Abstract
Osteosarcoma, the most common primary malignant bone tumor, usually arises in the metaphysis of long bones. Amplification and mutation of the epidermal growth factor receptor (EGFR) gene represent signature genetic abnormalities encountered in osteosarcoma. Noscapine is a benzylisoquinoline alkaloid derived from the opium poppy Papaver somniferum. Recently several studies have suggested its anti-cancer effect in melanoma, ovarian cancer, gliomas, breast cancer, lung cancer, and colon cancer. However, the underlying molecular mechanism for its anti-cancer effect still remains unclear. In this paper, we found the mechanism of noscapine effectively suppressed proliferation and invasion of MG63 cell line by inhibiting the phosphorylation of EGFR and its downstream pathway.
Similar content being viewed by others
Introduction
Osteosarcoma is the most common form of primary malignant bone tumor found in children1,2. Patients without clinical signs of systematic spread show 5-year survival rates of 60–80%3, whereas patients with metastasis at diagnosis exhibit 5-year survival rates of 20–30%4. Rosen proposed the current therapeutic sequence for high-grade osteosarcoma and it is now internationally accepted5,6. Since then, the prognosis of patients has more or less stagnated and no significant therapy improvements have been achieved7. In the last 10 years, better knowledge of oncogenic processes in osteosarcoma has led to the development of new therapeutic approaches based on single new drugs or administered in combination with conventional chemotherapy8. As such, vigorous efforts are ongoing to either improve current therapy or to identify and strike new molecular targets for osteosarcom therapy9. A number of genes and pathways have emerged as attractive therapeutic targets for osteosarcom, such as PI3K/mTOR, c-Src and VEGF10.
Noscapine (Fig. 1A) has been widely studied for its no analgesia, sedation and respiratory depression as an antitussive. Since its structure has certain similarities with colchicine, in its anti-tumor activity screening process found to have some anti-tumor activity through inhibiting tubulin. As a natural anti-cancer agent, noscapine was recently reported to exhibit activity against a variety of cancers through a poorly understood mechanism11.
Noscapine inhibits the growth and the invasion of MG63 and U2OS (A) The structure of noscapine. (B) Protein level of EGFR in tissues was detected by western blot. (C) MRNA level of EGFR in tissues was detected by RT-PCR. *P < 0.05 vs. normal group, **P < 0.01 vs. normal group. (D) MG63cells were cultured with indicated concentrations of noscapine for indicated hours in 96-well plates, then MTT assay was performed, results represent the mean ± SD of three experiments done in triplicate. (E) MG63cells were pre-incubated with DMSO or noscapine for 24 h, then cells were analyzed using a FACS vantage flow cytometer with the Cell Quest acquisition and analysis software program (Becton Dickinson and Co., San Jose, CA), the experiment was repeated three times. (F) MG63cells were pre-incubated with noscapine for 24 h then cells were treated with ANNEXIN-V-FITC apoptosis detection kit and analyzed with FCAS. The experiment was repeated for three independent times. (G,H) MG63cells were pre-incubated with noscapine for 24 h; transwell assay without matrigel was performed. Cells were counted and results represent the mean ± SD of three experiments. *P < 0.05 vs. DMSO treated group, **P < 0.01 vs. DMSO treated group. (I,J) MG63cells were pre-incubated with noscapine for 24 h; transwell assay with matrigel was performed. Cells were counted and results represent the mean ± SD of three experiments. *P < 0.05 vs. DMSO treated group, **P < 0.01 vs. DMSO treated group.
The amplification of the epidermal growth factor receptor (EGFR) is one of the most common genetic aberration associated with malignant osteosarcoma12. EGFR is a cell membrane receptor with intrinsic protein tyrosine kinase activity that has been the subject of rigorous investigation in view of its involvement in several human cancers and its potential as a target of therapy13. Phase I clinical trials of EGFR tyrosine kinase inhibitors, such as gefitinib, have included patients with osteosarcoma13. EGFR has been shown to be important for cell proliferation and migration as well as in tumor progression14. The raise of EGFRp-Tyr1068 increased the levels of Cyclin D1 expression and promoted cell proliferation15. Inhibition of EGFR/Akt pathway could induce cell apoptosis. MMP2, as the downstream molecule of MEK-1/ERK1/2 pathway, is regulated by EGFR and plays important role in tumor invasion16.
Here we report that noscapine could effectively suppress the proliferation and invasion of MG63 cells, promote its early apoptosis by inhibiting the phosphorylation of EGFR.
Materials and Methods
Patients and tissue samples
15 matched osteosarcoma cancer and corresponding normal tissues were obtained from patients undergoing resection of tumor in the Shengjing Hospital of China Medical University. All patients had a clear histologic diagnosis of osteosarcoma cancer based on the AJCC. All cases were diagnosed with osteosarcoma cancer and treated between January 2010 and December 2010 at the Shengjing Hospital of China Medical University. The study protocol was approved by Medical Ethics and Human Clinical Trial Committee. All the tissues were immediately frozen in liquid nitrogen after surgery for research. We confirm that all methods were performed in accordance with the relevant guidelines and regulations. We confirm that informed consent was obtained from all subjects.
Cell culture
Osteosarcoma cell lines MG63 and U2OS were obtained from American Type Culture Collection (Manassas, VA, USA). Cells were cultured in DMEM (Invitrogen, Carlsbad, CA, USA) containing 10% fetal calf serum (Invitrogen, Carlsbad, CA, USA). Cells were cultured at 37 °C with humidified atmosphere of 5% CO2.
MTT assays
Cells were plated in 96-well plates (1 × 104/well). 24 hours later, the medium was replaced with 100 ul medium containing different concentrations of noscapine and cultured for 0, 12, 24, 36 and 48 h. 20 μl of 5 mg/ml MTT solution was added to well. After incubation for 4 hours, the medium was removed and remaining MTT formazan was dissolved in 150 μl of DMSO. Solution was measured at 490 nm using a Microplate Reader (BIO-RAD).
Cell-cycle analysis by flow cytometry
After incubation with different concentrations of noscapine, MG63 cells were washed using cold PBS and suspended in staining buffer with 10 ug/ml propidium iodide. The cells were analyzed using BD FACS Vantage flow cytometer (Becton Dickinson) and analyzed using CellQuest software program.
Cell migration and invasion assay
Matrigel cell invasion assay was performed using a 24-well transwell chamber (8-μm pore size) (Corning). The transwell chambers were coated with 20 μl matrigel (1:4, BD Bioscience). Transfected cells were trypsinized and suspended in 100 μl of DMEM medium without serum, which was transferred to the upper chamber. 600 μl culture medium with 10% FBS was added to the lower chamber. After 18 hours incubation, the non-invaded cells on the upper membrane surface were removed using cotton swab and the cells that passed through the filter were fixed and stained with hematoxylin. The numbers of cells that pass through the membrane were counted in using microscope. This experiment was performed in triplicate.
Cell apoptosis
Apoptosis was examined using Annexin-V-PI apoptosis detection kit. MG63 cells are washed with cold PBS and suspended using binding buffer. 5 μl of Annexin-V-FITC and 10 μl of PI were added. Cells were incubated in the dark for 15 minutes. 400 μl of binding buffer was added and the apoptosis rate was examined using BD FACS Vantage flow cytometer (Becton Dickinson).
Reverse transcription and quantitative real-time PCR
Quantitative real-time PCR was performed using SYBR Green PCR master mix (TAKARA) in a total volume of 20 μl on Mx 3000 P Real-Time PCR System as follows: 95 °C for 30 seconds, 50 cycles of 95 °C for 10 seconds, 60 °C for 30 seconds. A dissociation step was performed to generate a melting curve to confirm the specificity of the amplification. β-actin was used as the reference gene. The relative levels of gene expression were calculated by the 2−ΔΔCt method. Primer sequences were synthesized as the Table 1.
Transfection of siRNA
Cells were transfected using pRS-siEGFR (Shanghai GeneChem Company) and then selected with puromycin (1.5 μg/mL) for 2 weeks. The cells transfected with pRS-si-NC (negative control) and cells without treatment were used as the control.
Western blot analyses
Whole cell extracts were prepared using cell lysis buffer and about 60 μg of protein was separated using 10% SDS-polyacrylamide gels. After electrophoresis, the proteins were eletrotransferred to nitrocellulose filters and membranes was blocked using 5% nonfat dry milk in TBST for 2 hours. The proteins were probed with specific antibodies—CyclinD1, CDK4, CDK6, MMP2, Flag (Bioworld), EGFR, phospho-EGFR(Tyr1068), Akt, phospho-Akt(Ser473) (Santa Cruz), Caspase3, Bax and Bcl-2 (Neomarker). To assaure equal loading, gels were stripped and reprobed with antibodies against β-actin GAPDH (Kangchen Bio-tech Inc., Shanghai, China). All PVDF membranes were detected by chemiluminescence (ECL, Pierce Technology).
Kinase Glo Luminescent assay
Indicated concentration of noscapine and 1 μL of HER1/2/3/4 kinases (Invitrogen) were mixed and filled with kinase buffer (50 mmol/L HEPES, pH 7.5, 10 mmol/L MgCl2, 2 mmol/L MnCl2 and 0.2 mmol/L DTT) to 20 μL. Incubated the mixture at 37 °C for 3 h then mixed with 20 μL Kinase Glo Luminescent (Promega) reaction solution, taking black 384-fluorescence values measured after standing 10 min.
Immunoprecipitation and Kinase Glo Luminescent assay
MG63cells were transfected with Flag-EGFR-WT (wild type) or Flag-EGFR-KM (T1068A)(the kinase mutant of Tyr to Ala) after 24 h cells were washed with ice-cold PBS and suspended in cold lysis buffer supplemented with protease and phosphatase inhibitors as described. Supernatants were preadsorbed with anti-Flag M2 magnetic beads (Sigma-aldrich) for 3 h at 4 °C. Then the beads were mixed and filled with kinase buffer (50 mmol/L HEPES, pH 7.5, 10 mmol/l MgCl2, 2 mmol/lMnCl2 and 0.2 mmol/l DTT) to 20 μl. Incubated the mixture at 37 °C for 3 h then mixed with 20 μl Kinase Glo Luminescent (Promega) reaction solution, taking black 384-fluorescence values measured after standing 10 min.
Tumor xenografts in nude mice
The procedures were approved by institutional animal research ethics committee with reference to the Chinese Community guidelines for the use of experimental animals (No. 201309). We confirm that all methods were performed in accordance with the relevant guidelines and regulations. Six-week-old male Balb/c nude mice were purchased from the Laboratory Animal center of Liaoning Province, China. All the animals were given free access to sterilized food and water. 1 × 107 MG63 cell were suspended in 200 μl of PBS and subcutaneously injected into animal. The mice were assigned into control and treatment groups and anesthetized with injection of 75 mg/kg ketamine and 10 mg/kg xylazine17. The mice were treated with intravenous injection of noscapine (5 mg/kg) or DMSO once daily (days 0–16). Tumors became palpable 3 days after xenografting. The mice were monitored for 16 d after tumor inoculation. Body weight and Mortality were recorded during experimental period.
Results
Noscapine inhibits the growth and the invasion of MG63 and U2OS cells
Through the detection of protein and RNA levels, we found that the EGFR in osteosarcoma tissue was higher than that in adjacent tissues (Fig. 1B,C). The inhibitory effects on growth of noscapine were detected in MG63 and U2OS cells. As shown in MTT assay, noscapine inhibited the proliferation of MG63 and U2OS cells in a concentration dependent manner (Figs 1D and 6B). To further study the mechanisms of noscapine inhibiting the growth of osteosarcoma cells, MG63 cells were exposed to the indicated concentrations of noscapine for 24 h, and then cell cycle analysis was performed. Noscapine prominently induced a dose-dependent increase in the percentage of cells in G1 phase and a decrease in S phase compared with the control (Fig. 1E), indicating that noscapine arrest MG63 cells at the G1 phase of the cell cycle. To test whether noscapine could induce apoptosis of MG63cells, we detected the apoptosis rate by Annexin-V-FITC. By Annexin-V-FITC staining, the noscapine-induced MG63 cell apoptosis was increased with the increased concentration (Fig. 1F). Inhibitory effect of noscapine on migration and invasion of MG63cell was analyzed by transwell assay (with or without matrigel). Results showed that noscapine significantly decreased invasion and migration potential of osteosarcoma cells MG63 and U2OS(Figs 1G–J and 6E,F) in a dose-dependent manner. The above results showed that noscapine can inhibit the growth and the invasion of MG63 cells in a concentration dependent manner.
Noscapine suppresses the kinase acivity of EGFR by inhibiting EGFRp-Tyr1068 in MG63 and U2OS cells
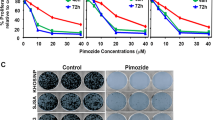
Because of the important role of EGFR phosphorylation in the signal pathway, we wonder whether noscapine could inhibit the phosphorylation level of EGFR and suppress the activation of EGFR in MG63cells and U2OS cells. By western blot analysis, we found that treatment of noscapine could markedly inhibit the level of EGFRp-Tyr1068 but without affected the total expression of EGFR (Figs 2A and 6A). To further detect the selective inhibition profile of noscapine, we chose four types of kinase- EGFR/ErbB1/HER1, ErbB2/HER2/neu, ErbB3/HER3 and ErbB4/HER4; all of them are belong to the epidermal growth factor receptor family, which share a certain homology, to test the inhibition effect of noscapine on their kinase activation. By Kinase-Glo® Luminescent Kinase Assays (Promega) which is a homogeneous non-radioactive methodin vitro, we got the kinase inhibition rate of noscapine (Fig. 2B). The results showed that noscapine markedly inhibited EGFR kinase activity in a dose-dependent manner, but had relatively weak effect on the other three kinases, there were statistically significant difference between EGFR and the other three kinases at different concentration of noscapine (Fig. 2B). Then the inhibitory effect of noscapine on EGFR kinase was also tested by the assay. Data showed that noscapine inhibited EGFR activity with an IC50 value of 19.26 μmol/l (Fig. 2C).
Noscapine inhibits the kinase acivity of EGFR by inhibiting EGFRp-Tyr1068 (A) MG63cells were treated with DMSO alone or indicated concentration of noscapine for 24 h, proteins were extracted and subjected to western blot analysis, the membrane was probed sequentially with EGFR and EGFRp-Tyr1068 antibody. (B) HER1/2/3/4 kinases were pre-incubated with the indicated concentrations of noscapine for 1 hour respectively, then Kinase Glo assay were performed. Data are shown as mean ± SD. *P < 0.05 vs. 10 μmol treated EGFR group; **P < 0.01 vs. 10 μmol treated EGFR group; #P < 0.05 vs. 20 μmol treated EGFR group; ##P < 0.01 vs. 20 μmol treated EGFR group; $P < 0.05 vs. 30 μmol treated EGFR group; $$P < 0.01 vs. 30 μmol treated EGFR group.(C) EGFR kinase were pre-incubated with the indicated concentrations of noscapine for 1 hour respectively, then Kinase Glo assay were performed and inhibition rate were calculated, linear fit curve was drawn with an equation of y = 0.02505x + 0.01751 R2 = 0.8715. (D) Flag-EGFR-KM and Flag-EGFR-WT proteins were pre-incubated with the indicated concentrations of noscapine for 1 hour respectively, then Kinase Glo assay were performed. Data are shown as mean ± SD. *P < 0.05 vs. DMSO treated Flag-EGFR-WT group; **P < 0.01 vs. DMSO treated Flag-EGFR-WT group; #P < 0.05, ##P < 0.01 vs. DMSO treated Flag-EGFR-KM group; $P < 0.05, $$P < 0.01 vs. Flag-EGFR-WT group treated Flag-EGFR-KM group; (E) MG63cells expressing Flag-vector, Flag-EGFR-KM or Flag-EGFR-WT and then treated with or without noscapine were detected with indicated antibody by western blot. (F) MG63cells transfected with si-EGFR or si-NC (negative control) and those cells were treated with or without noscapine were detected with indicated antibody by western blot.
To further verify the specific targeting of noscapine on EGFR, we performed two group experiments. Firstly, MG63 cells were transfected with Flag-vector, Flag-EGFR-WT (wild type) and Flag-EGFR-KM respectively and treated with the indicated noscapine for 24 h, the kinase inhibition rate of noscapine between EGFR-WT and EGFR-KM were compared by Kinase-Glo® Luminescent Kinase Assays. The results showed that noscapine markedly inhibited EGFR-WT kinase activity in a dose-dependent manner, but had relatively weak effect on EGFR-KM (Fig. 2D). Then the indicated proteins level was tested by western blot analysis (Fig. 2E). As the results showed, in the DMSO treated control group, the level of EGFRp-Tyr1068 in cells expressed Flag-EGFR-KM was significantly less than that in the cells expressed Flag-EGFR-WT. In the noscapine treated group, in both cells expressed Flag-EGFR-WT and Flag-EGFR-KM, the level of EGFRp-Tyr1068 dramatically decreased compared with the DMSO treated control group, but the total EGFR level were not changed(Fig. 2E).
In another set of experiments, the MG63/si-NC (negtive control) stable cell line and MG63/si-EGFR stable cell line were treated with or without noscapine, the level of EGFRp-Tyr1068 and total EGFR were tested by western blot analysis (Fig. 2F). The data showed that the phosphorylation degree of EGFRp-Tyr1068 significantly reduced after noscapine treatment in MG63/si-NC stable cell lines but not changed significantly in MG63/si-EGFR stable cell line compared with the DMSO control group.
The above results indicated that noscapine suppressed the kinase acivity of EGFR, at least partly by inhibiting the phosphorylation of EGFRp-Tyr1068 in MG63 cells.
Noscapine inhibits the growth of MG63 and U2OS by inhibiting EGFR/Akt/CDKs and EGFR/Akt/Bad pathway
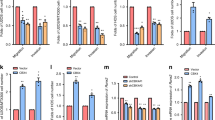
Since Cyclin D1, CDK4 and CDK6 are key regulators in the G1 phase of the cell cycle, here we examined the indicated regulators expression level in noscapine-treated cells. Western blot analysis showed that exposure of MG63 and U2OS to 10/20/30 μmol/l noscapine for 24 h dramatically decreased the expression of Akt, Aktp-Ser473, Cyclin D1, CDK4 and CDK6 (Figs 3A and 6C), indicating noscapine arrests cells at G1 phase and then suppresses cells growth via down-regulated Aktp-Ser473, Cyclin D1, CDK4 and CDK6. Furthermore, real time RT-PCR showed that expression of Cyclin D1, CDK4 and CDK6 in MG63 were down-regulated at mRNA level after exposure to noscapine (Fig. 3B). Furthermore the expressions of apoptosis regulators were also examined by western blot. The expression of Bcl-2 was obviously decreased and the levels of Caspase3 and Bax were increased in noscapine treated MG63 and U2OS cells (Figs 3D and 6D). Then real time RT-PCR results verified that changes of these factors were coincidence with protein levels (Fig. 3C).
Noscapine represses the growth of MG63cells by inhibiting EGFR/Akt/CDKs and EGFR/Akt/Bad pathways (A) MG63cells were treated with DMSO alone or indicated concentration of noscapine for 24 h, the protein expression of Cyclin D1, CDK4, CDK6, EGFR, EGFRp-Tyr1068, Akt, and Aktp-Ser473 were detected by western blot. (B) MG63cells were treated with DMSO alone or noscapine for 24 h, then cells were harvested, and the mRNA expression of Cyclin D1, CDK4 and CDK6 were detected by real-time RT-PCR; results represent the mean ± SD of three experiments done in triplicate. *P < 0.05 vs. DMSO treated group, **P < 0.01 vs. DMSO treated group. (C) MG63cells were treated with DMSO alone or indicated concentration of noscapine for 24 h, cells were harvested, and the mRNA expression of Caspase3, Bax and Bcl-2 were detected by real-time RT-PCR, results represent the mean ± SD of three experiments done triplicate. *P < 0.05 vs. DMSO treated group, **P < 0.01 vs. DMSO treated group. (D) MG63cells were treated with DMSO alone or indicated concentration of noscapine for 24 h, the protein expression of Caspase3, Bax, Bcl-2, EGFR, EGFRp-Tyr1068 Akt, and Aktp-Ser473 were detected by western blot. (E) MG63 cells expressing Flag-VECTOR, Flag-EGFR-KM or Flag-EGFR-WT were incubated with 20 μmol/l of noscapine, MTT assay was performed after indicated hours and results represent the mean ± SD of three experiments done in triplicate. **P < 0.01 vs. Flag-Akt-KM/Flag-Akt-WT. (F) MG63 cells transfected with si-EGFR or si-NC (negative control) were treated with 20 μmol/l of noscapine, MTT assay was performed after indicated hours and results represent the mean ± SD of three experiments done in triplicate. *P < 0.05 vs. si-EGFR/si-NC (negative control). (G) MG63cells expressing Flag-vector, Flag-EGFR-KM or Flag-EGFR-WT and then treated with or without noscapine were detected with Cyclin D1, CDK4, CDK6, EGFR, EGFRp-Tyr1068, Akt and Aktp-Ser473 antibody by western blot. (H) MG63cells expressing Flag-vector, Flag-EGFR-KM or Flag-EGFR-WT and then treated with or without noscapine were detected with Caspase3, Bax, Bcl-2, EGFR, EGFRp-Tyr1068, Akt and Aktp-Ser473 antibody by western blot.
To further confirm the involvement of EGFR in noscapine -induced MG63 cells growth arrest, cells respectively expressed Flag-EGFR-WT and Flag-EGFR-KM plasmids were treated with 20 μmol/l noscapine for 24 h. Then cell proliferation was analyzed by MTT assay. Results showed that the proliferation of cells expressed EGFR-WT was dramatically inhibited by noscapine compared with cells transfected with EGFR-KM plasmid, but there was no significant difference in the inhibition rate between EGFR-KM expressed cells and cells transfected with vector cells (Fig. 3E). Then, the same experiments were performed in MG63/si-NC (negtive control) cell line and MG63/si-EGFR cell line. Results showed that, there was significantly difference in the proliferation inhibition rate between MG63/si-NC and MG63/si-EGFR cell lines (Fig. 3F). While, western blot analysis showed that under the effect of noscapine, when the Aktp-Ser473 was over-expression EGFRp-Tyr1068, Cyclin D1, CDK4, CDK6, Bcl-2, Caspase3 and Bax changed more significantly (Fig. 3G,H).
Noscapine represses the migratory and invasive potential of MG63 by inhibiting EGFR/Akt/MMP2 pathway
To further investigate the mechanisms of noscapine migratory of osteosarcoma cells, MG63 and U2OS cells were exposed to various concentrations of noscapine for 24 h. Western blot analysis showed that levels of MMP2 dramatically decreased (Figs 4A and 6G). Real time RT-PCR showed that expression of MMP2 in MG63 was down-regulated at mRNA level after exposure to noscapine (Fig. 4B). The migration capacity was detected in EGFR-WT, EGFR-KM (kinase mutation EGFR) and MG63/si-EGFR cell lines with or without noscapine. And results suggested that EGFR is the target of noscapine (Fig. 4C,D). Western blot analysis showed that under the effect of noscapine, when the EGFR was over-expression EGFRp-Tyr1068 and MMP2 decreased more significantly (Fig. 4E).
Noscapine represses the migratory and invasive potential of MG63cells by inhibiting EGFR/Akt/MMP2 pathway (A) MG63cells were treated with DMSO alone or indicated concentration of noscapine for 24 h, the protein expression of EGFR, EGFRp-Tyr1068, Akt, Aktp-Ser473 and MMP2 were detected by western blot. (B) MG63cells were treated with DMSO alone or indicated concentrations of noscapine for 24 h, cells were harvested, and the mRNA expression of MMP2 was detected by real-time RT-PCR, results represent the mean ± SD of three experiments done in triplicate. *P < 0.05 vs. DMSO treated group; **P < 0.01 vs. DMSO treated group. (C,D) MG63 cells expressing Flag-vector, Flag-EGFR-KM or Flag-EGFR-WT and then treated with or without noscapine were detected by transwell without matrigel assay. The experiment was repeated for three independent times. (E) MG63cells expressing Flag-vector, Flag-EGFR-KM or Flag-EGFR-WT and then treated with or without noscapine were detected with EGFR, EGFRp-Tyr1068, Akt, Aktp-Ser473 and MMP2 antibody by western blot.
The anti-tumorigenic effect of noscapine in vivo
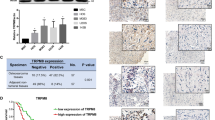
The anti-tumorigenic effect of noscapine on MG63 cells was further illustrated in vivo in a nude mouse xenogfraft. On the day of sacrifice (day 16), fangchinoline treatments at the given doses resulted in about 41.23% tumor suppression (Fig. 5A,B). Then the protein levels of EGFR and its pathways were detected by western blot (Fig. 5C). The above results suggested that noscapine inhibits the migratory and invasive of MG63 cells by inhibiting EGFR pathway. These results indicated that noscapine effectively suppressed proliferation and invasion of MG63 cells by inhibiting EGFRp-Tyr1068 (Fig. 5D).
(A) Photographic illustration of tumors from control and noscapine -treated nude mice on the day of sacrifice (day 16). (B) The tumor weights of them were showed in the graph. (C) The protein expression of Cyclin D1, CDK4, CDK6, Caspase 3, Bax, Bcl-2, MMP2, EGFR, EGFRp-Tyr1068, Akt, and Aktp-Ser473 were detected by western blot. (D) The ideograph showed that noscapine effectively suppressed proliferation and invasion of MG63 cells by inhibiting EGFR, then inhibiting EGFR pathway.
(A) The protein expression of EGFR, EGFRp-Tyr1068, Akt, and Aktp-Ser473 in U2OS cells were detected by western blot. (B) MG63cells were cultured with indicated concentrations of noscapine for indicated hours in 96-well plates, then MTT assay was performed, results represent the mean ± SD of three experiments done in triplicate. (C,D) The protein expression of Cyclin D1, CDK4, CDK6, Caspase 3, Bax and Bcl-2 in U2OS cells were detected by western blot. (E) U2OS cells were pre-incubated with noscapine for 24 h; transwell assay without matrigel was performed. Cells were counted and results represent the mean ± SD of three experiments. *P < 0.05 vs. DMSO treated group, **P < 0.01 vs. DMSO treated group. (F) U2OS cells were pre-incubated with noscapine for 24 h; transwell assay with matrigel was performed. Cells were counted and results represent the mean ± SD of three experiments. *P < 0.05 vs. DMSO treated group, **P < 0.01 vs. DMSO treated group. (G) The protein expression of MMP2 in U2OS cells were detected by western blot.
Discussion
In cancer cells, EGFR aberrations impact a variety of cell signaling pathways, notably the PI3K-AKT and JAK/STAT pathways18. In osteosarcoma, in vitro data from early passage osteosarcoma cells demonstrate constitutive EGFR phosphorylation whose abrogation leads to growth inhibition19. Overexpression of EGFR has been shown to promote cancer cell motility and invasion. In vitro data indicate that EGFR and Akt signaling play a role in the pathogenesis of osteosarcoma20.
Noscapine was shown to have potent antitumor activity against murine lymphoid tumors21. Since then, noscapine has been shown to exhibit activity against a wide variety of tumors in vitro and in vivo22,23,24,25. There are findings suggest that noscapine can promote apoptosis by suppressing Bcl-226. Besides antiapoptotic proteins, noscapine also downregulates the expression of proteins linked to cell proliferation, inflammation, invasion, adhesion, and angiogenesis. These observations imply that noscapine has anti-inflammatory, antiangiogenic, and antimetastatic activities27. At the same time in hypoxic human glioma cells, noscapine has been shown to inhibit the secretion of VEGF28,29.
In this study, MG63cells were used to detect the anti-cancer effect of noscapine. As shown in MTT assay and transwell assay, noscapine treatment inhibited the proliferation and migration of MG63cells in a concentration-dependent manner. We found that the phosphorylation of EGFR (Tyr1068) dramatically decreased with the increasing concentration of noscapine, which suggested noscapine suppressed the phosphorylation of EGFR and inhibited the proliferation and migration of MG63cells. We first found that noscapine did suppress the phosphprylation levels of EGFR, so it is reasonable to conclude that noscapine suppressed Cyclin D1 and CDK4/6 expression via suppression of EGFR pathway, and inhibited the transition of cells from G1 phase to S phase, and resulted in the anti-proliferative effect on MG63 cells together with the induction of apoptosis.
In addition to the effect on cell proliferation, we demonstrated the inhibition mechanism of noscapine on invasion of MG63 cells. One of the key steps in cancer invasion and metastasis is the degradation of extracellular matrix. MMP2 has been demonstrated to play important roles in the process30. Our results showed that noscapine significantly suppressed the invasive ability of MG63cells in parallel with down-regulation of MMP2 and inhibit EGFR pathway.
In summary, our data showed that noscapine could inhibit the malignant phenotype of MG63 cells by inhibit the phosphorylation of EGFR (Tyr1068) and further to suppress the EGFR associated signaling pathway, EGFR/Akt pathway. Also the anti-tumorigenic effect of noscapine on MG63 cells was illustrated in vivo. Although these results are warranted further testing, the present findings do support the conception that noscapine may offer a novel therapeutic strategy for advanced metastatic osteosarcoma.
Additional Information
How to cite this article: He, M. et al. Noscapine targets EGFRp-Tyr1068 to suppress the proliferation and invasion of MG63 cells. Sci. Rep. 6, 37062; doi: 10.1038/srep37062 (2016).
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Nikitin, B. M. [The pathogenesis of bone sarcomas in rats following administration of strontium 89 and the effect of strontium 89 on the progeny of these animals]. Biulleten’ eksperimental’noi biologii i meditsiny 49, 93–95 (1960).
Gobin, B. et al. Imatinib mesylate exerts anti-proliferative effects on osteosarcoma cells and inhibits the tumour growth in immunocompetent murine models. PloS One 9, e90795, doi: 10.1371/journal.pone.0090795 (2014).
Marina, N., Gebhardt, M., Teot, L. & Gorlick, R. Biology and therapeutic advances for pediatric osteosarcoma. The oncologist 9, 422–441 (2004).
Poos, K. et al. Structuring osteosarcoma knowledge: an osteosarcoma-gene association database based on literature mining and manual annotation. Database: the journal of biological databases and curation 2014, doi: 10.1093/database/bau042 (2014).
Huvos, A. G., Rosen, G. & Marcove, R. C. Primary osteogenic sarcoma: pathologic aspects in 20 patients after treatment with chemotherapy en bloc resection, and prosthetic bone replacement. Archives of pathology & laboratory medicine 101, 14–18 (1977).
Rosen, G., Murphy, M. L., Huvos, A. G., Gutierrez, M. & Marcove, R. C. Chemotherapy, en bloc resection, and prosthetic bone replacement in the treatment of osteogenic sarcoma. Cancer 37, 1–11 (1976).
Allison, D. C. et al. A meta-analysis of osteosarcoma outcomes in the modern medical era. Sarcoma 2012, 704872, doi: 10.1155/2012/704872 (2012).
Ando, K. et al. Current therapeutic strategies and novel approaches in osteosarcoma. Cancers 5, 591–616, doi: 10.3390/cancers5020591 (2013).
Ory, B., Moriceau, G., Redini, F. & Heymann, D. mTOR inhibitors (rapamycin and its derivatives) and nitrogen containing bisphosphonates: bi-functional compounds for the treatment of bone tumours. Current medicinal chemistry 14, 1381–1387 (2007).
Shor, A. C. et al. Dasatinib inhibits migration and invasion in diverse human sarcoma cell lines and induces apoptosis in bone sarcoma cells dependent on SRC kinase for survival. Cancer research 67, 2800–2808, doi: 10.1158/0008-5472.CAN-06-3469 (2007).
Manetti, F. et al. Identification of a novel pyrazolo[3,4-d]pyrimidine able to inhibit cell proliferation of a human osteogenic sarcoma in vitro and in a xenograft model in mice. Journal of medicinal chemistry 50, 5579–5588, doi: 10.1021/jm061449r (2007).
Kolb, E. A. et al. Initial testing of dasatinib by the pediatric preclinical testing program. Pediatric blood & cancer 50, 1198–1206, doi: 10.1002/pbc.21368 (2008).
Hassan, S. E. et al. Cell surface receptor expression patterns in osteosarcoma. Cancer 118, 740–749, doi: 10.1002/cncr.26339 (2012).
Ke, Y. et al. Noscapine inhibits tumor growth with little toxicity to normal tissues or inhibition of immune responses. Cancer immunology, immunotherapy: CII 49, 217–225 (2000).
Sung, B., Ahn, K. S. & Aggarwal, B. B. Noscapine, a benzylisoquinoline alkaloid, sensitizes leukemic cells to chemotherapeutic agents and cytokines by modulating the NF-kappaB signaling pathway. Cancer research 70, 3259–3268, doi: 10.1158/0008-5472.CAN-09-4230 (2010).
Vivanco, I. et al. The phosphatase and tensin homolog regulates epidermal growth factor receptor (EGFR) inhibitor response by targeting EGFR for degradation. Proceedings of the National Academy of Sciences of the United States of America 107, 6459–6464, doi: 10.1073/pnas.0911188107 (2010).
Wang, C. D. et al. Fangchinoline induced G1/S arrest by modulating expression of p27, PCNA, and cyclin D in human prostate carcinoma cancer PC3 cells and tumor xenograft. Bioscience, biotechnology, and biochemistry 74, 488–493, doi: 10.1271/bbb.90490 (2010).
Hynes, N. E. & Lane, H. A. ERBB receptors and cancer: the complexity of targeted inhibitors. Nature reviews. Cancer 5, 341–354, doi: 10.1038/nrc1609 (2005).
Daw, N. C. et al. Phase I and pharmacokinetic study of gefitinib in children with refractory solid tumors: a Children’s Oncology Group Study. Journal of clinical oncology: official journal of the American Society of Clinical Oncology 23, 6172–6180, doi: 10.1200/JCO.2005.11.429 (2005).
Freeman, B. B. 3rd, Daw, N. C., Geyer, J. R., Furman, W. L. & Stewart, C. F. Evaluation of gefitinib for treatment of refractory solid tumors and central nervous system malignancies in pediatric patients. Cancer investigation 24, 310–317, doi: 10.1080/07357900600632058 (2006).
Freeman, S. S. et al. Copy number gains in EGFR and copy number losses in PTEN are common events in osteosarcoma tumors. Cancer 113, 1453–1461, doi: 10.1002/cncr.23782 (2008).
Mueller, K. L., Powell, K., Madden, J. M., Eblen, S. T. & Boerner, J. L. EGFR Tyrosine 845 Phosphorylation-Dependent Proliferation and Transformation of Breast Cancer Cells Require Activation of p38 MAPK. Translational oncology 5, 327–334 (2012).
Pal, H. C. et al. Delphinidin reduces cell proliferation and induces apoptosis of non-small-cell lung cancer cells by targeting EGFR/VEGFR2 signaling pathways. PloS One 8, e77270, doi: 10.1371/journal.pone.0077270 (2013).
Morozevich, G. E., Kozlova, N. I., Ushakova, N. A., Preobrazhenskaya, M. E. & Berman, A. E. Integrin alpha5beta1 simultaneously controls EGFR-dependent proliferation and Akt-dependent pro-survival signaling in epidermoid carcinoma cells. Aging 4, 368–374 (2012).
Xiao, L. J. et al. ADAM17 targets MMP-2 and MMP-9 via EGFR-MEK-ERK pathway activation to promote prostate cancer cell invasion. International journal of oncology 40, 1714–1724, doi: 10.3892/ijo.2011.1320 (2012).
Baki, A., Bielik, A., Molnar, L., Szendrei, G. & Keseru, G. M. A high throughput luminescent assay for glycogen synthase kinase-3beta inhibitors. Assay and drug development technologies 5, 75–83, doi: 10.1089/adt.2006.029 (2007).
Hughes, D. P., Thomas, D. G., Giordano, T. J., Baker, L. H. & McDonagh, K. T. Cell surface expression of epidermal growth factor receptor and Her-2 with nuclear expression of Her-4 in primary osteosarcoma. Cancer research 64, 2047–2053 (2004).
Pedersen, M. W., Tkach, V., Pedersen, N., Berezin, V. & Poulsen, H. S. Expression of a naturally occurring constitutively active variant of the epidermal growth factor receptor in mouse fibroblasts increases motility. International journal of cancer. Journal international du cancer 108, 643–653, doi: 10.1002/ijc.11566 (2004).
Cai, X. M. et al. Protein phosphatase activity of PTEN inhibited the invasion of glioma cells with epidermal growth factor receptor mutation type III expression. International journal of cancer. Journal international du cancer 117, 905–912, doi: 10.1002/ijc.21251 (2005).
Fukaya, Y. et al. A role for PI3K-Akt signaling in pulmonary metastatic nodule formation of the osteosarcoma cell line, LM8. Oncology reports 14, 847–852 (2005).
Author information
Authors and Affiliations
Contributions
Ming He: conceived of the study, carried out the molecular studies. Linlin Jiang: carried out the molecular studies, helped to draft the manuscript. Zhaozhou Ren: participated in the design of the study and performed the statistical analysis. Guangbin Wang: participated in its design and coordination and helped to draft the manuscript. Jiashi Wang: conceived of the study.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
He, M., Jiang, L., Ren, Z. et al. Noscapine targets EGFRp-Tyr1068 to suppress the proliferation and invasion of MG63 cells. Sci Rep 6, 37062 (2016). https://doi.org/10.1038/srep37062
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep37062
This article is cited by
-
Establishment and characterization of the NCC-GCTB4-C1 cell line: a novel patient-derived cell line from giant cell tumor of bone
Human Cell (2022)
-
Noscapine, a Non-addictive Opioid and Microtubule-Inhibitor in Potential Treatment of Glioblastoma
Neurochemical Research (2019)
-
Enhanced thebaine and noscapine production and modulated gene expression of tyrosine/dopa decarboxylase and salutaridinol 7-O-acetyltransferase genes in induced autotetraploid seedlings of Papaver bracteatum Lindl
Acta Physiologiae Plantarum (2019)
-
The effect and mechanism of dopamine D1 receptors on the proliferation of osteosarcoma cells
Molecular and Cellular Biochemistry (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.