Abstract
Clinical studies report significant increases in acrolein (an α,β-unsaturated aldehyde) in the substantia nigra (SN) of patients with Parkinson’s disease (PD). In the present study, acrolein-induced neurotoxicity in the nigrostriatal dopaminergic system was investigated by local infusion of acrolein (15, 50, 150 nmoles/0.5 μl) in the SN of Sprague-Dawley rats. Acrolein-induced neurodegeneration of nigrostriatal dopaminergic system was delineated by reductions in tyrosine hydroxylase (TH) levels, dopamine transporter levels and TH-positive neurons in the infused SN as well as in striatal dopamine content. At the same time, apomorphine-induced turning behavior was evident in rats subjected to a unilateral infusion of acrolein in SN. Acrolein was pro-oxidative by increasing 4-hydroxy-2-nonenal and heme oxygenase-1 levels. Furthermore, acrolein conjugated with proteins at lysine residue and induced α-synuclein aggregation in the infused SN. Acrolein was pro-inflammatory by activating astrocytes and microglia. In addition, acrolein activated caspase 1 in the infused SN, suggesting acrolein-induced inflammasome formation. The neurotoxic mechanisms underlying acrolein-induced neurotoxicity involved programmed cell death, including apoptosis and necroptosis. Compared with well-known Parkinsonian neurotoxins, including 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine and rotenone which do not exist in the SN of PD patients, our in vivo study shows that acrolein acts as a Parkinsonian neurotoxin in the nigrostriatal dopaminergic system of rat brain.
Similar content being viewed by others
Introduction
Acrolein, an α,β-unsaturated aldehyde, is known as a toxin exogenously produced from environmental pollution, including tobacco smoking1, incomplete combustion of plastic materials2 and cooking fumes3. Endogenously, acrolein is produced from lipid peroxidation of polyunsaturated fatty acid, DNA and proteins4,5,6 as well as metabolism of allyl compounds7. Clinical studies have reported significant acrolein levels in brain and spinal cord of patients with central nervous system (CNS) neurodegenerative diseases, including Parkinson’s disease (PD)8, Alzheimer’s disease9 and spinal cord injury10. In vitro studies have demonstrated the neurotoxic effects of acrolein on HT22 hippocampal cells11, primary cortical neurons12,13 and dorsal root ganglionic neurons13, suggesting that acrolein plays a neurotoxic role in the CNS neurodegeneration14,15.
Oxidative stress is known to be involved in the acrolein-induced cytotoxicity. For example, acrolein is capable of initiating lipid peroxidation6. Furthermore, acrolein attacks mitochondrial membranes and produces reactive oxygen species (ROS)16. Due to its electrophilic activity, acrolein reportedly reacts with DNA17 and proteins4,5. A pathological role of acrolein-protein conjugation has been suggested by altering protein conformation and promoting protein aggregation in a cell-free model18. To support this notion, several in vitro studies have employed rotenone (a Parkinsonian neurotoxin) to demonstrate acrolein modified proteins, α-synuclein misfolding and aggregation in SH-SY5Y and PC12 cells19,20,21. Clinically, accumulation of acrolein-α-synuclein adducts was detected in the nigral dopaminergic neurons of PD patients8. So far, no in vivo studies have supported the influence of acrolein on α-synuclein aggregation in the brain of PD patients22.
A vicious cycle of oxidative stress, protein aggregation and cell death has been proposed for CNS neurodegeneration; this vicious cycle may be responsible for the acrolein-induced neurotoxicity in the nigrostriatal dopaminergic system, the most affected nervous system of PD. Along with the above-mentioned evidence, in vitro studies have demonstrated acrolein-induced necrosis, which may be due to attacking mitochondria, reducing ATP formation16 and increasing calpain activity13,16. Furthermore, acrolein-induced apoptosis was verified by activating caspase 3 and caspase 7 as well as forming DNA laddering, biomarkers of apoptosis23,24. Many in vivo studies have demonstrated the acrolein-induced neurotoxicity in Alzheimer’s disease and spinal cord injury10,25,26. In contrast, few in vivo studies have focused on the neurotoxic mechanisms of acrolein in the etiology of Parkinsonism. In the present study, intranigral infusion of acrolein was employed to mimic the elevated acrolein levels in the SN of PD patients8. The neurotoxic mechanisms of acrolein in nigrostriatal dopaminergic system was investigated by measuring involvement of oxidative stress, interaction of acrolein with proteins and α-synuclein, neuroinflammation and programmed cell death.
Results
Acrolein-induced neurodegeneration of nigrostriatal dopaminergic system
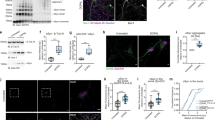
To study the role of acrolein in the pathophysiology of Parkinson’s disease, acrolein (15, 50, 150 nmoles) was locally infused in the SN of chloral hydrate-anesthetized rats. Seven days after the intranigral infusion of acrolein, several neurodegenerative features in the nigrostriatal dopaminergic system of rat brain were demonstrated. First, compared with the dopamine levels in the control striatum, higher doses of acrolein (50 and 150 nmoles) significantly reduced the dopamine content in the striatum ipsilateral to the acrolein-infused SN (Fig. 1A). Furthermore, acrolein dose-dependently decreased tyrosine hydroxylase (TH) and dopamine transporter levels (two biomarkers of dopaminergic neurons) in the infused SN (Fig. 1B,C). At the same time, the immunofluorescent staining study demonstrated acrolein (150 nmoles)-induced reduction in TH-positive neurons in the infused SN (Fig. 1D). Behaviorally, rats subjected to a unilateral infusion of acrolein in SN rotated ipsilaterally to the infused SN when challenged with apomorphine, indicating asymmetric levels of striatal dopamine contents in rat brain (Fig. 1E). These data suggest that intranigral infusion of acrolein induced neurodegeneration of nigrostriatal dopaminergic system of rat brain.
Acrolein (ARC, 15–150 nmoles) was locally infused in the substantia nigra (SN) and rats were sacrificed 7 days after intranigral infusion of acrolein. (A) Striatal dopamine content was measured using HPLC-ECD. Values are the mean ± S.E.M. (n = 5–6/group) *p < 0.05 in the striatum ipsilateral to acrolein-infused SN compared with that to the intact SN by one-way analysis of variance (one-way ANOVA) and followed by the LSD test as a post-hoc analysis. (B) Tyrosine hydroxylase (TH) in the SN was measured using Western blot. Each lane contained 3 μg proteins for all experiments. Graphs show statistic results from relative optical density of bands on the blots. Values are the mean ± S.E.M. (n = 3/group). *p < 0.05 in the acrolein-infused SN compared with the intact SN by one-way analysis of variance (one-way ANOVA) and followed by the LSD test as a post-hoc analysis. (C) Dopamine transporter in the SN was measured using Western blot. Each lane contained 25 μg proteins for all experiments. Values are the mean ± S.E.M. (n = 7/group). *p < 0.05 in the acrolein-infused SN compared with the intact SN by t-test. (D) Representative confocal microscopic data showed TH-positive neurons in the SN of rat subjected to intranigral infusion of acrolein (150 nmoles). TH-positive cells in acrolein-infused SN were counted and expressed as % of that in the contralateral intact SN. Values are the mean ± S.E.M. (n = 5). *p < 0.05 in the acrolein-infused SN compared with the control SN by t-test. (E) A behavioral study of apomorphine-induced rotations in rats subjected to a unilateral infusion of acrolein (n = 6) or vehicle (n = 4) in the SN. Values are the mean ± S.E.M. *p < 0.05 in the contralateral rotations compared with the ipsilateral rotations in rats with acrolein-infused SN by Mann-Whitney Rank Sum Test. n.s.: not significant.
Acrolein-induced oxidative stress and protein aggregation in nigrostriatal dopaminergic system
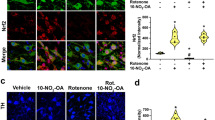
To investigate the involvement of oxidative stress in acrolein-induced neurotoxicity in the nigrostriatal dopaminergic system, both dose- and time-dependent effects of acrolein on 4-hydroxy-2-noneal (4-HNE, a by-product of lipid peroxidation) and heme oxygenase-1 levels (HO-1, a redox-regulated protein) were measured using Western blot assay. Seven days after the intranigral infusion of acrolein, dose-dependent increases in 4-HNE and HO-1 levels were observed in the acrolein-infused SN (Fig. 2A and C). Furthermore, intranigral infusion of acrolein (150 nmoles) increased 4-HNE and HO-1 levels in a time-dependent manner (Fig. 2B and D). These data indicate that intranigral infusion of acrolein is capable of inducing oxidative stress. Due to the electrophilic property of acrolein, we detected elevations in acrolein-protein adducts by increasing FDP-lysine levels in the acrolein-infused SN (Fig. 3A and B). At the same time, the ability of acrolein to induce α-synuclein aggregation was evaluated by measuring the levels of α-synuclein aggregates. Western blot assay showed that acrolein reduced α-synuclein monomer (17 kDa) and increased α-synuclein trimer levels (51 kDa) in time- and dose-dependent manners (Fig. 3C and D). Furthermore, the immunostaining study demonstrated co-localization of immunoreactivities of acrolein and α-synuclein in the acrolein-infused SN (Fig. 3E). These data indicate that acrolein is capable of inducing protein conjugation and α-synuclein aggregation in the nigrostriatal dopaminergic system of rat brain.
(A) and (C): For a dose-dependent effect, ARC (15–150 nmoles) was locally infused in the substantia nigra (SN) and rats were sacrificed 7 days after intranigral infusion of acrolein. (B) and (D): For a time-dependent effect, acrolein (150 nmoles) was locally infused in the SN and rats were sacrificed at the time indicated. Western blot assay was employed to detect 4-HNE (A,B) and HO-1 (C,D) in the SN. Each lane contained 25 μg proteins for all experiments. Graphs show statistical results from relative optical density of bands on the blots estimated by Image J. Values are the mean ± S.E.M. (n = 3/group). *p < 0.05 in the acrolein-infused SN compared with the intact SN by one-way analysis of variance (one-way ANOVA) and followed by the LSD test as a post-hoc analysis.
(A and C): For a dose-dependent effect, ARC (15–150 nmoles) was locally infused in the substantia nigra (SN) and rats were sacrificed 7 days after intranigral infusion of acrolein. (B and D): For a time-dependent effect, acrolein (150 nmoles) was locally infused in the SN and rats were sacrificed at the time indicated. Western blot assay was employed to detect FDP-lysine (A,B) and α-synuclein (C,D) in the SN. Each lane contained 25 μg proteins for all experiments. Graphs show statistical results from relative optical density of bands on the blots estimated by Image J. Values are the mean ± S.E.M. (n = 3/group). *p < 0.05 in the acrolein-infused SN compared with the intact SN by one-way analysis of variance (one-way ANOVA) and followed by the LSD test as a post-hoc analysis. (E) Representative confocal microscopic data showed co-localization of FDP-lysine and α-synuclein immunoreactivities in the infused SN of rat brain. Acrolein (150 nmoles) was locally infused in the SN and rats were sacrificed 48 hrs after intranigral infusion of acrolein. Scale bars: 10 μm. Results were repeated in independent experiments.
Acrolein-induced neuroinflammation in nigrostriatal dopaminergic system
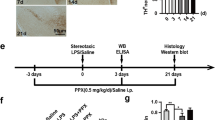
The involvement of neuroinflammation in acrolein-induced neurotoxicity was investigated by measuring GFAP and ED-1, respective biomarkers of activated astrocytes and microglia. Intranigral infusion of acrolein induced time- and dose-dependent increases in GFAP and ED-1 in the acrolein-infused SN (Fig. 4A and B). Furthermore, the effect of acrolein on inflammasome formation (a central role in neuroinflammation) was studied by measuring active caspase 1, an inflammatory caspase of inflammasome. Western blot assay showed that acrolein increased active caspase 1 levels (20 kDa) in the infused SN (Fig. 4C and D). These data suggest that acrolein is capable of inducing neuroinflammation, including glial activation and inflammasome formation.
(A and C), For a dose-dependent effect, ARC (15–150 nmoles) was locally infused in the substantia nigra (SN) and rats were sacrificed 7 days after intranigral infusion of acrolein. (B and D): For a time-dependent effect, acrolein (150 nmoles) was locally infused in the SN and rats were sacrificed at the time indicated. Western blot assay was employed to detect GFAP and ED-1 (A,B) as well as caspase 1 activation (C,D) in the SN. Each lane contained 25 μg protein for all experiments. Graphs show statistic results from relative optical density of bands on the blots estimated by Image J. Values are the mean ± S.E.M. (n = 3/group). *p < 0.05 in the acrolein-infused SN compared with the intact SN by one-way analysis of variance (one-way ANOVA) and followed by the LSD test as a post-hoc analysis.
Acrolein-induced programmed cell death in nigrostriatal dopaminergic system
The neurotoxic mechanisms underlying acrolein-induced neurodegeneration were investigated by measuring the incidences of apoptosis and necroptosis. Seven days after intranigral infusion of acrolein, dose-dependent reduction in procaspase 3 levels (35 kDa) and elevation in activated caspase 3 levels (19 kDa, a hallmark of apoptosis) were observed in acrolein-infused SN (Fig. 5A). Furthermore, acrolein dose-dependently increased receptor interacting protein kinases (RIPK)-1 (78 kDa) and RIPK-3 levels (53 kDa), biomarkers of necroptosis, in the infused SN (Fig. 5B). For a time-dependent effect, acrolein (150 nmoles) significantly increased active caspase 3, RIPK-1 and RIPK3 levels from 96–168 hrs after intranigral infusion (Fig. 5C and D). These data indicate that both apoptosis and necroptosis were involved in the acrolein-induced neurotoxicity in nigrostriatal dopaminergic system of rat brain.
(A and C), For a dose-dependent effect, ARC (15–150 nmoles) was locally infused in the substantia nigra (SN) and rats were sacrificed 7 days after intranigral infusion of acrolein. (B and D): For a time-dependent effect, acrolein (150 nmoles) was locally infused in the SN and rats were sacrificed at the time indicated. Western blot assay was employed to detect caspase 3 activation (A,B) as well as RIP-1 and RIP-3 (C,D) in the SN. Each lane contained 25 μg protein for all experiments. Graphs show statistic results from relative optical density of bands on the blots estimated by Image J. Values are the mean ± S.E.M. (n = 5/group for A, n = 3/group for B–D). *p < 0.05 in the acrolein-infused SN compared with the intact SN by one-way analysis of variance (one-way ANOVA) and followed by the LSD test as a post-hoc analysis.
Discussion
To study the neurodegeneration of nigrostriatal dopaminergic system in Parkinson’s disease, several well-known neurotoxins, including rotenone and 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine have been used in vitro and in vivo27. In the present study, we are the first to employ intranigral infusion of acrolein which better mimics the situation in PD patients as it accumulates in these patients8, while other Parkinsonian neurotoxins, including MPTP, do not. In the past, local infusion of acrolein has been used in a spinal cord injury animal model by infusing 1.6 μl of 1 M acrolein (equivalent to 1.6 μmole)28. Here, we infused a smaller volume (0.5 μl) of lower concentrations of acrolein (0.03–0.3 M) for the PD model. The acrolein doses we used were 15–150 nmoles which were only 1–10% of that in the spinal cord injury animals28. Using this PD model, our data are the first to show that acrolein is capable of inducing neurodegeneration of nigrostriatal dopaminergic system of rat brain, including acrolein-induced reductions in TH and dopamine transporter levels, decreases in TH-positive neurons in the acrolein-infused SN, depletion in striatal dopamine levels and apomorphine-induced asymmetric rotation. These in vivo results demonstrate a PD animal model of acrolein-induced neurodegeneration of nigrostriatal dopaminergic system of rat brain.
Due to its reactive properties, acrolein reportedly plays a pro-oxidative role in the CNS neurodegenerative diseases25. In support of this notion, we demonstrated that acrolein increased 4-HNE levels, indicating that acrolein initiated lipid peroxidation29 and thus elevated oxidative stress in the nigrostriatal dopaminergic system of rat brain. HO-1 is known to increase under oxidative stress30. Our previous studies have shown elevations in HO-1 expression in response to oxidative stress by iron and arsenite31,32. In vitro studies have reported acrolein-increased HO-1 protein expression in the endothelial cells33. Consistently, our in vivo data showed acrolein-induced elevation in HO-1 levels in the infused SN of rat brain, suggesting that acrolein is pro-oxidative and is capable of inducing oxidative injury.
Because of its electrophilic activity, acrolein reportedly attacks biomolecules, including proteins4,17. In the present study, we detected significant increases in FDP-lysine adducts i.e., acrolein-lysine modified proteins in the infused SN. Furthermore, we chose α-synuclein as a target protein for acrolein and found co-localization of acrolein and α-synuclein in the infused SN. These data further support the clinical finding of acrolein-α-synuclein conjugates in the SN of PD patients8. Moreover, we are the first to show that acrolein is capable of inducing α-synuclein aggregation in the infused SN, suggesting a pathological role of acrolein in forming α-synuclein aggregates detected in the Lewy bodies of PD brain22. Accordingly, acrolein may exert its neurotoxic action via conjugating proteins, altering protein conformation, forming misfolding proteins and protein aggregates in the affected brain tissues.
Oxidative stress, α-synuclein aggregation and cell death are suggested previously as a vicious cycle in the pathophysiology of Parkinsonism; neuroinflammation may be the center of this vicious cycle34 in acrolein-induced neurotoxicity. Indeed, we found that acrolein is pro-inflammatory by activating astrocytes and microglia. Activated glial cells are important sources of pro-inflammatory cytokines and free radicals35,36 which reportedly contribute to α-synuclein aggregation37. In this PD model, acrolein may exert its neurotoxic action by deregulating inflammasome activity38 in the activated microglia39. The first line of evidence for acrolein-induced inflammasome formation is caspase1 activation in the acrolein-infused SN. One possible mechanism for acrolein-induced inflammasome formation may be due to acrolein-induced α-synuclein aggregation40. Several pathological functions of caspase 1 have been suggested. First, caspase 1 has been shown to induce α-synuclein aggregation41 and thus may augment the vicious cycle in the affected nigrostriatal dopaminergic system. In addition, caspase 1 is known to proteolytically cleave pro IL-1β into the biologically active IL-1β, an pro-inflammatory cytokine42,43. In support of this notion, we detected reduction in proIL-1β and elevation in mature IL-1β levels in the acrolein-infused SN (data not shown).
Acrolein-induced neurotoxicity is reportedly mediated via non-programmed necrosis and apoptosis16,23,44. Consistently, we detected acrolein-induced apoptosis because intranigral infusion of acrolein activated caspase 3 in the infused SN. In addition, our data are the first to suggest two types of programmed necrosis involved in the acrolein-induced neurotoxicity in nigrostriatal dopaminergic system of rat brain. One is necroptosis, a kinase-regulated necrotic process involving RIPK in the necrosome complex45. Acrolein-induced elevations in RIPK-1 and RIPK-3 suggest that acrolein is capable of inducing necroptosis which results in rapid plasma membrane permeabilization, release of cell contents and exposure of damage-associated molecular patterns45. The other is pyroptosis, an inflammation-related cell death46,47. During the acrolein-induced inflammasome formation, activated caspase 1 may cleave gasdermin D and then result in pyroptosis, a lytic cell death46,47.
In conclusion, we establish a PD animal model by intranigral infusion of acrolein and show that acrolein is neurotoxic via first inducing oxidative stress (8–24 h), protein conjugation (8–24 h), and then α-synuclein aggregation (48 h) and neuroinflammation (48 h) in the nigrostriatal dopaminergic system of rat brain. Later on, acrolein induces apoptosis, necroptosis and pyroptosis (96 h) which finally leads to neurodegeneration of nigrostriatal dopaminergic system of rat brain.
Materials and Methods
Adult, male Sprague-Dawley rats, weighing 250–350 g, were purchased from by the National Laboratory Animal Breeding and Research Center, Taipei, Taiwan, R.O.C. All animals were housed in an air-conditioned room (22 ± 2 °C) on a 12-h light/dark cycle (06:00–18:00 h) and had free access to food and water. The use of animals has been approved by the Institutional Animal Care and Use Committee of Taipei Veterans General Hospital, Taipei, Taiwan, R.O.C. The methods were carried out in accordance with the approved guidelines. All experiments were performed in the accordance with relevant guidelines and regulation. The approval number is IACUC2014–186.
Intranigral infusion of acrolein
Rats were anesthetized with chloral hydrate (450 mg/kg, i.p., Sigma, St. Louis, MO) and placed in a stereotaxic instrument (David Kopf Instruments, Palo Alto, CA). After skin incision and exposure of the parietal bone, holes were drilled above the cortical surface for intranigral infusion of drugs. Acrolein (Sigma, St. Louis, MO) prepared in filtered normal saline was infused stereotaxically into substantia nigra (SN) according to the following coordinates (Paxinos and Watson, 1986): 3.2 mm anterior, 2.1 mm lateral to the midline 2 mm above the interaural zero, and 3.5 mm below the incisor bar. Acrolein prepared in saline (0.5 μl) was infused at a rate of 0.2 μl/min through a 30 gauge stainless steel needle. The injection needle was held in place for an additional 3 min following drug infusion. After surgery, rats recovered from anesthesia. For the dose-dependent effect of acrolein, 3 groups of rats (3–5 rats/group) were used for intranigral infusion of acrolein (15, 50, 150 nmoles). Rats were sacrificed 7 days after intranigral infusion of acrolein. For the time-dependent effect of acrolein, 5 groups of rats (3 rats/group) were used. Rats were sacrificed 8, 24, 48, 96, 168 h after intranigral infusion of acrolein (150 nmoles). The intact SN in the contralateral hemisphere was used as a control group to the acrolein-infused SN48,49.
HPLC-EC analysis of striatal dopamine content
After decapitation, striata were dissected and immediately frozen in liquid nitrogen and stored at −70 °C until analysis. An HPLC coupled with electrochemical detection procedure was used to quantify dopamine content in striatum.
Immunofluorescence staining
Forty-eight hours after intranigral infusion of acrolein, rats were deeply anesthetized and then perfused transcardially using 4% paraformaldehyde in 0.1 M PBS. Brains were removed and placed in 30% sucrose-PBS overnight and frozen-sectioned coronally at 30 μm thickness. Sections were washed with 0.1 M PBS, incubated with 0.3% Triton X-100 and 1% goat serum (GS; Sigma, St. Louis, MO), and blocked with 3% GS for 60 min. Sections were then incubated overnight at 4 °C with primary antibodies specific for TH (Cell Signaling Tech., Danvers, MA), α-synuclein (Abcam, Cambridge, UK) and FDP-lysine (Abcam, Cambridge, UK). Afterwards, sections were incubated for 1 h at room temperature with secondary antibodies conjugated with rhodamine and fluorescein isothiocyanate (Millipore Corporation, Billerica, MA,). Nuclei were labeled with 4′, 6-diamidino-2-phenylindole (1 mg/ml) for 10 min at room temperature. Sections were mounted in glycerol and visualized by a fluorescence confocal microscope (FluoView, Olympus, Tokyo, Japan). TH-positive cells in acrolein-infused SN were counted manually and expressed as % of that in the contralateral intact SN.
Western blot analysis of relevant proteins
Frozen SN was homogenized with a sonicator in 40 μl ice-cold protease inhibitor cocktail (Calbiochem, San Diego, CA). After homogenization, the lysates were centrifuged at 12,000 × g for 30 min at 4 °C, the supernatant was frozen in liquid nitrogen and stored at −80 °C. Protein samples (3–25 μg) were run on 8–15% sodium dodecyl sulfate (SDS)-polyacrylamide gel electrophoresis and then transferred onto a nitrocellulose membrane (Bio-Rad, Hercules, CA) at 80 V for 120 minutes. Blots were probed with a monoclonal antibody against tyrosine hydroxylase (TH) (1:3000, Chemicon, Temecula, CA), dopamine transporter (1:1000, Millipore, Bedford, MA), 4-hydroxy-2-noneal (4-HNE)(1:1000, Abcam, Cambridge, UK), heme-oxygenase-1 (HO-1) (1:2000, StressGen, Victoria, CA), N-(3-formyl-3,4-dehydropiperidino)lysine (FDP-lysine, an epitope for antibody against acrolein) (1:500, Abcam, Cambridge, UK), α-synuclein (1:1000, BD Transduction Lab., Lexington, KY), glial fibrillary acidic protein (GFAP) (1:3000, Millipore, Bedford, MA), ED-1 (1:1000, AbDSerotec, Raleigh, NC), caspase-1 (1:1000, Santa Cruz Biotech, Santa Cruz, CA), caspase-3 (1:1000, Cell Signaling Tech., Beverly, MA), RIPK-1 and RIPK-3 (1:1000, Cell Signaling Tech., Danvers, MA) at room temperature for 2 h. After primary antibody incubation, the membrane was washed and incubated with horseradish peroxidase-conjugated secondary IgG (1:3000; Chemicon, Temecula, CA) for 1 h at room temperature. The immunoreaction was visualized by Amersham enhanced chemiluminescence (Amersham Pharmacia Biotech, UK). After this detection, the bound primary and secondary antibodies were stripped by incubating the membrane in stripping buffer (100 mM 2-mercaptoethanol, 2% SDS) at 50 °C for 45 min. The membrane was reprobed with β-actin antibody (1:5000, Chemicon, Temecula, CA).
Behavioral study: apomorphine-induced rotation
Two groups of rats were used, one received intranigral infusion of acrolein (150 nmoles), the other received vehicle (saline). Seven days after intranigral infusion, rats were treated with apomorphine (1 mg/kg, s.c.)50,51 Apomorphine-induced rotations were monitored and recorded by a video camera. The extent of acrolein-induced neurotoxicity is presented as the number of contralateral turns for 60 mins after apomorphine injection.
Statistics
All data are expressed as the mean ± S.E.M. Statistical comparisons were made using t-test for dopamine transporter and Mann-Whitney rank sum test for apomorphine-induced rotation. Statistical comparisons of the rest data were made using one-way analysis of variance (one-way ANOVA) and followed by the LSD test for the rest results as a post-hoc analysis. A value of p < 0.05 was considered significant.
Additional Information
How to cite this article: Wang, Y.-T. et al. Acrolein acts as a neurotoxin in the nigrostriatal dopaminergic system of rat: involvement of α-synuclein aggregation and programmed cell death. Sci. Rep. 7, 45741; doi: 10.1038/srep45741 (2017).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Feng, Z., Hu, W., Hu, Y. & Tang, M. S. Acrolein is a major cigarette-related lung cancer agent: Preferential binding at p53 mutational hotspots and inhibition of DNA repair. Proceedings of the National Academy of Sciences of the United States of America 103, 15404–15409, doi: 10.1073/pnas.0607031103 (2006).
Magnusson, R., Nilsson, C. & Andersson, B. Emissions of aldehydes and ketones from a two-stroke engine using ethanol and ethanol-blended gasoline as fuel. Environmental science & technology 36, 1656–1664 (2002).
Ho, S. S., Yu, J. Z., Chu, K. W. & Yeung, L. L. Carbonyl emissions from commercial cooking sources in Hong Kong. Journal of the Air & Waste Management Association (1995) 56, 1091–1098 (2006).
Esterbauer, H., Schaur, R. J. & Zollner, H. Chemistry and biochemistry of 4-hydroxynonenal, malonaldehyde and related aldehydes. Free radical biology & medicine 11, 81–128 (1991).
Uchida, K. et al. Acrolein is a product of lipid peroxidation reaction. Formation of free acrolein and its conjugate with lysine residues in oxidized low density lipoproteins. The Journal of biological chemistry 273, 16058–16066 (1998).
Uchida, K. Current status of acrolein as a lipid peroxidation product. Trends in cardiovascular medicine 9, 109–113 (1999).
Auerbach, S. S., Mahler, J., Travlos, G. S. & Irwin, R. D. A comparative 90-day toxicity study of allyl acetate, allyl alcohol and acrolein. Toxicology 253, 79–88, doi: 10.1016/j.tox.2008.08.014 (2008).
Shamoto-Nagai, M. et al. In parkinsonian substantia nigra, alpha-synuclein is modified by acrolein, a lipid-peroxidation product, and accumulates in the dopamine neurons with inhibition of proteasome activity. Journal of neural transmission (Vienna, Austria: 1996) 114, 1559–1567, doi: 10.1007/s00702-007-0789-2 (2007).
Bradley, M. A., Markesbery, W. R. & Lovell, M. A. Increased levels of 4-hydroxynonenal and acrolein in the brain in preclinical Alzheimer disease. Free radical biology & medicine 48, 1570–1576, doi: 10.1016/j.freeradbiomed.2010.02.016 (2010).
Park, J., Muratori, B. & Shi, R. Acrolein as a novel therapeutic target for motor and sensory deficits in spinal cord injury. Neural regeneration research 9, 677–683, doi: 10.4103/1673-5374.131564 (2014).
Huang, Y. et al. Lithium prevents acrolein-induced neurotoxicity in HT22 mouse hippocampal cells. Neurochemical research 39, 677–684, doi: 10.1007/s11064-014-1252-z (2014).
Lovell, M. A., Xie, C. & Markesbery, W. R. Acrolein is increased in Alzheimer’s disease brain and is toxic to primary hippocampal cultures. Neurobiology of aging 22, 187–194 (2001).
Liu-Snyder, P., McNally, H., Shi, R. & Borgens, R. B. Acrolein-mediated mechanisms of neuronal death. Journal of neuroscience research 84, 209–218, doi: 10.1002/jnr.20863 (2006).
Moghe, A. et al. Molecular mechanisms of acrolein toxicity: relevance to human disease. Toxicological sciences: an official journal of the Society of Toxicology 143, 242–255, doi: 10.1093/toxsci/kfu233 (2015).
Faroon, O. et al. Acrolein health effects. Toxicology and industrial health 24, 447–490, doi: 10.1177/0748233708094188 (2008).
Luo, J., Robinson, J. P. & Shi, R. Acrolein-induced cell death in PC12 cells: role of mitochondria-mediated oxidative stress. Neurochemistry international 47, 449–457, doi: 10.1016/j.neuint.2005.07.002 (2005).
Li, L., Jiang, L., Geng, C., Cao, J. & Zhong, L. The role of oxidative stress in acrolein-induced DNA damage in HepG2 cells. Free radical research 42, 354–361, doi: 10.1080/10715760802008114 (2008).
Jeong, M. S. & Kang, J. H. Acrolein, the toxic endogenous aldehyde, induces neurofilament-L aggregation. BMB reports 41, 635–639 (2008).
Yuan, Y. H. et al. The molecular mechanism of rotenone-induced alpha-synuclein aggregation: emphasizing the role of the calcium/GSK3beta pathway. Toxicology letters 233, 163–171, doi: 10.1016/j.toxlet.2014.11.029 (2015).
Naoi, M. et al. Oxidative stress in mitochondria: decision to survival and death of neurons in neurodegenerative disorders. Molecular neurobiology 31, 81–93, doi: 10.1385/mn:31:1-3:081 (2005).
Shamoto-Nagai, M. et al. An inhibitor of mitochondrial complex I, rotenone, inactivates proteasome by oxidative modification and induces aggregation of oxidized proteins in SH-SY5Y cells. Journal of neuroscience research 74, 589–597, doi: 10.1002/jnr.10777 (2003).
Spillantini, M. G., Crowther, R. A., Jakes, R., Hasegawa, M. & Goedert, M. alpha-Synuclein in filamentous inclusions of Lewy bodies from Parkinson’s disease and dementia with lewy bodies. Proceedings of the National Academy of Sciences of the United States of America 95, 6469–6473 (1998).
Dong, L. et al. Magnolol protects against oxidative stress-mediated neural cell damage by modulating mitochondrial dysfunction and PI3K/Akt signaling. Journal of molecular neuroscience: MN 50, 469–481, doi: 10.1007/s12031-013-9964-0 (2013).
Lovell, M. A. & Markesbery, W. R. Amyloid beta peptide, 4-hydroxynonenal and apoptosis. Current Alzheimer research 3, 359–364 (2006).
Shi, R., Rickett, T. & Sun, W. Acrolein-mediated injury in nervous system trauma and diseases. Molecular nutrition & food research 55, 1320–1331, doi: 10.1002/mnfr.201100217 (2011).
Huang, Y. J. et al. Acrolein induces Alzheimer’s disease-like pathologies in vitro and in vivo . Toxicology letters 217, 184–191, doi: 10.1016/j.toxlet.2012.12.023 (2013).
Bove, J. & Perier, C. Neurotoxin-based models of Parkinson’s disease. Neuroscience 211, 51–76, doi: 10.1016/j.neuroscience.2011.10.057 (2012).
Due, M. R. et al. Acrolein involvement in sensory and behavioral hypersensitivity following spinal cord injury in the rat. Journal of neurochemistry 128, 776–786, doi: 10.1111/jnc.12500 (2014).
Schaur, R. J., Siems, W., Bresgen, N. & Eckl, P. M. 4-Hydroxy-nonenal-A Bioactive Lipid Peroxidation Product. Biomolecules 5, 2247–2337, doi: 10.3390/biom5042247 (2015).
Ryter, S. W. & Choi, A. M. Heme oxygenase-1: redox regulation of a stress protein in lung and cell culture models. Antioxidants & redox signaling 7, 80–91, doi: 10.1089/ars.2005.7.80 (2005).
Yu, H. C., Feng, S. F., Chao, P. L. & Lin, A. M. Anti-inflammatory effects of pioglitazone on iron-induced oxidative injury in the nigrostriatal dopaminergic system. Neuropathol Appl Neurobiol 36, 612–622, doi: 10.1111/j.1365-2990.2010.01107.x (2010).
Teng, Y. C., Tai, Y. I., Lee, Y. H. & Lin, A. M. Role of HO-1 in the arsenite-induced neurotoxicity in primary cultured cortical neurons. Molecular neurobiology 48, 281–287, doi: 10.1007/s12035-013-8492-9 (2013).
Wu, C. C. et al. Upregulation of endothelial heme oxygenase-1 expression through the activation of the JNK pathway by sublethal concentrations of acrolein. Toxicology and applied pharmacology 214, 244–252, doi: 10.1016/j.taap.2005.12.013 (2006).
Chen, W. W., Zhang, X. & Huang, W. J. Role of neuroinflammation in neurodegenerative diseases (Review). Molecular medicine reports 13, 3391–3396, doi: 10.3892/mmr.2016.4948 (2016).
Block, M. L. & Hong, J. S. Chronic microglial activation and progressive dopaminergic neurotoxicity. Biochemical Society transactions 35, 1127–1132, doi: 10.1042/bst0351127 (2007).
Hsieh, H. L. & Yang, C. M. Role of redox signaling in neuroinflammation and neurodegenerative diseases. BioMed research international 2013, 484613, doi: 10.1155/2013/484613 (2013).
Xiang, W. et al. Oxidative stress-induced posttranslational modifications of alpha-synuclein: specific modification of alpha-synuclein by 4-hydroxy-2-nonenal increases dopaminergic toxicity. Molecular and cellular neurosciences 54, 71–83, doi: 10.1016/j.mcn.2013.01.004 (2013).
Lamkanfi, M., Vande Walle, L. & Kanneganti, T. D. Deregulated inflammasome signaling in disease. Immunological reviews 243, 163–173, doi: 10.1111/j.1600-065X.2011.01042.x (2011).
Gustin, A. et al. NLRP3 Inflammasome Is Expressed and Functional in Mouse Brain Microglia but Not in Astrocytes. PloS one 10, e0130624, doi: 10.1371/journal.pone.0130624 (2015).
Codolo, G. et al. Triggering of inflammasome by aggregated alpha-synuclein, an inflammatory response in synucleinopathies. PloS one 8, e55375, doi: 10.1371/journal.pone.0055375 (2013).
Wang, W. et al. Caspase-1 causes truncation and aggregation of the Parkinson’s disease-associated protein alpha-synuclein. Proceedings of the National Academy of Sciences of the United States of America 113, 9587–9592, doi: 10.1073/pnas.1610099113 (2016).
Chakraborty, S., Kaushik, D. K., Gupta, M. & Basu, A. Inflammasome signaling at the heart of central nervous system pathology. Journal of neuroscience research 88, 1615–1631, doi: 10.1002/jnr.22343 (2010).
Sollberger, G., Strittmatter, G. E., Garstkiewicz, M., Sand, J. & Beer, H. D. Caspase-1: the inflammasome and beyond. Innate immunity 20, 115–125, doi: 10.1177/1753425913484374 (2014).
Tanel, A. & Averill-Bates, D. A. The aldehyde acrolein induces apoptosis via activation of the mitochondrial pathway. Biochimica et biophysica acta 1743, 255–267, doi: 10.1016/j.bbamcr.2004.11.007 (2005).
Kaczmarek, A., Vandenabeele, P. & Krysko, D. V. Necroptosis: the release of damage-associated molecular patterns and its physiological relevance. Immunity 38, 209–223, doi: 10.1016/j.immuni.2013.02.003 (2013).
Vanaja, S. K., Rathinam, V. A. & Fitzgerald, K. A. Mechanisms of inflammasome activation: recent advances and novel insights. Trends in cell biology 25, 308–315, doi: 10.1016/j.tcb.2014.12.009 (2015).
Vince, J. E. & Silke, J. The intersection of cell death and inflammasome activation. Cellular and molecular life sciences: CMLS 73, 2349–2367, doi: 10.1007/s00018-016-2205-2 (2016).
Lin, A. M., Fan, S. F., Yang, D. M., Hsu, L. L. & Yang, C. H. Zinc-induced apoptosis in substantia nigra of rat brain: neuroprotection by vitamin D3. Free radical biology & medicine 34, 1416–1425 (2003).
Lin, A. M., Chao, P. L., Fang, S. F., Chi, C. W. & Yang, C. H. Endoplasmic reticulum stress is involved in arsenite-induced oxidative injury in rat brain. Toxicology and applied pharmacology 224, 138–146, doi: 10.1016/j.taap.2007.06.016 (2007).
Schwarting, R. K. & Huston, J. P. The unilateral 6-hydroxydopamine lesion model in behavioral brain research. Analysis of functional deficits, recovery and treatments. Progress in neurobiology 50, 275–331 (1996).
Ximenes, J. C. et al. Valproic Acid Neuroprotection in the 6-OHDA Model of Parkinson’s Disease Is Possibly Related to Its Anti-Inflammatory and HDAC Inhibitory Properties. Journal of neurodegenerative diseases 2015, 313702, doi: 10.1155/2015/313702 (2015).
Acknowledgements
The authors would like to express their gratitude to Dr. C. Y Chai at Academia Sinica for his long-term support. This study was supported by MOST 104-2320-B-010-016, VGH105, and the Top-notched grant from National Yang-Ming University, Taipei, Taiwan.
Author information
Authors and Affiliations
Contributions
Y.T.W. carried out animal experiments, HPLC-ECD and Western blot assay. W.Z.Z. carried out animal experiments and Western blot assay. H.J.H. carried out Western blot assay and immunofluorescent staining study. H.C.L. conceived and designed the experiments. Y.L.L. designed and interpreted the experiments. H.T.W. designed and interpreted the experiments. A.M.Y.L. conceived, designed and interpreted the experiments and writing the manuscript. All authors approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Wang, YT., Lin, HC., Zhao, WZ. et al. Acrolein acts as a neurotoxin in the nigrostriatal dopaminergic system of rat: involvement of α-synuclein aggregation and programmed cell death. Sci Rep 7, 45741 (2017). https://doi.org/10.1038/srep45741
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep45741
This article is cited by
-
Physical Exercise-Induced Activation of NRF2 and BDNF as a Promising Strategy for Ferroptosis Regulation in Parkinson’s Disease
Neurochemical Research (2024)
-
Evidence of acrolein in synovial fluid of dogs with osteoarthritis as a potential inflammatory biomarker
BMC Musculoskeletal Disorders (2021)
-
Acrolein scavenger dimercaprol offers neuroprotection in an animal model of Parkinson’s disease: implication of acrolein and TRPA1
Translational Neurodegeneration (2021)
-
Neuroprotective effect of selumetinib on acrolein-induced neurotoxicity
Scientific Reports (2021)
-
Anti-inflammatory Effect of AZD6244 on Acrolein-Induced Neuroinflammation
Molecular Neurobiology (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.