Abstract
The association between alcohol intake and colorectal cancer (CRC) may vary secondary to single nucleotide polymorphisms (SNPs) in two pathways related to alcohol intake. 375 cases of CRC were identified among 38 373 Japan Public Health Center-based prospective Study (JPHC Study) participants who had returned a baseline questionnaire, reported no diagnosis of any cancer and provided blood samples. For each case, two controls were selected on matching variables. Logistic regression models were used to determine matched Odds Ratios (OR) and 95% Confidence Intervals (CI) for the association between alcohol consumption, genetic polymorphisms of enzymes in the alcohol- and folate metabolic pathways (e.g. methylenetetrahydrofolate reductase (MTHFR) rs1801133) and CRC risk. Compared to never/occasional alcohol intake, moderate to heavy alcohol intake was associated with CRC (OR = 2.12, 95% CI, 1.34–3.36). When compared to the CC genotype, the MTHFR rs1801133 CT/TT genotype was inversely associated with CRC (OR = 0.72, 95% CI, 0.54–0.97). Never/occasional consumers of alcohol with the MTHFR rs1801133 CT/TT genotype were also at a reduced risk of CRC compared to never/occasional drinkers with the CC genotype (OR = 0.68, 95% CI, 0.47–0.98) (P for interaction = 0.27). The results indicate that the folate pathway is likely to be involved in alcohol-related CRC development.
Similar content being viewed by others
Introduction
Alcohol consumption is a well-known and established risk factor for colorectal cancer (CRC)1,2,3,4,5,6 with studies proposing a causal relation between alcohol consumption and CRC risk4,7. Alcohol differs from other dietary risk factors for CRC as it is suggested to increase CRC risk through two separate pathways: 1) the alcohol metabolic pathway which involves the oxidation of ethanol into acetaldehyde and subsequently acetate, resulting in cell exposure to the potentially carcinogenic metabolite acetaldehyde8, and 2) the folate metabolic pathway where alcohol acts as a folate antagonist resulting in folate deficiency9 which may lead to DNA hypo-methylation and aberrant DNA synthesis10. Conversely, high folate status such as high folate intake or low alcohol consumption are associated with a reduced risk of CRC11.
In addition to the above, single nucleotide polymorphisms (SNPs) may modify individual susceptibility to CRC by affecting important enzymes in either of the two metabolic pathways. E.g., in the alcohol metabolic pathway, aldehyde dehydrogenase-2 (ALDH2) rs671 polymorphisms result in enzymatic activity that is reduced (ALDH2 rs671 GA genotype) or absent (ALDH2 rs671 AA genotype) which in turn leads to the accumulation of, and increased exposure to acetaldehyde following alcohol intake12. In the folate metabolic pathway, 5,10-methylenetetrahydrofolate reductase (MTHFR) rs1801133 polymorphisms reduce MTHFR activity (MTHFR rs1801133 CT/TT genotype) and shift the available folate pool from DNA methylation to DNA synthesis, in particular in individuals with the MTHFR rs1801133 TT genotype and a concomitantly high folate status13.
Only limited information is available from prospective studies on the effect of genetic polymorphisms of enzymes in the alcohol metabolic pathway (alcohol dehydrogenase 1B (ADH1B) rs1229984, ALDH2 rs671, cytochrome P450 2E1 (CYP2E1) rs3813867) and the folate metabolic pathway (MTHFR rs1801133, MTHFR rs1801131, methionine synthase (MTR) rs1805087, and methionine synthase reductase (MTRR) rs1801394) respectively, and their interaction with alcohol consumption. The aim of the current study was thus to investigate the effect of gene-alcohol interactions on CRC risk using a nested case-control study within the Japan Public Health Center-based prospective Study (JPHC Study). We hypothesize that genetic variants of alcohol- and folate metabolic enzymes will modify the association between alcohol intake and CRC risk as described in previous studies.
Method
Study population (including questionnaire survey and blood collection)
The JPHC Study14 is a large cohort with a baseline population of 140 420 individuals, and was conducted in two cohorts: Cohort I, aged 40–59, was initiated in 1990 and Cohort II, aged 40–69, was started in 1993. JPHC Study participants were identified by the population registries maintained by the local municipalities in 11 public health center (PHC) areas. The JPHC Study, including all methods described in the present study, has been approved by the Institutional Review Board of the National Cancer Center (approval number: 13-021) and the University of Tokyo (approval number: 10508), with reference to relevant ethical guidelines for medical research in Japan. Informed consent was obtained from each participant implicitly when they completed the baseline questionnaire, in which the purpose of the study and follow-up methods were described. Written information on the study was mailed to each participant and is published on the study web site ( http://epi.ncc.go.jp/jphc).
Study participants were asked to provide information through a self-administered questionnaire which included questions on personal and familial medical histories and lifestyle factors including smoking, alcohol consumption, physical exercise and dietary habits. Dietary habits were assessed through a food frequency questionnaire containing 44 items for Cohort I and 52 items for Cohort II. A total of 113 461 individuals returned the questionnaire. Additionally, collected at the time of health check-up (Cohort I 1990–1992; Cohort II: 1993–1995), 49 011 individuals donated 10-ml of venous blood drawn into vacutainer tubes containing heparin. Samples were divided into plasma and buffy layers, and preserved at −80 °C until analysis.
Selection of cases and controls (including follow-up)
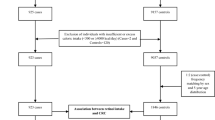
Cancer site and histology were coded using the International Classification of Diseases for Oncology, Third Edition (ICD-O-3)15. Details on the selection of cases and controls have been discussed elsewhere16. In brief, 375 cases of colorectal cancer (CRC) were identified up to 31 December 2003 through two sources: local major hospitals and population-based cancer registries. These cases occurred among a cohort of eligible subjects who had returned the baseline questionnaire, provided blood samples and reported no diagnosis of any cancer (n = 38 373 not including 13 ineligible subjects). All cases were pathologically confirmed as adenocarcinoma; 256 individuals were diagnosed with colon cancer (ICD-O-3: C180-C189) and 199 with rectal cancer (ICD-O-3: C199 and C209). For 370 of the 375 cases there was information about tumour depth; 120 tumours were of the intramucosal type and 250 of the invasive type.
Two controls were randomly selected from the cohort of 38 373 eligible subjects using incidence density sampling17. Controls, free of colorectal cancer history at the time when the case was diagnosed, were matched with each case on sex, age (within three years), date of blood drawn (within three months), time since last meal (within 4 hours) and study location (PHC area).
Assessment of alcohol consumption
Alcohol consumption during the baseline survey was assessed using a validated self-administered food frequency questionnaire (FFQ). The method has been described in detail elsewhere18, and the validity of FFQ-based alcohol consumption estimations have been evaluated for both Cohort I and Cohort II in JPHC Study subsamples19,20. In brief, Cohort I and Cohort II differed in their assessment of alcohol consumption. For Cohort I, there were six categories of alcohol consumption (almost never, 1–3 days per month, 1–2 days per week, 3–4 days per week, 5–6 days per week, and every day). For those drinking at least once per week, additional information was requested regarding amount and type of alcoholic beverage consumed, in addition to providing a consumption frequency score: 1.5 (1–2 days per week), 3.5 (3–4 days per week), 5.5 (5–6 days per week), and 7 (daily).
For Cohort II, information on alcohol consumption status (never, former, or current) was obtained with details on alcohol consumption for former or current drinkers. Average consumption scores for Cohort II were: 1.5 (1–2 days per week), 3.5 (3–4 days per week), and 6 (almost daily).
Alcohol consumption was quantified in grams of ethanol by type of beverage consumed: 180 ml of shochu or awamori corresponded to 36 g of ethanol, 180 ml sake corresponded to 23 g, 633 ml of beer corresponded to 23 g, 30 ml of whiskey corresponded to 10 g, and 60 ml of wine corresponded to 6 g. Weekly ethanol intake was calculated by multiplying the frequency score with the quantity of alcohol consumed, and participants were categorised into one of three groups; never to occasional drinkers, <150, and ≥150 g of ethanol per week.
Laboratory assay
To conduct genetic research within the framework of the JPHC Study, we obtained an additional approval from the institutional review board of the National Cancer Center (approval number: 2011-044), Tokyo, Japan, and provided all eligible subjects who donated a blood sample with the opportunity to refuse participation in the research. Genomic DNA was extracted from white blood cells in the buffy coat layer using a FlexiGene DNA kit (Qiagen, Hilden, Germany). Buffy coat samples were not available for all 16 pairs (i.e. 48 subjects) in one PHC area of Cohort II (Suita, Osaka). All but 12 buffy coat samples provided a sufficient amount of genomic DNA, and thus the following genotyping was performed among 356 cases and 709 controls. 46 SNPs including ADH1B rs1229984, ALDH2 rs671, CYP2E1 rs3813867, MTHFR rs1801133 (also known as MTHFR C677T), MTHFR rs1801131 (MTHFR A1298C), MTRR rs1801394 (MTRR A66G), and MTR rs1805087 (MTR A2756G ) were genotyped on the BioMark Dynamic Array platform (Fluidigm Corporation, South San Francisco, CA, USA) using the TaqMan SNP Genotyping Assays/Drug metabolism Genotyping Assays (Applied Biosystems, Foster City, CA) at GeneticLab, Hokkaido, Japan. Samples of cases and matched controls were genotyped in the same batch. All laboratory personnel were blinded with respect to case and control status.
Statistical Analysis
Differences in baseline characteristics between cases and controls were determined using the Chi-square test for categorical variables and the Wilcoxon signed rank sum test for continuous variables. Conditional logistic regression models were used to determine matched Odds Ratios (OR) and 95% Confidence Intervals (CI) for the association between alcohol consumption, polymorphisms (ADH1B rs1229984, ALDH2 rs671, CYP2E1 rs3813867, MTHFR rs1801133, MTHFR rs1801131, MTRR rs1801394, and MTR rs1805087) and CRC risk. Model 1 (OR1) was matched for age (±3 years), sex, area, blood donation date (±2 months), and fasting time at blood donation (±5 hours). Model 2 (OR2) was further adjusted for smoking status, body mass index, family history of colorectal cancer, physical activity, and energy adjusted intake of red meat, processed meat, vegetables, fruits, fish, calcium, vitamin D, vitamin B2, vitamin B6, vitamin B12, and folate. Unconditional logistic regression models were used to determine the interaction between alcohol intake and polymorphisms of the alcohol- and folate- metabolic pathway in relation to the risk of CRC.
The Chi-square test was used to test for departures of the genotype distribution from the Hardy Weinberg equilibrium. Statistical analyses were performed using SAS (SAS software version 9.3; SAS Institute Inc., Cary, NC). The significance level was set as p < 0.05.
Results
There were no statistically significant differences between cases and controls for any of the selected baseline characteristics (Table 1).
Alcohol intake was positively associated with colorectal cancer in both the minimally (OR = 1.66, 95% CI, 1.10–2.51) and fully adjusted conditional models (OR = 2.12, 95% CI, 1.34–3.36) (Table 2). In contrast, folate intake was not apparently associated with the risk of CRC.
All genotype frequencies (ADH1B rs1229984, ALDH2 rs671, CYP2E1 rs3813867, MTHFR rs1801133, MTHFR rs1801131, MTRR rs1801394, and MTR rs1805087) among controls were consistent with the Hardy Weinberg equilibrium (p > 0.05).
SNPs in the genes of alcohol-metabolic enzymes (ADH1B rs1229984, ALDH2 rs671, and CYP2E1 rs3813867) were not significantly associated with CRC risk (Table 2). Among SNPs in the genes of folate-metabolic enzymes, the MTHFR rs1801133 CT/TT genotype showed a reduced risk of CRC (OR = 0.72, 95% CI, 0.54–0.97) compared to the MTHFR rs1801133 CC genotype. The inverse association was significant in individuals with the MTHFR rs1801133 CT genotype (OR = 0.66, 95% CI, 0.48–0.91), while non-significant in those with the MTHFR rs1801133 TT genotype (OR = 0.87, 95% CI, 0.58–1.30).
We did not observe any interaction between alcohol intake and SNPs in the genes of alcohol- and folate metabolic enzymes in relation to the risk of CRC (p > 0.05, Table 3). In general, increased alcohol intake was positively associated with the risk of CRC irrespective of genotype. Of interest, among never/occasional drinkers, the MTHFR rs1801133 CT/TT genotype was related to a decreased risk of CRC (OR = 0.68, 95% CI, 0.47–0.98) compared to the MTHFR rs1801133 CC genotype. More precisely, the corresponding ORs were 0.71 (95% CI, 0.48–1.05) and 0.60 (95% CI, 0.36–1.01) for the MTHFR rs1801133 CT and TT genotype respectively. When further stratified by folate intake, we observed a similarly but non-significantly decreased risk among never/occasional drinkers with the MTHFR rs1801133 CT/TT genotype irrespective of their folate intake levels (Supplementary Table S1).
Sensitivity analyses excluding cases in the first two years of follow-up yielded similar results for Tables 2 and 3 (data not shown).
Discussion
Our findings show that moderate to heavy alcohol consumption increases the risk of CRC, whereas the MTHFR rs1801133 CT/TT genotype is inversely associated with CRC risk. Moreover, individuals with low alcohol consumption and the MTHFR rs1801133 CT/TT genotype were at a significantly reduced risk of CRC, while those with high alcohol consumption and the MTHFR rs1801133 CC genotype were at a significantly increased risk.
Our result of a potentially protective effect of the MTHFR rs1801133 CT/TT genotype on CRC is in accordance with previous findings21,22,23,24. The primary function of MTHFR is to catalyse the conversion of 5,10-methylenetetrahydrofolate to 5-methyltetrahydrofolate25. Individuals with the MTHFR rs1801133 CT/TT genotype are known to have the enzyme with a decreased activity, and likely have accumulated levels of 5,10-methylenetetrahydrofolate. Increased levels of 5,10-methylenetetrahydrofolate would allow for increased DNA synthesis1, and may thereby reduce the risk of CRC. Although it has been suggested that the MTHFR rs1801133 CT and TT genotype are related to a 35% and 70% reduction in the enzyme activity respectively26, we did not observe any apparent difference in a reduced risk of CRC between individuals with the CT and TT genotype.
We failed to find any associations between the MTHFR rs1801131 polymorphism and CRC. Previous studies have reported both an inverse and positive association between the MTHFR rs1801131 CC genotype and colon cancer27 and CRC28 respectively when compared to the MTHFR rs1801131 AA/AC genotype at low folate or high alcohol intake levels. Possible reasons for the discrepant results could be differences in end points between studies (i.e. colon cancer vs CRC) or the small sample sizes used28. In addition, our study could not find any association between MTR rs1805087 or MTRR rs1801394 polymorphisms and CRC risk.
Although some findings suggest that variant alleles in the genes of alcohol-metabolic enzymes are the main culprits of alcohol-related CRC29,30,31,32,33, other findings have instead shown that genetic variants of alcohol metabolic enzymes do not increase CRC risk34,35 and do not modify the effect of alcohol on CRC5,36. Our own findings show that the associations of ADH1B rs1229984, and CYP2E1 rs3813867 polymorphisms with CRC remain close to one whereas ALDH2 rs671 polymorphisms may even be inversely associated with CRC. A possibly protective effect of ALDH2 rs671 polymorphism is counter-intuitive due to the potentially carcinogenic effects of acetaldehyde8, but the frequency of daily drinkers among those with the ALDH2 rs671 AA genotype in the current study was very low (n = 2) which prevents us from drawing any conclusion from these results.
There are several limitations that need to be mentioned: Health check-up participants have healthier lifestyle habits compared to their counterparts37 which could lead to an underestimation of our results. We grouped minor allele homozygotes with minor allele heterozygotes which could lead to further underestimation of results. Finally, results may not be generalizable to other populations.
Despite such limitations, this study has a major strength: due to the prospective nature of the study, all data was collected before development of disease thereby minimizing recall bias and strengthening any associations found between predictors and outcome.
In summary, alcohol consumption is positively associated with CRC, whereas the MTHFR rs1801133 CT/TT genotype is inversely associated with CRC risk. Furthermore, low grade alcohol consumption together with the MTHFR rs1801133 CT/TT genotype reduces CRC risk whereas high grade alcohol consumption together with the MTHFR rs1801133 CC genotype increases CRC risk. These findings indicate that the folate metabolic pathway is likely to be involved in alcohol-related CRC development.
Additional Information
How to cite this article: Svensson, T. et al. Alcohol consumption, genetic variants in the alcohol- and folate metabolic pathways and colorectal cancer risk: the JPHC Study. Sci. Rep. 6, 36607; doi: 10.1038/srep36607 (2016).
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Chen, J. et al. A methylenetetrahydrofolate reductase polymorphism and the risk of colorectal cancer. Cancer research 56, 4862–4864 (1996).
Cho, E. et al. Alcohol intake and colorectal cancer: a pooled analysis of 8 cohort studies. Ann Intern Med 140, 603–613 (2004).
Ferrari, P. et al. Lifetime and baseline alcohol intake and risk of colon and rectal cancers in the European prospective investigation into cancer and nutrition (EPIC). Int J Cancer 121, 2065–2072, doi: 10.1002/ijc.22966 (2007).
Fedirko, V. et al. Alcohol drinking and colorectal cancer risk: an overall and dose-response meta-analysis of published studies. Ann Oncol 22, 1958–1972, doi: 10.1093/annonc/mdq653 (2011).
Crous-Bou, M. et al. Polymorphisms in alcohol metabolism genes ADH1B and ALDH2, alcohol consumption and colorectal cancer. PLoS One 8, e80158, doi: 10.1371/journal.pone.0080158 (2013).
Mizoue, T. et al. Alcohol drinking and colorectal cancer in Japanese: a pooled analysis of results from five cohort studies. Am J Epidemiol 167, 1397–1406, doi: 10.1093/aje/kwn073 (2008).
Boffetta, P. & Hashibe, M. Alcohol and cancer. Lancet Oncol 7, 149–156, doi: 10.1016/S1470-2045(06)70577-0 (2006).
Seitz, H. K. & Stickel, F. Molecular mechanisms of alcohol-mediated carcinogenesis. Nat Rev Cancer 7, 599–612, doi: 10.1038/nrc2191 (2007).
Halsted, C. H., Villanueva, J. A., Devlin, A. M. & Chandler, C. J. Metabolic interactions of alcohol and folate. J Nutr 132, 2367S–2372S (2002).
Duthie, S. J. Folic acid deficiency and cancer: mechanisms of DNA instability. Br Med Bull 55, 578–592 (1999).
Freudenheim, J. L. et al. Folate intake and carcinogenesis of the colon and rectum. Int J Epidemiol 20, 368–374 (1991).
Poschl, G. & Seitz, H. K. Alcohol and cancer. Alcohol Alcohol 39, 155–165 (2004).
Giovannucci, E. Alcohol, one-carbon metabolism, and colorectal cancer: recent insights from molecular studies. J Nutr 134, 2475S–2481S (2004).
Tsugane, S. & Sawada, N. The JPHC study: design and some findings on the typical Japanese diet. Japanese journal of clinical oncology 44, 777–782, doi: 10.1093/jjco/hyu096 (2014).
World Health Organization (Geneva, Switzerland, 2000).
Otani, T. et al. Plasma C-reactive protein and risk of colorectal cancer in a nested case-control study: Japan Public Health Center-based prospective study. Cancer Epidemiol Biomarkers Prev 15, 690–695, doi: 10.1158/1055-9965.EPI-05-0708 (2006).
Rothman, K. J., Greenland, S. & Lash, T. L. Modern Epidemiology, 3rd Edition 116 (Lippincott Williams & Wilkins, 2008).
Hidaka, A. et al. Genetic polymorphisms of ADH1B, ADH1C and ALDH2, alcohol consumption, and the risk of gastric cancer: the Japan Public Health Center-based prospective study. Carcinogenesis 36, 223–231, doi: 10.1093/carcin/bgu244 (2015).
Tsubono, Y., Kobayashi, M., Sasaki, S. & Tsugane, S. & Jphc. Validity and reproducibility of a self-administered food frequency questionnaire used in the baseline survey of the JPHC Study Cohort I. J Epidemiol 13, S125–S133 (2003).
Otani, T. et al. Alcohol consumption, smoking, and subsequent risk of colorectal cancer in middle-aged and elderly Japanese men and women: Japan Public Health Center-based prospective study. Cancer Epidemiol Biomarkers Prev 12, 1492–1500 (2003).
Huang, Y., Han, S., Li, Y., Mao, Y. & Xie, Y. Different roles of MTHFR C677T and A1298C polymorphisms in colorectal adenoma and colorectal cancer: a meta-analysis. J Hum Genet 52, 73–85, doi: 10.1007/s10038-006-0082-5 (2007).
Hubner, R. A. & Houlston, R. S. MTHFR C677T and colorectal cancer risk: A meta-analysis of 25 populations. Int J Cancer 120, 1027–1035, doi: 10.1002/ijc.22440 (2007).
Zhong, S., Yang, J. H., Liu, K., Jiao, B. H. & Chang, Z. J. Quantitative assessment of the association between MTHFR C677T polymorphism and colorectal cancer risk in East Asians. Tumour Biol 33, 2041–2051, doi: 10.1007/s13277-012-0463-7 (2012).
Zhao, M., Li, X., Xing, C. & Zhou, B. Association of methylenetetrahydrofolate reductase C677T and A1298C polymorphisms with colorectal cancer risk: A meta-analysis. Biomed Rep 1, 781–791, doi: 10.3892/br.2013.134 (2013).
Sharp, L. & Little, J. Polymorphisms in genes involved in folate metabolism and colorectal neoplasia: a HuGE review. Am J Epidemiol 159, 423–443 (2004).
Frosst, P. et al. A candidate genetic risk factor for vascular disease: a common mutation in methylenetetrahydrofolate reductase. Nat Genet 10, 111–113, doi: 10.1038/ng0595-111 (1995).
Keku, T. et al. 5,10-Methylenetetrahydrofolate reductase codon 677 and 1298 polymorphisms and colon cancer in African Americans and whites. Cancer Epidemiol Biomarkers Prev 11, 1611–1621 (2002).
Yin, G. et al. Methylenetetrahydrofolate reductase C677T and A1298C polymorphisms and colorectal cancer: the Fukuoka Colorectal Cancer Study. Cancer Sci 95, 908–913 (2004).
Matsuo, K. et al. Aldehyde dehydrogenase 2 (ALDH2) genotype affects rectal cancer susceptibility due to alcohol consumption. J Epidemiol 12, 70–76 (2002).
Murata, M. et al. Genotype difference of aldehyde dehydrogenase 2 gene in alcohol drinkers influences the incidence of Japanese colorectal cancer patients. Jpn J Cancer Res 90, 711–719 (1999).
Yokoyama, A. et al. Alcohol-related cancers and aldehyde dehydrogenase-2 in Japanese alcoholics. Carcinogenesis 19, 1383–1387 (1998).
Gao, C. M. et al. Polymorphisms of alcohol dehydrogenase 2 and aldehyde dehydrogenase 2 and colorectal cancer risk in Chinese males. World J Gastroenterol 14, 5078–5083 (2008).
Yang, H. et al. A novel polymorphism rs1329149 of CYP2E1 and a known polymorphism rs671 of ALDH2 of alcohol metabolizing enzymes are associated with colorectal cancer in a southwestern Chinese population. Cancer Epidemiol Biomarkers Prev 18, 2522–2527, doi: 10.1158/1055-9965.EPI-09-0398 (2009).
Peng, H., Xie, S. K., Huang, M. J. & Ren, D. L. Associations of CYP2E1 rs2031920 and rs3813867 polymorphisms with colorectal cancer risk: a systemic review and meta-analysis. Tumour Biol 34, 2389–2395, doi: 10.1007/s13277-013-0788-x (2013).
Matsuo, K. et al. A gene-gene interaction between ALDH2 Glu487Lys and ADH2 His47Arg polymorphisms regarding the risk of colorectal cancer in Japan. Carcinogenesis 27, 1018–1023, doi: 10.1093/carcin/bgi282 (2006).
Yin, G. et al. Alcohol dehydrogenase and aldehyde dehydrogenase polymorphisms and colorectal cancer: the Fukuoka Colorectal Cancer Study. Cancer Sci 98, 1248–1253, doi: 10.1111/j.1349-7006.2007.00519.x (2007).
Iwasaki, M. et al. Background characteristics of basic health examination participants: the JPHC Study Baseline Survey. J Epidemiol 13, 216–225 (2003).
Acknowledgements
Thomas Svensson is a Research Fellow of Japan Society for the Promotion of Science (JSPS). Dr. Yamaji had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. We are indebted to the Aomori, Iwate, Ibaraki, Niigata, Osaka, Kochi, Nagasaki, and Okinawa Cancer Registries for providing their incidence data. We would like to thank all members of the JPHC Study group (listed in the appendix available as Supplementary Information) for their contribution. This study was supported by National Cancer Center Research and Development Fund (23-A-31[toku] and 26-A-2 since 2011, and 25-A-14 since 2013), a Grant-in-Aid for Cancer Research from the Ministry of Health, Labour and Welfare of Japan (from 1989 to 2010), Funds for integrated promotion of social system reform and research and development (37201101-01 from 2011 to 2013) from Japan Science and Technology Agency, and a Grant-in-Aid for Scientific Research C (15K08722 since 2015) from the Japan Society for the Promotion of Science. Manami Inoue is the beneficiary of a financial contribution from the AXA Research fund as a chair holder on the AXA Department of Health and Human Security, Graduate School of Medicine, The University of Tokyo. The AXA Research Fund had no role in the design, data collection, analysis, interpretation or manuscript drafting, or in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
Thomas Svensson provided substantial contributions to the analysis and interpretation of data for the work, drafting of the manuscript, and final approval of the version to be published; Shoichiro Tsugane, Motoki Iwasaki, Taiki Yamaji, Norie Sawada, Manami Inoue, Shizuka Sasazuki, and Taichi Shimazu provided substantial contributions to conception or design of the work, the acquisition, and interpretation of data for the work, revising it critically for important intellectual content, and gave final approval of the version to be published; Sanjeev Budhathoki, and Akihisa Hidaka provided substantial contributions to the interpretation of data for the work, revising it critically for important intellectual content, and gave final approval of the version to be published.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Svensson, T., Yamaji, T., Budhathoki, S. et al. Alcohol consumption, genetic variants in the alcohol- and folate metabolic pathways and colorectal cancer risk: the JPHC Study. Sci Rep 6, 36607 (2016). https://doi.org/10.1038/srep36607
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep36607
This article is cited by
-
MicroRNA-937 is overexpressed and predicts poor prognosis in patients with colon cancer
Diagnostic Pathology (2019)
-
Environmental Influences in the Etiology of Colorectal Cancer: the Premise of Metabolomics
Current Pharmacology Reports (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.