Abstract
Over past several years, the cold plasma-stimulated medium (PSM) has shown its remarkable anti-cancer capacity in par with the direct cold plasma irradiation on cancer cells or tumor tissues. Independent of the cold plasma device, PSM has noticeable advantage of being a flexible platform in cancer treatment. Currently, the largest disadvantage of PSM is its degradation during the storage over a wide temperature range. So far, to stabilize PSM, it must be remained frozen at −80 °C. In this study, we first reveal that the degradation of PSM is mainly due to the reaction between the reactive species and specific amino acids; mainly cysteine and methionine in medium. Based on this finding, both H2O2 in PSM and the anti-cancer capacity of PSM can be significantly stabilized during the storage at 8 °C and −25 °C for at least 3 days by using phosphate-buffered saline (PBS) and cysteine/methionine-free Dulbecco’s Modified Eagle Medium (DMEM). In addition, we demonstrate that adding a tyrosine derivative, 3-Nitro-L-tyrosine, into DMEM can mitigate the degradation of PSM at 8 °C during 3 days of storage. This study provides a solid foundation for the future anti-cancer application of PSM.
Similar content being viewed by others
Introduction
Over the past decade, cold atmospheric plasma has shown a selective anti-cancer capacity both in vitro1,2,3,4,5,6,7,8 and in vivo9,10,11,12,13. Various type of cold plasma devices were used to directly irradiate cancer cells cultured in the multi-well plates4,14, petri-dishes1,15, or tumor tissues9,12. Recently, plasma-stimulated medium (PSM) proved to exhibit a significant anti-cancer capacity as strong as the direct cold plasma treatment on glioblastoma cells16,17,18, lung carcinoma cells19, and bladder cancer cells20. Very recently, it is reported that microsecond-pulsed plasma-activated media is able to selectively inhibit the growth of lung cancer (H460) cells rather than normal lung cancer (L132) cells21. Another very recent study about the selective apoptosis in the PSM treated glioblastoma cells22, further confirming that PSM is a selective anti-cancer tool. The injection of PSM into mice also significantly inhibits the growth of tumor23. Thus, PSM may have wide application in cancer treatment including specific situations where cold atmospheric plasma cannot reach deep seated tumors or when the cold plasma device is not portable.
The cold plasma-originated reactive species are thought to be the main factor in cancer cell death and growth inhibition24. In fact, the feasibility of using PSM to kill cancer cells is a direct evidence to support this conclusion. When cold plasma interacts with the medium both reactive oxygen species (ROS) such as hydroxyl free radicals (OH)25 and hydrogen peroxide (H2O2)19,26 and reactive nitrogen species (RNS) such as nitric oxide (NO)27 and nitrite (NO2−)17,28 are dissolved in the aqueous solution. Among them, H2O2 has been found to mainly contribute to the death of cancer cells after the direct cold plasma irradiation on cancer cells29,30,31 or the indirect cold plasma irradiation on the culture medium18,19.
To date, the degradation of PSM during the storage is its largest disadvantage for future clinical application. For pharmaceutical reasons, PSM should be stably stored for relative long time. However, as it is known PSM gradually loses its anti-cancer capacity during the storage at the room temperature17,19 or down to the temperature a few degrees above the freezing point of water19. Accordingly, the H2O2 concentration in PSM also gradually decreases during the storage under these conditions19. Because the degradation of the anti-cancer capacity of PSM has been reported by different groups using different plasma devices and treatment doses17,19, the instability of PSM during the storage can be regarded as a basic feature of PSM.
So far, the sole strategy to inhibit the degradation of PSM during the storage is freeze at an adequately low temperature. Tetsuo Adachi et al. reported that a freeze at −80 °C was able to stabilize the anti-cancer capacity of cold plasma-stimulated Dulbecco’s Modified Eagle Medium (DMEM) for a week19. However, we found that freezing PSM at around −20 °C would significantly accelerate the degradation of PSM17. In fact, Tetsuo Adachi et al. also reported that the noticeable degradation of PSM still existed during the storage at −30 °C19. These observations indicate that the degradation of PSM during the storage may be due to a slow temperature-dependent reaction which can be inhibited in an adequately cold atmosphere. Nonetheless, according to the description of most manufacturers of cell culture media, the ideal storage temperature range for medium is over 2 °C to 8 °C, rather than the freezing condition. Thus, considering the clinical application prospective, PSM at least should be stable at such a temperature range. So far, no method has been reported about improving the stability of PSM over 2 °C to 8 °C.
In this study, by comparing the H2O2 concentration in the cold plasma-stimulated phosphate-buffered saline (PBS) and the cold plasma-stimulated DMEM during the storage at 8 °C, 22 °C and −25 °C, we found that the degradation of PSM was mainly due to the reaction between the plasma-originated reactive species and components in DMEM. A further detailed investigation showed that cysteine and methioine were the main components in DMEM contributing to this process. Based on these principles, we further proved that the plasma-stimulated cysteine/methionine-free DMEM was much more stable than the plasma-stimulated standard DMEM during the storage at 8 °C, 22 °C and −25 °C. In addition, adding a tyrosine derivative, 3-Nitro-L-tyrosine, could also improve the stability of cold plasma-stimulated DMEM at 8 °C but not at −25 °C.
Results
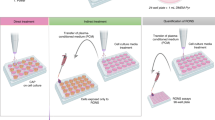
The cold plasma device (Fig. 1a) was a typical helium cold atmospheric plasma jet generator which has been used in a series of studies17,18,32,33,34. Cold plasma jet was generated between the central electrode and the grounded ring electrode. The carrying gas was helium with a flow of 4.7 L/min and was controlled by a flow meter. The output voltage was 3.16 kV. The general research strategy is illustrated in Fig. 1b. 1 mL of PSM was made by the vertical irradiation on the medium in a well on a 12-well plate. Then, PSM was transferred into a 1.5 mL of centrifuge tube by pipette. The centrifuge tubes were stored in refrigerators with different internal temperatures (8 °C and −25 °C) for 3 days. Similarly, the centrifuge tubes were stored at 22 °C when we investigated the degradation of PSM at the room temperature (not shown in Fig. 1b). Ultimately, PSM was either transferred to culture the seeded cancer cells in a 96-well plate or transferred into a black-wall 96-well plate to perform the measurement for H2O2. The detailed protocols for the transfer are illustrated in Methods and Fig. S1a,b. Because PBS is not suitable for cell culture, the protocols used to transfer the plasma-stimulated PBS is slightly different from the protocols used to transfer the plasma-stimulated DMEM (Fig. S1).
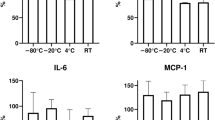
To understand the mechanism of PSM degradation, we first compared the H2O2 generation in the cold plasma-stimulated DMEM and PBS after 26 hours of storage and found that the H2O2 in plasma-stimulated PBS was quite stable during the storage while most H2O2 in the plasma-stimulated DMEM had been lost after 26 hours at 8 °C and 22 °C (Fig. 2a). The higher storage temperature for PSM, the stronger degradation occurs in PSM (Fig. 2a). Obviously, the instability of PSM is mainly due to the reaction between component of DMEM and reactive species generated by the cold plasma. Recently, we have demonstrated that the H2O2 in PSM tended to react with cysteine among all 20 amino acids after the plasma irradiation18. Thus, the plasma-stimulated PBS has higher H2O2 concentration than the plasma-stimulated DMEM (Fig. 2a). We further found that the H2O2 concentration in the plasma-stimulated PBS was not only stable over 7 days of storage at 8 °C (Fig. 2b) but also stable over 3 days at −25 °C (Fig. 2c). The stable anti-cancer capacity of the plasma-stimulated PBS over 3 days at 8 °C and −25 °C was further confirmed by using the corresponding treated PBS to affect the growth of breast cancer (MDA-MB-231) cells (Fig. 2d). In addition, we demonstrated that the plasma-stimulated PBS could also effectively inhibit the growth of glioblastoma (U87MG) cells and pancreatic cancer (PA-TU-8988T) cells with a dose-dependent manner (Fig. 2e), making it a stable anti-cancer PSM over a wide temperature range. Ultimately, we tested whether the H2O2-containing PBS would be as stable as the cold plasma-stimulated PBS, and found that the H2O2-containing PBS just experienced a slight degradation over the storage at 8 °C for 3 days (Fig. 2f), which is similar to the slight degradation observed in the plasma-stimulated PBS (Fig. 2c). The H2O2 in PBS will experience a natural degradation during the storage at 8 °C. Thus, the gradual H2O2 consumption in the cold plasma-stimulated DMEM is due to the combined effect of the natural degradation of H2O2 in aqueous solution and the reaction between H2O2 and the component in DMEM. The latter mainly controls the degradation at 8 °C.
(a) The change of H2O2 concentration in the cold plasma-stimulated DMEM and PBS during the storage at 8 °C and 22 °C for 26 hours. (b) The change of H2O2 concentration in the cold plasma-stimulated PBS during the storage at 8 °C for 7 days. (c) The change of H2O2 concentration in the cold plasma-stimulated PBS during the storage at 8 °C and −25 °C for 3 days. (d) The change of anti-cancer capacity of the cold plasma-stimulated PBS during the storage at 8 °C and −25 °C for 3 days. (e) The effect of the cold plasma-stimulated PBS on the cell viability of U87MG, PA-TU-8988T, and MDA-MB-231 cells cultured in the cold plasma-stimulated PBS. (f) The change of H2O2 concentration in 37.3 μM H2O2-containing PBS during the storage at 8 °C for 3 days. The volume of solution for each well was 1 mL for all experiments. The treatment time for (a–d) was 1min and 2 min, respectively. Results are presented as the mean ± s.d. of three independently repeated experiments performed in triplicate (a–c,f) or in sextuplicate (d,e). For the cell viability, the data have been normalized to corresponding control group.Student’s t-test was performed and the significance is indicated as ***p < 0.005.
Furthermore, the effect of specific components in DMEM on the PSM degradation was comprehensively investigated. A comparison between DMEM and PBS reveals that 15 amino acids, glucose, calcium ion, magnesium ion, and phenol red are the main composition difference between DMEM and PBS (Fig. S2). Thus, 15 specific amino acids solutions, 1 glucose solution, 2 saline solutions (CaCl2, MgCl2), and 1 phenol red solution were respectively made by adding or dissolving specific component in PBS according to their concentrations in the standard DMEM (Fig. S3). After the plasma treatment and subsequent 26 hours of storage at 22 °C, the H2O2 concentrations in these solutions were measured and compared with corresponding H2O2 concentration in the solution just after the cold plasma treatment (Fig. 3a). The H2O2 in the plasma-stimulated PBS is quite stable over the storage. In contrast, most of the studied components cause different levels of H2O2 degradation in the plasma-stimulated PBS-based solution, except tryptophan, tyrosine, and lysine. Cysteine and methionine cause the most significant degradation of H2O2 during the storage at room temperature. Phenylalanine also cause the noticeably degradation of H2O2. Based on these data, it is reasonable to predict that a modified DMEM without cysteine, methionine, phenylalanine or other components will be a stable PSM. So far, however, the modified DMEM without phenylalanine is not available on the market. Thus, we just focused on studying the role of cysteine and methionine on the PSM degradation. We first compared the plasma-stimulated cysteine/methionine/glutamine-free DMEM with the plasma-stimulated arginine/lysine/glutamine-free DMEM and the plasma-stimulated standard DMEM and found that only the former was stable during the storage at 22 °C for 26 hours (Fig. S4). The absence of arginine and lysine did not inhibit the H2O2 degradation in PSM (Fig. S4). These results are consistent with the trends revealed in Fig. 3a.
(a) The change of H2O2 concentration in the cold plasma-stimulated PBS containing specific component in DMEM during the storage at 22°C for 26 hours. (b) The change of H2O2 concentration in the cold plasma-stimulated cysteine/methionine-free DMEM, cysteine-free DMEM, methionine-free DMEM, and standard DMEM during the storage at 8 °C for 3 days. (c) The change of anti-cancer capacity of the cold plasma-stimulated cysteine/methionine-free DMEM, cysteine-free DMEM, methionine-free DMEM, and standard DMEM during the storage at 8°C for 3 days. For all experiments, the volume of solution and the treatment time in each well was 1 mL and 1 min, respectively. Results are presented as the mean ± s.d. of three independently repeated experiments performed in triplicate (a,b) or in sextuplicate (c). For the cell viability, the data have been normalized to corresponding control group. Student’s t-test was performed and the significance is indicated as *p < 0.05, **p < 0.01, ***p < 0.005.
To make cysteine/methionine-free DMEM, 4 mM glutamine was added in the purchased cysteine/methionine/glutamine-free DMEM. Based on these cysteine/methionine-free DMEM, we further prepared the modified DMEM just without cysteine and the modified DMEM just without methionine according to the description in Methods. Then, the specific effect of cysteine and methionine on the instability of PSM was investigated. After three days of storage at 8 °C, only the cold plasma-stimulated cysteine/methionine-free DMEM shows strong capacity inhibiting the H2O2 degradation (Fig. 3b). For cysteine and methionine, either of them will result in noticeable H2O2 degradation in PSM during the storage (Fig. 3b). Furthermore, the anti-cancer capacity of these PSM on breast cancer (MDA-MB-231) cells was investigated. In contrast to the experiments performed in the immediately treated medium, 3 days of storage at 8 °C causes noticeable degradation of the anti-cancer capacity of PSM even the modified DMEM does not contain cysteine and methionine (Fig. 3c). However, compared with other three cases, the cysteine/methionine-free DMEM still shows the strongest capacity to retain the effective species in PSM. The cysteine/methionine-free DMEM does not completely inhibit the H2O2 degradation, which may be due to two reasons. One is that many components other than cysteine and methionine in DMEM also contribute to the instability of PSM during the storage (Fig. 3a). The modified DMEM without all these reactive components may be as stable as PBS after the plasma irradiation. Another possibility is that some reactive species other than H2O2 may also contribute to the anti-cancer capacity of PSM.
Despite the optimized storage temperature for the culture medium should be between 2 °C to 8 °C, the cryopreservation of PSM may still be necessary at some special circumstances. For most of refrigerators served in pharmacies, the temperature in the freezing chamber is around −20 °C. To date, however, PSM has been found even more degradable when stored at temperature around −20 °C than that at 22 °C17 or at 4 °C19. General observation is that freezing aggravates the degradation of PSM. As we demonstrated above, both the H2O2 concentration (Fig. 2c) and the anti-cancer capacity (Fig. 2d) of the cold plasma-stimulated PBS are stably retained during the storage at −25 °C. Thus, the degradation of the plasma-stimulated DMEM should also be due to the reaction between component in DMEM and the plasma-originated reactive species such as H2O2. To verify this proposition, we first investigated the stability of H2O2-containing DMEM and H2O2-containing PBS under the freezing conditions for 3 days. It is found that, in contrast to the immediately prepared H2O2-containing DMEM and H2O2-containing PBS, H2O2 has been completely consumed (Fig. 4a) and has been well retained (Fig. 4b) in the frozen DMEM and the frozen PBS at −25 °C, respectively. Thus, the plasma-originated or other sources-originated H2O2 naturally tend to strongly react with specific component in DMEM under the freezing conditions. In addition, similar to the trend shown in Fig. 2f, H2O2 also shows a natural tend to be slightly consumed in PBS during the freezing storage. Thus, the degradation of H2O2 in PSM under the freezing condition is also due to the reaction between H2O2 and the components in media and a natural degradation in aqueous solution. The former is the main factor.
(a) The change of H2O2 concentration in 34.5 μM H2O2-containing DMEM during the storage at −25 °C for 3 days. (b) The change of H2O2 concentration in 37.3 μM H2O2-containing PBS during the storage at −25 °C for 3 days. (c) The change of H2O2 concentration in the cold plasma-stimulated PBS containing specific component in DMEM during the storage at −25 °C for 26 hours. (d) The change of H2O2 concentration in the cold plasma-stimulated cysteine/methionine-free DMEM, cysteine-free DMEM, methionine-free DMEM, and standard DMEM during the storage at −25 °C for 3 days. (e) The anti-cancer capacity of the cold plasma-stimulated cysteine/methionine-free DMEM, cysteine-free DMEM, methionine-free DMEM, and standard DMEM during the storage at −25 °C for 3 days. For all experiments, the volume of solution in each well was 1 mL. The treatment time was 1 min for (c,d). Results are presented as the mean ± s.d. of three independently repeated experiments performed in triplicate (a–d) or in sextuplicate (e). For the cell viability, the data have been normalized to corresponding control group. Student’s t-test was performed and the significance is indicated as ***p < 0.005.
Similar to the research strategy described above, we further investigated which component in DMEM contribute to the degradation of PSM during the freezing storage. This was done by comparing the degradation of H2O2 in 15 amino acids solutions, 1 glucose solution, 2 saline solutions (CaCl2, MgCl2), 1 phenol red solution, and PBS. These solutions were made by previously mentioned methods according to the concentration shown in Fig. S3. As presented in Fig. 4c, cysteine and methionine are still the two most reactive components in DMEM consuming the plasma-originated H2O2 during the freezing storage. Different from the trend shown in Fig. 3a, all studied components tend to aggravate the degradation of H2O2 in the cold plasma-stimulated PBS at −25 °C, including tyrosine, tryptophan, and lysine, which in fact inhibit the degradation of H2O2 in the cold plasma-stimulated PBS at 8 °C (Fig. 3a). Under the freezing conditions, the H2O2 degradation in the methionine solution is stronger than that in the cysteine solution. Furthermore, we investigated the anti-degradation effect of the cysteine/methionine-free DMEM under the freezing conditions using the above mentioned methods. The appearance of either of cysteine and methionine in DMEM will result in the complete consumption of H2O2 after 3 days of storage at −25 °C (Fig. 4d). The cysteine-free DMEM is slightly more resistant to the H2O2 degradation than the methionine-free DMEM, which is consistent with the trend revealed in Fig. 4c that methionine is more reactive with H2O2 than cysteine during the freezing storage. For the cysteine/methionine-free DMEM, more than half of H2O2 has been consumed during the 3 days of storage at −25 °C, which is also consisted with trend shown in Fig. 4c that many other components in DMEM also contribute to the instability of PSM. Ultimately, we compared the anti-cancer capacity of these modified DMEM on MDA-MB-231 cells. When the plasma treatment time is just 1 min (Fig. 4e), the difference between four experimental groups is not obvious. Such phenomenon may be due to the low concentration of residual H2O2 or reactive species in frozen plasma-stimulated cysteine/methionine-free DMEM, which are too weak to cause noticeable anti-cancer effect (Fig. 4d). When the plasma treatment time extends to 2 min (Fig. 4e), the appearance of cysteine or methionine will significantly aggravate the degradation of the anti-cancer capacity of PSM. In contrast, the plasma-stimulated cysteine/methionine-free DMEM still causes a 60% of anti-cancer growth effect.
In addition to above mentioned methods, we presented a third anti-degradation method based on the results shown in Fig. 3a. It is clear that tyrosine is able to slightly increase the H2O2 concentration in the plasma-stimulated PBS during the storage at 8 °C. Among 15 amino acids in DMEM, only tyrosine and phenylalanine have aromatic ring structures (Fig. 5a). However, phenylalanine causes noticeable H2O2 degradation in the cold plasma-stimulated PBS during the storage at 8 °C (Fig. 3a). The only difference between tyrosine and phenylalanine is a hydroxyl on the aromatic ring (Fig. 5a), indicating that the modification on the aromatic ring of amino acids may endow the amino acids with a capacity inhibiting the degradation of H2O2 during the storage at 8 °C. We utilized a tyrosine derivative, 3-Nitro-L-tyrosine, which had a nitro group on the aromatic ring of tyrosine (Fig. 5a). 2 mM 3-Nitro-L-tyrosine-containing DMEM, 2 mM phenylalanine-containing DMEM, and 2 mM tyrosine-containing DMEM were prepared by dissolving purchased 3-Nitro-L-tyrosine, phenylalanine, and tyrosine powders in the standard DMEM, respectively. Subsequently, the stability of H2O2 in the plasma-stimulated DMEM, tyrosine-containing DMEM, phenylalanine-containing DMEM, and 3-Nitro-L-tyrosine-containing DMEM stored at 8 °C were compared. 3-Nitro-L-tyrosine significantly inhibits the degradation of H2O2 in PSM (Fig. 5b). On the contrary, tyrosine and phenylalanine do not improve the stability of PSM (Fig. 5b). Furthermore, it is found that noticeable H2O2 degradation still occur in the cold plasma-stimulated 3-Nitro-L-tyrosine-containing DMEM and the cold plasma-stimulated standard DMEM after the storage at 8 °C for 3 days (Fig. 5c). Despite 60% of plasma-originated H2O2 has been lost during the storage, it is more effective than the plasma-stimulated standard DMEM, in which 74% of plasma-originated H2O2 has been lost during the 3 days of storage. Nonetheless, after the storage, the cold plasma-stimulated 3-Nitro-L-tyrosine-containing DMEM still shows a noticeable anti-breast cancer cells capacity as strong as the immediately treated 3-Nitro-L-tyrosine-containing DMEM (Fig. 5d). In contrast, the anti-cancer capacity of the plasma-stimulated standard DMEM significantly decays during the storage (Fig. 5d).
(a) Chemical formulas of phenylalanine, tyrosine, and 3-Nitro-L-tyrosine. (b) The change of H2O2 concentration in the cold plasma-stimulated standard DMEM, phenylalanine-containing DMEM, tyrosine-containing DMEM, and 3-Nitro-L-tyrosine-containing DMEM during the storage at 8 °C for 26 hours. (c) The change of H2O2 concentration in the cold plasma-stimulated standard DMEM and 3-Nitro-L-tyrosine-containing DMEM during the storage at 8 °C for 3 days. (d) The change of anti-cancer capacity of the cold plasma-stimulated standard DMEM and 3-Nitro-L-tyrosine-containing DMEM during the storage at 8 °C for 3 days. (e) The change of H2O2 concentration in the cold plasma-stimulated single amino acids-containing PBS and double amino acids-containing PBS during the storage at 22 °C for 26 hours. Corresponding concentration of cysteine, methionine, phenylalanine, and 3-Nitro-L-tyrosine in PBS were 0.2 mM, 0.2 mM, 0.4 mM and 2 mM, respectively. (f) The change of H2O2 concentration in the cold plasma-stimulated 3-Nitro-L-tyrosine-containing DMEM with different concentrations during the storage at 8 °C for 3 days. (g) The change of H2O2 concentration in the cold plasma-stimulated standard DMEM and 3-Nitro-L-tyrosine-containing DMEM during the storage at −25 °C for 3 days. For all experiments, the volume of solution in each well was 1 mL. The treatment time was 1 min for (b,e,f) and was 2 min for (c,d,g), respectively. Results are presented as the mean ± s.d. of three independently repeated experiments performed in triplicate (b,c,e–g) or in sextuplicate (d). For the cell viability, the data have been normalized to corresponding control group. Student’s t-test was performed and the significance is indicated as *p < 0.05, **p < 0.01, ***p < 0.005.
To reveal the anti-degradation mechanism of 3-Nitro-L-tyrosine in the plasma-stimulated DMEM, we first investigated whether 3-Nitro-L-tyrosine was able to inhibit the H2O2 degradation in 0.2 mM cysteine-containing PBS, 0.2 mM methionine-containing PBS, and 0.4 mM phenylalanine-containing PBS. As shown in Fig. 5e, 2 mM 3-Nitro-L-tyrosine is able to completely inhibit the H2O2 degradation in all three cold plasma-stimulated amino acids-containing PBS solutions at 22 °C. Thus, the cold plasma-stimulated DMEM may be stabilized by 3-Nitro-L-tyrosine through inhibiting the reaction between some components in DMEM such as cysteine, methionine, or phenylalanine with the cold plasma-originated H2O2. Furthermore, we studied the concentration-effect of 3-Nitro-L-tyrosine on its anti-degradation effect in the plasma-stimulated DMEM. For the plasma-stimulated 3-Nitro-L-tyrosine-containing DMEM, the residual H2O2 after 3 days of storage increases as the concentration of 3-Nitro-L-tyrosine increases from 1 mM to 4 mM (Fig. 5f). After 3 days of storage at 8 °C, 4 mM 3-Nitro-L-tyrosine-containing DMEM loses 30% of the H2O2 originated from the plasma treatment. In contrast, the standard DMEM loses 81% of the plasma-originated H2O2 (Fig. 5f). Finally, we identified that the degradation of H2O2 in the 3-Nitro-L-tyrosine-containing DMEM during the freezing storage is as extensive as that occurs in the standard DMEM after the plasma treatment (Fig. 5g). In short, adding 3-Nitro-L-tyrosine in DMEM weakens the degradation of PSM stored at 8 °C, though it cannot weaken the degradation of PSM stored at −25 °C.
Discussion
Understanding the interaction between the cold atmospheric plasma and molecules in an aqueous solution builds the foundation of the plasma medicine. Current experimentation is mainly limited to studying chemical reactions between the cold plasma-originated reactive species and components in an aqueous solutions such as cell culture medium35. Among diverse chemicals, amino acids are not only the building blocks of all proteins involving in nearly all biological processes but also the main component in most cell culture media utilized in the studies in vitro4,6,16. The interaction between the cold plasma and the amino acids in culture media has been extensively investigated in past two years. A general investigation regarding the chemical modification and change of 20 amino acids after the cold plasma treatment has been performed via high-resolution mass spectrometry35. It was found that hydroxylation, nitration, sulfonation, disulfide formation and sulfoxidation were the main chemical modification of 14 amino acids upon the cold plasma irradiation35. In addition, sulfur-containing amino acids such as cysteine and methionine and aromatic amino acids such as tryptophan, phenylalanine, and tyrosine were preferentially consumed during the plasma treatment35. It was also demonstrated that proteins in FBS consume the reactive species generated by cold plasma treatment significantly17. Recently, we further demonstrated that among 20 amino acids, cysteine was most reactive to plasma produced species including H2O218. These results clearly revealed that the plasma-originated reactive species will be partially consumed immediately after their formation in PSM. Furthermore, in this study, we proved that many components of medium particularly cysteine and methionine will slowly consume the plasma-originated reactive species such as H2O2 during storage. Thus, in designing the ideal PSM, cysteine and methionine should be avoided. Such slow reaction between reactive species and components in medium should be temperature-dependent, because it can be completely inhibited through an adequately low temperature freeze at −80 °C19.
The discovery of the anti-degradation property of 3-Nitro-L-tyrosine provides a promising strategy to improve the stability of PSM because the original component of DMEM does not need to be removed. Despite the fact that the chemical mechanism of such anti-degradation capacity is unknown yet, adding modifications to the aromatic ring of tyrosine or phenylalanine may be the general strategy to obtain new derivatives capable to preserve H2O2 and perhaps other plasma produced reactive species. In addition, the anti-degradation effect of 3-Nitro-L-tyrosine first reveals that the interaction between the cold plasma and media cannot be simply described as the consumption of plasma-originated reactive species such as H2O2 or the modification of component such as cysteine and methionine in the medium. Indeed, most of components in the medium tend to consume the plasma-originated reactive species; however, specific amino acid derivatives are able to inhibit the reaction between plasma-originated reactive species and specific components in the medium such as cysteine and methionine. These results demonstrate that the chemical essence of interaction between cold plasma and aqueous solution is far from clear. We not only need to measure the immediate reaction in media due to the plasma irradiation but we also have to monitor the long term dynamic reactions in PSM after the plasma irradiation.
The essence of the anti-cancer reactive species in cold plasma or PSM is still disputable. A simple comparison between the concentration of H2O2 (Fig. 3b) and the anti-cancer effect (Fig. 3c) in the plasma-stimulated cysteine/methionine-free DMEM stored at 8 °C for 3 days reveals that though H2O2 just loses about 23% during the storage, corresponding anti-cancer capacity loses about 45% during the same storage. Perhaps other plasma-originated reactive species also contributes to the anti-cancer effect of PSM and decay faster than H2O2. Currently, H2O2 has just been regarded as the main plasma-originated reactive species contributing to the anti-cancer capacity of cold plasma29,30. However, evidence exist that both cellular-level18,26,27 and molecular-level29,36 response of cancer cells to the cold plasma treatment are different from that positive control using H2O2. The cold plasma-originated atomic oxygen has been proven to be a main toxic reactive species to epithelial kidney cells under a specific plasma treatment condition37. So far, based on the accumulated data in the literature, it is premature to reach final conclusion regarding the mechanism of action of cold atmospheric plasma. A further comprehensive investigation on the role of key plasma-originated reactive species on the anti-cancer effect of cold plasma is necessary and urgent.
Conclusions
The degradation of PSM during storage is due to the reaction between the plasma-originated reactive species and components of the cell culture medium. We have found that cysteine and methionine are two most reactive components in DMEM contributing to the consumption of plasma-originated H2O2. The cold plasma-stimulated PBS and the cold plasma-stimulated cysteine/methionine-free DMEM can be stably stored at 8 °C and −25 °C for at least 3 days. In addition, adding 3-Nitro-L-tyrosine into DMEM could weaken the degradation of the cold plasma-stimulated DMEM at 8 °C for 3 days. These stabilizing strategies build a solid foundation for the application of PSM in future cancer treatment.
Methods
Medium and cell cultures
Standard Dulbecco’s modified Eagle’s medium (11965-118), the modified cysteine/methionine/glutamine-free DMEM (21013-024), the modified arginine/lysine/glutamine-free DMEM (A14431-01) and PBS (14040-133) were purchased from Gibco Life Technologies. In addition, all DMEM and PBS were mixed with 1% (v/v) antibiotic (penicillin and streptomycin) (Life Technologies) before any experiments. Human glioblastoma (U87MG) cells and pancreatic cancer (PA-TU-8988T) cells were provided by Dr. Murad’s Lab at the George Washington University. Human breast cancer (MDA-MB-231) cells were provided by Dr. Zhang’s Lab at the George Washington University. All cancer cell lines were seeded with a confluence of 3 × 104 cells/mL and a volume of 100 μL in each well on 96-well plate and were cultured for 6 hours in a complete media composed of Dulbecco’s modified Eagle’s medium (Life Technologies) supplemented with 10% (v/v) fetal bovine serum (ThermoFisher Scientific) and 1% (v/v) antibiotic (penicillin and streptomycin) solution (Life Technologies) under the standard cell culture conditions (a humidified, 37 °C, 5% CO2 environment). In each experiment, 6 wells in a single column on 96-well plate would be seeded with cancer cells.
Making plasma-stimulated PBS and DMEM
In this study, the protocols to make PSM are the same among different experiments. 1 mL of PBS or DMEM or other modified DMEM such as cysteine/methionine-free DMEM in a well on 12-well plate (Falcon) was treated by cold plasma for 1 min or 2 min. The gap between the end of dielectric plasma tube and the bottom of 12-well plate was 3 cm.
Making H2O2-containing PBS and DMEM
The H2O2-containing PBS and H2O2-containing DMEM were prepared by adding purchased 30 wt% H2O2 solution (Sigma-Aldrich) into PBS and DMEM, respectively. The H2O2 concentration in H2O2-containing PBS and H2O2-containing DMEM were close to the H2O2 concentration in the 1 min of cold plasma-treated 1 mL of PBS or DMEM in 12-well plate, respectively.
Making the specific component-containing PBS and DMEM
The amino acids-containing PBS, the calcium-containing PBS, the magnesium-containing PBS, the glucose-containing PBS, the phenol red-containing PBS, and amino acids-containing DMEM were prepared by adding and dissolving purchased specific amino acids, calcium chloride solution, magnesium chloride solution, D-glucose and phenol red solution or amino acids derivative such as 3-Nitro-L-tyrosine into PBS and DMEM, respectively. Except PBS and DMEM, all above chemicals were purchased from Sigma-Aldrich.
Affecting the growth of cancer cells seeded in 96-well plate by the cold plasma-stimulated DMEM or PBS
First, the initial culture medium which has been cultured cells for 6 hours has been removed before this step. Then, for the plasma-stimulated DMEM (Fig. S1a), 100 μL of treated DMEM was transferred from a well on 12-well plate or other tubes stored in refrigerator into a well on 96-well plate, in which 3 × 103 cancer cells were seeded and has been cultured for 6 hours. In each experiment, 6 wells in a single column on 96-well plate have been seeded with cancer cells. In the control group, the DMEM used to culture cancer cells was the untreated DMEM. For the plasma-stimulated PBS (Fig. S1b), considering that cancer cells cannot grow in PBS over a long time range, 100 μL of untreated DMEM was first transferred into the well seeded with 3 × 103 cancer cells on 96-well plate. Then, 100 μL of treated PBS was transferred into the well which contained 100 μL of untreated DMEM and 3 × 103 cancer cells. Thus, after this step, the total volume of the mixed medium in each well seeded with cancer cells were 200 μL. For the control group, the PBS transferred into the well would not be treated. Ultimately, for above two cases, the cancer cells on 96-well plate were cultured under a standard cell culture condition (a humidified, 37 °C, 5% CO2 environment) for 3 days.
Measuring and processing the cell viability
After the experiments, the cancer cells in 96-well plates were cultured in 96-well plate under the standard cell culture conditions (a humidified, 37 °C, 5% CO2 environment) for 3 days. Then, according to the standard two-steps MTT measurement protocols, the viability of cancer cells was qualified by MTT test and was read by an H1 microplate reader (Hybrid Technology) at the absorbance of 570 nm. In each independent experiment, 6 wells in a single column on 96-well plate would be seeded with cancer cells and would be taken cell viability test. The average value of measured cell viability from 6 wells was regarded as the cell viability measured from one independent experiment. To facilitate the understanding on data, all data about cell viability shown in figures has been normalized to the control group by dividing the measured cell viability of experimental group by the measured cell viability of control group. The final data shown in all figures are the mean ± s.d. of the normalized cell viability from three independently repeated experiments.
Measuring H2O2 concentration
50 μL of medium or PBS which needs to be measured was transferred to a well on a black-wall 96-well clear bottom plate (Falcon) in triplicate. Next, according to the standard protocols provided by Sigma-Aldrich, the H2O2 concentration in the cold plasma-stimulated medium was measured. The fluorescence at 540/590 nm was read using an H1 microplate reader (Hybrid Technology).
Additional Information
How to cite this article: Yan, D. et al. Stabilizing the cold plasma-stimulated medium by regulating medium's composition. Sci. Rep. 6, 26016; doi: 10.1038/srep26016 (2016).
References
Fridman, G. et al. Floating Electrode Dielectric Barrier Discharge Plasma in Air Promoting Apoptotic Behavior in Melanoma Skin Cancer Cell Lines. Plasma Chem Plasma P. 27, 163–176, doi: 10.1007/s11090-007-9048-4 (2007).
Keidar, M. Plasma for cancer treatment. Plasma Sources Sci T. 24, 033001–033020, doi: 10.1088/0963-0252/24/3/033001 (2015).
Ratovitski, E. A. et al. Anti-Cancer Therapies of 21st Century: Novel Approach to Treat Human Cancers Using Cold Atmospheric Plasma. Plasma Process Polym. 11, 1128–1137, doi: 10.1002/ppap.201400071 (2014).
Zhang, X., Li, M., Zhou, R., Feng, K. & Yang, S. Ablation of liver cancer cells in vitro by a plasma needle. Appl Phys Lett. 93, 0215021–0215023, doi: 10.1063/1.2959735 (2008).
Schlegel, J., Köritzer, J. & Boxhammer, V. Plasma in cancer treatment. Clin Plasma Med. 1, 2–7, doi: 10.1016/j.cpme.2013.08.001 (2013).
Yan, D. et al. Toward understanding the selective anticancer capacity of cold atmospheric plasma—A model based on aquaporins. Biointerphases. 10, 04080101–04080113, doi: 10.1116/1.4938020 (2015).
Wang, M. et al. Cold Atmospheric Plasma for Selectively Ablating Metastatic Breast Cancer Cells. PloS One. 8, e7374101–e7374111, doi: 10.1371/journal.pone.0073741 (2013).
Zhu, W. et al. Synergistic Effect of Cold Atmospheric Plasma and Drug Loaded Core-shell Nanoparticles on Inhibiting Breast Cancer Cell Growth. Sci Rep. 6, 2197401–2197411, doi: 10.1038/srep21974 (2016).
Keidar, M. et al. Cold plasma selectivity and the possibility of a paradigm shift in cancer therapy. Brit J Cancer. 105, 1295–1301, doi: 10.1038/bjc.2011.386 (2011).
Brulle, L. et al. Effects of a non thermal plasma treatment alone or in combination with gemcitabine in a MIA PaCa2-luc orthotopic pancreatic carcinoma model. PloS One. 7, e5265301–e5265310, doi: 10.1371/journal.pone.0052653 (2012).
Vandamme, M. et al. Response of human glioma U87 xenografted on mice to non thermal plasma treatment. Plasma Med. 1, 27–43, doi: 10.1615/PlasmaMed.v1.i1.30 (2011).
Partecke, L. I. et al. Tissue tolerable plasma (TTP) induces apoptosis in pancreatic cancer cells in vitro and in vivo . BMC Cancer. 12, 47301–47310, doi: 10.1186/1471-2407-12-473 (2012).
Vandamme, M. et al. ROS implication in a new antitumor strategy based on non-thermal plasma. Int J Cancer. 130, 2185–2194, doi: 10.1002/ijc.26252 (2012).
Lee, H. J. et al. Degradation of adhesion molecules of G361 melanoma cells by a non-thermal atmospheric pressure microplasma. New J Phys. 11, 11502601–11502613, doi: 10.1088/1367-2630/11/11/115026 (2009).
Kim, S. J., Chung, T. H., Bae, S. H. & Leem, S. H. Induction of apoptosis in human breast cancer cells by a pulsed atmospheric pressure plasma jet. Appl Phys Lett. 97, 02370201–02370203, doi: 10.1063/1.3462293 (2010).
Tanaka, H. et al. Plasma-Activated Medium Selectively Kills Glioblastoma Brain Tumor Cells by Down-Regulating a Survival Signaling Molecule, AKT Kinase. Plasma Med. 1, 265–277, doi: 10.1615/PlasmaMed.2012006275 (2011).
Yan, D. et al. Controlling plasma stimulated media in cancer treatment application. Appl Phys Lett. 105, 22410101–22410104, doi: 10.1063/1.4902875 (2014).
Yan, D. et al. Principles of using Cold Atmospheric Plasma Stimulated Media for Cancer Treatment. Sci Rep. 5, 1833901-1833901-17, doi: 10.1038/srep18339 (2015).
Adachi, T. et al. Plasma-activated medium induces A549 cell injury via a spiral apoptotic cascade involving the mitochondrial-nuclear network. Free Radical Bio Med. 79C, 28–44, doi: 10.1016/j.freeradbiomed.2014.11.014 (2014).
Mohades, S., Laroussi, M., Sears, J., Barekzi, N. & Razavi, H. Evaluation of the effects of a plasma activated medium on cancer cells. Phys Plasmas. 22, 12200101–12200106, doi: 10.1063/1.4933367 (2015).
Kumar, N. et al. The action of microsecond-pulsed plasma-activated media on the inactivation of human lung cancer cells. J Phys D Appl Phys. 49, 11540101–11540109, doi: 10.1088/0022-3727/49/11/115401 (2016).
Kurake, N. et al. Cell survival of glioblastoma grown in medium containing hydrogen peroxide and/or nitrite, or in plasma-activated medium. Arch Biochem Biophys. available online, doi: 10.1016/j.abb.2016.01.011 (2016).
Utsumi, F. et al. Effect of indirect nonequilibrium atmospheric pressure plasma on anti-proliferative activity against chronic chemo-resistant ovarian cancer cells in vitro and in vivo . PloS One. 8, e8157601–e815760110, doi: 10.1371/journal.pone.0081576 (2013).
Kalghatgi, S. et al. Effects of non-thermal plasma on mammalian cells. PloS One. 6, e1627001–e1627011 (2011).
Ninomiya, K. et al. Evaluation of extra- and intracellular OH radical generation, cancer cell injury, and apoptosis induced by a non-thermal atmospheric-pressure plasma jet. J Phys D Appl Phys. 46, 42540101–42540108, doi: 10.1088/0022-3727/46/42/425401 (2013).
Ahn, H. J. et al. Atmospheric-pressure plasma jet induces apoptosis involving mitochondria via generation of free radicals. PloS One. 6, e2815401–e2815407 (2011).
Ma, Y. et al. Non-Thermal Atmospheric Pressure Plasma Preferentially Induces Apoptosis in p53-Mutated Cancer Cells by Activating ROS Stress-Response Pathways. PloS One. 9, e9194701–e9194714, doi: 10.1371/journal.pone.0091947 (2014).
Gibson, A. R., McCarthy, H. O., Ali, A. A., O’Connell, D. & Graham, W. G. Interactions of a Non-Thermal Atmospheric Pressure Plasma Effluent with PC-3 Prostate Cancer Cells. Plasma Process Polym. 11, 1142–1149, doi: 10.1002/ppap.201400111 (2014).
Ahn, H. J. et al. Targeting cancer cells with reactive oxygen and nitrogen species generated by atmospheric-pressure air plasma. PloS One. 9, e8617301–e8617313, doi: 10.1371/journal.pone.0086173 (2014).
Bekeschus, S. et al. Hydrogen peroxide: A central player in physical plasma-induced oxidative stress in human blood cells. Free Radical Res. 48, 542–549, doi: 10.3109/10715762.2014.892937 (2014).
Kumar, N., Attri, P., Choi, E. H. & Sup Uhm, H. Influence of water vapour with non-thermal plasma jet on the apoptosis of SK-BR-3 breast cancer cells. RSC Adv. 5, 14670–14677, doi: 10.1039/c4ra15879b (2015).
Shashurin, A. et al. Influence of Cold Plasma Atmospheric Jet on Surface Integrin Expression of Living Cells. Plasma Process Polym. 7, 294–300, doi: 10.1002/ppap.200900086 (2010).
Volotskova, O., Hawley, T. S., Stepp, M. A. & Keidar, M. Targeting the cancer cell cycle by cold atmospheric plasma. Sci Rep. 2, 63601–63610, doi: 10.1038/srep00636 (2012).
Cheng, X. et al. Synergistic effect of gold nanoparticles and cold plasma on glioblastoma cancer therapy. J Phys D Appl Phys. 47, 33540201–33540208, doi: 10.1088/0022-3727/47/33/335402 (2014).
Takai, E. et al. Chemical modification of amino acids by atmospheric-pressure cold plasma in aqueous solution. J Phys D Appl Phys. 47, 28540301–28540315, doi: 10.1088/0022-3727/47/28/285403 (2014).
Ishaq, M. et al. Atmospheric gas plasma-induced ROS production activates TNF-ASK1 pathway for the induction of melanoma cancer cell apoptosis. Mol Bio Cell. 25, 1523–1531, doi: 10.1091/mbc.E13-10-0590 (2014).
Wende, K. et al. Identification of the biologically active liquid chemistry induced by a nonthermal atmospheric pressure plasma jet. Biointerphases 10, 02951801–02951816, doi: 10.1116/1.4919710 (2015).
Acknowledgements
This work was supported in part by a National Science Foundation, grant 1465061.
Author information
Authors and Affiliations
Contributions
D.Y. and M.K. designed all experiments. D.Y. and N.N. performed all experiments. J.S., K.B. and F.M. contributed the materials. D.Y. and M.K. contributed to data analysis and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Yan, D., Nourmohammadi, N., Bian, K. et al. Stabilizing the cold plasma-stimulated medium by regulating medium’s composition. Sci Rep 6, 26016 (2016). https://doi.org/10.1038/srep26016
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep26016
This article is cited by
-
Influence of a transient spark plasma discharge on producing high molecular masses of chemical products from l-cysteine
Scientific Reports (2023)
-
Plasma medicine for neuroscience—an introduction
Chinese Neurosurgical Journal (2019)
-
Oxidative stress-dependent and -independent death of glioblastoma cells induced by non-thermal plasma-exposed solutions
Scientific Reports (2019)
-
Dynamics of Singlet Oxygen-Triggered, RONS-Based Apoptosis Induction after Treatment of Tumor Cells with Cold Atmospheric Plasma or Plasma-Activated Medium
Scientific Reports (2019)
-
Production of reactive species in alginate hydrogels for cold atmospheric plasma-based therapies
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.