Abstract
The α7 subtype of nicotinic acetylcholine receptor (nAChR) plays a role in the inflammation which is implicated in depression. This study was undertaken to examine the role of α7 nAChR in depression using α7 nAChR knock-out (KO) mice. Serum levels of tumor necrosis factor-α and interlukin-1β in KO mice were higher than wild-type mice, suggesting an inflammatory process in KO mice. α7 nAChR KO mice showed depression-like phenotype. Furthermore, KO mice showed increased brain-derived neurotrophic factor (BDNF) and its receptor TrkB signaling, as well as increased synaptogenesis and spine density in the nucleus accumbens (NAc), although BDNF-TrkB signaling and synaptogenesis were not altered in the prefrontal cortex and hippocampus. Systemic administration of the TrkB antagonist ANA-12, but not the TrkB agonist 7,8-dihydroxyflavone and the selective serotonin reuptake inhibitor fluoxetine, showed a rapid antidepressant effect in KO mice by normalizing increased synaptogenesis in the NAc. In addition, bilateral infusion of ANA-12 into NAc promoted a rapid antidepressant effect in KO mice by normalizing increased synaptogenesis in the NAc. These findings suggest that increased BDNF-TrkB signaling and synaptogenesis in the NAc by deletion of α7 nAChR plays a key role in depression.
Similar content being viewed by others
Introduction
Depression is one of the most common psychiatric disorders in the world. Although the precise mechanism underlying the pathophysiology of depression is unknown, accumulating evidence suggests that inflammation plays a crucial role in depression1,2,3,4,5,6. Meta-analyses show higher blood levels of pro-inflammatory cytokines, such as tumor necrosis factor (TNF)-α and interleukin-6 (IL-6), in drug-free depressed patients, compared with healthy controls7,8. In addition, a study on postmortem brains revealed elevated gene expression of pro-inflammatory cytokines in the frontal cortex of subjects with a history of major depression9. These findings suggest that both peripheral and central inflammation, are associated with depressive symptoms.
Nicotinic acetylcholine receptors (nAChRs) may play a role in the pathophysiology of depression. It is reported that both pharmacological and molecular genetic studies show decreases in hippocampal acetylcholinesterase activity increased anxiety and depression-like behaviors and decreased resilience to repeated stress in a social defeat paradigm10, suggesting that abnormalities in the cholinergic system may be critical for the etiology of depression. However, the precise mechanisms underlying the role of nAChRs in depression are not understood11,12,13,14. It is known that the α7 subtype of the nAChR regulates the so-called cholinergic ascending anti-inflammatory pathway, in which activation of the vagus nerve diminishes inflammation through decreased peripheral macrophage activity15,16,17,18,19. Given the role of α7 nAChR in inflammation, it is of great interest to study the role of α7 nAChR in depression associated with inflammation.
Although the pathophysiology of depression remains enigmatic, brain-derived neurotrophic factor (BDNF) and its specific receptor, tropomyosin-receptor-kinase B (TrkB), plays a key role in depression, as well as the therapeutic mechanisms of antidepressants20,21,22,23,24,25,26. Preclinical studies suggest that BDNF acts within the ventral tegmental area (VTA) – nucleus accumbens (NAc) pathway, to induce a depression-like phenotype, whereas it produces antidepressant-like effects in the prefrontal cortex (PFC) and hippocampus6,27,28,29,30,31,32,33,34. Currently, there are no reports showing the relationship between α7 nAChR and BDNF–TrkB signaling in depression.
The purpose of this study is to examine whether α7 nAChR plays a role in the pathophysiology of depression. First, we examined whether α7 nAChR knock-out (KO) mice show depression-like phenotype and inflammation. Second, the role of BDNF–TrkB signaling and synaptogenesis in the selected brain regions from α7 nAChR KO mice was examined. Finally, the effects of TrkB agonist 7,8-dihydroxyflavone (7,8-DHF)35, TrkB antagonist ANA-1236, and selective serotonin reuptake inhibitor (SSRI) fluoxetine in depression-like phenotype of α7 nAChR KO mice were examined.
Results
Depression -like phenotype and inflammation of α7 nAChR KO mice
Locomotion was no difference between two groups (P = 0.989) (Fig. 1a). In the tail-suspension test (TST) and forced swimming test (FST), the immobility times of α7 nAChR KO mice were significantly (TST: P = 0.042; FST: P = 0.001) higher than those of wild-type (WT) mice (Fig. 1b,c). In the 1% sucrose preference test (SPT), the preference of α7 nAChR KO mice was significantly (P = 0.022) lower than that of WT mice (Fig. 1d), indicative of anhedonia. These data suggest that deletion of α7 nAChR gene causes depression-like phenotypes including anhedonia.
Depression-like phenotypes, and inflammation in α7 nAChR KO mice.
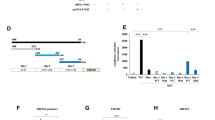
(a) locomotion, (b): tail-suspension test (TST), (c): forced swimming test (FST), (d): 1% sucrose preference test (SPT). Data represent the mean ± S.E.M. (n = 8 or 9). (e): Dexamethasone (DEX) suppression test. Data represent the mean ± S.E.M. (n = 8 or 9). (f): Serum levels of TNF-α. Data represent the mean ± S.E.M. (n = 11). (g): Serum levels of IL-1β. Data represent the mean ± S.E.M. (n = 7 or 8). (h): Serum levels of IL-6. Data represent the mean ± S.E.M. (n = 12 or 13). *P < 0.05, **P < 0.01 compared with the WT group (Student t-test). N.S.: not significant.
The dexamethasone (DEX) suppression test is an effective way of quantifying dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis, a system involved in depression33,37,38. Serum corticosterone levels in α7 nAChR KO mice were significantly (P = 0.039) higher than those in WT mice six hours after DEX injection (0.1 mg/kg) (Fig. 1e), indicating HPA axis hyperactivity in KO mice. Furthermore, serum levels of TNF-α (P = 0.023) (Fig. 1f) and interlukin-1β (IL-1β) (P = 0.016) (Fig. 1g), but not IL-6 (P = 0.911) (Fig. 1h), in KO mice were significantly higher than those of WT mice, indicating an enhanced inflammatory process in α7 nAChR KO mice.
Increased BDNF-TrkB signaling and synaptogenesis in the NAc of α7 nAChR KO mice
Using Western blot analysis, we examined levels of BDNF and its precursor proBDNF in different brain regions since BDNF-TrkB signaling plays a key role in depression-like phenotype6,27,28,29,30,31,32,33,34. Levels of proBDNF in the NAc of α7 nAChR KO mice were significantly (P < 0.001) lower than those of WT mice, whereas levels of mature BDNF in the NAc of KO mice were significantly (P = 0.048) higher than those of WT mice (Fig. 2a,b). Both proBDNF and BDNF levels in other brain regions, including CA1, CA3, DG and PFC, remained the same (Fig. 2a,b). Furthermore, the ratio of phosphor-TrkB to total TrkB in the NAc of KO mice was also significantly (P = 0.002) higher than that of WT mice although the ratio in other regions was not altered (Fig. 2c).
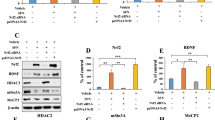
Increased BDNF-TrkB signaling in the NAc of α7 nAChR KO mice.
(a,b): Levels of proBDNF and BDNF in the CA1, CA3, DG, PFC, and NAc. Data represent the mean ± S.E.M. (n = 5 or 6). (c): The ratio of phosphor-TrkB to total TrkB. Data represent the mean ± S.E.M. (n = 6). (d,e): Levels of GluA1 and PSD-95 in the CA1, CA3, DG, PFC, and NAc. Data represent the mean ± S.E.M. (n = 5 or 6). *P < 0.05, **P < 0.01 and ***P < 0.001 compared with the WT group (Student t-test). See the supplemental material 1 for the data of Western blot analyses.
Next, we measured the markers for synaptogenesis. Levels of the AMPA receptor 1 (GluA1) and postsynaptic density protein 95 (PSD-95) in the NAc of α7 nAChR KO mice were significantly (GluA1: P = 0.027, PSD-95: P = 0.025) higher than those of WT mice, although levels of GluA1 and PSD-95 in other regions were unaltered (Fig. 2d,e).
Increased dendritic spine density in the NAc of α7 nAChR KO mice
Changes in dendritic length and spine density in the brain is thought to contribute to the neurobiology of depression, and antidepressant treatment is mediated, in part, by blocking or reversing these changes33,39,40,41. It is, therefore, of interest to examine whether the spine density is altered in the brain regions from α7 nAChR KO mice. Spine density in the CA1, CA3, DG and mPFC (prelimbic and infralimbic areas) was not altered (Fig. 3a,b). In contrast, the spine density in the core and shell of NAc in KO mice was significantly (shell: P = 0.015, core: P = 0.028) higher than that of WT mice (Fig. 3c).
Antidepressant effect by systemic administration of ANA-12
Since increased BDNF-TrkB signaling in the NAc was shown in α7 nAChR KO mice, we examined whether the TrkB antagonist ANA-1231,33,34,36,42,43,44 could confer antidepressant effects in KO mice. A single dose of ANA-12 (0.5 mg/kg, i.p.) was no effect on locomotion (Fig. 4a). In both the TST and FST, ANA-12 significantly attenuated the increased immobility time of KO mice. Two-way ANOVA analysis revealed significant effects (TST: genotype: F(1,36) = 12.68, P = 0.001, treatment: F(1,36) = 10.46, P = 0.003, interaction: F(1,36) = 7.923, P = 0.008; FST: genotype: F(1,36) = 10.221, P = 0.003, treatment: F(1,36) = 7.723, P = 0.009, interaction: F(1,36) = 0.179, P = 0.675) (Fig. 4b,c). Furthermore, ANA-12 significantly attenuated the reduced sucrose preference of KO mice. Two-way ANOVA analysis revealed significant effects (genotype: F(1,37) = 19.87, P < 0.001, treatment: F(1,37) = 9.876, P = 0.003, interaction: F(1,37) = 7.112, P = 0.012) (Fig. 4d).
Antidepressant effect of ANA-12, a TrkB antagonist.
(a): Locomotion, (b): TST, (c): FST, (d): SPT. Data represent the mean ± S.E.M. (n = 8–10). (e): proBDNF, (f): BDNF, (g): p-TrkB/TrkB ratio, (h): GluA1, (i): PSD-95. Data represent the mean ± S.E.M. (n = 5 or 6). *P < 0.05, **P < 0.01, ***P < 0.001 compared with the WT or KO group (two-way ANOVA). N.S.: not significant. See the supplemental material 2 for the data of Western blot analyses.
Treatment with ANA-12 did not alter protein levels of proBDNF or BDNF in the NAc of all groups (Fig. 4e,f). However, treatment with ANA-12 significantly attenuated the increased ratio of phospho-TrkB to total TrkB in the NAc of α7 nAChR KO mice. Two-way ANOVA analysis revealed significant effects (genotype: F(1,22) = 8.299, P = 0.010, treatment: F(1,22) = 19.28, P < 0.001, interaction: F(1,22) = 9.979, P = 0.005) (Fig. 4g). In addition, ANA-12 significantly attenuated the increased levels of GluA1 and PSD-95 in the NAc of the KO mice. Two-way ANOVA analysis of GluA1 data revealed significant effects (genotype: F(1,22) = 4.832, P = 0.041, treatment: F(1,22) = 7.574, P = 0.013, interaction: F(1,22) = 7.929, P = 0.011). Furthermore, two-way ANOVA analysis of PSD-95 data revealed significant effects (genotype: F(1,22) = 10.26, P = 0.005, treatment: F(1,22) = 9.531, P = 0.006, interaction: F(1,22) = 21.81, P < 0.001) (Fig. 4h,i).
In contrast, a single administration with 7,8-dihydroxyflavone (7,8-DHF; 10 mg/kg), a TrkB agonist and selective serotonin reuptake inhibitor (SSRI) fluoxetine (10 mg/kg)31,33,34,35,42,43,44,45, did not produce antidepressant effects in these mice in TST, FST and 1% SPT (Fig. 5a–h).
Effects of 7,8-DHF and fluoxetine in α7 nAChR KO mice.
(a,e): locomotion, (b,f): TST, (c,g): FST, (d,h): SPT): The TrkB agonist 7,8-DHF and SSRI fluoxetine did not show antidepressant effects in α7 nAChR KO mice. Data represent the mean ± S.E.M. (n = 12–14). *P < 0.05, **P < 0.01 compared with the vehicle-treated WT group (two-way ANOVA). N.S.: not significant.
Antidepressant effect by bilateral infusion into NAc of ANA-12
In order to confirm the role of increased BDNF-TrkB signaling in the NAc of α7 nAChR KO mice, ANA-12 (0.1 nmol/L, 0.1 μL/min for 5 min) was injected bilaterally into NAc shell of WT or KO mice (Fig. 6a). There was no change in locomotion among four groups (Fig. 6b). Bilateral infusion of ANA-12 significantly attenuated the increased immobility time of KO mice in both TST and FST. Two-way ANOVA analysis revealed significant effects (TST: genotype: F(1,33) = 6.067, P = 0.020, treatment: F(1,33) = 4.852, P = 0.035, interaction: F(1,33) = 4.578, P = 0.041; FST: genotype: F(1,34) = 4.911, P = 0.034, treatment: F(1,34) = 4.390, P = 0.044, interaction: F(1,34) = 3.665, P = 0.065) (Fig. 6c,d). Furthermore, ANA-12 significantly attenuated the reduced sucrose preference of KO mice. Two-way ANOVA analysis revealed significant effects (genotype: F(1,34) = 22.431, P < 0.001, treatment: F(1,34) = 6.809, P = 0.014, interaction: F(1,34) = 7.749, P = 0.009) (Fig. 6e).
Antidepressant effects of bilateral injection of ANA-12 into NAc shell.
(a): Scheme of bilateral injection of ANA-12 into NAc shell. (b): Locomotion, (c): TST, (d): FST, (e): SPT. Data represent the mean ± S.E.M. (n = 8 or 9). (f): proBDNF, (g): BDNF, (h): p-TrkB/TrkB ratio, (i): GluA1, (j): PSD-95. Data represent the mean ± S.E.M. (n = 6). *P < 0.05, **P < 0.01, ***P < 0.001 compared with the vehicle-treated KO group (two-way ANOVA). N.S.: not significant. See the supplemental material 2 for the data of Western blot analyses.
Bilateral injection of ANA-12 into NAc-shell of α7 nAChR KO mice did not alter the levels of proBDNF and BDNF in the NAc (Fig. 6f,g). However, bilateral injection of ANA-12 significantly attenuated the increased ratio of phospho-TrkB to total TrkB in the NAc. Two-way ANOVA analysis revealed significant effects (genotype: F(1,23) = 6.032, P = 0.023, treatment: F(1,23) = 27.86, P < 0.001, interaction: F(1,23) = 8.257, P = 0.009) (Fig. 6h). Moreover, bilateral injection of ANA-12 into NAc-shell of α7 nAChR KO mice significantly attenuated the increased levels of GluA1 and PSD-95. Two-way ANOVA analysis of GluA1 data revealed significant effects (genotype: F(1,23) = 9.345, P = 0.006, treatment: F(1,23) = 10.34, P = 0.004, interaction: F(1,23) = 16.89, P = 0.001). Furthermore, two-way ANOVA analysis of PSD-95 data revealed significant effects (genotype: F(1,23) = 16.86, P = 0.001, treatment: F(1,23) = 14.69, P = 0.001, interaction: F(1,23) = 12.90, P = 0.002) (Fig. 6i,j).
Discussion
The present findings support three important conclusions. First, α7 nAChR KO mice showed depression-like phenotype, including anhedonia. Second, serum levels of TNF-α and IL-1β in α7 nAChR KO mice were higher than those of WT mice, indicative of elevated inflammatory processes in KO mice. Third, we found an increased BDNF-TrkB signaling and synaptogenesis in the NAc (but not PFC and hippocampus) of α7 nAChR KO mice. Interestingly, TrkB antagonist ANA-12, but not TrkB agonist 7,8-DHF and SSRI fluoxetine, showed antidepressant-like effect in KO mice. Interestingly, bilateral infusion of ANA-12 into NAc showed antidepressant effect in KO mice. Taken together, it is likely that the increased BDNF-TrkB signaling in the NAc, but not other brain regions, plays a key role in the depression-like behavior of α7 nAChR KO mice.
Inflammation is known to play a role in depression1,2,3,4,5,6. Peripheral administration of the bacterial endotoxin lipopolysaccharide (LPS) can induce depression-like behavior and alteration in serum pro-inflammatory cytokines in mice1,6,46. Anti-inflammatory drugs and antidepressants, including SSRIs and serotonin and norepinephrine reuptake inhibitors (SNRIs) showed antidepressant effects and alteration pro-inflammatory cytokines in mice after LPS administration45,47. These findings suggest that peripheral inflammations are associated with depressive symptoms, and it is therefore highly plausible that anti-inflammatory drugs could ameliorate depressive symptoms. In this study, the serum levels of TNF-α and IL-1β, in α7 nAChR KO mice were significantly higher than those of WT mice, indicating that KO mice have inflammation. Thus, it seems that abnormal pro-inflammatory cytokines levels in the serum of α7 nAChR KO mice may play a causative role in the pathophysiology of depression. Given the role of α7 nAChR in the inflammation17, treatment with anti-inflammatory compounds might show antidepressant effects in α7 nAChR KO mice, although further detailed studies are needed.
Growing evidence reveals that BDNF in the VTA –NAc pathway is integral to the neurobiology of depression27,28,29,30,31,32,33. It was reported that intra-VTA BDNF injections lead to depression-like behavior, while a blockade of BDNF activity in the NAc produced antidepressant effects29. Recently, we reported that inflammation and learned helplessness induced a marked increase in BDNF protein within the NAc, resulting in depression-like behavior in rodents31,32,33,34. Furthermore, we reported that bilateral injections of ANA-12 into the NAc promoted antidepressant effects in LPS-treated mice33 and learned helplessness rats31. A study using postmortem brain samples showed increased BDNF levels in the NAc of depression patients, implying a key role for increased BDNF–TrkB signaling in NAc for the development of depression30. Thus it seems that abnormal BDNF levels in the VTA–NAc pathways play a causative role in the pathophysiology of depression. In this study, we found the increased BDNF–TrkB signaling in the NAc, but not PFC and hippocampus, of α7 nAChR KO mice, and the TrkB antagonist, ANA-12, but not the TrkB agonist 7,8-DHF, conferred an antidepressant effects by normalizing increased synaptogenesis in the NAc. Furthermore, we found that fluoxetine did not show antidepressant effect in α7nAchR KO mice. It is well known that chronic treatment with SSRIs can increase BDNF levels in the hippocampus and PFC22,23,25,40, suggesting that activation of BDNF-TrkB signaling in the PFC and hippocampus, but not in the NAc, might be involved in the antidepressant effects of SSRIs. Taken all together, it is likely that increased BDNF–TrkB signaling in the NAc, due to a deletion of the α7 nAChR gene, may generate the depression-like phenotype seen in α7 nAChR KO mice.
The precise relationship between the α7 nAChR and BDNF is currently unknown. It has been reported that endogenous BDNF is necessary to sustain the distribution patterns of α7 nAChR on the GABAergic hippocampal neurons48,49, suggesting a close regulation between BDNF and α7 nAChR in the brain. BDNF can enhance neuregulin release at the neuromuscular junction, and neuregulin upregulates functional α7 nAChR on hippocampal neurons48. Furthermore, BDNF can increase the number of α7 nAChR clusters on GABAergic hippocampal neurons, suggesting that BDNF can modulate hippocampal output by controlling α7 nAChR levels49. In addition, direct injection of nicotine into the posterior ventral tegmental area increased BDNF gene expression in the NAc shell50. Moreover, previous studies demonstrated the effect of inflammation on the expression of BDNF in the brain33. We reported that administration of LPS significantly increased BDNF protein expression in the NAc33. Given the role of α7 nAChR in inflammation, it is likely that inflammation might increase BDNF protein expression in the NAc of α7 nAChR KO mice. Further detailed study on the mechanisms underlying increased BDNF-TrkB signaling in the NAc by deletion of α7 nAChR gene is needed.
Tracking dendritic morphology, revealed increased spine density in the NAc of α7 nAChR KO mice. Recently, we reported increased spine density and BDNF in the NAc of the inflammation-induced model of depression in mice33, learned helplessness rats31,32, social defeat stress in mice51, and methamphetamine withdrawal42. Given that synaptogenesis is a key function in the mechanism of antidepressants39,40,41, the therapeutic effect of ANA-12 on depression-like behavior and the increased spine density seen in NAc of α7 nAChR KO mice are of great interest. It is also therefore likely that α7 nAChR KO mice may be an animal model for depression to screen new TrkB antagonists.
In conclusion, these findings suggest that increased BDNF–TrkB signaling in the NAc plays a key role in depression phenotype of α7 nAChR KO mice. Therefore, TrkB antagonists could represent novel therapeutic drugs for depressed patients with increased BDNF–TrkB signaling in the NAc.
Methods and Materials
Animals
Mice deficient for the α7 nAChR (C57BL/6 background) were purchased from The Jackson Laboratory (Bar Harbor, ME). Male wild-type (WT) and knock-out (KO) mice aged 2–3 months were used for experiment. The mice were housed in clear polycarbonate cages (22.5 × 33.8 × 14.0 cm) in groups of 5 or 6 per cage under a controlled 12/12-h light–dark cycle (lights on from 7:00 a.m. to 7:00 p.m.), with a room temperature of 23 ± 1 °C and humidity of 55 ± 5%. All experiments were carried out in accordance with the Guide for Animal Experimentation of Chiba University. The protocol was approved by the Chiba University Institutional Animal Care and Use Committee.
Drug administration
On the day of injection, fresh solutions were prepared by dissolving compounds in sterile endotoxin-free isotonic saline. ANA-12, N2-(2-{[(2-oxoazepan-3-yl) amino]carbonyl}phenyl)benzo[b] thiophene-2-carboxamide (0.5 mg/kg, Catalog number: BTB06525SC, Maybridge), was dissolved in 1% dimethylsulfoxide (DMSO) in physiological saline. 7,8-Dihydroxyflavone (7,8-DHF; 10 mg/kg, Catalog number: D1916, Tokyo Chemical Industry, Tokyo, Japan) was prepared in a vehicle of 17% DMSO in phosphate-buffered saline. Fluoxetine (10 mg/kg, Wako Chemical Co., Ltd, Tokyo, Japan) was prepared in physiological saline. 7,8-DHF and ANA-12 was administered intraperitoneally (i.p.). The doses of 7,8-DHF, ANA-12 and fluoxetine were selected as previously reported33,34,42,43,44,45.
Behavioral tests
Behavioral tests were performed as reported previously33,34. Locomotion: the mice were placed in experimental cages (length × width × height: 560 × 560 × 330 mm). Locomotor activity of mice was counted by the SCANETMV-40 (MELQUEST Co., Ltd., Toyama, Japan), and cumulative exercise was recorded for 60 minutes. Cages were cleaned between testing session. Tail suspension test (TST): The mice were taken from their home cage and a small piece of adhesive tape was placed approximately 2 cm from the tip of their tail. A single hole was punched in the tape and mice were hung individually, on a hook. The immobility time of each mouse was recorded for 10 minutes. Mice were considered immobile only when they hung passively and completely motionless. Forced swimming test (FST): The mice were placed individually in a cylinder (diameter: 23 cm; height: 31 cm) containing 15 cm of water, maintained at 23 ± 1 °C. Animals were tested in an automated forced-swim apparatus using SCANETMV-40 (MELQUEST Co., Ltd., Toyama, Japan). Immobility time was calculated from activity time as (total) – (active) time, using the apparatus analysis software. Cumulative immobility time was scored for 6 minutes during the test. Sucrose preference test (SPT): Mice were habituated to a 1% sucrose solution for 48 h before the test day. Mice were deprived of water and food for 4 h, followed by a preference test spanning 1 h with water and 1% sucrose, delivered from identical bottles. The bottles containing water and sucrose were weighed before and at the end of this period and the sucrose preference was determined.
Dexamethasone (DEX) suppression test
Dexamethasone (DEX: Wako Pure Chemical Co., 0.1 mg/kg) was injected i.p. into mice, as reported previously33,37. Six hours after injection of DEX, mice were anesthetized with pentobarbital, and blood was collected from heart. Blood was centrifuged at 2000 g for 20 minutes to generate serum samples. The serum levels of corticosterone were measured using an Assay MAX corticosterone ELISA kit (St. Charles, MO).
Measurement of pro-inflammatory cytokines
The WT mice and KO mice were anesthetized with pentobarbital, and blood was collected from heart. Blood was centrifuged at 2000 g for 20 minutes to generate serum samples. The serum samples were diluted 10-fold with ELISA diluent solution (eBioscience, San Diego, CA, USA). The serum levels of TNF-α, IL-1β or IL-6 concentrations were measured using a Ready-SET-Go ELISA kit (eBioscience) according to the manufacturer’s instructions.
Western blot analysis of proBDNF, BDNF, p-TrkB, TrkB, PSD-95 and GluA1
The WT and KO mice brain samples of CA1, CA3 and dentate gyrus (DG) of the hippocampus, prefrontal cortex (PFC) and nucleus accumbens (NAc) were collected as previously reported32,33,34. For the ANA-12 treated mice, the brain samples (NAc) were collected after SPT. Tissue samples were homogenized in Laemmli lysis buffer. Aliquots (10 μg for mouse tissue) of protein were measured using the DC protein assay kit (Bio-Rad, Hercules, CA), and incubated for 5 min at 95 °C, with an equal volume of 125 mM Tris/HCl, pH 6.8, 20% glycerol, 0.1% bromophenol blue, 10% β-mercaptoethanol, 4% sodium dodecyl sulfate, and subjected to sodium dodecyl sulfate polyacrylamide gel electrophoresis, using 10% mini-gels (Mini-PROTEAN® TGX™ Precast Gel; Bio-Rad, CA). Proteins were transferred onto polyvinylidenedifluoride (PVDF) membranes using a Trans Blot Mini Cell (Bio-Rad). For immunodetection, the blots were blocked with 2% BSA in TBST (TBS + 0.1% Tween-20) for 1 h at room temperature (RT), and kept with primary antibodies overnight at 4 °C. The following primary antibody was used: BDNF (1: 200, Santa Cruz Biotechnology, Inc., CA), phosphor-TrkB (Tyr 706) (1:200, Santa Cruz Biotechnology, Inc., CA), TrkB (80E3) (1:1000, Cell Signaling Technology, MA), postsynaptic density protein 95 (PSD-95) (1 μg/ml Invitrogen, Carlsbad, CA), and glutamate receptor 1 (GluA1) (1 μg/ml Abcam, Cambridge, MA). The BDNF antibody recognized both proBDNF and mature BDNF. The next day, blot were washed three times in TBST and incubated with horseradish peroxidase conjugated anti-rabbit antibody (1:1000 for TrkB and 1:5000 for BDNF, PSD-95 and GluA1) and goat anti-rabbit antibody (1:2000 for p-TrkB) 1 hour, at RT. After final three washes with TBST, bands were detected using enhanced chemiluminescence (ECL) plus the Western Blotting Detection system (GE Healthcare Bioscience). The blots then were incubated in the stripping buffer (2% SDS, 100 mM β-mercaptoethanol, 62.5 mM Tris/HCL PH 6.8) for 30 min at 60 °C followed by three time washed with TBST. The stripped blots were kept blocking solution for 1 hour and incubated with the primary antibody directed against TrkB protein, GluA1 protein and β-Actin. Images were captured with a Fuji LAS3000-mini imaging system (Fujifilm, Tokyo, Japan), and immunoreactive bands were quantified.
Golgi staining
Golgi staining was performed using the FD Rapid GolgiStainTM Kit (FD Neuro Technologies, Inc., Columbia, MD), following the manufacturer’s instructions. Animals were deeply anesthetized with sodium pentobarbital, and brains were removed from the skull and rinsed in double distilled water. Brains were immersed in the impregnation solution, made by mixing equal volumes of Solution A and B, overnight and then stored in fresh solution, for 2 weeks in the dark. Brains were transferred into Solution C overnight and then stored in fresh solution at 4 °C for 1 week, in the dark. Coronal brain sections (100 μm thickness) were cut on a cryostat (3050S, Leica Microsystems AG, Wetzlar, Germany), with the chamber temperature set at −20 °C. Each section was mounted in Solution C, on saline-coated microscope slides. After absorption of excess solution, sections were dried naturally, at room temperature. Dried sections were processed following the manufacturer’s instructions. Briefly, images of dendrites within CA1, CA3, and DG of the hippocampus, PFC and NAc were captured using a 100x objective with a Keyence BZ-9000 Generation II microscope (Osaka, Japan). Spines were counted along CA1, CA3, DG, PFC and NAc dendrites starting from their point of origin from the primary denarite, as previously reported32,33. For spine density measurements, all clearly evaluable areas containing 50–100 μm of secondary dendrites from each imaged neuron were used. To determine relative spine density, spines on multiple dendritic branches from a single neuron were counted to obtain an average spine number per 10 μm. For spine number measurements, only spines that emerged perpendicular to the dendritic shaft were counted. Three neurons per section, three sections per animal and five animals were analyzed. The average value for each region, in each individual was obtained. These individual averages were then combined to yield a grand average for each region.
Systemic administration of ANA-12, 7,8-DHF and fluoxetine
ANA-12 (0.5 mg/kg), 7,8-DHF (10 mg/kg), fluoxetine (10 mg/kg) or vehicle (10 ml/kg) was administered i.p. into α7 nAChR KO mice or WT mice. Behavioral evaluation was performed at 1 hour (locomotion), 4 hours (TST) and 6 hours (FST). The SPT was performed at 36 hours after a single administration.
Bilateral injection of ANA-12 into NAc
Mice were anesthetized with pentobarbital (5 mg/ml, 0.15 ml/mouse), and placed in a stereotaxic frame. Microinjection needles were placed bilaterally into the NAc shell (+1.7 AP, ± 0.75 ML, −3.6 DV)33. Twenty-four hours after surgery, ANA-12 (0.1 nmol/L, 0.1 μL/min for 5 min) or vehicle was injected bilaterally. Behavioral evaluation was performed at 1 hour (locomotion), 4 hours (TST) and 6 hours (FST), the SPT was performed at 36 hours after the final infusion.
Statistical analysis
The data are show as the mean ± standard error of the mean (SEM). Analysis was performed using PASW Statistics 20 (formerly SPSS Statistics; SPSS). Comparisons between groups were performed using the Student’s t-test and two-way ANOVA, when appropriate, post hoc comparisons were performed using the unpaired t-test. The P-values of less than 0.05 were considered statistically significant.
Additional Information
How to cite this article: Zhang, J.-C. et al. Depression-like phenotype by deletion of α7 nicotinic acetylcholine receptor: Role of BDNF-TrkB in nucleus accumbens. Sci. Rep. 6, 36705; doi: 10.1038/srep36705 (2016).
References
Dantzer, R. et al. From inflammation to sickness and depression: when the immune system subjugates the brain. Nat Rev Neurosci 9, 46–57 (2008).
Hashimoto, K. Emerging role of glutamate in the pathophysiology of major depressive disorder. Brain Res Rev 61, 105–123 (2009).
Hashimoto, K. Inflammatory biomarkers as differential predictors of antidepressant response. Int J Mol Sci 16, 7796–7801 (2015).
Miller, A. H., Maletic, V. & Raison, C. L. Inflammation and its discontents: the role of cytokines in the pathophysiology of major depression. Biol Psychiatry 65, 732–741 (2009).
Raison, C. L., Lowry, C. A. & Rook, G. A. Inflammation, sanitation, and consternation: loss of contact with coevolved, tolerogenic microorganisms and the pathophysiology and treatment of major depression. Arch Gen Psychiatry 67, 1211–1224 (2010).
Zhang, J. C., Yao, W. & Hashimoto, K. Brain-derived neurotrophic factor (BDNF) – TrkB signaling in inflammation-related depression and potential therapeutic targets. Curr Neuropharmacol 14, 721–731 (2016).
Dowlati, Y. et al. A meta-analysis of cytokines in major depression. Biol Psychiatry 67, 446–457 (2010).
Goldsmith, D. R., Rapaport, M. H. & Miller, B. J. A meta-analysis of blood cytokine network alterations in psychiatric patients: comparisons between schizophrenia, bipolar disorder and depression. Mol Psychiatry Feb 23, doi: 10.1038/mp.2016.3 (2016).
Shelton, R. C. et al. Altered expression of genes involved in inflammation and apoptosis in frontal cortex in major depression. Mol Psychiatry 16, 751–762 (2011).
Mineur, Y. S. et al. Cholinergic signaling in the hippocampus regulates social stress resilience and anxiety- and depression-like behavior. Proc Natl Acad Sci USA 110, 3573–3578 (2013).
Hurst, R., Rollema, H. & Bertrand, D. Nicotinic acetylcholine receptors: from basic science to therapeutics. Pharmacol Ther 137, 22–54 (2013).
Mineur, Y. S. & Picciotto, M. R. Nicotine receptors and depression: revisiting and revising the cholinergic hypothesis. Trends Pharmacol Sci 31, 580–586 (2010).
Picciotto, M. R., Lewis, A. S., van Schalkwyk, G. I. & Mineur, Y. S. Mood and anxiety regulation by nicotinic acetylcholine receptors: A potential pathway to modulate aggression and related behavioral states. Neuropharmacology 96 (Pt B), 235–243 (2015).
Zurkovsky, L., Taylor, W. D. & Newhouse, P. A. Cognition as a therapeutic target in late-life depression: potential for nicotinic therapeutics. Biochem Pharmacol 86, 1133–1144 (2013).
Lu, B. et al. α7 nicotinic acetylcholine receptor signaling inhibits inflammasome activation by preventing mitochondrial DNA release. Mol Med 14, 350–358 (2014).
Martelli, D., McKinley, M. J. & McAllen, R. M. The cholinergic anti-inflammatory pathway: a critical review. Auton Neurosci 182, 65–69 (2014).
Wang, H. et al. Nicotinic acetylcholine receptor α7 subunit is an essential regulator of inflammation. Nature 421, 384–388 (2003).
Thomsen, M. S. & Mikkelsen, J. D. The α7 nicotinic acetylcholine receptor ligands methyllycaconitine, NS6740 and GTS-21 reduce lipopolysaccharide-induced TNF-α release from microglia. J Neuroimmunol 251, 65–72 (2012).
Suzuki, T. et al. Microglial alpha7 nicotinic acetylcholine receptors drive a phospholipase C/IP3 pathway and modulate the cell activation toward a neuroprotective role. J Neurosci Res 83, 1461–1470 (2006).
Autry, A. E. & Monteggia, L. M. Brain-derived neurotrophic factor and neuropsychiatric disorders. Pharmacol Rev 64, 238–258 (2012).
Castrén, E. & Rantamäki, T. The role of BDNF and its receptors in depression and antidepressant drug action: Reactivation of developmental plasticity. Dev Neurobiol 70, 289–297 (2010).
Duman, R. S. & Monteggia, L. M. A. A neurotrophic model for stress-related mood disorders. Biol Psychiatry 59, 1116–1127 (2006).
Hashimoto, K. Brain-derived neurotrophic factor as a biomarker for mood disorders: an historical overview and future directions. Psychiatry Clin Neurosci 64, 341–357 (2010).
Hashimoto, K. Sigma-1 receptor chaperone and brain-derived neurotrophic factor: emerging links between cardiovascular disease and depression. Prog Neurobiol 100, 15–29 (2013).
Hashimoto, K., Shimizu, E. & Iyo, M. Critical role of brain-derived neurotrophic factor in mood disorders. Brain Res Rev 45, 104–114 (2004).
Nestler, E. J., Barrot, M., DiLeone, R. J., Eisch, A. J., Gold, S. J. & Monteggia, L. M. Neurobiology of depression. Neuron 34, 13–25 (2002).
Berton, O. et al. Essential role of BDNF in the mesolimbic dopamine pathway in social defeat stress. Science 311, 864–868 (2006).
Eisch, A. J. et al. Brain-derived neurotrophic factor in the ventral midbrain-nucleus accumbens pathway: a role in depression. Biol Psychiatry 54, 994–1005 (2003).
Nestler, E. J. & Carlezon, W. A. Jr. The mesolimbic dopamine reward circuit in depression. Biol Psychiatry 59, 1151–1159 (2006).
Krishnan, V. et al. Molecular adaptations underlying susceptibility and resistance to social defeat in brain reward regions. Cell 131, 391–404 (2007).
Shirayama, Y. et al. Alterations in brain-derived neurotrophic factor (BDNF) and its precursor proBDNF in the brain regions of a learned helplessness rat model and the antidepressant effects of a TrkB agonist and antagonist. Eur Neuropsychopharmacol 25, 2449–2458 (2015).
Yang, C., Shirayama, Y., Zhang, J. C., Ren, Q. & Hashimoto, K. Regional differences in brain-derived neurotrophic factor and dendritic spine density confer resilience to inescapable stress. Int J Neuropsychopharmacol 18, pyu121 (2015).
Zhang, J. C. et al. Antidepressant effects of TrkB ligands on depression-like behavior and dendritic changes in mice after inflammation. Int J Neuropsychopharmacol 18, pyu077 (2015).
Zhang, J. C. et al. Comparison of ketamine, 7,8-dihydroxyflavone, and ANA-12 antidepressant effects in the social defeat stress model of depression. Psychopharmacology 232, 4325–4335 (2015).
Jang, S. W. et al. A selective TrkB agonist with potent neurotrophic activities by 7,8-dihydroxyflavone. Proc Natl Acad Sci USA 107, 2687–2692 (2010).
Cazorla, M. et al. Identification of a low-molecular weight TrkB antagonist with anxiolytic and antidepressant activity in mice. J Clin Invest 121, 1846–1857 (2011).
Li, S. X. et al. Role of the NMDA receptor in cognitive deficits, anxiety and depressive-like behavior in juvenile and adult mice after neonatal dexamethasone exposure. Neurobiol Dis 62, 124–134 (2014).
Pariante, C. M. & Miller, A. H. Glucocorticoid receptors in major depression: relevance to pathophysiology and treatment. Biol Psychiatry 49, 391–404 (2001).
McEwen, B. Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiol Rev 87, 873–904 (2007).
Duman, R. S. & Aghajanian, G. K. Synaptic dysfunction in depression: potential therapeutic targets. Science 338, 68–72 (2012).
Ohgi, Y., Futamura, T. & Hashimoto, K. Glutamate signaling in synaptogenesis and NMDA receptors as potential therapeutic targets for psychiatric disorders. Curr Mol Med 15, 206–221 (2015).
Ren, Q. et al. BDNF-TrkB signaling in the nucleus accumbens shell of mice has key role in methamphetamine withdrawal symptoms. Transl Psychiatry 5, e666 (2015).
Ren, Q. et al. Effects of TrkB agonist 7,8-dihydroxyflavone on sensory gating deficits in mice after administration of methamphetamine. Pharmacol Biochem Behav 106, 124–127 (2013).
Ren, Q. et al. 7,8-Dihydroxyflavone, a TrkB agonist, attenuates behavioral abnormalities and neurotoxicity in mice after administration of methamphetamine. Psychopharmacology (Berl) 231, 159–166 (2014).
Ohgi, Y., Futamura, T., Kikuchi, T. & Hashimoto, K. Effects of antidepressants on alternations in serum cytokines and depressive-like behavior in mice after lipopolysaccharide administration. Pharmacol Biochem Behav 103, 856–859 (2013).
O’Connor, J. C. et al. Lipopolysaccharide-induced depressive-like behavior is mediated by indoleamine 2,3-dioxygenase activation in mice. Mol Psychiatry 14, 511–522 (2009).
de Paiva, V. N. et al. Prostaglandins mediate depressive-like behaviour induced by endotoxin in mice. Behav Brain Res 215, 146–151 (2010).
Kawai, H., Zago, W. & Berg, D. K. Nicotinic α7 receptor clusters on hippocampal GABAergic neurons: regulation by synaptic activity and neurotrophins. J Neurosci 22, 7903–7912 (2002).
Massey, K. A., Zago, W. M. & Berg, D. K. BDNF up-regulate alpha-7 nicotinic acetylcholine receptor levels on subpopulation of hippocampal interneurons. Mol Cell Neurosci 33, 381–388 (2006).
Truitt, W. A. et al. Ethanol and nicotine interaction within the posterior ventral tegmental area in male and female alcohol-preferring rats: evidence of synergy and differential gene activation in the nucleus accumbens shell. Psychopharmacology (Berl) 232, 639–649 (2015).
Yang, C. et al. R-ketamine: a rapid-onset and sustained antidepressant without psychotomimetic side effects. Transl Psychiatry 5, e632 (2015).
Acknowledgements
This study was supported by a Grant-in-Aid for Scientific Research from Japan Society for Promotion of Science (to J.C.Z. and K.H.), a Grant-in-Aid for Scientific Research on Innovative Areas of the Ministry of Education, Culture, Sports, Science and Technology, Japan (to K.H.) the Strategic Research Program for Brain Sciences from Japan Agency for Medical Research and development, AMED (to K.H.), and Smoking Research Foundation, Tokyo, Japan (to K.H.). Dr. Wei Yao was supported by Ishidsu Shun Memorial Scholarship (Tokyo, Japan). Dr. Qian Ren and Dr. Chun Yang were supported by Research Fellowship for Young Scientists of the Japan Society for the Promotion of Science. Dr. Chao Dong was supported by Uehara Memorial Foundation (Tokyo, Japan). Ms. Min Ma was supported by Leading Graduate School at Chiba University.
Author information
Authors and Affiliations
Contributions
J.C.Z. and K.H. conceived and designed the experiments; J.C.Z., W.Y., C.D., C.Y., Q.R., M.M. and J.W. performed the experiments. J.C.Z. and W.Y. analyzed the data, and J.C.Z. and K.H. wrote the manuscript.
Ethics declarations
Competing interests
Dr. Kenji Hashimoto has served as a scientific consultant to Taisho, and he has also received research support from Dainippon-Sumitomo, Mochida, Otsuka, and Taisho.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zhang, Jc., Yao, W., Ren, Q. et al. Depression-like phenotype by deletion of α7 nicotinic acetylcholine receptor: Role of BDNF-TrkB in nucleus accumbens. Sci Rep 6, 36705 (2016). https://doi.org/10.1038/srep36705
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep36705
This article is cited by
-
Nicotinic Acetylcholine Receptors of PC12 Cells
Cellular and Molecular Neurobiology (2021)
-
Increased EphA4-ephexin1 signaling in the medial prefrontal cortex plays a role in depression-like phenotype
Scientific Reports (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.