Abstract
Prospective studies on the association of green tea with risk of coronary heart disease (CHD) incidence were scarce. This study examined whether green tea can reduce CHD incidence and have a beneficial effect on CHD-related risk markers in middle-aged and older Chinese population. We included 19 471 participants who were free of CHD, stroke or cancer at baseline from September 2008 to June 2010, and were followed until October 2013. Cox proportional hazard models were used to examine the hazard ratios (HR) of CHD incidence in relation to green tea consumption. Linear regression models were used to evaluate the effect of green tea on 5-year changes of CHD-related biomarkers. Compared with non-green tea consumers, the multivariable-adjusted HR for CHD was 0.89 (95% CI, 0.81-0.98) in green tea consumers. Particularly, the reduced risk of CHD incidence with green tea consumption was more evident among participants who were male, more than 60 years old, overweight, or with diabetes mellitus. In addition, green tea consumption improved multiple CHD-related risk markers including total cholesterol, HDL-cholesterol, triglycerides, mean platelet volume, and uric acid. In conclusion, green tea consumption was associated with a reduced risk of CHD incidence in the middle-aged and older Chinese populations, and the association might be partly due to altered CHD-related biomarkers.
Similar content being viewed by others
Introduction
Cardiovascular disease (CVD) has become the leading cause of death and continues to exert a heavy burden in China. The number of patients with CVD increased to 290 million in 2014 with one out five Chinese adults suffering from the disease1. Coronary heart disease (CHD) accounts for the greatest proportion of CVD2, and the prevalence of Chinese people with CHD is increasing substantially due to ageing, imbalanced diets, unhealthy behaviors and the raising standard of living3. Thus, early prevention and control of CHD has become an extremely important public health concern.
Tea, a beverage made from leaves of Camellia sinensis, is the second most consumed beverage worldwide, only close to plain water4. Tea was generally categorized into black, green and oolong tea according to the manufacturing process. Black tea, which covers about 78% of the total tea production, is usually consumed in the West; whereas green tea, which covers 20%, is consumed primarily in Japan, China and other East Asian countries5. A recent meta-analysis of prospective studies based mainly on evidence from black tea or unspecified tea showed that tea consumption was associated with a reduced risk of CHD, and found that the associations between tea consumption and cardiovascular outcomes differ according to sex, ethnicity, and the type of tea consumed6. On the contrary, data on the association between green tea and CHD was limited and inconclusive. Several cohort studies have suggested an inverse association between green tea and CVD mortality7,8,9,10. Although dose-response relationship between green tea and risk of CHD was reported in case-control and cross-sectional studies11,12,13, only two cohort studies have examined the impact of green tea consumption on risk of CHD incidence and no significant association was observed11,14. On the other hand, favorable changes in CHD-related biomarkers, such as blood pressure, LDL cholesterol and glucose levels, were reported with green tea in randomized controlled trials15,16,17,18, which suggested a possible protective effect of green tea against CHD. However, most existing studies have only focused on one aspect: either green tea versus CHD, or green tea versus biomarkers; seldom studies have so far examined both of them on a same population.
Because of the high consumption of green tea in China and relatively high rate of CHD incidence and mortality, exploring the health effects of green tea on CHD might provide clues to resolve an important public health issue. Therefore, we aimed to 1) verify the relationship between green tea and CHD incidence in the Dongfeng-Tongji cohort; 2) examine whether the association between green tea and CHD was modified by differences in population characteristics and disease status; and 3) evaluate the effect of green tea on changes of multiple CHD-related biomarkers.
Results
Baseline characteristics of study population
As shown in Table 1, in 19 471 eligible participants, a total of 7021 were green tea consumers (36.06%). Men and participants with higher education level were more likely to consume green tea. The mean age of green tea consumers was higher than that of non-green tea consumers, and the age distribution was different. Higher rate of smoking and alcohol drinking, two of the most common and inveterate habits linked with poor health in China, were also observed in green tea consumers. Meanwhile, green tea consumers more often tended to be physically inactive, with higher BMI and uric acid level, and with hyperlipidemia. However, they exhibited lower levels of total cholesterol and LDL-C.
Green tea consumption reduced incident CHD risk
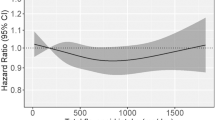
Table 2 presents the 5-year cumulative CHD incidence rate of green tea consumers compared to non-green tea consumers, along with adjusted HR of incident CHD. Overall, green tea consumers had a reduced CHD incidence of 9.80% compared to 11.06% for non-green tea consumers (P = 0.006). In crude models, green tea consumption was associated with lower risk of CHD incidence (HR = 0.88, 95% CI = 0.80–0.96). After adjustment for age, sex, BMI, education, smoking status, alcohol drinking status, physical activity, hypertension status, hyperlipidemia status, diabetes status and family history of CHD at baseline, these associations became more obvious (HR = 0.85, 95% CI = 0.77–0.94). Additional adjustment for four other common beverages including coffee, black tea, juice and cola, the effect was slightly attenuated, but still remained statistically significant and corresponded to an 11% reduced risk of CHD incidence (HR = 0.89, 95% CI = 0.81–0.98).
We subsequently conducted stratified analyses by major characteristics of the study population. Substantial reduction of CHD incidence with green tea consumption was only seen in participants who were male, older than 60 years, overweight (BMI ≥ 25) or with diabetes mellitus. No significant interactions between green tea consumption and these characteristics on risk of CHD were observed.
Green tea consumption improved CHD-related biomarkers
As shown in Table 3, the mean levels of total cholesterol, LDL-C, and MPV were significantly decreased, while HDL-C and uric acid were significantly elevated at 5-year follow-up compared to baseline in both green tea consumers and non-green tea consumers (all P < 0.001). On the contrary, significantly increased levels of triglycerides (P < 0.001) and fast glucose (P = 0.028) were only observed in non-green tea consumers. Moreover, after adjustment for age, sex, BMI, education, smoking status, alcohol drinking status, physical activity and the baseline level of each biomarker, green tea consumers had greater reductions in total cholesterol and MPV, greater increase in HDL-C, and smaller increase in triglycerides and uric acid than did non-green tea consumers over time (all P < 0.05). Overall, each tested biomarker improved more or worsened less over 5 years for green tea consumers.
Discussion
The present study demonstrated that green tea consumption was independently related to an 11% reduction of CHD incidence, notwithstanding green tea consumers appear to have an unfavorable risk profile. Our findings add a considerable body of knowledge to previous studies. Some prior case-control or cross-sectional studies conducted in Japan generated inconsistent results regarding green tea and angiographically proven CHD. Several of those studies showed a protective relationship between green tea intake and CHD or coronary atherosclerosis11,13, whereas Hirano et al. did not find any inverse association of green tea intake with CHD19. Evidence in Chinese population was also limited. In a case-control study, Wang et al. found that green tea intake was associated with a reduced risk of CHD among Chinese male patients, but not in female patients12. More recently, Pang et al. also reported a dose-response relationship between green tea consumption and the risk of CHD in male patients20. Although insightful, those studies were case-control or cross-sectional, and may yield recall or reverse causality biases. Our prospective study is the first to agree with the majority of previous case-control or cross-sectional studies on the positive relationship between green tea and risk of CHD. Until now, no prospective study had shown evidence that green tea consumption is preventive of CHD incidence, as they generally indicated beneficial effects on CVD mortality only7,8,9,10. However, participants who consumed green tea in these cohort studies7,8,9,10 more often tended to have unfavorable risk profiles such as being older, current smoker, current alcohol drinker, having a history of hypertension or diabetes, or less likely to walk, which was consistent with the characteristics of our green tea consumers.
Several reasons could explain the disparity between our findings and those from previous prospective studies. Sano et al. found that green tea intake was not a predictor of CHD events after 4.9 ± 0.1 years follow-up, partly because of the small number of CHD events (n = 38)11. In another large prospective study conducted in a Japanese population, inverse associations of green tea consumption were only observed with the incidences of CVD and strokes, but not with CHD14. In the study from Japan, the mean age of participants was about 53 years at baseline and the average follow-up duration was 13 years; while in our study, the participants had a mean age of 62.8 years at baseline and they were only followed for about 5 years. Meanwhile, in that study, only MI and cardiac death was defined as outcomes. A total of 910 CHD events in 82 369 subjects (1.10%) were documented during a 13-year follow-up. In contrast, our study included SA, UA, MI, unspecified CHD and cardiac death as endpoints, and a total of 2065 cases were documented from 19 471 subjects (10.61%). Therefore, the low incidence rate and insufficient statistical power might be a possible reason for not detecting a significant effect of green tea on CHD incidence in that study. In addition, the disparate results might also be due to inherent differences in population characteristics such as age distribution, different definitions of end points, the processing of the tea, and sample size.
Interestingly, the above-mentioned association between green tea consumption and reduced risk of CHD incidence appeared to be more pronounced in individuals who were male, more than 60 years old, overweight or with diabetes, but no interaction noted. Consistent with the observations of our subgroups, results in all subgroups defined by traditional CVD risk factors from a former study also showed no interactions between green tea consumption and CVD risk factors on CVD mortality10. We cannot explain the underlying mechanism for this observation, but similar results in males were reported from several previous studies12,13. It is believed that estrogen may reduce the risk of CHD, while Wu et al. suggested that green tea consumption could decrease circulating estrogen levels21. So, we speculate that in female participants the protective association with green tea would be masked by this uncontrolled confounding variable. As green tea has been reported to generate weight loss, anti-aging, anti-diabetic22 and anti-androgen23 effects, individuals who were more than 60 years old, overweight or suffering from diabetes tended to consume more green tea to counteract these problems, thus, a stronger protective effect of green tea against CHD was observed in these high-risk populations. However, we could not directly compare our results with previous studies because no similar findings were reported.
Although the biological mechanisms underlying the protective effects of green tea on CHD remain unclear, most of randomized controlled trials have demonstrated beneficial effects of green tea on CVD risk profiles17,24. We therefore simultaneously explored the changes of CHD-related biomarkers at 5-year follow-up compared to baseline. We observed that green tea consumers had a greater reduction in total cholesterol, smaller increase in triglycerides, and a greater increase in HDL-C, which was in accordance with previous human and animal studies25. Similarly, green tea consumers also exhibited greater decrease in MPV, an indicator of platelet activation. A high MPV value represents an increase in platelet aggregation, thromboxane synthesis, and adhesion molecules expression26,27. An elevated MPV has also been associated with an increased risk of CHD28,29. Our results supported previous evidence that green tea had anti-platelet and anti-thrombotic activity30,31. In addition, despite higher baseline levels of uric acid, another risk marker of incident CHD32, we also found a smaller increase of uric acid in green tea consumers, in agreement with clinical trials33,34. In general, the above favorable changes in CHD-related biomarkers could be partially responsible for the protective effect of green tea on CHD incidence, whereas other mechanisms including radical scavenging, antioxidant bioactivity, and improvement of endothelial function still need further investigation.
There are several limitations in the present study. First, green tea consumption was based on self-reporting by the participants and only documented as green tea consumers or non-green tea consumers. The amount, frequency, duration, concentration of green tea consumption and other details were not included in the questionnaire. Thus we cannot perform a dose-response analysis to quantitatively elucidate the relationship between tea consumption and incident CHD or changes in CHD-related biomarkers. Second, we considered tea consumption as a lifelong habit, and did not perform a second check to determine status of consumption. Third, the study was carried out in middle-aged and older Chinese who were free of CVD and cancer; therefore our results may not be generalized to populations of all ages, different health conditions, or other ethnicities. Fourth, we did not adjust for multiple testing because the repeated measurements of biomarkers at baseline and follow up were highly correlated in our study. Over adjustment for multiple comparisons may increase the type II error, which reduces the power to detect significant differences. Finally, although a wide range of potential confounding factors were included in our analysis, we could not rule out the possibility of residual and unmeasured confounders.
This study showed that green tea consumption was associated with a reduced risk of CHD incidence, especially among individuals who were male, more than 60 years old, overweight, or suffering from diabetes. Substantial improvement in the changes of lipid profiles, MPV and uric acid might partly explain the potential beneficial effect of green tea on CHD incidence. Our results provided interesting and important evidence that are relevant to the field of CHD prevention. However, these findings need to be verified in future intervention studies with large sample sizes.
Methods
Study population
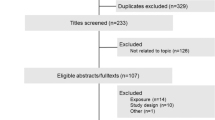
Data was collected from the Dongfeng-Tongji cohort, and the details of the cohort were described in a previous report35. Briefly, a total of 27 009 retired employees of the Dongfeng Motor Corporation (DMC) completed baseline questionnaire, medical examinations and provided fasting blood samples between September 2008 and June 2010. Five years later, the participants were invited to the follow-up survey via telephone. In total, 25978 individuals (96.2% of those at baseline) completed the follow-up until October 2013. At the follow-up investigation, participants repeated the questionnaire interview, physical examinations, and blood collection as those during the baseline survey. Of these 25978 individuals, we excluded participants with cancer, CHD or stroke at baseline (n = 5865), who had missing data on beverage consumption or other covariates (n = 642). Thus, 19 471 participants with a mean age of 62.8 ± 7.7 years were eligible, of which 8585 were males (65.8 ± 6.7 years) and 10 886 were females (60.5 ± 7.7 years). Among them, 2065 new onset CHD cases were documented. Informed consent was obtained from every participant. The protocol was approved by the Ethics Committee of Dongfeng General Hospital, DMC and the Medical Ethics Committee of the School of Public Health, Tongji Medical College, Huazhong University of Science and Technology, and the study was subsequently carried out in accordance with the approved guidelines.
Baseline assessment
Trained interviewers used a structured questionnaire to collect baseline information including socio-demographic characteristics (age, sex, education, and marital status), lifestyle habits such as smoking status (current, former, never), alcohol drinking status (current, former, never), physical activity, occupational history, environmental exposures, and family and medical histories in face-to-face interviews. Beverage consumption was assessed by asking: “Did you usually consume beverages including plain water, black tea, green tea, coffee, cola and juice during the last year?” and participants were asked to select one or two most often consumed beverages. Green tea consumers were defined as participant who selected green tea as one of the most often consumed beverages. Participants who were smoking at least one cigarette per day for more than half a year were defined as current smokers. Those who were drinking alcohol at least one time per week for more than half a year were regarded as current alcohol drinkers36. Physical activity was considered as those who regularly exercised more than 20 min per day for more than 6 months37,38. Physical examination was performed on all participants at DMC-owned hospitals by trained physicians, nurses and technicians. Standing height, body weight and waist circumference were measured in individuals with light indoor clothing and without shoes. Clinical examinations in the liver, gall bladder, spleen, kidney, prostate (for males) and uterus, ovaries and fallopian tubes (for females) were conducted35. Body mass index (BMI) was calculated as weight (kilogram) divided by height (meter) squared. Hypertension was defined as individuals with self-reported physician diagnosis of hypertension, or blood pressure ≥140/90 mmHg, or current use of antihypertensive medication39. Diabetes was defined as self-reported physician diagnosis of diabetes, fasting glucose ≥7.0 mmol/L, or taking oral hypoglycemic medication or insulin40. Hyperlipidemia was defined as total cholesterol >5.72 mmol/L or triglycerides >1.70 mmol/L at medical examination, or a previous physician diagnosis of hyperlipidemia, or taking lipid lowering medication41.
Blood samples were collected after an overnight fast. Total cholesterol, triglycerides, high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), mean platelet volume (MPV), fasting glucose and uric acid were determined at the DMC-owned hospital’s laboratory.
Outcome ascertainment
The outcome of the present study was CHD incidence, including stable angina (SA), unstable angina (UA), non-fatal myocardial infarction (non-fatal MI), unspecified CHD and CHD death, between the baseline survey and October 2013. All retired employees were covered by DMC’s health-care service system and each participant had a unique medical insurance card number and ID, which made it easy to track disease incidence and mortality. CHD was identified through this medical insurance system and medical record reviews in the DMC-owned hospitals. The diagnosis of CHD was made based on well-accepted international standards by cardiologists in the DMC-owned hospitals. SA was defined as angina with no change in frequency, duration, or intensity of symptoms in 6 weeks. UA was defined as angina at rest, accelerated angina or new onset of severe angina. Non-fatal MI was diagnosed based on typical symptoms, ECG change, and cardiac enzyme values42. CHD death was determined by the recorded underlying cause of death on death certificates according to ICD-9: 410–41443 or ICD-10: I20–I2544.
Statistical analysis
Baseline characteristics are presented as percentages for categorical variables and mean ± SD for continuous variables. Categorical data were analyzed with chi-square tests. Continuous variables were analyzed with t-tests. We used Cox’s proportional hazards regression model to evaluate the relation between green tea consumption and CHD incidence without any adjustment and adjusting for covariates including age, sex, BMI, education, smoking status, alcohol drinking status, physical activity, hypertension, hyperlipidemia, diabetes and family history of CHD. To examine whether the effect of green tea on CHD incidence was dependent on consumption of other beverages, we further adjusted for black tea, coffee, cola and juice. Stratified analyses by baseline characteristics were conducted with the same confounding variables being adjusted except for the stratified variable itself. Moreover, to analyze potential interactions between green tea and main characteristics, an interaction product term was included in the model. Difference of CHD-related biomarkers between baseline and follow-up was assessed with paired t-tests. The effects of green tea on 5-year changes of CHD-related biomarkers were analyzed by using general linear model. The covariates described in the Cox model and baseline values of the respective biomarkers were adjusted and additional adjustment for lipid-lowering medications and glucose-lowering medications were conducted in the analysis of the lipid profile and fast blood glucose changes respectively.
All statistical analyses were performed using SAS 9.3 (SAS institute Inc., Cary, NC). Differences were considered significant if the two-tailed p value was less than 0.05.
Additional Information
How to cite this article: Tian, C. et al. Green tea consumption is associated with reduced incident CHD and improved CHD-related biomarkers in the Dongfeng-Tongji cohort. Sci. Rep. 6, 24353; doi: 10.1038/srep24353 (2016).
Change history
31 May 2017
A correction has been published and is appended to both the HTML and PDF versions of this paper. The error has been fixed in the paper.
References
National center for cardiovascular disease, China. Report on cardiovascular diseases in China 2014 11–15 (Encyclopedia of China Publishing House, 2015).
GBD Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 385, 117–171, doi: 10.1016/S0140-6736(14)61682-2 (2015).
Jiang, L., Krumholz, H. M., Li, X., Li, J. & Hu, S. Achieving best outcomes for patients with cardiovascular disease in China by enhancing the quality of medical care and establishing a learning health-care system. Lancet 386, 1493–1505, doi: 10.1016/S0140-6736(15)00343-8 (2015).
Khan, N. & Mukhtar, H. Tea and health: studies in humans. Current pharmaceutical design 19, 6141–6147 (2013).
Khan, N. & Mukhtar, H. Tea polyphenols for health promotion. Life sciences 81, 519–533, doi: 10.1016/j.lfs.2007.06.011 (2007).
Zhang, C. et al. Tea consumption and risk of cardiovascular outcomes and total mortality: a systematic review and meta-analysis of prospective observational studies. Eur J Epidemiol 30, 103–113, doi: 10.1007/s10654-014-9960-x (2015).
Mineharu, Y. et al. Coffee, green tea, black tea and oolong tea consumption and risk of mortality from cardiovascular disease in Japanese men and women. J Epidemiol Community Health 65, 230–240, doi: 10.1136/jech.2009.097311 (2011).
Saito, E. et al. Association of green tea consumption with mortality due to all causes and major causes of death in a Japanese population: the Japan Public Health Center-based Prospective Study (JPHC Study). Ann Epidemiol 25, 512–518.e513, doi: 10.1016/j.annepidem.2015.03.007 (2015).
Suzuki, E. et al. Green tea consumption and mortality among Japanese elderly people: the prospective Shizuoka elderly cohort. Ann Epidemiol 19, 732–739, doi: 10.1016/j.annepidem.2009.06.003 (2009).
Kuriyama, S. et al. Green tea consumption and mortality due to cardiovascular disease, cancer, and all causes in Japan: the Ohsaki study. JAMA 296, 1255–1265, doi: 10.1001/jama.296.10.1255 (2006).
Sano, J. et al. Effects of green tea intake on the development of coronary artery disease. Circ J 68, 665–670 (2004).
Wang, Q. M. et al. Association Between Green Tea Intake and Coronary Artery Disease in a Chinese Population. Circ J 74, 294–300, doi: 10.1253/circj.CJ-09-0543 (2010).
Sasazuki, S. et al. Relation between green tea consumption and the severity of coronary atherosclerosis among Japanese men and women. Ann Epidemiol 10, 401–408 (2000).
Kokubo, Y. et al. The impact of green tea and coffee consumption on the reduced risk of stroke incidence in Japanese population: the Japan public health center-based study cohort. Stroke 44, 1369–1374, doi: 10.1161/STROKEAHA.111.677500 (2013).
Liu, C. Y. et al. Effects of green tea extract on insulin resistance and glucagon-like peptide 1 in patients with type 2 diabetes and lipid abnormalities: a randomized, double-blinded, and placebo-controlled trial. Plos One 9, e91163, doi: 10.1371/journal.pone.0091163 (2014).
Nagao, T., Hase, T. & Tokimitsu, I. A green tea extract high in catechins reduces body fat and cardiovascular risks in humans. Obesity (Silver Spring) 15, 1473–1483, doi: 10.1038/oby.2007.176 (2007).
Suliburska, J. et al. A Effects of green tea supplementation on elements, total antioxidants, lipids, and glucose values in the serum of obese patients. Biol Trace Elem Res 149, 315–322. doi: 10.1007/s12011-012-9448-z. (2012).
Bogdanski, P. et al. Green tea extract reduces blood pressure, inflammatory biomarkers, and oxidative stress and improves parameters associated with insulin resistance in obese, hypertensive patients. Nutr Res 32, 421–427, doi: 10.1016/j.nutres.2012.05.007 (2012).
Hirano, R. et al. Comparison of green tea intake in Japanese patients with and without angiographic coronary artery disease. Am J Cardiol 90, 1150–1153, doi: 10.1016/S0002-9149(02)02787-X (2002).
Pang, J. et al. Association of green tea consumption with risk of coronary heart disease in Chinese population. Int J Cardiol 179, 275–278, doi: 10.1016/j.ijcard.2014.11.093 (2015).
Wu, A. H. et al. Tea and circulating estrogen levels in postmenopausal Chinese women in Singapore. Carcinogenesis 26, 976–980, doi: 10.1093/carcin/bgi028 (2005).
Afzal, M., Safer, A. M. & Menon, M. Green tea polyphenols and their potential role in health and disease. Inflammopharmacology 23, 151–161, doi: 10.1007/s10787-015-0236-1 (2015).
Grant, P. & Ramasamy, S. An update on plant derived anti-androgens. Int J Endocrinol Metab 10, 497–502, doi: 10.5812/ijem.3644 (2012).
Zheng, X. X. et al. Green tea intake lowers fasting serum total and LDL cholesterol in adults: a meta-analysis of 14 randomized controlled trials. Am J Clin Nutr 94, 601–610, doi: 10.3945/ajcn.110.010926 (2011).
Kim, A. et al. Green tea catechins decrease total and low-density lipoprotein cholesterol: a systematic review and meta-analysis. J Am Diet Assoc 111, 1720–1729, doi: 10.1016/j.jada.2011.08.009 (2011).
Colkesen, Y. & Muderrisoglu, H. The role of mean platelet volume in predicting thrombotic events. Clin Chem Lab Med 50, 631–634, doi: 10.1515/CCLM.2011.806 (2012).
Shah, B. et al. Mean platelet volume reproducibility and association with platelet activity and anti-platelet therapy. Platelets 25, 188–192, doi: 10.3109/09537104.2013.793794 (2014).
Henning, B. F., Zidek, W., Linder, B. & Tepel, M. Mean platelet volume and coronary heart disease in hemodialysis patients. Kidney Blood Press Res 25, 103–108, doi: 63516 (2002).
Tavil, Y. et al. Coronary heart disease is associated with mean platelet volume in type 2 diabetic patients. Platelets 21, 368–372, doi: 10.3109/09537101003628421 (2010).
Bhardwaj, P. & Khanna, D. Green tea catechins: defensive role in cardiovascular disorders. Chin J Nat Med 11, 345–353, doi: 10.1016/S1875-5364(13)60051-5 (2013).
Steptoe, A. et al. The effects of chronic tea intake on platelet activation and inflammation: a double-blind placebo controlled trial. Atherosclerosis 193, 277–282, doi: 10.1016/j.atherosclerosis.2006.08.054 (2007).
Wu, A. H., Gladden, J. D., Ahmed, M., Ahmed, A. & Filippatos, G. Relation of serum uric acid to cardiovascular disease. Int J Cardiol, doi: 10.1016/j.ijcard.2015.08.110 (2015).
Jatuworapruk, K. et al. Effects of green tea extract on serum uric acid and urate clearance in healthy individuals. J Clin Rheumatol 20, 310–313, doi: 10.1097/RHU.0000000000000148 (2014).
Panza, V. S. et al. Consumption of green tea favorably affects oxidative stress markers in weight-trained men. Nutrition 24, 433–442, doi: 10.1016/j.nut.2008.01.009 (2008).
Wang, F. et al. Cohort Profile: the Dongfeng-Tongji cohort study of retired workers. Int J Epidemiol 42, 731–740, doi: 10.1093/ije/dys053 (2013).
Grønbaek, M. et al. Changes in alcohol intake and mortality: a longitudinal population-based study. Epidemiology 15, 222–228, doi: 10.1097/01.ede.0000112219.01955.56 (2004).
World health organization. Global Strategy on Diet, Physical Activity and Health. Physical Activity and Adults: Recommended levels of physical activity for adults aged 18–64 years. Available at: http://www.who.int/dietphysicalactivity/factsheet_adults/en/. (Accessed: 6th July 2015).
Okamoto, N., Nakatani, T., Morita, N., Saeki, K. & Kurumatani, N. Home-based walking improves cardiopulmonary function and health-related QOL in community-dwelling adults. Int J Sports Med 28, 1040–1045, doi: 10.1055/s-2007-965073 (2007).
Meng, L., Chen, D., Yang, Y., Zheng, Y. & Hui, R. Depression increases the risk of hypertension incidence: a meta-analysis of prospective cohort studies. J Hypertens 30, 842–851, doi: 10.1097/HJH.0b013e32835080b7 (2012).
Lam, K. B. et al. Napping is associated with increased risk of type 2 diabetes: the Guangzhou Biobank Cohort Study. Sleep 33, 402–407 (2010).
Feng, W. et al. Urinary metals and heart rate variability: a cross-sectional study of urban adults in Wuhan, China. Environ Health Perspect 123, 217–222, doi: 10.1289/ehp.1307563 (2015).
Cannon, C. P. et al. American College of Cardiology key data elements and definitions for measuring the clinical management and outcomes of patients with acute coronary syndromes. A report of the American College of Cardiology Task Force on Clinical Data Standards (Acute Coronary Syndromes Writing Committee). J Am Coll Cardiol 38, 2114–2130, doi: 10.1016/S0735-1097(01)01702-8 (2001).
World Health Organization (WHO). International classification of diseases (9th ed.) (Geneva, 1977).
World health organization. International Statistical Classification of Diseases and Related Health Problems 10th Revision (ICD-10)-2014-WHO Version for 2014. Chapter IX Diseases of the circulatory system(I00-I99) Ischaemic heart diseases (I20-I25). Available at: http://apps.who.int/classifications/icd10/browse/2014/en#/I20-I25 (Accessed: 18th February 2014).
Acknowledgements
Great thanks go to all the participants for their continuously high level of cooperation and to all group members for their outstanding efforts in conducting the survey at baseline and the follow-up. The work was supported by the National Natural Science Foundation of China (81373093, 81230069, and 81390542), 111 Project (No. B12004); the Program for Changjiang Scholars and Innovative Research Team in University of Ministry of Education of China (No. IRT1246); China Medical Board (No. 12–113); the Fundamental Research Funds for the Central Universities (2015QN096).
Author information
Authors and Affiliations
Contributions
X.M.Z. and T.C.W. designed the research; H.D.Y., X.L.L., X.W.M., C.Z., C.W.X., J.Y., X.P.M., M.A.H., T.C.W. and X.M.Z. conducted the research; C.T., Q.H., L.L.Y., S.L., F.A. and X.M.Z. analyzed or interpreted the data; C.T., Q.H. and X.M.Z. wrote the article; S.L. and F.A. contributed to providing critical revision of the manuscript; all authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Tian, C., Huang, Q., Yang, L. et al. Green tea consumption is associated with reduced incident CHD and improved CHD-related biomarkers in the Dongfeng-Tongji cohort. Sci Rep 6, 24353 (2016). https://doi.org/10.1038/srep24353
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep24353
This article is cited by
-
Impact of Tobacco Smoking on Health Care Utilization and Medical Costs in Chronic Obstructive Pulmonary Disease, Coronary Heart Disease and Diabetes
Current Medical Science (2022)
-
Effect of Physical Activity on Hospital Service Use and Expenditures of Patients with Coronary Heart Disease: Results from Dongfeng-Tongji Cohort Study in China
Current Medical Science (2019)
-
Effects of green tea extract on overweight and obese women with high levels of low density-lipoprotein-cholesterol (LDL-C): a randomised, double-blind, and cross-over placebo-controlled clinical trial
BMC Complementary and Alternative Medicine (2018)
-
Is tea consumption associated with the serum uric acid level, hyperuricemia or the risk of gout? A systematic review and meta-analysis
BMC Musculoskeletal Disorders (2017)
-
Plant-based foods containing cell wall polysaccharides rich in specific active monosaccharides protect against myocardial injury in rat myocardial infarction models
Scientific Reports (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.