animals by group. F(4,19)=140.2, *p<0.05, SSR181507 compared with control; F(4,27)=289.0, #p<0.05, SSR181507 with WAY100635 compared with SSR181507 (Dunnett's test following ANOVA).(b) Repeated treatment: SSR181507 (3 mg/kg, i.p.) or vehicle were administered once a day for 21 days. On the day of the experiment (24 h after the last chronic injection), SSR181507 or vehicle was administered. Results are means with SEM of four to six animals per group. F(5,23)=30.0, *p<0.05, compared with respective control; F(2,8)=402.1, #p<0.05, SSR181507 with WAY100635 compared with SSR181507 (Dunnett's test following ANOVA).
Following repeated administration (22 days, 3 mg/kg, i.p., o.d.), SSR181507 decreased the number of spontaneously active DA cells in the A10, but not in the A9 area, as compared to controls. The effect of the drug in the A10 area was reversed by an acute injection of apomorphine (63 μg/kg, i.v.), thus demonstrating the induction of depolarization block. The involvement of the 5-HT1A agonist property in this selective regional effect was demonstrated by the fact that the injection of WAY100635 (0.1 mg/kg, i.v.) with an inactive dose of SSR181507 (3 mg/kg/day, i.p.), induced an increase in the number of spontaneously active DA cells in the A9 area (Figure 6b).
Basal DA Efflux Measured by In Vivo Microdialysis
SSR181507 (3 mg/kg, i.p.) markedly increased extracellular DA levels in the nucleus accumbens (164±11% of controls), but was devoid of effect in the striatum (Figure 7a). At 1 mg/kg, i.p., it also increased extracellular DA levels in the medial prefrontal cortex (153±10% of controls, Figure 7b). Under similar experimental conditions, clozapine (10 mg/kg, i.p.) increased this parameter by 173±25 and 164±32% of controls in the nucleus accumbens and striatum, respectively (results not shown), and by 188±14% of controls in the medial prefrontal cortex (Figure 7b).
Effect of SSR181507 on basal DA efflux (a) in the nucleus accumbens and striatum and (b) in the medial prefrontal cortex. Compounds were evaluated on basal DA efflux as described in Materials and methods. Results are expressed as percent of area under the curves between 0 and 120 min after compound administration and are means with SEM of data obtained from four to nine rats per group. (a) Nucleus accumbens F(2,10)=9.9, *p<0.05, compared with control (Dunnett's test following ANOVA). (b) Medial prefrontal cortex, SSR181507 F(2,17)=7.0, and clozapine F(1,12)=34.4, *p<0.05, compared with control (Dunnett's test following ANOVA).
Evoked CA Efflux Measured by In Vivo Electrochemistry
Electrical stimulation of the ascending dopaminergic pathway evoked immediate, reversible, and highly reproducible increases in DA efflux in the nucleus accumbens and CA efflux in the medial prefrontal cortex (Suaud-Chagny et al, 1992; Brun et al, 1995).
In the nucleus accumbens, haloperidol (50 μg/kg, s.c.) significantly increased the evoked DA efflux to a maximum of 114±21% above predrug values (Figure 8a). Both doses of SSR181507 (1 and 3 mg/kg, i.p.) elicited a large, sustained, and significant increase in the evoked DA efflux (Figure 8a). This increase was larger with the highest dose of SSR181507 (maximum, 106±22 and 444±53% above predrug values for the lowest and highest dose of SSR181507, respectively). WAY100635 (1 mg/kg, i.p.) almost completely blocked the response induced by SSR181507 (3 mg/kg, i.p., Figure 8a). In the medial prefrontal cortex, haloperidol (50 μg/kg, s.c.) and clozapine (10 mg/kg, s.c.) did not significantly modify the evoked CA efflux (Figure 8b). In contrast, both doses of SSR181507 (1 and 3 mg/kg, i.p.) elicited a significant increase in the evoked CA efflux (Figure 8b). Moreover, as observed in the nucleus accumbens, post hoc comparison indicated a significant difference (p<0.05) between both doses of SSR181507 in the medial prefrontal cortex (Figure 8b).
Effect of SSR181507 on phasic DA efflux (a) in the nucleus accumbens and (b) in the medial prefrontal cortex. (a) Effect of the administration (arrow) of vehicle, haloperidol (50 μg/kg, s.c.), and SSR181507 (1 and 3 mg/kg, i.p.) on the electrically evoked DA efflux recorded by DPA in the nucleus accumbens. When present, WAY100635 was given 20 min before SSR181507. Stimulations of the medial forebrain bundle (20 Hz, 10 s) were repeated every 10 min. The amplitude of each effect is expressed as a percentage of the mean of the three responses to stimulation recorded before drug injection. Data represent means with SEM from four to seven experiments. *p<0.05 compared with vehicle-treated animals and #p<0.05 compared with SSR181507 (3 mg/kg, i.p.) group (Fisher's PLSD test following ANOVA). (b) Effect of the administration (arrow) of vehicle, haloperidol (50 μg/kg, s.c.), SSR181507 (1 and 3 mg/kg, i.p.), and clozapine (10 mg/kg, s.c.) on the electrically evoked CA efflux recorded by DPA in the medial prefrontal cortex. The amplitude of each effect is expressed as a percentage of the mean of the three responses to stimulation recorded before drug injection. Data represent means with SEM from four to seven experiments. *p<0.05 compared with vehicle-treated animals and #p<0.05 compared with a low dose of SSR181507 (1.0 mg/kg, i.p.)-treated animals (Fisher's PLSD test following ANOVA).
In Vivo Recording of Dorsal Raphe Neuronal Firing
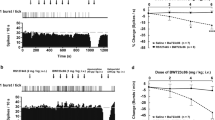
5-HT neurons present a slow (0.5–3 Hz) and regular firing rate and long-duration (0.8–2 ms) biphasic action potentials. SSR181507 induced a marked and dose-dependent inhibition of the neuronal firing rate in the rat DRN (0.03–0.3 mg/kg, i.v., Figure 9a). Treatment with WAY100635 (0.1 mg/kg, i.v.) reversed the SSR180507-induced inhibition of raphe neurons (Figure 9b). When administered alone, WAY100635 (0.1 mg/kg, i.v.) had no effect (not shown).
Effect of SSR181507 on DRN firing in the rat brain. (a) Decrease in firing rate, expressed in percent of baseline activity, is plotted against the dose of SSR181507. Each curve is the mean with SEM of three to four independent determinations. SSR181507 0.01 mg/kg, i.v., F(4,12)=17.8; 0.03 mg/kg, i.v., F(3,6)=51.7; 0.1 mg/kg, i.v., F(3,6)=22.1; 0.3 mg/kg, i.v., F(2,4)=156.5; *p<0.05, **p<0.01, SSR181507 compared with control (Dunnett's test following ANOVA). (b) Antagonism by WAY100635 (0.1 mg/kg, i.v.) of the inhibition by SSR181507 (0.1 mg/kg, i.v.) of dorsal raphe cell firing. Points represent the mean±SEM for n=3–4 cells. (▴, SSR181507 alone; ▪, SSR181507 with WAY100635). F(1,5)=60.4, **p<0.01, SSR181507 and WAY100635 compared with SSR181507 alone (Dunnett's test following ANOVA).
Fos Immunoreactivity
In the rat, SSR181507 (1–10 mg/kg, i.p.), like clozapine (20 mg/kg, i.p.), selectively increased the number of Fos-positive cells in mesocorticolimbic areas (prefrontal cortex, nucleus accumbens shell, dorsomedial caudate putamen (CPu)) and did not alter or weakly affected this parameter in motor-related structures (nucleus accumbens core, dorsolateral CPu) (Figure 10). In contrast, haloperidol (0.5 mg/kg, i.p.) increased the number of Fos-positive cells to a similar extent in all these limbic and motor-related brain regions and failed to affect this parameter in the prefrontal cortex (Figure 10).
Number of Fos-positive neurons after administration of vehicle, SSR181507 (1–10 mg/kg, i.p.), haloperidol (0.5 mg/kg, i.p.), or clozapine (20 mg/kg, i.p.). Results were evaluated as described in Materials and methods and are mean with SEM of four to six animals per group. CPu: caudate putamen. *p<0.05 compared with vehicle-treated rats (Dunnett's test following ANOVA).
DISCUSSION
We took advantage of the discovery of SSR181507 to test whether the combination in the same molecule of selective DA D2 receptor antagonism and 5-HT1A agonist activity would result in a pharmacological and neurochemical profile characteristic of atypical antipsychotics. The present report and its companion paper dealing with the psychopharmacological profile of SSR181507 (Depoortere et al, 2003) provide strong evidence that this dual mechanism of action results in a drug profile compatible with an original, atypical antipsychotic activity.
Selectivity for DA D2 and 5-HT1A receptors
SSR181507 has a similar and high-nanomolar affinity for DA D2 and D3 receptors in vitro. It does not bind to DA D1 and DA D5 subtypes and in contrast to almost all atypical antipsychotics (clozapine, risperidone, olanzapine, ziprasidone), it has no appreciable affinity for the DA D4 subtype (Miyamoto et al, 2000).
It also has a high affinity and selectivity for the 5-HT1A receptor subtype. Some atypical antipsychotics such as ziprasidone, iloperidone, and aripiprazole also display significant affinity for 5-HT1A receptor but in contrast to SSR181507, they also bind to other 5-HT receptor subtypes, for example, the 5-HT2A subtype (Richelson and Souder, 2000; Jordan et al, 2002).
SSR181507 also has no noticeable affinity for α-adrenergic, muscarinic M1, and histamine H1 receptors (that are thought to be involved in the autonomic and sedative side effects of antipsychotics).
Thus, in vitro, SSR181507 shows a unique profile in the sense that it selectively binds to the DA D2 and 5-HT1A receptor subtypes with similar nanomolar affinity.
Our findings in vivo confirmed this binding profile. Thus, SSR181507 inhibits the in vivo binding of [3H]raclopride to DA D2 receptors in the rat striatum and limbic system with a similar high potency. Moreover, SSR181507 fails to inhibit (ID50>30 mg/kg, i.p.) the in vivo binding of [3H]spiperone to the 5-HT2 receptor of the mouse frontal cortex and the in vivo binding of [3H]RS-79948 to the α2 receptor in the mouse hypothalamus (results not shown).
Intrinsic Activity at DA D2 and 5-HT1A Receptors
The functional activity of SSR181507 at DA D2 and 5-HT1A receptors was evaluated in the [35S]GTPγS-binding model. In this in vitro model, SSR181507 behaved as a potent antagonist at the DA D2 receptor and had the profile of a full agonist or of a high-efficacy partial agonist at the 5-HT1A receptor. In contrast, ziprasidone, clozapine, and aripiprazole behave as partial agonists at cloned 5-HT1A receptors (Newman-Tancredi et al, 1998; Jordan et al, 2002). SSR181507 also antagonized rat presynaptic DA D2 receptors, as demonstrated by the rightward shift by this drug of the concentration–response curve of DA agonist-induced decrease of [3H]dopamine release in rat striatal slices.
That SSR181507 blocks rat DA D2 receptors in vivo was suggested by the fact that this drug increased striatal and limbic DA synthesis. As would be expected for a 5-HT1A agonist, SSR181507, in the same dose range, inhibited the synthesis of 5-HT in several rat brain areas, and its maximal effect was similar to that of 8-OH-DPAT, thus confirming that it behaves as a full 5-HT1A agonist on the serotonergic transmission. Electrophysiological data showing that SSR181507 decreased the firing rate of 5-HT neurons in the dorsal raphe are also compatible with activation of 5-HT1A receptors by this drug. This effect is mediated by selective activation of 5-HT1A receptors as revealed by its sensitivity to the 5-HT1A antagonist WAY100635. In this model, the total inhibition of firing rate at the dose of 0.3 mg/kg, i.v. is also in agreement with a full 5-HT1A agonist profile. However, it is known that the intrinsic activity is dependent on the experimental model. In the in vitro GTPγS model, it is highly dependent on the density of recombinant 5-HT1A receptors and in the two preceding in vivo models, it reflects the activity at presynaptic 5-HT1A receptors (Newman-Tancredi et al, 1998). Interestingly, in an integrated functional model in rats involving 5-HT1A postsynaptic receptors (serotonergic syndrome), SSR181507 has the profile of a partial 5-HT1A agonist (Depoortere et al, 2003). The effects of SSR181507 on DA and 5-HT synthesis were of long duration (at least 6 h, results not shown) and persisted after repeated treatment for 20 days, demonstrating that there is no development of tolerance.
Mesocorticolimbic Selectivity and Atypical Antipsychotic Profile
The combination of DA D2 receptor antagonism and 5-HT1A agonist effect was expected to confer on SSR181507 selectivity for mesocortical and mesolimbic dopaminergic activity, resulting in a pharmacological profile compatible with atypical antipsychotic properties (see Introduction).
Electrophysiological studies confirmed the limbic selectivity of SSR181507. Thus, acute treatment with SSR181507 resulted in an increased number of spontaneously active DA neurons in the VTA, but not in the SN. Repeated treatment with SSR181507 reduced the number of spontaneously active DA neurons in the VTA without modifying it in the SN. In this latter model, SSR181507 behaved like olanzapine, sertindole, and risperidone, which decrease the number of spontaneously active DA cells in the mesolimbic system only, but differed from quetiapine and ziprasidone that also affect the nigrostriatal system (Skarsfeldt, 1995). This model of depolarization inactivation of DA neurons is generally considered to be of predictive value of the nature of antipsychotic compounds (Jones-Humble et al, 1996). The regional selectivity of SSR181507 could be due to its agonist activity at 5-HT1A receptors. Indeed, the capacity of SSR181507 to affect selectively the number of spontaneously active DA cells in the VTA disappeared in the presence of WAY100635. Moreover, the fact that this limbic selectivity was still present after a chronic treatment with SSR181507 confirms the lack of desensitization of 5-HT1A receptors.
The regional effect of antipsychotics on DA release has also been shown to highlight their typical or atypical profile (Nomikos et al, 1994; Volonté et al, 1997). The effect of SSR181507 on basal and evoked DA efflux in rat brain areas also supports the mesocorticolimbic selectivity of this compound. Thus, SSR181507 enhanced basal DA efflux in the nucleus accumbens and medial prefrontal cortex, but not in the striatum. A similar regional selectivity was previously found for the atypical antipsychotics ziprasidone, clozapine, olanzapine, and risperidone, while haloperidol increased DA efflux more markedly in the striatum than in the nucleus accumbens, and was inactive in the prefrontal cortex (Kuroki et al, 1999; Rollema et al, 2000). The limbic selectivity of SSR181507 is likely related to 5-HT1A receptor activation, as its cortical response is antagonized (results not shown) by a 5-HT1A antagonist (SL88.0338-08). Moreover 5-HT1A agonists are known to increase cortical DA efflux without affecting striatal DA efflux (Arborelius et al, 1993; Rollema et al, 2000). Ichikawa et al (2001) recently hypothesized that simultaneous blockade of 5-HT2A and DA D2 receptors causes an increase in cortical DA efflux by facilitating 5-HT1A agonist activity by endogenous 5-HT. It may thus be suggested that, by directly activating 5-HT1A receptors, SSR181507 is functionally equivalent to atypical antipsychotics that indirectly achieve this effect.
The 5-HT1A agonist activity of SSR181507 may also account for its original neurochemical profile on evoked DA efflux, as its effect in the nucleus accumbens was antagonized by WAY100635. In the medial prefrontal cortex, in contrast to clozapine and haloperidol, SSR181507 dose-dependently increased evoked CA efflux. The site(s) at which 5-HT1A receptors control DA neuron activity is still a matter of debate. A direct effect on DA cell bodies seems to be excluded as neither 5-HT1A receptor protein nor mRNA have been detected in the VTA and SN (Miquel et al, 1991). Moreover, since DA efflux was evoked by electrical stimulation of the ascending dopaminergic pathway, activation of 5-HT1A autoreceptors present on DRN neurons afferent to the VTA cannot be invoked. As suggested by Sakaue et al (2000), 5-HT/DA interactions could take place directly in the medial prefrontal cortex, via the activation of 5-HT1A receptors located on postsynaptic neurons.
A disruption in the function of the prefrontal cortex (‘hypofrontality’) is thought to play a major role in the negative symptoms and cognitive deficit of schizophrenia. The robust increase in basal and evoked DA output in the medial prefrontal cortex induced by SSR181507 suggests that this drug may improve negative symptoms (Weinberger and Lipska, 1995) and also cognitive-attentional symptoms of the pathology (Meltzer and McGurk, 1999).
We have shown that SSR181507 has a high affinity for the DA D3 receptor subtype. However, complementary experiments have revealed that SSR181507 behaves as a partial agonist at this receptor (result not shown), thus suggesting that its antipsychotic profile can hardly be explained by an interaction with this receptor. Moreover, disappointing results regarding the behavioral phenotype of DA D3 receptor knockout mice, and the lack of consistency in the behavioral effects of the different putative DA D3 receptor ligands, have cast some doubt about the in vivo function of this receptor, and one step beyond, about its possible relevance in schizophrenia (Depoortere et al, 2002).
The immunochemistry of the Fos protein has been shown to be useful in mapping functional pathways in the central nervous system and especially in identifying brain areas that are targets for antipsychotics. Moreover, the ability of these drugs to increase Fos protein expression in the striatal complex has been considered useful in discriminating between typical and atypical antipsychotic compounds (Deutch et al, 1992; Robertson and Fibiger, 1992). In contrast to haloperidol, but like most atypical antipsychotics, SSR181507 did not affect Fos immunoreactivity in the regions implicated in the control of extrapyramidal motor function. However, like clozapine, it markedly enhanced the expression of Fos protein in mesocorticolimbic regions that are involved in the control of affective and motivational behaviors. In this respect, SSR181507 clearly behaves as an atypical antipsychotic. It is noticeable, however, that among atypical antipsychotics that similarly increase Fos expression in limbic areas, only some of them also enhance this expression in the medial prefrontal cortex (Deutch et al, 1992; Semba et al, 1996). Interestingly, it has been shown (Tremblay et al, 1998) that the 5-HT1A agonist 8-OH-DPAT is able to convert the ‘typical’ pattern of haloperidol on c-fos expression into a pattern resembling that of clozapine, suggesting that the original profile of Fos protein expression of SSR181507 may be due to its dual 5-HT1A agonist and DA D2 antagonist properties.
CONCLUSION
SSR181507 has a unique neurochemical and electrophysiological profile that is linked to its dual properties (DA D2 antagonist and 5-HT1A agonist) expressed in the same dose range. Several advantages may be expected from such a profile and SSR181507 should have the features of an atypical antipsychotic compound. It should have efficacy against positive, and also negative and cognitive symptoms of schizophrenia and should lack the liability of extrapyra-midal and other significant side effects. In addition, it should be efficacious on schizophrenia-associated mood and anxiety disorders. A companion paper dealing with the psychopharmacological profile of SSR181507 (Depoortere et al, 2003) adds further weight to these hypotheses.
References
Alonso R, Voutsinos B, Fournier M, Labie C, Steinberg R, Souilhac J et al (1999). Blockade of cannabinoid receptors by SR141716 selectively increases fos expression in rat mesocorticolimbic areas via reduced dopamine D2 function. Neuroscience 91: 607–620.
Arborelius LE, Nomikos GG, Hacksell U, Svenson TH (1993). (R)-8-OH-DPAT preferentially increases dopamine release in rat medial prefrontal cortex. Acta Physiol Scand 148: 465–466.
Bantick RA, Deakin JF, Grasby PM (2001). The 5-HT1A receptor in schizophrenia: a promising target for novel atypical neuroleptics? J Psychopharmacol 15: 37–46.
Bonhaus DW, Bach C, De Souza A, Salazar FHR, Matsuoka BD, Zuppan P et al (1995). The pharmacology and distribution of human 5-hydroxytryptamine2B (5-HT2B) receptor gene products: comparison with 5-HT2A and 5-HT2C receptors. Br J Pharmacol 115: 622–628.
Borison RL, Albrecht JW, Diamond BL (1990). Efficacy and safety of a putative anxiolytic agent: ipsapirone. Psychopharmacol Bull 26: 207–210.
Boyer P, Lecrubier Y, Puech AJ, Dewailly J, Aubin F (1995). Treatment of negative symptoms in schizophrenia with amisulpride. Br J Psychiatry 166: 68–72.
Briley M, Langer SZ (1978). Two binding sites for 3H-spiroperidol on rat striatal membranes. Eur J Pharmacol 50: 283–284.
Brun P, Steinberg R, Le Fur G, Soubrié P (1995). Blockade of neurotensin receptor by SR 48692 potentiates the facilitatory effect of haloperidol on the evoked in vivo dopamine release in the rat nucleus accumbens. J Neurochem 64: 2073–2079.
Buckley NJ, Bonner TI, Buckley CM, Brann MR (1989). Antagonist binding properties of five cloned muscarinic receptors expressed in CHO-K1 cells. Mol Pharmacol 35: 469–476.
Burnet PWJ, Eastwood SL, Harrison PJ (1996). 5-HT1A and 5-HT2A receptor mRNAs and binding site densities are differentially altered in schizophrenia. Neuropsychopharmacology 15: 442–455.
Cheng Y, Prusoff WH (1973). Relationship between the inhibition constant (Ki) and the concentration of the inhibitor which causes 50% inhibition (IC50) of an enzymatic reaction. Biochem Pharmacol 22: 3099–3108.
Dearry A, Gringrich JA, Falardeau P, Fremeau RT, Bates MD, Caron MG (1990). Molecular cloning and expression of the gene for a human D1 dopamine receptor. Nature 347: 72–76.
Depoortere R, Boulay D, Perrault G, Bergis O, Decobert M, Françon D et al SSR181507, a dopamine D2 receptor antagonist and 5-HT1A receptor agonist. II. Behavioral profile predictive of an atypical antipsychotic activity. Neuropsychopharmacology, 2003.
Depoortere R, Boulay D, Perrault G, Sanger DJ (2002). Behavioral pharmacology of dopamine D2 and D3 receptors: use of the knock-out mice approach. In: Di Chiara G (ed) Dopamine in the CNS II. Springer: Heidelberg. pp 239–264.
Deutch AY, Lee MC, Iadarola MJ (1992). Regionally specific effects of atypical antipsychotic drugs on striatal fos expression: the nucleus accumbens shell as a locus of antipsychotic action. Mol Cell Neurosci 3: 332–341.
Furchgott RF (1972). The classification of adrenoceptors (adrenergic receptors). An evaluation from the standpoint of receptor theory. In: Blaschko H, Muscholl E (eds) Handbook of Experimental Pharmacology Vol. XXXIII Springer: Berlin, Heidelberg, New York. pp 283–335.
Goff D, Midha K, Brotman A, McCormick S, Waites M, Amico E (1991). An open trial of buspirone added to neuroleptics in schizophrenic patients. J Clin Psychopharmacol 11: 193–197.
Grace AA, Bunney BS (1983). Intracellular and extracellular electrophysiology of nigral dopaminergic neurons 1. Identification and characterization. Neuroscience 10: 301–315.
Grandy DK, Marchionni MA, Makam H, Stofko RE, Alfano M, Frothingham L et al (1989). Cloning of the cDNA and gene for a human D2 dopamine receptor. Proc Natl Acad Sci USA 86: 9762–9766.
Greengrass P, Bremner R (1979). Binding characteristics of 3H-prazosin to rat brain alpha-adrenergic receptors. Eur J Pharmacol 55: 323–326.
Haigler HJ, Aghajanian GK (1974). Lysergic acid diethylamide and serotonin: a comparison of effects on serotonergic neurons and neurons receiving a serotonergic inputs. J Pharmacol Exp Ther 188: 688–699.
Ichikawa J, Ishii H, Bonaccorso S, Fowler WL, O'Laughlin IA, Meltzer HY (2001). 5-HT2A and D2 receptor blockade increases cortical DA release via 5-HT1A receptor activation: a possible mechanism of atypical antipsychotic-induced cortical dopamine release. J Neurochem 76: 1521–1531.
Jones-Humble SA, Durcan MJ, Lyerly D, Norton RM, Tang FLM, Russell AV et al (1996). Preclinical neurochemical and electrophysiological profile of 1192U90 a potential antipsychotic. Neuropsychopharmacology 15: 217–230.
Jordan S, Koprivica V, Chen R, Tottori K, Kikuchi T, Altar CA (2002). The antipsychotic aripiprazole is a potent, partial agonist at the human 5-HT1A receptor. Eur J Pharmacol 441: 137–140.
Kapur S, Remington G (1996). Serotonin–dopamine interaction and its relevance to schizophrenia. Am J Psychiatry 153: 466–476.
Kasper S, Tauscher J, Willeit M, Stamenkovic M, Neumeister A, Kufferle B et al (2002). Receptor and transporter imaging studies in schizophrenia, depression, bulimia and Tourette's disorder implication for psychopharmacology. World J Biol Psychiatry 3: 133–146.
Kenny BA, Chalmers DH, Philpott PC, Naylor AM (1995). Characterization of an alpha 1D-adrenoceptor mediating the contractile response of rat aorta to noradrenaline. Br J Pharmacol 115: 981–986.
Köhler C, Hall H, Ogren SO, Gawell L (1985). Specific in vitro and in vivo binding of 3H-raclopride, a potent substituted benzamide drug with high affinity for dopamine D-2 receptors in the rat brain. Biochem Pharmacol 34: 2251–2259.
Koreen AR, Siris SG, Chakos M, Alvir J, Mayerhoff D, Lieberman J (1993). Depression in first-episode schizophrenia. Am J Psychiatry 150: 1643–1648.
Kuroki T, Meltzer HY, Ichikawa J (1999). Effects of antipsychotic drugs on extracellular dopamine levels in rat medial prefrontal cortex and nucleus accumbens. J Pharmacol Exp Ther 288: 774–781.
Liberman RP, Corrigan PW (1992). Is schizophrenia a neurological disorder? J Neuropsychiatry Clin Neurosci 4: 119–124.
Martin GR, Humphrey PA (1994). Receptors for 5-hydroxytryptamine: current perspectives on classification and nomenclature. Neuropharmacology 33: 261–273.
Meltzer HY (1999). The role of serotonin in antipsychotic drug action. Neuropharmacology 21: 1065–1155.
Meltzer HY, McGurk SR (1999). The effects of clozapine, risperidone and olanzapine on cognitive function in schizophrenia. Schizophr Bull 25: 233–255.
Millan MJ (2000). Improving the treatment of schizophrenia: focus on serotonin (5-HT)1A receptors. J Pharmacol Exp Ther 295: 853–861.
Miquel MC, Doucet E, Boni C, El Mestikawy S, Mathiessen L, David G et al (1991). Central serotonin1A receptors: respective distributions of encoding mRNA, receptor protein and binding sites by in situ hybridization histochemistry, radioimmunohistochemistry and autoradiographic mapping in the rat brain. Neurochem Int 19: 453–465.
Miyamoto S, Duncan G, Mailman R, Lieberman J (2000). Developing novel antipsychotic drugs: strategies and goals. Curr Opin CPNS Invest Drugs 2: 25–39.
Monsma FJ, Shen Y, Ward RP, Hamblin MW, Sibley DR (1993). Cloning and expression of a novel serotonin receptor with high affinity for tricyclic psychotropic drugs. Mol Pharmacol 43: 320–327.
Newman-Tancredi A, Cussac D, Audinot V, Pasteau V, Cavaudan S, Millan MJ (1999). G protein activation by human dopamine D3 receptors in high-expressing Chinese hamster ovary cells: a guanosine-5′-O-(3-[32S]thio)-triphosphate binding and antibody study. Mol Pharmacol 55: 564–574.
Newman-Tancredi A, Gavaudan S, Conte C, Chaput C, Touzard M, Verriele L et al (1998). Agonist and antagonist actions of antipsychotic agents at 5-HT1A receptors. Eur J Pharmacol 355: 245–256.
Nomikos GG, Iurlo M, Andersson JL, Kimura K, Svensson TH (1994). Systemic administration of amperozide, a new atypical antipsychotic drug, preferentially increases dopamine release in the rat medial prefrontal cortex. Psychopharmacology 115: 147–156.
Paxinos G, Watson C (1998). The Rat Brain in Stereotaxic Coordinates. Academic Press: Sydney, Australia.
Richelson E, Souder T (2000). Binding of antipsychotic drugs to human brain receptors. Focus on newer generation compounds. Life Sci 68: 29–39.
Robertson GS, Fibiger HC (1992). Neuroleptics increase c-fos expression in the forebrain: contrasting effects of haloperidol and clozapine. Neuroscience 46: 315–328.
Robinson DS, Alms DR, Shrotriya RC, Messina M, Wickramarante P (1989). Serotonergic anxiolytics and treatment of depression. Psychopathology 22: 27–36.
Rollema H, Lu Yi, Schmidt AW, Sprouse JS, Zorn SH (2000). 5-HT1A receptor activation contributes to ziprasidone-induced dopamine release in the rat prefrontal cortex. Biol Psychiatry 48: 229–237.
Sakaue M, Somboonthum P, Nishihara B, Koyama Y, Hashimoto H, Baba A et al (2000). Postsynaptic 5-hydroxytryptamine (1A) receptor activation increases in vivo dopamine release in rat prefrontal cortex. Br J Pharmacol 129: 1028–1034.
Sanger DJ, Schoemaker H (1992). Discriminative properties of 8-OH-DPAT. Relationship to affinity for 5-HT1A receptors. Psychopharmacology 108: 85–92.
Scatton B, Sanger DJ (2000). Pharmacological and molecular targets in the search for novel antipsychotics. Behav Pharmacol 11: 242–256.
Schoemaker H (1993). [3H]7-OH-DPAT labels both dopamine D3 receptors and σ sites in the bovine caudate nucleus. Eur J Pharmacol 242: R1–R2.
Schoemaker H, Claustre Y, Fage D, Rouquier L, Chergui O, Curet O et al (1997). Neurochemical characteristics of amisulpride, an atypical dopamine D2/D3 receptor antagonist with both presynaptic and limbic selectivity. J Pharmacol Exp Ther 280: 83–97.
Schoemaker H, Langer SZ (1986). [3H]8-OH-DPAT labels the serotonin transporter in the rat striatum. Eur J Pharmacol 124: 371–373.
Semba J, Sakai M, Miyoshi R, Mataga N, Fukamauch F, Kito S (1996). Differential expression of c-fos mRNA in rat prefrontal cortex, striatum, n. accumbens and lateral septum after typical and atypical antipsychotics: an in situ hybridization study. Neurochem Int 29: 435–442.
Shen Y, Monsma FJ, Metcalf MA, Jose PA, Hamblin MW, Sibley D (1993). Molecular cloning and expression of 5-hydroxytryptamine7 serotonin receptor subtype. J Biol Chem 268: 18200–18204.
Sibley DR, Monsma FJ (1992). Molecular biology of dopamine receptors. Trends Pharmacol Sci 13: 61–69.
Simpson MDC, Lubman DI, Slater P, Deakin JFW (1996). Autoradiography with [3H]8-OH-DPAT reveals increases in 5-HT1A receptors in ventral prefrontal cortex in schizophrenia. Biol Psychiatry 39: 919–928.
Skarsfeldt T (1995). Differential effects of repeated administration of novel antipsychotic drugs on the activity of midbrain dopamine neurons in the rat. Eur J Pharmacol 281: 289–294.
Sokoloff P, Giros B, Martres MP, Bouthenet ML, Schwartz JC (1990). Molecular cloning and characterization of a novel dopamine receptor (D3) as a target for neuroleptics. Nature 247: 146–151.
Suaud-Chagny MF, Brun P, Buda M, Gonon F (1992). Fast in vivo monitoring of electrically evoked dopamine release by differential pulse amperometry with untreated carbon fibre electrodes. J Neurosci Methods 45: 183–190.
Sumiyoshi T, Matsui M, Nohara S, Yamashita I, Kurachi M, Sumiyoshi C et al (2001). Enhancement of cognitive performance in schizophrenia by addition of tandospirone to neuroleptic treatment. Am J Psychiatry 158: 1722–1725.
Sumiyoshi T, Matsui M, Yamashita I, Nohara S, Uehara T, Kurachi M et al (2000). Effect of adjunctive treatment with serotonin-1A agonist tandospirone on memory functions in schizophrenia. J Clin Psychopharmacol 20: 386–388.
Tremblay PO, Gervais J, Rouillard C (1998). Modification of haloperidol-induced pattern of c-fos expression by serotonin agonists. Eur J Neurosci 10: 3546–3555.
Van Tol HHM, Bunzow JR, Guan HG, Sunahara RK, Seeman P, Niznik HB et al (1991). Cloning of the gene for a human dopamine D4 receptor with high affinity for the antipsychotic clozapine. Nature 350: 610–614.
Volonté M, Monferini E, Cerutti M, Fodritto F, Borsini F (1997). BIMG 80, a novel potential antipsychotic drug: evidence for multireceptor actions and preferential release of dopamine in prefrontal cortex. J Neurochem 59: 182–190.
Wadenberg ML, Ahlenius S (1991). Antipsychotic-like profile of combined treatment with raclopride and 8-OH-DPAT in the rat: enhancement of antipsychotic-like effects without catalepsy. J Neural Transm [Gen Sect] 83: 43–53.
Weinberger DR, Lipska BK (1995). Cortical maldevelopment, antipsychotic drugs and schizophrenia: a search for common ground. Schizophr Rev 16: 87–110.
White FJ, Wang RY (1983). Differential effects of classical and atypical antipsychotic drugs on A9 and A10 dopamine neurons. Science 221: 1054–1057.
Acknowledgements
We thank N Brunel, G Danielou, and M Vinay for technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Note: This paper is the first of two companion studies published in Neuropsychopharmacology. The second paper's citation is SSR181507, A Dopamine D2 Receptor Antagonist and 5-HT1A Receptor Agonist. II: Behavioral Profile Predictive of an Atypical Antipsychotic Activity (2003) 28, 1889–1902. doi: 1038/sj.npp.1300261. These two papers should be read together.
Rights and permissions
About this article
Cite this article
Claustre, Y., Peretti, D., Brun, P. et al. SSR181507, A Dopamine D2 Receptor Antagonist and 5-HT1A Receptor Agonist. I: Neurochemical and Electrophysiological Profile. Neuropsychopharmacol 28, 2064–2076 (2003). https://doi.org/10.1038/sj.npp.1300262
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1300262
Keywords
This article is cited by
-
F15063, a potential antipsychotic with D2/D3 antagonist, 5‐HT1A agonist and D4 partial agonist properties: (I) in vitro receptor affinity and efficacy profile
British Journal of Pharmacology (2007)
-
F15063, a compound with D2/D3 antagonist, 5‐HT1A agonist and D4 partial agonist properties: (II) Activity in models of positive symptoms of schizophrenia
British Journal of Pharmacology (2007)
-
F15063, a compound with D2/D3 antagonist, 5‐HT1A agonist and D4 partial agonist properties: (III) Activity in models of cognition and negative symptoms
British Journal of Pharmacology (2007)
-
Putative antipsychotics with pronounced agonism at serotonin 5-HT1A and partial agonist activity at dopamine D2 receptors disrupt basal PPI of the startle reflex in rats
Psychopharmacology (2007)
-
SLV313 (1-(2,3-Dihydro-Benzo[1,4]Dioxin-5-yl)-4- [5-(4-Fluoro-Phenyl)-Pyridin-3-ylmethyl]-Piperazine Monohydrochloride): A Novel Dopamine D2 Receptor Antagonist and 5-HT1A Receptor Agonist Potential Antipsychotic Drug
Neuropsychopharmacology (2007)