Abstract
This study aims to determine the prevalence of health personnel with normal weight central obesity and to investigate whether this group had higher cardiovascular disease (CVD) risk factors than those of the people with normal weight and without central obesity. A waist-to-height ratio was calculated as waist circumference (at umbilical level) in cm divided by height in cm. The central obesity cut-off level was 0.5. The body mass index was calculated as weight in kg divided by height in meters squared. The obesity cut-off level was 25 kg/m2. The prevalence of health personnel with normal weight central obesity was 15.4% (499 out of 3235). When compare this group to 1787 health personnel who had normal weight and without central obesity, they were 2.03 times (95% CI of adjusted OR; 1.62 to 2.54) more likely to have at least one CVD factor. The waist-to-height ratio cut-off value of 0.5 can be used as a self-assessment tool for central obesity without the need for a standard measuring tape. It is feasible to be implemented in screening or self-monitoring for the general population.
Similar content being viewed by others
Introduction
The World Health Organization has reported that the relative distribution of excess fat could be used to determine risks of cardiovascular disease more effectively than its total amount1. Computed tomography (CT) and magnetic resonance imaging (MRI) have been used to classify fat distribution2,3. A preferential deposition of fat in the internal visceral region is classified as an apple shape, which has been deemed unhealthy. An external subcutaneous fat deposition has been classified as the pear shape, which has been assessed as being healthier4. CT and MRI scans are expensive and are not really feasible in a developing country. Waist circumference (WC) has been proposed as an anthropometric indicator for obesity5,6,7. The cut-off values are varied and are lower in Asians than those of Europeans7,8,9. There are different protocols of WC measurement, including measuring at umbilical level, the narrowest waist, at the midpoint between the lowest rib and the iliac crest, and immediately above the iliac crest10,11,12. These measurement methods produce different WC values. Furthermore, WC values also vary by gender13,14,15. Thus, different cut-off levels of WC are not practically appropriate indicators for CVD risk factors. A more simple anthropometric measurement used for self-assessment or monitoring of CVD risk factors is proposed, which is WC weighted by each individual’s height or ‘waist-to-height ratio (WHtR)’16. The cut-off value of WHtR indicating increased health risk reported by studies in different races and age groups is above 0.5. These races included people from Australia, India, Korea, China, and Thailand13,17,18,19,20. A large cohort of the British population showed that WHtR was a better predictor of mortality than BMI21,22. The WC commonly used in calculating WHtR is measured at the midpoint between the lower costal margin and superior iliac crest15. However, the level of precision is more difficult and also less practical than measurement at an umbilical level. The Thai Ministry of Public Health launched a campaign addressing obesity prevention “keep your waist circumference lower than half of your height” using WC measurement at umbilical level. These two measurements of WC gave different results and led to bias. In Japan, the differences had a range of 3.9 cm among men to 12.6 cm among women14. Experts from the UK proposed a WHtR cut-off value of 0.5 in adults, with a similar ratio in children and adolescents4,18. A systematic review found an appropriate cut-off level of a 0.5 WHtR in various ethnic groups and indicated that WHtR could be used as a screening tool for predicting CVD and diabetes23. The study involving health personnel in Thailand also found a WHtR cut-off value of 0.5 associated with CVD risk factors20. Although the campaign of “keep your waist circumference lower than half of your height” has been promoted for many years in Thailand, health personnel still use BMI for screening and monitoring in their services. This practice is our concern because the sector of the population with weight within normal limits (defined by BMI) and central obesity (defined by WHtR) are missed. This group with normal weight central obesity had a higher mortality than people with normal weight and without central obesity24. Recently, there is evidence which supports the fact that central obesity increases mortality risk and CVD mortality rates25,26. The collaborative analysis of 58 prospective studies found that subgroups of WC were associated with increased mortality risk for a given BMI category in prediction models26. Another study found that central obesity measurement was more highly associated with total and CVD mortality rates than with BMI25. On analysis the data of individual-patients with coronary artery disease showed that people in the top tertile of central obesity measures who had normal BMI had the highest total mortality rate25. A study in the UK showed that 9% of men and 11% of women who were deemed low risk by their BMI were at risk according to WHtR because they had central obesity4. Unfortunately, the recent suggested management on obesity guidelines by the American Heart Association/American College of Cardiology/The Obesity Society 2013 does not clearly recommend WHtR measurement due to limited evidence27.
WHtR requires WC measurement for calculation. Although the values of WC vary by measurement methods and gender, WHtR does not different much13. WHtR using WC measurement at umbilical level has a greater correlation with present trunk fat and a higher sensitivity than those of WHtR using other WC measurements. The UK study used WC measurement at the midpoint between the lower costal margin and iliac crest for WHtR calculation (WHtRM)4. Thaikruea et al. conducted a study involving the health personnel of Faculty of Medicine, Chiang Mai University (CMU), Thailand. They found that although the value of WC measured at umbilical level (WHtRU) was different from WHtRM in each individual but the WHtR calculations delivered by both WC methods were not significantly different. They also found that WHtRU was a better indicator for CVD risk factors than WHtRM20. From a prevention and health promotion perspective, WHtRU may be used for community screening and in self-assessment for central obesity rather than BMI. The WHtRU is simple and does not require height and WC measurements in centimetres or inches. The study aims to estimate the prevalence of normal weight central obesity among healthcare personnel and to investigate whether this group were of higher risk of CVD factors than those of the people with normal weight and without central obesity.
Results
Demographic
3235 health personnel participated in the study. The majority of them were female (76.65%) with a mean age of 40.20 years (SD 10.73 years). 64.61% had Bachelor or higher. 15.4% of the health personnel had a classification of a normal weight central obesity (WHtRU of at least 0.5 and a BMI below 25 kg/m2). 55.2% of health personnel had both a BMI and waist circumference within normal limits (WHtRU below 0.5 and BMI below 25 kg/m2) (Table 1).
Risk group by waist-to-height ratio
42.9% of the health personnel who were in the increased risk and very high risk groups (Table 2).
CVD risk factors by waist-to-height ratio and body mass index
The group with WHtRU of at least 0.5 and a BMI of at least 25 kg/m2 had the highest values of cholesterol, TG, LDL, and FBG compared to those of other groups. This group had the lowest HDL compared to those of other groups (Table 3). They had higher cholesterol, TG, LDL, and FBG than those of the group with WHtRU below 0.5 regardless of their BMI (Table 3).
The prevalence of CVD risk factors among the normal weight central obesity were high. The normal weight central obesity group was more likely to have CVD risk factors than those of the normal weight group. The relative risks ranged from 1.27 (95% CI: 1.18 to 1.37) to 3.20 (95% CI: 1.88 to 5.43) (Table 4).
Relationship between CVD risk factors and waist-to-height ratio and body mass index
When adjusted for age and gender, people in the normal weight central obesity group were more likely to have a CVD risk factor than those of the normal weight group (Table 5). They were also more likely to have a lower HDL than those of reference. Over all, the normal weight central obesity group were 2.03 times (95% adjusted OR; 1.62 to 2.54) more likely to have at least one CVD risk factor compared to the normal weight group (Table 5).
Discussions
WC shows a correlation with intra-abdominal adipose tissue and subcutaneous abdominal adipose tissue, which is related to diabetes5,6,18,28,29. Thus, WC is a better anthropometric marker of intra-abdominal adipose tissue than is BMI30. There are different protocols of WC measurement, including measuring at umbilical level, the narrowest waist, at midpoint between the lowest rib and the iliac crest, and immediately above the iliac crest12,30. These measurement methods produce different WC values. Furthermore, WC values also vary by gender13,14,15. Thus, different cut-off levels of WC are not practically appropriate indicators for the assessment of CVD risk factors15. A more simple anthropometric measurement used for self-assessment or monitoring of CVD risk factors is proposed, which is WC as a ratio to each individual’s height or ‘waist-to-height ratio’16. Our study used WHtR for the assessment of CVD risk factors. Although values of WC vary by measurement method and gender, WHtR does not vary much when using different WC measurement methods. Our study used WC measurement at umbilical level because it has a higher correlation with present trunk fat and a high level of sensitivity13,20. It is also easy to measure and understandable for laypeople. The cut-off value of WHtR indicating increased health risk was found to be 0.5, which is supported by studies in different races and age groups4,17,20,31,32.
Our study showed that there were 42.9% of CMU health personnel who were in the increased risk and very high risk groups. The health personnel who had WHtRU of at least 0.5 but had a BMI below 25 kg/m2 (in the normal weight central obesity group) were more likely to have CVD risk factors than those of the health personnel who had WHtRU below 0.5 and BMI below 25 kg/m2. This group, which was about 15% of health personnel, was missed using the BMI definition method. They might perceive that they had no risk, although they had. A study among Thai people found that individuals with a BMI at low as 23 kg/m2 were associated with CVD risk factors20. The normal weight central obesity who were at risk was 25% of the UK population31.
Our study found that the prevalence of CVD risk factors among the normal weight central obesity were high. When adjusted for age and gender, the normal weight central obesity group were more likely to have hypertension and to have high cholesterol, TG, LDL, and a FBG higher than those of a reference group. The adjusted OR ranged from 1.27 (95% CI = 1.18–1.37) of total cholesterol to 3.20 (95% CI = 1.88–5.43) of diabetics. Over all, the normal weight central obesity group were two times more likely to have at least one CVD risk factor than those of reference group. Other studies involving systematic reviews and meta-analyses have found that WHtR predicted CVD risk factors better than WC23,32,33. A study which included more than 300,000 adults from several ethnic groups supported our findings. It showed that WHtR had a higher discriminatory power than WC in indicating diabetes, hypertension, CVD and all outcomes regardless of gender. Furthermore, the rank order from highest to lowest for AUC was always WHtR, WC, then BMI. The findings also showed that Asian people had more positive results of WHtR and a higher correlation than Caucasians33. The study in Singapore based on an Asian employee health screening in 2012 had similar findings to our study. The research team also used WC measurement at umbilical level and defined a WHtR cut-off value of 0.5 for central obesity similar to data used in our study. They found that a WHtRU of at least 0.5 could identify the highest proportion of all the CVD risk factors regardless of gender, which supported our findings34.
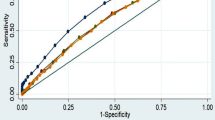
The study in the UK described central obesity and peripheral obesity as shapes of apples and pears, terms which are easy for the general population to understand4. An apple shape reflects an internal visceral fat deposition. A pear shape reflects external subcutaneous fat deposition. Although, Thai people are familiar with apples, pear and their shape may be less well-known. Therefore, for health risk communication, the phase of ‘keep waistline less than half of your height’ is easy to understand by laypeople in Thailand. Anthropometric measures usually practically enable the assessment of CVD risk factors with between 60% and 70% accuracy in practice and also in population-based screening measures33. However this study of WHtRU in CMU health personnel has 73.6% sensitivity, 67.6% specificity, and 69.1% corrected classification of having at least two risk factors of CVD. Thus, WHtRU has good accuracy in screening measures20.
Due to the nature of a cross-sectional study design, the identification of risk cannot be guaranteed in our study. However, other prospective and meta-analysis studies support the association and prediction of WHtR for CVD risk factors and health related outcomes. An 11-year prospective study among over 45,000 women below the age of 60 found that WHtR was the strongest predictor of strokes in women when compared to WC and waist-to-hip ratio, whilst BMI was not a good predictor. Although the location of visceral adipose tissue (VAT) measurement affected an association magnitude of the metabolic syndrome definitions, VAT still remained significantly associated with metabolic syndrome regardless of measurement location. Also a clinical interpretation was not changed regardless of different measurement methods or metabolic syndrome definitions21,22,32,33,34. This means our findings might not be affected much by this condition. The strengths of our study include the large sample size (more than 3,000 persons), the conduction of the investigations by trained health personnel, and the standardisation of laboratory investigations by the Medicine Faculty.
Conclusion
About 42.9% of our study population had an increased risk or a very high risk of CVD. A screening tool sensitive to visceral/trunk fat rather than body mass is more appropriate. BMI misclassified 15.4% of central obesity as non-obesity. WHtRU was more effective than BMI and WC as a screening method for CVD risk factors. The cut-off value of 0.5 can be used as a self-assessment tool for central obesity without the requirement of a standard measuring tape because it is just half the length compared to individual height20. It is worth to study about implementing this method in screening or self-assessment for the population who have normal weight central obesity. Further research is needed to evaluate the effectiveness of WHtRU in public health screening among the general population who are overweight.
Methods
Data
The Medicine Faculty of CMU provided a non-communicable disease screening for all health personnel during 2012 to 2013. All health personnel were eligible. Sample size estimation was 491 persons based on expected prevalence of a normal weight central obesity 15%, acceptable error margin of 3%, confidence level of 95%, and design effect 1.0. The participants were interviewed, had a physical examination, and had blood drawn for laboratory testing. Anthropometric measurements included height, weight, and waist circumference. A portable stadiometer and an electronic scale were used for measuring standing height (without shoes) in centimetres (cm) and weight in kilograms (kg). A standard measuring tape was used to measure horizontal waist circumference at the umbilical level. Trained investigators performed all measurements. Three blood pressure readings were taken five minutes apart using an ADC ® Digital E-Sphyg and two non-mercury sphygmomanometers with appropriate cuff size. These machines were calibrated every two months. Venous blood samples were drawn and processed at the Central Diagnostic Laboratory in CMU Hospital for a fasting blood glucose and lipid profile.
The BMI was calculated as weight in kg divided by height in meters squared (kg/m2). The obesity cut-off level was 25 kg/m2. The waist-to-height ratio (WHtR) was calculated as WC in cm divided by height in cm. Based on the Thai Ministry of Public Health, the obesity cut-off level was at least 0.5. Health personnel who had WHtR of at least 0.5 and BMI below 25 kg/m2 were defined as the ‘normal weight central obesity group’. Health personnel who had WHtR below 0.5 and BMI below 25 kg/m2 were normal weight, non-central obesity group who were used as the reference group.
Risk factors for cardiovascular disease (CVD) included hypertension, diabetes, and dyslipidemia. High blood pressure or hypertension was present if each individual was a known case of HT or had a systolic blood pressure of at least 140 and/or a diastolic blood pressure of at least 90 mmHg35. Diabetes was present if each individual was either diagnosed by physician or had a fasting blood glucose of at least 126 milligram per decilitre (mg/dl)36. Dyslipidaemia was defined as present if the individual had any one of the following conditions: 1) known case of dyslipidemia, or 2) one of these abnormal lipid profiles, which were total cholesterol of at least 200 mg/dl, triglycerides (TG) of at least 150 mg/dl, low density lipoprotein (LDL) of at least 160 mg/dl, or high density lipoprotein (HDL) below 40 mg/dl in men and below 46 mg/dl in women20,37.
All methods were carried out in accordance with relevant guidelines and regulations. All experimental protocols were approved by the Ethics Committee of the Faculty of Medicine, CMU (No. 069/2012). Informed consent was obtained from all subjects.
Statistical analysis
Descriptive analyses included proportion, mean +/− standard deviation (SD), or median (range) depending on data distribution. Univariate analysis includes relative risk (RR) with 95% confidence interval (95% CI), Chi Square test, and Kruskal-Wallis test. Multivariate analysis included multiple logistic regression (adjusted odds ratio with 95% CI). A p-value of below 0.05 was considered as statistically significant. Data management and analyses were performed using Epi Info for Windows version 3.5.4 (Centers for Disease Control and Prevention, Atlanta, GA) and STATA version 11 (Statacorp LP. College Station, TX).
Additional Information
How to cite this article: Thaikruea, L. and Thammasarot, J. Prevalence of normal weight central obesity among Thai healthcare providers and their association with CVD risk: a cross-sectional study. Sci. Rep. 6, 37100; doi: 10.1038/srep37100 (2016).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
World Health Organization. Obesity: preventing and managing the global epidemic: report of a WHO consultation on obesity, Geneva, 3–5 June 1997 Geneva. (1998).
Ashwell, M., Cole, T. J. & Dixon, A. K. Obesity: new insight into the anthropometric classification of fat distribution shown by computed tomography. Br Med J (Clin Res Ed) 290, doi: 10.1136/bmj.290.6483.1692 (1985).
Seidell, J. C., Cigolini, M., Charzewska, J., Ellsinger, B. M. & di Biase, G. Fat distribution in European women: a comparison of anthropometric measurements in relation to cardiovascular risk factors. Int J Epidemiol 19, doi: 10.1093/ije/19.2.303 (1990).
Ashwell, M. & Gibson, S. A proposal for a primary screening tool: ‘Keep your waist circumference to less than half your height’. BMC Medicine 12, 1–6, doi: 10.1186/s12916-014-0207-1 (2014).
Han, T. S., van Leer, E. M., Seidell, J. C. & Lean, M. E. J. Waist circumference action levels in the identification of cardiovascular risk factors: prevalence study in a random sample BMJ 311, 1401–1405 (1995).
Janssen, I., Katzmarzyk, P. T. & Ross, R. Waist circumference and not body mass index explains obesity-related health risk. Am J Clin Nutr 79, 379–384 (2004).
World Health Organization. Waist Circumference and Waist-Hip Ratio: Report of a WHO Expert Consultation Geneva (2008).
Lin, W. Y. et al. Optimal cut-off values for obesity: using simple anthropometric indices to predict cardiovascular risk factors in Taiwan. Int J Obes 26, 1232 (2002).
Bao, Y. et al. Optimal waist circumference cutoffs for abdominal obesity in Chinese. Atherosclerosis 201, 378–384, doi: 10.1016/j.atherosclerosis.2008.03.001 (2008).
World Health Organization. Physical status: the use and interpretation of anthropometry: report of a WHO Expert Committee. Geneva (1995).
National Institutes of Health. The practical guide: identification, evaluation, and treatment of overweight and obesity in adults. Bethesda. NIH publication no. 00–4084 (2000).
The Examination Committee of Criteria for ‘Obesity Disease’ in Japan. Japan Society for the Study of Obesity: New Criteria for ‘Obesity Disease’ in Japan. Circulation 66, 987–992 (2002).
Kagawa, M., Byrne, N. M. & Hills, A. P. Comparison of body fat estimation using waist: height ratio using different ‘waist’measurements in Australian adults. Br J Nutr 100, 1135–1141 (2008).
Matsushita, Y., Tomita, K., Yokoyama, T. & Mizoue, T. Relations Between Waist Circumference at Four Sites and Metabolic Risk Factors. Obesity 18, 2374–2378, doi: 10.1038/oby.2010.33 (2010).
Wang, Z., Ma, J. & Si, D. Optimal cut-off values and population means of waist circumference in different populations. Nutr Res Rev 23, 191–199 (2010).
Ashwell, M., Cole, T. J. & Dixon, A. K. Ratio of waist circumference to height is strong predictor of intra-abdominal fat. BMJ 313, 559–560, doi: 10.1136/bmj.313.7056.559d (1996).
Cai, L., Liu, A., Zhang, Y. & Wang, P. Waist-to-height ratio and cardiovascular risk factors among Chinese adults in Beijing. PLoS One 8, doi: 10.1371/journal.pone.0069298 (2013).
Graves, L. et al. Waist-to-height ratio and cardiometabolic risk factors in adolescence: findings from a prospective birth cohort. Pediatr Obes 9, doi: 10.1111/j.2047-6310.2013.00192.x (2014).
Park, Y. S. & Kim, J. S. Association between waist-to-height ratio and metabolic risk factors in Korean adults with normal body mass index and waist circumference. Tohoku J Exp Med 228, doi: 10.1620/tjem.228.1 (2012).
Thaikruea, L. & Yavichai, S. Proposed Waist Circumference Measurement for Waist-to-Height Ratio as a Cardiovascular Disease Risk Indicator: Self-Assessment Feasibility. J J of Obesity 1, 012 (2015).
Ashwell, M., Mayhew, L., Richardson, J. & Rickayzen, B. Waist-to-height ratio is more accurate than body mass index to quantify reduced life expectancy. Obes Facts 6 (2013).
Ashwell, M., Mayhew, L., Richardson, J. & Rickayzen, B. Waist-to-height ratio is more predictive of years of life lost than body mass index. PLoS One 9, doi: 10.1371/journal.pone.0103483 (2014).
Browning, L. M., Hsieh, S. D. & Ashwell, M. A systematic review of waist-to-height ratio as a screening tool for the prediction of cardiovascular disease and diabetes: 0.5 could be a suitable global boundary value. Nutr Res Rev 23, doi: 10.1017/s0954422410000144 (2010).
Sahakyan, K. R. et al. Normal-Weight Central Obesity: Implications for Total and Cardiovascular MortalityMortality Risk in Persons With Normal-Weight Central Obesity. Ann of Intern Med 163, 827–835, doi: 10.7326/M14-2525 (2015).
Coutinho, T. et al. Combining body mass index with measures of central obesity in the assessment of mortality in subjects with coronary disease: role of “normal weight central obesity”. J Am Coll Cardiol 61, 553–560 (2013).
Wormser, D. et al. Emerging Risk Factors Collaboration: Separate and combined associations of body-mass index and abdominal adiposity with cardiovascular disease: collaborative analysis of 58 prospective studies. Lancet 377, 1085–1095, doi: 10.1016/S0140-6736(11)60105-0 (2011).
Jensen, M. D. et al. American College of Cardiology/American Heart Association Task Force on Practice Guidelines: 2013 AHA/ACC/TOS Guideline for the Management of Overweight and Obesity in AdultsA Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Journal of the American College of Cardiology 63, doi: 10.1016/j.jacc.2013.11.004 (2014).
Ashwell, M. Plea for simplicity: use of waist-to-height ratio as a primary screening tool to assess cardiometabolic risk. Clin Obesity 2, doi: 10.1111/j.1758-8111.2012.00037.x (2012).
Hou, X. et al. Impact of waist circumference and body mass index on risk of cardiometabolic disorder and cardiovascular disease in Chinese adults: a national diabetes and metabolic disorders survey. PLoS One 8, e57319 (2013).
Klein, S. et al. Waist Circumference and Cardiometabolic Risk: A Consensus Statement from Shaping America’s Health: Association for Weight Management and Obesity Prevention; NAASO, The Obesity Society; the American Society for Nutrition; and the American Diabetes Association. Obesity 15, 1061–1067, doi: 10.1038/oby.2007.632 (2007).
Ashwell, M. & Gibson, S. Waist-to-height ratio as an indicator of ‘early health risk’: simpler and more predictive than using a ‘matrix’ based on BMI and waist circumference. BMJ Open 6, doi: 10.1136/bmjopen-2015-010159 (2016).
Savva, S. C., Lamnisos, D. & Kafatos, A. G. Predicting cardiometabolic risk: waist-to-height ratio or BMI. A meta-analysis. Diabetes Metab Syndr Obes 6, 403–419, doi: 10.2147/DMSO.S34220 (2013).
Ashwell, M., Gunn, P. & Gibson, S. Waist-to-height ratio is a better screening tool than waist circumference and BMI for adult cardiometabolic risk factors: systematic review and meta-analysis. Obesity Reviews 13, 275–286, doi: 10.1111/j.1467-789X.2011.00952.x (2012).
Lam, B. C. C., Koh, G. C. H., Chen, C., Wong, M. T. K. & Fallows, S. J. Comparison of Body Mass Index (BMI), Body Adiposity Index (BAI), Waist Circumference (WC), Waist-To-Hip Ratio (WHR) and Waist-To-Height Ratio (WHtR) as Predictors of Cardiovascular Disease Risk Factors in an Adult Population in Singapore. PLoS ONE 10, e0122985, doi: 10.1371/journal.pone.0122985 (2015).
Chobanian, A. V. et al. Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 42, 1206–1252 (2003).
American Diabetes Association. Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 34, S62–S69 (2011).
McPherson, R., Frohlich, J., Fodor, G. & Genest, J. S. Canadian Cardiovascular Society position statement–recommendations for the diagnosis and treatment of dyslipidemia and prevention of cardiovascular disease. Can J Cardiol 22, 913–927 (2006).
Acknowledgements
We would like to express our thankfulness to the Faculty of Medicine for supporting us in the conduct of this study and also the health personnel for participating in the study. Funding for the fieldwork was provided by the Faculty of Medicine Research Fund, Chiang Mai University.
Author information
Authors and Affiliations
Contributions
L.T. designed a study, analyzed data, and wrote the main manuscript text. J.T. collected data and wrote the main manuscript text. All authors reviewed the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Thaikruea, L., Thammasarot, J. Prevalence of normal weight central obesity among Thai healthcare providers and their association with CVD risk: a cross-sectional study. Sci Rep 6, 37100 (2016). https://doi.org/10.1038/srep37100
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep37100
This article is cited by
-
Combined consideration of body mass index and waist circumference identifies obesity patterns associated with risk of stroke in a Chinese prospective cohort study
BMC Public Health (2022)
-
Cross-sectional study of associations between normal body weight with central obesity and hyperuricemia in Japan
BMC Endocrine Disorders (2020)
-
Abdominal obesity increases metabolic risk factors in non-obese adults: a Hungarian cross-sectional study
BMC Public Health (2019)
-
Associations between normal weight central obesity and cardiovascular disease risk factors in Japanese middle-aged adults: a cross-sectional study
Journal of Health, Population and Nutrition (2019)
-
Temporal trends in normal weight central obesity and its associations with cardiometabolic risk among Chinese adults
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.