Abstract
An objective, laboratory-based diagnostic tool could increase the diagnostic accuracy of major depressive disorders (MDDs), identify factors that characterize patients and promote individualized therapy. The goal of this study was to assess a blood-based biomarker panel, which showed promise in adolescents with MDD, in adult primary care patients with MDD and age-, gender- and race-matched nondepressed (ND) controls. Patients with MDD received cognitive behavioral therapy (CBT) and clinical assessment using self-reported depression with the Patient Health Questionnaire–9 (PHQ-9). The measures, including blood RNA collection, were obtained before and after 18 weeks of CBT. Blood transcript levels of nine markers of ADCY3, DGKA, FAM46A, IGSF4A/CADM1, KIAA1539, MARCKS, PSME1, RAPH1 and TLR7, differed significantly between participants with MDD (N=32) and ND controls (N=32) at baseline (q< 0.05). Abundance of the DGKA, KIAA1539 and RAPH1 transcripts remained significantly different between subjects with MDD and ND controls even after post-CBT remission (defined as PHQ-9 <5). The ROC area under the curve for these transcripts demonstrated high discriminative ability between MDD and ND participants, regardless of their current clinical status. Before CBT, significant co-expression network of specific transcripts existed in MDD subjects who subsequently remitted in response to CBT, but not in those who remained depressed. Thus, blood levels of different transcript panels may identify the depressed from the nondepressed among primary care patients, during a depressive episode or in remission, or follow and predict response to CBT in depressed individuals.
Similar content being viewed by others
Introduction
Major depressive disorder (MDD) is a complex psychiatric disease affecting 6.7% of the US adult population in a year,1 with a steadily increasing prevalence.2,3 The World Health Organization has determined that depressive disorders are the leading cause of disability worldwide.4 The recurrent and chronic forms of depression account for the bulk of the high burden associated with the disorder.5 Approximately 50% of patients who recover from an initial episode of depression will have at least one subsequent depressive episode, and those patients with a history of two or more past episodes will have a 70–80% likelihood of recurrence in their lives. The number of previous episodes and subclinical residual symptoms are the most important predictors of relapse.6 Successful treatment of depression relies first upon accurate diagnosis. Currently, depression is diagnosed based on the patients’ self-report of their symptoms and the evaluation of a structured psychiatric interview(s) with the patient by a psychiatrist, psychologist or primary care physician. The severity of self-reported and clinician rated depression symptoms is sometimes in disagreement, since depressed patients frequently underreport depression symptoms or inadequately characterize them.7 Similarly, there is no perfect harmony between the different depression scoring systems.8 There are no reliable, objective biological diagnostic tests for major depression either.9 The diagnostic delay is 2–40 months; and the longer this period, more difficult it is to treat depression.10,11 Most depression is treated in primary care: it is estimated that 12.5% of primary care patients have had MDD in any given year, but only 47% of those cases are recognized clinically.12
Biological markers of different etiologic pathways and/or endophenotypes could provide objective, laboratory-based data to augment patient reported symptoms and improve the accuracy of diagnosis. Biomarkers may be useful in providing information about prognosis under different treatment regimens. The diagnosis and classification of MDD could lead to enhanced individualized care. We have recently identified a panel of blood biomarkers in specific animal models of depression13 and showed that they can distinguish subjects with early-onset MDD from matched controls.14 The present study explores these candidate biomarkers in a clinical setting, in which subjects with MDD are treated with cognitive behavioral therapy (CBT).
Materials and methods
This study was conducted in the context of a previously reported trial comparing the efficacy of face-to-face and telephone-administered CBT.15 Participants with MDD were randomized to two groups, comparing 18 sessions of CBT, administered either face-to-face or by telephone by a PhD level psychologist. These methods of treatment administration produced equivalent outcomes for depression.16
Recruitment and procedures
Participants, recruited from November 2007 to December 2010 were from Northwestern General Internal Medicine clinics and were included if they were ⩾18 years old, could speak and read English and provided informed consent. MDD subjects met criteria for MDD based on the Mini International Neuropsychiatry Interview,17 had a Hamilton Depression Rating Scale (Ham-D)18 score ⩾16 and were able to participate in face-to-face or telephone therapy. Nondepressed controls matched by age, race and sex, were recruited with the help of NUgene (Northwestern Medicine, Northwestern University) and included if they did not meet criteria for depression and scored⩽four on Patient Health Questionnaire–9 (PHQ-9).
Participants were excluded if they: (1) had visual or hearing impairments; (2) met diagnostic criteria for other psychiatric disorders (for example, bipolar disorder, psychotic disorders, and so on) or depression of organic etiology (for example, hypothyroidism); (3) reported alcohol or substance abuse severe enough that two psychologists agreed psychotherapy would be inappropriate, (4) met criteria for dementia by scoring <25 on the telephone interview for cognitive status;19 (5) exhibited severe suicidality, including a plan and intent, or a suicide attempt in the past 5 years; (6) were receiving or planning to receive individual psychotherapy; or (7) had initiated antidepressant pharmacotherapy in the previous 10 days. This trial was approved by the Northwestern University IRB and was monitored by an independent data safety monitoring board.
MDD diagnosis was evaluated at baseline and at posttreatment (week 18) using the Mini International Neuropsychiatry Interview. Depression severity was evaluated by self-report using the PHQ-9 at baseline and posttreatment. The PHQ-9 was selected because its items map onto diagnostic criteria for MDD and are, therefore, specific to depression. Because patients who no longer reach criteria for MDD at posttreatment may still experience significant symptoms, patients were also classified as reaching full remission based on the MacArthur criterion of PHQ-9⩽5.20 Venous blood (2.5 ml) was collected into PAXgene Blood RNA tubes (Qiagen, Germantown, MD, USA) for RNA analysis both at baseline and posttreatment from subjects with MDD and at baseline from ND controls.
Determination of blood transcript levels of candidate markers
Blood RNA was extracted using the PAXgene Blood RNA Kit (Qiagen), according to the manufacturer’s protocol. The yield and quality of extracted RNA were assessed using the NanoDrop 1000 spectrophotometer (NanoDrop Technologies, Wilmington, DE, USA). cDNA was prepared using random primers and the TaqMan RT reagents (ABI). Specific primers are listed in Supplementary Table S1, some of which were reported previously.14 Quantitative real time PCR (qPCR) was carried out using SYBR Green and the ABI 7900 (Applied Biosystems, Foster City, CA, USA), with 18s rRNA as the internal control. 18s was chosen as the normalizing gene after an extensive comparative pilot study using several housekeeping genes (data not shown). Each sample for each transcript was measured in triplicate using 5 ng of template.
Baseline samples, collected from 32 patients with a current MDD episode and 32 ND subjects, were analyzed in parallel. ΔCT values from qPCR characterized transcript abundance, where ΔCT is the cycle threshold difference between the target gene and the housekeeping gene. Then, to avoid inter-assay variations, we re-assayed the triads: baseline MDD, post-CBT MDD and ND samples. In the statistical analyses of these results, we either compared MDD and ND transcript levels using the ΔCT values, or took advantage of the control matching design and normalized the ΔCT values of MDD subject to that of the matching ND control (which is 1) and this relative quantification number (RQ) was used.
Statistical analyses
Baseline PHQ-9 and ΔCT transcript levels were compared between MDD and ND using paired t-tests, and presented with mean and standard deviation. To avoid inflated type I errors, false discovery rates21 were estimated by q-values using the q-value package22 in R.23 We made an a priori decision to interpret significant q-values and an effect size of >0.45 as clinically significant, which corresponds to Cohen’s medium effect size.24
Posttreatment RQ were compared between those who were in clinical remission (PHQ-9 ⩽5) and those who remained depressed using generalized linear models, adjusting for age, sex and race. Nonparametric tests were also used with similar results (not reported). Note that when comparisons were made between matched data (MDD and ND), analyses were not further adjusted for age, sex and race; however, in the comparisons of remission or not at week 18, analyses were adjusted. Correlational expression analyses of RQ values were carried out by Spearman correlation. Two genes were considered to be co-expressed if their Spearman correlation was >0.7 and the test statistics against zero correlation was <0.01.
Area under the receiver operating curve (AUC) was calculated against ND for those who remitted and those who did not. As an alternative analysis,25 1000 bootstrap samples of size 50 (including non-remitters, remitters and ND) were taken, and AUC was calculated for non-remitters relative to ND, and remitters relative to ND, separately. Median AUC and empirical 95% intervals are presented for each comparison. Transcripts showing significant AUC using both methods of analyses are reported.
Results
Participant characteristics
A total of 64 participants were enrolled, 32 with MDD and 32 who were not depressed (ND). As expected, the MDD sample was significantly more depressed on the PHQ-9 measure at baseline (P<0.001; Table 1).
Posttreatment depression scores were available for 27 MDD subjects. There was a significant (P<0.001) reduction in PHQ-9, dropping from baseline 18.4 (s.d.=4.5) to 8.2 (s.d.=6.1). Of these 27 MDD participants, 22 completed week 18 blood draws. MDD subjects were characterized posttreatment, using the MacArthur criteria of PHQ-9 <5 for full remission,20 into those in full remission (N=9) and those who were not (N=13). Patients meeting the remission criterion had a mean PHQ-9=2.44 (s.d.=1.94) whereas those who did not meet the criterion had a mean PHQ-9=11.46 (s.d.=4.71). Patients who remitted were younger (age 42.8 (s.d.=11.4) vs 57.4 (s.d.=14.7), Student’s t-test P=0.008), and more likely employed (82% vs 38%, Fisher’s exact test, P=0.047). There were no differences between remitters and non-remitters in comorbidities, education, marital status, race, sex or antidepressant use.
Transcript level differences at baseline and post-CBT
Levels of twenty transcripts were measured at both baseline and post-CBT. (Tables 2, 3 and Supplementary Figures 1 and 2). At baseline, blood transcript levels differed between subjects with MDD from their age, sex and race-matched ND controls for adenylate cyclase 3 (ADCY3), diacylglycerol kinase, alpha (DGKA), family with sequence similarity 46, member A (FAM46A), immunoglobulin superfamily, member 4 (IGSF4) also known as cell adhesion molecule 1 (CADM1), KIAA1539, which either have no brain-related functions to date or no known function, myristoylated alanine-rich protein kinase C substrate (MARCKS), proteasome activator subunit 1 (PSME1), Ras association and pleckstrin homology domains 1 also known as LPD (RAPH1) and intracellular Toll-like receptor 7 (TLR7) (q-values <0.05; Table 2). Post-CBT transcript abundance in MDD samples remained significantly different from ND controls for DGKA, IGSF4A/CADM1, KIAA1539, MARCKS and RAPH1 (Table 3). There was no difference in baseline gene expression between the group assigned to face-to-face CBT compared with telephone-administered CBT (mean Wilcoxon rank-sum P=0.679 (range=0.071–0.969)); nor were there differences observed by age, sex, education, marital status, race, antidepressant medication use, employment, history of generalized anxiety, history of obsessive compulsive disorder, alcohol dependence, melancholia, panic disorder or social phobia.
Scatter plots of ΔCT values for each transcript measured at baseline and post-CBT in MDD subjects and their matched controls are presented in Supplementary Figures 1 and 2.
Transcript level differences by remission
Subjects were divided into those who remitted at the end of CBT (PHQ-9<5), and those who did not remit. Post-CBT RQ values differed between these subjects in levels of N-acylsphingosine amidohydrolase (acid ceramidase) 1 (ASAH1), ATPase, Class VI, Type 11C (ATP11C) and KIAA1539 (Table 4). These differences, however, were not significant when adjusted for multiple comparisons (q-values not shown). Post-CBT, there was no difference in transcript levels between the group assigned to face-to-face CBT compared with telephone-administered CBT (mean Wilcoxon rank-sum P=0.694 (range=0.336–0.999)).
Trait markers: transcript level differences between subjects with MDD and controls regardless of current clinical diagnosis
Both baseline and post-CBT blood transcript levels differed between MDD vs ND controls in DGKA, IGSF4A/CADM1, KIAA1539, MARCKS and RAPH1. Rec eiver-operating characteristics for post-CBT measures of blood transcript levels revealed that RAPH1, KIAA1539 and DGKA had significant AUC for subjects who remitted after CBT, but also for subjects who did not remit (Supplementary Table S2). Thus, these markers had good discriminative characteristics, with significant specificity and selectivity for subjects with MDD vs ND controls even when MDD patients were no longer depressed.
Co-expression patterns of transcripts at baseline predict remission or persisting clinical depression post CBT
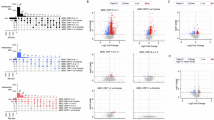
Correlational expression networks representing baseline co-expression patterns of transcripts, normalized to their matched controls (RQ), in subjects remitted and non-remitted after CBT are shown in Figure 1. In total, 15 co-expressed gene-pairs were found in the non-remitted group and 20 pairs were found in the remitted group. The extensiveness of correlation at baseline was greater for those who remitted compared with those who did not at post-CBT. Eleven ‘hubs’, identified as having significant correlations with three or more transcripts, were in the remitted, compared with five in the non-remitted population of MDD patients. Specifically, transcript levels of ADCY3, DGKA, IGSF4A/CADM1, PSME1 and RAPH1 are correlated significantly at baseline in subjects who remitted in response to CBT. None of these transcripts correlated in their expression at baseline in those subjects who remained clinically depressed after CBT.
Correlational expression networks. Co-expression patterns of transcript levels at baseline, normalized to their matched controls (RQ), of subjects remitted (a) and non-remitted (b) after CBT. Two genes were considered to be co-expressed if their Spearman correlation was >0.7 and the test statistics against zero correlation was <0.01. Red lines represent common co-expression of non-remitted and remitted groups, and black lines represent group-specific co-expression. Transcripts showing significantly different levels at baseline between subjects with MDD and ND controls are plotted with filled circles. CBT, cognitive behavioral therapy; MDD, major depressive disorder; ND, nondepressed.
Discussion
The search for an objective diagnostic test with high sensitivity and specificity for MDD has been ongoing for decades. We and others have shown that it is possible to approach this question using unbiased ‘omics’ to identify candidate blood marker panels, as reviewed by Menke.26 In the present work, we examined the performance of a panel of blood transcriptomic markers in a clinical population of subjects with MDD. The results are the first at many levels. Abundance of nine transcripts differed significantly between subjects with MDD and ND controls, suggesting that this panel could be diagnostic in a clinical, not medication-free population. Transcript levels of three genes follow the remission status post CBT, raising the possibility that these can be used to survey treatment efficacy. Blood levels of three transcripts differed between ND controls and MDD subjects, in those who remitted in response to CBT, and in those who did not respond to CBT and remained clinically depressed. These markers come closest to the ultimate goal of identifying predisposition to depression, even in the absence of a current depressive episode. Finally, another first is the fingerprint-like co-expression network that could predict whether the patient will get well after CBT or not, before the therapy begins.
In our previous studies, we described the discovery of a blood transcriptomic marker panel using two animal models of depression, a genetic and a chronic stress model.13,14 In a pilot study we had shown that some of the transcriptomic markers comprising this panel differ in their abundance between teenagers with MDD and those with no disorder.14 The present study differs in the wide age range (23–83) and concurrent medication status of the participants compared with the tight age range (15–19) and medication-free requirement of the adolescent study. Despite these differences, three of the nine transcripts, whose blood levels differed significantly between subjects with MDD and ND controls in the current study, PSME1, RAPH1 and IGSF4A also differed between medication-free MDD teenagers and controls.14 These results, therefore, represent a confirmation and suggest that these transcripts participate in processes that are characteristic of depressed mood, or of other endophenotypes intricately involved in MDD.
Earlier studies of transcriptional profiling of psychiatric illnesses used RNA derived from postmortem brain tissue.27 However, the limitation of this approach and accessibility of peripheral blood cells prompted a series of investigations to prove the overlap between gene expression in peripheral blood and brain.28, 29, 30 Transcriptional profiling in peripheral blood has been used to find biomarkers for patients with psychiatric disorders.31, 32, 33, 34, 35, 36 A multi-assay, serum-based biological diagnostic tests for MDD has also been proposed by Papakostas et al.37 Serum levels of nine biomarkers are measured in this test and a proprietary algorithm generates the results. These blood-based biomarker studies, together with our present and previous14 reports, demonstrate the potential of using blood as a proxy for the brain.28,30
Here we report the first identification of molecular trait markers for MDD. Three transcripts, with levels that differed significantly between MDD patients and controls when subjects with MDD were depressed, remained different even when patients were no longer clinically depressed. This pattern may be due to direct or indirect consequences of genetic variation between controls and MDD subjects. However, none of these three genes, RAPH1, which is also named as amyotrophic lateral sclerosis 2 (juvenile) chromosome region, candidate 9, KIAA1539, also known as FAM214B, and DGKA were found to be associated with major depression in individual genome-wide association studies or meta-analyses.38, 39, 40 Thus, sequence variation or copy number variation in other functionally connected genes might be responsible for the observed trait-marker status. The simultaneous transcript level differences from ND controls in these three genes could possibly mark subjects with future recurrent depression. Liotti et al.41 used a similar design to identify depression-specific cerebral blood flow changes. They found that the pattern of acute flow changes in unipolar euthymic patients in full remission is distinct from that seen in euthymic healthy volunteers and mirrors the untreated depressed state seen during a major depressive episode. Thus, our findings along with others, suggest that disease-specific modifications of pathways present in unipolar depression are independent of clinical illness status, providing implications for the vulnerability of patients for illness relapse. Should these vulnerability markers be confirmed in larger studies, they could distinguish MDD patients from ND controls, with or without current active depressive episode. These patients, who are likely to have more than one depressive episode, once identified would benefit from active long-term antidepressant or psychotherapy treatment, which could protect, at least in part, from relapse.42
After CBT, blood transcript levels of ASAH1, ATP11C and KIAA1539 differed between remitted and non-remitted MDD patients. In a recent study, four transcripts, different from the present ones, were identified as peripheral transcriptional markers of responders and non-responders to differing antidepressant treatment.43 These markers, therefore, may be markers of depressive state, as opposed to an underlying vulnerability. Our confidence in the relationship between the presently identified markers described here and depressive state is strengthened by the fact that in our study the treatment was psychological. Furthermore, as most remitted and non-remitted patients were medicated (Supplementary Table S3), the medications themselves did not interfere with the blood marker measurements.
In a comprehensive and timely summary, Gaiteri et al.44 suggest that co-expression networks may reflect endogenous regulatory systems, and co-expression modules can be significant predictors of disease. Moreover, they propose that disease severity may interact with molecular connectivity in such a way that it places disease genes at different network locations. This possibility is explored here when we found that differences in co-expression patterns could become a predictor of CBT efficacy before therapy. Specifically, concomitant differences in the abundance of ADCY3, DGKA, IGSF4A/ CADM1, PSME1 and RAPH1 transcripts between MDD subjects and ND controls could have predictive value. This is a very promising finding as to date, there are no biomarkers or predictors of effectiveness of psychotherapy. Biomarkers of antidepressant therapy employed pharmacogenomics studies with modest results.26,45 A nonmolecular frontal quantitative electroencephalographic biomarker has also been proposed as a predictor of response to escitalopram after 1 week of treatment.46 Thus, the co-expression criteria of the specific markers before treatment could be developed, if confirmed, into an aid of CBT treatment choice in clinical practice. A current meta-analysis identified that only 14% more patients achieve remission after psychotherapy compared with care-as-usual,47 but this number may be substantially greater if patients who are likely to respond to CBT could be identified ahead of time. The significance of this possibility is clearly stated by Licinio and Wong48,49 who state that when we discover a priori biomarkers, identifying which patients will respond to which drugs (or treatment, as we suggest), therapeutics in psychiatry will be much further ahead than it is now.
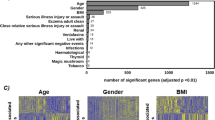
This study has a number of limitations. These include the modest sample size. In addition, there were only two samples for each MDD subject, and only one ND sample. Repeated sampling of the ND subjects would have added to the power of the design, although gene expression patterns are thought to be stable within, but differ between individuals.50, 51, 52 Should we have measured levels of transcripts at different time points during and after CBT, the kinetics of changes in transcript levels could have been determined in parallel with those of mood. An interesting finding that points to the need of large number of age-, gender- and race-stratified controls was that baseline gene expression of MDD subjects and their matched controls did vary between pairs with and without a second MDD draw (Supplementary Table S4). The cause of this is unknown, although there seems to be an age difference between women who did and did not give blood at post-CBT (see Table 1) and, therefore, an age difference in the matching control sample. This age difference did not reach significance, due to the very large age range of our sample, but it could affect gene expression differences. Even more interesting is that although matching was done only by age, sex and race, gene expression overall was not strongly associated with any of these factors. Still, transcript levels in the blood of both MDD and ND subjects varied at baseline by status of the second draw. It is worthwhile to note that the ‘trait’ marker candidates, DGKA, KIAA1359 and RAPH1 showed none of the differences between the groups with and without post-CBT blood sample.
Conclusions
This study identified nine transcripts that differentiated depressed from nondepressed participants, three of which can distinguish subjects with MDD from nondepressed controls, even after remission. A three-transcript panel discerned remitted from non-remitted patients post CBT, and concomitant abundance differences in some transcripts at baseline might indicate treatment responsiveness a priori. Thus, blood levels of different transcript panels may be useful in identifying depressed primary care patients, as well as in predicting and monitoring response to CBT. Future studies are aimed at validating these results in a larger patient population and determining the selectivity of these panels in patient population that include other psychiatric illnesses.
References
Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, Walters EE . Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 2005; 62: 593–602.
Hidaka BH . Depression as a disease of modernity: explanations for increasing prevalence. J Affect Disord 2012; 140: 205–214.
Lepine JP, Briley M . The increasing burden of depression. Neuropsychiatr Dis Treat 2011; 7: 3–7.
Ferrari AJ, Charlson FJ, Norman RE, Patten SB, Freedman G, Murray CJ et al. Burden of depressive disorders by country, sex, age, and year: findings from the global burden of disease study 2010. PLoS Med 2013; 10: e1001547.
Hardeveld F, Spijker J, De Graaf R, Nolen WA, Beekman AT . Prevalence and predictors of recurrence of major depressive disorder in the adult population. Acta Psychiatr Scand 2010; 122: 184–191.
ten Doesschate MC, Bockting CL, Koeter MW, Schene AH . Prediction of recurrence in recurrent depression: a 5.5-year prospective study. J Clin Psychiatry 2010; 71: 984–991.
Carter JD, Frampton CM, Mulder RT, Luty SE, Joyce PR . The relationship of demographic, clinical, cognitive and personality variables to the discrepancy between self and clinician rated depression. J Affect Disord 2010; 124: 202–206.
Riedel M, Moller HJ, Obermeier M, Schennach-Wolff R, Bauer M, Adli M et al. Response and remission criteria in major depression—a validation of current practice. J Psychiatr Res 2010; 44: 1063–1068.
Belmaker RH, Agam G . Major depressive disorder. N Engl J Med 2008; 358: 55–68.
Altamura AC, Buoli M, Albano A, Dell'Osso B . Age at onset and latency to treatment (duration of untreated illness) in patients with mood and anxiety disorders: a naturalistic study. Int Clin Psychopharmacol 2010; 25: 172–179.
Huerta-Ramirez R, Bertsch J, Cabello M, Roca M, Haro JM, Ayuso-Mateos JL . Diagnosis delay in first episodes of major depression: a study of primary care patients in Spain. J Affect Disord 2013; 150: 1247–1250.
Pence BW, O'Donnell JK, Gaynes BN . The depression treatment cascade in primary care: a public health perspective. Curr Psychiatry Rep 2012; 14: 328–335.
Andrus BM, Blizinsky K, Vedell PT, Dennis K, Shukla PK, Schaffer DJ et al. Gene expression patterns in the hippocampus and amygdala of endogenous depression and chronic stress models. Mol Psychiatry 2012; 17: 49–61.
Pajer K, Andrus BM, Gardner W, Lourie A, Strange B, Campo J et al. Discovery of blood transcriptomic markers for depression in animal models and pilot validation in subjects with early-onset major depression. Transl Psychiatry 2012; 2: e101.
Mohr DC, Ho J, Duffecy J, Reifler D, Sokol L, Burns MN et al. Effect of telephone-administered vs face-to-face cognitive behavioral therapy on adherence to therapy and depression outcomes among primary care patients: a randomized trial. JAMA 2012; 307: 2278–2285.
Mohr DC, Vella L, Hart SL, Heckman T, Simon GE . The effect of telephone-administered psychotherapy on depression and attrition: a meta-analysis. Clin Psych 2008; 15: 243–253.
Sheehan DV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, Weiller E et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 1998, 59((Suppl 20)): 22–33. quiz 34–57.
Hamilton M . A rating scale for depression. J Neurol Neurosurg Psychiatry 1960; 23: 56–62.
Desmond DW, Tatemichi TK, Hanzawa L . The Telephone Interview for Cognitive Status (TICS): reliability and validity in a stroke sample. Int J Geriatr Psychiatry 1994; 9: 803–807.
MacArthur Foundation's Initiative on Depression and Primary Care. The MacArthur Initiative on Depression and Primary Care at Dartmouth and Duke: Depression Management Toolkit. Hanover, NH, USA: Dartmouth, 2004.
Benjamini Y, Hochberg Y . Controlling the False Discovery Rate - a Practical and Powerful Approach to Multiple Testing. J Roy Stat Soc B Met 1995; 57: 289–300.
Storey JD, Tibshirani R . Statistical significance for genomewide studies. Proc Natl Acad Sci USA 2003; 100: 9440–9445.
Team RC R: A language and environment for statistical computing. ISBN 3-900051-07-0. R Foundation for Statistical Computing. Vienna, Austria, 2013. Avaliable online at http://www.R-project.org; 2005.
Cohen J . Statistical Power Analysis for the Behavioral Sciences. 2nd edn, Hillsdale, NJ, USA: L Erlbaum Associates, 1988.
Pepe M, Longton G, Janes H . Estimation and Comparison of Receiver Operating Characteristic Curves. Stata J 2009; 9: 1.
Menke A . Gene expression: biomarker of antidepressant therapy? Int Rev Psychiatry 2013; 25: 579–591.
Mehta D, Menke A, Binder EB . Gene expression studies in major depression. Curr Psychiatry Rep 2010; 12: 135–144.
Liew CC, Ma J, Tang HC, Zheng R, Dempsey AA . The peripheral blood transcriptome dynamically reflects system wide biology: a potential diagnostic tool. J Lab Clin Med 2006; 147: 126–132.
Rollins B, Martin MV, Morgan L, Vawter MP . Analysis of whole genome biomarker expression in blood and brain. Am J Med Genet B Neuropsychiatr Genet 2010; 153B: 919–936.
Sullivan PF, Fan C, Perou CM . Evaluating the comparability of gene expression in blood and brain. Am J Med Genet B Neuropsychiatr Genet 2006; 141B: 261–268.
Kurian SM, Le-Niculescu H, Patel SD, Bertram D, Davis J, Dike C et al. Identification of blood biomarkers for psychosis using convergent functional genomics. Mol Psychiatry 2011; 16: 37–58.
Le-Niculescu H, Kurian SM, Yehyawi N, Dike C, Patel SD, Edenberg HJ et al. Identifying blood biomarkers for mood disorders using convergent functional genomics. Mol Psychiatry 2009; 14: 156–174.
Padmos RC, Hillegers MH, Knijff EM, Vonk R, Bouvy A, Staal FJ et al. A discriminating messenger RNA signature for bipolar disorder formed by an aberrant expression of inflammatory genes in monocytes. Arch Gen Psychiatry 2008; 65: 395–407.
Menke A, Arloth J, Putz B, Weber P, Klengel T, Mehta D et al. Dexamethasone stimulated gene expression in peripheral blood is a sensitive marker for glucocorticoid receptor resistance in depressed patients. Neuropsychopharmacology 2012; 37: 1455–1464.
Segman RH, Goltser-Dubner T, Weiner I, Canetti L, Galili-Weisstub E, Milwidsky A et al. Blood mononuclear cell gene expression signature of postpartum depression. Mol Psychiatry 2010; 15: 2.
Spijker S, Van Zanten JS, De Jong S, Penninx BW, van Dyck R, Zitman FG et al. Stimulated gene expression profiles as a blood marker of major depressive disorder. Biol Psychiatry 2010; 68: 179–186.
Papakostas GI, Shelton RC, Kinrys G, Henry ME, Bakow BR, Lipkin SH et al. Assessment of a multi-assay, serum-based biological diagnostic test for major depressive disorder: a pilot and replication study. Mol Psychiatry 2013; 18: 332–339.
Shyn SI, Shi J, Kraft JB, Potash JB, Knowles JA, Weissman MM et al. Novel loci for major depression identified by genome-wide association study of Sequenced Treatment Alternatives to Relieve Depression and meta-analysis of three studies. Mol Psychiatry 2011; 16: 202–215.
Cross-Disorder Group of the Psychiatric Genomics Consortium. Identification of risk loci with shared effects on five major psychiatric disorders: a genome-wide analysis. Lancet 2013; 381: 1371–1379.
Wray NR, Pergadia ML, Blackwood DHR, Penninx BWJH, Gordon SD, Nyholt DR et al. Genome-wide association study of major depressive disorder: new results, meta-analysis, and lessons learned. Mol Psychiatry 2012; 17: 36–48.
Liotti M, Mayberg HS, McGinnis S, Brannan SL, Jerabek P . Unmasking disease-specific cerebral blood flow abnormalities: mood challenge in patients with remitted unipolar depression. Am J Psychiatry 2002; 159: 1830–1840.
Segal ZV, Bieling P, Young T, MacQueen G, Cooke R, Martin L et al. Antidepressant monotherapy vs sequential pharmacotherapy and mindfulness-based cognitive therapy, or placebo, for relapse prophylaxis in recurrent depression. Arch Gen Psychiatry 2010; 67: 1256–1264.
Belzeaux R, Bergon A, Jeanjean V, Loriod B, Formisano-Treziny C, Verrier L et al. Responder and nonresponder patients exhibit different peripheral transcriptional signatures during major depressive episode. Transl Psychiatry 2012; 2: e185.
Gaiteri C, Ding Y, French B, Tseng GC, Sibille E . Beyond modules and hubs: the potential of gene coexpression networks for investigating molecular mechanisms of complex brain disorders. Genes Brain Behav 2014; 13: 13–24.
Gunther EC, Stone DJ, Gerwien RW, Bento P, Heyes MP . Prediction of clinical drug efficacy by classification of drug-induced genomic expression profiles in vitro. Proc Natl Acad Sci USA 2003; 100: 9608–9613.
Leuchter AF, Cook IA, Marangell LB, Gilmer WS, Burgoyne KS, Howland RH et al. Comparative effectiveness of biomarkers and clinical indicators for predicting outcomes of SSRI treatment in major depressive disorder: results of the BRITE-MD study. Psychiatry Res 2009; 169: 124–131.
Cuijpers P, Karyotaki E, Weitz E, Andersson G, Hollon SD, van Straten A . The effects of psychotherapies for major depression in adults on remission, recovery and improvement: a meta-analysis. J Affect Disord 2014, 159: 118–126.
Licinio J, Wong ML . Launching the 'war on mental illness'. Mol Psychiatry 2014; 19: 1–5.
Licinio J, Wong ML . Pharmacogenomics of antidepressant treatment effects. Dialogues Clin Neurosci 2011; 13: 63–71.
Radich JP, Mao M, Stepaniants S, Biery M, Castle J, Ward T et al. Individual-specific variation of gene expression in peripheral blood leukocytes. Genomics 2004; 83: 980–988.
Eady JJ, Wortley GM, Wormstone YM, Hughes JC, Astley SB, Foxall RJ et al. Variation in gene expression profiles of peripheral blood mononuclear cells from healthy volunteers. Physiol Genomics 2005; 22: 402–411.
Mohr S, Liew C-C . The peripheral-blood transcriptome: new insights into disease and risk assessment. Trends Mol Med 2007; 13: 422–432.
Acknowledgements
This study was supported by the National Institute of Mental Health (grant R21 MH077234 and R01 MH059708) and by grants from the Davee Foundation. The sponsors had no role in the design and conduct of the study; collection, management, analysis or interpretation of the data; preparation, review or approval of the manuscript; and decision to submit the manuscript for publication. We acknowledge Neha Mehta for her help in finalizing the manuscript. We thank all subjects for the participation in this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
EER is named as an inventor on two pending patent applications, filed and owned by Northwestern University. The remaining authors declare no conflict of interest.
Additional information
For Gabor Sarkadi, MD, in memoriam.
Supplementary Information accompanies the paper on the Translational Psychiatry website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Redei, E., Andrus, B., Kwasny, M. et al. Blood transcriptomic biomarkers in adult primary care patients with major depressive disorder undergoing cognitive behavioral therapy. Transl Psychiatry 4, e442 (2014). https://doi.org/10.1038/tp.2014.66
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tp.2014.66
This article is cited by
-
Genome-wide DNA methylation and gene expression analyses in monozygotic twins identify potential biomarkers of depression
Translational Psychiatry (2021)
-
Pilot validation of blood-based biomarkers during pregnancy and postpartum in women with prior or current depression
Translational Psychiatry (2021)
-
Whole genome sequencing of nearly isogenic WMI and WLI inbred rats identifies genes potentially involved in depression and stress reactivity
Scientific Reports (2021)
-
Cerebrospinal fluid proteome evaluation in major depressive disorder by mass spectrometry
BMC Psychiatry (2020)
-
Precision medicine in perinatal depression in light of the human microbiome
Psychopharmacology (2020)