Abstract
Isothermal nucleic acid amplification assays such as the loop mediated isothermal amplification (LAMP), are well suited for field use as they do not require thermal cyclers to amplify the DNA. To further facilitate the use of LAMP assays in remote settings, simpler sample preparation methods and lyophilized reagents are required. The performance of a commercial malaria LAMP assay (Illumigene Malaria LAMP) was evaluated using two sample preparation workflows (simple filtration prep (SFP)) and gravity-driven filtration prep (GFP)) and pre-dispensed lyophilized reagents. Laboratory and clinical samples were tested in a field laboratory in Senegal and the results independently confirmed in a reference laboratory in the U.S.A. The Illumigene Malaria LAMP assay was easily implemented in the clinical laboratory and gave similar results to a real-time PCR reference test with limits of detection of ≤2.0 parasites/μl depending on the sample preparation method used. This assay reliably detected Plasmodium sp. parasites in a simple low-tech format, providing a much needed alternative to the more complex molecular tests for malaria diagnosis.
Similar content being viewed by others
Introduction
Current malaria diagnostic tests rely on parasite detection by microscopy or antigen-based rapid diagnostic tests (RDT). Molecular methods such as polymerase chain reaction (PCR), mostly used in reference laboratory settings, have been shown to increase the sensitivity of detection. However, molecular tools are not commonly used in endemic countries as they require sophisticated laboratory capacity. The scope of performing molecular diagnosis in resource limited settings expanded when the loop mediated isothermal amplification (LAMP) technique was introduced to detect infectious disease agents1. Unlike PCR, which requires alternating temperature conditions, LAMP amplifies nucleic acids (RNA and DNA) at a constant temperature (isothermal), typically around 62 °C–65 °C. This facilitated further innovations to adapt this technology as a portable platform for field use2,3,4. The LAMP assay has been shown to be a highly sensitive and rapid molecular method and malaria LAMP assays have been developed for the detection of Plasmodium species5,6,7,8. In an effort to simplify the LAMP assay for use in resource limited countries, several different formats of LAMP have been investigated and evaluated, including the use of colorimetric high throughput assays such as hydroxynaphthol blue9 and the malachite green dyes10.
The field deployment of any molecular testing, including LAMP, should address certain challenges such as 1) simplification of sample preparation from blood to obtain amplifiable DNA, 2) assay reagent stability under ambient conditions, and 3) ease-of-use for the end-user. With the exception of the Loopamp MALARIA kit (Eiken Chemical Co.), which utilizes a simpler sample preparation method as well as lyophilized reagents, many of the malaria LAMP assays described to date still rely on the conventional DNA extraction methods and liquid-based assay reagents that require maintenance in the cold. The use of lyophilized reagents and simplified sample preparation methods has potential to make it easier to deploy the LAMP assays in resource limited regions.
Recently, another commercially available malaria LAMP kit, the Illumigene Malaria LAMP, was developed by Meridian Bioscience Inc. (Cincinnati, OH). This kit consists of pre-dispensed, ambient temperature stable LAMP reagents designed to detect malaria parasites at the genus level. The LAMP assay is performed using the illumipro-10™ Incubator/Reader, which is capable of testing 10 samples per run. The change in turbidity associated with LAMP assays, due to the magnesium-pyrophosphate build-up as a by-product, is measured by the illumipro-10™ reader and a qualitative result is determined. Two simple centrifuge-free methods to extract DNA from EDTA whole blood were designed: a simple filtration method (Illumigene Malaria; herein referred to as SFP for simple filtration prep as shown in Fig. 1a) and a gravity-driven gel filtration column (Illumigene Malaria PLUS; herein referred to as GFP for gravity filtration prep, as shown in Fig. 1b). Both procedures rely on chemical lysis and produce amplifiable DNA within 10 minutes.
Illumigene Malaria LAMP workflow.
The Illumigene Malaria LAMP assay workflows include a sample preparation step followed by an amplification step. Two sample preparation workflows were developed: one using a simple filtration sample preparation method, Fig. 1a, and the other a 7–10 minutes gravity-driven gel filtration sample preparation method, Fig. 1b. The assays are performed as described in the corresponding insert. The necessary LAMP reagents are lyophilized in the Illumigene Malaria Test Device which consist of a TEST tube with primers targeting the Plasmodium genus and a CONTROL tube with primers to detect the housekeeping human gene, used as a DNA isolation and amplification control. The runs are performed using the illumipro-10™ incubator Reader and a qualitative result (positive, negative or invalid) is printed put after the run. These figures were prepared and provided by Meridian Bioscience, Inc.
Here, we report results from the first evaluation, conducted in a clinical laboratory in Senegal, on the performance of the Illumigene Malaria LAMP assay using both the SFP and GFP sample preparation methods.
Results
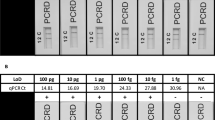
Cross-reactivity and Limits of Detection of the Illumigene Malaria LAMP
The cross-reactivity and limits of detection (LoD) experiments were performed by Meridian Biosciences with technical assistance from CDC prior to the field evaluation of the assays. Based on the Plasmodium target DNA sequence alignments, the LAMP targets selected for Illumigene Malaria LAMP primers are highly conserved across the Plasmodium genus. No DNA sequence homology was observed with the selected targets other than the Plasmodium sequences using BLAST sequence analysis software at NCBI against the entire content of GenBank non-redundant sequences database. The assay was shown to detect all five human-infecting Plasmodium species: P. falciparum, P. vivax, P. ovale, P. malariae and P. knowlesi. No cross-reactivity was observed with human genomic DNA or with all the non-Plasmodium species tested. Using P. falciparum strain 3D7 DNA, the Limit of Detection (LoD) of the SFP and the GFP methods were determined to be 2.0 parasites/μl and 0.3 parasites/μl, respectively. LoD using the WHO standard were determined to be 4, 256 IU/μl (equivalent to 2 parasites/μl) for the SPF method and 851 IU/μl (0.4 parasites/μl) for the GFP method. The LoD using P. vivax DNA (India VII strain) was found to be 0.1 parasites/μL for both the SFP and GFP assays.
Evaluation of the Illumigene Malaria LAMP Assays in a Clinical Laboratory in Senegal
A total of two hundred sixteen (216) whole blood and corresponding dried blood spots (DBS) samples were collected from 3 clinical sites in Senegal: Pikine, Rufisque and Thies. The three sites are found in a malaria hypo endemic area in which three human infecting species, P. falciparum, P. malariae and P. ovale are known to circulate. The parasite prevalence in Pikine and Rufisque is about 3% and it is about 1% in Thies. All the samples were tested in a clinical laboratory located in Thies, that routinely conducts microscopic and RDT evaluations. The whole blood was used for the LAMP assays while the DBS were utilized for the PET-PCR assay. Sixty six of the whole blood samples were utilized immediately upon collection or stored between 2–4 °C for1 to 7 days before use for Illumigene LAMP (prospective samples). The remaining 150 blood samples were collected and evaluated by microscopy and then frozen at <20 °C until utilized for the LAMP assays which was within 30 days of storage (retrospective). The patient population included 84 females and 131 males (the gender of 1 patient was not defined). Only 209 samples were included in the analysis because 5 samples (3 positive, 2 negative by microscopy) were excluded because the incorrect assay program was used for GFP testing and 2 samples gave invalid results using the SFP method in that the assay control (run with every sample) gave invalid results. The SFP and GFP performance characteristics were compared to the local microscopy performed in the field. The collected DBS were send to the CDC to be evaluated using the PET-PCR assay. These assays were performed blinded to the microscopy and LAMP results obtained in the field.
Performance Characteristics of the Illumigene Malaria LAMP by Specimen Storage
No significant difference was observed in the obtained specificity by using either prospective or retrospective samples with the GFP (p = 0.146) and SFP assays (p = 0.5921) compared to microscopy.
Performance Characteristics of the Illumigene Malaria LAMP compared to microscopy and the PET-PCR
The species distribution of the 209 samples utilized in this study was 134 P. falciparum, 1 P. ovale and 1 mixed infection: P. falciparum and P. malariae. The average parasite density, as determined by microscopy, was 36,942 parasites/μl and range 40 to 404,000 parasites/μl. Both PET-PCR and the Illumigene Malaria LAMP assays identified additional positive samples compared to microscopy; 11 by GFP method and 7 by both PET-PCR and SFP method. Table 1 and Fig. 2, summarizes the obtained sensitivity and specificity of Illumigene Malaria LAMP and microscopy, compared to PET-PCR, used as the reference test.
Graphical representation of sensitivity and specificity of microscopy, SFP and GFP compared to PET-PCR.
The sensitivity and specificity of SFP (simple filtration prep), GFP (gravity-driven prep) methods and microscopy were calculated using the PET-PCR as the reference test. The whiskers show the 95% confidence intervals for sensitivity and specificity (centre diamonds).
Discrepant samples
Twelve samples had discrepant results between the PET-PCR and LAMP tests, Table 2. Four PET-PCR samples of Ct values above 37.0 were shown to be negative by the LAMP assays while 8 samples negative by PET-PCR were shown to be positive by either the SFP (4/8) and/or the GFP assay (8/8).
Comparison between the SFP and GFP Sample Preparation Methods
Both sample preparation methods were easy to perform in the field with minimum laboratory training. The GFP assay detected four more positive samples than the SFP assay (148 samples compared to 144). These four samples were also found to be negative by the PET-PCR assay, Table 2.
Discussion
The Illumigene Malaria LAMP assays are capable of detecting malaria infections at the genus level with analytical sensitivity (LoD) equal to (SFP assay) or below (GFP) the WHO recommended 2 parasites/μl11 while using two simple sample preparation procedures. Results were obtained in less than one hour, including the sample preparation steps. This report compared the performance of Illumigene Malaria LAMP to the PET-PCR assay, a real-time PCR assay commonly used in research or reference labs. Not surprisingly, both SFP and GFP assays, like the reference test, PET-PCR assay, detected more positive samples than microscopy, the gold standard diagnostic test in many malaria endemic countries. The analytical sensitivity of the GFP assay was about 7 fold more than that of the simpler SFP assay, providing a much lower LoD of 0.3 parasites/μL than the SFP assay (2 parasites/μL). Indeed, this could explain the fact that the GFP assay detected 4 samples as positive that both the SFP and PET-PCR did not detect, as shown in Table 2. This was not surprising given that the GFP assay provides a cleaner DNA preparation due to the additional column purification step not found in the simpler Illumigene Malaria method. Nonetheless, the parasite detection limits observed for the two sample preparation methods implies that these assays are capable of detecting low density infections below the detection limits of both microscopy and RDTs.
The PET-PCR assay detected as positive four samples that both the GFP and SFP did not identify as positive. This raises the question as to whether these were false positive samples by PET-PCR or if these were indeed positive samples that were missed by both the LAMP assays. The fact that these samples had high Ct (Table 2) indicate that, if these were indeed positive samples, they have very low parasite densities. These observations are not entirely surprising given that similar inconsistencies in PCR replicates of low parasitemia samples have been demonstrated2,12. The reproducibility of PCR assays in the detection of samples with very low parasitemia was shown to alternate between positive and negative in about 38% of PCR replicates tested12. Therefore, it is very possible that these were indeed positive samples of low parasitemia which if retested with the LAMP assays would probably give positive results however, we also cannot rule out false positivity by PET-PCR.
Sub-microscopic infections have been shown to occur in all transmission settings and the use of microscopy for epidemiological studies greatly underestimates the prevalence of malaria infections13. It is important that low density infections are detected, as they have been shown to contribute to as much as 20–50% of all human to mosquito transmission in very low transmission settings14. Several studies have demonstrated that molecular assays are more sensitive at detecting low density infections, often missed by microscopy15,16,17. The need to detect even asymptomatic low density infections in the wake of calls to eliminate malaria has led to the development of simple field-adaptable molecular assays for parasites detection. Our results demonstrate that theIllumigene Malaria LAMP assays are comparable in sensitivity and specificity to a real-time PCR assay (PET-PCR) which is more technically challenging. The LAMP technique, unlike many other molecular tests, is well suited for field laboratory use as it does not require a thermal cycler. Indeed, in this study, the LAMP assays were performed in a clinical laboratory in a field setting. Results from this evaluation clearly demonstrate that the Illumigene Malaria LAMP assays are as sensitive as the reference test and therefore can be useful in the detection of asymptomatic cases that are often sub-microscopic. However, the described evaluation was not designed to address the utility of this test for detecting asymptomatic infection in field survey as the main objective of this first evaluation was to determine the performance of this test in a clinical laboratory setting in a malaria endemic country by comparing with microscopic diagnosis and a reference molecular test. Therefore, future studies aimed at evaluating these assays for detection of asymptomatic cases in both low and high transmission settings are warranted.
Several malaria LAMP assays have been described2,3,6,7,9,18,19,20,21,22,23,24. However, to date, the only truly field deployment commercial LAMP kits that we are aware of are the Loopamp MALARIA kit (Eiken Chemical Co)2,25,26 and the Illumigene Malaria LAMP described here. Both of these LAMP platforms address the challenges associated with the field deployment of many molecular tests such as simplification of sample preparation from blood, reagent stability under ambient conditions, and ease-of-use for the end user, making it easier to deploy sensitive molecular assays in resource limited laboratory settings. By way of differences, the “PURE” sample preparation method utilized in the Loopamp MALARIA kit (Eiken Chemical Co) requires a 5-minutes heating step and the use of a series of interlocking tubes which is unlike the straightforward simpler methods utilized in the Illumigene Malaria LAMP. Additionally, the amplification and readout steps in the Illumigene Malaria LAMP are both performed in one platform resulting in an objective “positive” or “negative” readout similar to the use of a turbidimeter, in the Loopamp MALARIA kit (Eiken Chemical Co).
The current recommendations for case management of suspected malaria cases and passive case detection, even in low transmission settings, are still microscopy and quality-assured RDTs11. The objective of this test evaluation was not to change this recommendation for primary diagnosis but to demonstrate the feasibility and utility of simpler molecular assays such as LAMP assays for diagnosis of malaria in a point of care clinical laboratory setting. The results of this evaluation demonstrates that this test can improve the detection limit of the diagnostic test at point of care as they would allow for the detection of cases missed by microscopy and RDTs as demonstrated in our study. The increased sensitivity of this molecular test is certainly valuable for case management in non-endemic countries as most of the patients may be non-immune to malaria and this test can help to treat cases that will be missed by current standard primary diagnostic tests. However, the utility of this test for case management in an endemic setting will require further consideration from ministries of health and World Health Organization and their recommendations for appropriate use. Nevertheless, this new sensitive test provides opportunities for other use as the malaria control ecosystem includes several different operational scenarios which call for more sensitive detection tools. These include 1) epidemiological surveys in which a large proportion of sub-microscopic cases are missed, 2) elimination-certification process where finding the last parasite is necessary, in the detection of asymptomatic cases and in reactive case detection studies such as mass screen and treat (MSaT), 3) focal screen and treat (FSaT) studies in which individuals are screened with (FSaT) or without (MSaT) identification of an index case and the positive cases are treated11 and 4) in follow up tests post- treatment or in vaccine trials. All these scenarios require highly sensitive tests and the Illumigene Malaria LAMP assays provides such a test due to its impressive limit of detection. However, like many other malaria LAMP platforms reported to date, the Illumigene Malaria LAMP assays can test a limited number of samples per run. Therefore, scenarios that require the testing of a large number of samples may require other platforms such as the recently described colorimetric LAMP assays9,10 with the limitation that these high-throughput colorimetric malaria LAMP assays still require sample preparation and lyophilized reagents for ease of use in the field. As technology advances, it is possible to envision the possibility of adapting the Illumigene reader to facilitate the testing of larger sample size.
Simpler sample collection methods such as the use of a finger prick blood and filter papers are preferable in field settings in resource limited regions. A limitation of this study is the fact that a venous blood collection was used, however, this does not mean that this is the recommended sample collection method for use with the Illumigene Malaria LAMP assays and while we did not evaluate the use a finger prick sample in our study, we do not see any scientific reason why such a sample collection method would not work with the LAMP assays described here which require only 50 μL of blood.
The Illumigene Malaria LAMP kit described here is designed to detect parasites of the Plasmodium genus and would serve as a screening test for malaria parasites infections. However, the development of species specific primers for species identification, is easily achievable. Several malaria LAMP assays have been described capable of detecting both the Plasmodium genus as well as the different human infecting species3,5,6,7,8,27. The need to identify the infecting species is important in situations where treatment is required post testing, in which case species identification is necessary in order to provide the correct antimalarial and in providing valuable information on the burden and relative distribution of malaria species. Nonetheless, a genus-specific assay has utility in studies that monitor and evaluate malaria control programs in which species identification might not be absolutely necessary. Furthermore, in a clinical setting, a simple, highly accurate, genus-specific LAMP assay has the ability to eliminate the need for significant expertise, training, and experience associated with microscopy, and can be an excellent safeguard against possible false-negative results associated with conventional tests optimized for detecting higher density symptomatic infections.
In conclusion, the Illumigene Malaria LAMP assays can be used reliably for the detection of Plasmodium in a simple low-tech but sensitive assay format providing a much needed alternative to more complex molecular tests for malaria diagnosis. Additionally, introducing innovative diagnostics like Illumigene Malaria LAMP eliminates challenges associated with conventional molecular tests and provides new opportunities to diagnose malaria in point of care settings in non-endemic and in endemic settings. Given the impressive low limits of detection and ease of use of these assays, it is reasonable to assume that these assays can provide sensitive options for the detection of asymptomatic cases in elimination settings; however, this requires appropriate field evaluations for such use.
Methods
Ethics
The study protocol was approved by the National Ethics Committee for Health Research, of the Republic of Senegal before participant recruitment and sample collection were initiated. CDC investigators did not participate in specimen collection or interact with study subjects and did not have access to personal identifying information. Therefore, their participation was determined to be non-engaged in human subjects’ research under CDC human subjects’ protections procedures. All participants, or their parents or guardians, provided written informed consent. All the methods were carried out in accordance with the approved guidelines.
Study site, participants and sample collection
The study was conducted between September and December, 2015 in Hospital A. LeDantec Laboratoire de Parasitologie in Dakar, Senegal. Study participants were selected from health clinics in hypoendemic settings in Pikine, Rufisque and Thies, using the following criteria: patient age of ≥3 years, presence of fever at time of enrollment, or history of fever during the 48 previous hours, absence of severe illnesses and willingness to participate in the study, and consenting. The test plan was designed to evaluate the performance of both prospective and archived EDTA treated blood samples from symptomatic patients. Retrospective samples were collected previously, tested by microscopy and stored frozen (≤−20 °C) until testing with Illumigene LAMP assays. For the prospective arm, a 5 mL volume of venous whole blood was collected in EDTA tubes and used to prepare both thick and thin blood smears for microscopy.
Illumigene Malaria LAMP Assays
The Illumigene Malaria LAMP assay consist of two main steps: a sample preparation step and an amplification step, Fig. 1. Two centrifuge-free sample preparation methods were designed to extract DNA from whole blood collected in EDTA as anticoagulant: 1) a simple filtration method (Illumigene Malaria, herein referred to as SFP for simple filtration prep as shown in Fig. 1a) and a 7–10 minutes gravity-driven gel filtration method (Illumigene Malaria PLUS; herein referred to as GFP for gravity-driven filtration prep as shown in Fig. 1b). All the reagents and supplies are kept at room temperature. A blood sample is mixed with the provided lysis buffer and the lysate transferred to either SFP or GFP columns as described in Fig. 1. The collected eluates from each sample preparation were directly added to the Illumigene Malaria test device consisting of lyophilized LAMP reagents. The lyophilized reagents in the LAMP device consist of the primers targeting the Plasmodium mitochondrial genome and the other necessary components including dNTPs and Bst DNA Polymerase to perform the LAMP assay. The control tube consist of LAMP reaction components and Bst Polymerase with primers to detect the housekeeping human gene, NADH dehydrogenase subunit 1. The design of this control supports that the whole blood extraction process step was performed correctly and identifies any potential sample inhibition.
The clinical trial site in Senegal utilized a full production lot of Illumigene Malaria LAMP kits that were labeled for Investigational Use Only (IUO). The kits, the illumipro-10™ Incubator/Reader, and record sheets were shipped to the test site at the beginning the study. All tests were performed using the illumipro-10™ incubator Reader, installed with Software version 2.00:602 and an IUO Malaria Assay protocol. External controls consisting of a known positive sample (Meridian Bioscience Inc. (Cincinnati, OH) and known non-malaria human blood were run on each day of patient testing. These samples were processed in the same manner as the patient samples. The runs were considered valid if the control test tube gave a positive result and if all the other controls gave the expected results. A qualitative result (positive, negative or invalid) was printed after every run.
Microscopy
Thick and thin blood smears were prepared in the field for microscopy reading at the Laboratory of Parasitology and Mycology at Cheikh Anta Diop University (UCAD), A. Le Dantec Hospital in Dakar, Senegal. The blood smears were stained with 10% Giemsa for 10 minutes using WHO procedures http://www.who.int/malaria/publications/atoz/9241547820/en/. A thick blood smear was considered negative when the examination of 300 high power fields did not reveal asexual parasites or gametocytes. Parasite densities were calculated by counting the number of asexual parasites per 200 leukocytes (or per 500, if the count is less than 100 parasites or gametocytes per 200 leukocytes), assuming a leukocyte count of 8,000/μl. For quality control, all slides were read by two expert microscopists and a third microscopist settled any discrepant readings.
Cross-reactivity and inclusivity studies
Cross reactivity studies were performed by Meridian during their primer/assay validation phase. This was tested using the five human-infecting Plasmodium spp. P. falciparum, P. vivax, P. malariae, P. ovale and P. knowlesi DNA (obtained from the CDC) and negative human whole blood specimens inoculated with non-Plasmodium organisms including bacterial or fungal organisms to a minimum concentration of 1.0 × 106 CFU/mL, virus at a minimum of 1.0 × 105 TCID50/mL, or protozoans to a minimum concentration of 1.0 × 105 organisms/mL. Where whole organisms were not available, 1.0 × 106 copies/mL for genomic DNA were tested. The following organisms were evaluated: Babesia microti, Borrelia burgdorferi, Haemophilus influenza, Klebsiella pneumoniae, Leishmania donovani, Leishmania infantum, Leptospira interrogans, Mycobacterium smegmatis, Salmonella typhi, Staphylococcus aureus, Staphylococcus epidermidis, Streptococcus pneumoniae, Treponema pallidum, Trypanosoma cruzi, Trypanosoma rangeli, Vibrio parahaemolyticus, Cytomegalovirus (CMV), Epstein-Barr virus (EBV), Hepatitis B virus, Hepatitis C virus, Herpes simplex virus 1 (HSV 1), HIV-1, Human Papilloma Virus (HPV), and Rubella virus. In addition, the following organisms were evaluated through in silico analysis since the organism or their DNA could not be obtained for testing: Anaplasma phagocytophilium, Clostridium botulinum, Orientia tsutsugamushi, Rickettsia conorii, Rickettsia rickettsii, Rickettsia typhi, Chikungunya virus, Dengue virus (types 1–4), West Nile virus, and Yellow Fever virus. Human genomic DNA was also tested at 1.0 × 106 copies/mL.
Determination of the Analytical Sensitivity
Limit of Detection (LoD) of the two sample preparation methods was also determined by Meridian during their primer/assay validation phase. Both P. falciparum (3D7 strain) and P. vivax (India VII strain) samples, obtained from the CDC, were utilized. At least twenty replicates were tested at different concentrations with both SFP and GFP methods. A minimum of 20 valid results per dilution were used to determine the LoD using a statistically-based methodology which allows for the determination of LoD with a 95% confidence interval. LoD was calculated using a linear logistic model that assesses the relationship between the probability of the response and the parasite concentration. In addition, a lyophilized P. falciparum WHO standard (National Institute for Biological Standards, Hertfordshire, England) was used to determine the LoD of the assays. The sample was reconstituted in sterile water and different dilutions, in International Units/mL, were made in uninfected human whole blood. Twenty replicates of appropriate dilutions were tested with SFP and GFP. LoD was defined as the lowest parasite concentration detected at a 95% confidence level.
PET-PCR assay
Two dried blood spots were spotted with EDTA preserved blood from each of the clinical samples and stored at 4 °C. One of the dried blood spot was shipped to CDC, Atlanta for evaluation using the Plasmodium PET-PCR assay. DNA was extracted using the QIAamp blood kit (QIAGEN, Inc., Chatsworth, CA) according to the manufacturer’s instructions and stored at 4 °C until processed. Each sample was tested once. Briefly, the Plasmodium PET-PCR reaction was performed in a 20 μl reaction containing 2X TaqMan Environmental Master Mix 2.0 (Applied BioSystems), 250 nM each forward and reverse primer for Plasmodium genus and 2 μl of DNA template. The reactions were performed under the following cycling parameters: initial hot-start at 95 °C for 15 minutes, followed by 45 cycles of denaturation at 95 °C for 20 seconds, annealing at 60 °C for 40 seconds. Samples with a CT value of 40.0 or below were considered positive.
Statistics
The sensitivity and specificity of Illumigene Malaria LAMP assays was calculated using both microscopy and PET-PCR as reference tests. The percentage specificity and sensitivity were calculated using the formulae shown below:


Probit analysis was used to determine the LoD for each Illumigene Malaria LAMP assay. The LoDs were calculated using a linear logistic model that assesses the relationship between the probability of the response and the parasite density (parasites/μL). Data were entered into Microsoft Excel 2010 (Microsoft, Redmond, WA) and analysed using SPSS software, version 18 (SPSS Inc., Chicago, IL, USA). Precision of the estimates was determined by calculating exact 95% confidence intervals for each test statistic.
Additional Information
How to cite this article: Lucchi, N. W. et al. Evaluation of the illumigene Malaria LAMP: A Robust Molecular Diagnostic Tool for Malaria Parasites. Sci. Rep. 6, 36808; doi: 10.1038/srep36808 (2016).
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Notomi, T. et al. Loop-mediated isothermal amplification of DNA. Nucleic Acids Res 28, E63 (2000).
Hopkins, H. et al. Highly sensitive detection of malaria parasitemia in a malaria-endemic setting: performance of a new loop-mediated isothermal amplification kit in a remote clinic in Uganda. The Journal of infectious diseases 208, 645–652, doi: 10.1093/infdis/jit184 (2013).
Lucchi, N. W. et al. Real-time fluorescence loop mediated isothermal amplification for the diagnosis of malaria. PloS one 5, e13733, doi: 10.1371/journal.pone.0013733 (2010).
Sema, M. et al. Evaluation of non-instrumented nucleic acid amplification by loop-mediated isothermal amplification (NINA-LAMP) for the diagnosis of malaria in Northwest Ethiopia. Malaria journal 14, 44, doi: 10.1186/s12936-015-0559-9 (2015).
Britton, S. et al. Sensitive Detection of Plasmodium vivax Using a High-Throughput, Colourimetric Loop Mediated Isothermal Amplification (HtLAMP) Platform: A Potential Novel Tool for Malaria Elimination. PLoS neglected tropical diseases 10, e0004443, doi: 10.1371/journal.pntd.0004443 (2016).
Han, E. T. et al. Detection of four Plasmodium species by genus- and species-specific loop-mediated isothermal amplification for clinical diagnosis. Journal of clinical microbiology 45, 2521–2528 (2007).
Patel, J. C. et al. Real-time loop-mediated isothermal amplification (RealAmp) for the species-specific identification of Plasmodium vivax. PloS one 8, e54986, doi: 10.1371/journal.pone.0054986 (2013).
Yamamura, M., Makimura, K. & Ota, Y. Evaluation of a new rapid molecular diagnostic system for Plasmodium falciparum combined with DNA filter paper, loop-mediated isothermal amplification, and melting curve analysis. Japanese journal of infectious diseases 62, 20–25 (2009).
Britton, S., Cheng, Q., Sutherland, C. J. & McCarthy, J. S. A simple, high-throughput, colourimetric, field applicable loop-mediated isothermal amplification (HtLAMP) assay for malaria elimination. Malaria journal 14, 335, doi: 10.1186/s12936-015-0848-3 (2015).
Lucchi, N. W., Ljolje, D., Silva-Flannery, L. & Udhayakumar, V. Use of Malachite Green-Loop Mediated Isothermal Amplification for Detection of Plasmodium spp. Parasites. PloS one 11, e0151437, doi: 10.1371/journal.pone.0151437 (2016).
WHO Evidence Review Group on Malaria Diagnosis in Low Transmission Settingshttp://www.who.int/malaria/mpac/mpac_mar2014_diagnosis_low_transmission_settings_report.pdf (2014).
Costa, D. C. et al. Submicroscopic malaria parasite carriage: how reproducible are polymerase chain reaction-based methods? Memorias do Instituto Oswaldo Cruz 109, 21–28, doi: 10.1590/0074-0276140102 (2014).
Okell, L. C., Ghani, A. C., Lyons, E. & Drakeley, C. J. Submicroscopic infection in Plasmodium falciparum-endemic populations: a systematic review and meta-analysis. The Journal of infectious diseases 200, 1509–1517, doi: 10.1086/644781 (2009).
Okell, L. C. et al. Factors determining the occurrence of submicroscopic malaria infections and their relevance for control. Nat Commun 3, 1237, doi: 10.1038/ncomms2241 (2012).
Golassa, L., Enweji, N., Erko, B., Aseffa, A. & Swedberg, G. Detection of a substantial number of sub-microscopic Plasmodium falciparum infections by polymerase chain reaction: a potential threat to malaria control and diagnosis in Ethiopia. Malaria journal 12, 352, doi: 10.1186/1475-2875-12-352 (2013).
Harris, I. et al. A large proportion of asymptomatic Plasmodium infections with low and sub-microscopic parasite densities in the low transmission setting of Temotu Province, Solomon Islands: challenges for malaria diagnostics in an elimination setting. Malaria journal 9, 254, doi: 10.1186/1475-2875-9-254 (2010).
Talundzic, E. et al. Field evaluation of the photo-induced electron transfer fluorogenic primers (PET) real-time PCR for the detection of Plasmodium falciparum in Tanzania. Malaria journal 13, 31, doi: 10.1186/1475-2875-13-31 (2014).
Patel, J. C. et al. Field Evaluation of a Real-Time Fluorescence Loop-Mediated Isothermal Amplification Assay, RealAmp, for the Diagnosis of Malaria in Thailand and India. The Journal of infectious diseases, doi: 10.1093/infdis/jiu252 (2014).
Polley, S. D. et al. Mitochondrial DNA targets increase sensitivity of malaria detection using loop-mediated isothermal amplification. Journal of clinical microbiology 48, 2866–2871, doi: 10.1128/JCM.00355-10 (2010).
Cook, J. et al. Loop-mediated isothermal amplification (LAMP) for point-of-care detection of asymptomatic low-density malaria parasite carriers in Zanzibar. Malaria journal 14, 43, doi: 10.1186/s12936-015-0573-y (2015).
Han, E. T. Loop-mediated isothermal amplification test for the molecular diagnosis of malaria. Expert review of molecular diagnostics 13, 205–218, doi: 10.1586/erm.12.144 (2013).
Sema, M. et al. Evaluation of non-instrumented nucleic acid amplification by loop-mediated isothermal amplification (NINA-LAMP) for the diagnosis of malaria in Northwest Ethiopia. Malaria journal 14, 44, doi: 10.1186/s12936-015-0559-9 (2015).
Morris, U. et al. Field deployment of loop-mediated isothermal amplification for centralized mass-screening of asymptomatic malaria in Zanzibar: a pre-elimination setting. Malaria journal 14, 205, doi: 10.1186/s12936-015-0731-2 (2015).
Oriero, E. C., Jacobs, J., Van Geertruyden, J. P., Nwakanma, D. & D’Alessandro, U. Molecular-based isothermal tests for field diagnosis of malaria and their potential contribution to malaria elimination. The Journal of antimicrobial chemotherapy 70, 2–13, doi: 10.1093/jac/dku343 (2015).
Polley, S. D. et al. Clinical evaluation of a loop-mediated amplification kit for diagnosis of imported malaria. The Journal of infectious diseases 208, 637–644, doi: 10.1093/infdis/jit183 (2013).
Aydin-Schmidt, B. et al. Loop mediated isothermal amplification (LAMP) accurately detects malaria DNA from filter paper blood samples of low density parasitaemias. PloS one 9, e103905, doi: 10.1371/journal.pone.0103905 (2014).
Lau, Y. L. et al. Specific, sensitive and rapid detection of human plasmodium knowlesi infection by loop-mediated isothermal amplification (LAMP) in blood samples. Malaria journal 10, 197, doi: 1475-2875-10-197 [pii]10.1186/1475-2875-10-197 (2011).
Acknowledgements
We would like to thank Mbaye Pene, Mbaye Thiam, Ngayo Sy, Younouss Diedhiou, Amadou Mactar Mbaye, Guete Diallo, Daba Zoumarou, Nana Fatoumata Diop, Anna Seck, and the patients and health staff from Deggo (Pikine), Health facility, Hopital Youssou Mbargan. This report was made possible through support provided by the Malaria Branch at the Centers for Disease Control and Prevention and the Atlanta Research and Education Foundation. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
Author information
Authors and Affiliations
Contributions
N.W.L., D.N., V.U. and J.W.B. contributed to the conception and design of the study. D.N. provided technical support in field and was responsible for supervision of the study and laboratory work in Senegal. M.G., M.A.D., A.B.D., A.B., Y.D.N. collected the LAMP data in Senegal including patient enrolment, sample processing and microscopy. N.W.L., D.L. and I.G. performed the DNA extraction and carried out the PET-PCR assays and V.U. and J.W.B. supervised the laboratory assays in the CDC laboratory. N.W.L., M.G., D.N. and V.U. drafted the manuscript and N.W.L. performed the analysis. All authors have read and approved the final manuscript.
Ethics declarations
Competing interests
All the supplies and reagents (including the LAMP kits) for this evaluation were provided by Meridian Inc. Meridian also covered the field operational costs for this evaluation.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Lucchi, N., Gaye, M., Diallo, M. et al. Evaluation of the Illumigene Malaria LAMP: A Robust Molecular Diagnostic Tool for Malaria Parasites. Sci Rep 6, 36808 (2016). https://doi.org/10.1038/srep36808
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep36808
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.