Abstract
Atrophic vaginitis (AV) is common in postmenopausal women, but its causes are not well understood. The symptoms, which include vaginal itching, burning, dryness, irritation, and dyspareunia, can usually be alleviated by low doses of estrogen given orally or locally. Regrettably, the composition of vaginal bacterial communities in women with AV have not been fully characterized and little is known as to how these communities change over time in response to hormonal therapy. In the present intervention study we determined the response of vaginal bacterial communities in postmenopausal women with AV to low-dose estrogen therapy. The changes in community composition in response to hormonal therapy were rapid and typified by significant increases in the relative abundance of Lactobacillus spp. that were mirrored by a decreased relative abundance of Gardnerella. These changes were paralleled by a significant four-fold increase in serum estradiol levels and decreased vaginal pH, as well as nearly a two-fold increase in the Vaginal Maturation Index (VMI). The results suggest that after menopause a vaginal microbiota dominated by species of Lactobacillus may have a beneficial role in the maintenance of health and these findings that could lead to new strategies to protect postmenopausal women from AV.
Similar content being viewed by others
Introduction
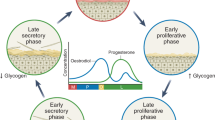
Atrophic vaginitis (AV) is a common affliction that develops in 25% to 50% of postmenopausal women1. Its symptoms include vaginal itching, burning, dryness, irritation, and dyspareunia, which degrade a woman’s quality of life and are unlikely to diminish without treatment2. Studies have shown that AV is associated with estrogen deficiencies during menopause that cause reduced vaginal secretions, vulvovaginal atrophy, and decreased glycogen production by vaginal epithelial cells. It is accompanied by decreased numbers of lactobacilli and lactic acid production, causing an increased vaginal pH that possibly renders the vagina more susceptible to infections1,2. Although the occurrence of vulvovaginal atrophy and increased vaginal pH are nearly universal in menopause, most elderly women do not present with genital complaints, which suggests there are unknown factors that distinguish AV patients and asymptomatic women. So far the preferred treatment of AV symptoms is low-dose estrogen therapy, which minimizes the risk of endometrial and breast cancers that are responsive to estrogen3,4,5. However, the effects of this therapy on the vaginal microbiome are not well understood.
The vaginal microbiome and host immunity are two components of a mutualistic relationship that play a pivotal role in maintaining health and minimizing risk to adverse urogenital problems such as AV. In reproductive age women the vaginal microbiome is often dominated by various species of Lactobacillus that occur in high numbers. This is widely thought to be a normal and healthy state. In contrast, communities in which lactobacilli are supplanted by any of various strictly anaerobic bacteria are often accompanied by symptoms of bacterial vaginosis (BV) that places these women at higher risk to disease as well as obstetric and gynecological complications6. Although considerable efforts have been made to better understand these communities in reproductive-age women, far less is known about the composition and function of these communities in women after menopause.
In this study we compared the vaginal microbiota of healthy post-menopausal women (H group) to those of post-menopausal women with atrophic vaginitis (AV group). Women in the AV group were given low-dose estrogen therapy and followed over a four-week treatment period to observe the response of their vaginal microbiota to the treatment. These were compared to the vaginal microbiota of the untreated H group over the same period of time.
Results
Sixty of the 67 women originally enrolled completed this longitudinal study. Reasons for not continuing in the study included: loss to follow-up (N = 3 in H group), adverse events (nausea in one subject of the AV group), non-compliance (one subject of the AV group), and other reasons (N = 2, one from each group). The microbial community data from samples of one subject (subject 20) in the H group were not included in data analysis because the numbers of DNA sequence reads from vaginal samples were too low. Finally, 59 postmenopausal women with (N = 30) or without (N = 29) AV were enrolled in the present study. Overall, there were no major differences in the baseline characteristics of women in the two groups (Table 1). Subjects had a mean age of 56 years and the range of time since last menses was 21–118 months.
The species composition and structure of vaginal bacterial communities were determined by classifying 16S rRNA gene sequences recovered from mid-vaginal swab samples collected by a physician at 0, 2 and 4 weeks. DNA sequencing using barcoded primers (Supplementary Table S1) produced a dataset that consisted of 982,704 high-quality 16S rRNA gene sequences from 177 samples. On average 5459 ± 2345 (SD) reads were obtained from each sample and these were classified using the Ribosomal Database Project Naïve Bayesian Classifier7. Overall, a total of 288 taxa were observed in the vaginal microbiota of women in the two groups (Supplementary Table S2). The taxonomic assignments of vaginal bacterial community members and the associated metadata for each subject are shown in Supplementary Table S3.
Characterization of vaginal bacterial communities of healthy post-menopausal women
Contrary to the common wisdom that Lactobacillus spp. are usually absent from the vaginal microbiome after menopause8, we found that lactobacilli were prominent members of vaginal communities of most healthy post-menopausal women. They constituted more than half of communities in 55.2% of the women enrolled in the study and more than 0.1% of all bacteria in 83% of the subjects. Other bacteria such as Gardnerella, Lactobacillales, Prevotella and Atopobium were also common and found in 82.8%, 79.3%, 75.9% and 65.5% of communities, respectively, but on average occurred in lower proportions (16.7%, 0.7%, 7.4% and 2.7%, respectively).
The vaginal bacterial communities of healthy post-menopausal women sampled at three visits (weeks 0, 2 and 4 weeks) were clustered based on differences in species composition and their relative abundances (see Fig. 1 and Supplemental Material). We identified three major clusters of vaginal community types. Communities of cluster I were most common and present in 50.6% of the samples. These communities were dominated by Lactobacillus that constituted >50% of all sequences obtained. The communities of cluster II were present in 10.3% of the samples and had high proportions of Prevotella, Atopobium, Streptococcus or Gardnerella. The remainder of communities in Cluster III (39.1%) contained appreciable proportions of various species of strictly anaerobic bacteria, including Gardnerella, Prevotella, Streptococcus, Atopobium, Anaerococcus, Sneathia, Aerococcus, Peptoniphilus, Dialister and Finegoldia along with lower proportions of Lactobacillus. Even though many of these bacterial taxa, including Gardnerella, Prevotella, Atopobium and Sneathia have previously been associated with BV, none of these women had clinical symptoms associated with BV.
Changes in the composition of vaginal microbiota in healthy post-menopausal women over time were visualized in interpolated bar plots of phylotype relative abundance (Fig. 2 and Supplementary Fig. S1). The species composition of vaginal communities in healthy post-menopausal women were rather persistent over time despite differences in their composition among individuals (Fig. 3). This was also reflected in the Shannon diversity and equitability (evenness) indices that did not vary significantly over the 4-week study period (Table 2). The stability was exemplified by the vaginal community of subject H-13, which was dominated by Lactobacillus and exhibited only minor changes over the four-week study period and all three samples remained in cluster I. Similarly, the communities of subject H-12 (dominated by Streptococcus, cluster II) and H-17 (that exhibited co-dominance of several bacterial taxa, cluster III) remained steady during the observation period (Fig. 2B,C) without substantial changes in either the kinds or relative abundances of bacterial taxa present. In contrast, the relative abundances of bacterial taxa in the vaginal community of subject H-4 (cluster III, Fig. 2D) varied at the three time points but the overall composition remained about the same.
Differences in vaginal microbiota between post-menopausal women with and without atrophic vaginitis
Prior to low-dose estrogen therapy the vaginal communities of women with AV differed markedly from those of healthy women in terms of the relative abundances of bacterial taxa (Table 3), especially with regard to the relative abundances of Lactobacillus and Gardnerella. Although species of Lactobacillus were common in women with AV (80% of subjects), they were less abundant and on average constituted only 11.2% of these communities. This contrasts with the vaginal communities of healthy women wherein lactobacilli were significantly more abundant (p < 0.0001) and on average constituted 53.2% of vaginal communities. Conversely, Gardnerella was significantly more abundant than Lactobacillus in the vaginal communities of subjects with AV (p < 0.0001), while also richer in abundance as compared to those of healthy women (41.7% versus 16.7%, p < 0.0001).
Using canonical variable analysis (Fig. 3) we compared the vaginal microbiota profiles of subjects in the H and AV groups. The first canonical variable, which is a linear function of the transformed species proportions, best separated women in these groups at the time of enrollment. At the first sampling time the mean canonical variables of the two groups were significantly different (F = 233.5, P < 0.0001, df = 1, 114, Fig. 3). Differences in the composition of vaginal bacterial communities of healthy women and women with AV at the time of enrollment were visualized by principal component analysis (PCA) (Fig. 4A). However, the overall diversity and evenness of bacterial communities in these two groups were not significantly different between healthy women and those with AV (Table 2).
Each point corresponds to a single subject at a single time point and was colored according to group membership and time of sampling. The percentages given in the axis labels wee the proportion of variation explained by that principal component. (A) Comparison of vaginal bacterial communities of healthy post-menopausal women at week 0 (green dots) to those of women with atrophic vaginitis at week 0 (red dots). (B) Comparison of vaginal bacterial communities of women with atrophic vaginitis at week 0 (red dot) to those in the AV group after 4 weeks of estrogen therapy (blue dots).
Vaginal clinical and microbiota response to low-dose estrogen treatment
AV patients indicated a significant change in their condition when treated with low-doses of estrogen, which was consistent with previous results9,10. In response to treatments the serum concentration of estradiol increased from an average of 42.05 ± 7.68 pmol/L prior to treatment to an average of 168.07 ± 8.30 pmol/L at week 2 with virtually no further increase between weeks 2 and 4 (Table 4). These changes in serum estradiol levels were accompanied by progressive increases in the VMI and decreases in both symptom scores and vaginal pH (Table 4). The positive effects of estrogen therapy were quite evident after two weeks of treatment. In subjects with AV the mean VMI was 28.1 at the time of enrollment, but increased to 39.3 by week 2 and reached 55.4 by week 4. These changes in VMI were paralleled by decreases in vaginal pH, which was initially 6.6 (on average) at the time of enrollment but decreased to 5.4 and 5.0 after two and four weeks of therapy, respectively. It is not known if further decreases in pH would have occurred with continued therapy.
Low-dose estrogen therapy also had marked effects on the composition of vaginal microbiota. When displayed by PCA, the majority of samples from women in the AV group at week 0 and week 4 were clearly assembled in different regions, indicated that the communities of individuals significantly changed when the host was treated with estrogen (Fig. 4B). A repeated measures ANOVA on the canonical variable for differences between groups and across time showed a significant interaction between group and time (F = 188.7, df = 2, 114, P < 0.0001). Simple effects tests to investigate group differences at each time point showed a trend where the highly significant group difference at time zero (described above) became not quite significant after two weeks and then not significant after four weeks (F = 233.5, P < 0.0001; F = 3.29, P = 0.072; F = 0.28, P = 0.60, respectively, with df = 1, 114 for all three tests). The box plots in Fig. 3 illustrate this pattern wherein communities in most women of the AV group became similar to those in the H group after estrogen treatment. Moreover, decreases of Shannon diversity and Shannon equitability indices were observed (Table 2) indicating that the observed community diversity appeared to decrease in response to treatment.
Concomitant with these changes were profound changes in the species composition of vaginal communities of most women (24/30) treated for AV. The relative proportions of Lactobacillus increased dramatically from 11.2 to 71.0% (p < 0.0001) and dominated the vaginal communities of 76.7% of treated subjects. This was accompanied by corresponding decreases in the abundances of other prominent bacteria such as Gardnerella, Prevotella, and Atopobium (Table 5). These changes were illustrated in interpolated bar plots of phylotype relative abundances for Subject AV-3 whose vaginal community was dominated by Gardnerella before treatment and Subject AV-24 whose vaginal community included a mixture of strictly anaerobic bacteria. In both cases the two communities were transformed to ones dominated by Lactobacillus (Fig. 5A,B). Statistical analyses were done to assess whether there was an association between the severity of genital symptoms and specific taxa. We found that Lactobacillus was negative correlated (P < 0.0001; Spearman’s test) with symptom scores, whereas Gardnerella and Atopobium were positively correlated with genital symptoms (Table 5).
Color codes for each phylotype represented in the interpolated bar plots are displayed on the right side of the figure. See Supplementary Fig. S2 interpolated bar plots for all subjects.
Interestingly, the vaginal communities of six women (6/30) treated with estrogen did not transition to a state in which the community was dominated by lactobacilli even though their serum estradiol levels had increased. Instead, there were differing responses among the subjects. Although the communities of four subjects (AV-4, AV-6, AV-7 and AV-9) initially differed from each other, they came to be dominated by Gardnerella by week 4 of estrogen therapy (Fig. 5 and Supplementary Fig. S2). In contrast, at the conclusion of estrogen therapy the vaginal communities of two other subjects (AV-11 and AV-26; Supplementary Fig. S2 and Fig. 5) were dominated by Streptococcus alone or Bifidobacterium and Streptococcus, respectively. This showed there can be interpersonal variation among vaginal bacterial communities in response to low dose estrogen therapy.
Discussion
In this study we found there was a marked and rapid shift in the composition of vaginal communities in most AV patients (24/30) that was accompanied by an alleviation of symptoms. Specifically, Lactobacillus came to dominate the vaginal communities by increasing from 11.2 to 71.0% (p < 0.0001) of communities on average in 80% of treated subjects, with a corresponding decrease in the relative proportions of Gardnerella, Atopobium and Prevotella. In most cases the resulting communities closely resembled those found in healthy postmenopausal women. These findings suggest that the emergence of a Lactobacillus-dominated vaginal community may be considered as one of the signs of AV treatment success along with the alleviation of genital symptoms, elevated serum estradiol levels and VMI scores. This is consistent with the findings of Hummelen et al.11 who also found an inverse correlation between the relative abundances of Lactobacillus and genital symptom scores although the number of subjects in their study was small (4 AV cases and 6 healthy women).
The results of our study challenge the assertion that to maintain health of the female lower genital tract vaginal communities must be dominated by species of Lactobacillus that lower the vaginal pH12. We found that while Lactobacillus spp. were found in the majority of healthy post-menopausal women it was the dominant species in only 53.2% of vaginal communities that had a mean pH of 6.6 ± 0.2. This is substantially higher than the pH 4.5 threshold that is thought to be necessary for vaginal health and protection in reproductive age women, but concordant with the findings of other studies on postmenopausal women13,14. Moreover, we found no difference between the vaginal pH of healthy postmenopausal women and women with AV. These findings show that neither high proportions of lactobacilli or a low vaginal pH are required for health in postmenopausal women. The inverse relationship between serum estradiol levels and vaginal pH has long been known1,2,3,4 and our findings lend further support to this relationship as we too observed that the vaginal pH of AV patients typically decreased in response to low-dose of estrogen therapy and it remained higher and stable when there were lower levels of serum estradiol. There is increasing evidence that total lactic acid bacterial numbers in the vaginas of post-menopausal women might be 10–100 fold lower than in reproductive age women15,16 that would sharply reduce the amount of lactic acid production. These data suggest that the vaginal pH of postmenopausal women might best reflect systemic estrogen levels, which are negatively correlated with VMI scores.
Our findings also contravene the widely held view that vaginal communities of post-menopausal women are depauperate of Lactobacillus17,18,19,20,21. Instead our findings are entirely consistent with those who have demonstrated the presence of lactobacilli in a fair proportion of postmenopausal women22,23,24,25,26,27. For example, Hillier and Lau et al.27 found that various species of Lactobacillus could be cultured from 50% of postmenopausal women, but the numbers of Lactobacillus were 10–100X lower than in reproductive age women. These investigators speculated that the microbiota of postmenopausal women might be similar to those of pre-menarchal girls that also have lower levels of peripheral estrogen. Hickey et al.28 have recently substantiated this postulate by determining that lactic acid bacteria, primarily Lactobacillus spp., were dominant in the microbiota of most girls well before the onset of menarche in the early to middle stages of puberty. In recent years the prominence of Lactobacillus in the vaginal microbial communities of some postmenopausal women has been reported11,24, which is consistent with our findings. This suggests that Lactobacillus spp. per se might be more important than pH in sustaining vaginal health after menopause. Aside from the production of lactic acid which itself has antimicrobial properties, Lactobacillus spp. produce other antimicrobial compounds such as antibiotics and target-specific bacteriocins29 that probably contribute to the antagonistic capacity of Lactobacillus and contribute to preventing invasion of the vaginal microbiome by non-indigenous species. Supporting evidence was reported by Rose et al.30 who showed that certain lactobacilli reduced cytokine secretion in an isolate-specific fashion following TLR stimulation of cultured vaginal epithelial cells and by Bisanz et al.31 who showed that lactobacilli may regulate epithelial innate immunity in a species-specific manner and by doing so contribute to the microbiome’s ability to effectively exclude pathogenic organisms.
Two bacterial genera, Gardnerella and Atopobium, were statistically associated with AV in postmenopausal women. Likewise both of these genera have also been associated with the incidence of BV in reproductive age women and shown to have a number of putative virulence determinants32. For example, Gardnerella has a propensity to form dense biofilms and produce vaginolysin, a member of the cholesterol-dependent family of pore-forming toxins leading to vaginal epithelial cells lysis and death33,34 while Atopobium has been shown to trigger an innate immune response in an in vitro model of BV35. Others have reported a potential synergism between Gardnerella and Atopobium because more than 90% of bacteria in biofilms adhering to the vaginal epithelium were comprised of these two genera in women with BV36,37. However, the roles of these bacteria in AV are unclear since they were also often present in the vaginal communities of healthy post-menopausal women, albeit at somewhat lower proportions. Additionally, these two genera have also occur in the vaginal communities of healthy younger reproductive women and adolescent girls7,38. The occurrence of Gardnerella and Atopobium in vaginal microbiomes of healthy and diseased individuals of all ages is a conundrum that might be explained by genetic differences among strains of these species39; a proposition that is entirely plausible given the genetic diversity found within both genera.
Brotman et al. recently reported that a distinct bacterial community characterized by Streptococcus and Prevotella with a low relative abundance of Lactobacillus is associated with vulvovaginal atrophy24. In this study 28 women at different stages of menopause (pre-, peri- and postmenopause) were sampled, but there were only two cases of AV and 14 women with vulvovaginal atrophy. They found no statistically significant associations between clinical variables (menopause stage, signs of vulvovaginal atrophy and vaginal dryness) and any specific species in the communities. Our findings differ from those of Brotman et al.24 in so far as Gardnerella and Atopobium were the most frequent and abundant taxa in vaginal communities of women with AV and there was a statistically positive correlation between their prevalence and genital symptom scores. These compelling findings imply that strains of various bacterial species might be associated with the emergence of AV and that new therapeutic targets might emerge as more is learned about the possible causes of AV.
Methods
Study Design and Subjects
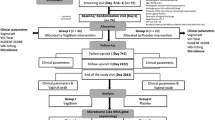
The individuals enrolled in the study were drawn from outpatients in the Department of Obstetrics and Gynecology of Ruijin Hospital, which is affiliated with the Shanghai Jiaotong University School of Medicine in Shanghai, China. The University’s Institutional Review Board reviewed and approved the project. All patient enrollment occurred between June 2011 and February 2012. After obtaining informed consent participants were screened to confirm eligibility before enrollment. As part of this screening we assessed Vaginal Maturation Index (VMI)40, vaginal pH, baseline serum, sexual hormone levels and baseline menopausal quality of life. Women were asked to refrain from sexual activity in the 48 h before the visit.
All methods were carried out in accordance with the guidelines and study protocol approved by the Institutional Review Board and written informed consent was obtained from all subjects that participated in the study. Study subjects with AV (hereafter referred to as the AV Group) met the following criteria: (a) experienced twelve consecutive months of amenorrhea without a period secondary to decreased levels of circulating estrogen caused by depletion of follicles; (b) obvious genital symptoms (e.g. burning, dryness, itching, irritation, soreness and/or bleeding, dyspareunia) with distinct vulvar symptoms that included diminished elasticity, skin turgor, sparse pubic hair, dry labia, dermatoses, lesions, fusion of labia minora, and vaginal symptoms with pale, smooth, lubrication-lacking epithelium or inflammation with patchy erythema, petechiae, increased friability; (c) a positive result on microscopic examination of 5% or less superficial vaginal cells and increased vaginal pH (>5.0); (d) increased follicle stimulating hormone (FSH) concentrations (40 IU/L or more); (e) decreased serum estradiol concentrations (20 pg/mL or less); (f) an endometrial thickness of 5 mm or less as determined by transvaginal ultrasonography, (g) a body mass index between 18.0 and 35.0 kg/m2; (h) did not smoke or use tobacco or nicotine; and (i) did not have trichomoniasis or candidiasis. A group of healthy post-menopausal women that did not meet these criteria and had no other preexisting condition were also enrolled and referred to as the H group.
Postmenopausal women were excluded from the study if they had used any antibiotics or antimycotics, vaginal medications, vaginal suppositories, douches, feminine sprays, or genital wipes in the past 30 days, or if they had taken any estrogen products 6 months prior to screening visit (week 0). Other exclusion criteria were systemic diseases or chronic conditions (diabetes mellitus, immunological disease), use of immunosuppressive drugs, exogenous corticosteroids, chemotherapy, or having impaired bladder emptying or pelvic-floor dysfunction causing urinary incontinence, genital prolapse, cystocele, or a history of urogenital surgery24.
After enrollment, subjects in the AV Group received low-dose (0.3 mg) conjugated estrogens (Premarin, Wyeth) orally once per day for a 4-week period.
Sample collection and clinical exams
A physician used the Elution-swab system (Copan) to collect vaginal swab samples from subjects in the AV Group and the H Group at the initial visit (week 0) as well as 2 and 4 weeks later. All swabs were stored in 1 ml of Amies transport medium (Copan) and frozen upright on dry ice until they could be transported to the laboratory, where they were stored at −80 °C. These were used for analysis of bacterial community composition.
During these visits VMI, vaginal pH, serum estradiol and menopausal quality of life were appraised. To determine the VMI of the vaginal mucosa cytology specimens were collected at enrollment (week 0) and at each treatment visit (weeks 2 & 4). The collected cells and mucus were mixed in a fixative solution to form a cell suspension, which was viewed microscopically. The number of superficial, intermediate, and parabasal cells were counted and the percentages of each cell type were calculated. These percentages were used to determine the VMI, which is calculated as follows: VMI = (% intermediate cells × 0.5) + % superficial cells. During the same visit vaginal pH was measured by inserting pH paper into the vagina and comparing the color change result with the manufacturer’s color chart (pHEM-ALERT®, Gynex Corporation, Redmond, WA). The serum concentrations of sexual hormones were assessed using electro-chemiluminescence immunoassays (Elecsys 1010 Analyzer, Roche). Lastly, each participant completed a self-assessment of symptoms score which was rated as none, mild, moderate or severe11 to assess the severity of genital symptoms such as vaginal dryness, irritation or itching, pain during urination not associated with infection, vaginal soreness, pain during sexual intercourse and bleeding after sexual intercourse.
Classification of bacterial populations based on sequences of the V1-V3 region of bacterial 16S rRNA genes
All methods and algorithms used to gather and analyze DNA sequence data are provided in Supplementary Methods. In brief, a validated method7 was used to extract total genomic DNA (gDNA) from vaginal swabs using the QIAamp DNA Mini Kit (Qiagen, Hilden, GER). The variable V1-V3 regions of 16S rRNA genes in each gDNA sample were amplified in two rounds of PCR with dual barcode indexing using the PCR primer sequences shown in Supplementary Table S1. The final amplicons were sequenced using an Illumina MiSeq platform (Illumina, San Diego, CA, USA) and the RDP Bayesian classifier was used to assign clipped and concatenated sequences to phylotypes (RDP 2.5; http://rdp.cme.msu.edu). For constructing phylotype abundance tables we used a simple heuristic rule: to be included in the table a phylotype had to either: (a) be present in more than one sample at an abundance of 1% or more, or (b) constitute more than 5% of a single community. Phylotypes that did not meet either of these criteria were aggregated into an “Other” category.
Additional Information
How to cite this article: Shen, J. et al. Effects of low dose estrogen therapy on the vaginal microbiomes of women with atrophic vaginitis. Sci. Rep. 6, 24380; doi: 10.1038/srep24380 (2016).
Change history
29 November 2016
A correction has been published and is appended to both the HTML and PDF versions of this paper. The error has been fixed in the paper.
References
Sturdee, D. W. & Panay, N. International Menopause Society Writing Group. Recommendations for the management of postmenopausal vaginal atrophy. Climacteric 13, 509–522 (2010).
Castelo-Branco, C., Cancelo, M. J., Villero, J., Nohales, F. & Juliá, M. D. Management of post-menopausal vaginal atrophy and atrophic vaginitis. Maturitas 52S, S46–S52 (2005).
Skouby, S. O. et al. Climacteric medicine: European Menopause and Andropause Society (EMAS) 2004/2005 position statements on peri- and postmenopausal hormone replacement therapy. Maturitas 51, 8–14 (2005).
The North American Menopause Society. Management of symptomatic vulvovaginal atrophy: 2013 position statement of The North American Menopause Society. Menopause. 20, 888–902 (2013).
Simon, J. A., Reape, K. Z., Wininger, S. & Hait, H. Randomized, multicenter, double-blind, placebo-controlled trial to evaluate the efficacy and safety of synthetic conjugated estrogens B for the treatment of vulvovaginal atrophy in healthy postmenopausal women. Fertil. Steril. 90, 1132–1138 (2008).
Zhou, X. et al. Recent advances in understanding the microbiology of the female reproductive tract and the causes of premature birth. Infect. Dis. Obstet. Gynecol. 2010, 737425 (2010).
Ravel, J. et al. Vaginal microbiome of reproductive-age women. Proc. Natl. Acad. Sci. 108S1, 4680–4687 (2011).
Raz, R. & Stamm, W. E. A controlled trial of intravaginal estriol in postmenopausal women with recurrent urinary tract infections. N. Engl. J. Med. 329, 753–756 (1993).
Marx, P., Schade, G., Wilbourn, S., Blank, S., Moyer, D. L. & Nett, R. Low-dose (0.3 mg) synthetic conjugated estrogens A is effective for managing atrophic vaginitis. Maturitas 47, 47–54 (2004).
Bachmann, G., Lobo, R. A., Gut, R., Nachtigall, L. & Notelovitz, M. Efficacy of low-dose estradiol vaginal tablets in the treatment of atrophic vaginitis: a randomized controlled trial. Obstet. Gynecol. 111, 67–76 (2008).
Hummelen, R. et al. Vaginal microbiome and epithelial gene array in post-menopausal women with moderate to severe dryness. PloS One 6, e26602 (2011).
Sobel, J. D. Is there a protective role for vaginal flora? Curr. Infect. Dis. Rep. 1, 379–383 (1999).
Caillouette, J. C., Sharp, C. F. Jr., Zimmerman, G. J. & Roy, S. Vaginal pH as a marker for bacterial pathogens and menopausal status. Am. J. Obstet. Gynecol. 176, 1270–1277 (1997).
Crandall, C. Vaginal estrogen preparations: A review of safety and efficacy for vaginal atrophy. J. Women’s Health 11, 857–877 (2002).
Mirmonsef, P. et al. Exploratory comparison of vaginal glycogen and Lactobacillus levels in premenopausal and postmenopausal women. Menopause 22, 702–709 (2015).
Galhardo, C. L., Soares, J. M., Simoes, R. S., Haidar, M. A., Rodrigues, D. L. G. & Baracat, E. C. Estrogen effects on the vaginal pH, flora and cytology in late postmenopause after a long period without hormone therapy. Clin. Exp. Obstet. Gynecol. 33, 85–89 (2006).
Colodner, R., Edelstein, H., Chazan, B. & Raz, R. Vaginal colonization by orally administered Lactobacillus rhamnosus GG. Isr. Med. Assoc. J. 5, 767–769.(2003).
Mac, B. M. B., Rhodes, D. J. & Shuster, L. T. Vulvovaginal atrophy. Mayo Clin. Proc. 85, 87–94 (2010).
Yoshimura, T. & Okamura, H. Short term oral estriol treatment restores normal premenopausal vaginal flora to elderly women. Maturitas 39, 253–257 (2001).
Pabich, W. L., Fihn, S. D., Stamm, W. E., Scholes, D., Boyko, E. J. & Gupta, K. Prevalence and determinants of vaginal flora alterations in postmenopausal women. J. Infect. Dis. 188, 1054–1058 (2003).
Cauci, S. et al. Prevalence of bacterial vaginosis and vaginal flora changes in peri- and postmenopausal women. J. Clin. Microbiol. 40, 2147–2152.(2002).
Zhang, R., Daroczy, K., Xiao, B., Yu, L., Chen, R. & Liao, Q. Qualitative and semiquantitative analysis of Lactobacillus species in the vaginas of healthy fertile and postmenopausal Chinese women. J. Med. Microbiol. 61, 729–739 (2012).
Petricevic, L. et al. Differences in the vaginal lactobacilli of postmenopausal women and influence of rectal lactobacilli. Climacteric 16, 356–361 (2012).
Brotman, R. M. et al. Association between the vaginal microbiota, menopause status, and signs of vulvovaginal atrophy. Menopause 21, 450–458 (2014).
Gustafsson, R. J. et al. The Lactobacillus flora in vagina and rectum of fertile and postmenopausal healthy Swedish women. BMC Womens Health 11, 17 (2001).
Heinemann, C. & Reid, G. Vaginal microbial diversity among postmenopausal women with and without hormone replacement therapy. Can. J. Microbiol. 51, 777–781 (2005).
Hillier, S. L. & Lau, R. J. Vaginal microflora in postmenopausal women who have not received estrogen replacement therapy. Clin. Infect. Dis. 25S2, S123–126 (1997).
Hickey, R. J. et al. Vaginal microbiota of adolescent girls prior to the onset of menarche resemble those of reproductive-age women. mBio 6(2), e00097–15 (2015).
Linhares, I. M., Summers, P. R., Larsen, B., Giraldo, P. C. & Witkin, S. S. Contemporary perspectives on vaginal pH and lactobacilli. Am. J. Obstet. Gynecol. 204,120.e1-5 (2011).
Rose 2nd, W. A., McGowin, C. L., Spagnuolo, R. A., Eaves-Pyles, T. D., Popov, V. L. & Pyles, R. B. Commensal bacteria modulate innate immune responses of vaginal epithelial cell multilayer cultures. PLoS One. 7, e32728 (2012).
Bisanz, J. E. et al. A systems biology approach investigating the effect of probiotics on the vaginal microbiome and host responses in a double blind, placebo-controlled clinical trial of post-menopausal women. PLoS One. 9, e104511 (2014).
Pybus, V. & Onderdonk, A. B. Microbial interactions in the vaginal ecosystem, with emphasis on the pathogenesis of bacterial vaginosis. Microbes Infect. 1, 285–92 (1999).
Patterson, J. L., Stull-Lane, A., Girerd, P. H. & Jefferson, K. K. Analysis of adherence, biofilm formation and cytotoxicity suggests a greater virulence potential of Gardnerella vaginalis relative to other bacterial-vaginosis-associated anaerobes. Microbiol. 156, 392–399 (2010).
Gelber, S. E., Aguilar, J. L., Lewis, K. L. & Ratner, A. J. Functional and phylogenetic characterization of vaginolysin, the human-specific cytolysin from Gardnerella vaginalis. J. Bacteriol. 190, 3896–3903 (2008).
Libby, E. K., Pascal, K. E., Mordechai, E., Adelson, M. E. & Trama, J. P. Atopobium vaginae triggers an innate immune response in an in vitro model of bacterial vaginosis. Microb. Infect. 10, 439–446 (2008).
Hale, L. P., Swidsinski, A. & Mendling, W. Bacteria associated with bacterial vaginosis. N. Engl. J. Med. 354, 202–203 (2006).
Swidsinski, A. et al. Adherent biofilms in bacterial vaginosis. Obstet. Gynecol. 106, 1013–1023 (2005).
Mitchell, C. M., Fredricks, D. N., Winer, R. L. & Koutsky, L. Effect of sexual debut on vaginal microbiota in a cohort of young women. Obstet Gynecol. 120, 1306–1313 (2012).
Ahmed, A. et al. Comparative genomic analyses of 17 clinical isolates of Gardnerella vaginalis provide evidence of multiple genetically isolated clades consistent with subspeciation into genovars. J. Bacteriol. 194, 3922–3937 (2012).
Willhite, L. & O’Connell, M. B. Urogenital atrophy: prevention and treatment. Pharmacotherapy 21, 464–480 (2001).
Acknowledgements
This research was supported by a grant from the National Institute of General Medical Sciences of the National Institutes of Health (P30GM103324) to Larry J. Forney, grants from Shanghai Population and Family Planning Commission (2007JG04, 2009JG04) to Chen Xu and a grant from Shanghai Health and Family Planning Commission (201440339) to Jian Shen. We thank G. Maria Schneider, Sanqing Yuan and Dongsheng Hou for technical assistance with DNA extraction. We thank Matthew Settles, Dan New and Suresh Iyer for technical assistance with sequence analysis and taxonomic assignments. We thank Dr. Yan Liu and Wenqing Long for support with sampling.
Author information
Authors and Affiliations
Contributions
J.S., C.X. and L.J.F. conceived the original idea and designed the study. J.S. conducted sampling and most of the experiments. N.S. contributed to the statistical modeling analyses. C.W., C.B. Z.Y. and N.S. performed the statistical analyses. J.S., L.J.F. and C.X. interpreted the data and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Shen, J., Song, N., Williams, C. et al. Effects of low dose estrogen therapy on the vaginal microbiomes of women with atrophic vaginitis. Sci Rep 6, 24380 (2016). https://doi.org/10.1038/srep24380
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep24380
This article is cited by
-
Changes in the Vaginal Microbiome During Pregnancy and the Postpartum Period in South African Women: a Longitudinal Study
Reproductive Sciences (2024)
-
Towards a deeper understanding of the vaginal microbiota
Nature Microbiology (2022)
-
The effect of local estrogen therapy on the urinary microbiome composition of postmenopausal women with and without recurrent urinary tract infections
International Urogynecology Journal (2022)
-
Effect of 17β-estradiol on a human vaginal Lactobacillus crispatus strain
Scientific Reports (2021)
-
Changes in the vaginal microbiota across a gradient of urbanization
Scientific Reports (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.