Abstract
Clinical gait analysis incorporating three-dimensional motion analysis plays a key role in planning surgical treatments in people with gait disability. The position of the Hip Joint Centre (HJC) within the pelvis is thus critical to ensure accurate data interpretation. The position of the HJC is determined from regression equations based on anthropometric measurements derived from relatively small datasets. Current equations do not take sex or age into account, even though pelvis shape is known to differ between sex, and gait analysis is performed in populations with wide range of age. Three dimensional images of 157 deceased individuals (37 children, 120 skeletally matured) were collected with computed tomography. The location of the HJC within the pelvis was determined and regression equations to locate the HJC were developed using various anthropometrics predictors. We determined if accuracy improved when age and sex were introduced as variables. Statistical analysis did not support differentiating the equations according to sex. We found that age only modestly improved accuracy. We propose a range of new regression equations, derived from the largest dataset collected for this purpose to date.
Similar content being viewed by others
Introduction
Human motion analysis has broad applications in sport, workplace ergonomics and more recently in biometrics, through the recognition of individuals from their gait pattern. A common application of motion analysis in the clinical setting is gait analysis, which plays a key role in planning orthopaedics surgical treatments in persons with walking disabilities1,2.
The location of the hip joint centres (HJC) is an important part of biomechanics modelling and has repercussion in accuracy and subsequent interpretation of gait data. For example, Stagni et al.3 studied the effect of HJC mislocation on kinematics and kinetics, and showed a 3 cm error may lead to approximately 50% difference in mean flexion-extension hip moment over the gait cycle, or a delay in the cross-over from extensor to flexor moment of 26% of the gait cycle. More recently, authors investigating the effect of HJC mislocation on results from musculoskeletal modelling showed major effect on hip joint contact forces and on hip abductor muscle forces during gait4,5.
The HJC cannot be palpated and its location needs to be estimated. In the clinical gait laboratory setting, the commonly used method is to use regression equations derived from anthropometric measurements6. Existing regression equations estimate the location of the HJC with variable accuracy, from 1.5 cm to more than 3 cm7,8,9,10,11,12. Functional calibration13,14,15 was proposed as an alternative to improve accuracy and initial results obtained in healthy adult populations were encouraging7,8,9. However, functional calibration is challenging for those with impaired movement control or reduced range of motion and recent studies suggest it may be less accurate in clinical populations10,11,16. Consequently, regression equations remain the norm in the clinical setting.
Most of the existing regression equations were developed from small sample sizes, not exceeding 32 individuals, and most of them lack variation in age and or sex. Despite known differences in the shape of the pelvis according to sex and age17,18,19 a single equation is currently used for all subjects. The aim of this study was to investigate whether sex and/or age specific regression equations improve the accuracy in locating the HJC.
Results
Data were collected from 157 individuals. Thirty scans were collected for each subgroup according to sex (male/female) and age group (children, adolescents and adults) with the exception of the children group for which scans were available only for 24 males and 13 females. The sample characteristics, the coordinates of the HJC and anthropometric measurements are summarized in Table 1 of the supplementary material. The age between males and females did not differ except for the children group, where females were older than males. The age difference led to taller females in this age group. In the other groups, the males tended to have larger body size (height and weight) than females. Anthropometric measurements were not statistically different between the adolescents and adults groups, except for inter-ASIS distance (p < 0.01) with minimal effect size (Cohen’s d = 0.03). Hence, only two age groups, 1: children and 2: skeletally matured (adolescents + adults) were considered in the remainder of the study.
The accuracy of our protocol to locate the centre of the femoral head visually was 1.1 mm (SD: 0.3 mm, cf. Supplementary materials). The repeatability intra-assessor (i.e. ± 1.96 x standard error of the measurement) was ±1.4, ±1.5 and ±1.8 mm for the posterior-anterior, medial-lateral, and inferior-superior directions respectively.
Regression equations and effect of age group and sex
The best subset analysis led to leg length (LL) being the best single predictor for all HJC coordinates (Table 2). The equations with LL demonstrated higher R2 value and smaller prediction error than the equations with inter-ASIS distance (IA) in all components of HJC coordinates. The use of pelvic depth as a single predictor would have led to significant improvement compared to leg length for the posterior-anterior and medial-lateral directions but not for the inferior-superior direction. Although the combination of predictors improved the R2 of the regressions and the mean absolute prediction error from LOOCV, this was not significant at α = 0.01.
The stepwise regression analysis identified age group as a significant categorical variable for all HJC coordinates and sex was found significant for the posterior-anterior and medial-lateral directions only. However, no interaction (i.e. different slope coefficient according to the categorical variables) was advised for any coordinate with IA and/or LL as predictor(s). Insignificant interaction between predictors and the categorical variables was confirmed visually. Indeed, Fig. 1 illustrates examples of regression equations where the slopes were allowed to change with age groups. The regression line did not fit the skeletally mature group better because the data points are clustered and do not show a clear trend. Figure 2 illustrates regression lines using a single predictor (LL or IA).
Examples of differentiating slopes according to age category: inter ASIS distance and HJCX (top) and leg length and HJCY (bottom).
The regression line drawn from the skeletally matured groups did not generalise (left graphs) and provides minimal or no improvement (Table 2) over the lines drawn from the combined groups (right graphs). Origin of the pelvis is the midpoint between the left and right ASIS and X: posterior-anterior direction, negative is posterior, Y: medial-lateral direction, positive is lateral, and Z: inferior-superior direction, negative is inferior.
Although the stepwise regression analysis suggested different intercepts for males and females, it did not reduce the leave-one-out cross-validation (LOOCV) prediction error by more than 0.2 mm (Table 2). With leg length as predictor, using different intercepts per age groups decreased the error only for the Y coordinate, and only by tenths of a millimetre and small effect size (Cohen’s d = 0.17). The differences between groups when IA was used as a predictor were larger. Different intercepts per age groups improved the accuracy for all HJC coordinates with IA, with small to medium effect sizes: Cohen’s d = 0.27, 0.45, and 0.24, for posterior-anterior, medial-lateral, and inferior-superior directions respectively. In addition, the value of R2 increased from 0.25 to 0.51 for the posterior-anterior direction (Table 2).
Generalisability of the equations
For all equations, the mean absolute prediction errors on the left side demonstrated similar values to the errors from LOOCV, with differences within 0.2 mm (Table 3, upper part). We propose the equations with leg length as single predictor for use in clinical gait analysis:

The results from Harrington et al.20 presented similar errors compared to these equations while the errors were slightly larger with the data from Leardini et al.7 (Table 3, upper part). The mean absolute prediction error from the equations of the current study was comparable to Harrington et al.20 and considerably smaller than that from Bell et al.21,22 or Davis et al.23 (Table 3, lower part). Figure 3 highlights similarities of the data available from Leardini et al.7, Harrington et al.20 and the current study.
Distribution of data samples between the current and previously published studies.
Samples of the current study are similarly distributed particularly with ones from Harrington et al.20. Origin of the pelvis is the midpoint between the left and right ASIS and X: posterior-anterior direction, negative is posterior, Y: medial-lateral direction, positive is lateral, and Z: inferior-superior direction, negative is inferior.
Discussion
Although the pelvis is known to have considerable morphological differences between sex19,24, the results of our study showed the position of the HJC in the pelvic anatomical coordinate system was not one of these major differences. Leg length was found to be the best predictor for all coordinates and our analysis did not support the use of additional anthropometric (inter ASIS distance) or categorical (age, sex) predictors. Using leg length as the single predictor, the accuracy of the regression equations to locate the HJC was 5.2 mm, 4.4 mm, and 3.8 mm in the posterior-anterior, medial-lateral and inferior-superior directions respectively (Table 3). Although inter ASIS distance is a commonly used predictor, the equations with inter ASIS distance as predictor did not perform as well as those using leg length.
For all coordinates, differentiating the rate of change with the predictors (leg length or inter ASIS distance) according to age groups did not improve the prediction accuracy statistically. The scatter plots on Fig. 1, in particular for the posterior-anterior direction (X), shows the trend is weaker when only data from skeletally mature individuals are used (especially with inter ASIS distance) and does not generalize well. By utilizing data from all age groups, the range of values increases for both the dependent and independent variables, and the trend is more representative for the overall group. Most studies prior to Harrington et al.20 determined the regression equations based on adult data only and these performed less well in children10. Our results confirm that anthropometric regression equations require the widest possible range of sizes and skeletal maturity level to generalize.
The results indicate that using different intercepts for age groups improves the prediction accuracy for the medial-lateral direction (Y) only, when using leg length as the anthropometric variable. That may be explained by the continued growth of the segments in the lateral direction, well after longitudinal growth of long bones ceased25. However, differentiating intercepts by age groups in this case led to small improvements (Cohen’s d = 0.17). Overall, our results do not suggest the equations with leg length need to change according to sex or age group (Fig. 2).
Differentiating intercepts according to age group might have a greater influence for equations with inter ASIS distance as demonstrated by the reduction of the mean prediction error: 1.3, 1.7, 1.0 mm for the posterior-anterior, medial-lateral, and inferior-superior directions, respectively. It is important to note that regression equations using inter ASIS distance as predictor may still be preferable for individuals with conditions in which leg length does not reflect the overall anatomy, such as in dwarf syndrome.
The generalizability of the equations, obtained from data on the right side, was tested using leave one out cross validation and prediction accuracy compared to data from the left side. Both tests presented equivalent values of prediction error. Our equations also demonstrated comparable accuracy when applied to an independent data set, (Table 3, upper-part, Harrington et al.20). Slightly larger errors were found when our equations was applied to data only including adult subjects (Table 3, upper-part, Leardini et al.7).
Improved accuracy of our equations was found when compared to previously published equations, except to those using pelvic depth as predictor (Table 3, lower-part). It is important to note that accuracy in this study, and in previous studies20, was calculated from medical imaging using the true pelvic depth. The accuracy of regression equations using pelvic depth may not translate to the clinical setting because of the thickness of soft tissues over the ASI and PSI bony landmarks. Soft tissues over the ASIs and PSIs affect the clinical measurement of pelvic depth and Sangeux12 found measurements of pelvic depth were systematically larger in the clinical setting compared to medical imaging, whereas inter ASIS distance and leg length measurements were not. Systematic bias was found when pelvic depth was used as a predictor for the posterior-anterior and medial-lateral directions12.
It is important to note that soft tissue thickness over the ASIs affects the origin of the pelvis anatomical coordinate system in the posterior-anterior direction and therefore the accuracy of all equations12. Consequently, a solution to measure the thickness of soft tissue over the ASI bony landmarks during static standing calibration appears as the next logical step to improve the localisation of the HJC from regression equations.
Selection criteria in our study excluded subjects with known musculoskeletal problems to avoid including abnormal proportions in the anthropometric predictors. Therefore, our results have uncertain ability to generalize to individuals with pathology or gait impairment and may still require validation for specific clinical applications. However, it is worth noting that Harrington et al.20 found no difference in the HJC prediction error between typically developed children and children with cerebral palsy, using a range of equations including theirs and that of Bell et al.21,22, Davis et al.23, and Orthotrak20.
A limitation of our study is the restricted details of the subjects. For example, the health and nutritional status, physical activity level or onset of puberty within the sample was not controlled nor known due to the nature of the data. These factors may have influenced bone development or structure. Similarly, race was not determined. We found similar relationships in the data between the position of the hip joint centres and inter ASIS distance, leg length, and pelvic depth from a variety of samples drawn from different countries (England20, Italy7, and Australia: current study, Fig. 3). However, the Caucasian race may be the most prevalent in these countries and our results may need to be confirmed with samples including different races.
Material and Methods
Study materials
Approval was granted by the custodian of the medical images, the Ethics Committee at the Victorian Institute of Forensic Medicine (VIFM, ref#: EC 15/2012) and the University of Melbourne. All methods were performed in accordance with the relevant guidelines and regulations. De-identified full-body cadaveric CT scans from individuals of different ages and sex were reviewed. All CT scans were collected between January 2007 and May 2013 as part of routine procedures. Images were taken every 1.0 mm with a slice thickness of 1.5 mm in all planes, leading to 33% overlap between slices to improve 3D display and multi-planar reconstruction26.
A sample of 180 scans, 30 scans in each of 6 groups: 3 age groups of both sex, was sought for collection. The age groups were classified as 1) children, 2) adolescents, and 3) adults, and consisted of individuals aged 5–11, 16–19, and 25–40 years old, respectively. Children aged between 12 and 15 were excluded since individuals in these ages would likely be in the middle of puberty during which peak growth in height is most likely to occur27. Subjects older than 40 years old were not included to avoid including persons with age-related degeneration of bones and joints.
To maximize the likelihood of attaining ‘typically developed’ or ‘healthy’ samples, exclusion criteria were: a) known trauma to pelvis and/or lower extremity, b) known prior musculoskeletal disease or conditions which caused obvious changes in bony structure, or c) known growth or developmental disorders affecting growth or musculoskeletal structure (e.g. Down’s syndrome, cerebral palsy, myelomeningocele, arthrogryposis, Dravet’s syndrome, osteoarthritis, etc.).
In addition to CT-scans, sex, age, height, weight, and cause of death were obtained. Sample characteristics were compared using descriptive statistics and two-sample t-tests.
Data processing
On each scan, the locations of 12 anatomical landmarks (Table 1) were identified by visual inspection from a single assessor (RH) using 3D Slicer (http://www.slicer.org). The method for localisation of the centre of the femoral head, assumed to be the HJC, followed an established protocol to determine femoral neck anteversion and neck shaft angle28. Coordinates of the landmarks were exported to calculate inter ASIS distance (IA), leg length (LL), pelvic depth (PD) and total pelvic width (TPW, Table 1). Although used in some equations in prior studies21,29,30, the pubic symphysis landmark and related measurements were not included in the current study due to the difficulty in identification of these landmarks in routine clinical examinations.
The position and orientation of the pelvis was defined according to the conventional gait model23. Coordinates of the HJC were determined in relation to the pelvic origin: the midpoint between the left and right ASIS with the HJC posterior, lateral and inferior compared to the origin. The X coordinate (posterior-anterior direction) was negative when posterior to the origin, the Y coordinate (medial-lateral direction) was positive when lateral to the origin and the Z coordinate (inferior-superior direction) was negative when inferior to the origin.
To estimate the accuracy of localisation of the HJC28, data from 10 subjects (20 limbs) selected at random were compared with automatic fitting of a sphere to 3D shape model of the femoral heads (ref. 31, details in supplementary material). To assess intra-assessor repeatability, identification of all landmarks was repeated three times on the same 10 subjects (20 limbs). Repeatability was assessed for the X, Y and Z coordinates of the right and left HJC and we calculated the standard error of the measurement (SEM).
Generation of equations
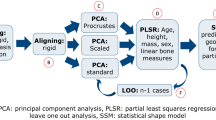
Regression equations were developed to estimate the location of the HJC from linear combinations of predictors with intercept. Data from the right side of each subject was utilized to generate equations and the best predictors were identified from a best subset regression analysis (Minitab 17, Minitab Inc., USA) between the predictors IA and LL. Pelvic depth was not included in the best subset regression analysis as the purpose was to develop equations with clinical utility. Although pelvic depth, derived from medical images, may be a good predictor for the position of the HJC20, the presence of skin and adipose tissue between the skin surface and the bony landmarks introduces an unknown magnitude of error in the corresponding clinical examination measurement and, as a consequence, in the estimate of the location of the HJC12. Regression equations including PD were derived and provided for comparison purposes only. The subjects’ age was also not included in the regression model since age did not display a linear trend with respect to the response variables across groups (cf. Fig. 1 in Supplementary Material) and age was kept as a categorical variable (1: children, 2: adolescents and 3: adults).
For each equation, the goodness of fit was estimated with the coefficient of determination (R2) of the multiple linear regression and the prediction accuracy by the mean absolute error from leave-one-out cross-validation (LOOCV)20,32. LOOCV provides a means to estimate the prediction accuracy of the regression equations for new samples. It is a particular case of k-fold cross-validation when k = 1. Given n data points, LOOCV derives n regression equations each based on n-1 data points, hence for each equation, one data point has been removed from the dataset and the absolute difference between the data point value and its estimate from the regression equation provides the prediction error.
To determine whether equations with increasing numbers of predictors led to significant improvement, the absolute prediction errors from the equations with increasing number of predictors were compared to those of the single predictor equation with paired t-test at α = 0.01. A stepwise regression analysis was also performed to investigate whether the two categorical variables, age group and sex, may be considered in the regression model. The model included the predictors, the categorical variables and the interactions between predictors and categorical variables.
Generalisability of the equations
To examine the generalisability of the equations, we applied them to the data from the left side, which was not included in the development of equations, and computed the mean absolute errors (MAE) for each subject. The generalisability of the equations was further evaluated, using data sets available from previously published studies (Harrington et al.20 and Leardini et al.7. The accuracy of equations derived in this study was also compared with common regression equations that have previously been published, e.g. Bell et al.22, Davis et al.23, and Harrington et al.12,20.
Statistical analysis was performed in Matlab with the statistics and machine learning toolbox (version 10.1, The Mathworks, USA).
Additional Information
How to cite this article: Hara, R. et al. Predicting the location of the hip joint centres, impact of age group and sex. Sci. Rep. 6, 37707; doi: 10.1038/srep37707 (2016).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Burnfield, J. M. & Perry, J. Gait analysis: normal and pathological function. (Slack, 2010).
Wren, T. A., Gorton, G. E. 3rd, Ounpuu, S. & Tucker, C. A. Efficacy of clinical gait analysis: A systematic review. Gait Posture 34, 149–153 (2011).
Stagni, R., Leardini, A., Cappozzo, A., Benedetti, M. G. & Cappello, A. Effects of hip joint centre mislocation on gait analysis results. Journal of Biomechanics 33, 1479–1487 (2000).
Lenaerts, G. et al. Subject-specific hip geometry and hip joint centre location affects calculated contact forces at the hip during gait. Journal of Biomechanics 42, 1246–1251 (2009).
Passmore, E., Pandy, M., Graham, H. K. & Sangeux, M. What is the respective effect of joint position and bone shape on clinical musculoskeletal modelling? An EOS study. Gait & Posture 49 Supplement 2, 26 (2016).
Baker, R. Measuring walking: a handbook of clinical gait analysis. (Mac Keith Press, 2013).
Leardini, A. et al. Validation of a functional method for the estimation of hip joint centre location. J Biomech 32, 99–103 (1999).
Hicks, J. L. & Richards, J. G. Clinical applicability of using spherical fitting to find hip joint centers. Gait Posture 22, 138–145 (2005).
Sangeux, M., Peters, A. & Baker, R. Hip joint center localization: evaluation on normal subjects in the context of gait analysis. Gait & posture 34, 324–328 (2011).
Peters, A., Baker, R., Morris, M. E. & Sangeux, M. A comparison of hip joint centre localisation techniques with 3-DUS for clinical gait analysis in children with cerebral palsy. Gait Posture 36, 282–286 (2012).
Sangeux, M., Pillet, H. & Skalli, W. Which method of hip joint centre localisation should be used in gait analysis? Gait Posture 40, 20–25 (2014).
Sangeux, M. On the implementation of predictive methods to locate the hip joint centres. Gait Posture 42, 402–405 (2015).
Ehrig, R. M., Taylor, W. R., Duda, G. N. & Heller, M. O. A survey of formal methods for determining the centre of rotation of ball joints. Journal of Biomechanics 39, 2798–2809 (2006).
Cappozzo, A. Gait analysis methodology. Human Movement Science 3, 27–51 (1984).
Piazza, S. J., Okita, N. & Cavanagh, P. R. Accuracy of the functional method of hip joint center location: effects of limited motion and varied implementation. J Biomech 34, 967–973 (2001).
Assi, A. et al. Validation of hip joint center localization methods during gait analysis using 3D EOS imaging in typically developing and cerebral palsy children. Gait & Posture 48, 30–35 (2016).
Preece, S. J. et al. Variation in pelvic morphology may prevent the identification of anterior pelvic tilt. J Man Manip Ther 16, 113–117 (2008).
Martini, F. H., Timmons, M. J. & McKinley, M. P. Human Anatomy. Third edn, (Prentice-Hall, 2000).
Eizenberg, N., Briggs, C., Barker, P. & Grkovic, I. (An@tomedia Pty. Ltd., 1999).
Harrington, M. E., Zavatsky, A. B., Lawson, S. E., Yuan, Z. & Theologis, T. N. Prediction of the hip joint centre in adults, children, and patients with cerebral palsy based on magnetic resonance imaging. J Biomech 40, 595–602 (2007).
Bell, A. L., Brand, R. A. & Pedersen, D. R. Prediction of hip joint centre location from external landmarks. Human Movement Science 8, 3–16 (1989).
Bell, A. L., Pedersen, D. R. & Brand, R. A. A comparison of the accuracy of several hip center location prediction methods. J Biomech 23, 617–621 (1990).
Davis, R. B., Ounpuu, S., Tyburski, D. & Gage, J. R. A gait analysis data collection and reduction technique. Human Movement Science 10, 575–587 (1991).
Arsuaga, J. L. & Carretero, J. M. Multivariate analysis of the sexual dimorphism of the hip bone in a modern human population and in early hominids. Am J Phys Anthropol 93, 241–257 (1994).
Volgyi, E. et al. Bone and body segment lengthening and widening: a 7-year follow-up study in pubertal girls. Bone 47, 773–782 (2010).
Kalender, W. A. Computed Tomography: Fundamentals, System Technology, Image Quality, Applications 3rd edition. (Publicis Publishing, 2011).
Aksglaede, L., Olsen, L. W., Sorensen, T. I. & Juul, A. Forty years trends in timing of pubertal growth spurt in 157,000 Danish school children. PLoS One 3, e2728 (2008).
Sangeux, M., Pascoe, J., Graham, H. K., Ramanauskas, F. & Cain, T. Three-dimensional measurement of femoral neck anteversion and neck shaft angle. J Comput Assist Tomogr 39, 83–85 (2015).
Seidel, G. K., Marchinda, D. M., Dijkers, M. & Soutas-Little, R. W. Hip joint center location from palpable bony landmarks–a cadaver study. J Biomech 28, 995–998 (1995).
Tylkowski, C. M., Simon, S. R. & Mansour, J. M. The Frank Stinchfield Award Paper. Internal rotation gait in spastic cerebral palsy. Hip 89–125 (1982).
Levinger, P. et al. Knee biomechanics early after knee replacement surgery predict abnormal gait patterns 12 months postoperatively. J Orthop Res 30, 371–376 (2012).
Christensen, R. Plane Answers to Complex Questions. 4 edn, (Springer-Verlag: New York, 2011).
Acknowledgements
The authors would like to thank Ms. Patricia O’Brien for her assistance and support in the study and appreciate the University of Melbourne (Faculty of Medicine, Dentistry and Health Sciences) and the Australian Federal Government for the scholarship funding for Dr. Reiko Hara.
Author information
Authors and Affiliations
Contributions
R.H., J.M., R.B. and M.S. designed the study, R.H. and C.B. organised data collection, M.S. performed the statistical analyses, R.H. and M.S. drafted the manuscript, all authors reviewed the final version.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Hara, R., McGinley, J., Briggs, C. et al. Predicting the location of the hip joint centres, impact of age group and sex. Sci Rep 6, 37707 (2016). https://doi.org/10.1038/srep37707
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep37707
This article is cited by
-
A dataset of asymptomatic human gait and movements obtained from markers, IMUs, insoles and force plates
Scientific Data (2023)
-
A multibody methodological approach to the biomechanics of swimmers including hydrodynamic forces
Multibody System Dynamics (2023)
-
Limited transfer and retention of locomotor adaptations from virtual reality obstacle avoidance to the physical world
Scientific Reports (2022)
-
On the Modeling of Biomechanical Systems for Human Movement Analysis: A Narrative Review
Archives of Computational Methods in Engineering (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.