Abstract
Hepsin, a membrane-associated serine protease, is frequently upregulated in epithelial cancers and involved in cancer progression. Our study aims to describe the expression pattern and evaluate the clinical implication of hepsin in gastric cancer patients. The mRNA expression of hepsin was analyzed in 50 gastric cancer and matched non-tumor tissues, which was downregulated in 78% (39/50) of gastric cancer. By searching and analyzing four independent datasets from Oncomine, we obtained the similar results. Furthermore, we evaluated the hepsin expression by IHC in tissue microarray (TMA) containing 220 Gastric Cancer specimens. More importantly, Kaplan-Meier survival and Cox regression analyses were taken to access the prognosis of gastric cancer and predicted that hepsin protein expression was one of the significant and independent prognostic factors for overall survival of Gastric Cancer.
Similar content being viewed by others
Introduction
Gastric cancer, one of the most common malignant cancers in the world, is responsible for the second leading cause of cancer death in both sexes worldwide, although the incidence has decreased over past several decades1,2. And most patients diagnosed with gastric cancer at advanced stage have a low 5-year survival rate3. The crucial reason for the poor prognosis of the most malignant cancers including gastric cancer is invasion and metastasis4. Traditionally, the tumor-node-metastasis (TNM) classification of International Union Against Cancer is composed of tumor invasive depth, lymph node metastasis and distant metastasis. Because of the heterogeneity of the tumor, patients of gastric cancer in the same stage may have diverse outcomes5. To improve the life quality and survival rate of gastric cancer patients, some novel and effective therapeutic methods must be created and developed.
Serine proteases have been known to mediate many biological processes. Hepsin (also called TMPRSS1), a putative type II transmembrane serine protease (TTSPs) of 417 amino acid residues, was originally identified as a human liver cDNA clone6. Hepsin has the active site triad residues of His(H), Asp(D), and Ser(S), which make up the catalytic triad common to all serine proteases and participate in enzyme catalysis7,8. The mRNA for hepsin is present in many tissues, with the high level in the liver tissue, and the low level in the kidney, pancreas, lung, thyroid, pituitary gland, and the testis9. Furthermore, hepsin is frequently overexpressed in prostate cancer10,11,12,13, breast cancer14, ovarian cancer15,16 and renal cell carcinoma17 and implicated in augmenting the prostate and ovarian tumorigenesis and metastatic dissemination16,18,19,20, mammalian cell growth and maintenance of cell of morphology21, activation of human Factor VII, blood coagulation and thrombin formation22 and developmental processes, such as blastocyst hatching23. Since hepsin is a transmembrane serine protease, it may play significant roles in biological and pathological processes occurring on the cell surfaces, including participating in signal transduction, processing of protein hormones, growth factors and receptors and activation of latent proteases. The expression pattern and impact of hepsin in gastric cancer remain unclear, so we aim to investigate the correlation between hepsin protein and overall survival (OS) of gastric cancer patients.
In this study, we examined the hepsin expression pattern in gastric cancer and its relationship with clinicopathological characteristics. Moreover, we generated a predictive nomogram to delineate the 3- and 5-year overall survival of the patients with gastric cancer after surgery.
Results
Hepsin mRNA and protein expression in Gastric cancer
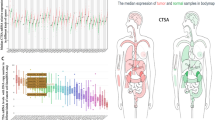
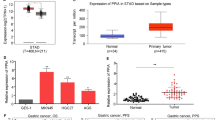
We used real-time quantitative PCR to determine Hepsin mRNA expression level in 10 normal tissues, 50 gastric cancer tumor tissues and patient-matched adjacent peritumor tissues. Representative images of three tumor samples stained by hematoxylin-eosin (HE) (Supplemental Figure 2). The tumor samples have similar tumor cell content (60% approximately) would be used to detect the mRNA or protein expression according to HE staining. The Hepsin mRNA expression level was downregulated in 78% (39/50) of gastric cancer patients (Fig. 1A). Furthermore, we searched and analyzed Hepsin mRNA expression in five independent microarray datasets from Oncomine database (Cho, Cui, Wang, Chen, and DErrico) (Fig. 1B, Supplemental Figure 1), which is consistent with our data. Hepsin protein expression levels were examined by western blot and immunohistochemical staining (IHC) methods (Figs 1C and 2). As shown in Fig. 1C, one protein bands, whose molecular weight is about 42 kDa, is observed in gastric cancer tissues and matched adjacent pericancer tissues in western blot analysis. A decrease in hepsin expression was observed in 55% (22/40) of the gastric cancer tumor tissues compared with the matched adjacent peritumor tissues (Fig. 1C,D). Further, the expression of hepsin protein was examined in a tissue microarray (TMA) containing 220 pairs of gastric tissues by IHC staining analysis. Evidence was presented that hepsin protein expression was mainly located in the nuclear and cytoplasm of gastric tumor cells, peritumoral tissue cells and normal tissue cells (Fig. 2). The IHC density of hepsin exhibits a significant difference in gastric tumor tissues and their matched adjacent non-tumor tissues (P < 0.001) (Fig. 2G).
Hepsin expression is decreased in gastric cancer at mRNA and proetein level.
(A) The Hepsin mRNA expression levels in 10 normal tissues, 50 matched peritumor and tumor tissues were determined by real-time quantitative PCR. (B) The Hepsin mRNA expression levels in five independent microarray datasets from Oncomine database reported by Cho, Cui, Wang, Chen, and DErrico. (C) Western blotting analysis of hepsin expression in gastric cancer 40 pairs of resection specimens from gastric cancer patients. (P: peritumor, T: tumor) (D) The relative hepsin protein expression levels in 40 pairs of representative gastric cancer tumor tissues and the matched adjacent non-tumor tissues.
Hepsin expression in gastric cancer tissue samples.
(A–F) Representative images of hepsin protein expression in gastric cancer tissues, compared with corresponding peritumor tissues and normal tissues; (A) peritumor tissue, scored as low. (B) Peritumor tissue, scored as strong. (C) Gastric cancer tissue, scored as low; (D) gastric cancer tissue, scored as moderate; (E) gastric cancer tissue, scored as high; (F) normal tissue, scored as high; (G) Comparison of hepsin IHC density between normal gastric tissues and gastric cancer tissues.
Hepsin is a transmembrane serine protease and has one predicted N-glycosylation site in Asn-112. We found that N-glycosylation at Asn-112 is important for hepsin cell surface targeting and tumor invasion and migration. Wild hepsin was mainly localized in the cytoplasm and the cell membrane, while hepsin mutant N112Q was localized predominantly in the nucleus of the AGS cells (Supplemental Figure 3). So we speculated that nuclear hepsin in IHC should be de-glycosylated or not fully glycosylated. In addition, wild hepsin overexpression enhanced cell migration and invasion (Supplemental Figure 4), whereas hepsin mutant N112Q attenuated the invasion and metastatic potential compared to wild hepsin in MGC80-3 cells (Supplemental Figure 4). Similar roles of N-glycosylation in regulating cell surface expression and protease activity have been reported in other type II transmembrane serine proteases, such as corin24, enteropeptidase25, matriptase26, and matriptase-227, which are involved in blood pressure regulation, food digestion, epithelial function, and iron metabolism, respectively24,28,29.
Relationship between Hepsin expression and clinical parameters
To determine the clinical significance of hepsin expression in gastric cancer, the Chi-square test was taken to assess the associations between hepsin protein expression and clinicopathological parameters (including age, gender, tumor location, Histological differentiation, Lauren classification, T classification, N classification, distant metastasis, clinical stage and intravascular cancer emboli). The results demonstrated that hepsin expression in gastric cancer tissues is closely associated with histological differentiation (P = 0.001), Lauren classification (P = 0.001), T classification (P = 0.011) N classification (P = 0.039) and clinical stage (P = 0.007). No significant associations were detected between hepsin expression and age, gender, tumor location, distant metastasis or intravascular cancer emboli (Table 1). The results were confirmed in the validation set of patients. It was also demonstrated that hepsin expression was correlated to Lauren classification (P = 0.038), T classification (P = 0.033) N classification (P = 0.031) and clinical stage (P = 0.023) (Supplementary Table 1).
Correlation between Hepsin expression and prognosis in Gastric cancer patients
To further evaluate the prognostic value of hepsin in gastric cancer, we explored the correlation between hepsin expression and clinical data by Kaplan-Meier analysis and log-rank test. As shown in Fig. 3, high hepsin expression was associated with poor overall survival (P = 0.0014). Furthermore, we explored the association between hepsin expression and overall survival in gastric cancer patients with early or advanced clinical stages and with or without lymphatic metastasis and vascular invasion. According to Kaplan-Meier analyses, we found the overall survival is shorter in gastric cancer patients with high hepsin expression in all stages (Fig. 3A) or in III–IV stage (Fig. 3C). Similar result was confirmed in our validation set (Supplementary Figure 5). High expression of hepsin was also found to be associated with poor overall survival in gastric cancer patients without vascular invasion or with lymphatic metastasis (Supplemental Figure 6). Consistent with our results, the prognostic value of hepsin in gastric cancer was verified by online survival analysis software (http://www.kmplot.com/analysis/index.php?p=service&cancer=gastric), which integrated reported microarray datasets. The result demonstrated that high expression of hepsin correlated to poorer overall survival (Fig. 3D) as well as progression-free survival (Fig. 3E) in gastric cancer patients. In order to obtain a more sensitive predictive model for outcomes of gastric cancer patients, we combined hepsin expression and TNM stage to create a prognostic score system. ROC analysis revealed that the combination of hepsin and TNM stage showed better prognostic value [area under curve (AUC) 0.785, 95% confidence interval (CI) 0.723–0.846] than TNM stage alone (AUC 0.755, 95% CI 0.689–0.820, P = 0.044) or hepsin expression alone (AUC 0.591, 95% CI 0.516–0.666, P < 0.001) (Fig. 3F). We also analyzed the recurrence free survival information of GSE26253 datebase (Supplemental Figure 7).
Hepsin expression is correlated with the overall survival rate in gastric cancer patients.
(A) Kaplan-Merier survival curves show high expression level of hepsin was significantly correlated with poor survival of gastric cancer. (B,C) Comparisons of overall survival between hepsin high expression and hepsin low expression in early clinical stage (I–II) cohort and in advanced clinical stage (III–IV) cohort. (D,E) The prognostic value of Hepsin in gastric cancer was verified by online survival analysis software (http://www.kmplot.com/analysis/index.php?p=service&cancer=gastric), which integrated reported microarray datasets. It also showed that high expression of Hepsin was significantly associated with poorer overall survival as well as progression-free survival in gastric cancer patients (P < 0.001). (F) ROC analysis of the sensitivity and specificity for the prognosis of overall survival by TNM stage/hepsin expression model, TNM stage model, and hepsin expression model. P-values were calculated by log-rank test.
In addition, univariate and multivariate analyses showed that hepsin could be useful as an independent risk factor for poor prognosis in the 220 cases of gastric cancer. The univariate Cox regression analyses showed that T classification (P < 0.001), N classification (P < 0.001), distant metastasis (P < 0.001), clinical TNM stage (P < 0.001), Intravascular cancer emboli (P = 0.0024) and hepsin expression (P = 0.0014) were significantly relevant with overall survival in gastric cancer. The multivariate Cox regression analyses, however, showed that T classification (P = 0.016), distant metastasis (P < 0.001), clinical TNM stage (P = 0.011) and hepsin expression (P = 0.036) were significantly different (Table 2). Then the Harrell’s concordance index (C-index) analyses were examined to assess the predictive accuracies of TNM stage and hepsin protein expression (Table 3).
Nomogram and calibration plot analyses for gastric cancer patients
Based on obtained evidence, we used patients’ data in the two cohorts to develop a nomogram to predict OS at 3 and 5 years after surgery (Fig. 4A). The predictors included tumor T stage, N stage, M stage and hepsin expression, all of which were independent prognostic indicators for OS. In the nomogram, a higher total point represents a worse survival. The calibration plot predicted 5-year overall survival were built to give the internal validation, which performed well compared with the ideal model (Fig. 4B). We next stratified the gastric cancer patients into 3 groups according to the score calculated using the nomogram: low-risk (<25th percentile), intermediate-risk (25th–75th percentile), and high-risk (>75th percentile) groups (Fig. 4C). As shown in Fig. 4C, the nomogram could effectively discriminate the risk of OS in gastric cancer patients.
Nomogram and calibration plot analyses for the predictive value of hepsin protein expression in gastric cancer patients.
(A) Nomogram generation for predicting overall survival integrated with T stage (1 represents T1, 2 represents T2, 3 represents T3, 4 represents T4), N stage (0 represents N0, 1 represents N1, 2 represents N2, 3 represents N3), distant metastasis (0 represents absence, 1 represents presence), and hepsin expression (0 represents low expression, 1 represents high expression). (B) Calibration curve for nomogram-predicted and observed 5-year overall survival. (C) The patients were stratified into 3 groups according to their percentile of the nomogram-predicted score: low risk group (<25th percentile), intermediate risk group (25th–75th percentile), and high risk group (>75th percentile).
Discussion
Although gastric cancer incidence has declined for decades, it remains the fifth most common cancer and the fifth leading cause of cancer-related mortality in USA30. The majority of gastric cancer patients are diagnosed at advanced stage, due to lacking early detecting methods31. To date, the outcomes for gastric cancer patients with similar TNM stage can be very different because of the heterogeneity of this tumor, and the prognostic models for gastric cancer patients are largely relied on the TNM stage5. Therefore, we need to identify some novel molecules associated with tumorigenesis of gastric cancer and better understand the tumor progression and predict the cancer clinical outcomes. It will be helpful to compare expression levels of mRNA and protein of hepsin in tumor tissues with matched normal tissues of gastric cancer patients to describe the physiological and pathophysiological importance of hepsin in gastric cancer.
To this end, we have first time described the hepsin expression pattern in gastric cancer tissues in both protein and mRNA levels in this study. Additionally, the hepsin protein expression and its relationship with the clinicopathological parameters and clinical prognosis values are illustrated.
In the study, hepsin mRNA and protein expression level is mainly downregulated in Gastric cancer tissues. High expression of hepsin is correlated with poorer overall survival, as well as progression-free survival in patients with gastric cancer. There is a significance between high hepsin expression and low hepsin expression in gastric cancer patients with advanced stage, III–IV, so we speculate that hepsin may contribute to gastric cancer in later stage. In Zuyan Luo’s study, the OLFM4 expression pattern and correlation with gastric cancer patients’ overall survival are similar with our results32. Our findings reflect distinct actions of gastric and gastric carcinoma cells in response to hepsin protein. Probably, gastric and gastric carcinoma cells use different signaling pathways in response to hepsin expression. For example, hepatocytes react differently than hepatoma cells to IL-6 stimulation in regulating HBV replication. In hepatoma cells, IL-6 stimulates HBV transcription by activating STAT-3, which interacts with HNF3 bound to the HBV enhancer33. However, in primary human hepatocytes, IL-6 suppresses HBV gene expression and replication through the down-regulation of HNF4a and HNF1a34.
Although a large quantity of membrane-associated proteinase has been found, their biological roles are still unknown. Associations between TMPRSS2 and TMPRSS4 and cancers have been reported. TMPRSS2 may be a potential diagnostic or therapeutic target for prostate cancer, which is considered to have a role in cell biology35. TMPRSS4 is usually overexpressed in pancreatic cancer, however, its functional significance remains to be illustrated36. Low expression levels of hepsin and TMPRSS3 are associated with poor breast cancer survival37. Because hepsin is upregulated in advanced stage of gastric cancer, it may contribute to expansion, growth, invasion and metastasis of these tumor cells.
As investigated, membrane-associated serine proteases play a vital role in tumor invasion and metastasis38,39. Hepsin expression may contribute to gastric cancer progression and metastasis by a few molecular mechanisms. For instance, hepsin could act as a growth factor, which plays a role in stimulating the proliferation and increase progression ability of cancer cells40,41. This hepsin activity for cultured hepatocytes has been determined21. Hepsin may also directly or indirectly degrade extracellular matrix proteins by activating matrix metalloproteinases (MMPs)42. As well known, proteolytic digestion of extracellular matrix proteins plays a crucial role in tumor invasion and metastasis. High hepsin expression in gastric cancer tissues may at some certain reflect the state of poorly differentiated gastric cancer cells. Testing gastric cancer models in hepsin-deficient mice should indicate the biological significance and the true molecular mechanism of hepsin in gastric cancer.
In conclusion, our study has demonstrated that increased hepsin expression is correlated with poor prognosis in gastric cancer patients, and hepsin may be identified as an independent prognostic factor and may be a potential target for the treatment of gastric cancer patients. In order to better understand hepsin’s physiological functions, additional experimentation remains to be determined.
Materials and Methods
Cell culture and reagents
Human gastric cancer cell lines AGS and MGC80-3 were purchased from the Cell Bank of the Type Culture Collection of the Chinese Academy of Sciences (Shanghai, China), and cultured in Dulbecco’s modified Eagle’s medium (DMEM) or RPMI1640 supplemented with 10% fetal bovine serum (FBS) (catalogue no. 16000-044; Gibco, Grand Island, NY, USA) at 37 °C in a humidified atmosphere containing 5% CO2 separately. The gastric cancer cell lines used have been authenticated and tested to exclude the possibility of mycoplasma contamination.
Patient samples
For tissue microarray (TMA) detection, human gastric cancer tumor specimens containing 220 cases of tumor and matched non-tumor tissues were all enrolled between 2004 and 2008 from the Department of General Surgery, Zhongshan Hospital, School of Medicine, Fudan University, Shanghai, China. Another independent set of patients comprising a total of 102 patients from Zhongshan Hospital was recruited during 2005. All the patients received standard gastrectomy with lymphadenectomy by the same surgical team. None of these patients received any preoperative anticancer therapy. The clinicopathologic features of patients are provided in Table 1. The tumor differentiation grade and clinical stages were reclassified according to the seventh American Joint Committee on Cancer (AJCC) TNM classification. The cases of gastric cancer in our study were selected only if clinical data were available. We calculated the follow-up time from the date of surgery to the date of death, or last visit. An additional independent group of 40 paired frozen gastric cancer and corresponding normal mucosa tissues were also obtained from the Department of General Surgery, Zhongshan Hospital, Fudan University, Shanghai, China, in 2014. The use of human tissue samples and clinical data was approved by the Clinical Research Ethics Committee of Zhongshan Hospital, Fudan University. All donors provided written informed consent to donate their samples. All methods were taken in accordance with the approved guidelines of School of Medical graduate Fudan University.
Real-time PCR
Real-time PCR analyses were carried out as described previously43. The total RNA was isolated from the normal gastric tissues, gastric cancer tissues and matched peritumor tissues by using TRIzol reagent (Invitrogen, USA) according to the manufacturer’s instruction. Hepsin mRNA expression levels were determined by using specific primers after normalization with glyceraldehyde 3 phosphate dehydrogenase (GAPDH). The primer sequence were: GAPDH, (Forwad) 5′-GTCAAGGCTGAGAACGGGAA-3 and (Reverse) 5′-AAATGAGCCCCAGCCTTCTC-3; Hepsin, (Forward) 5′-GTCTGCAATGGCGCTGACTTCT-3′ and (Reverse) 5′-TCCGAGAGATGCTGTCCTCACA-3′.
Western blotting
Western blot analyses were performed as described previously44. Primary antibodies were rabbit anti-hepsin (Abcam, UK), mouse anti-actin (Cell Signal Technology, USA). And species-specific (mouse or rabbit) secondary antibody was purchased from Santa Cruz Biotechnology.
Immunochemistry staining
Immunohistochemical staining protocol was constructed as previous described43. Depending on the staining extent, the score of hepsin expression was conducted: 0, 0–5%; 1, 5–25%; 2, 26–50%; 3, 51–75%; and 4, >75%, and the staining intensity was categorized as follows: no staining scored 0, weakly staining scored 1, moderately staining scored 2 and strongly staining scored 3, respectively. The staining score was designated by multiplying staining area score by staining intensity score, yielding a series of results ranging from 0 to 12. High expression was considered as a total score >4 and low expression with a total score ≤4 according to receiver operating characteristic (ROC) analysis. The immunochemistry staining scores were determined independently by two pathologists who were blinded to the patients’ clinical data.
Immunofluorescent staining
Immunofluorescent staining analyses were carried out as described previously43. Hepsin was detected with Anti-V5 (Invitrogen) and visualized with goat anti-mouse IgG-Alexa Fluor 488 (Jackson). 5 mg/ml DAPI (Beyotime) was used for nuclear staining. Images were taken by a Confocal Laser Scanning Microscope (Leica TCS SP5, Germany).
Transwell assay
Transwell assay was performed as described previously45. AGS cells were transfected with plasmids, V5-hepsin and V5-hepsin N112Q. Migration and invasion of cells were determined 24 h and 40 h later, respectively. The infiltrating cells were stained with crystal violet, and cell numbers were counted from five fields. Each experiment was repeated three times.
Statistical analysis
SPSS19.0 (SPSS Inc.; Chicago, IL, USA) and GraphPad Prism 5 (San Diego, CA) software were used for statistical analyses and graphical representations. The χ2 test was used to analyze the relations between hepsin expression and clinicopathological parameters in gastric cancer patients. Survival curves were evaluated using the Kaplan-Meier method, and differences between survival curves were tested by the log-rank test. Cox proportional hazards regression model was used to examine univariate and multivariate analyses. Only significantly different variables in univariate analysis were entered into the next multivariate analysis. Nomogram was generated by R software with “rms” package. Calibration plot for 5-year overall survival was constructed to examine the performance characteristics of the generated nomogram. The prognostic accuracy was measured by calculating the Harrell’s concordance index (c-index). A two-sided P-value < 0.05 was considered statistically significant.
Additional Information
How to cite this article: Zhang, M. et al. High Hepsin expression predicts poor prognosis in Gastric Cancer. Sci. Rep. 6, 36902; doi: 10.1038/srep36902 (2016).
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Hartgrink, H. H., Jansen, E. P., van Grieken, N. C. & van de Velde, C. J. Gastric cancer. Lancet 374, 477–490, doi: 10.1016/S0140-6736(09)60617-6 (2009).
Torre, L. A. et al. Global cancer statistics, 2012. CA: a cancer journal for clinicians 65, 87–108, doi: 10.3322/caac.21262 (2015).
Washington, K. 7th edition of the AJCC cancer staging manual: stomach. Annals of surgical oncology 17, 3077–3079, doi: 10.1245/s10434-010-1362-z (2010).
Deng, J. Y. & Liang, H. Clinical significance of lymph node metastasis in gastric cancer. World journal of gastroenterology 20, 3967–3975, doi: 10.3748/wjg.v20.i14.3967 (2014).
Lim, L., Michael, M., Mann, G. B. & Leong, T. Adjuvant therapy in gastric cancer. Journal of clinical oncology: official journal of the American Society of Clinical Oncology 23, 6220–6232, doi: 10.1200/JCO.2005.11.593 (2005).
Leytus, S. P., Loeb, K. R., Hagen, F. S., Kurachi, K. & Davie, E. W. A novel trypsin-like serine protease (hepsin) with a putative transmembrane domain expressed by human liver and hepatoma cells. Biochemistry 27, 1067–1074 (1988).
Hooper, J. D., Clements, J. A., Quigley, J. P. & Antalis, T. M. Type II transmembrane serine proteases. Insights into an emerging class of cell surface proteolytic enzymes. The Journal of biological chemistry 276, 857–860, doi: 10.1074/jbc.R000020200 (2001).
Szabo, R. et al. Type II transmembrane serine proteases. Thrombosis and haemostasis 90, 185–193, doi: 10.1160/TH03-02-0071 (2003).
Tsuji, A. et al. Hepsin, a cell membrane-associated protease. Characterization, tissue distribution, and gene localization. The Journal of biological chemistry 266, 16948–16953 (1991).
Dhanasekaran, S. M. et al. Delineation of prognostic biomarkers in prostate cancer. Nature 412, 822–826, doi: 10.1038/35090585 (2001).
Luo, J. et al. Human prostate cancer and benign prostatic hyperplasia: molecular dissection by gene expression profiling. Cancer research 61, 4683–4688 (2001).
Magee, J. A. et al. Expression profiling reveals hepsin overexpression in prostate cancer. Cancer research 61, 5692–5696 (2001).
Ernst, T. et al. Decrease and gain of gene expression are equally discriminatory markers for prostate carcinoma: a gene expression analysis on total and microdissected prostate tissue. The American journal of pathology 160, 2169–2180, doi: 10.1016/S0002-9440(10)61165-0 (2002).
Xing, P. et al. Clinical and biological significance of hepsin overexpression in breast cancer. Journal of investigative medicine: the official publication of the American Federation for Clinical Research 59, 803–810, doi: 10.231/JIM.0b013e31821451a1 (2011).
Tanimoto, H. et al. Hepsin, a cell surface serine protease identified in hepatoma cells, is overexpressed in ovarian cancer. Cancer research 57, 2884–2887 (1997).
Miao, J. et al. Hepsin colocalizes with desmosomes and induces progression of ovarian cancer in a mouse model. International journal of cancer 123, 2041–2047, doi: 10.1002/ijc.23726 (2008).
Zacharski, L. R., Ornstein, D. L., Memoli, V. A., Rousseau, S. M. & Kisiel, W. Expression of the factor VII activating protease, hepsin, in situ in renal cell carcinoma. Thrombosis and haemostasis 79, 876–877 (1998).
Klezovitch, O. et al. Hepsin promotes prostate cancer progression and metastasis. Cancer cell 6, 185–195, doi: 10.1016/j.ccr.2004.07.008 (2004).
Li, W. et al. Pegylated kunitz domain inhibitor suppresses hepsin-mediated invasive tumor growth and metastasis. Cancer research 69, 8395–8402, doi: 10.1158/0008-5472.CAN-09-1995 (2009).
Xuan, J. A. et al. Antibodies neutralizing hepsin protease activity do not impact cell growth but inhibit invasion of prostate and ovarian tumor cells in culture. Cancer research 66, 3611–3619, doi: 10.1158/0008-5472.CAN-05-2983 (2006).
Torres-Rosado, A., O’Shea, K. S., Tsuji, A., Chou, S. H. & Kurachi, K. Hepsin, a putative cell-surface serine protease, is required for mammalian cell growth. Proceedings of the National Academy of Sciences of the United States of America 90, 7181–7185 (1993).
Kazama, Y., Hamamoto, T., Foster, D. C. & Kisiel, W. Hepsin, a putative membrane-associated serine protease, activates human factor VII and initiates a pathway of blood coagulation on the cell surface leading to thrombin formation. The Journal of biological chemistry 270, 66–72 (1995).
Vu, T. K., Liu, R. W., Haaksma, C. J., Tomasek, J. J. & Howard, E. W. Identification and cloning of the membrane-associated serine protease, hepsin, from mouse preimplantation embryos. The Journal of biological chemistry 272, 31315–31320 (1997).
Wang, H. et al. Distinct roles of N-glycosylation at different sites of corin in cell membrane targeting and ectodomain shedding. The Journal of biological chemistry 290, 1654–1663, doi: 10.1074/jbc.M114.606442 (2015).
Zheng, X., Lu, D. & Sadler, J. E. Apical sorting of bovine enteropeptidase does not involve detergent-resistant association with sphingolipid-cholesterol rafts. The Journal of biological chemistry 274, 1596–1605 (1999).
Oberst, M. D., Williams, C. A., Dickson, R. B., Johnson, M. D. & Lin, C. Y. The activation of matriptase requires its noncatalytic domains, serine protease domain, and its cognate inhibitor. The Journal of biological chemistry 278, 26773–26779, doi: 10.1074/jbc.M304282200 (2003).
Jiang, J. et al. N-glycosylation is required for matriptase-2 autoactivation and ectodomain shedding. The Journal of biological chemistry 289, 19500–19507, doi: 10.1074/jbc.M114.555110 (2014).
Antalis, T. M., Bugge, T. H. & Wu, Q. Membrane-anchored serine proteases in health and disease. Progress in molecular biology and translational science 99, 1–50, doi: 10.1016/B978-0-12-385504-6.00001-4 (2011).
Miller, G. S. & List, K. The matriptase-prostasin proteolytic cascade in epithelial development and pathology. Cell and tissue research 351, 245–253, doi: 10.1007/s00441-012-1348-1 (2013).
Siegel, R., Ma, J., Zou, Z. & Jemal, A. Cancer statistics, 2014. CA: a cancer journal for clinicians 64, 9–29, doi: 10.3322/caac.21208 (2014).
Yamada, T. et al. The survival difference between gastric cancer patients from the UK and Japan remains after weighted propensity score analysis considering all background factors. Gastric cancer: official journal of the International Gastric Cancer Association and the Japanese Gastric Cancer Association 19, 479–489, doi: 10.1007/s10120-015-0480-5 (2016).
Luo, Z. et al. OLFM4 is associated with lymph node metastasis and poor prognosis in patients with gastric cancer. Journal of cancer research and clinical oncology 137, 1713–1720, doi: 10.1007/s00432-011-1042-9 (2011).
Waris, G. & Siddiqui, A. Interaction between STAT-3 and HNF-3 leads to the activation of liver-specific hepatitis B virus enhancer 1 function. Journal of virology 76, 2721–2729 (2002).
Hosel, M. et al. Not interferon, but interleukin-6 controls early gene expression in hepatitis B virus infection. Hepatology 50, 1773–1782, doi: 10.1002/hep.23226 (2009).
Lin, B. et al. Prostate-localized and androgen-regulated expression of the membrane-bound serine protease TMPRSS2. Cancer research 59, 4180–4184 (1999).
Wallrapp, C. et al. A novel transmembrane serine protease (TMPRSS3) overexpressed in pancreatic cancer. Cancer research 60, 2602–2606 (2000).
Pelkonen, M. et al. Low expression levels of hepsin and TMPRSS3 are associated with poor breast cancer survival. BMC cancer 15, 431, doi: 10.1186/s12885-015-1440-5 (2015).
Mignatti, P. & Rifkin, D. B. Biology and biochemistry of proteinases in tumor invasion. Physiological reviews 73, 161–195 (1993).
Mullins, D. E. & Rohrlich, S. T. The role of proteinases in cellular invasiveness. Biochimica et biophysica acta 695, 177–214 (1983).
Herter, S. et al. Hepatocyte growth factor is a preferred in vitro substrate for human hepsin, a membrane-anchored serine protease implicated in prostate and ovarian cancers. The Biochemical journal 390, 125–136, doi: 10.1042/BJ20041955 (2005).
Kirchhofer, D. et al. Hepsin activates pro-hepatocyte growth factor and is inhibited by hepatocyte growth factor activator inhibitor-1B (HAI-1B) and HAI-2. FEBS letters 579, 1945–1950, doi: 10.1016/j.febslet.2005.01.085 (2005).
Wu, Q. Type II transmembrane serine proteases. Current topics in developmental biology 54, 167–206 (2003).
Zhang, M., Gu, J. & Zhang, C. Hepatitis B virus X protein binding to hepsin promotes C3 production by inducing IL-6 secretion from hepatocytes. Oncotarget 7, 7780–7800, doi: 10.18632/oncotarget.6846 (2016).
Zhang, C. et al. Hepsin inhibits CDK11p58 IRES activity by suppressing unr expression and eIF-2alpha phosphorylation in prostate cancer. Cellular signalling 27, 789–797, doi: 10.1016/j.cellsig.2014.12.020 (2015).
Min, L. et al. Overexpression of Ras-GTPase-activating protein SH3 domain-binding protein 1 correlates with poor prognosis in gastric cancer patients. Histopathology 67, 677–688, doi: 10.1111/his.12695 (2015).
Acknowledgements
This work was supported by the National Natural Science Fund (31100977, KRF101453).
Author information
Authors and Affiliations
Contributions
M.M.Z. and J.J.Z. contributed equally to this manuscript. X.F.W., C.Y.Z. and J.X.G. designed the research and revised the manuscript. W.Y.T., Y.R.W., P.K.P., L.L.L., S.S.S., H.W., C.L. and C.T.Y. analyzed the data; M.M.Z. and J.J.Z. performed the research and wrote the paper. All authors read and approved the final manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zhang, M., Zhao, J., Tang, W. et al. High Hepsin expression predicts poor prognosis in Gastric Cancer. Sci Rep 6, 36902 (2016). https://doi.org/10.1038/srep36902
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep36902
This article is cited by
-
LncRNA-LA16c-313D11.11,A Signature to Predict Endometrial Carcinoma Patients with a Better Survival
Reproductive Sciences (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.