Abstract
Chronic kidney disease (CKD) is a major health problem worldwide. Indoxyl sulfate (IS) and p-cresyl sulfate (PCS) are highly protein-bound nephro-cardiovascular toxins, which are not efficiently removed through hemodialysis. The renal excretions of IS and PCS were mediated by organic anion transporters (OATs) such as OAT1 and OAT3. Green tea (GT) is a popular beverage containing plenty of catechins. Previous pharmacokinetic studies of teas have shown that the major molecules present in the bloodstream are the glucuronides/sulfates of tea catechins, which are putative substrates of OATs. Here we demonstrated that GT ingestion significantly elevated the systemic exposures of endogenous IS and PCS in rats with chronic renal failure (CRF). More importantly, GT also significantly increased the levels of serum creatinine (Cr) and blood urea nitrogen (BUN) in CRF rats. Mechanism studies indicated that the serum metabolites of GT (GTM) inhibited the uptake transporting functions of OAT1 and OAT3. In conclusion, GT inhibited the elimination of nephro-cardiovascular toxins such as IS and PCS and deteriorated the renal function in CRF rats.
Similar content being viewed by others
Introduction
Chronic kidney disease (CKD) is affecting the health of more and more people worldwide1. The main feature at the end stage of CKD is the accumulation of endogenous uremic toxins2,3, among which indoxyl sulfate (IS) and p-cresyl sulfate (PCS) are highly protein-bound and cannot be efficiently removed through hemodialysis4. Moreover, the elevated serum levels of IS and PCS were associated with the progression of CKD and cardiovascular diseases (CVD) as well as all-cause mortality5,6,7. Owing to the acidic properties, IS and PCS are existing as anions under physiological pH in the systemic circulation and the uptake transports of IS and PCS across the cell membranes of renal proximal tubules were mediated by organic anion transporters (OATs) such as OAT1 and OAT38,9,10.
Habitual consumption of teas, leaves and buds of Cammellia sinensis, has long been considered to have many health benefits such as prevention of CVD and cancers11,12. Green tea (GT) is one of the most popular teas containing plenty of catechins such as (−)-epicatechin (EC), (−)-epigallocatechin (EGC), (−)-epicatechin-3-gallate (ECG) and (−)-epigallocatechin-3-gallate (EGCG), which account for up to 30% of the dry leaf weight13. Previous studies on tea catechin pharmacokinetics have reported that EC glucuronides/sulfates and EGC glucuronides/sulfates were the major molecules in the bloodstream14,15,16. Given the anionic nature of glucuronides/sulfates under physiological pH, these conjugated metabolites of tea catechins are putative substrates of OATs17. We therefore hypothesized that the serum metabolites of GT (GTM) might inhibit the uptake transport of IS and PCS across the cell membrane of renal proximal tubule mediated by OAT1 and OAT3, which in turn would lead to elevated blood levels of IS and PCS in CKD patients with lower expressions of OATs18,19 and consequently promote the progression of CKD and CVD.
Although GT has been found to show renal and cardiovascular protective effects in healthy subjects20,21,22, till now whether GT likely benefits CKD patients remains unknown. Previous studies have reported that adenine-induced chronic renal failure (CRF) rats showed lower protein expressions of OAT1 and OAT3 along with the decreased clearance of IS and PCS19,23. Hence, a CRF rat model induced with adenine was adopted in this study to investigate the effect of GT on the serum levels of endogenous IS and PCS. Moreover, the effect of GT on the renal function of CRF rats was also evaluated. Furthermore, cell models were used to verify the involvement of OAT1 and OAT3 in the mechanism.
Results
Quantitation of tea catechins in GT infusion
GT infusion was analyzed by LC-MS/MS and the chromatograms were shown in Fig. 1. The quantitation results showed that the concentrations of EC, EGC, ECG and EGCG were 966.7, 919.9, 739.7 and 1960.1 μg/mL (3.33, 3.17, 2.55 and 6.75 mM), respectively, in the GT infusion.
Characterization of the serum metabolites of GT (GTM)
For mimicking the molecules interacting with OAT1 and OAT3 located on the membrane of renal proximal tubular cells, GTM was prepared from rats after receiving GT infusion. Characterization of GTM indicated that the concentrations of the free forms of EC, EGC, ECG and EGCG were 0.86, 2.17, 0.06 and 0.13 μM, respectively. After hydrolysis with sulfatase/glucuronidase, the peaks of EC, EGC, ECG and EGCG were all enhanced, in particular EC and EGC as shown in Fig. 2. The concentrations of free form and the sulfates/glucuronides of each tea catechin in GTM are listed in Table 1, showing that the major molecules in GTM were the sulfates/glucuronides of EC and EGC. The concentrations of the sulfates/glucuronides of EC, EGC, ECG and EGCG were 32.47, 33.29, 0.13 and 0.40 μM, respectively, which have been obtained by subtracting the free form concentrations from those after hydrolysis.
Quantitation of IS and PCS in serum
The analytical methods of IS and PCS were established and validated in this study. Good linear relationships existed in the concentration ranges of 0.4–25.0 μg/mL (Y = 0.246 X + 0.006, r = 0.9999) for IS and 0.3–20.0 μg/mL (Y = 0.045 X + 0.010, r = 0.9996) for PCS in serum. Validation of the analytical methods for IS indicated that the coefficients of variation (CVs) of intraday and interday analysis were below 6.4% and 7.6% and the relative errors (R.E.) were below 12.1% and 9.9%, respectively. The CVs of PCS of intraday and interday analysis were below 17.0% and 12.6% and the R.E. were below 10.9% and 7.8%. The recoveries of IS at 0.8, 3.1 and 12.5 μg/mL from serum were 88, 101 and 100% and those of PCS at 0.6, 2.5 and 10.0 μg/mL were 104, 103 and 105%. The LLOQ of IS and PCS were 0.4 and 0.3 μg/mL and LOD were 0.01 and 0.04 μg/mL.
Establishment of CRF model and effect of GT on the serum levels of IS and PCS in CRF rats
The dosing times of adenine and GT as well as scheduled time of blood collection are summarized in Fig. 3. After administration of five consecutive doses of adenine, the mean serum IS level in 28 rats was significantly elevated from 6.85 to 15.35 μM (P < 0.001) and PCS level was increased from 5.59 to 7.49 μM (P = 0.14) on day 4 as shown in Fig. 4. The serum profiles of endogenous IS and PCS in CRF rats following oral administration of GT at 200 and 400 mg/kg are shown in Fig. 5. The profiles clearly showed that ingestion of GT dose-dependently increased the serum levels of IS and PCS. The pharmacokinetic parameters of IS and PCS are listed in Table 2. The results showed that ingestion of 400 mg/kg of GT significantly increased the AUC0-360 of IS and PCS by 139.2% and 118.4%, respectively and elevated Cmax of IS by 123.3%, whereas the Cmax of PCS was not affected. In contrast, when GT was given at a lower dose of 200 mg/kg, the profiles of IS and PCS were higher than the control curves, however, the differences of Cmax and AUC0-360 did not reach statistical significance.
Effect of GT on the renal function of CRF rats
After administration of five consecutive doses of adenine, the mean Cr of 14 rats was significantly elevated from 0.30 to 0.58 mg/dL and BUN was increased from 21.0 to 60.1 mg/dL on day 4. The concentrations of Cr and BUN in CRF rats after giving the 7th dose of GT and water are shown in Table 3. The mean Cr and BUN in GT group were 0.79 and 55.1 mg/dL, respectively, which were significantly higher than those in water group (0.49 and 40.9 mg/dL).
Effects of GTM on the uptake transport mediated by hOAT1 and hOAT3
The effects of GTM on the uptake activity of hOAT1 and hOAT3 are shown in Fig. 6. GTM at 1/4−, 1/2− and 1-fold serum concentrations significantly reduced the intracellular accumulation of 6-CF, an OAT1 substrate, by 43.9, 41.9 and 58.1%, respectively, when compared with blank serum specimen at corresponding concentrations. Likewise, GTM at 1/2− and 1-fold serum concentration significantly reduced the intracellular accumulation of 5-CF, an OAT3 substrate, by 36.4% and 31.3%, respectively, when compared to blank serum specimen at corresponding concentration. As positive control inhibitors of hOAT1 and hOAT3, probenecid (80 μM) significantly reduced the intracellular accumulation of 6-CF and 5-CF by 50.4 and 50.7%, respectively. These in vitro studies indicated that GTM significantly inhibited the uptake transport mediated by hOAT1 and hOAT3.
Discussion
Quantitation results revealed that EGCG was the major tea catechin in GT infusion, whereas the major molecules in GTM were the sulfates/glucuronides of EC and EGC. These finding largely resonated with the results reported previously16. Based on these facts, we could infer that ECG and EGCG were feasibly hydrolyzed by esterase to form EC and EGC, respectively, which were then extensively metabolized by conjugation reactions to yield EC sulfates/glucuronides and EGC sulfates/glucuronides as the major molecules circulating in the bloodstream.
In regard to the quantitation of IS and PCS in serum, two HPLC methods using different internal standard and detection wavelengths have been developed and optimized in this study owing to the discrepant physicochemical properties between IS and PCS. Validation of the analytical methods confirmed that the precision, accuracy and recovery were satisfactory for the quantitation of IS and PCS in serum.
In clinical setting, CKD patients are often exposed to increased blood levels of endogenous uremic toxins such as IS and PCS, which are by-products of protein metabolism24,25. A recent study reported that the serum concentrations of IS and PCS in healthy subjects were 1.03 and 13.03 μM26. In contrast, for non-hemodialyzed stage 3–5 CKD patients the serum concentrations of IS and PCS were 17.45 and 73.47 μM, while in those CKD patients undergoing treatment with hemodialysis (stage 5D), they were 81.04 and 120.54 μM26. This highlights the fact that IS and PCS are highly protein bound (89% and 96%) and thus not efficiently removed through hemodialysis27,28,29,30. In regard to the relative abundance of IS and PCS in blood, the IS level was found consistently higher than PCS level in rats31,32,33, which appears opposite to that in humans. This discrepancy between rats and humans might stem from species difference in protein metabolism23,27,34.
In order to mimic the biological condition of CKD with lower expression of OATs, adenine was used to induce CRF in this study19,23,35,36. The serum levels of IS and PCS in our CRF rats had been elevated to 15.4 and 7.6 μM, which were largely close to those values in previous studies31,32,33. On other hand, the levels of serum Cr and BUN were significantly elevated, indicating that the renal function of rats was impaired by adenine36,37. After giving seven doses of GT to the CRF rats, the higher dose of GT at 400 mg/kg significantly increased the systemic exposures of IS and PCS, whereas the lower dose at 200 mg/kg did not result in significant increases, indicating that large quantity of GT inhibited the elimination of IS and PCS. Moreover, the levels of serum Cr and BUN were significantly increased by 400 mg/kg of GT, indicating that GT deteriorated the renal function of CRF rats, which might be accounted for by the increased systemic exposure of uremic toxins such as IS and PCS.
The uptake transports of IS and PCS across cell membrane were well known to be mediated by OAT1 and OAT38,9. In regard to the magnitudes of influences, it was apparent that the effect of GT on the serum levels of IS was in a greater extent than PCS. It has been reported that the uptakes of IS by OAT1 and OAT3 were saturable with Km values of 21 μM and 263 μM, respectively38. Regarding PCS, the Km for the OAT1-mediated uptake was 128 μM, whereas saturation was not observed for OAT3-mediated transport up to 5 mM39. Given the lower Km values of IS than PCS in both OAT1- and OAT3- mediated uptake, IS should be a substrate for OAT1 and OAT3 with lower capacity. Therefore, the uptake transports of IS mediated by OAT1 and OAT3, especially OAT1, were more easily to be saturated than those of PCS, which can account for the fact that GT elevated the serum levels of IS more than PCS.
In order to explore the mechanisms involved, GTM was prepared for mimicking the molecules interacting with renal OAT1 and OAT340,41. Characterization of GTM demonstrated that the major molecules in the serum were EC glucuronides/sulfates and EGC glucuronides/sulfates, which echoed the finding in precedent studies14,16. Cell line studies showing that GTM exhibited inhibition on the uptake transport mediated by OAT1 and OAT3 could explain the increased serum levels of IS and PCS caused by GT. We speculated that these mechanisms associated with OAT1 and OAT3 in CRF rats could be extrapolated to CKD patients, because the distribution and function of OATs in rat kidney are similar to those in humans42,43,44.
Despite various health benefits of tea consumption to healthy humans20,21,22, the present study demonstrated that GT inhibited the elimination of nepro-vascular toxins such as IS and PCS and deteriorated the renal function in CRF rats. Considering that high blood levels of IS and PCS increased oxidative stress, inflammatory mediators and chemokines in the body45, we suspect consuming large quantity of GT might result in promoting the progression of CKD and CVD in CKD patients. Moreover, owing to the inefficient removal of IS and PCS through hemodialysis, GT consumption might also exacerbate the pathologies of CKD and CVD in end-stage CKD patients even under hemodialysis treatment5,6,7. Therefore, we suggest that CKD patients should avoid drinking large quantity of tea beverages before benefits or risks to CKD patients assessed by future clinical studies. In conclusion, GT inhibited the elimination of nephro-cardiovascular toxins such as IS and PCS through inhibition on OAT1 and OAT3 and deteriorated the renal function in CRF rats.
Materials and Methods
Chemicals and reagents
GT was purchased from the market in Taichung, Taiwan. IS (purity 97%) was obtained from Alfa Aesar (Lancaster, UK). 6,7-dimethoxycoumarin (6,7-DMC, purity 98%) was supplied by Aldrich Chemical Co. (Milwaukee, WI, U.S.A.). EC (purity 90%), ECG (purity 98%), EGCG (purity 95%), formic acid, probenecid, phosphoric acid (glacial, 85%) and methyl-paraben were purchased from Sigma Chemical Co. (St. Louis, MO, U.S.A.). EGC (purity 92.7%) was obtained from ChromaDex, Inc. (Irvine, CA, U.S.A.). and ethyl acetate were LC grade and obtained from ECHO Chemical Co. (Miaoli Hsien, Taiwan). Acetonitrile was LC/MS grade and was purchased from Millinckrodt Baker, Inc. (Phillipsburg, NJ, U.S.A.). Fetal bovine serum was obtained from Biological Industries Inc. (Kibbutz, Beit Haemek, Israel). Penicillin-Streptomycin-Glutamine, Dulbecco’ s Modified Eagle Medium, trypsin/EDTA, Hank’s Balanced Salt Solution and 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid were purchased from Invitrogen (Carlsbad, CA, U.S.A.). Dulbecco’s Modified Eagle Medium F12 was obtained from Thermo Fisher Scientific Inc (Waltham, MA, U.S.A.). 6-Carboxyfluorescein was purchased from AAT Bioquest Inc. (Sunnyvale, CA, U.S.A.) and 5-carboxyfluorescein was obtained from Acros Organics (Geel, Belgium). Milli-Q plus water (Millipore, Bedford, MA, U.S.A.) was used for all preparations.
Preparation and characterization of GT infusion
The infusion was produced by steeping either 2 or 4 g of GT in 50 mL of hot deionized water (98–100 °C) for 30 min. The infusion was filtered with gauze while hot to afford concentrations of 40 and 80 mg/mL, respectively, which was freshly administered to rats via gastric gavage.
For the characterization of GT infusion, after filtration of GT infusion with 0.2 μm RC15 filter (Sartorious, Goettingen Germany), 100 μL of the filtrate was mixed with 900 μL of methanol and centrifuged to remove the precipitate. The properly diluted infusion (50 μL) was combined with 50 μL of 6,7-DMC solution (2.0 μg/mL in methanol) as internal standard and 5 μL was subject to LC-MS/MS analysis. The HPLC system included Accela 1250 pump and auto-sampler (Thermo Fisher Scientific Inc. U.S.A.). Chromatographic separation was achieved using a Phenomenex® C18 analytical column (150 mm × 1.0 mm, 5 μm) with a prefilter. The mobile phase consisted of acetonitrile containing 0.01% formic acid (A) and water containing 0.01% formic acid (B) and programmed in a gradient manner as follows: A/B: 2/98 (0–2 min), 15/85 (4 min), 40/60 (6 min), 90/10 (8–10 min) and 2/98 (12 min). The flow rate was 0.2 mL/min. The column effluent was detected by H-ESI (heated-electrospray ionization) -II probe with Quantum Access MAX triple stage quadrupole (TSQ) mass spectrometer (Thermo Fisher Scientific Inc. U.S.A.). Nitrogen was used as sheath gas at 35 arbitrary units and auxiliary gas at 10 arbitrary units. The collision energy was set at −19/18 V, spray voltage at −3000/3000 V, capillary temperature at 350 °C, vaporizer temperature at 350 °C and tube lens offset at −80/88 V. The following mass transitions were used for selected reaction monitoring analysis (SRM): EC (289/245), EGC (305/125), ECG (441/289), EGCG (457/169) and 6,7-DMC (207/151). The ESI-MS spectra were recorded in negative ion mode for EC, EGC, ECG and EGCG and positive ion mode for 6,7-DMC.
Animals
Male Sprague-Dawley rats (270–360 g) were purchased from National Laboratory Animal Center (Taipei, Taiwan) and housed in conditioned environment with 12-h light/dark cycles. Food and water were acquired ad libitum until 12 h prior to experiments. Rats were divided into two groups. The first experiment used 28 rats to determine the effect of GT on the serum levels of IS and PCS in CRF rats; the second experiment used 14 rats to evaluate the effect of GT on the renal function of CRF rats. All animal experiments were carried out in strict accordance with the recommendations by ‘‘The Guidebook for the Care and Use of Laboratory Animals (2002)’’ published by the Chinese Society of Animal Science, Taiwan, R.O.C. The experimental protocol had been reviewed and approved on 08/01/2014 (Permit Number: 103–126-N) by the Insititutional Animal Care and Use Committee of China Medical University, Taiwan, R.O.C.
Establishment of CRF model and administration of GT infusion
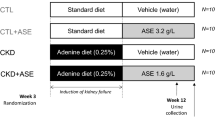
CRF was induced via oral administration of adenine following previous studies, but with some modification19,23,35,36. Briefly, adenine suspended in 0.5% methylcellulose 400 (15 mg/mL) was orally administered to 28 rats via gastric gavage twice daily for seven consecutive doses (15 mg/rat) throughout the experimental period. On day 4, the serum levels of IS were determined. Upon confirming attenuated renal function by significant elevation of serum IS levels, the CRF rats were divided into three groups (8–10 rats in each group) with comparable IS levels. The first group received 400 mg/5 mL/kg of GT infusion twice daily for seven consecutive doses; the second group received 200 mg/5 mL/kg of GT twice daily for seven consecutive doses; and the third group received 5 mL/kg of water in parallel as control. On day 8, rats were administered the 7th dose of GT at 9:00 am after overnight fast and the blood samples were collected at 0, 15, 30, 60, 120, 180 and 360 min after dosing. The scheduled time of blood collection and administrations of adenine and GT are summarized in Fig. 3. At each sampling time, 0.5 mL of blood was withdrawn under isoflurane anesthesia. The blood samples were collected in microtubes and centrifuged at 10,000 g for 15 min to obtain serum, which was stored at −20 °C before analysis.
Determination of the concentrations of IS and PCS in serum
For the determination of IS and PCS concentrations in serum, 50 μL of serum specimen was vortexed with 200 μL of methanol containing 10 μg/mL of 6,7-DMC or 100 μg/mL of methylparaben as internal standards, respectively and centrifuged to remove the precipitate, then a 20 μL aliquot was subject to HPLC analysis.
For calibrator preparations, 50 μL of serum was spiked with a series of concentrations of IS and PCS to afford concentration ranges of 0.4–25.0 μg/mL (1.8–117.3 μM) and 0.3–20.0 μg/mL (1.7–106.3 μM), respectively. The later procedure followed that described above for serum samples. The calibration curves were drawn by linear regression of the peak area ratios (IS or PCS to internal standard) against the known concentrations of IS and PCS, respectively.
The HPLC apparatus included a pump (LC-10AT, Shimadzu, Kyoto, Japan), fluorescence detector (RF-20A, Shimadzu, Kyoto, Japan) and automatic injector (SIL-10AF, Shimadzu, Kyoto, Japan). The Apollo C18 (5 μm, 4.6 mm × 250 mm, Alltech, Deerfield, IL, USA) column was equipped with a guard column (4.6 × 50 mm, 5 μm) (GL Science Inc., Tokyo, Japan). The mobile phase consisted of acetonitrile (A)–0.1% phosphoric acid (B) and programmed in a gradient manner as follows: A/B: 15/85 (0–7 min), 30/70 (9–22 min) and 15/85 (24–35 min) for IS and 16/84 (0–10 min), 30/70 (13–22 min) and 16/84 (24–36 min) for PCS. Detector settings were Ex 280 nm/Em 375 nm for IS and Ex 214 nm/Em 306 nm for PCS. The flow rates were 1.0 mL/min.
Effect of GT on Cr and BUN in CRF rats
In another experiment, the same animal protocol mentioned above was employed and the concentrations of Cr and BUN were determined before adenine treatment (Day 0), before GT dosing (Day 4) and after 7th dose of GT (Day 8). Upon confirming attenuated renal function by significant elevation of Cr and BUN on day 4, the CRF rats were divided into two groups (7 rats per group) with comparable Cr levels. The first group received 400 mg/5 mL/kg of GT twice daily for seven consecutive doses; the second group received 5 mL/kg of water in parallel as control. On day 8, rats were administered the 7th dose of GT and water after overnight fast and the blood samples were collected 30 min later. Cr was determined by a kinetic alkaline picrate method in an ADVIA 2400 Chemistry System (Siemens Health Care Diagnostics, Inc. Tarrytown, NY, U.S.A.). BUN was assayed by the urease/glutamate dehydrogenase coupled-enzyme reaction using the same analyser.
Cell line and culture conditions
Construction of the stably transfected cell lines used for transport studies, Chinese hamster ovary (CHO) cells expressing hOAT1 (CHO-hOAT1), human embryonic kidney 293 (HEK) cells expressing hOAT3 (HEK-hOAT3) and their corresponding empty vector-transfected control cell lines, was described previously40,41. CHO cells were maintained at 37 °C with 5% CO2 in DMEM F-12 media (Thermo Fisher Scientific Inc., USA) containing 10% serum, 1% penicillin/streptomycin and 1 mg/mL G418. HEK cells were maintained at 37 °C with 5% CO2 in DMEM high glucose media (Thermo Fisher Scientific Inc., USA) containing 10% serum, 1% penicillin/streptomycin and 50 μg/mL hygromycin B. Cells were cultured in Poly-D-Lysine coated dishes.
Preparation and characterization of the serum metabolites of GT (GTM)
In order to mimic the molecules interacting with OATs in vivo, GTM were prepared from rats and characterized. Briefly, GT infusion (800 mg/10 mL/kg) was orally administered to rats fasted overnight. Blood was collected at 15 min after dosing of GT infusion. After coagulation, the serum was collected and vortexed with 3-fold methanol. Following centrifugation at 10,000 g for 15 min, the supernatant was concentrated in a rotatory evaporator under vacuum to dryness. An appropriate volume of water was added to the residue yielding a solution with 10-fold serum concentration, which was divided into aliquots and stored at −80 °C for later use.
A portion of GTM was characterized following a previous method with some modifications16,46. Briefly, 100 μL of serum sample was mixed with 50 μL of sulfatase (containing 1000 units/mL of sulfatase and 39,861 units/ml of ß-glucuronidase), 50 μL of ascorbic acid (200 mg/mL) and incubated at 37 °C for 45 min under anaerobic condition. After hydrolysis, the serum was added to 50 μL 0.1 N HCl and then partitioned with 250 μL of ethyl acetate (containing 100 ng/mL of 6,7-DMC as internal standard). The ethyl acetate layer was evaporated under N2 to dryness and reconstituted with an appropriate volume of mobile phase prior to LC-MS/MS analysis. The mobile phase consisted of acetonitrile (A) – water containing 0.1% formic acid (B) and programmed in a gradient manner as follows: A/B: 2/98 (0–2 min), 15/85 (4 min), 40/60 (6 min), 90/10 (8–10 min) and 2/98 (12 min). The flow rate was 0.2 mL/min.
Effects of GTM on the uptake transport mediated by hOAT1 and hOAT3
CHO-hOAT1 and HEK-hOAT3 cells (1 × 105 cells/well) were cultured in a 96-well plate. 6-Carboxyfluorescein (6-CF) and 5-carboxyfluorescein (5-CF) were used as probes for evaluating the effect of GTM on the activity of hOAT1 and hOAT3, respectively47,48. In addition, probenecid (80 μM) was used as a positive control for inhibition of hOAT1 and hOAT349. After 24 h or 48 h incubation of CHO-hOAT1 or HEK-hOAT3, the medium was removed and washed three times with PBS buffer. Before the transport experiment, CHO-hOAT1 and HEK-hOAT3 cells were pre-incubated with test agents (GTM and probenecid) at 37 °C. After 30 min incubation, 6-CF or 5-CF was then added and incubated for another 5 min and 10 min, respectively. The plates were immediately placed on ice bath and the supernatants were removed and the cells were washed three times with ice-cold PBS. Subsequently, 100 μL of 0.1% Triton X-100 was added to lyse the cells and the fluorescence was measured with excitation at 485 nm and emission at 528 nm. To quantitate the content of protein in each well, 10 μL of cell lysate was added to 200 μL of diluted protein assay reagent (Bio-Rad, Hercules, CA, U.S.A.) and the optical density was measured at 570 nm. The relative intracellular accumulation of 6-CF or 5-CF was calculated by comparing with that of controls after protein correction.
Data analysis
The peak serum concentration (Cmax) was obtained from experimental observation. The area under the serum concentration - time curve (AUC0-t) was calculated using trapezoidal rule to the last point. The differences of IS and PCS among three groups were analyzed by using one-way ANOVA, while the difference of Cr and BUN between two groups was analyzed by using unpaired Student’s t-test, taking p < 0.05 as significant level. Unpaired Student’s t-test was also used for the analysis of in vitro assays.
Additional Information
How to cite this article: Peng, Y.-H. et al. Green tea inhibited the elimination of nephro-cardiovascular toxins and deteriorated the renal function in rats with renal failure. Sci. Rep. 5, 16226; doi: 10.1038/srep16226 (2015).
References
Fatema, K. et al. Screening for chronic kidney diseases among an adult population. Saudi J. Kidney Dis. Transpl. 24, 534–541 (2013).
Vanholder, R., Van Laecke, S. & Glorieux, G. What is new in uremic toxicity? Pediatr. Nephrol. 23, 1211–1221 (2008).
Masereeuw, R. et al. The kidney and uremic toxin removal: glomerulus or tubule? Semin. Nephrol. 34, 191–208 (2014).
Lesaffer, G. et al. Intradialytic removal of protein-bound uraemic toxins: role of solute characteristics and of dialyser membrane. Nephrol. Dial. Transplant. 15, 50–57 (2000).
Barreto, F. C. et al. Serum indoxyl sulfate is associated with vascular disease and mortality in chronic kidney disease patients. Clin. J. Am. Soc. Nephrol. 4, 1551–1558 (2009).
Liabeuf, S. et al. Free p-cresylsulphate is a predictor of mortality in patients at different stages of chronic kidney disease. Nephrol. Dial. Transplant. 25, 1183–1191 (2010).
Wu, I. W. et al. p-Cresyl sulphate and indoxyl sulphate predict progression of chronic kidney disease. Nephrol. Dial. Transplant. 26, 938–947 (2011).
Enomoto, A. et al. Role of organic anion transporters in the tubular transport of indoxyl sulfate and the induction of its nephrotoxicity. J. Am. Soc. Nephrol. 13, 1711–1720 (2002).
Miyamoto, Y. et al. Organic anion transporters play an important role in the uptake of p-cresyl sulfate, a uremic toxin, in the kidney. Nephrol. Dial. Transplant. 26, 2498–2502 (2011).
Sweet, D. H. Organic anion transporter (Slc22a) family members as mediators of toxicity. Toxicol. Appl. Pharmacol. 204, 198–215 (2005).
Khan, N. & Mukhtar, H. Tea and health: studies in humans. Curr. Pharm. Des. 19, 6141–6147 (2013).
Lambert, J. D. Does tea prevent cancer? Evidence from laboratory and human intervention studies. Am. J. Clin. Nutr. 98, 1667s–1675s (2013).
Balentine, D. A., Wiseman, S. A. & Bouwens, L. C. The chemistry of tea flavonoids. Crit. Rev. Food Sci. Nutr. 37, 693–704 (1997).
Lee, M. J. et al. Pharmacokinetics of tea catechins after ingestion of green tea and (−)-epigallocatechin-3-gallate by humans: formation of different metabolites and individual variability. Cancer Epidemiol. Biomarkers Prev. 11, 1025–1032 (2002).
Lee, M. J. et al. Analysis of plasma and urinary tea polyphenols in human subjects. Cancer Epidemiol. Biomarkers Prev. 4, 393–399 (1995).
Chen, L., Lee, M. J., Li, H. & Yang, C. S. Absorption, distribution, elimination of tea polyphenols in rats. Drug Metab. Dispos. 25, 1045–1050 (1997).
Sekine, T., Cha, S. H. & Endou, H. The multispecific organic anion transporter (OAT) family. Pflugers Arch. 440, 337–350 (2000).
Sakurai, Y. et al. Expression levels of renal organic anion transporters (OATs) and their correlation with anionic drug excretion in patients with renal diseases. Pharm. Res. 21, 61–67 (2004).
Komazawa, H. et al. Renal uptake of substrates for organic anion transporters Oat1 and Oat3 and organic cation transporters Oct1 and Oct2 is altered in rats with adenine-induced chronic renal failure. J. Pharm. Sci. 102, 1086–1094 (2013).
Clement, Y. Can green tea do that? A literature review of the clinical evidence. Prev. Med. 49, 83–87 (2009).
El-Mowafy, A. M., Al-Gayyar, M. M., Salem, H. A., El-Mesery, M. E. & Darweish, M. M. Novel chemotherapeutic and renal protective effects for the green tea (EGCG): role of oxidative stress and inflammatory-cytokine signaling. Phytomedicine 17, 1067–1075 (2010).
Turner, J. E. Glomerulonephritis therapy: is there a role for green tea? Kidney Int. 80, 563–564 (2011).
Zhao, Y. Y. et al. Intrarenal metabolomic investigation of chronic kidney disease and its TGF-beta1 mechanism in induced-adenine rats using UPLC Q-TOF/HSMS/MS(E). J. Proteome Res. 12, 692–703 (2013).
Watanabe, H., Miyamoto, Y., Otagiri, M. & Maruyama, T. Update on the pharmacokinetics and redox properties of protein-bound uremic toxins. J. Pharm. Sci. 100, 3682–3695 (2011).
Meijers, B. K. & Evenepoel, P. The gut-kidney axis: indoxyl sulfate, p-cresyl sulfate and CKD progression. Nephrol. Dial. Transplant. 26, 759–761 (2011).
Calaf, R. et al. Determination of uremic solutes in biological fluids of chronic kidney disease patients by HPLC assay. J. Chromatogr. B Analyt. Technol. Biomed. Life Sci. 879, 2281–2286 (2011).
Meijers, B. K. et al. p-Cresyl sulfate and indoxyl sulfate in hemodialysis patients. Clin. J. Am. Soc. Nephrol. 4, 1932–1938 (2009).
Dhondt, A., Vanholder, R., Van Biesen, W. & Lameire, N. The removal of uremic toxins. Kidney Int. Suppl. 76, S47–59 (2000).
Liabeuf, S., Drueke, T. B. & Massy, Z. A. Protein-bound uremic toxins: new insight from clinical studies. Toxins 3, 911–919 (2011).
Fagugli, R. M., De Smet, R., Buoncristiani, U., Lameire, N. & Vanholder, R. Behavior of non-protein-bound and protein-bound uremic solutes during daily hemodialysis. Am. J. Kidney Dis. 40, 339–347 (2002).
Taki, K. & Niwa, T. Indoxyl sulfate-lowering capacity of oral sorbents affects the prognosis of kidney function and oxidative stress in chronic kidney disease. J. Ren. Nutr. 17, 48–52 (2007).
Lekawanvijit, S. et al. Chronic kidney disease-induced cardiac fibrosis is ameliorated by reducing circulating levels of a non-dialysable uremic toxin, indoxyl sulfate. PLoS One 7, e41281 (2012).
Miyazaki, T., Aoyama, I., Ise, M., Seo, H. & Niwa, T. An oral sorbent reduces overload of indoxyl sulphate and gene expression of TGF-beta1 in uraemic rat kidneys. Nephrol. Dial. Transplant. 15, 1773–1781 (2000).
Evenepoel, P., Meijers, B. K., Bammens, B. R. & Verbeke, K. Uremic toxins originating from colonic microbial metabolism. Kidney Int. Suppl S12–19, 10.1038/ki.2009.402 (2009).
Terai, K. et al. Vascular calcification and secondary hyperparathyroidism of severe chronic kidney disease and its relation to serum phosphate and calcium levels. Br. J. Pharmacol. 156, 1267–1278 (2009).
Kadowaki, D. et al. Effect of acetaminophen on the progression of renal damage in adenine induced renal failure model rats. Life Sci. 91, 1304–1308 (2012).
Nakagawa, K. et al. Cinacalcet does not affect longitudinal growth but increases body weight gain in experimental uraemia. Nephrol. Dial. Transplant. 23, 2761–2767 (2008).
Deguchi, T. et al. Characterization of uremic toxin transport by organic anion transporters in the kidney. Kidney Int. 65, 162–174 (2004).
Watanabe, H. et al. Human organic anion transporters function as a high-capacity transporter for p-cresyl sulfate, a uremic toxin. Clin. Exp. Nephrol. 18, 814–820 (2014).
Ho, E. S., Lin, D. C., Mendel, D. B. & Cihlar, T. Cytotoxicity of antiviral nucleotides adefovir and cidofovir is induced by the expression of human renal organic anion transporter 1. J. Am. Soc. Nephrol. 11, 383–393 (2000).
Vanwert, A. L., Srimaroeng, C. & Sweet, D. H. Organic anion transporter 3 (oat3/slc22a8) interacts with carboxyfluoroquinolones and deletion increases systemic exposure to ciprofloxacin. Mol. Pharmacol. 74, 122–131 (2008).
Klaassen, C. D. & Aleksunes, L. M. Xenobiotic, bile acid and cholesterol transporters: function and regulation. Pharmacol. Rev. 62, 1–96 (2010).
Burckhardt, G. & Wolff, N. A. Structure of renal organic anion and cation transporters. Am. J. Physiol. Renal Physiol. 278, F853–866 (2000).
Volk, C. OCTs, OATs and OCTNs: structure and function of the polyspecific organic ion transporters of the SLC22 family. Wiley Interdisciplinary Reviews: Membrane Transport and Signaling 3, 1–13 (2014).
Vanholder, R., Schepers, E., Pletinck, A., Nagler, E. V. & Glorieux, G. The uremic toxicity of indoxyl sulfate and p-cresyl sulfate: a systematic review. J. Am. Soc. Nephrol. 25, 1897–1907 (2014).
Mata-Bilbao Mde, L. et al. A new LC/MS/MS rapid and sensitive method for the determination of green tea catechins and their metabolites in biological samples. J. Agric. Food Chem. 55, 8857–8863 (2007).
Truong, D. M., Kaler, G., Khandelwal, A., Swaan, P. W. & Nigam, S. K. Multi-level analysis of organic anion transporters 1, 3 and 6 reveals major differences in structural determinants of antiviral discrimination. J. Biol. Chem. 283, 8654–8663 (2008).
Nagle, M. A. et al. Analysis of three-dimensional systems for developing and mature kidneys clarifies the role of OAT1 and OAT3 in antiviral handling. J. Biol. Chem. 286, 243–251 (2011).
Wang, L. & Sweet, D. H. Potential for food-drug interactions by dietary phenolic acids on human organic anion transporters 1 (SLC22A6), 3 (SLC22A8) and 4 (SLC22A11). Biochem. Pharmacol. 84, 1088–1095 (2012).
Acknowledgements
The work was, in part, supported by the Ministry of Science and Technology, R.O.C. (MOST 103-2320-B-039-025 and NSC 102-2320-B-039-014-MY2) and China Medical University, Taichung, Taiwan, R.O.C. (CMU 103-N-01) and China Medical University hospital, Taichung, Taiwan, R.O.C. (DMR-104-092).
Author information
Authors and Affiliations
Contributions
Y.-H.P. contributed study design and formulation of the article. D.H.S. constructed the transfected cell lines and revised the manuscript. S.-P.L. and C.-P.Y. were involved in the experimental work. P.-D.L.C. and Y.-C.H. made contributions to conception, study design and supervision of the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Peng, YH., Sweet, D., Lin, SP. et al. Green tea inhibited the elimination of nephro-cardiovascular toxins and deteriorated the renal function in rats with renal failure. Sci Rep 5, 16226 (2015). https://doi.org/10.1038/srep16226
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep16226
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.