Abstract
High-fat diet (HFD) triggers insulin resistance and diabetes mellitus, but their link remains unclear. Characterization of overt hyperglycemia in insulin receptor mutant (InsrP1195L/+) mice exposed to HFD (InsrP1195L/+/HFD mice) revealed increased glucose-6-phosphatase (G6pc) expression in liver and increased gluconeogenesis from glycerol. Lipolysis in white adipose tissues (WAT) and lipolysis-induced blood glucose rise were increased in InsrP1195L/+/HFD mice, while wild-type WAT transplantation ameliorated the hyperglycemia and the increased G6pc expression. We found that the expressions of genes involved in bile acid (BA) metabolism were altered in InsrP1195L/+/HFD liver. Among these, the expression of Cyp7a1, a BA synthesis enzyme, was insulin-dependent and was markedly decreased in InsrP1195L/+/HFD liver. Reduced Cyp7a1 expression in InsrP1195L/+/HFD liver was rescued by WAT transplantation and the expression of Cyp7a1 was suppressed by glycerol administration in wild-type liver. These findings suggest that unsuppressed lipolysis in adipocytes elicited by HFD feeding is linked with enhanced gluconeogenesis from glycerol and with alterations in BA physiology in InsrP1195L/+/HFD liver.
Similar content being viewed by others
Introduction
The rapid increase in the prevalence of type 2 diabetes mellitus (T2DM) worldwide can be attributed to changes in environmental factors including less physical activity and over-nutrition. Excessive fat intake is known to promote onset of T2DM in genetically susceptible humans and rodents1. However, there are few animal models that exhibit normal glucose tolerance under normal diet but develop overt hyperglycemia in response to high-fat diet (HFD)2. Partly for this reason, the pathophysiology of HFD-induced diabetes mellitus has not been fully elucidated. T2DM is a metabolic disorder characterized by a chronic rise in blood glucose levels, principally due to insufficient insulin secretion and/or action. Insulin resistance is a pathogenic component of the disease and can be induced both genetically and environmentally3. Genetic mutation or disruption of the insulin receptor (Insr) has been shown to cause insulin resistance and T2DM in both humans and mice3,4. In mice, whole body, homozygous deletion of the Insr gene results in neonatal lethality, which hinders studies on the pathophysiological relevance of the insulin receptor. As the insulin receptor is expressed in all cell types and insulin signaling mediates diverse cellular functions, the detailed insulin function of each tissue has been extensively studied using tissue-specific Insr knockout mice3,5, in which Insr expression is almost completely disrupted in a specific cell type.
A number of studies have shown that the various insulin signaling pathways affected by insulin resistance are not homogeneously affected3. Kahn et al. categorized such pathways into those remaining ‘insulin sensitive’ and those becoming ‘insulin resistant’, according to their relevance in Metabolic Syndrome. The concept of ‘selective insulin resistance’ is therefore critical for understanding the complex pathophysiology of T2DM, in which the insulin resistant state prevails in many tissues, but in a tissue-dependent, pathway-specific manner. Nevertheless, it has not been fully clarified which pathways contribute crucially to the development of T2DM.
In the present study, we examined changes in glucose metabolism in a mouse systemically harboring a loss of function mutation in Insr (a single amino acid substitution from proline to leucine at 1195 amino acid residue (P1195L)), which has been shown to act as a dominant-negative mutant in heterozygosity6. Heterozygous mutant (InsrP1195L/+) mice exhibit marked insulin resistance but avoid glucose intolerance even by glucose loading test6. Since this heterozygous mutation in Insr alone was insufficient to induce defective glucose homeostasis, we challenged the mice with HFD. Interestingly, InsrP1195L/+ mice were extremely susceptible to overt hyperglycemia by HFD. The mechanism of HFD-induced hyperglycemia was therefore investigated in InsrP1195L/+ mice.
Our findings reveal a concerted mechanism linking exacerbated lipolysis in WAT and increased gluconeogenesis from glycerol in liver of InsrP1195L/+/HFD mice, ultimately leading to the development of overt hyperglycemia. We also identified alterations in bile acid (BA) physiology in the liver of InsrP1195L/+/HFD mice.
Results
HFD feeding induces overt hyperglycemia and prevents body weight gain in InsrP1195L/+ mice
The blood glucose levels of InsrP1195L/+ mice under normal diet (ND) (InsrP1195L/+/ND mice) were not different from those of wild-type (WT) mice; however, InsrP1195L/+ mice under HFD (InsrP1195L/+/HFD mice) developed hyperglycemia (Fig. 1a). The expected increase in body weight of InsrP1195L/+/HFD mice was significantly blunted (Fig. 1b). Glucose intolerance in InsrP1195L/+/HFD mice was confirmed by oral glucose tolerance test (OGTT) (Fig. 1c). In addition, the glucose lowering effect of insulin was severely impaired in InsrP1195L/+/HFD mice, as assessed by insulin tolerance test (ITT) (Fig. 1d).
InsrP1195L/+/HFD mice exhibit glucose intolerance, insulin resistance and increased gluconeogenesis from glycerol.
(a) Blood glucose levels of InsrP1195L/+ and WT mice fed ad libitum (n = 8–10 per each group). (b) Body weight of InsrP1195L/+ and WT mice (n = 8–10 per each group). (c) OGTT (n = 8–10 per each group). (d) ITT (n = 6–10 per each group). (e,f) mRNA expressions of Pck1 (e) and G6pc (f) in liver (n = 10–12 per each group). (g,h) Blood glucose levels after pyruvate (g) and glycerol (h) administration (n = 10–12 per each group). Data are mean ± SEM. Only the statistical difference between WT/HFD and InsrP1195L/+/HFD mice is depicted by asterisks in (a–d,g,h). Significance between strains (WT/HFD and InsrP1195L/+/HFD mice) at individual time points by two-tailed Student’s t-test (a–d,g,h). Two-way ANOVA plus Bonferroni post-hoc analysis (e,f). *P < 0.05, **P < 0.01, ***P < 0.001.
Gluconeogenesis from glycerol but not from pyruvate is elevated in InsrP1195L/+/HFD mice
Because severe insulin resistance in InsrP1195L/+/HFD mice suggested unsuppressed gluconeogenesis in an otherwise insulin resistant liver, as is found in liver-specific Insr knockout (LIRKO) mice7, mRNA expressions of two key enzymes, phosphoenolpyruvate carboxykinase 1 (Pck1) and glucose-6-phosphatase (G6pc), were examined (Fig. 1e,f). Although Pck1 expression in InsrP1195L/+/HFD mice was not significantly different from that in WT/HFD mice, G6pc expression in InsrP1195L/+/HFD mice was markedly elevated by re-feeding. Pck1 is a key enzyme involved in gluconeogenesis from amino acids and pyruvate, while G6pc participates in gluconeogenesis from glycerol as well as from amino acids and pyruvate. We therefore assessed gluconeogenesis from pyruvate (Fig. 1g) and glycerol (Fig. 1h) in vivo by measuring the blood glucose rise after intraperitoneal administration of either of the two substrates. Pyruvate administration increased the blood glucose levels similarly in InsrP1195L/+/HFD and WT/HFD mice (Fig. 1g). By contrast, glycerol administration to InsrP1195L/+/HFD mice evoked a larger increase in blood glucose levels compared with those of WT/HFD mice (Fig. 1h), suggesting that gluconeogenesis from glycerol but not from pyruvate was elevated in InsrP1195L/+/HFD mice.
Fat accumulation is decreased in InsrP1195L/+/HFD mice compared with that in WT/HFD mice
Glycerol is produced by lipolysis of the triacylglycerols (TG) accumulated in the main energy reservoir, the white adipose tissues (WAT). When compared with WT/HFD mice, InsrP1195L/+/HFD mice had lower body weight (Fig. 1b), lower serum leptin levels (Fig. 2a) and less subcutaneous and visceral fat as assessed by computed tomography (CT) scanning (Fig. 2b), indicating that InsrP1195L/+/HFD mice have reduced fat mass. Histological analysis of epididymal fat revealed that InsrP1195L/+/HFD mice had smaller adipocytes than those of WT/HFD mice, while there was no difference in adipocyte size between InsrP1195L/+/ND and WT/ND mice (Fig. 2c, Supplementary Fig. S1a–d). In addition, the liver of InsrP1195L/+/HFD mice had lower TG content (Supplementary Fig. S2a) and less lipid accumulation in hepatocytes compared with WT/HFD mice (Supplementary Fig. S2c), indicating that ectopic fat accumulation is not a major cause of hyperglycemia in InsrP1195L/+/HFD mice. Alternatively, there was a positive correlation between body weight and TG content in all animal groups (Supplementary Fig. S2b).
Fat combustion in vivo and lipolysis in WAT under HFD are increased in InsrP1195L/+ mice.
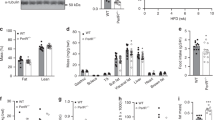
(a) Serum leptin levels at 16 weeks (n = 8–10 per each group). (b) Representative CT images (22week of age) at the level of lower end of right kidney. Visceral and subcutaneous fat are indicated in pink and yellow, respectively. (c) Hematoxylin and eosin staining of epididymal fat. (d–g) Oxygen consumption rate (d) and RQ (e) under ND in InsrP1195L/+ and WT mice. Oxygen consumption rate (f) and RQ (g) under HFD in InsrP1195L/+ and WT mice (n = 6–7 per each group). (h) Western blot analysis of phospho-HSL in fasted and refed conditions. (left) A representative result showing increased phospho-HSL in InsrP1195L/+/HFD mice. (right) Quantified result of phospho-HSL levels. (n = 6–9 per each group). (i) Western blot analysis of phospho-Akt induced by insulin (0.1 IU/kg i.v.) in WAT. (left) A representative result showing attenuated phospho-Akt in InsrP1195L/+/HFD mice. (right) Quantified result of phospho-Akt levels. (n = 4–6 per each group). (j) Western blot analysis of phospho-Akt induced by insulin (0.1 IU/kg i.v.) in liver. (left) A representative result showing attenuated phospho-Akt in InsrP1195L/+/HFD mice. (right) Quantified result of phospho-Akt levels. (n = 4–6 per each group). Cropped blots were used. Full-length blots are presented in Supplementary Fig. S6. Data are mean ± SEM. Two-way ANOVA plus Bonferroni post-hoc analysis (a). Significance between treatment and strains by two-tailed Student’s t-test (h–j) and by One-way ANOVA plus Bonferroni post-hoc analysis (d-g, h-j), respectively. *P < 0.05, **P < 0.01, ***P < 0.001, NS; not significant.
Respiratory quotient (RQ) is increased during dark phase in InsrP1195L/+ mice under both ND and HFD
The decrease in fat accumulation in WAT and liver of InsrP1195L/+/HFD mice suggested that these animals may have increased energy dissipation and/or fat usage. We therefore measured the oxygen consumption rate and RQ in InsrP1195L/+ and WT mice (Fig. 2d–g). Although the oxygen consumption rate was not different between InsrP1195L/+ and WT mice under ND (Fig. 2d), InsrP1195L/+/ND mice exhibited lower RQ during dark phase compared with WT/ND mice (Fig. 2e). Although the oxygen consumption rate in InsrP1195L/+/HFD mice was plotted higher than that in WT/HFD mice when expressed per body weight (Fig. 2f), this difference is considered to be due to the significant decrease in their body weight. Nevertheless, the RQ during dark phase of InsrP1195L/+/HFD mice was lower than that of WT/HFD mice (Fig. 2g), suggesting the increased fat usage in these mice. These results also indicate that the diurnal metabolic switching of energy source by insulin is impaired in the state.
Lipolysis is increased in InsrP1195L/+ mice only under HFD
We then examined whether lipolysis was increased in InsrP1195L/+/HFD mice. Lipolysis in WAT is activated by β-adrenergic signaling and inhibited by insulin signaling via regulation of intracellular cAMP levels. Insulin suppresses lipolysis through PKA-dependent inactivation of hormone sensitive lipase (HSL)8. However, phospho-HSL levels in WAT of InsrP1195L/+/ND mice were increased after fasting and were decreased by re-feeding similarly to those of WT/ND mice (Fig. 2h). Importantly, HFD feeding markedly suppressed phospho-HSL levels in WT mice, but suppressed them much less in InsrP1195L/+ mice (Fig. 2h), indicating that the defective insulin signaling in WAT resulted in the increased HSL phosphorylation in InsrP1195L/+ mice preferentially under HFD condition.
Akt phosphorylation by insulin is impaired in InsrP1195L/+/HFD mice, both in WAT and in liver
Insulin inhibits lipolysis in adipocytes and gluconeogenesis in hepatocytes. Since lipolysis and gluconeogenesis were increased in InsrP1195L/+/HFD mice, we evaluated insulin signaling in WAT and liver by analyzing Akt phosphorylation in response to insulin administration in vivo (Fig. 2i,j). Quantification of phospho-Akt protein revealed that insulin-induced Akt phosphorylation was significantly less in InsrP1195L/+/ND mice and in WT/HFD mice compared with that in WT/ND mice. Notably, Akt phosphorylation in InsrP1195L/+/HFD mice was barely induced by insulin, indicating that insulin signaling is markedly impaired by combination of genetic mutation (InsrP1195L) in the insulin receptor and environmental condition (HFD feeding) in both WAT and liver.
Lipolysis in the primary adipocytes of InsrP1195L/+ mice is suppressed under ND but increased under HFD
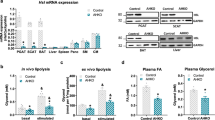
To exclude the influence of the sympathetic nervous system and hyperinsulinemia in InsrP1195L/+ mice, we measured glycerol release in primary adipocytes in vitro. Lipolysis was measured directly using isolated primary adipocytes (Fig. 3a,b). In InsrP1195L/+/ND mice, the basal and isoproterenol-stimulated lipolysis were significantly lower than that in WT/ND mice (Fig. 3a). By contrast, the inhibition of lipolysis by insulin was attenuated in InsrP1195L/+/ND mice. As a result, the lipolytic activity of InsrP1195L/+/ND mice in the presence of isoproterenol plus insulin was lower than that of WT/ND mice. HFD feeding blunted the sensitivity of isoproterenol-stimulated lipolysis in both WT and InsrP1195L/+ mice (Fig. 3b). Therefore, in mice under HFD, the anti-lipolytic action of insulin was evaluated in adipocytes stimulated with a higher dose (300 nM) of isoproterenol. Although the basal lipolysis in InsrP1195L/+/HFD adipocytes was similar to that in WT/HFD adipocytes, isoproterenol-stimulated lipolysis was significantly higher in InsrP1195L/+/HFD adipocytes and insulin suppressed glycerol release poorly (Fig. 3b). The increased lipolysis by isoproterenol alone (in the absence of co-treatment with insulin) in InsrP1195L/+/HFD adipocytes also suggests that some factors [such as activities of perilipin9 and/or adipocyte triglyceride lipase10 (ATGL)] other than insulin-dependent suppression of phospho-HSL may contribute to the increased lipolysis11.
Lipolysis in primary adipocytes is increased in InsrP1195L/+/HFD mice.
(a,b) Glycerol release of primary adipocytes isolated from InsrP1195L/+ and WT mice under ND (a) and HFD (b) (n = 6 per each group). Data are mean ± SEM. *, †; comparison against isoproterenol-stimulated glycerol release (in the absence of insulin) in WT and InsrP1195L/+ mice, respectively. One-way ANOVA plus Bonferroni post-hoc analysis. Iso; isoproterenol, *P < 0.05, **P < 0.01, ***P < 0.001, †P < 0.05, †††P < 0.001, NS; not significant.
Stimulation of lipolysis by CL316432 evokes hyperglycemia in InsrP1195L/+/HFD mice
We also examined whether the increase in lipolysis could contribute to hyperglycemia in InsrP1195L/+/HFD mice under in vivo conditions. We treated the mice with CL316432, a β3-adrenergic receptor-specific agonist and monitored the changes in serum glycerol (Fig. 4a) and blood glucose (Fig. 4b) levels. Although the serum glycerol levels were similarly increased in WT/HFD mice and InsrP1195L/+/HFD mice, the blood glucose levels after CL316432 administration were significantly higher in InsrP1195L/+/HFD mice, indicating that enhanced lipolysis exacerbates hyperglycemia in InsrP1195L/+/HFD mice.
Lipolysis-induced gluconeogenesis is increased in InsrP1195L/+/HFD mice.
(a,b) Serum glycerol (a) and blood glucose levels (b) after CL316432 administration (n = 5–10 per each group). (c,d) Expression of G6pc (c) and Pck1 (d) in the WT liver after intraperitoneal glycerol administration (n = 7–10 per each group). Data are mean ± SEM. Only the statistical difference between WT/HFD and InsrP1195L/+/HFD mice is depicted by asterisk in b. Significance between strains (WT/HFD and InsrP1195L/+/HFD mice) at individual time points by two-tailed Student’s t-test (a,b) One-way ANOVA plus Bonferroni post-hoc analysis (c,d). *P < 0.05, **P < 0.01, ***P < 0.001.
Our results also indicate increased gluconeogenesis from glycerol. G6pc is a key enzyme that mediates gluconeogenesis from glycerol and its gene expression is suppressed by insulin. Increased G6pc expression in InsrP1195L/+/HFD liver could therefore result from impaired repression by insulin in liver and/or be secondary to increased glycerol influx to liver. Therefore, we examined whether glycerol administration increases G6pc expression in WT liver in vivo (Fig. 4c). Glycerol significantly increased the expression of G6pc while Pck1 expression was decreased by glycerol administration (Fig. 4d), suggesting that the intracellular abundance of substrates for gluconeogenesis determines the expressions of their regulatory enzymes.
Transplantation of wild-type subcutaneous WAT ameliorates hyperglycemia of InsrP1195L/+/HFD mice
To assess the involvement of increased lipolysis in WAT of InsrP1195L/+/HFD mice on the development of hyperglycemia, we transplanted wild-type subcutaneous WAT to InsrP1195L/+ mice. Although transplanted InsrP1195L/+/HFD mice gained weight similarly to un-transplanted InsrP1195L/+/HFD mice (Fig. 5a), the blood glucose levels in fed conditions were significantly lower than those of un-transplanted InsrP1195L/+/HFD mice at 14 and 16 weeks of age (Fig. 5b). In addition, the rise in blood glucose levels of transplanted InsrP1195L/+/HFD mice on re-feeding was significantly reduced compared with those of un-transplanted InsrP1195L/+/HFD mice (Fig. 5c). As the phospho-HSL level in the transplanted fat pad was similar to that of endogenous WAT in WT/HFD mice (Fig. 5d,e), suppression of lipolysis in the transplant might well have ameliorated the systemic hyperglycemia of InsrP1195L/+/HFD mice. As expected, the increased G6pc expression in InsrP1195L/+/HFD liver on re-feeding was markedly reduced by the transplantation of wild-type subcutaneous fat to the mice (Fig. 5f). To assess the involvement of anti-inflammatory cytokines released from the transplant, we measured serum adiponectin levels (Fig. 5g). In our experimental conditions with 45% HFD, adiponectin was not decreased in WT/HFD mice. By contrast, adiponectin of InsrP1195L/+/HFD mice was significantly lower than that of InsrP1195L/+/ND mice. Notably, fat transplantation to InsrP1195L/+/HFD mice did not increase adiponectin, suggesting that change in adiponectin did not contribute to improved glycemia.
Hyperglycemia in InsrP1195L/+/HFD mice is ameliorated by transplantation of wild-type subcutaneous WAT.
(a,b) Body weight (a) and blood glucose levels (b) (n = 13–15 per each group). (c) The blood glucose levels at 16-hr fasted and 3 hrs after food replenishment at 18–20 weeks of age (n = 7–10 per each group). (d,e) Western blot analysis of phospho-HSL levels in fasted and refed conditions. (d) A representative result showing increased phospho-HSL in InsrP1195L/+/HFD mice. Endo., endogenous fat; Trans., transplanted fat. Cropped blots were used. Full-length blots are presented in Supplementary Fig. S6. (e) Quantified result of phospho-HSL levels. (n = 4 per each group). (f) mRNA expressions of G6pc in liver on fasted and refed conditions (nv6–8 per each group). (g) Serum adiponectin levels (n = 8 per each group). Data are mean ± SEM. Significance between treatment (un-transplanted InsrP1195L/+/HFD and transplanted InsrP1195L/+/HFD mice) at individual time points by two-tailed Student’s t-test (a–c,f). One-way ANOVA plus Bonferroni post-hoc analysis (e,g). *P < 0.05, **P < 0.01, ***P < 0.001, NS; not significant.
BA physiology is diversely altered in InsrP1195L/+/HFD mice
As fat-specific insulin receptor deficient mice (FIRKO mice) failed to exhibit glucose intolerance, we examined the contribution of insulin resistance in liver. To clarify its molecular mechanism, we performed microarray analysis in liver of InsrP1195L/+/HFD and WT/HFD mice and found that expressions of several genes involved in BA physiology were altered. We therefore quantified mRNA expressions of the enzymes involved in BA synthesis (Fig. 6a–d) and BA transporters (Fig. 6e,f). Expression of Cyp7a1, the rate-limiting enzyme of BA synthesis, was significantly increased by re-feeding similarly in WT/ND mice and InsrP1195L/+/ND mice, while that in WT/HFD mice was significantly elevated under fasted condition and did not show further increase by re-feeding. Interestingly, Cyp7a1 expression in InsrP1195L/+/HFD mice was markedly decreased by re-feeding (Fig. 6a). By contrast, expression of Cyp7b1, another enzyme of BA synthesis, was increased in InsrP1195L/+/HFD mice (Fig. 6b). Expression of Cyp27a1 was not altered among the 4 animal groups (Fig. 6c). Expression of Cyp8b1, the sterol 12α-hydroxylase required for generation of CA, was decreased in InsrP1195L/+/HFD mice (Fig. 6d). In addition, we examined expressions of BA transporters, Slc10a1 and Slco1a1 (Fig. 6e,f). Expression of Slco1a1 but not Slc10a1 was significantly increased in InsrP1195L/+/HFD mice.
BA physiology is diversely altered in InsrP1195L/+/HFD liver.
(a–d) mRNA expressions of genes involved in BA synthesis (n = 8–12 per each group). (e,f) mRNA expressions of genes involved in BA transport (n = 8–12 per each group). (g) Relative BA composition in liver in refed condition (n = 3). (h) The ratio of muricholates to cholates, calculated with the molar percentage of tauro α-, tauro β- and tauro ω-mucricholates and taurocholate. (i) mRNA expression of Cyp7a1 after oral glucose loading in Kir6.2−/− mice (n = 7–12 per each group). (j) mRNA expression of Cyp7a1 in fat transplanted InsrP1195L/+/HFD mice (n = 5–7 per each group). (k) mRNA expression of Cyp7a1 in the WT liver after intraperitoneal glycerol administration (n = 7–10 per each group). Data are mean ± SEM. Two-way ANOVA plus Bonferroni post-hoc analysis (a–f). Significance between treatment by two-tailed Student’s t-test (i). One-way ANOVA plus Bonferroni post-hoc analysis (g,h,j,k). *P < 0.05, **P < 0.01, ***P < 0.001, NS; not significant.
We therefore measured the BA content in liver by LC-MS/MS analysis and found that BA composition was altered in InsrP1195L/+/HFD liver (Fig. 6g,h) as well as in serum (Supplementary Fig. S5a,b). In contrast, total BA content in InsrP1195L/+/HFD liver was not different from that in WT/HFD liver, suggesting that BA content might be maintained through various compensatory mechanisms, such as altered BA synthesis, absorption and secretion. It remains undetermined whether or not the decreased Cyp7a1 expression in InsrP1195L/+/HFD liver is the primary or a secondary change induced by HFD feeding plus insulin resistance. However, our present findings show that HFD feeding plus insulin resistance induces alterations in BA physiology in liver.
We then examined acute regulation of Cyp7a1 expression in liver. We found that Cyp7a1 expression was significantly increased by refeeding in WT/ND and InsrP1195L/+/ND mice. Both glucose and insulin signaling have been reported to regulate Cyp7a1 expression in liver12. To clarify their relative importance, we examined Cyp7a1 induction in response to oral glucose loading in Kir6.2 deficient mice (Kir6.2−/− mice), which lack glucose-stimulated insulin secretion13. Glucose loading failed to induce Cyp7a1 expression in Kir6.2−/− mice (Fig. 6i), suggesting that insulin plays a critical role in Cyp7a1 expression. In addition, the effect on BA physiology of fat transplantation to InsrP1195L/+/HFD mice was assessed by measuring Cyp7a1 in transplanted InsrP1195L/+/HFD mice (Fig. 6j). Reduced mRNA expression of Cyp7a1 in InsrP1195L/+/HFD mice on re-feeding was significantly increased by fat transplantation, suggesting that modulation of metabolism in adipocytes by WAT transplantation may elicit alteration in BA physiology in liver. To test this, we examined whether in vivo administration of glycerol suppresses Cyp7a1 in wild-type liver. Interestingly, intraperitoneal glycerol administration significantly inhibited Cyp7a1 expression in liver (Fig. 6k), suggesting that the unsuppressed lipolysis in WAT might alter BA physiology in liver via glycerol dynamics.
Recent studies have shown that BAs play an important role in the regulation of energy and glucose metabolism. Various molecules including the farnesoid X receptor (FXR)14 and the G-protein coupled receptor TGR515 are known to be involved in the BA-medicated metabolic regulation. In accord with the previous reports16, we found that supplementation with CA significantly decreased the gain in body weight in both WT/HFD and InsrP1195L/+/HFD mice (Fig. 7a). In addition, supplementation with ursodeoxycholic acid (UDCA) elicited a reduced body weight gain similar to that by CA supplementation. Notably, the supplementation with either CA or UDCA restored euglycemia in InsrP1195L/+/HFD mice (Fig. 7b) and prevented the rise in G6pc expression on re-feeding (Fig. 7c), suggesting that alteration in BAs may influence glucose homeostasis in InsrP1195L/+/HFD mice.
Supplementation with either CA or UDCA ameliorated hyperglycemia of InsrP1195L/+/HFD mice.
(a,b) Changes in body weight (a) and blood glucose levels (b). (c) mRNA expressions of G6pc in liver in fasted and refed conditions (n = 5–8 per each group). *,†only the statistical difference between supplementation with or without CA in InsrP1195L/+/HFD mice (*) and in WT/HFD (†) is depicted by symbols in (a,b). Data are mean ± SEM. Significance between treatment at individual time points by two-tailed Student’s t-test (a,b). Two-way ANOVA plus Bonferroni post-hoc analysis (c). *,†P < 0.05, **,††P < 0.01, ***,†††P < 0.001.
Discussion
We previously reported that mutant mice harboring a single amino acid substitution in the insulin receptor (InsrP1195L/+ mice) exhibit insulin resistance but normal glucose tolerance6. In the present study, we found that InsrP1195L/+ mice develop overt hyperglycemia and only mild obesity under HFD. In some ways, the lesser degree of obesity and exacerbated metabolic disturbances in these mice resembles the clinical characteristics of Asian patients with T2DM17,18, suggesting that InsrP1195L/+/HFD mice are suitable for investigating the pathophysiology of HFD-sensitive T2DM in humans.
The glucose intolerance and impaired glucose lowering effect of insulin in InsrP1195L/+/HFD mice resemble those in LIRKO mice3,7. Hyperglycemia in LIRKO mice is characterized by unsuppressed hepatic gluconeogenesis associated with increased mRNA expressions of two gluconeogenesis enzymes, Pck1 and G6pc. Although Pck1 expression was only mildly elevated, G6pc expression was markedly elevated in InsrP1195L/+/HFD mice. InsrP1195L/+/HFD mice exhibited enhanced gluconeogenesis from glycerol (Fig. 1h) but not from pyruvate (Fig. 1g), compared with WT/HFD mice. In addition, lipolysis and subsequent gluconeogenesis from glycerol was found to be increased in InsrP1195L/+/HFD mice. By contrast, the expression of fatty acid synthase (Fas) in liver, for example, was not decreased in InsrP1195L/+/HFD mice (Supplementary Fig. S3), although its transcription is known to be stimulated by insulin, principally through SREBP-1c19. In addition, Srebp-1 expression in the liver by re-feeding was not attenuated in InsrP1195L/+/HFD mice, indicating that hepatic Srebp-1 expression in the liver by re-feeding and by HFD feeding remains intact under insulin resistance (i.e., is insulin sensitive3). On the other hand, RQ during dark phase was significantly reduced in InsrP1195L/+ mice even under ND condition (Fig. 2e,g), suggesting that diurnal switching of the energy usage was inflexible under insulin resistance (i.e., is insulin resistant3). This metabolic inflexibility in InsrP1195L/+ mice could be also due to compensatory increase in fat utilization in fat and skeletal muscle during dark phase caused by impaired glucose uptake in these tissues.
We found that fat transplantation significantly ameliorated hyperglycemia in InsrP1195L/+/HFD mice. We also found that serum FFA levels in InsrP1195L/+/HFD mice were significantly higher than those in WT/HFD mice (Supplementary Fig. S4), suggesting that pro-inflammatory factors may participate in hyperglycemia of InsrP1195L/+/HFD mice in addition to the unsuppressed glycerol release.
With regard to the amelioration of hyperglycemia in fat-transplanted InsrP1195L/+/HFD mice, it is unclear whether the improved glucose uptake into the transplant may play a major role, as WAT has been reported to play a minor role in glucose uptake in rodents20. However, increased glucose uptake and elevated lipogenesis in WAT has been found to improve glucose tolerance through synthesis of branched fatty acid esters of hydroxy fatty acids (FAHFAs)21. Although the presence of the insulin-sensitive fat transplant might increase the FAHFAs in fat-transplanted InsrP1195L/+/HFD mice, our present results suggest that normal glycerol metabolism in WAT is also important for the maintenance of glucose homeostasis under insulin resistance. Nevertheless, the lack of glucose intolerance in FIRKO mice suggested that insulin resistance in tissues other than WAT is involved in developing hyperglycemia in InsrP1195L/+/HFD mice. Importantly, liver-specific insulin receptor-deficient mice (LIRKO mice) exhibit hyperglycemia associated with increased G6pc expression7. Although insufficient insulin secretion also is likely to contribute to the hyperglycemia in InsrP1195L/+/HFD mice, as found in both humans and rodents22, in the present study, we focused on the involvement of insulin resistance in liver. Notably, we found that the expressions of genes involved in BA metabolism are diversely altered. Quantification of BA composition revealed that BAs of InsrP1195L/+/HFD liver were more hydrophobic than those of WT/HFD liver. However, it remains unknown whether BA hydrophobicity is related to the hyperglycemia in InsrP1195L/+/HFD mice. It has been reported that hydrophobicity in liver is increased in LIRKO mice, which develop gallstones under lithogenic diet23. In contrast, our present study suggests that HFD feeding plus hepatic insulin resistance is involved in the alterations in BA composition.
Hepatic expression of Cyp7a1 was dramatically reduced in InsrP1195L/+/HFD mice. Interestingly, in LIRKO mice, Cyp7a1 expression was also markedly decreased, suggesting that insulin signaling is involved in Cyp7a1 expression23. Although Cyp7a1 expression is reported to be induced acutely by glucose and insulin12, our study in Kir6.2−/− mice, which lack glucose-stimulated insulin secretion, revealed the importance of insulin in its transactivation. In addition, Cyp7a1-overexpressing transgenic mice have been reported to show improved glucose tolerance and reduced G6pc expression under HFD condition24. Furthermore, tauro-CA (TCA) has been reported to suppress G6pc expression in primary hepatocytes25. Reduction of blood glucose levels and suppression of G6pc expression in liver of InsrP1195L/+/HFD mice by supplementation with either CA or UDCA suggest that alterations in BAs might contribute to the development of hyperglycemia in these mice. Amelioration of Cyp7a1 and G6pc by fat transplantation in InsrP1195L/+/HFD liver and suppression of Cyp7a1 by glycerol in wild-type mice suggest that suppressed hepatic expression of Cyp7a1 might well play a role in the regulation of glucose homeostasis in InsrP1195L/+/HFD mice. Although the underlying mechanisms of BA physiology in glucose metabolism remain unknown, many studies have found that BA physiology is altered in T2DM patients26. Considering that FXR signaling is activated by CA but not by UDCA, the anti-diabetic action of BAs in InsrP1195L/+/HFD mice might be mediated also by a FXR-independent mechanism.
In conclusion, excessive glycerol supply from WAT is suggested to induce enhanced G6pc expression, leading to unsuppressed gluconeogenesis and resulting in hyperglycemia in InsrP1195L/+/HFD mice. In addition, alterations of metabolism in adipocytes are linked with abnormal BA physiology in InsrP1195L/+/HFD mice (Fig. 8).
Methods
Animals and metabolic analyses
InsrP1195L/+ mice were generated as described previously27. The mice have been backcrossed to the C57BL/6 strain over more than 10 generations. Mice were fed ad libitum and kept on a 12-hr light/12-hr dark cycle. For ND feeding, the mice were maintained on standard chow (CE-2) (12.1 % kcal from fat) (Clea Japan Inc., Tokyo, Japan). For HFD feeding, the mice were maintained on a HFD (D12492) (60.0 % kcal from fat) (Research Diets Inc., New Brunswick, NJ, USA) starting at 8 weeks of age unless stated otherwise. OGTT and ITT were performed as previously described13, using 1 g/kg glucose and 0.75 IU/kg insulin after 16-hr fast. For pyruvate tolerance test, glycerol tolerance test and CL316432 loading test, 16-hr fasted mice were administered intraperitoneally with 1 g/kg sodium pyruvate, 0.5 g/kg glycerol and 0.1 mg/kg CL316432 (Tocris Bioscience, Bristol, UK), respectively and blood glucose levels were monitored at the indicated time points. Blood glucose was measured as previously described13. Glycerol in the serum was measured using the kit from BioVision, Inc. (San Francisco, CA, USA). Serum adiponectin levels were measured using the kit from Otsuka pharmaceuticals. (Tokyo, Japan). For CA and UDCA supplementation, CA (0.25 % wt/wt) (Sigma, St. Louis, MO, USA) or UDCA (0.25 % wt/wt) (Tokyo chemical industry, Tokyo, Japan) was added to the HFD (D12492) and the diet was given to the mice at 8 weeks of age for 8 weeks. All animal studies were conducted in accordance with the International Guiding Principles for Biomedical Research Involving Animals and were approved by the Animal Care and Use Committees of Chiba University and the National Institute for Physiological Sciences in Japan.
Real-time qRT-PCR analyses
Total RNA was isolated from WAT (epididymal fat pad, unless stated otherwise) and liver and subjected to qRT-PCR analyses using SYBR Green, according to the manufacturer’s protocol. The primers used were 5′-caccatcacctcctggaaga-3′ and 5′-gggtgcagaatctcgagttg-3′ for Pck1, 5′-gtggcagtggtcggagact-3′ and 5′-acgggcgttgtccaaac-3′ for G6pc, 5′-tacagagtgctggccaagag-3′ and 5′-ttcaaggatgcactggagag-3′ for Cyp7a1, 5′-tagccctctttcctccactcata-3′ and 5′-gaagcgatcgaacctaaattcct-3′ for Cyp7b1, 5′-gcctcacctatgggatcttca-3v and 5v-tcaaagcctgacgcagatg-3v for Cyp27a1, 5′-ggctggcttcctgagcttatt-3′ and 5′-acttcctgaacagctcatcgg-3′ for Cyp8b1, 5′-acctgtctaacctcttcacc-3′ and 5′-caatgctgaggttcatgtcc-3′ for Slc10a1, 5′-ggaagattgttggcccgatt-3′ and 5′-agtgggagttatggtcaggt-3v for Slco1a1, 5′-gcgtcgtgattagcgatga-3′ and 5′-atggcctcccatctcctt-3′ for Hprt.
Western blotting
Western blotting analyses were carried out with tissue homogenates from WAT under standardized methods. To elucidate HSL phosphorylation of WAT in fasted and refed conditions, the mice were fasted for 16 hrs in fasted groups and refed for 3 hrs in refed groups. To elucidate insulin signaling in response to intravenous insulin, the cervical vein was exposed and 0.1 IU/kg insulin was injected via the vein. Five minutes later, WAT and liver were removed. The tissues were lysed in sonication buffer (20 mM HEPES pH7.5; 150 mM NaCl; 25 mM EDTA 1% NP-40; 10% glycerol, 1 mM sodium vanadate, 1 mM phenylmethylsulfonyl fluoride [PMSF] and protease and phosphatase inhibitors). Twenty μg protein for WAT and 50 μg protein for liver was subjected to SDS-PAGE. Antibodies against the following proteins were used (all from Cell Signaling): phospho-HSL (p-S660) (1:1000), HSL (1:1000), phospho-Akt (p-S473) (1:1000), Akt (1:1000) and β-actin (1:1000).
Histological examination
Histological examination of WAT and liver was carried out under standardized methods. The tissues were dissected, fixed in 10% buffered formalin overnight, washed with PBS and embedded in paraffin. Sections were stained with hematoxylin and eosin for histological analysis and the slides were examined under a Keyence BZ-8100 microscope (Keyence Japan, Osaka, Japan).
CT scanning
Mice were anesthetized and placed in the chamber of a CT scanner for mouse (Latheta LCT-200, Aloka, Tokyo, Japan). The CT scanner was calibrated according to the manufacturer’s protocols.
Oxygen consumption
Oxygen consumption was measured using a MK-5000RQ (MK-5000RQ, Muromachi Kikai, Tokyo, Japan), with one mouse per chamber. Four groups of mice (InsrP1195L/+ and WT mice under either ND or HFD) aged 14 weeks (after 6 weeks of HFD feeding) were tested simultaneously. Mice had free access to food and water. Oxygen consumption was measured after the acclimatizing period for more than 2 weeks.
Fat transplantation
Subcutaneous fat pad isolated from abdominal walls of 8-week-old male WT mice was transplanted into the subcutaneous area below the skin on the back of InsrP1195L/+ mice at 7 weeks of age, as previously reported28. The fat pad isolated from two donor mice (~0.7g of fat tissue/2 mice) was used for a single recipient. After one week of recovery period, only the recipient mice that exceeded the initial body weight (i.e., body weight of the recipient plus weight of the transplant) were subjected to a HFD (D12451) (45.0 % kcal from fat) (Research Diets Inc.) for 8 weeks. Sham operation was performed on the un-transplanted mice in the fat transplantation experiments (Fig. 5a–g).
Isolation of mouse primary adipocytes and lipolysis assay
Epididymal fat was excised, minced and digested with 0.2 % (w/v) collagenase type I (Life Technologies) for 30 min at 37 °C under shaking, as previously described29. The cells were passed through 500-μm nylon mesh and washed by Krebs Ringer Bicarbonate buffer 4 times. After 30 min pre-incubation, adipocytes were incubated with or without insulin (0.1 ~ 3 nM) for 5 min and the cells were further incubated with isoproterenol (30 or 300 nM) for 30 min. The reaction solution was subjected to glycerol assay to assess the lipolysis activity. Glycerol in the buffer was measured using the kits from BioVision, Inc.
Measurement of BA composition
Liver samples and serum for measuring BA composition were collected from the mice at 3 hrs after refeeding. BA composition was measured in Junshin Clinic Bile Acid Institute (Tokyo, Japan) by LC-MS/MS in reference to the method described previously30,31. The standard for tauro-αMCA-3-sulfate was kindly provided by Dr. Takashi Iida at Nippon University.
Statistics
Results are expressed as means ± SEM. Differences between two groups were assessed using the unpaired two-tailed Student’s t-test. Data sets involving more than three groups were assessed by One-way ANOVA or Two-way ANOVA with Bonferroni post-hoc test. P < 0.05 was considered to be statistically significant.
Additional Information
How to cite this article: Young Lee, E. et al. Unsuppressed lipolysis in adipocytes is linked with enhanced gluconeogenesis and altered bile acid physiology in InsrP1195L/+ mice fed high-fat-diet. Sci. Rep. 5, 17565; doi: 10.1038/srep17565 (2015).
References
Nolan, C. J., Damm, P. & Prentki, M. Type 2 diabetes across generations: from pathophysiology to prevention and management. The Lancet 378, 169–181 (2011).
Nakamura, A. et al. Protection from non-alcoholic steatohepatitis and liver tumourigenesis in high fat-fed insulin receptor substrate-1-knockout mice despite insulin resistance. Diabetologia 55, 3382–3391 (2012).
Biddinger, S. B. & Kahn, C. R. From mice to men: insights into the insulin resistance syndromes. Annu. Rev. Physiol. 68, 123–158 (2006).
Semple, R. K., Savage, D. B., Cochran, E. K., Gorden, P. & O'Rahilly, S. Genetic syndromes of severe insulin resistance. Endocr. Rev. 32, 498–514 (2011).
Kadowaki, T., Ueki, K., Yamauchi, T. & Kubota, N. SnapShot: Insulin signaling pathways. Cell 148, 624 624.e1 (2012).
Ogino, J. et al. Insulin resistance and increased pancreatic beta-cell proliferation in mice expressing a mutant insulin receptor (P1195L). J. Endocrinol. 190, 739–747 (2006).
Michael, M. D. et al. Loss of insulin signaling in hepatocytes leads to severe insulin resistance and progressive hepatic dysfunction. Mol. Cell 6, 87–97 (2000).
Czech, M. P., Tencerova, M., Pedersen, D. J. & Aouadi, M. Insulin signalling mechanisms for triacylglycerol storage. Diabetologia 56, 949–964 (2013).
Martinez-Botas, J. et al. Absence of perilipin results in leanness and reverses obesity in Lepr(db/db) mice. Nat. Genet. 26, 474–479 (2000).
Zimmermann, R. et al. Fat mobilization in adipose tissue is promoted by adipose triglyceride lipase. Science 306, 1383–1386 (2004).
Peirce, V., Carobbio, S. & Vidal-Puig, A. The different shades of fat. Nature 510, 76–83 (2014).
Li, T. et al. Glucose and insulin induction of bile acid synthesis: mechanisms and implication in diabetes and obesity. J. Biol. Chem. 287, 1861–1873 (2012).
Miki, T. et al. Defective insulin secretion and enhanced insulin action in KATP channel-deficient mice. Proc. Natl. Acad. Sci. USA 95, 10402–10406 (1998).
Cipriani, S., Mencarelli, A., Palladino, G. & Fiorucci, S. FXR activation reverses insulin resistance and lipid abnormalities and protects against liver steatosis in Zucker (fa/fa) obese rats. J. Lipid Res. 51, 771–784 (2010).
Thomas, C. et al. TGR5-mediated bile acid sensing controls glucose homeostasis. Cell Metab. 10, 167–177 (2009).
Watanabe, M. et al. Bile acids induce energy expenditure by promoting intracellular thyroid hormone activation. Nature 439, 484–489 (2006).
Yoon, K. H. et al. Epidemic obesity and type 2 diabetes in Asia. The Lancet 368, 1681–1688 (2006).
Waki, K. et al. Alcohol consumption and other risk factors for self-reported diabetes among middle-aged Japanese: a population-based prospective study in the JPHC study cohort I. Diabet. Med. 22, 323–331 (2005).
Wong, R. H. & Sul, H. S. Insulin signaling in fatty acid and fat synthesis: a transcriptional perspective. Curr. Opin. Pharmacol. 10, 684–691 (2010).
James, D. E., Burleigh, K. M. & Kraegen, E. W. Time dependence of insulin action in muscle and adipose tissue in the rat in vivo. An increasing response in adipose tissue with time. Diabetes 34, 1049–1054 (1985).
Yore, M. M. et al. Discovery of a class of endogenous mammalian lipids with anti-diabetic and anti-inflammatory effects. Cell 159, 318–332 (2014).
Kahn, S. E., Cooper, M. E. & Del Prato, S. Pathophysiology and treatment of type 2 diabetes: perspectives on the past, present and future. The Lancet 383, 1068–1083 (2014).
Biddinger, S. B. et al. Hepatic insulin resistance directly promotes formation of cholesterol gallstones. Nat. Med. 14, 778–782 (2008).
Li, T. et al. Transgenic expression of cholesterol 7alpha-hydroxylase in the liver prevents high-fat diet-induced obesity and insulin resistance in mice. Hepatology 52, 678–690 (2010).
Cao, R. et al. Bile acids regulate hepatic gluconeogenic genes and farnesoid X receptor via G(alpha)i-protein-coupled receptors and the AKT pathway. J. Lipid Res. 51, 2234–2244 (2010).
Prawitt, J., Caron, S. & Staels, B. Glucose-lowering effects of intestinal bile acid sequestration through enhancement of splanchnic glucose utilization. Trends Endocrinol. Metab. 25, 235–244 (2014).
Baba, T. et al. Estrogen, insulin and dietary signals cooperatively regulate longevity signals to enhance resistance to oxidative stress in mice. J. Biol. Chem. 280, 16417–16426 (2005).
Ishikawa, K. et al. Subcutaneous fat modulates insulin sensitivity in mice by regulating TNF-alpha expression in visceral fat. Horm. Metab. Res. 38, 631–638 (2006).
Rodbell, M. Metabolism of isolated fat cells. I. Effects of hormones on glucose metabolism and lipolysis. J. Biol. Chem. 239, 375–380 (1964).
Hagio, M., Matsumoto, M., Fukushima, M., Hara, H. & Ishizuka, S. Improved analysis of bile acids in tissues and intestinal contents of rats using LC/ESI-MS. J. Lipid Res. 50, 173–180 (2009).
Muto, A. et al. Detection of Delta4-3-oxo-steroid 5beta-reductase deficiency by LC-ESI-MS/MS measurement of urinary bile acids. J. Chromatogr. B. Analyt. Technol. Biomed. Life Sci. 900, 24–31 (2012).
Acknowledgements
We thank Sawako Suzuki (Chiba University) and Hideaki Bujo (Toho University) for helpful advice during the course of the study. This work was supported by Grant-in-Aid from the Ministry of Education, Science, Sports and Culture of Japan (23700900 to EY. L. and 25293051 to T.M.). Vidal-Puig lab is supported by MRC, BHF and EU 2020 EpoS grant.
Author information
Authors and Affiliations
Contributions
EY.L. designed and performed experiments, analyzed data and wrote the manuscript. K.S. analyzed and discussed data and wrote the manuscript. X.Z. helped with in vivo experiments. C.T. measured oxygen consumption. T.T. helped with qPCR analysis. M.J. helped with fat transplantation. T.S. provided the experimental materials. K.T. and K.Y. discussed data. A.V-P. and Y.M. analyzed and discussed data and wrote the manuscript. T.M. designed experiments, performed experiments, analyzed data and wrote the manuscript. T.M. is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Lee, E., Sakurai, K., Zhang, X. et al. Unsuppressed lipolysis in adipocytes is linked with enhanced gluconeogenesis and altered bile acid physiology in InsrP1195L/+ mice fed high-fat-diet. Sci Rep 5, 17565 (2015). https://doi.org/10.1038/srep17565
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep17565
This article is cited by
-
Altered glucose metabolism and insulin resistance in cancer-induced cachexia: a sweet poison
Pharmacological Reports (2021)
-
Sequential Exposure to Obesogenic Factors in Females Rats: From Physiological Changes to Lipid Metabolism in Liver and Mesenteric Adipose Tissue
Scientific Reports (2017)
-
Eicosapentaenoic acid ameliorates hyperglycemia in high-fat diet-sensitive diabetes mice in conjunction with restoration of hypoadiponectinemia
Nutrition & Diabetes (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.