Abstract
Acupuncture and related therapies such as moxibustion and transcutaneous electrical nerve stimulation are often used to manage cancer-related symptoms, but their effectiveness and safety are controversial. We conducted this overview to summarise the evidence on acupuncture for palliative care of cancer. Our systematic review synthesised the results from clinical trials of patients with any type of cancer. The methodological quality of the 23 systematic reviews in this overview, assessed using the Methodological Quality of Systematic Reviews Instrument, was found to be satisfactory. There is evidence for the therapeutic effects of acupuncture for the management of cancer-related fatigue, chemotherapy-induced nausea and vomiting and leucopenia in patients with cancer. There is conflicting evidence regarding the treatment of cancer-related pain, hot flashes and hiccups and improving patients’ quality of life. The available evidence is currently insufficient to support or refute the potential of acupuncture and related therapies in the management of xerostomia, dyspnea and lymphedema and in the improvement of psychological well-being. No serious adverse effects were reported in any study. Because acupuncture appears to be relatively safe, it could be considered as a complementary form of palliative care for cancer, especially for clinical problems for which conventional care options are limited.
Similar content being viewed by others
Introduction
Cancer is a major cause of disease burden worldwide. According to estimates from the International Agency for Research of Cancer1, the global adult population in 2012 included 14.1 million new cancer cases, 32.6 million existing cancer patients who had received a diagnosis within the previous 5 years and 8.2 million cancer deaths, accounting for 14.7% of all deaths. The incidence of cancer continues to increase. It is predicted that in 2035, approximately 24.0 million new cancer cases will be diagnosed and 14.6 million deaths will be attributable to cancer. This increasing cancer incidence and the continual improvement in cancer treatment will lead to an increase in the number of patients living with cancer. This will mandate progress in palliative care strategies for the control of symptoms related to cancer itself, as well as symptoms induced by cancer therapies.
According to the World Health Organisation2, palliative care is an approach that aims to improve the quality of life (QoL) of patients with life-threatening illnesses by relieving pain, distressing symptoms or other side effects related to treatment. Unlike the traditional concept of confining palliative care to the last 6 months of life, the current model recommended by the US National Comprehensive Cancer Network extends palliative care across the entire disease trajectory. Based on this concept, cancer palliative care focuses not only on the treatment of cancer-related symptoms such as pain, fatigue and insomnia, but also on relief of the side effects of chemotherapy or radiotherapy such as nausea, vomiting, leukopenia and xerostomia3. This shift in the treatment model is partly related to the failure of aggressive care such as prolonged hospitalisation or intensive care unit admission to increase the life expectancy or improve the QoL of patients with incurable cancer4.
Acupuncture is one of the major treatment methods in traditional Chinese medicine. Related therapies such as moxibustion and transcutaneous electrical nerve stimulation (TENS) are also often used separately or in combination with acupuncture. These therapies are widely used for supportive and palliative care of patients with cancer5. The existing systematic reviews (SRs) have summarised the evidence on the use of acupuncture and related therapies for the management of various cancer-related symptoms, including nausea and vomiting6,7, cancer-related pain (CRP)7,8 and fatigue7,9. These SRs have drawn contradictory conclusions. For example, Posadzki and colleagues9 reviewed seven randomised controlled trials (RCTs) that assessed the effectiveness of acupuncture and related therapies in the treatment of cancer-related fatigue (CRF) and concluded that the risk of bias (RoB) amongst the included RCTs was too high for any reliable conclusions to be drawn. In contrast, another SR7 suggested that acupuncture is useful for the reduction of fatigue on the basis of one well-designed RCT. The disagreement amongst these four SRs could be attributed to differences in their inclusion and exclusion criteria, search strategies, databases and search periods.
The contradictory results of these individual SRs make it difficult to draw conclusions on the potential effectiveness of acupuncture and related therapies. An overview of the existing SRs is needed to provide an update on all synthesised clinical evidence on acupuncture and related therapies for palliative cancer care10. Although such an overview11 has already been conducted, its trustworthiness is limited for the following reasons: first, the search dates were limited to 2000 to 2011; hence, SRs published outside this time frame, including those published or updated since8,9,12,13,14, were not included. Second, the search strategy of the previous overview did not include Chinese-language databases, which may have led to the omission of clinical evidence15. Third, the methodological quality of the included SRs was not appraised with a validated instrument16, which limits the interpretation of their overall trustworthiness.
To overcome these limitations, we conducted an up-to-date overview of SRs to evaluate the methodological quality of SRs and meta-analyses of acupuncture for management of symptoms for palliative care of cancer and to describe the clinical evidence reported in these SRs and meta-analyses.
Results
SR search and screening results
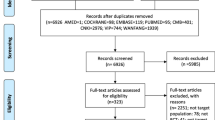
The database search strategies yielded 236 records and 37 duplicates were identified and excluded. We excluded 168 citations after screening the titles and abstracts; thus, the full texts of the remaining 31 citations were retrieved for further assessment. Nine publications were excluded for the following reasons: two included patients with and without cancer and did not report the cancer-specific results separately, three were not SRs, three did not report the results of acupuncture and related therapies separately from those of other treatments and one was an early version of an updated SR. After this process, 22 SRs met the inclusion criteria. We further identified one additional SR by checking the reference list of a previous overview11. The other nine SRs included in that overview11 had already been identified by the literature search. Thus, a total of 23 SRs were included in this overview. Details of the literature search and selection can be found in Fig. 1.
Characteristics of included SRs
The 23 SRs were published between 2005 and 2014 and 14 (60.9%) of them were published after 2012. This overview includes 14 new SRs that were not included in the previous overview. Of the 22 SRs that provided a cut-off date on their literature search, 12 (55.0%) conducted their literature search after 2011 (i.e., after the publication of the previous overview11).
Overall, these SRs reported the results from 248 primary studies (median, 7) and 17,392 patients (median, 548). Three SRs (13.0%) were published in Chinese and the rest were written in English. Three (13.0%) were Cochrane SRs. Thirteen (56.5%) SRs included only RCTs and the rest included multiple study designs, including both clinical trials and observational studies. Seventeen (73.9%) of the SRs covered various types of cancer. Three SRs focused on patients with breast cancer6,7,17 and three other SRs summarised only evidence on patients with prostate cancer18, head and neck cancer19 and lung cancer20. Eleven SRs6,7,14,18,20,21,22,23,24,25,26 included any type of acupuncture or related therapy either with or without needle insertion. Nine SRs8,9,12,17,19,27,28,29,30 included only acupuncture with needle insertion and excluded other forms of related therapy, including TENS, laser acupuncture, acupressure and moxibustion. The remaining three SRs focused only on one particular form of acupuncture or related therapy, including TENS13, moxibustion31 and acupoint injection32.
Sixteen SRs summarised the evidence on a single outcome, including CRP8,13,21,22,26,27, fatigue9,24,31, hot flashes17,18, chemotherapy-induced nausea and vomiting (CINV)14,20, hiccups29 and irradiation-induced xerostomia19. The remaining seven SRs6,7,12,20,28,30,32 reported evidence on a wide range of outcomes in the palliative care of patients with cancer. The characteristics of these SRs can be found in Tables 1, 2, 3. Table 1 describes the SRs that included only RCTs on needle acupuncture. Table 2 reports the SRs that included RCTs that focused on acupuncture-related therapies. Table 3 highlights the SRs that included results from various study designs on both needle acupuncture and related therapies. The methodological quality of the included SRs as assessed by the Methodological Quality of Systematic Reviews (AMSTAR) is shown in Table 4 and Appendix 3. The corresponding results from these SRs can be found in Tables 5, 6, 7 and are supplemented with quantitative results reported in Appendix 4.
Methodological quality of included SRs
All of the SRs conducted a comprehensive literature search (AMSTAR Item 3). Twenty-two (95.7%) assessed the scientific quality of the included studies (AMSTAR Item 7). Only five (21.7%) provided an a priori design to the SRs (AMSTAR Item 1). Although all of the SRs provided references to the included studies, only six (26.1%) provided lists of both included and excluded studies (AMSTAR Item 5). None of the SRs stated any conflict of interest on the included studies as well as on the SR itself (AMSTAR Item 11). Only 13 SRs (56.5%) included conflict of interest of the SR itself (AMSTAR Item 11). Of the 11 SRs that conducted meta-analyses, eight (81.8%) used appropriate statistical methods to combine the study findings (AMSTAR Item 9), but none assessed the likelihood of publication bias (AMSTAR Item 10). The details can be found in Table 4 and Appendix 3.
Effectiveness of acupuncture and related therapies
Cancer-related pain
Ten SRs6,7,8,12,13,21,22,26,27,32 synthesised clinical evidence on the use of acupuncture and related therapies in the reduction of CRP, of which only two22,26 conducted a meta-analysis (Table 7, Appendix 4). Zheng and colleagues26 included five studies (395 patients) that evaluated the effectiveness of wrist-ankle acupuncture on the symptom improvement rate. Their results showed no statistical differences in the symptom improvement rate between wrist-ankle acupuncture plus conventional care and conventional care alone (pooled risk ratio [RR], 1.12; 95% confidence interval [CI], 0.92 to 1.36). Choi and colleagues22 summarised evidence from various forms of acupuncture and related therapies and their synthesised results showed that acupuncture and related therapies plus conventional care had a slightly stronger effect in the reduction of CRP (pooled RR, 1.36; 95% CI, 1.13 to 1.64) than conventional care alone. However, no statistical differences were found in the response rates of acupuncture and related therapies and those of conventional analgesic treatment (pooled RR, 1.12; 95% CI, 0.98 to 1.28). No significant difference was seen in the pain score between acupuncture (including auricular acupuncture and electro-acupuncture) and sham acupuncture (pooled standard mean difference [SMD], –0.41; 95% CI, –1.39 to 0.49).
Meta-analysis was not conducted in the other SRs6,7,8,13,21,27,32 (Tables 5, 6, 7 and Appendix 4). Three SRs8,21,27 (Tables 5 and 7 and Appendix 4) identified one RCT with a low RoB and mentioned that auricular acupuncture provided statistically significant relief on CRP when compared with sham acupuncture.
Cancer-related fatigue
Five SRs7,9,24,28,31 summarised evidence on the effectiveness of acupuncture and related therapies in the treatment of CRF and two conducted meta-analyses (Tables 5, 6, 7 and Appendix 4). Zeng and colleagues28 assessed the effectiveness of acupuncture for CRF in various types of cancer patients (Table 5 and Appendix 4). Four meta-analyses were conducted for different comparisons and all results showed a reduction of CRF with acupuncture. However, only one meta-analysis showed that acupuncture plus education could significantly reduce CRF in cancer patients when compared to conventional care (two RCTs; pooled SMD, –2.12; 95% CI, –3.21 to –1.03). One of the pooled RCTs provided information on the net benefit of acupuncture. In this trial, acupuncture plus conventional care was compared with conventional care alone; the mean difference was –2.52 (95% CI, –2.85 to –2.19). However, the validity of these results was compromised because the two RCTs did not implement allocation concealment and blinding.
Another SR31 investigated the effects of moxibustion on CRF (Table 6 and Appendix 4). The pooled results demonstrated that moxibustion plus conventional care could significantly improve CRF over conventional care alone (pooled RR, 1.73; 95% CI, 1.29 to 2.32), but it is uncertain whether the outcomes were assessed with validated scales. Readers should note that all four trials included in this meta-analysis had poor reporting quality, so their RoB was unclear.
Hot flashes
Five SRs6,7,17,18,25 summarised evidence on acupuncture and related therapies for the treatment of hot flashes in patients with breast cancer6,7,17, prostate cancer18, or both25 (Tables 5 and 7 and Appendix 4). Only one study17 conducted a meta-analysis to compare acupuncture with sham acupuncture (Table 5 and Appendix 4). The results favoured acupuncture in the reduction of the frequency of hot flashes during treatment (pooled weighted mean difference [WMD], 1.91; 95% CI, 0.10 to 3.71). However, this difference was attenuated after treatment (pooled WMD, 3.09; 95% CI, –0.04 to 6.23). In contrast, one SR28 investigated the long-term effects of acupuncture (3 to 21 months of follow-up) and concluded that its benefits could be sustained for at least 3 months in women with breast cancer and in men with prostate cancer (Table 5 and Appendix 4).
Nausea and vomiting
Six SRs6,7,14,20,30,32 synthesised evidence on the effectiveness of acupuncture and related therapies on CINV (Tables 5, 6, 7 and Appendix 4). Four14,20,30,32 SRs conducted meta-analyses. Two20,32 reported that the results of acupuncture and related therapies for CINV were better than those of the control group (no details on the control intervention were provided). Another SR14 found that acupuncture could reduce the proportion of patients who experienced acute vomiting but did not reduce the mean number of delayed vomiting episodes or the severity of acute or delayed nausea. The remaining SR30 suggested that acupuncture and conventional medications had similar effects in the reduction of CINV, but this conclusion was based on a single RCT with an unclear RoB.
Quality of life
Four SRs12,20,28,32 synthesised evidence on the effectiveness of acupuncture and related therapies for improving cancer patients’ QoL (Tables 5, 6 and Appendix 4). Two SRs20,28 conducted meta-analyses; one20 reported that acupuncture improves QoL in patients with lung cancer when compared to conventional care alone (pooled SMD, 0.47; 95% CI, 0.04 to 0.90), but the other28 found no favourable effects of acupuncture when compared to sham acupuncture (pooled SMD, 0.99; 95% CI, –0.70 to 2.68). The results of the two SRs12,32 that narratively summarised the results of the included RCTs described the favourable effects of acupuncture and related therapies in improving QoL when compared with conventional care or chemotherapy alone. It should be highlighted that only one SR12 reported a low RoB for all included trials and the other three SRs12,20,32 did not provide details on the RoB of the included studies.
Leucopenia
Two SRs6,23 summarised the effectiveness of acupuncture and related therapies in the reversal of cancer treatment–induced leucopenia (Table 7 and Appendix 4). One SR23 focused on chemotherapy-induced leucopenia and the results of the meta-analysis demonstrated that acupuncture promoted an increase in the white blood cell count (pooled WMD, 1.22; 95% CI, 0.64 to 1.81). The other SR6 reported a positive effect on radiotherapy-induced leucopenia, but this conclusion was supported by only one small case series with seven patients.
Lymphedema
Two SRs6,7 reported the results from one case series study, which concluded that acupuncture was effective in reducing lymphedema related to breast cancer. It was mentioned that the patients experienced significant improvement in their range of movements for shoulder flexion and abduction of the affected limb. Attention should be paid to the lack of a control group and the small sample size (29 patients) in this study (Table 7 and Appendix 4).
Hiccups
Choi and colleagues29 reviewed the effectiveness of needle or electro-acupuncture in the relief of hiccups in cancer patients (Table 5 and Appendix 4). Their meta-analysis showed that acupuncture can significantly reduce hiccups (pooled RR, 1.87; 95% CI, 1.26 to 2.78) when compared with conventional care alone. It should be noted that all three included studies had unclear RoB and that the reliability of the outcome measurement approaches were doubtful.
Xerostomia
An SR19 assessed the effectiveness of needle or electro-acupuncture for the treatment of irradiation-induced xerostomia in patients with head and neck cancer (Table 7 and Appendix 4). All three trials reported a significant reduction in xerostomia compared to baseline salivary flow rates after acupuncture or sham acupuncture. There was no significant difference between the acupuncture and sham acupuncture groups.
Dyspnea
Dos Santos and colleagues7 identified one RCT with a low RoB that evaluated the effects of acupuncture in the treatment of dyspnea in patients with breast cancer (Table 7 and Appendix 4). Patients in both the acupuncture and sham acupuncture groups showed statistically significant improvement in their dyspnea scores immediately after treatment. Although the improvement was slightly greater in the acupuncture group, it was not significantly different from the sham acupuncture group.
Psychological well-being
The effect of acupuncture on psychological well-being was discussed in two SRs7,28; however, neither found any significant beneficial effect of acupuncture when compared to a control group.
Adverse effects of acupuncture and related therapies
Of the 23 SRs, six7,8,20,21,24,25 did not describe any information on adverse events, two23,29 reported that the included studies did not mention any adverse events and two22,30 mentioned that all of the included studies reported no adverse events. The remaining 13 SRs6,9,12,13,14,17,18,19,26,27,28,31,32 reported adverse events that were attributable to acupuncture and related therapies. A wide range of minor adverse events was reported, which including bleeding at the acupuncture site, skin irritation, discomfort, transient rash, electrical shock sensation and tingling. There were no reports of serious AE that required medical management.
Discussion
This updated overview of 23 SRs summarised the clinical evidence on the effectiveness of acupuncture in palliative care for cancer from 248 primary studies that included 17,392 participants. The effects of acupuncture on 12 outcomes that are highly relevant to palliative care of cancer, including CRP, CRF, hot flashes, vomiting and nausea, QoL, leucopenia, lymphedema, hiccups, xerostomia, dyspnea, psychological well-being and adverse events, were synthesised. Compared to the previous overview11, we identified and reported results from 14 additional, updated SRs. The clinical evidence from this overview suggests that acupuncture and related therapies are likely to be effective in improving CRF, CINV and leucopenia. In the context of current best practice, acupuncture and related therapies may be considered as additional treatments to the guideline-recommended treatment with glucocorticoids, 5-HT3 antagonists and/or NK1R antagonists in patients with moderate or high risk of emesis33. For leucopenia, antibacterial and antifungal prophylaxis are currently not recommended for patients with solid tumors who are undergoing conventional chemotherapy34. Acupuncture and related therapies may serve as an alternative prophylaxis, with a therapeutic goal of reducing the duration of neutropenia (absolute neutrophil count of less than 1500 cells/μL) to less than 7 days. Finally, acupuncture and related therapies can be considered as an adjunct in patients who experience persistent CRF after they receive first-line treatment. Such application is of high clinical relevance because it is well acknowledged that management of CRF is often suboptimal35. Although one SR demonstrated the effectiveness of acupuncture in the management of chronic pain36, we identified conflicting results on the effectiveness of acupuncture and related therapies in the management of CRP. Conflicting results were also found in the treatment of hot flashes and hiccups and in the improvement of QoL. No adequately powered, well-designed RCT has been performed to clarify the potential role of acupuncture and related therapies in the management of xerostomia, dyspnea, lymphedema and psychological well-being. Future trials should focus on these under-investigated areas.
Although the application of acupuncture and related therapies in the management of CRF, CINV and leucopenia is supported by results from RCTs, the reporting quality of these studies is often poor, which hindered us from assessing the RoB in these RCTs and future confirmatory trials should adhere to CONSORT recommendations for reporting. Researchers should also adopt a comparative effectiveness approach and design trials that allow real-world evaluation of acupuncture and related therapies. Specifically, the combined effects of acupuncture and related therapies in addition to guideline-recommended conventional care (e.g., glucocorticoids, 5-HT3 antagonists and/or NK1R antagonists in CINV) should be compared with conventional care alone so that the additional benefits of acupuncture can be elucidated37. Although this approach can make the choice of control intervention more straightforward, the design of a treatment protocol for acupuncture and related therapies is more challenging because it includes a wide variety of techniques38. Different researchers may use different techniques and in other cases the treatment protocol can be individualised according to Chinese medicine diagnostic principles. Such variation is reflected in the included SRs–many adopted a less-restrictive approach and embraced various techniques6,7,8,9,14,18,20,21,22,23,25, whereas others focused only on a single technique such as moxibustion31 and TENS13. As a result, the meta-analyses often pooled trials with highly heterogeneous acupuncture and control interventions14,23, which makes interpretation of their results very difficult. Network meta-analysis39 could be a solution that takes into account the heterogeneity amongst treatments in both groups. Unfortunately, the exact intervention protocols used in trials are often not reported31, which prevented us from performing such an analysis. Finally, the interpretability of the reported results is also limited because of the wide variations in the choice of outcome measures. For example, pain was measured with a visual analogue scale in some primary studies, but in others it was reported as a binary response rate22. Future trials should choose the most clinically relevant endpoint as the primary outcome40 and measure it using a validated method11 so as to ensure the utility of future clinical evidence41.
When deciding on the scope of this overview, we tried to balance the need to reduce heterogeneity at the intervention level on the one hand and the need to ensure appropriate reflection of real clinical practice on the other. Although focusing exclusively on needle acupuncture may facilitate understanding of the effects of a single style of acupuncture, failure to report results from other related therapies may also reduce the comprehensiveness of this overview42. From a pragmatic perspective, a combination of needle acupuncture and related therapies such as moxibustion43 or TENS44 is often used in everyday clinical practice. In addition to treatment heterogeneity, the inclusion criteria in the original study design amongst SRs also requires a balance between reporting only the best available evidence from RCTs and taking a more inclusive approach to ensure comprehensiveness. Although the RCT is the best study design to provide evidence on effectiveness, the results from studies with weaker designs may inform the planning of future RCTs45, of which both are valuable from research and clinical practice perspectives. To make this overview informative for clinicians and researchers, we set broad inclusion criteria so that all available evidence on needle acupuncture and related therapies was presented46,47, but the data are separated according to the type of treatment and study design.
The methodological quality of the SRs included in this overview was satisfactory. Good performance in the following areas was noted: conducting duplicate study selection and data extraction, implementing comprehensive literature search, assessing the scientific quality of included studies and appropriately incorporating scientific quality in the formulation of conclusions. At the same time, improvements should be made in the following areas.
-
(i) The provision of an a priori design for the SRs would reduce the potential bias from reviewers, increase the SR’s transparency and prevent duplicate work on the same topic10.
-
(ii) Listing both included and excluded studies would ensure comprehensive reporting of SRs and allow readers to examine the excluded studies if they had a different perspective on eligibility criteria10.
-
(iii) Assessing the publication bias of included studies would inform readers on whether the results were generated from an unbiased sample of related studies10.
-
(iv) Clarifying conflicts of interest is important because it is well known that financial support might introduce bias to the SR process48.
In conclusion, acupuncture and related therapies have demonstrated favourable therapeutic effects in the management of CRF, CINV and leucopenia in cancer patients. Conflicting evidence exists for the treatment of CRP, hot flashes and hiccups and in the improvement of QoL. The currently available evidence is insufficient to support or refute the potential of acupuncture and related therapies in the management of xerostomia, dyspnea and lymphedema and in the improvement of psychological well-being. No serious adverse effects were reported in the included studies, consistent with the results of previous SRs that concluded that acupuncture is a relatively safe treatment option49,50. Future comparative effectiveness research in this area should pay attention to:
-
(i) improving the reporting and methodological quality of trials;
-
(ii) developing an acupuncture treatment protocol using an expert consensus technique, taking into account regulatory requirements and the constraints of the practice setting;
-
(iii) describing the treatment protocol according to the STRICTA51 and TIDieR checklist52, so that the procedure can be replicated in other trials or be adopted into clinical practice if it is found to be effective; and
-
(iv) choosing guideline-recommended treatment for the control group and validating outcome measures.
Methods
Criteria for considering reviews for inclusion
The Cochrane handbook version 5.1.0.10 states that an SR should aim to ‘identify, appraise and synthesise all the empirical evidence that meets pre-specified eligibility criteria to answer a given research question’. Following this definition, we judged a publication as an SR if it sought to answer an explicit clinical question by examining evidence from at least two electronic databases. In this overview, any SRs (including both Cochrane SRs and non-Cochrane SRs) that summarised clinical evidence on the effectiveness of acupuncture and related therapies for palliative care of cancer were considered eligible. If an SR summarised evidence on multiple palliative care techniques, those that reported evidence on acupuncture and related therapies separately were also included.
Participants
To be eligible, the SRs had to include clinical trials that recruited patients with a diagnosis of any type of cancer who have received acupuncture and related therapies for supportive or palliative care.
Interventions & control treatments
Any form of acupuncture was considered in this overview. We included SRs that summarised evidence on invasive acupuncture (including needle acupuncture, electro-acupuncture and auricular acupuncture) and non-invasive techniques such as laser acupuncture or acupressure. We also included acupoint injection, moxibustion and TENS. For control treatments, we included SRs that summarised studies that included any type of intervention without acupuncture or the related treatments described above. These interventions included conventional treatment, behavioural therapy, Chinese herbal medicine treatment, sham acupuncture, addition to a waiting list or no treatment.
Outcomes of interest
We summarised all reported cancer-related or treatment-related outcomes in this overview to provide a comprehensive picture of the available clinical evidence on acupuncture and related therapies for palliative care of cancer.
Literature search
We searched four international databases (MEDLINE, EMBASE, the Cochrane Database of Systematic Reviews and the Database of Abstracts of Reviews of Effect ) and three Chinese databases (Chinese Biomedical Databases, Wan Fang Digital Journals and Taiwan Periodical Literature Databases) from their inception through July 2014 to identify potential SRs. For MEDLINE and EMBASE, a specialised search filter for SR articles was used53,54. Comprehensive searches of each database with a full Boolean search strategy were conducted and the details are reported in Appendix 1.
Literature selection, data extraction and methodological quality assessment
The citations retrieved from the databases were independently screened and assessed for eligibility by two researchers (XY, RH); disagreements were resolved by discussion and consensus. If a disagreement could not be resolved, a third reviewer (VC) was invited to make a judgment. For duplicate publications, the most updated version was selected.
The following data were extracted from each eligible SR: (i) basic characteristics, including eligibility criteria, designs of included studies, number of included studies, total number of patients and bibliographic information; (ii) details on patients, interventions, controls and outcomes; (iii) synthesised results, including pooled summary effects of each comparison for each outcome if meta-analysis were conducted.
The methodological quality of the included SRs was assessed with the validated Methodological Quality of Systematic Reviews (AMSTAR)55 instrument. A detailed operational guide for AMSTAR can be found in Appendix 2. Data extraction and methodological quality assessment were conducted independently by two researchers; disagreements were resolved by discussion and consensus. Any unresolved discrepancies were judged by a third reviewer.
Data synthesis
The clinical evidence reported in the included SRs was synthesised narratively under each outcome. The effects on dichotomous data were summarised with the pooled RR, which measures the risk of a certain outcome in the treatment group as compared to the risk in the control group across trials. The pooled SMD or WMD was used for continuous outcomes. The SMD was used if a variety of measurement methods were used for the same outcome and the WMD was used when the outcome was measured with the same method. The protocol of this overview has been registered in PROSPERO (http://www.crd.york.ac.uk/PROSPERO/DisplayPDF.php?ID=CRD42014015576).
Additional Information
How to cite this article: Wu, X. et al. Effectiveness of acupuncture and related therapies for palliative care of cancer: overview of systematic reviews. Sci. Rep. 5, 16776; doi: 10.1038/srep16776 (2015).
References
International Agency for Research on Cancer, GLOBOCAN 2012: Estimated Cancer Incidence, Mortality and Prevalence Worldwide in 2012. (2012) Available at: http://globocan.iarc.fr/Pages/fact_sheets_population.aspx. (Accessed: 9th November 2014).
World Health Organization, WHO Definition of Palliative Care. Available at: http://www.who.int/cancer/palliative/definition/en/. (Accessed: 9th November 2014).
Levy, M. H. et al. NCCN clinical practice guidelines in oncology: palliative care. J Natl Compr Canc Netw 7, 436–473 (2009).
Anonymous. Too much treatment? Aggressive medical care can lead to more pain, with no gain. Consum Rep 73, 40–44 (2008).
Lu, W. D., Dean-Clower, E., Doherty-Gilman, A. & Rosenthal, D. S. The Value of Acupuncture in Cancer Care. Hematol Oncol Clin North Am 22, 631–648, doi: 10.1016/j.hoc.2008.04.005 (2008).
Chao, L. F. et al. The efficacy of acupoint stimulation for the management of therapy-related adverse events in patients with breast cancer: a systematic review. Breast Cancer Res Treat 118, 255–267, doi: 10.1007/s10549-009-0533-8 (2009).
Dos-Santos, S. et al. Acupuncture for Treating Common Side Effects Associated With Breast Cancer Treatment: A Systematic Review. Medical Acupuncture 22, 81–97, doi: 10.1089/acu.2009.0730 (2010).
Paley, C. A., Johnson, M. I., Tashani, O. A. & Bagnall, A. Acupuncture for cancer pain in adults. Cochrane Database Syst Rev, CD007753, doi: 10.1002/14651858.CD007753.pub2 (2011).
Posadzki, P. et al. Acupuncture for cancer-related fatigue: a systematic review of randomized clinical trials. Support care cancer : official journal of the Multinational Association of Supportive Care in Cancer 21, 2067–2073, doi: 10.1007/s00520-013-1765-z (2013).
Higgins, J. & Green, S., Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. (2011) Available at: www.cochrane-handbook.org. (Accessed: 9th November 2014).
Towler, P., Molassiotis, A. & Brearley, S. G. What is the evidence for the use of acupuncture as an intervention for symptom management in cancer supportive and palliative care: an integrative overview of reviews. Support care 21, 2913–2923, doi: 10.1007/s00520-013-1882-8 (2013).
Lian, W. L., Pan, M. Q., Zhou, D. H. & Zhang, Z. J. Effectiveness of acupuncture for palliative care in cancer patients: A systematic review. Chin J Integr Med 20, 136–147, doi: 10.1007/s11655-013-1439-1 (2014).
Hurlow, A. et al. Transcutaneous electric nerve stimulation (TENS) for cancer pain in adults. Cochrane Database Syst Rev 3, CD006276, doi: 10.1002/14651858.CD006276.pub3 (2012).
Ezzo, J. et al. Acupuncture-point stimulation for chemotherapy-induced nausea or vomiting. Cochrane Database Syst Rev, CD002285, doi: 10.1002/14651858.CD002285.pub2 (2014).
Wu, X. Y. et al. Systematic reviews and meta-analyses of traditional chinese medicine must search chinese databases to reduce language bias. Evid Based Complement Alternat Med 2013, 812179, doi: 10.1155/2013/812179 (2013).
Critical Appraisal Skills Programme. 10 Questions to help you make sense of reviews. Available at: www.sph.nhs/sph-files/casp. (Accessed: 9th November 2014).
Lee, M., Kim, K. H., Choi, S. M. & Ernst, E. Acupuncture for treating hot flashes in breast cancer patients: a systematic review. Breast Cancer Res Treat 115, 497–503, doi: 10.1007/s10549-008-0230-z (2009).
Lee, M., Kim, K. H., Shin, B. C., Choi, S. M. & Ernst, E. Acupuncture for treating hot flushes in men with prostate cancer: a systematic review. Support care 17, 763–770, doi: 10.1007/s00520-009-0589-3 (2009).
O’Sullivan, E. M. & Higginson, I. J. Clinical effectiveness and safety of acupuncture in the treatment of irradiation-induced xerostomia in patients with head and neck cancer: a systematic review. Acupunct Med 28, 191–199, doi: 10.1136/aim.2010.002733 (2010).
Chen, H. Y., Li, S. G., Cho, W. C. S. & Zhang, Z. J. The role of acupoint stimulation as an adjunct therapy for lung cancer: A systematic review and meta-analysis. BMC Complem Altern M 13, doi: 10.1186/1472-6882-13-362 (2013).
Peng, H., Peng, H. D., Xu, L. & Lao, L. X. Efficacy of acupuncture in treatment of cancer pain: a systematic review Journal of Chinese Integrative Medicine [Chinese] 8, 501–509, doi: 10.3736/jcim20100601 (2010).
Choi, T. Y., Lee, M. S., Kim, T. H., Zaslawski, C. & Ernst, E. Acupuncture for the treatment of cancer pain: a systematic review of randomised clinical trials. Support care cancer 20, 1147–1158, doi: 10.1007/s00520-012-1432-9 (2012).
Lu, W. et al. Acupuncture for chemotherapy-induced leukopenia: exploratory meta-analysis of randomized controlled trials. J Soc Integr Oncol 5, 1–10 (2007).
Finnegan-John, J., Molassiotis, A., Richardson, A. & Ream, E. A systematic review of complementary and alternative medicine interventions for the management of cancer-related fatigue. Integr Cancer Ther 12, 276–290, doi: 10.1177/1534735413485816 (2013).
Frisk, J. W., Hammar, M. L., Ingvar, M. & Spetz Holm, A. C. E. How long do the effects of acupuncture on hot flashes persist in cancer patients? Support care 22, 1409–1415, doi: 10.1007/s00520-014-2126-2 (2014).
Zheng, Y., Yu, Y. H. & Fang, F. F. Meta-Analysis on Wrist-Ankle Acupuncture of Cancerous Pain. Jouranl of Liaoning University of TCM [Chinese] 16, 152–155 (2014).
Lee, H., Schmidt, K. & Ernst, E. Acupuncture for the relief of cancer-related pain–A systematic review. Eur J Pain 9, 437–444, doi: 10.1016/j.ejpain.2004.10.004 (2005).
Zeng, Y., Luo, T., Finnegan-John, J. & Cheng, A. S. K. Meta-analysis of randomized controlled trials of acupuncture for cancer-related fatigue. Integr Cancer Ther 13, 193–200, doi: 10.1177/1534735413510024 (2013).
Choi, T. Y., Lee, M. S. & Ernst, E. Acupuncture for cancer patients suffering from hiccups: A systematic review and meta-analysis. Complement Ther Med 20, 447–455, doi: 10.1016/j.ctim.2012.07.007 (2012).
Pu, H. h., Yu, T., Gao, X. & Mao, J. J. Systematic Evaluation on Clinical Therapetic Effect of Acupuncture for Treatmen of Gastrointestinal Untoward Reaction by Malignant Tumor Chemotherapy. Lishizhen Medicine and Materia Medica Research [Chinese] 21, 1476–1480, doi: 10.3969/j.issn.1008-0805.2010.06.087 (2010).
Lee, S. et al. The effectiveness and safety of moxibustion for treating cancer-related fatigue: A systematic review and meta-analyses. Support care cancer 22, 1429–1440, doi: 10.1007/s00520-014-2161-z (2014).
Cheon, S. et al. Pharmacopuncture for cancer care: A systematic review. Evid Based Complement Alternat Med 2014, 1–14, doi: 10.1155/2014/804746 (2014).
Basch, E. et al. Antiemetics: American Society of Clinical Oncology Clinical Practice Guideline Update. J Clin Oncol 29, 4189–4198, doi: 10.1200/jco.2010.34.4614 (2011).
Bow, E. Treatment and prevention of neutropenic fever syndromes in adult cancer patients at low risk for complications. (2014) Available at: http://www.uptodate.com/contents/treatment-and-prevention-of-neutropenic-fever-syndromes-in-adult-cancer-patients-at-low-risk-for-complications. (Accessed: 9th November 2014).
Koornstra, R. H. T., Peters, M., Donofrio, S., van den Borne, B. & de Jong, F. A. Management of fatigue in patients with cancer–A practical overview. Cancer Treat Rev 40, 791–799, doi: 10.1016/j.ctrv.2014.01.004 (2014).
Vickers, A. J. et al. Acupuncture for chronic pain: Individual patient data meta-analysis. Arch Intern Med 172, 1444–1453, doi: 10.1001/archinternmed.2012.3654 (2012).
Witt, C. et al. Effectiveness guidance document (EGD) for acupuncture research–a consensus document for conducting trials. BMC Complem Altern M 12, 148, doi: 10.1186/1472-6882-12-148 (2012).
Anonymous. NIH Consensus Conference. Acupuncture. JAMA 280, 1518–1524, doi: 10.1001/jama.280.17.1518 (1998).
Cipriani, A., Higgins, J. P. T., Geddes, J. R. & Salanti, G. Conceptual and Technical Challenges in Network Meta-analysis. Ann Intern Med 159, 130–137, doi: 10.7326/0003-4819-159-2-201307160-00008 (2013).
Gargon, E. et al. Choosing Important Health Outcomes for Comparative Effectiveness Research: A Systematic Review. PLoS ONE 9, e99111, doi: 10.1371/journal.pone.0099111 (2014).
Coster, W. J. Making the Best Match: Selecting Outcome Measures for Clinical Trials and Outcome Studies. Am J Occup Ther 67, 162–170, doi: 10.5014/ajot.2013.006015 (2013).
Loudon, K. et al. The PRECIS-2 tool: designing trials that are fit for purpose. BMJ 350, h2147, doi: 10.1136/bmj.h2147 (2015).
Joos, S. et al. Acupuncture and moxibustion in the treatment of ulcerative colitis: A randomized controlled study. Scand J Gastroenterol 41, 1056–1063, doi: d10.1080/00365520600580688 (2006).
Itoh, K., Hirota, S., Katsumi, Y., Ochi, H. & Kitakoji, H. A pilot study on using acupuncture and transcutaneous electrical nerve stimulation (TENS) to treat knee osteoarthritis (OA). Chin Med 3, 2, doi: 10.1186/1749-8546-3-2 (2008).
Noordzij, M. et al. Sample size calculations: basic principles and common pitfalls. Nephrol Dial Transplant 25, 1388–1393, doi: 10.1093/ndt/gfp732 (2010).
Haidich, A.B., Pilalas, D., Contopoulos-Ioannidis, D. G. & Ioannidis, J. P. A. Most meta-analyses of drug interventions have narrow scopes and many focus on specific agents. J Clin Epidemiol 66, 371–378, doi: 10.1016/j.jclinepi.2012.10.014 (2013).
Ioannidis, J. P. A. & Karassa, F. B. The need to consider the wider agenda in systematic reviews and meta-analyses: breadth, timing and depth of the evidence. BMJ 341, c4875, doi: 10.1136/bmj.c4875 (2010).
Yank, V., Rennie, D. & Bero, L. A. Financial ties and concordance between results and conclusions in meta-analyses: retrospective cohort study. BMJ 335, 1202, doi: 10.1136/bmj.39376.447211.BE (2007).
Zhang, J., Shang, H., Gao, X. & Ernst, E. Acupuncture-related adverse events: a systematic review of the Chinese literature. Bull World Health Organ 88, 915–921c, doi: 10.2471/blt.10.076737 (2010).
Adams, D. et al. The Safety of Pediatric Acupuncture: A Systematic Review. Pediatrics 128, e1575, doi: 10.1542/peds.2011-1091 (2011).
Prady, S. L., Richmond, S. J., Morton, V. M. & MacPherson, H. A Systematic Evaluation of the Impact of STRICTA and CONSORT Recommendations on Quality of Reporting for Acupuncture Trials. PLoS ONE 3, e1577, doi: 10.1371/journal.pone.0001577 (2008).
Hoffmann, T. C. et al. Better reporting of interventions: template for intervention description and replication (TIDieR) checklist and guide. BMJ 348, g1687, doi: 10.1136/bmj.g1687 (2014).
Montori, V. M., Wilczynski, N. L., Morgan, D. & Haynes, R. B. Optimal search strategies for retrieving systematic reviews from Medline: analytical survey. BMJ 330, 68, doi: 10.1136/bmj.38336.804167.47 (2005).
Wilczynski, N. L. & Haynes, R. B. EMBASE search strategies achieved high sensitivity and specificity for retrieving methodologically sound systematic reviews. J Clin Epidemiol 60, 29–33, doi: 10.1016/j.jclinepi.2006.04.001 (2007).
Shea, B. et al. Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol 7, 10, doi: 10.1186/1471-2288-7-10 (2007).
Acknowledgements
This study was funded by Hospital Authority of Hong Kong (Reference number: 8110016609).
Author information
Authors and Affiliations
Contributions
Study concept and design: V.C., E.H. and J.W. Acquisition of data: X.Y.W. and R.H. Analysis and interpretation of data: X.Y.W. and R.H. Drafting of the manuscript: X.Y.W and V.C. Critical revision of the manuscript for important intellectual content: V.C., E.Z., B.N. and K.T. Administrative, technical, or material support: S.W. and J.W. All authors reviewed the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Wu, X., Chung, V., Hui, E. et al. Effectiveness of acupuncture and related therapies for palliative care of cancer: overview of systematic reviews. Sci Rep 5, 16776 (2015). https://doi.org/10.1038/srep16776
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep16776
This article is cited by
-
2023 MASCC/ESMO consensus antiemetic guidelines related to integrative and non-pharmacological therapies
Supportive Care in Cancer (2024)
-
Effect of acupuncture in myelosuppression and quality of life in women with breast cancer undergoing chemotherapy: a randomized clinical study
Supportive Care in Cancer (2023)
-
MASCC/ISOO expert opinion on the management of oral problems in patients with advanced cancer
Supportive Care in Cancer (2022)
-
DER TUMORSCHMERZ: GRUNDLAGEN UND THERAPIE
Akupunktur & Aurikulomedizin (2020)
-
The use of complementary medicine in palliative care in France: an observational cross-sectional study
Supportive Care in Cancer (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.