Abstract
Mice deficient in SHARPIN (Sharpincpdm mice), a member of linear ubiquitin chain assembly complex (LUBAC), develop severe dermatitis associated with systemic inflammation. Previous studies have demonstrated that components of the TNF-signaling pathway, NLRP3 inflammasome and IL-1R signaling are required to provoke skin inflammation in Sharpincpdm mice. However, whether IL-1α or IL-1β, both of which signals through IL-1R, instigates skin inflammation and systemic disease is not known. Here, we have performed extensive cellular analysis of pre-diseased and diseased Sharpincpdm mice and demonstrated that cellular dysregulation precedes skin inflammation. Furthermore, we demonstrate a specific role for IL-1β, but not IL-1α, in instigating dermatitis in Sharpincpdm mice. Our results altogether demonstrate distinct roles of SHARPIN in initiating systemic inflammation and dermatitis. Furthermore, skin inflammation in Sharpincpdm mice is specifically modulated by IL-1β, highlighting the importance of specific targeted therapies in the IL-1 signaling blockade.
Similar content being viewed by others
Introduction
The chronic proliferative dermatitis (cpdm) phenotype was first identified in C57BL/Ka mice that arose as a result of a spontaneous mutation1. A single base-pair deletion in exon 1 of the gene encoding Shank-associated RH domain interacting protein (SHARPIN) was later found to be associated with the cpdm phenotype2. As a result, these cpdm mice completely lack SHARPIN expression, and are hereafter referred to as Sharpincpdm mice2. Sharpincpdm mice develop severe dermatitis, multiorgan inflammation, and immune system dysregulation2. Phenotypically, the dermatitis observed in the Sharpincpdm mice is similar to those in several human inflammatory skin diseases like cryopyrin-associated periodic syndrome, familial Mediterranean fever, and neutrophilic dermatoses3.
SHARPIN, Heme-oxidized IRP2 ubiquitin ligase 1 homolog (HOIL-1) and HOIL-1-interacting protein (HOIP) assemble the linear ubiquitin assembly chain complex (LUBAC), which regulates signaling pathways by linearly ubiquitinating target proteins4,5,6. Specifically, SHARPIN is a critical regulator of TNF-mediated cell death pathways- apoptosis and necroptosis4,5,6. As such, Sharpincpdm keratinocytes and fibroblasts are highly sensitive to TNF-induced cell death4,5,6. Indeed, TNF-induced keratinocyte cell death has been proposed to be the major cause of dermatitis observed in Sharpincpdm mice, and TNF-deficiency in Sharpincpdm mice completely prevents dermatitis4. More recent studies have identified molecules involved in both apoptotic and necroptotic pathways to be required for cell death induced by TNF in Sharpincpdm mice7,8. Specifically, deficiency in either caspase-8, FADD, RIPK3, or RIPK1 can prevent induction of dermatitis in Sharpincpdm mice7,8.
The NLRP3 inflammasome has also been reported to play a role in instigating skin inflammation in Sharpincpdm mice9. In comparison to Sharpincpdm mice, Sharpincpdm × Nlrp3−⁄− and Sharpincpdm × Casp1−⁄− × Casp11−⁄− mice display a delayed onset of clinical signs of dermatitis9. The NLRP3 inflammasome is a critical regulator of IL-1 cytokines, which signals through IL-1R10,11,12,13,14. Given that IL-1R deficiency delays the progression of dermatitis in Sharpincpdm mice8, we sought to examine the contribution of specific IL-1 cytokines (IL-1α and IL-1β, both of which signal via IL-1R) in the progression of dermatitis and systemic immune perturbation. Herein, we extensively characterize and establish parameters of the immune cell dysregulation found in Sharpincpdm mice. Our data herein demonstrate a specific role for IL-1β in promoting dermatitis in Sharpincpdm mice. Interestingly, IL-1β is dispensable for immune cell dysregulation. Thus, our results suggest that independent mechanisms regulate dermatitis and cellular dysregulation in Sharpincpdm mice. Moreover, IL-1α is completely dispensable for disease progression in Sharpincpdm mice. Altogether, our study further highlights a specific role of IL-1β in provoking dermatitis in Sharpincpdm mice and provides additional evidence advocating the use of specific IL-1 targeted therapies in the treatment of inflammatory diseases.
Results
Sharpincpdm mice develop severe dermatitis and systemic inflammation
Sharpincpdm mice develop severe dermatitis that is associated with systemic inflammation. Sharpincpdm mice that were bred in-house developed dermatitis with 100% penetrance at around 30–60 days after birth, with a median age of onset of dermatitis around 42.5 days (Fig. 1a,b). The dermatitis worsened with age, and these mice were eventually euthanized for humane reasons. Further phenotypic analysis demonstrated that 70-day-old diseased Sharpincpdm mice had significantly larger and heavier spleens than those of control mice (Fig. 1c,d). Consistent with the increased spleen size and weight, the total number of splenocytes was also significantly increased in Sharpincpdm mice (Fig. 1e). Analysis of major immune cell populations within the spleen by flow cytometry revealed various abnormalities that were indicative of systemic inflammation in Sharpincpdm mice. The frequency of neutrophils (determined by Gr1+CD11b+ stained cells) was significantly higher in Sharpincpdm mice than in controls (Fig. 1f,g). In contrast, the frequencies of CD4+, CD8+, and CD19+ cells were significantly lower in the Sharpincpdm spleen than in the control spleen (Fig. 1h–l), which could be a consequence of the increased frequency of neutrophils in the diseased Sharpincpdm mice. As expected with this disease, the frequency of activated antigen-experienced CD8+ and CD4+ T cells (determined by their surface expression of CD11a15,16) was also significantly increased in the spleens of Sharpincpdm mice (Extended Data Fig. 1). In accordance with the occurrence of systemic inflammation in Sharpincpdm mice, analysis of neutrophils, T cells, and B cells in peripheral blood leukocytes (PBL) yielded results that were similar to those from the analysis of spleen (Extended Data Fig. 2).
Phenotypic analysis and cellular characterization of diseased Sharpincpdm mice.
(a) Control (n = 15) and Sharpincpdm (n = 18) mice were followed after weaning and scored for the onset of dermatitis. Mice that showed any sign of skin inflammation were scored as disease-positive and indicated in the disease score curves on that day. (b) Representative images of control and Sharpincpdm mice on day 70 post birth, depicting the extent of dermatitis on the dorsal and ventral sides. White dotted line outlines the area of dermatitis in Sharpincpdm mice. (c–e) Spleen harvested from control and Sharpincpdm mice on day 70. Representative images (c) spleen weight (d) and splenocyte count (e) of control and Sharpincpdm mice. (f–l) Flow cytometry analysis of splenocytes from control and Sharpincpdm mice on day 70. Representative flow plots of CD11b+Gr1+ neutrophils (f) CD4+ and CD8+ T cells (h) and CD19+MHCII+ B cells (k) in the spleen. Cumulative bar graphs representing frequencies of CD11b+Gr1+ neutrophils (g) CD4+ T cells (i), CD8+ T cells (j) and CD19+MHCII+ B cells (l) in the spleen. Control, n = 4; Sharpincpdm, n = 4 for (d, e, g, i, j, l). The disease curve in (a) was analyzed by log rank (Mantel-Cox) testing. Bar graphs are presented as means ± s.e.m. and are representative of at least three independent experiments. Statistical significance was determined by Mann-Whitney testing, and P values less than 0.05 are considered statistically significant. *P < 0.05, ****P < 0.0001.
Immune cellular dysregulation precedes dermatitis in Sharpincpdm mice
Although dermatitis and systemic inflammation (associated with splenomegaly and neutrophilia) are two major phenotypes that are observed in diseased Sharpincpdm mice, it is not clear whether systemic inflammation is a consequence of severe dermatitis. Because SHARPIN has distinct roles in different cell types, we examined earlier time points to evaluate the link between dermatitis and systemic inflammation. Sharpincpdm mice developed dermatitis and had significantly increased spleen size and weight at 45 days of age, prompting us to examine earlier time points (Fig. 2a–c). Phenotypic analysis of Sharpincpdm mice showed no signs of dermatitis at 25 days of age (Fig. 2d). Furthermore, the spleen size and weight of Sharpincpdm and control mice were similar, suggesting that no systemic inflammation had occurred by day 25 (Fig. 2e,f).
Splenic cell population analysis of pre-diseased Sharpincpdm mice demonstrates cellular dysregulation.
Representative images of control and Sharpincpdm mice on day 45 post birth (a) and day 25 post birth (d), depicting the extent of dermatitis on the dorsal and ventral sides. White dotted line outlines the area of dermatitis in the Sharpincpdm mice. Spleen image (b,e) and weight (c,f) of control and Sharpincpdm mice on indicated days. (g–m) Flow cytometry analysis of splenocytes from control and Sharpincpdm mice on day 25. Representative flow plots of CD11b+Gr1+ neutrophils (g), CD4+ and CD8+ T cells (i), and CD19+MHCII+ B cells (l) in the spleen. Cumulative bar graphs representing frequencies of CD11b+Gr1+ neutrophils (h), CD4+ T cells (j), CD8+ T cells (k), and CD19+MHCII+ B cells (m) in the spleen. Control, n = 7; Sharpincpdm, n = 6 for (c). Control, n = 4; Sharpincpdm, n = 4 for h, j, k, and m. Bar graphs are presented as means ± s.e.m. and are representative of at least two independent experiments. Statistical significance was determined by Mann-Whitney testing, and P values less than 0.05 are considered statistically significant. *P < 0.05.
Interestingly, neutrophil frequency in the spleen was significantly greater in the 25-day-old pre-diseased Sharpincpdm mice than in control mice (Fig. 2g,h). Peripheral blood lymphocytes (PBLs) from pre-diseased Sharpincpdm mice had a similar increase in the frequency of neutrophils (Extended Data Fig. 3a,b). Further, flow cytometry analyses of T- and B-cell populations in the spleen and PBLs revealed that lymphocytes were similarly dysregulated (in comparison with Fig. 1) in 25-day-old pre-diseased Sharpincpdm mice. Both the frequencies of T- and B-cell populations were significantly lower in the spleen and PBLs of 25-day-old Sharpincpdm mice than in those of control mice (Fig. 2i–m and Extended Data Fig. 3c–g). When CD8+ and CD4+ T cells were further analyzed for activation, as in Fig. 1, we observed increased frequencies of activated CD8+ T cells (increased CD11a expression) in both the spleen and PBLs of pre-diseased Sharpincpdm mice compared to control mice (Extended Data Fig. 3h,i and Extended Data Fig. 4a,b). However, the proportion of CD11ahi-expressing CD4+ T cells in the spleen and PBLs was similar between 25-day-old Sharpincpdm mice and controls (Extended Data Fig. 3j,k and Extended Data Fig. 4c,d).
To investigate whether immune cell dysregulation precedes skin inflammation, we directly analyzed the skin sections from 25-day-old and 70-day-old Sharpincpdm mice by histology. As ascertained from the H&E stained sections, the epidermal thickness of d25-old Sharpincpdm skin was similar to the skin of control mice, although the 25-day-old Sharpincpdm skin had slightly increased cellular infiltration in the dermis (Fig. 3a). In contrast, the 70-day-old Sharpincpdm skin was visibly inflamed with significantly increased epidermal thickening and cellular infiltrates (Fig. 3a,b). Altogether, these data suggest that systemic dysregulation of immune cells (i.e. increase in neutrophils and activated T cells) precedes dermatitis. However, a previously published study in which Sharpincpdm bone marrow cells were transferred to lethally irradiated WT recipients (Sharpincpdm ≫ WT chimeras) showed that these chimeras did not develop dermatitis, suggesting that dysregulated Sharpincpdm immune cells do not provoke skin inflammation8. We independently confirmed these results and found that Sharpincpdm ≫ WT chimeras do not develop dermatitis (Extended Data Fig. 5a). However, PBL analysis of the immune cell population from Sharpincpdm ≫ WT chimeras demonstrated that immune cells have activated T cells and increased neutrophils when compared to WT ≫ WT chimeras (Extended Data Fig. 5b–i). Thus, the immune cell dysregulation and dermatitis observed in Sharpincpdm mice is independent of each other and due to distinct roles of SHARPIN in immune cells and non-hematopoietic cells.
Histological analysis of skin sections from pre-diseased and diseased Sharpincpdm mice.
(a) Representative hematoxylin and eosin (H&E) images of control, pre-diseased (d25) and diseased (d70) Sharpincpdm mice. (b) Epidermal thickness of skin sections from control, pre-diseased (d25) and diseased (d70) Sharpincpdm mice. The epidermis of the H&E sections were measured using FIJI Image J open source software. For each section, four independent measurements were taken and averaged to get a measurement of epidermis thickening. n = 4 for control, n = 4 for pre-diseased and n = 4 for diseased Sharpincpdm groups. Statistical significance was determined by Mann-Whitney testing, and P values less than 0.05 are considered statistically significant. *P < 0.05.
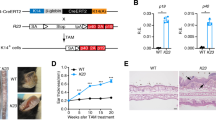
IL-1R deficiency delays progression of disease in Sharpincpdm mice
The NLRP3 inflammasome is important in regulating disease progression (dermatitis) in Sharpincpdm mice. Specifically, mice deficient in either NLRP3, caspase-1, or caspase-11 demonstrate a delay in progression of disease by about 15–30 days9. The NLRP3 inflammasome is a critical regulator of pleiotropic IL-1 cytokines, and cell death termed pyroptosis. Concurrently, mice deficient in IL-1R also delay the onset of dermatitis8. To corroborate whether IL-1R deficiency protects Sharpincpdm mice from progression to dermatitis, we generated Sharpincpdm × Il1r−⁄− mice and monitored the development of dermatitis in this mice. The disease progression curves of Sharpincpdm and Sharpincpdm × Il1r−⁄− mice demonstrated that IL-1R deficiency delayed the progression of disease by 21–30 days (Fig. 4a,b). Overall, the median age of onset of dermatitis for Sharpincpdm mice was 47 days compared to 81 days for Sharpincpdm × Il1r−⁄− mice. However, it should be noted that IL-1R deficiency did not provide complete protection and, ultimately, 100% of Sharpincpdm × Il1r−⁄− mice developed dermatitis (Fig. 4a).
IL-1R deficiency in Sharpincpdm mice delays the development of skin disease.
(a) Control (n = 9), Sharpincpdm (n = 7), and Sharpincpdm × Il1r−⁄− (n = 7) mice were followed after weaning and scored for the onset of dermatitis. Mice that showed any sign of skin inflammation were scored as disease-positive and indicated in the disease score curves on that day. (b) Representative images of control and Sharpincpdm mice on day 45 and Sharpincpdm × Il1r−⁄− mice on day 70 post birth, depicting the extent of dermatitis on the dorsal and ventral sides. White dotted line outlines the area of dermatitis in Sharpincpdm mice. The disease curve in (a) was analyzed by log rank (Mantel-Cox) testing. ***P < 0.001.
IL-1α does not regulate disease progression in Sharpincpdm mice
IL-1α is highly expressed in keratinocytes and secreted by cells following cell death. Keratinocyte-specific deletion of TNF and TNFR (signaling molecules involved in apoptotic and necrotic cell death) prevents induction of disease and dermatitis in Sharpincpdm mice4,7,8. Moreover, Sharpincpdm mice also deficient in RIPK1 kinase activity (Sharpincpdm × Ripk1K45A mice) are completely protected from disease induction, further demonstrating the importance of cell death pathways17. To determine whether IL-1α promotes dermatitis in Sharpincpdm mice, we generated Sharpincpdm × Il1a−⁄− mice and observed these mice for signs of disease. Sharpincpdm × Il1a−⁄− mice developed dermatitis as early as 30 days after birth, and 100% of these mice developed dermatitis by 70 days with similar kinetics (Fig. 5a). The median age of onset of dermatitis was 42.5 days for Sharpincpdm and 45 days for Sharpincpdm × Il1a−⁄− mice (Fig. 5a). Sharpincpdm and Sharpincpdm × Il1a−⁄− mice also showed a similar extent of dermatitis and splenomegaly at day 45 post birth (Fig. 5b–d). Histological analysis of skin sections from Sharpincpdm and Sharpincpdm × Il1a−⁄− mice showed that both groups had significantly increased cellular infiltration and epidermal thickening when compared to WT controls (Extended data Fig. 6).
IL-1α is dispensable for induction of disease in Sharpincpdm mice.
(a) Control (n = 11), Sharpincpdm (n = 10), and Sharpincpdm × Il1a−⁄− (n = 10) mice were followed after weaning and scored for the onset of dermatitis. Mice that showed any sign of skin inflammation were scored as disease-positive and indicated in the disease score curves on that day. (b) Representative images of control, Sharpincpdm, and Sharpincpdm × Il1a−⁄− mice on day 45 post birth, depicting the extent of dermatitis on the dorsal and ventral sides. White dotted line outlines the area of dermatitis in Sharpincpdm and Sharpincpdm × Il1a−⁄− mice. (c–d) Spleen harvested from control, Sharpincpdm and Sharpincpdm × Il1a−⁄− mice on day 45. Representative images (c) and spleen weight (d) of control, Sharpincpdm, and Sharpincpdm × Il1a−⁄− mice. (e–k) Flow cytometry analysis of splenocytes from control, Sharpincpdm, and Sharpincpdm × Il1a−⁄− on day 45. Representative flow plots of CD11b+Gr1+ neutrophils (e) CD4+ and CD8+ T cells (g) and CD19+MHCII+ B cells (j) in the spleen. Cumulative bar graphs representing frequencies of CD11b+Gr1+ neutrophils (f) CD4+ T cells (h) CD8+ T cells (i) and CD19+MHCII+ B cells (k) in the spleen. Control, n = 6; Sharpincpdm, n = 6; Sharpincpdm × Il1a−⁄−, n = 4 for d, f, h, i, and k. Disease curve in (a) was analyzed by log rank (Mantel-Cox) testing. Bar graphs are presented as means ± s.e.m. Statistical significance between groups was determined by one-way ANOVA followed Dunnett’s multiple comparisons testing, and P values less than 0.05 are considered statistically significant. ns = not significant, *P < 0.05, **P < 0.01.
Although IL-1α did not provide any protection from dermatitis, we speculated that IL-1α deficiency would rescue the cellular dysregulation observed in Sharpincpdm mice. Analysis of the splenic population for neutrophils, T cells, and B cells revealed dysregulation in Sharpincpdm × Il1a−⁄− mice similar to that seen in Sharpincpdm mice (Fig. 5e–k). Specifically, the frequency of Gr1+CD11b+ neutrophils was significantly increased (Fig. 5e,f), while CD4+ T cells (Fig. 5g,h), CD8+ T cells (Fig. 5g,i), and CD19+ B cells (Fig. 5j,k) were significantly decreased in Sharpincpdm × Il1a−⁄− mice, similar to Sharpincpdm mice. Furthermore, the increased activation of CD4+ and CD8+ T cells observed in Sharpincpdm mice was also observed in Sharpincpdm × Il1a−⁄− mice (Extended Data Fig. 7). Similar cellular dysregulation also persisted in the PBLs of Sharpincpdm × Il1a−⁄− mice (Extended Data Fig. 8). Altogether, these data suggest that IL-1α is dispensable for induction of dermatitis and cellular dysregulation in Sharpincpdm mice.
IL-1β deficiency delays the onset of dermatitis in Sharpincpdm mice
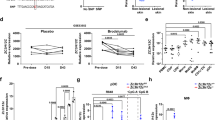
Given that IL-1α deficiency did not provide protection from dermatitis or systemic inflammation in Sharpincpdm mice (Fig. 5 and Extended Data Figs 7 and 8), we hypothesized that IL-1β (the other IL-1 cytokine that signals through IL-1R) would be involved in the progression of disease in Sharpincpdm mice. As hypothesized, IL-1β deficiency in Sharpincpdm mice significantly delayed the onset of dermatitis (Fig. 6a). Although all Sharpincpdm mice developed dermatitis between 30–70 days, signs of dermatitis in Sharpincpdm × Il1b−⁄− mice were not observed until day 60, with all mice showing some signs of skin inflammation by day 90 (Fig. 6a). The median age of onset of dermatitis for Sharpincpdm mice was 48 days compared to 63 days for Sharpincpdm × Il1b−⁄− mice (Fig. 6a). Sharpincpdm mice which were 45 days old developed severe dermatitis, whereas Sharpincpdm × Il1b−⁄− mice at this age showed no signs of skin inflammation (Fig. 6b). Histological analysis revealed severe inflammation in the skin of 45-day-old Sharpincpdm mice, characterized by epidermal thickening and the presence of inflammatory cells in the dermis. In contrast, skin sections from pre-diseased 45-day-old Sharpincpdm × Il1b−⁄− mice showed significantly reduced epidermal thickening and immune cell infiltration in the dermis (Extended Data Fig. 9). However, Sharpincpdm × Il1b−⁄− mice eventually developed dermatitis, as shown for 70-day-old Sharpincpdm × Il1b−⁄− mice (Fig. 6b). Although the extent of dermatitis might appear milder in Sharpincpdm × Il1b−⁄− mice, they eventually develop severe dermatitis similar to that observed in Sharpincpdm mice.
IL-1β deficiency delays the onset of dermatitis in Sharpincpdm mice.
(a) Control (n = 13), Sharpincpdm (n = 11), and Sharpincpdm × Il1b−⁄− (n = 12) mice were followed after weaning and scored for the onset of dermatitis. Mice that showed any sign of skin inflammation were scored as disease-positive and indicated in the disease score curves on that day. (b) Representative images of control, Sharpincpdm, and Sharpincpdm × Il1b−⁄− mice on the indicated days, depicting the extent of dermatitis on the dorsal and ventral sides. White dotted line outlines the area of dermatitis in the Sharpincpdm and Sharpincpdm × Il1b−⁄− mice. (c–d) Spleen harvested from control, Sharpincpdm, and Sharpincpdm × Il1b−⁄− mice. Representative images (c) and spleen weight (d) of control, Sharpincpdm, and Sharpincpdm × Il1b−⁄− mice. (e–k) Flow cytometry analysis of splenocytes from control (d45), Sharpincpdm (d45), and Sharpincpdm × Il1b−⁄− mice (d45 and d70 combined). Representative flow plots of CD11b+Gr1+ neutrophils (e) CD4+ and CD8+ T cells (g) and CD19+MHCII+ B cells (j) in the spleen. Cumulative bar graphs representing frequencies of CD11b+Gr1+ neutrophils (f) CD4+ T cells (h) CD8+ T cells (i), and CD19+MHCII+ B cells (k) in the spleen. Control, n = 13; Sharpincpdm, n = 11; Sharpincpdm × Il1b−⁄−, n = 10 for d, f, h, i, and k. Disease curve in (a) was analyzed by log rank (Mantel-Cox) testing. Bar graphs are presented as means ± s.e.m. Statistical significance between groups was determined by one-way ANOVA followed by Dunnett’s multiple comparisons testing, and P values less than 0.05 are considered statistically significant. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001.
Analysis of the spleen for signs of systemic inflammation showed that Sharpincpdm × Il1b−⁄− mice had increased spleen size and weight, similar to those of Sharpincpdm mice (Fig. 6c,d). To determine whether deficiency in IL-1β rescued cellular dysregulation, we examined various cellular populations in the spleen and PBLs. Interestingly, IL-1β deficiency did not rescue defects in the cell population of Sharpincpdm mice. The frequency of neutrophils significantly increased in both the spleen and PBLs of Sharpincpdm and Sharpincpdm × Il1b−⁄− mice compared to control mice (Fig. 6e,f and Extended Data Fig. 10a,b). The frequencies of both CD4+ and CD8+ T-cells were similarly reduced in Sharpincpdm and Sharpincpdm × Il1b−⁄− mice when compared to control mice (Fig. 6g–i and Extended Data Fig. 10c–e). Moreover, further analysis of these T cells showed that higher percentages of the T cells were activated and antigen-experienced in Sharpincpdm and Sharpincpdm × Il1b−⁄− mice (Extended Data Fig. 10f–i and Extended Data Fig. 11). Lastly, the frequency of CD19+ cells was also reduced in Sharpincpdm and Sharpincpdm × Il1b−⁄− mice (Fig. 6j,k). These data demonstrate that although IL-1β delays the onset of dermatitis, it does not provide any protection from cellular dysregulation.
Discussion
The disease observed in SHARPIN-deficient mice is multifactorial and includes severe dermatitis associated with systemic inflammation and immune cell dysregulation1,2,18. Molecules involved in cell death pathways, including TNFR, FADD, and caspase-8, have a critical role in the development of dermatitis in Sharpincpdm mice7,8. However, whether genetic deletion of these molecules, which protects Sharpincpdm mice from dermatitis7,8, also prevents systemic inflammation and immune cell dysregulation has not been thoroughly investigated.
Recent studies from two different groups have demonstrated T-cell intrinsic roles for SHARPIN, revealing a requirement for SHARPIN in regulatory T-cell development and function19,20. Herein, our studies demonstrate that immune cell dysregulation precedes the development of dermatitis in Sharpincpdm mice. However, SHARPIN-deficient immune cells are not sufficient to establish dermatitis when transferred to WT recipients, as the Sharpincpdm ≫ WT chimeras do not develop any signs of dermatitis, even up to 12 months of age8. Supporting this notion, T and B cell–deficient Sharpincpdm mice (Sharpincpdm × Rag−⁄− mice) develop dermatitis, although with reduced systemic inflammation21. Conversely, Sharpincdpm skin sections that are grafted into nude mice (mice deficient in T cells) maintain their inflamed phenotype even at 3 months post transplant22. Taken together, it could be proposed that SHARPIN has distinct roles in the initiation of immune cell dysregulation and dermatitis and that skin intrinsic defects drive dermatitis in Sharpincdpm mice. Importantly, although dysregulated immune cells in Sharpincpdm mice might not be necessary to instigate dermatitis, they are involved in the development of systemic inflammation and their potential role in exacerbating dermatitis in Sharpincdpm mice cannot be excluded.
We have previously shown that SHARPIN is a critical regulator of the NLRP3 inflammasome in mouse bone marrow–derived macrophages and dendritic cells23. Macrophages and dendritic cells deficient in SHARPIN are unable to activate caspase-1 and produce IL-1β and IL-18 in response to both canonical (LPS + ATP, LPS + nigericin) and non-canonical (Citrobacter rodentium infection) activators of the NLRP3 inflammasome23. This work was further corroborated by studies showing that HOIL-1, which comprises the LUBAC in the presence of SHARPIN and HOIP4,5,6, is required for activation of the NLRP3 inflammasome in mouse bone marrow–derived macrophages24. In contrast, the lack of SHARPIN promotes NLRP3 inflammasome activation and the secretion of IL-1β, IL-1α, and IL-18 in mouse skin tissues9. As a result, Sharpincpdm mice deficient in NLRP3 or caspase-1 demonstrate a delayed onset of dermatitis9. Altogether, these results point towards specific roles of SHARPIN in myeloid cells and keratinocytes. Further investigations are required to determine the specific nature of SHARPIN functions in different cell types3.
The NLRP3 inflammasome regulates the production of IL-1 cytokines and, thus, the IL-1R signaling axis25. In line with the proposed role for NLRP3 in instigating dermatitis9, IL-1R deficiency also delays the onset of disease in Sharpincpdm mice8. Both IL-1α and IL-1β signal through IL-1R26. Recent studies from our laboratory have demonstrated that IL-1β and IL-1α play specific roles in mediating distinct inflammatory diseases27,28,29,30. Although IL-1β promotes an inflammatory bone disorder associated with a mouse model of osteomyelitis27,29, IL-1α is specifically required to promote dermatitis in a mouse model of neutrophilic dermatoses30. The specific nature of IL-1α and IL-1β in regulating inflammatory diseases prompted us to examine the contribution of these cytokines in disease progression in Sharpincpdm mice.
Both IL-1α and IL-1β cytokines are upregulated in the diseased Sharpincpdm mice9. Cell death pathways involving TNFR, caspase-8, FADD, RIPK3, and RIPK1 are all involved in the disease progression of Sharpincpdm mice3. Because IL-1α is released following cell death and plays an important role in the skin inflammation observed in a mouse model of neutrophilic dermatoses31, we proposed that IL-1α would have a major role in driving the disease in Sharpincpdm mice. However, IL-1α deficiency did not provide any protection from dermatitis or systemic inflammation in Sharpincpdm mice. These results argue for careful examination of the cause of inflammatory diseases before prescribing a specific treatment therapy.
Although IL-1β deficiency delayed the progression of disease in Sharpincpdm mice, the disease curves of Sharpincpdm × Il1b−⁄− mice (Fig. 6) were slightly accelerated than that of Sharpincpdm × Il1r−⁄− mice (Fig. 4). Given that both IL-1α and IL-1β signals through IL-1R, the difference in disease curves of Sharpincpdm × Il1b−⁄− and Sharpincpdm × Il1r−⁄− mice suggests a possible role for IL-1α as well. Interestingly, IL-1α deficiency does not provide any significant protection from disease instigation in Sharpincpdm mice, suggesting a minor role of IL-1α that is revealed upon genetic ablation of IL-1β. Given our hypothesis, we expect that disease curves of Sharpincpdm × Il1a−⁄− × Il1b−⁄− mice will be similar to that of Sharpincpdm × Il1r−⁄− mice.
Our results herein demonstrate that IL-1β is specifically required for the development of dermatitis, but not cellular dysregulation, in Sharpincpdm mice. These results raise several important points that need to be considered. It is possible that other inflammasome-dependent cytokines and effector molecules downstream of caspase-1 could be involved in cellular dysregulation and/or dermatitis development. Specifically, the role of IL-18 in induction of these diseases in Sharpincdpm mice has not been investigated. However, caspase-1–deficiency in Sharpincpdm mice does not prevent splenomegaly, suggesting that the dysregulation of immune cells might be inflammasome-independent9. NLRP3 inflammasome activation and release of IL-1β from the cell are associated with pyroptotic cell death. Specifically, pyroptosis is mediated by cleavage of gasdermin D32,33. Given that several cell death modalities are critical in driving dermatitis in Sharpincpdm mice3, it is important to investigate the role of gasdermin D in this inflammatory disease. It will also be of importance to thoroughly investigate whether cellular dysregulation is rescued in Sharpincpdm mice lacking TNF, TNFR, or RIPK1 kinase activity (all these mice are completely protected from developing dermatitis)3.
In conclusion, our study examined various cell populations in both the spleen and PBLs and established cellular parameters that can be used to determine cellular dysregulation in Sharpincpdm mice. Our results demonstrate that cellular dysregulation precedes dermatitis in Sharpincpdm mice; however, dermatitis and cellular dysregulation have distinct immunological underpinnings. Our results further show that the onset of dermatitis is specifically modulated by IL-1β, but not by IL-1α. Interestingly, deficiency of IL-1β does not rescue cellular dysregulation, similar to what has been reported for caspase-1/-11–deficient Sharpincpdm mice. Specific effector molecules that promote cellular dysregulation still elude us, and future studies will be required to completely understand and unravel the molecular mechanisms involved in the instigation of this complex disease. Finally, our study provides further evidence that IL-1β and IL-1α have specific roles in regulating inflammatory diseases and appeal for the use of specific therapeutics in treating IL-1–driven diseases.
Methods
Guideline statement
All methods used in this study are in accordance with protocols approved by St. Jude Children’s Research Hospital. All studies and experiments were conducted under guidelines and protocols approved by St. Jude Children’s Research Hospital’s Committee on the Use and Care of Animals.
Mice
C57BL/6J and Sharpincpdm (stock no: 007599) mice were purchased from The Jackson Laboratory and bred at St. Jude Children’s Research Hospital in a specific pathogen–free animal care facility. Il1a−⁄− 34, Il1b−⁄− 35, and Il1r−⁄− 36 mice have been previously described and were bred with Sharpincpdm mice to generate Sharpincpdm × Il1a−⁄−, Sharpincpdm × Il1b−⁄−, and Sharpincpdm × Il1r−⁄− crosses. Controls used in all figures include combinations of SharpinWT and SharpinHT mice. SharpinHT mice are completely normal and do not develop any dermatitis or inflammatory disease7,8. Animal studies were conducted under protocols approved by St. Jude Children’s Research Hospital’s Committee on the Use and Care of Animals.
Generation of chimeras
To generate Sharpincpdm ≫ WT and WT ≫ WT chimeras, WT recipients were lethally irradiated with 900 rads using the Cesium-137 irradiator. Donor bone marrow cells were harvested from the hind limbs (femur and tibia) of Sharpincpdm and WT mice and single cell suspension of bone marrow cells was made. Approximately 5 × 106 Sharpincpdm and WT bone marrow cells were transferred to the lethally irradiated recipients after 6 hours to generate the respective chimeras. These chimeras were followed for up to 120 days and monitored for any signs of disease and dermatitis.
Scoring of mice for dermatitis for disease-free curves
Sharpincpdm, Sharpincpdm × Il1a−⁄−, Sharpincpdm × Il1b−⁄−, and Sharpincpdm × Il1r−⁄− mice were examined twice weekly for signs of dermatitis. The mice were scored as diseased on the day that the first signs of dermatitis were observed.
Spleen and PBL processing, fluorescent antibody staining, and flow cytometry analysis
Spleens were harvested from mice after euthanasia, grinded by using a 3-mL syringe plunger, and passed through a 40-μm filter to generate single-cell suspensions. Splenocytes were then treated with 2 mL of ammonium-chloride-potassium (ACK) lysis buffer for 3 minutes to lyse red blood cells (RBCs). After RBC lysis, splenocytes were re-suspended in FACS buffer (PBS + 0.01% NaN3 + 2% FBS) and stained with appropriate flow cytometry antibodies.
PBLs (100 μL) were removed from mice through the retroorbital sinus by using a capillary tube (Drummond Scientific Company, Cat # 2-000-100) and collected in 1.5-mL centrifuge tubes. ACK lysis buffer (1 mL) was added to the cells for 5 minutes to lyse RBCs. After washing, if RBCs still remained, then the process with the ACK lysis buffer was repeated. Following complete RBC lysis, PBLs were stained with flow cytometry antibodies.
RBC-free, single-cell suspensions from spleen or PBL were stained with FITC anti-CD11a (2D7), PE anti-MHCII (M5/114.15.2), PerCP Cy5.5 anti-CD4 (RM4-5), PerCP Cy5.5 anti-Gr1 (RB6-8C5), APC anti-CD44 (IM7), APC anti-CD19 (6D5), eFluor455 anti-CD8 (53–6.7), and eFluor450 anti-CD11b (M1/70) monoclonal antibodies as previously described37. Fluorescently labeled cells were then analyzed by using FACS Calibur (BD Biosciences) and FlowJo software (GraphPad PRISM 6, GraphPad Sofware).
Images and Histopathology
Mouse images were acquired by using a Canon digital camera. Formalin-preserved skin sections were processed and embedded in paraffin according to standard procedures. Sections (5-μm thick) were stained with hematoxylin and eosin (H&E), and images were acquired using light Nikon widefield light microscope.
Statistical Analysis
All data are represented as the means ± s.e.m., and all experiments were repeated at least twice.
Additional Information
How to cite this article: Gurung, P. et al. Distinct role of IL-1β in instigating disease in Sharpincpdm mice. Sci. Rep. 6, 36634; doi: 10.1038/srep36634 (2016).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
HogenEsch, H. et al. A spontaneous mutation characterized by chronic proliferative dermatitis in C57BL mice. Am J Pathol 143, 972–982 (1993).
Seymour, R. E. et al. Spontaneous mutations in the mouse Sharpin gene result in multiorgan inflammation, immune system dysregulation and dermatitis. Genes Immun 8, 416–421 (2007).
Gurung, P. & Kanneganti, T. D. Autoinflammatory Skin Disorders: The Inflammasomme in Focus. Trends Mol Med (2016).
Gerlach, B. et al. Linear ubiquitination prevents inflammation and regulates immune signalling. Nature 471, 591–596 (2011).
Ikeda, F. et al. SHARPIN forms a linear ubiquitin ligase complex regulating NF-kappaB activity and apoptosis. Nature 471, 637–641 (2011).
Tokunaga, F. et al. SHARPIN is a component of the NF-kappaB-activating linear ubiquitin chain assembly complex. Nature 471, 633–636 (2011).
Kumari, S. et al. Sharpin prevents skin inflammation by inhibiting TNFR1-induced keratinocyte apoptosis. Elife 3 (2014).
Rickard, J. A. et al. TNFR1-dependent cell death drives inflammation in Sharpin-deficient mice. Elife 3 (2014).
Douglas, T., Champagne, C., Morizot, A., Lapointe, J. M. & Saleh, M. The Inflammatory Caspases-1 and -11 Mediate the Pathogenesis of Dermatitis in Sharpin-Deficient Mice. J Immunol 195, 2365–2373 (2015).
Dinarello, C. A. IL-1: discoveries, controversies and future directions. Eur J Immunol 40, 599–606 (2010).
Garlanda, C., Dinarello, C. A. & Mantovani, A. The interleukin-1 family: back to the future. Immunity 39, 1003–1018 (2013).
Kanneganti, T. D. The inflammasome: firing up innate immunity. Immunol Rev 265, 1–5 (2015).
Lamkanfi, M. & Kanneganti, T. D. Nlrp3: an immune sensor of cellular stress and infection. Int J Biochem Cell Biol 42, 792–795 (2010).
Man, S. M. & Kanneganti, T. D. Regulation of inflammasome activation. Immunol Rev 265, 6–21 (2015).
McDermott, D. S. & Varga, S. M. Quantifying antigen-specific CD4 T cells during a viral infection: CD4 T cell responses are larger than we think. J Immunol 187, 5568–5576 (2011).
Rai, D., Pham, N. L., Harty, J. T. & Badovinac, V. P. Tracking the total CD8 T cell response to infection reveals substantial discordance in magnitude and kinetics between inbred and outbred hosts. J Immunol 183, 7672–7681 (2009).
Berger, S. B. et al. Cutting Edge: RIP1 kinase activity is dispensable for normal development but is a key regulator of inflammation in SHARPIN-deficient mice. J Immunol 192, 5476–5480 (2014).
HogenEsch, H., Janke, S., Boggess, D. & Sundberg, J. P. Absence of Peyer’s patches and abnormal lymphoid architecture in chronic proliferative dermatitis (cpdm/cpdm) mice. J Immunol 162, 3890–3896 (1999).
Redecke, V., Chaturvedi, V., Kuriakose, J. & Hacker, H. SHARPIN controls the development of regulatory T cells. Immunology 148, 216–226 (2016).
Park, Y. et al. SHARPIN controls regulatory T cells by negatively modulating the T cell antigen receptor complex. Nat Immunol 17, 286–296 (2016).
Potter, C. S. et al. Chronic proliferative dermatitis in Sharpin null mice: development of an autoinflammatory disease in the absence of B and T lymphocytes and IL4/IL13 signaling. PLoS One 9, e85666 (2014).
Gijbels, M. J., HogenEsch, H., Bruijnzeel, P. L., Elliott, G. R. & Zurcher, C. Maintenance of donor phenotype after full-thickness skin transplantation from mice with chronic proliferative dermatitis (cpdm/cpdm) to C57BL/Ka and nude mice and vice versa. J Invest Dermatol 105, 769–773 (1995).
Gurung, P., Lamkanfi, M. & Kanneganti, T. D. Cutting edge: SHARPIN is required for optimal NLRP3 inflammasome activation. J Immunol 194, 2064–2067 (2015).
Rodgers, M. A. et al. The linear ubiquitin assembly complex (LUBAC) is essential for NLRP3 inflammasome activation. J Exp Med 211, 1333–1347 (2014).
Gurung, P., Lukens, J. R. & Kanneganti, T. D. Mitochondria: diversity in the regulation of the NLRP3 inflammasome. Trends Mol Med 21, 193–201 (2015).
Cavalli, G. & Dinarello, C. A. Treating rheumatological diseases and co-morbidities with interleukin-1 blocking therapies. Rheumatology (Oxford) 54, 2134–2144 (2015).
Lukens, J. R. et al. Critical role for inflammasome-independent IL-1beta production in osteomyelitis. Proc Natl Acad Sci USA 111, 1066–1071 (2014).
Gurung, P., Burton, A. & Kanneganti, T. D. NLRP3 inflammasome plays a redundant role with caspase 8 to promote IL-1beta-mediated osteomyelitis. Proc Natl Acad Sci USA 113, 4452–4457 (2016).
Lukens, J. R. et al. Dietary modulation of the microbiome affects autoinflammatory disease. Nature 516, 246–249 (2014).
Lukens, J. R. et al. RIP1-driven autoinflammation targets IL-1alpha independently of inflammasomes and RIP3. Nature 498, 224–227 (2013).
Lukens, J. R. & Kanneganti, T. D. SHP-1 and IL-1alpha conspire to provoke neutrophilic dermatoses. Rare Dis 2, e27742 (2014).
Kayagaki, N. et al. Caspase-11 cleaves gasdermin D for non-canonical inflammasome signalling. Nature 526, 666–671 (2015).
Shi, J. et al. Cleavage of GSDMD by inflammatory caspases determines pyroptotic cell death. Nature 526, 660–665 (2015).
Matsuki, T., Nakae, S., Sudo, K., Horai, R. & Iwakura, Y. Abnormal T cell activation caused by the imbalance of the IL-1/IL-1R antagonist system is responsible for the development of experimental autoimmune encephalomyelitis. Int Immunol 18, 399–407 (2006).
Shornick, L. P. et al. Mice deficient in IL-1beta manifest impaired contact hypersensitivity to trinitrochlorobenzone. J Exp Med 183, 1427–1436 (1996).
Glaccum, M. B. et al. Phenotypic and functional characterization of mice that lack the type I receptor for IL-1. J Immunol 159, 3364–3371 (1997).
Gurung, P. et al. An NLRP3 inflammasome-triggered Th2-biased adaptive immune response promotes leishmaniasis. J Clin Invest 125, 1329–1338 (2015).
Acknowledgements
We thank Dr. Cherise M Guess for her help with scientific editing of the manuscript. We also thank Drs. Si Ming Man and Ankit Malik for their help with manuscript editing. Images were acquired at the SJCRH Cell & Tissue Imaging Center, which is supported by SJCRH and NCI P30 CA021765-35. T.-D.K. is supported by grants from the National Institute of Health (Grants AI101935, AI124346, AR056296 and CA163507) and by American Lebanese Syrian Associated Charities (ALSAC).
Author information
Authors and Affiliations
Contributions
P.G. and T.DK. designed the study. P.G. and B.R.S. performed experiments. P.G. and T.D.K. analyzed the data and wrote the manuscript. T.D.K. oversaw the project.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Gurung, P., Sharma, B. & Kanneganti, TD. Distinct role of IL-1β in instigating disease in Sharpincpdm mice. Sci Rep 6, 36634 (2016). https://doi.org/10.1038/srep36634
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep36634
This article is cited by
-
The mechanism of linear ubiquitination in regulating cell death and correlative diseases
Cell Death & Disease (2023)
-
SHARPIN: Role in Finding NEMO and in Amyloid-Beta Clearance and Degradation (ABCD) Pathway in Alzheimer’s Disease?
Cellular and Molecular Neurobiology (2022)
-
Innate immune adaptor MyD88 deficiency prevents skin inflammation in SHARPIN-deficient mice
Cell Death & Differentiation (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.