Abstract
Oral infectious diseases are epidemiologically associated with stroke. We previously showed that oral Streptococcus mutans with the cnm gene encoding a collagen-binding Cnm protein induced intracerebral hemorrhage (ICH) experimentally and was also associated with cerebral microbleeds (CMBs) in our population-based cohort study. We therefore investigated the roles of cnm-positive Streptococcus mutans in this single hospital-based, observational study that enrolled 100 acute stroke subjects. The cnm gene in Streptococcus mutans isolated from saliva was screened using PCR techniques and its collagen-binding activities examined. CMBs were evaluated on T2* gradient-recalled echo MRI. One subject withdrew informed consent and 99 subjects (63 males) were analyzed, consisting of 67 subjects with ischemic stroke, 5 with transient ischemic attack and 27 with ICH. Eleven cases showed Streptococcus mutans strains positive for cnm. The presence of cnm-positive Streptococcus mutans was significantly associated with ICH [OR vs. ischemic stroke, 4.5; 95% CI, 1.17–19.1] and increased number of deep CMBs [median (IQR), 3 (2–9) vs. 0 (0–1), p = 0.0002]. In subjects positive for Streptococcus mutans, collagen binding activity was positively correlated with the number of deep CMBs (R2 = 0.405; p < 0.0001). These results provide further evidence for the key role of oral health in stroke.
Similar content being viewed by others
Introduction
Small vessel diseases (SVDs) of the brain (e.g. cerebral microbleeds (CMBs), lacunar infarcts and white matter lesions) are important biomarkers of vascular injury and burden of brain dysfunction. The underlying mechanisms and risk factors of the SVDs of the brain are poorly understood. CMBs are small round hypo-intense on T2* weighted gradient-recalled echo MRI sequence1, histologically corresponding with focal leakage of hemosiderin from abnormal small vessels2. Deep CMBs located in the caudate head, lentiform nucleus, internal/external capsules and thalamus are related to hypertensive angiopathy in perforating arterioles, arteriosclerosis and lipohyalinosis3. Deep CMBs are strongly associated with the presence of hypertensive intracerebral hemorrhage (ICH) in the same distribution4 and are common in recurrent lacunar stroke5, supporting the notion that CMBs are markers of cerebral microangiopathy6. Risk factors of deep CMBs are long-standing hypertension5, advanced age, male sex7 and chronic kidney disease8; however, deep CMBs may be found in subjects who have no apparent risk factors9.
Our recent population-based study showed a strong correlation of CMBs with cnm gene positive Streptococcus mutans (cnm-positive S. mutans) in the oral cavity10. The adjusted odds ratio for CMBs in the cnm-positive S. mutans group was 14.410. Consistent with this, Nakano et al. found that the cnm-positive S. mutans contributes to the development of intracerebral hemorrhage by expressing a collagen-binding protein (CBP) that the cnm gene encodes on the bacterial surface which disrupts the blood-brain barrier11 (BBB). This is in line with the fact that periodontal and other infections have been shown to be risk factors for stroke12,13. S. mutans is a major pathogen of dental caries and causes bacteremia by dental procedures in daily life14. Cell-surface CBP of S. mutans mediates its invasion of endothelial cells in vitro15 and the resultant endothelial failure may underlie CMBs16,17.
In this hospital cohort study, we aimed to confirm the potential roles of cnm-positive S. mutans in development of CMBs and ICH in patients with acute cerebrovascular disease and to explore underlying mechanisms by which this specific pathogen of dental caries directly influences the pathogenesis of SVDs.
Results
Background difference between those positive and negative for cnm-positive S. mutans
One patient withdrew informed consent and 99 subjects (age 70.1 ± 12.9 years old, 63 male) were subsequently analyzed. S. mutans was detected in 51 subjects (52%). Eleven of the 51 subjects (22%) showed positivity for the cnm gene. No significant differences were found between those positive for cnm-positive S. mutans and those negative for cnm-positive S. mutans in the past medical history of cardiovascular diseases or frequency of vascular risk factors. In terms of results of laboratory blood testing, cnm-positive S. mutans was significantly associated with higher CRP [0.2 mg/dl (0.1–0.5) vs. 0.1 mg/dl (0–0.2); p = 0.04] and fibrinogen value [361 mg/dl (336–459) vs. 320 mg/dl (274–365); p = 0.01] (Table 1). There were 67 subjects with ischemic stroke (IS), 27 with ICH and 5 with transient ischemic attack (TIA). The 67 subjects with IS consisted of 25 subjects with lacunar stroke (small vessel occlusion), 15 subjects with atherothrombotic stroke (large artery atherosclerosis), 16 subjects with cardiogenic stroke and 11 other known or unknown etiologies. The 27 subjects with ICH consisted of 23 subjects with hypertensive ICH and 4 subjects with probable cerebral amyloid angiopathy (CAA) (Table 1).
Difference in stroke subtypes between those positive and negative for cnm-positive S.mutans
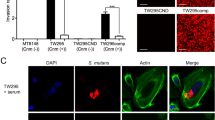
Six of the 27 subjects with ICH and 4 of the 67 subjects with IS were positive for cnm-positive S. mutans [odds ratio (OR), ICH vs. IS, 4.5; 95% confidence interval (CI), 1.17–19.1]. The frequency of cnm-positive S. mutans was greater in those with hypertensive ICH (26%) than those with other stroke types (6%) (Fig. 1a). When analyzed only among subjects with IS, the frequency of cnm-positive S. mutans was the greatest in those with lacunar stroke (12%) (Fig. 1a). No subjects with probable CAA were found to harbor cnm-positive S. mutans. The OR for hypertensive ICH by cnm-positive S. mutans was 5.56 [95% confidence interval (CI), 1.43–23.9], while it was 7.51 [95% CI, 1.75–37.2] when adjusted for age and sex (model 1) and 7.10 [95%CI, 1.50–39.5] when adjusted for age, sex, mean blood pressure and creatinine clearance (model 2) (Fig. 1b).
Association of cnm-positive S. mutans with ICH.
(a) cnm-positive S. mutans was detected in 26% of hypertensive intracerebral hemorrhage and 12% of lacunar stroke but in only 6% of cardioembolic stroke and none of atherosclerotic stroke. The odds ratio of cnm-positive S. mutans in hypertensive ICH versus the other stroke subtypes was 5.56. (b) cnm-positive S. mutans was associated with hypertensive ICH before and after adjusted for established risk factors for ICH, such as age, sex, mean blood pressure and creatinine clearance. Error bars show 95% confidence interval. ICH indicates intracerebral hemorrhage; S. mutans, Streptococcus mutans.
Deep CMBs were significantly greater in subjects with cnm-positive S. mutans
We investigated whether cnm-positive S. mutans is associated with CMBs that are known to be one of the characteristic features of SVDs and often underlie ICH. In 95 subjects whose MRI were available (4 subjects contraindicated due to their pacemakers), CMBs were found in 53 (56%) which comprised of 9 of the 11 subjects with cnm-positive S. mutans (81%) and 44 of the other 84 subjects (52%), with a marginal intergroup difference (p = 0.06). Total number of CMBs was significantly higher in subjects with cnm-positive S. mutans compared to those without (median (IQR), 8 (3–13) vs. 0.5 (0–4); p = 0.002) (Fig. 2a). The relative ratio for total CMBs with cnm-positive S. mutans compared to those without was 1.93 [95% CI, 1.06–3.88]. In terms of their locations, the number of deep CMBs was significantly higher in subjects with cnm-positive S. mutans compared to those without (3 (2–9) vs. 0 (0–1); p = 0.0002) (Fig. 2b). The relative ratio for number of deep CMBs with cnm-positive S. mutans compared to those without was 2.2 [95% CI, 1.1–4.7], while it was 2.3 [95% CI, 1.1–5.1] when adjusted by the model 1 and 2.3 [95% CI, 1.1–5.3] when adjusted by the model 2 (Fig. 2c). Such a significant difference was also seen among the ICH subjects depending on the presence or absence of cnm-positive S. mutans (8 (2.8–9.0) vs. 2 (0–8); p = 0.0037) (Fig. 2d). In contrast, the score of the lobar and infratentorial CMBs were not significantly different between the two groups (lobar CMBs, 0 (0–4) vs. 1 (0–1); p = 0.43; infratentorial CMBs, 0 (0–3) vs. 0 (0–0.8); p = 0.60). When the number of total or deep CMBs was categorized into 0 (none), 1 or 2 (few) and ≥ 3 (multiple) groups, there were significant differences in the positive rate of cnm–positive S. mutans among the three groups (p < 0.01 for total CMBs; p < 0.001 for deep CMBs): the group with multiple CMBs showed significantly greater rate of cnm–positive S. mutans (Table 1).
Association of cnm-positive S. mutans with CMBs.
(a,b) In total subjects with acute cerebrovascular disease (n = 99), the numbers of CMBs (a) and deep CMBs (b) were significantly greater in subjects with cnm-positive S. mutans than those without. (c) cnm-positive S. mutans was associated with deep CMBs before and after adjusted for established risk factors for ICH, such as age, sex, mean blood pressure and creatinine clearance. (d) Among subjects with hypertensive ICH (n = 23), the number of deep CMBs was significantly higher in subjects with cnm-positive S. mutans than those without. Error bars show 95% confidence interval. S. mutans indicates Streptococcus mutans; CMBs, cerebral microbleeds; ICH, intracerebral hemorrhage. *p < 0.01, **p < 0.001.
Collagen binding activity of cnm-positive S. mutans are correlates with number of deep cerebral microbleeds
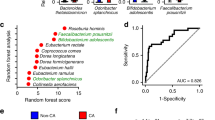
The collagen-binding activity was measured for the 12 strains of S. mutans from 11 subjects who were positive for cnm. The collagen-binding activity of cnm-negative S. mutans retrieved from subjects with deep CMBs was also measured, which were not detectable in most of cases, as reported in other studies. Collagen binding activity was correlated with numbers of deep CMBs (γ = 0.054; R2 = 0.405; p < 0.0001) (Fig. 3) after one extreme outlier was identified by jackknife test and excluded from the analysis because the number of deep CMBs was more than median plus 5SD.
Correlation between collagen binding activity of S. mutans and number of deep CMBs.
The collagen-binding activity of S. mutans significantly correlated with the number of deep CMBs (n = 50, γ = 0.054, P < 0.0001, R2 = 0.405) after one extreme outlier was excluded by using jackknife technique. S. mutans, Streptococcus mutans; CMBs, cerebral microbleeds.
Short case report of recurrent ICH with cnm-positive S. mutans
A 57-year-old woman with left putaminal hemorrhage was found to have cnm-positive S. mutans and had a recurrent hemorrhage in the right putamen within a one-year interval despite good control of hypertension with medications and absence of other apparent risk factors, such as hyperlipidemia, diabetes mellitus, smoking or alcohol abuse. The location of the recurrent hemorrhage corresponded to the location of CMBs that had been detected in the previous T2* gradient-recalled echo (GRE) MRI on the first admission and the number of deep CMBs increased on the second admission (Fig. 4). The isolation rate of cnm-positive S. mutans strains in the five cultured plates was increased (first vs. second admission; 1/5 vs. 5/5). The collagen binging activities of cnm-positive S. mutans were 76% and 111% in the first and second isolation, respectively. These findings suggest a poor prognosis, or a higher tendency for recurrent bleeding in subjects with cnm-positive S. mutans strains.
Discussion
This study conducted in our acute stroke cohort showed a significant correlation of cnm-positive S. mutans with hypertensive ICH and deep CMBs, two of the major hemorrhagic phenotypes of arteriolosclerosis in the perforating arteries. Other forms of SVDs, including white matter hyperintensity, lobar CMBs and lacunar infarctions, did not show associations with cnm-positive S. mutans. In addition, the relatively increased positivity of cnm-positive S. mutans in subjects with lacunar infarction (small vessel occlusion) compared to other IS subtypes (Fig. 1) further suggests the linkage between cnm-positivity and small vessel changes. The elevated levels of two inflammatory markers, CRP and fibrinogen, in subjects with cnm-positive S. mutans suggest that inflammation can be derived from the cnm-positive S. mutans infection, as the bacteria latently found in the dental caries can cause daily bacteremia14. The correlation of the collagen-binding activity with the number of deep CMBs suggests a pathogenic role for CBP expressed on the cell surface of S. mutans strains in the development of hemorrhagic phenotype of SVD. Although both inflammation and endothelial damage are thought to contribute to small vessel disease16, little is known about specific mechanism underlying CMBs17. Therefore, infection with cnm-positive S. mutans may explain the causation of inflammation and endothelial damage as underlying etiologies of CMBs.
Our study shows a possible mechanism by which cnm-positive S. mutans induces hemorrhagic changes in perforating arterioles. The permeability of the BBB is known to increase with age18 as a result of loss of endothelial integrity. Long-standing hypertension further affects the structure of small vessels leading not only to BBB disruption but also to accumulation of type I collagen19. Dental caries results in the destruction of enamel on the tooth surface enabling cnm-positive S.mutans access to bloodstream20,21. Age and hypertension related vascular changes in cerebral small vessel disease may release vascular factors that attract concentration dependent collagen binding factors22, including those of cnm-positive S. mutans. Once cnm-positive S. mutans attach to the exposed collagen of perforating arterioles, infiltration of neutrophils may aggravate local inflammation, resulting in increasing permeability of the BBB23 and higher delivery of enzymes, such as myeloperoxidase16, to accelerate endothelial damage. Furthermore, the negative charges of the bacterial surface proteoglycans may prevent negatively charged platelets from interacting with collagen11,24, which will impair primary hemostasis resulting in prolongation of focal hemorrhage. There is an emerging concept of the brain-gut axis. The brain-gut axis and its association with several disorders including cardiovascular disease25 and neurodegenerative disorders26 has been considered mainly in regard to the flora in the stomach and lower intestine. Since S. mutans is a major pathogen of oral caries, our data provides a new concept of brain-oral association. Future experimental work should focus on determining how oral infectious pathogens induce or aggravate CMBs and CAA. Furthermore, S. mutans with CBP has some mechanistic implications in other systemic disorders including infective endocarditis15, ulcerative colitis27 and IgA nephropathy28. The strong correlation between highly virulent S. mutans and systemic disease including CMBs/ICH may provide a new breakthrough for future prevention and intervention.
Some limitations should be addressed. First, the isolation rate of S. mutans strains was lower than that from normal volunteers. This may be associated with better oral hygiene after the oral care the stroke subjects received in the acute phase or with oral drying because of the comorbidities of stroke prior to sampling of oral plaque in this study. Alternatively, the lesser number of teeth in the aged stroke subjects may have affected the lower isolation rate of S. mutans strains because S. mutans only resides in hard tissue, such as tooth. It should be determined whether stroke subjects have lower isolation rates of S. mutans with thorough screening tests in consideration of future prevention strategy of cerebral hemorrhagic disorders. Second, MRI images were taken with 1.5-tesla and 3-tesla MR scanners interchangeably because of the issue of day and night availability of MR scanners in the acute settings. However, the ratio of usage of 3-tesla MRI images was not different between cnm-positive and -negative subjects, minimizing the possibility that the resolution of MRI images affected the results. The third limitation was that this cross-sectional study did not determine the exact interval between infection of cnm-positive S. mutans and appearance of CMBs. Finally, this study enrolled a relatively small number of stroke patients from single ethnic group. This study should therefore be viewed as hypothesis generating although the data certainly merits further study to investigate the difference in frequency of cnm-positive S. mutans and the impact of the oral bacteria on pathogenesis of stroke in different ethnic groups.
In summary, Cnm proteins of S. mutans may be associated with development of deep CMBs and ICH with a mechanistic link to chronic inflammation.
Materials and Methods
Participants
One hundred subjects admitted to the National Cerebral and Cardiovascular Center (NCVC) because of acute IS, TIA and ICH between February and August 2014 were enrolled. All subjects underwent neurological examination by National Institute of Health Stroke Scale (NIHSS) score and modified Rankin scale pre-admission, at discharge and 3 months after discharge. Those with disturbances of consciousness were not enrolled because of difficulty of oral sampling. IS was classified using the trial of Org 10172 in Acute Stroke Treatment (TOAST) classification29, ICH was classified by the structural vascular lesion; medication; CAA; systemic disease; hypertension; undetermined (SMASH-UICH) classification30 and TIA was defined as related syndrome of stroke symptoms that resolve completely within 24 hours. The diagnosis of probable CAA was established by the modified Boston criteria31. As traditional vascular risk factors, we recorded hypertension, diabetes, dyslipidemia, atrial fibrillation (all medically diagnosed and/or on relevant drugs), ever smoker and drinking (interview on admission). We collected past medical history of IS, ICH and ischemic heart disease in clinical records. Laboratory tests included complete blood counts, metabolite profile and blood coagulation.
Sample collection
Oral saliva and dental plaque specimens were collected from the subjects in the first 3 days following admission.
Culture condition of Streptococcus mutans
Oral samples were inoculated on Mitis-Salivarius medium with bacitracin (MSB, 100 U/ml; Sigma-Aldrich, St. Louis, MO, USA) and 15% sucrose (MSB agar) and anaerobically incubated at 37 centigrade for 48 hours. Streptococcus mutans strains were isolated morphologically and all strains were anaerobically grown in brain heart infusion (BHI) broth (Difco Laboratories, Detroit, MI, USA) at 37 centigrade for 24 hours.
cnm gene positivity and collagen binding assay
After cultured in BHI broth, DNA of each strain was extracted. S.mutans and cnm gene encoding CBP was screened using polymerase chain reaction techniques. MKD primer32 was used to detect S.mutans and cnm primer was used to identify cmm gene33. A collagen-binding assay with type I collagen was conducted to examine collagen-binding activities of each isolated S. mutans strain according to the method described by Waterhouse and Russell34, with some modifications32. The activities was evaluated under fixed conditions of 1 mg of type I collagen and 1 ×1010 bacterial cells. The activities for each strain are expressed as a percentage compared with the positive control S. mutans TW871 which has known binding activity to type I collagen32 as 100%. These experiments were conducted by a researcher (R.N.) who was blinded to clinical information.
Imaging acquisition
Magnetic resonance imaging (MRI) was performed either with 1.5 Tesla (Magnetom Sonata or Vision; Siemens Medical Solutions, Erlangen, Germany) or 3.0 Tesla (Magnetom Verio or Spectra; Siemens Medical Solutions, Erlangen, Germany) scanners. A standardized protocol was employed for all time points that included DWI and apparent diffusion coefficient (ADC), fluid attenuated inversion recovery (FLAIR) and T2* GRE.
Imaging analysis
The number and location of CMBs and severity of white matter lesions were analyzed. Cerebral microbleeds were evaluated on T2* GRE MRI and were defined according to the published criteria1. The locations of CMBs were categorized into lobar (cortical gray or subcortical white matter), deep (deep gray matter in the basal ganglia and thalamus; or white matter in the corpus callosum, internal, external and extreme capsule) and infratentorial (cerebellum and brainstem) regions. The number and location of CMBs were rated by one neurologist (S.T.) and independently by another neurologist (Y.O.). Inter-rater correlation coefficients were 0.97 for deep, 0.97 for lobar and 0.90 for infratentorial CMBs.
Ethics regarding human subjects
All subjects or their family members provided written informed consent and the study was approved by the Institutional Ethical Committee of the National Cerebral and Cardiovascular Center. The methods were carried out in accordance with the Ethical Guidelines for Medical and Health Research Involving Human Subjects.
Statistical analyses
For statistical analyses, JMP 11 software (SAS Institute Inc., Cary, NC) was used. Differences in dichotomous variables were analyzed using Chi-square test. Wilcoxon signed rank test was used to analyze differences in the median of continuous variables between groups. Multivariable models were generated to determine the contribution of cnm-positive S. mutans to hypertensive ICH and number of deep CMBs after adjusting for known risk factors (age, sex, mean blood pressure and creatinine clearance). To further determine the association between cnm-positive S. mutans and CMBs, patients were categorized into three groups according to the number of total or deep CMBs; 0 (none), 1 or 2 (few) and ≥3 (multiple) groups and intergroup differences were assessed with Pearson’s chi-square test. To assess the relationship between collagen binding activity of S. mutans and deep CMBs, correlation analysis was used after the jackknife test was applied to exclude outliers. Statistical significance level was set at 0.05 for all analyses. Subjects without cnm-negative S. mutans included both those positive for cnm-negative S. mutans and those negative for S. mutans.
Additional Information
How to cite this article: Tonomura, S. et al. Intracerebral hemorrhage and deep microbleeds associated with cnm-positive Streptococcus mutans; a hospital cohort study. Sci. Rep. 6, 20074; doi: 10.1038/srep20074 (2016).
References
Greenberg, S. M. et al. Cerebral microbleeds: a guide to detection and interpretation. Lancet Neurol 8, 165–174 (2009).
Tanaka, A., Ueno, Y., Nakayama, Y., Takano, K. & Takebayashi, S. Small chronic hemorrhages and ischemic lesions in association with spontaneous intracerebral hematomas. Stroke 30, 1637–1642 (1999).
Tatsumi, S., Shinohara, M. & Yamamoto, T. Direct comparison of histology of microbleeds with postmortem MR images: a case report. Cerebrovasc Dis 26, 142–146 (2008).
Lee, S. H., Kwon, S. J., Kim, K. S., Yoon, B. W. & Roh, J. K. Cerebral microbleeds in patients with hypertensive stroke. Topographical distribution in the supratentorial area. J Neurol 251, 1183–1189 (2004).
Cordonnier, C., Al-Shahi Salman, R. & Wardlaw, J. Spontaneous brain microbleeds: systematic review, subgroup analyses and standards for study design and reporting. Brain 130, 1988–2003 (2007).
Greenberg, S. M., Eng, J. A., Ning, M., Smith, E. E. & Rosand, J. Hemorrhage burden predicts recurrent intracerebral hemorrhage after lobar hemorrhage. Stroke 35, 1415–1420 (2004).
Jeerakathil, T. et al. Cerebral microbleeds - Prevalence and associations with cardiovascular risk factors in the Framingham Study. Stroke 35, 1831–1835 (2004).
Ovbiagele, B. et al. Association of Chronic Kidney Disease With Cerebral Microbleeds in Patients With Primary Intracerebral Hemorrhage. Stroke 44, 2409–2413 (2013).
van Dijk, E. J., Prins, N. D., Vrooman, H. A., Hofman, A., Koudstaal, P. J. & Breteler, M. M. B. Progression of cerebral small vessel disease in relation to risk factors and cognitive consequences - Rotterdam Scan Study. Stroke 39, 2712–2719 (2008).
Miyatani, F. et al. Relationship between Cnm-positive Streptococcus mutans and cerebral microbleeds in humans. Oral Dis 21(7), 886–893 (2015).
Nakano, K. et al. The collagen-binding protein of Streptococcus mutans is involved in haemorrhagic stroke. Nat Commun 2, 485 (2011).
Lee, Y. L., Hu, H. Y., Huang, N., Hwang, D. K., Chou, P. & Chu, D. C. Dental Prophylaxis and Periodontal Treatment Are Protective Factors to Ischemic Stroke. Stroke 44, 1026–1030 (2013).
Desvarieux, M., Demmer, R. T., Jacobs, D. R., Papapanou, P. N., Sacco, R. L. & Rundek, T. Changes in Clinical and Microbiological Periodontal Profiles Relate to Progression of Carotid Intima-Media Thickness: The Oral Infections and Vascular Disease Epidemiology Study. J Am Heart Assoc 2, e000254 (2013).
Lockhart, P. B., Brennan, M. T., Sasser, H. C., Fox, P. C., Paster, B. J. & Bahrani-Mougeot, F. K. Bacteremia associated with toothbrushing and dental extraction. Circulation 117, 3118–3125 (2008).
Abranches, J., Miller, J. H., Martinez, A. R., Simpson-Haidaris, P. J., Burne, R. A. & Lemos, J. A. The collagen-binding protein Cnm is required for Streptococcus mutans adherence to and intracellular invasion of human coronary artery endothelial cells. Infect Immun 79, 2277–2284 (2011).
Shoamanesh, A. et al. Inflammatory biomarkers, cerebral microbleeds and small vessel disease: Framingham Heart Study. Neurology 84, 825–832 (2015).
Wardlaw, J. M., Smith, C. & Dichgans, M. Mechanisms of sporadic cerebral small vessel disease: insights from neuroimaging. Lancet Neurol 12, 483–497 (2013).
Farrall, A. J. & Wardlaw, J. M. Blood-brain barrier: Aging and microvascular disease-systematic review and meta-analysis. Neurobiol Aging 30, 337–352 (2009).
Intengan, H. D. & Schiffrin, E. L. Structure and mechanical properties of resistance arteries in hypertension - Role of adhesion molecules and extracellular matrix determinants. Hypertension 36, 312–318 (2000).
Selwitz, R., Ismail, A. & Pitts, N. Dental caries. Lancet 369, 51–59 (2007)
Switalski, L. M., Butcher, W. G., Caufield, P. C. & Lantz, M. S. Collagen mediates adhesion of Streptococcus mutans to human dentin. Infect Immun 61, 4119–4125 (1993).
Giwa, M. O. et al. Neuropathologic evidence of endothelial changes in cerebral small vessel disease. Neurology 78, 167–174 (2012).
Abbott, N. J. Inflammatory mediators and modulation of blood-brain barrier permeability. Cell Mol Neurobiol 20, 131–147 (2000).
Paderi, J. E., Stuart, K., Sturek, M., Park, K. & Panitch, A. The inhibition of platelet adhesion and activation on collagen during balloon angioplasty by collagen-binding peptidoglycans. Biomaterials 32, 2516–2523 (2011).
Wang, Z. et al. Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature 472, 57–82 (2011).
Friedland, R. P. Mechanisms of molecular mimicry involving the microbiota in neurodegeneration. J Alzheimers Dis 45, 349–362 (2015).
Kojima, A. et al. Infection of specific strains of Streptococcus mutans, oral bacteria, confers a risk of ulcerative colitis. Sci Rep 2, 332 (2012).
Misaki, T. et al. Distribution of Streptococcus mutans strains with collagen-binding proteins in the oral cavity of IgA nephropathy patients. Clin Exp Nephrol 19, 844–850 (2015).
Adams, H. P. et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24, 35–41 (1993).
Meretoja, A. et al. SMASH-U: a proposal for etiologic classification of intracerebral hemorrhage. Stroke 43, 2592–2597 (2012).
Linn, J. et al. Prevalence of superficial siderosis in patients with cerebral amyloid angiopathy. Neurology 74, 1346–1350 (2010).
Nomura, R. et al. Molecular and clinical analyses of the gene encoding the collagen-binding adhesin of Streptococcus mutans. J Med Microbiol 58, 469–475 (2009).
Sato, Y., Okamoto, K., Kagami, A., Yamamoto, Y., Igarashi, T. & Kizaki, H. Streptococcus mutans strains harboring collagen-binding adhesin. J Dent Res 83, 534–539 (2004).
Waterhouse, J. C. & Russell, R. R. B. Dispensable genes and foreign DNA in Streptococcus mutans. Microbiology 152, 1777–1788 (2006).
Acknowledgements
This study was partially supported by grants from Mitsui Sumitomo Insurance Welfare Foundation (M.I.) and SENSHIN Medical Research Foundation (M.I.).
Author information
Authors and Affiliations
Contributions
S.T., M.I., T.K. and Y.O. participated in patient recruitment and sample collections. M.I., R.F., N.K., Y.W. and K.N. designed the study. S.T., T.T. and S.S. performed the MR evaluations and statistical analyses. S.T. and R.N. performed the laboratory experiments. S.T. and M.I. drafted the manuscript. K.T. and K.N. interpreted the data and made substantive comments on the study.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Tonomura, S., Ihara, M., Kawano, T. et al. Intracerebral hemorrhage and deep microbleeds associated with cnm-positive Streptococcus mutans; a hospital cohort study. Sci Rep 6, 20074 (2016). https://doi.org/10.1038/srep20074
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep20074
This article is cited by
-
Porphyromonas gingivalis infection in the oral cavity is associated with elevated galactose-deficient IgA1 and increased nephritis severity in IgA nephropathy
Clinical and Experimental Nephrology (2024)
-
Association between gingival bleeding and hematuria as biomarkers of periodontitis and renal disease: a review
Odontology (2024)
-
Antimicrobial photodynamic therapy with Ligularia fischeri against methicillin-resistant Staphylococcus aureus infection in Caenorhabditis elegans model
Applied Biological Chemistry (2023)
-
The interaction between the nervous system and the stomatognathic system: from development to diseases
International Journal of Oral Science (2023)
-
Evaluation of the collagen-binding properties and virulence of killed Streptococcus mutans in a silkworm model
Scientific Reports (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.