Abstract
Previous studies have demonstrated that afternoon naps can have a negative effect on subsequent nighttime sleep in children. These studies have mainly been based on sleep questionnaires completed by parents. To investigate the effect of napping on such aspects of sleep quality, we performed a study in which child activity and sleep levels were recorded using actigraphy. The parents were asked to attach actigraphy units to their child’s waist by an adjustable elastic belt and complete a sleep diary for 7 consecutive days. 50 healthy young toddlers of approximately 1.5 years of age were recruited. There was a significant negative correlation between nap duration and both nighttime sleep duration and sleep onset time, suggesting that long nap sleep induces short nighttime sleep duration and late sleep onset time. We also found a significant negative correlation between nap timing and nighttime sleep duration and also a significant positive correlation between nap timing and sleep onset time, suggesting that naps in the late afternoon also lead to short nighttime sleep duration and late sleep onset. Our findings suggest that duration-controlled naps starting early in the afternoon can induce a longer nighttime sleep in full-term infants of approximately 1.5 years of age.
Similar content being viewed by others
Introduction
The first few years of life are associated with marked changes in the amount and distribution of sleep. Between 0 and 5 years of age, the frequency of afternoon naps declines and the biphasic sleep-wake pattern gives way to a consolidated pattern of sleep occurring only at night. Moreover, the basic sleep structure for young children has been reported to be established by 1.5 years of age and remains similar at least until 5 years of age1,2,3,4,5,6.
There have been several population studies concerning changes in the amount and diurnal distribution of infants’ and children’s sleep mainly based on sleep questionnaires completed by parents, indicating that the longer the nap durations of children, the later they went to bed7,8,9,10. Using activity recording devices, Acebo et al.1 also confirmed similar effects of nap duration on the nighttime sleep of children. Although their study greatly contributed to the scientific understanding of sleep development of young children between 1 and 5 years of age, their study population was relatively small. In particular, the number of children aged 1.5 years-a key age at which children form their sleep structure-was less than 30. In addition, they calculated nap duration with a time resolution of 30 minute units and may have underestimated the effects of nap on bedtime timing since the nap duration of children aged 1.5 years is a relatively short duration of approximately 2 hours1. A recent systematic review also indicated that previous studies on infant sleep rely mostly on parent reports and suggested that the studies should use independent physiological measurement of sleep behaviors. The review concluded that there is consistent, but low-quality, evidence that napping is increasingly associated with delayed night sleep onset and disrupted night sleep at least at >2 years of age6.
In the current study, to examine the effects of daytime nap on the nighttime sleep quality of young toddlers of approximately 1.5 years of age, we investigated the daytime napping patterns and nocturnal sleep-wake patterns of 50 children using actigraphy and also examined if long nap duration actually deteriorates sleep quality in the subsequent night among toddlers. Our study is the first report on trends in actigraphic findings on daytime activity and nighttime sleep of young toddlers of 1.5 years of age, an age at which a regular child health examination is performed nationwide in Japan.
Results
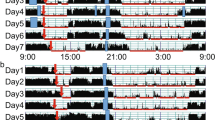
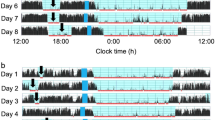
The characteristics of the 50 infants are shown in Table 1. Toddlers’ sleep environment is shown in Table 2. Toddlers’ sleep variables such as average bedtime, average wake time, average nighttime sleep duration and average nap duration are also shown in Table 3. No differences were found between boys and girls in any of the sleep variables (t-test, p > 0.05). In addition, no differences were found in the durations of naps and nighttime sleep between weekdays and weekends (t-test, p > 0.05). Figure 1 demonstrates representative daily activity-rest patterns of full-term infants of approximately 1.5 years of age, indicating the existence of various nap patterns among toddlers. There were significant negative correlations between nap duration and nighttime sleep duration (r = −0.57, p = 0.000) and also positive correlations between nap duration and sleep onset time (r = 0.37, p = 0.008) and nap-end time (r = 0.36, p = 0.011) (Table 4, Fig. 2). Like nap duration, we also found significant negative correlations between nap-end time and nighttime sleep duration (r = −0.31, p = 0.028) and positive correlation with sleep onset time (r = 0.52, p = 0.000) and nap duration (r = 0.36, p = 0.011) (Table 4, Fig. 3). The data suggested that both long nap duration and naps in the late afternoon induce short nighttime sleep duration and late sleep onset. The analysis also suggested that late nap-end time leads to long nap duration since a significant positive correlation between the nap-end time and nap duration were found.
The actograms show representative daily activity-rest patterns of full-term infants of approximately 1.5 years of age with advanced nap phases (a) and delayed nap phases (b). The vertical axis shows the 7 consecutive observation days and the horizontal axis shows the course of each 24 h day from 00:00 h (12:00 am) to 24:00 h (12:00 am). Activity counts per minute are represented by the height of the vertical black bars on each actogram. The arrows and the blue rectangles indicate naps and bathing periods, respectively. The red underlines are the periods that were automatically judged as sleep periods by the actigraph software.
Discussion
The present study indicates two significant factors influencing the nighttime sleep of toddlers at approximately 1.5 years of age. First, our actigraphic data confirm that, in 1.5-year-old children, naps affect nighttime sleep, consistent with previous studies based on sleep questionnaires, which have indicated that the longer the nap duration of children, the later they went to bed. Using actigraphy, the current study also found that ‘longer nap duration’ is significantly associated with shorter nighttime sleep duration and later sleep onset. However, our data differs from the actigraphic data of 1.5-year-old children from Acebo et al.1, in that their data did not show a significant association between nap duration and sleep onset time. The difference may come mainly from the time resolution used for nap recording (30 minute units and 1 minute units for Acebo et al.1 and the present study, respectively) because the toddlers’ average nap duration of 1.9 ± 0.8 hours in the present study could be under- or over-evaluated by a parents’ sleep diary using a 30-minute time resolution, which would tend to cause larger data variation. In addition, difference between the data by Acebo et al.1 and our data may also come from the difference in the sample number of children for statistical analysis (29 and 50 children for Acebo et al.1 and the present study, respectively). In addition a previous questionnaire study11 reporting that children (50–72 months, n = 168) who experienced >60 minutes of mandatory nap time in child care had significantly less nighttime sleep than those with 0 to 60 minutes of mandatory nap time. The same group also closely investigated the nap patterns of preschool children (3–5 years, n = 2,114)12. They reported that 83.5% of child care settings implemented a mandatory nap time (range = 15–145 min) while 14.2% provided alternate activities for children throughout the nap time period and also found that 31% of all children napped during nap times.
Second, the current study also described a new finding, which was that, like nap duration, “later nap-ending time” is significantly associated with shorter nighttime sleep duration, later sleep onset time and also nap durations. This suggests that parents might be able to prolong toddlers’ nighttime sleep duration simply by advancing the nap-ending time since correlation analysis indicates that nap durations might be significantly affected by nap-ending time. In addition, interestingly, both nap durations and nap-ending time do not have significant correlations with total sleep duration, which is the summation of nap and nighttime sleep durations. The data suggest that nap duration and nap-ending time simply controls the distribution ratio between nap and nighttime sleep durations in total sleep duration but does not affect the amount of total sleep duration. There is still an ongoing debate whether either nap or nighttime sleep is more valuable to achieve proper child health and development or if only total sleep duration is an important factor for healthy child development. However, a recent study at least reported that daytime naps improve word learning in toddlers of 16 months of age13,14. A further study using additional physiological parameters will be required to obtain appropriate answers regarding sleep issues in child development.
There are a number of limitations that should be considered in the interpretation of the results. First, because of the relatively small sample size (n = 50), this study did not fully perform analysis on sex difference in actigraph variables. Since the study population is also not well-balanced between boys (n = 32) and girls (n = 18), a study population with a larger sample size will be required to make a satisfactory statistical analysis on the effect of sex difference on toddlers’ sleep variables in any future study. In accordance with Acebo’s study, however, the present study confirms that effect of sex difference was not significant for any actigraph variable among the toddlers at approximately 1.5 years of age (Table 3). Second, because a detailed parent questionnaire was not included in the study, we were not able to precisely examine the similarities and dissimilarities between actigraph data and parent questionnaires. In a previous study, Acebo et al.1 found well-matched data between actigraph data and parent-reported observations. Finally, the present study did not fully investigate the effect of nap duration or timing on night time sleep because we did not perform an RCT study, which would expose children to two different nap durations. Such an RCT study would further strengthen the findings of the present study that daily naps with short periods and starting early in the afternoon can induce a longer nighttime sleep for toddlers at approximately 1.5 years of age.
Methods
Participants
Young toddlers of approximately 1.5 years of age were recruited at the Children’s Clinic of St. Luke’s International Hospital (Tokyo, Japan). Inclusion criteria were as follows: (1) full-term pregnancy (defined as ≥37 weeks’ gestational age) and (2) the absence of known physical or mental disability or of severe developmental delay in the infant. Exclusion criteria was parental language difficulties. Of 72 eligible toddlers, 22 were excluded because sleep data were invalid due to technical problems with the activity recording devices or incomplete description of sleep diary. The final sample thus consisted of 50 young toddlers (32 boys, 18 girls). The ethics committees of the St. Luke’s International Hospital and the National Center of Neurology and Psychiatry approved the study protocol (UMIN000019696) and all procedures were carried out in accordance with the approved guidelines. Written informed consent was obtained from the parents.
Activity and sleep assessment
Actigraphy
For activity and sleep measurement we used actigraphy. Actigraphy is based on a miniature wristwatch-like accelerometer which is attached to the wrist, ankle or waist and continuously records movement for an extended period. The actigraphy device used in the present study was the Actigraph (Micro-mini RC, Ambulatory Monitoring Inc., NY, USA). The parents were asked to attach the Actigraphs to their child’s waist with an adjustable elastic belt for 7 consecutive days. Waist attachment was chosen as we found it less disturbing than wrist or ankle attachment and actigraphic data has been reported to be reliable at various attachment locations, including the wrist, ankles and waist. Previous studies have also demonstrated that a minimum of 7 nights was necessary to obtain reliable data15.
Motility levels were sampled in the zero-crossing mode in 1-min epochs. The resolution of the Actigraph was set at 0.01 G/s. The activity data recorded by the Actigraph was later downloaded using ActMe software (ver. 3.10.0.3,Ambulatory Monitoring Inc.) and then sleep measurements were analyzed using Action-W software (ver. 2.4.20, Ambulatory Monitoring Inc.). During the study, time intervals when the device was removed, for example, during bathing, were recorded in a sleep diary by parents.
Sleep diary
Parents were instructed to complete a sleep diary for the 7-day period while their child was wearing the Actigraph. The diary consisted of seven 24-hr single-sheet schedules, in which parents were asked to write information such as time of nap, going in/out of bed, bathing and night awakenings of which they were aware.
Statistical analysis
Statistical analyses were performed with SPSS Statistics 21.0 (IBM Corp. Armonk, NY, USA). Summary measurements are presented as means ± s.d.s. Pearson correlation was used to assess associations between variables, respectively. The gender difference in sleep environment and bedtime routine was analyzed using a χ2 test for categorical data and a t-test for continuous data.
Additional Information
How to cite this article: Nakagawa, M. et al. Daytime nap controls toddlers’ nighttime sleep. Sci. Rep. 6, 27246; doi: 10.1038/srep27246 (2016).
References
Acebo, C. et al. Sleep/wake patterns derived from activity monitoring and maternal report for healthy 1- to 5-year-old children. Sleep 28, 1568–1577 (2005).
Harada, T., Hirotani, M., Maeda, M., Nomura, H. & Takeuchi, H. Correlation between breakfast tryptophan content and morning-evening in Japanese infants and students aged 0–15 yrs. J Physiol Anthropol 26, 201–207 (2007).
Asaka, Y. & Takada, S. Activity-based assessment of the sleep behaviors of VLBW preterm infants and full-term infants at around 12 months of age. Brain Dev 32, 150–155, doi: 10.1016/j.braindev.2008.12.006 (2010).
Nakade, M., Takeuchi, H., Taniwaki, N., Noji, T. & Harada, T. An integrated effect of protein intake at breakfast and morning exposure to sunlight on the circadian typology in Japanese infants aged 2–6 years. J Physiol Anthropol 28, 239–245 (2009).
Akacem, L. D. et al. The Timing of the Circadian Clock and Sleep Differ between Napping and Non-Napping Toddlers. PLoS One 10, e0125181, doi: 10.1371/journal.pone.0125181 (2015).
Thorpe, K. et al. Napping, development and health from 0 to 5 years: a systematic review. Arch Dis Child 100, 615–622, doi: 10.1136/archdischild-2014-307241 (2015).
Fukuda, K. & Sakashita, Y. Sleeping pattern of kindergartners and nursery school children: function of daytime nap. Percept Mot Skills 94, 219–228, doi: 10.2466/pms.2002.94.1.219 (2002).
Yokomaku, A. et al. A study of the association between sleep habits and problematic behaviors in preschool children. Chronobiol Int 25, 549–564, doi: 10.1080/07420520802261705 (2008).
Jones, C. H. & Ball, H. L. Napping in English preschool children and the association with parents’ attitudes. Sleep Med 14, 352–358, doi: 10.1016/j.sleep.2012.12.010 (2013).
Komada, Y. et al. Relationship between napping pattern and nocturnal sleep among Japanese nursery school children. Sleep Med 13, 107–110, doi: 10.1016/j.sleep.2011.10.017 (2012).
Staton, S. L., Smith, S. S., Pattinson, C. L. & Thorpe, K. J. Mandatory Naptimes in Child Care and Children’s Nighttime Sleep. J Dev Behav Pediatr 36, 235–242, doi: 10.1097/DBP.0000000000000157 (2015).
Staton, S. L., Smith, S. S., Hurst, C., Pattinson, C. L. & Thorpe, K. J. Mandatory Nap Times and Group Napping Patterns in Child Care: An Observational Study. Behav Sleep Med 11, 1–15 (2016)
Horváth K., Myers K., Foster R. & Plunkett K. Napping facilitates word learning in early lexical development. J Sleep Res 5, 503–509, doi: 10.1111/jsr.12306. (2015).
Horváth K., Liu S. & Plunkett K. A daytime nap facilitates generalization of word meanings in young toddlers. Sleep 39, 203–207, doi: org/10.5665/sleep.5348. (2016)
Souders, M. C. et al. Sleep behaviors and sleep quality in children with autism spectrum disorders. Sleep 32, 1566–1578 (2009).
Acknowledgements
We thank all the participants and their parents for their generous contributions. This work was supported by Grants-in-Aid for Scientific Research (to H.O. # 26650176) from the Ministry of Education, Culture, Sports, Science and Technology of Japan and grants (to M.N.) from St. Luke’s Life Science Institute, Public Health Research Foundation and Japan Foundation for Neuroscience and Mental Health.
Author information
Authors and Affiliations
Contributions
H.O., I.K. and H.Y. conceived of the study. M.N., H.O., I.K. and H.Y. designed the experiments. Y.N., R.S., Y.A., N.T., T.N., Y.K., K.M., Y.O., Y.A., M.I., M.T., M.H., M.O. and K.C. performed and analyzed the experiments. M.N., H.O., I.K. and H.Y. wrote the paper.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Nakagawa, M., Ohta, H., Nagaoki, Y. et al. Daytime nap controls toddlers’ nighttime sleep. Sci Rep 6, 27246 (2016). https://doi.org/10.1038/srep27246
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep27246
This article is cited by
-
The Architecture of Early Childhood Sleep Over the First Two Years
Maternal and Child Health Journal (2023)
-
LifeSnaps, a 4-month multi-modal dataset capturing unobtrusive snapshots of our lives in the wild
Scientific Data (2022)
-
Daytime nap and nighttime breastfeeding are associated with toddlers’ nighttime sleep
Scientific Reports (2021)
-
Sleep maturation influences cognitive development of preterm toddlers
Scientific Reports (2021)
-
Postural change for supine position does not disturb toddlers’ nap
Scientific Reports (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.