Abstract
Glucocorticosteroids (GCS) are used on a daily basis to reduce airway inflammation in asthma and chronic obstructive pulmonary disease (COPD). This treatment is usually escalated during acute disease exacerbations, events often associated with virus infections. We examined the impact of GCS on anti-viral defences and virus replication and assessed supplementary interferon (IFN) treatment. Here, we report that treatment of primary human airway cells in vitro with GCS prior to rhinovirus (RV) or influenza A virus (IAV) infection significantly reduces the expression of innate anti-viral genes and increases viral replication. Mice given intranasal treatment with GCS prior to IAV infection developed more severe disease associated with amplified virus replication and elevated inflammation in the airways. Adjuvant IFN treatment markedly reduced GCS-amplified infections in human airway cells and in mouse lung. This study demonstrates that GCS cause an extrinsic compromise in anti-viral defences, enhancing respiratory virus infections and provides a rationale for adjuvant IFN treatment.
Similar content being viewed by others
Introduction
Influenza A virus (IAV) and rhinovirus (RV) cause human respiratory infections leading to acute exacerbations of chronic respiratory diseases such as asthma and chronic obstructive pulmonary disease (COPD). These infections place patients at increased risk of severe lung disease, often requiring hospitalization1,2. For example, during the 2009 IAV H1N1 pandemic, pneumonia occurred chiefly in persons who had exacerbations of pre-existing asthma or COPD3,4. It is as yet unclear why this patient group is susceptible to viruses and go on to develop life-threatening lower airway infections. Intrinsic disease-related or extrinsic treatment-associated factors may contribute.
GCS have potent anti-inflammatory actions that are clinically effective and therapy has become entrenched as daily inhaled treatment for patients with asthma and COPD. Despite known beneficial clinical effects, GCS have documented risks5,6 and recent evidence indicates that this treatment requires caution. Inhaled GCS may be associated with an increased incidence of pneumonia in individuals with asthma and COPD exacerbations7,8 and GCS inhalers may offer little protection against virus-induced exacerbations of asthma9 and COPD10. It reflects a complex pathology initiated when respiratory virus infection occurs in the context of pre-existing airway inflammation and a therapy (GCS) having both anti-inflammatory and immune-suppressive characteristics.
Studies examining the impact of GCS therapy on respiratory virus infection in healthy individuals suggest that GCS may enhance virus replication. Treatment with intranasal GCS during naturally occurring RV infections was associated with prolonged shedding of virus in nasal washes11, whilst oral GCS therapy prior to experimental RV infections in healthy individuals increased virus replication in nasal washes12. This evidence, albeit circumstantial, implies that GCS therapy, when combined with intercurrent respiratory virus infection, may lead to more severe infections and detrimental outcomes.
Innate anti-viral immunity is a key defence mechanism against viruses but the impact of GCS on these responses in the airways is also unclear. Although in vitro studies have illustrated the ability of GCS to suppress RV-induced pro-inflammatory cytokine production by lung epithelial cells13,14 and fibroblasts15, the influence of GCS on type I and III interferon (IFN) production and subsequent induction of IFN-stimulated genes (ISGs) is not well characterized. In the only pertinent study, GCS were shown to inhibit the induction of the ISG MxA in RV-stimulated human peripheral blood mononuclear cells from healthy individuals16.
In this proof-of-concept study we demonstrate that GCS treatment dampens anti-viral responses and enhances respiratory virus replication. Furthermore, intranasal treatment of mice with GCS enhances IAV replication, reduces anti-viral responses and increases mortality. Addition of IFNs lessens the impact of GCS on virus replication. Together, these data demonstrate that GCS may have deleterious consequences during respiratory virus infections by blunting IFN-mediated anti-viral responses, effects that may be offset by adjuvant IFN therapy.
Results
GCS inhibit anti-viral and cytokine responses in primary human airway cells
Innate anti-viral responses induced by type I and III IFNs play an important role in host defense following virus infection. To examine the effects of GCS on anti-viral and cytokine responses, primary human airway cells isolated from healthy subjects were treated with fluticasone propionate (GCS) for 24 hrs, with a concentration as reported and reflective of levels achieved by inhalation in humans (10 nM14,17). Cell monolayers were then washed and incubated with RV (RV16) or IAV (A/Solomon Islands/3/2006, H1N1) and anti-viral and cytokine responses were examined at several time points following infection.
We first examined type I and III IFN proteins in cell supernatants from virus-infected primary human airway cells by ELISA. Consistent with previous reports15,18,19, the levels of IFNα and IFNλ proteins in cell supernatants from human primary bronchial epithelial cells (PBEC), primary airway fibroblasts (PAF) and primary airway macrophages (PAM) were below the level of detection, at 24 and 48 hrs following RV or IAV infection (data not shown). We therefore examined the mRNA expression of IFN genes by RT-PCR. GCS treatment of PBEC, PAF or PAM prior to IAV or RV infection did not significantly alter the expression of IFNα, IFNβ or IFNλ1 genes, 24 hrs post-infection (Fig. 1A–C).
Treatment of primary human airway cells with GCS prior to respiratory virus infection reduces innate anti-viral responses.
Monolayers of PBEC, PAF or PAM were treated with GCS for 24 hrs, washed and then infected with IAV (left panels) or RV (right panels). RNA was extracted from cell monolayers at 24 or 48 hrs post-infection and RT-PCR performed. mRNA expression of (A–C) IFNα, IFNβ and IFNλ1 genes and (D–F) ISGs IFIT1, ISG15, MxA, 2′5′OAS, viperin and RIG-I was measured. Data is relative to the expression of 18S and represents the mean of a minimum of 3 replicate samples ± SD. Data is representative of cultures from a minimum of 3 independent donors. Expression significantly reduced in virus-infected samples treated with GCS, * p < 0.05, ** p < 0.01, *** p < 0.001, one-way ANOVA and Tukey's post-test.
Binding of type I and III IFNs to their unique receptors results in the induction of a large number of ISGs with anti-viral properties20. We next assessed if GCS treatment of human airway cells prior to virus infection alters the induction of anti-viral genes using RT-PCR. Preliminary experiments were performed to determine the time at which significant up-regulation of ISG mRNA was detected following RV and IAV infection. mRNA expression of the ISGs IFIT1, ISG15, MxA, 2′5′OAS, viperin and RIG-I was significantly reduced 24 hrs following IAV infection and 48 hrs following RV infection, in GCS pre-treated PBEC (Fig. 1D) and PAF (Fig. 1E). In addition, mRNA levels of MxA, viperin and RIG-I were significantly lower in GCS pre-treated PAM 24 hrs following IAV infection, while ISG15, viperin and RIG-I gene expression was significantly decreased 24 hrs post-RV infection in PAM pre-treated with GCS (Fig. 1F).
We next aimed to confirm the previously reported inhibitory effects of GCS on virus-induced pro-inflammatory cytokine production in vitro13,15,18. Initial experiments were performed to determine the optimal time points to examine cytokine production by each cell type, following RV and IAV infection. GCS pre-treatment of PBEC significantly reduced IL-6, IL-8 and IP-10 production, 24 and 48 hrs following IAV and RV infection, respectively (Fig. 2A). Significant production of MCP-1 was not observed following RV or IAV infection (data not shown). GCS pre-treatment of PAF prior to IAV infection decreased IL-6, IL-8 and IP-10 production at 48 hrs post-infection but had no effect on MCP-1 production (Fig. 2B). Production of IP-10 was not altered by GCS pre-treatment of PAF prior to RV infection and levels of IL-6, IL-8 and MCP-1 were not increased by RV infection alone at 48 hrs post-infection (Fig. 2B). There was no significant production of RANTES by PAF following IAV or RV infection (data not shown). Finally, GCS pre-treatment of PAM reduced levels of IL-6, IL-8 and TNFα at 24 hrs following IAV infection, as well as IL-8 and IP-10 following RV infection (Fig. 2C). Significant production of IL-1β, MCP-1 or RANTES by PAM was not observed in response to RV or IAV infection (data not shown). Taken together these in vitro studies demonstrate that GCS inhibit anti-viral responses and confirm the reported anti-inflammatory actions of GCS in vitro.
GCS pre-treatment of primary human airway cells reduces the production of pro-inflammatory cytokines following virus infection.
Monolayers of (A) PBEC, (B) PAF or (C) PAM were treated with GCS for 24 hrs, washed and then infected with RV or IAV. Concentrations of cytokines in cell culture supernatants were determined by CBA at 24 or 48 hrs post-infection. The detection limit of each mediator is indicated as a dotted line. Data represents the mean of a minimum of 3 replicate samples ± SD and is representative of cultures from a minimum of 3 independent donors. Levels significantly reduced in virus-infected samples treated with GCS, * p < 0.05, ** p < 0.01, *** p < 0.001, one-way ANOVA and Tukey's post-test.
GCS treatment enhances viral replication in primary human airway cells
IAV and RV infection of airway epithelial cells and fibroblasts leads to virus replication21,22. In contrast, resident alveolar macrophages are susceptible to IAV and RV infection but virus replication is limited23,24. We investigated if the GCS-mediated impairment of anti-viral responses in primary human airway cells we observed (Fig. 1) was associated with changes in virus infection and/or replication.
Treatment of PBEC and PAF with GCS for 24 hrs prior to IAV infection significantly increased the levels of infectious virus in cell supernatants 24, 48 and 72 hrs following infection (Fig. 3A, left panels). In agreement with previous reports18,25, GCS pre-treatment of PBEC did not alter RV replication at 24 or 48 hrs following infection but levels of infectious virus in supernatants from PBEC were significantly increased by GCS at 72 hrs. In addition, we did not observe any significant differences in viral titers 24 hrs following RV infection of PAF (Fig. 3A, right panel), as described by Val Ly et al15. We did, however, detect elevated viral replication in GCS pre-treated PAF at 48 and 72 hrs following RV infection. In addition, the GCS-mediated elevation of infectious RV in cell supernatants correlated with significant increases in viral RNA isolated from PBEC and PAF (Supplementary Fig. S1). No substantial virus amplification was detected between 2 and 24 hrs following IAV or RV infection of PAM (data not shown). Immunofluorescent staining for viral proteins indicated that GCS pre-treatment of PBEC, PAF or PAM did not significantly alter the proportion of cells infected at 8 hrs following RV or IAV infection (Supplementary Table S1). This finding indicates that the observed effects on viral titers were due to enhanced virus replication overall rather than being the result of greater numbers of cells primarily infected.
GCS pre-treatment of primary human airway cells enhances viral replication; an effect blunted by IFN.
PBEC or PAF were treated with GCS for 24 hrs, washed and then infected with IAV (left panels) or RV (right panels). (A) Levels of infectious virus in cell supernatants were determined by plaque assay (IAV) or titration (RV). Data represent the mean ± SD from triplicate samples and are representative of a minimum of cultures from 3 independent donors. Infectious virus in cell supernatants significantly increased with GCS treatment, * p < 0.05, *** p < 0.001, Student's t-test. (B) At 1 hr following IAV or RV infection, monolayers were stimulated with 250 IU/ml of human IFNα2, IFNβ or IFNλ1 and levels of infectious virus in cell supernatants were determined at the time points indicated. The detection limit of the assay is indicated as a dotted line. Data represent the mean ± SD from triplicate samples and are representative of a minimum of cultures from 3 independent donors. Infectious virus in cell supernatants significantly reduced by addition of IFN in both GCS treated and mock-treated infected cells, * p < 0.05, ** p < 0.01, *** p < 0.001, one-way ANOVA and Tukey's post-test.
We have demonstrated that pre-treatment of PBEC and PAF with fluticasone propionate (GCS) increases virus replication (Fig. 3A). We next examined the effects of additional GCS routinely used for the management of respiratory diseases, such as dexamethasone (Dex) and budesonide (Bud), on virus replication. Treatment of PBEC with 10 nM Dex or 10 nM Bud for 24 hrs prior to IAV infection resulted in increased levels of infectious virus in cell supernatants at 24, 48 and 72 hrs post-infection (Supplementary Fig. S2).
Type I and III IFNs counteract the effect of GCS on virus replication in primary human airway cells
We next examined the ability of human type I and III IFNs to reduce the impact of GCS on viral replication in primary human airway cells. It has been reported that fibroblasts do not respond to IFNλ26. We therefore performed initial studies to evaluate whether stimulation of PBEC, PAF or PAM with human IFNα2, IFNβ or IFNλ1 (250 IU/ml) increased mRNA expression of ISGs. Addition of IFNα2 or IFNβ to PBEC, PAF and PAM resulted in significant induction of ISG15, IFIT1 and viperin at 3 hrs following stimulation. However, as expected only PBEC and PAM responded to IFNλ1 (data not shown).
We next pre-treated PBEC and PAF with GCS for 24 hrs, infected with IAV or RV for 1 hr and then stimulated with human IFN or media alone. Addition of IFNα2, IFNβ or IFNλ1 to GCS pre-treated PBEC reduced the levels of infectious RV and IAV in cell supernatants compared to control cells not treated with IFN (Fig. 3B). Furthermore, addition of IFNα2 or IFNβ to GCS-treated PAF 1 hr following infection significantly lessened RV and IAV titers.
Treatment of mice with GCS prior to IAV infection results in the induction of severe disease associated with amplified viral replication
Having established in vitro that GCS treatment of primary human airway cells dampens the innate anti-viral response (Fig. 1) and enhances viral replication (Fig. 3), we treated primary mouse airway epithelial cells (mAEC) cultured from C57BL/6 mice with GCS in vitro for 24 hrs prior to IAV infection (HKx31, H3N2). Consistent with our experiments in human PBEC, GCS pre-treatment of primary mAEC significantly increased IAV replication at 24 and 48 hrs following infection (Fig. 4A).
Mice treated with GCS prior to IAV infection develop severe disease.
(A) Monolayers of primary mouse airway epithelial cells (mAEC) were treated with GCS for 24 hrs, washed and infected with IAV (HKx31, MOI 1). Levels of infectious virus in cell supernatants were determined by plaque assay at 24 and 48 hrs post-infection. Bars represent the mean ± SD from triplicate samples. Viral titer significantly increased with GCS treatment, *** p < 0.001, Student's t-test. (B) Groups of 5 C57BL/6 mice were treated with 20 μg GCS via the intranasal route 48 hrs and 24 hrs prior to inoculation with 102 PFU of IAV (HKx31). Mice received additional doses of GCS 24 hr post-infection and every 48 hrs thereafter. Uninfected mice treated with PBS or GCS were included for comparison. Mice were observed daily for weight loss (left panel). Mice which had lost ≥15% of their original body weight were euthanized. Data represents the mean % weight change ± SEM. Survival plots are shown (right panel). (C) Titers of infectious virus in lung (left panel) and nasal tissue (right panel) homogenates were determined by plaque assay at days 1, 3 and 5 post-infection. Bars represent the mean viral titer from a group of 5 mice ± SD. Virus titers from GCS-treated mice were significantly higher than those from PBS-treated mice, *** p < 0.001, one-way ANOVA and Tukey's post-test. Data is representative of a minimum of 2 independent experiments.
We next used a well-characterized mouse model of IAV infection (HKx31) to examine the effects of GCS treatment in vivo. Mice were treated with GCS (20 μg) or PBS alone via the intranasal route 48 and 24 hrs prior to infection with 102 PFU of IAV. Mice received additional doses of GCS 24 hrs following infection and every 48 hrs thereafter. This GCS dose schedule is comparable to the doses of inhaled GCS given to humans and has been used in other studies27,28. Animals were monitored daily for changes in body weight and survival over an 8-day period. GCS-treated mice infected with IAV lost significant weight, displayed signs of disease (inactivity and ruffled fur) and all mice were euthanized 5 days following infection (Fig. 4B). In contrast, IAV-infected mice treated with PBS did not lose weight or display visible signs of disease over the 5-day period, nor did uninfected PBS or GCS-treated control animals (Fig. 4B).
We next examined the viral loads in the upper (nasal tissues) and lower (lung) respiratory tract of IAV-infected mice treated with PBS or GCS. Viral loads were significantly elevated in the lung and nasal tissues of GCS-treated mice compared to PBS-treated controls on days 1, 3 and 5 following IAV infection (Fig. 4C).
GCS treatment of mice results in heightened inflammatory responses in the airways following IAV infection
The cellular infiltrate and pro-inflammatory cytokines produced in the airways could be critical factors contributing to the enhanced disease severity observed in GCS-treated mice infected with IAV. The cellular inflammatory response to IAV infection was assessed in the airways via flow cytometry analysis of bronchoalveolar lavage (BAL) fluid. Mice were treated with GCS or PBS 48 and 24 hrs prior to infection with IAV as described previously. At days 3 and 5 following IAV infection, no differences were noted in the total numbers of CD45+ leukocytes in the BAL fluid between GCS and PBS-treated mice (Fig. 5A). Increased numbers of neutrophils were detected in the airways of GCS-treated mice at day 3 post-infection (Fig. 5A). Airway macrophages (AM), dendritic cells (DCs) and inflammatory macrophages (IM) numbers in the BAL fluid were decreased by GCS treatment at day 3 but not at day 5 post-infection (Fig. 5A).
Treatment of mice with GCS alters the inflammatory response in the airways.
Groups of 5 C57BL/6 mice were treated with 20 μg GCS via the intranasal route 48 hrs and 24 hrs prior to inoculation with 102 PFU of IAV (HKx31). Mice received additional doses of GCS 24 hrs post-infection and every 48 hrs thereafter. Uninfected mice treated with PBS or GCS were included for comparison. At days 3 and 5 post-infection, mice were sacrificed and BAL performed. (A) BAL cells were examined by flow cytometry for the presence of CD45+ leukocytes, neutrophils (Neut), airway macrophages (AM), dendritic cells (DC) and inflammatory macrophages (IM). Bars represent the mean cell number ± SD. Data is representative of 2 independent experiments. Cell numbers from GCS-treated IAV-infected mice were significantly different compared to PBS-treated IAV-infected mice, * p < 0.05, ** p < 0.01, *** p < 0.001, one-way ANOVA and Tukey's post-test. (B) Concentrations of cytokines in BAL supernatants were determined by CBA at days 3 and 5 post-infection. Bars represent the mean concentration ± SD. The detection limit of each assay is indicated as a dotted line. Data is representative of 2 independent experiments. Levels from GCS-treated mice that were significantly elevated compared to PBS-treated, infected with IAV, * p < 0.05, ** p < 0.01, *** p < 0.001, one-way ANOVA and Tukey's post-test.
We next examined levels of cytokines in BAL fluids from IAV-infected mice. Significantly elevated levels of IL-6 and MCP-1 were detected in the BAL fluid from mice treated with GCS compared to PBS controls, at day 3 and 5 post-infection (Fig. 5B). Levels of TNFα and KC were increased in GCS-treated mice at day 3 but not at day 5 post-infection. No differences were seen in the levels of RANTES or IFNγ at either time point (data not shown).
Treatment of mice with GCS prior to IAV infection inhibits the anti-viral response
Having established that GCS treatment in mice prior to IAV infection results in more severe disease, enhanced viral replication and an increased inflammatory response, we sought to examine if treatment of mice with GCS alters the anti-viral response elicited following IAV infection. Mice were treated with GCS and infected with IAV, as previously described. At day 1 following IAV-infection, GCS-treated mice had significantly reduced levels of IFNα, IFNβ and IFNλ2 proteins in BAL fluid (Fig. 6A). Furthermore, at day 2 post-infection, mRNA expression of Ifnα and Ifnλ2 as well as the ISGs Ifit1, Ifit2 and Isg15, were significantly reduced in lung tissue from mice treated with GCS (Fig. 6B–C).
GCS treatment of mice inhibits the induction of the anti-viral response following IAV infection.
Groups of 5–7 mice were treated with 20 μg GCS via the intranasal route 48 hrs and 24 hrs prior to inoculation with 102 PFU of IAV (HKx31). Mice received an additional dose of GCS 24 hrs post-infection. Uninfected PBS and GCS controls were included for comparison. (A) Mouse IFNα, IFNβ and IFNλ2 protein levels in BAL fluids 24 hrs post-infection were determined by ELISA. Bars represent the mean concentration ± SD. The detection limit of each assay is indicated as a dotted line. mRNA expression of (B) IFN genes Ifnα, Ifnβ and Ifnλ2 and (C) anti-viral genes Ifit1, Ifiti2 and Isg15, in lung tissue 48 hrs post-infection was detected by RT-PCR. Data is relative to the expression of Gapdh. Bars represent the mean ± SD. Data is representative of 2 independent experiments. Significantly reduced compared to PBS-treated IAV-infected mice, ** p < 0.01, *** p < 0.001, one-way ANOVA and Tukey's post-test.
A single intranasal treatment of IFN delays the onset of severe disease in GCS-treated animals
As we had established a deficiency in the anti-viral response in mice treated with GCS, we next evaluated the ability of intranasal administration of type I and III IFNs to lessen disease severity in these mice. Mice were treated with GCS or PBS alone prior to and during infection with IAV, as previously described. GCS-treated mice were administered a single dose (3000 IU) of mouse IFNα1, IFNβ or IFNλ2 via the intranasal route 24 hrs post-infection. Mice were monitored daily for changes in body weight (Fig. 7A) and survival (Fig. 7B) over an 11-day period. GCS-treated mice that did not receive IFN developed severe disease and were euthanized 5 days following IAV infection. In contrast, GCS-treated mice that received IFNα1, IFNβ or IFNλ2 were euthanized on days 7 (IFNα1) and 9 (IFNβ or IFNλ2) post-infection.
Intranasal administration of recombinant IFN following IAV infection improves the severe disease observed in GCS-treated mice.
Groups of 5 C57BL/6 mice were treated with 20 μg of GCS via the intranasal route 48 hrs and 24 hrs prior to inoculation with 102 PFU of IAV (HKx31). Mice received additional doses of GCS at 24 hrs post-infection and every 48 hrs thereafter. At day 1 post-infection, GCS-treated mice were administered 3000 IU of mouse IFNα1, IFNβ or IFNλ2 via the intranasal route. (A) Mice were weighed daily and data represents the mean % weight change ± SEM. Animals that had lost ≥15% of their original body weight were euthanized. (B) Survival curves are shown. (C) Titers of infectious virus in lung homogenates were determined by plaque assay at day 2 post-infection (24 hrs following IFN treatment). Bars represent the mean viral titer from a group of 5 mice ± SD. Virus titers from GCS-treated mice treated with IFN were significantly lower than GCS-treated mice not treated with IFN, *** p < 0.001, one-way ANOVA and Tukey's post-test.
We also examined viral loads in the respiratory tract of GCS-treated, IAV-infected mice treated with IFN or PBS alone. Viral loads were significantly reduced in the lungs and nasal tissues of GCS-treated mice that received intranasal IFNα1, IFNβ or IFNλ2, compared to GCS-treated mice that received PBS alone, at day 2 following IAV infection (Fig. 7C).
Discussion
In this proof-of-concept study we demonstrate in vitro and in vivo that GCS treatment increases virus replication in the respiratory tract. The mechanism is dampened type I and III IFN production with diminished downstream IFN-regulated responses. GCS treatment of mice also altered inflammatory cell profiles and caused a paradoxical increase in pro-inflammatory cytokines in the airways accompanied by enhanced disease severity. Taken together our findings highlight the complex and potentially detrimental impact of GCS on respiratory tract virus infections.
The interaction between GCS and virus infection is controversial. In contrast to our findings, Bochkov et al found no effect of the GCS budesonide on RV replication or IFN production in vitro18. However, the GCS dose was high (approximately 170 times higher than in the current study) which may have suppressed cellular ICAM expression and concealed increased virus replication. The 24 hr time point may also have been too early to detect increased replication since this only occurred at 72 hrs (see Fig. 3A). Also in contrast to our results with a group A RV strain, Suzuki et al demonstrated that GCS treatment of human tracheal epithelial cells reduced replication of a genetically distinct group B strain (RV14)29. Although IFN responses were not reported and investigational protocols were different, these findings suggest that the effect of GCS on virus infections may vary depending on cell type and experimental factors.
The effect of GCS on IFN responses is also not clear since asthma itself may be associated with higher IFN production during virus exacerbations30,31. Miller et al detected raised IFN-λ1 in children with wheeze30 and IFN-γ was raised in another clinical study31. Neither study investigated separately the effect of GCS treatments on virus replication and IFN production. Assays for IFNs were performed on nasal secretions and induced sputum and not in airway epithelial cells and further research is warranted.
Analogous clinical studies have been limited by methodological constraints. A large retrospective study found no evidence of excess risk of pneumonia in asthma32 and another study reported that GCS is equally effective in cold-related and unrelated asthma exacerbations33. Nevertheless, prospective studies have never been done employing virus sampling as well as accurate diagnosis of pneumonia and these will be required to verify safety of GCS in the setting of virus infections and asthma exacerbations.
There are strong indications that type I and III IFN gene expression is reduced in patients with moderate25,34 and severe35 atopic asthma and this phenomenon has also been reported in COPD36. Impairment is associated with increased RV replication25,34. Importantly, individuals with mild/well-controlled asthma37,38 and mild asthma39 displayed no differences in IFN levels suggesting that reduced IFN production may be the consequence of airway inflammation and connected to disease severity. A key consideration is that moderate and severe asthmatics and patients with COPD are invariably treated with GCS that may cause immune suppression, more so at higher doses. Intrinsic disease-related immune suppression has thus made it problematic to investigate whether extrinsic factors (GCS) contribute to a blunted immune response. This is further complicated by anti-inflammatory benefits of GCS that may obscure their detrimental actions. With this perspective we have excluded the effect of underlying lung disease and primarily examined GCS activities in healthy human lung cells in vitro and an in vivo mouse model. Additionally, we have examined the effect of a single dose of GCS treatment of human cells in vitro, which may underestimate the effects of repetitive use of GCS by patients with asthma or COPD.
GCS in clinically relevant doses increased virus replication but we did not observe significant reductions in the expression of IFNα, IFNβ and IFNλ genes in PBEC, PAF or PAM treated with GCS prior to RV or IAV infection (Fig. 1). This was not unexpected since IFN responses are transient, peaking at variable times, therefore changes may be difficult to detect in vitro. However, our in vivo studies unambiguously demonstrated that mRNA expression and protein levels of IFNα, IFNβ and IFNλ were significantly reduced in the lungs of GCS-treated mice following IAV infection (Fig. 6). As an alternative approach we also measured ISG expression since they are reliable surrogate indicators of IFN-signaling20. As shown, GCS reduced the expression of ISGs such as IFIT1 and ISG15 (Fig. 1), whilst increasing virus replication (Fig. 3, Supplementary Fig. S2), in both primary human airway cells and mouse lung (Fig. 4C). In the mouse model GCS-mediated enhanced infection was associated with more severe illness and in human disease it is possible that amplified virus infections may predispose to more frequent bacterial secondary infections and pneumonia40,41. Higher levels of virus infection may also oppose some of the beneficial anti-inflammatory actions of GCS as suggested by findings noted in our mouse model.
GCS treatment of human PBEC, PAF and PAM inhibited production of pro-inflammatory cytokines such as IL-8 and IL-6, following virus infection (Fig. 2) but this contrasted with responses in our mouse model. In mice, GCS treatment was associated with an increase in neutrophils and a reduction in dendritic cell (DC), airway macrophage (AM) and inflammatory macrophage (IM) numbers, 3 days following infection (Fig. 5A). In addition, GCS-treated mice displayed elevated levels of the cytokines IL-6, MCP-1 and KC in the airways (Fig. 5B). The usual anti-inflammatory properties of GCS may therefore be counterbalanced in vivo by enhancement of virus replication and augmented inflammatory responses. This observation is in accord with BAL and biopsy studies that have shown that GCS do not prevent airway inflammation caused by RV infection of both healthy and asthmatic volunteers42,43.
GCS therapies have been implicated in the development of pneumonia in asthma and COPD in some7,8 but not all studies32. In addition, GCS may have limited ability to prevent virus exacerbations9,10. Given the anti-inflammatory clinical benefits of GCS in these diseases, the development of improved preventive therapies or strategies to counter virus infections will be a significant advance. IFNα and IFNβ have been used therapeutically to treat several conditions such as viral hepatitis and multiple sclerosis and a recent study of inhaled IFNβ in asthma demonstrated safety and efficacy in patients with disease exacerbations44. In the mouse model, intranasal delivery of IFNα, IFNβ or IFNλ2 into the lung of GCS-treated mice 24 hours following infection delayed the onset of disease by several days (Fig. 7A/B) and reduced viral loads (Fig. 7C). This approach is feasible since the type I IFN receptor complex (IFNAR1/2) is ubiquitously expressed on all cell types, while the type III receptor (IFNλR1) is selectively expressed on epithelial cells, such as those that line the airways (reviewed by45). Recent studies have suggested that type III IFNs could provide a therapeutic alternative over type I IFNs, as they appear to induce fewer side effects, possibly due to their cell-specific actions46. Inhaled IFNλ may therefore be a potential therapeutic adjuvant for improved treatment of virus infections in patients undergoing GCS therapy and further studies are needed.
In summary, our findings indicate that GCS suppress host innate immune responses, reducing cardinal early protective mechanisms and causing more severe infections. We also demonstrate the potential of IFNs to offset the impact of GCS on innate immune responses. Overall, although GCS therapy can be beneficial, our studies provide a rationale for further studies to examine GCS activities and the potential of IFN as an adjuvant therapy for individuals who rely on GCS treatments.
Methods
Culture of primary human airway cells
Primary human airway cells were obtained from normal subjects whom were non-smokers or had not smoked for >15 years and none had a diagnosis of asthma or COPD (normal FEV1 measurements). Studies were approved by the Monash Health and Monash Medical Centre Human Research Ethics Committee, consent was obtained from all subjects and studies were conducted in accordance with the approved guidelines. Primary bronchial epithelial cells (PBEC) were obtained from bronchial brushings and cultured under submerged conditions on collagen-coated flasks (MP Biomedicals, USA) in supplemented bronchial epithelial growth medium (BEGM; Lonza, Australia). Primary airway fibroblasts (PAF) were obtained from bronchial tissue obtained from resection or biopsy as described previously21. All bronchial biopsies and brushings were obtained from the same anatomical regions (bronchial generations 4–7) and were used within 5 passages. Primary airway macrophages (PAM) were obtained via bronchoalveolar lavage (BAL) during routine bronchoscopy and cultured overnight before experimentation. PAF and PAM were cultured in minimum essential medium (MEM, Gibco, USA) supplemented with 10% FCS, 2 mM L-glutamine, 100 U/ml penicillin and 100 μg/ml streptomycin.
Virus infection and GCS treatment of primary human airway cells
Human RV serotype 16 and the seasonal IAV strain A/Solomon Islands/3/2006 (H1N1) were propagated, purified and titrated as previously described21,23. Preliminary experiments were performed to determine the optimal virus dose for each cell type. Human airway cells were treated with 10 nM fluticasone propionate (GCS, Sigma Aldrich, USA) or diluent alone (mock) for 24 hrs in 24-well plates. Cell counts were performed to ensure GCS did not significantly alter cell numbers 24 hrs following treatment. In some experiments, cells were treated for 24 hrs with 10 nM dexamethasone (Dex; Sigma Aldrich, USA) or 10 nM budesonide (Bud; AstraZeneca, Australia).
Primary human airway cells (approximately 80% confluency) were washed and infected with RV or IAV in serum free MEM or BEGM without hydrocortisone for 1 hr at a multiplicity of infection (MOI) of 1 (PBEC), 3 (PAF) or 5 (PAM). Cell monolayers were then washed and incubated in BEGM without hydrocortisone (PBEC) or MEM supplemented with 2% FCS (PAF and PAM). Samples infected with IAV were cultured in the presence of 4 μg/ml trypsin to permit multiple rounds of replication.
In some experiments, primary human cells were treated with GCS for 24 hrs, infected and then incubated in media containing 250 IU/ml human IFNα2a (Roferon-A, Roche, USA), IFNβ1a (Rebif 44, Merck, Germany) or IFNλ1 (PBL Interferon Source, USA) for 24, 48 or 72 hrs.
Levels of infectious virus in primary cell culture supernatants were determined at 24, 48 and 72 hrs following infection by titration on Ohio Hela cells (RV) or by standard plaque assay on MDCK cells (IAV). To examine virus infection, cells were fixed at 8 hrs post-infection with 80% acetone and then stained with anti-nuclear protein (IAV) or anti-3C protease (RV) antibodies (a gift from James Gern, Madison, WI), as previously described23.
Gene expression in human airway cells
Total RNA was isolated from frozen primary human cell lysates 24 and 48 hrs following RV or IAV infection using TRI Reagent (Molecular Research Centre, Cincinnati, USA) and reverse transcription performed using Multiscribe Reverse Transcriptase (Invitrogen, USA). RT-PCR reactions were performed using FastStart SYBR Green Master Mix (Roche, USA) on a Corbett Rotor-Gene 3000 machine21. Gene expression was calculated relative to 18S. See Supplementary Table S2 in the supplemental material for target genes and primer sequences. Viral RV RNA was quantified as previously described21.
Detection of human cytokines
Levels of cytokines in primary human cell supernatants were determined at 24 and 48 hrs following virus infection by Cytometric Bead Array (CBA) Human Inflammation and Chemokine Kits (BD Biosciences, USA). Levels of human IFNα in cell supernatants were determined by sandwich ELISA using mouse monoclonal (clone MMHA-11) and rabbit polyclonal antibodies (PBL Interferon Source, USA). Human IFNλ2 was quantified by ELISA (R&D Systems, USA).
Preparation and infection of primary mouse airway epithelial cells (mAEC)
Mouse AEC cultures were prepared from female C57BL/6 mice as previously described22, with minor modifications. Briefly, lungs from mice were digested in 1.5 mg/ml Pronase (Roche, USA), 0.1 mg/ml DNase I (Sigma-Aldrich, USA) for 1 hr at 37°C in 5% CO2. Single cell suspensions were incubated with purified rat anti-mouse CD45 antibody (BD Biosciences, USA) and epithelial cells negatively enriched with BioMag goat anti-rat Ig-coupled magnetic beads (Qiagen, USA). Cells were cultured on collagen-coated (MP Biomedicals, USA) plates in DMEM/F-12 media (Gibco, USA) supplemented with 10% FCS, 2 mM L-glutamine, 100 U/ml penicillin, 100 μg/ml streptomycin and 5 μg/ml insulin (Sigma-Aldrich). To confirm cell purity, monolayers were detached with 3 mM EDTA and cells stained with mouse anti-EpCAM antibodies (BioLegend, USA) and examined by flow cytometry. Cell monolayers were negative for the presence of fibroblasts (anti-mouse vimentin (Santa Cruz, USA)). Monolayers were infected with the HKx31 strain of IAV (H3N2, MOI 1) in serum free DMEM/F-12 for 1 hr and then washed and incubated in DMEM/F-12 supplemented with 2% FCS and 4 μg/ml trypsin for 24 or 48 hrs.
Influenza virus infection and treatment of mice
Mice (6–8 week old female C57BL/6) were anesthetized and infected with 102 PFU of HKx31 (H3N2) via the intranasal (i.n.) route in 50 μl PBS. Groups of 5 mice were treated i.n. with 20 μg fluticasone propionate diluted in 50 μl PBS or PBS alone for 48 and 24 hrs prior to infection and additional doses 24 hrs post-infection and every 48 hrs thereafter. In some experiments, mice were treated i.n. with 3000 IU of mouse IFNα1, IFNβ or IFNλ2 (PBL Interferon Source, USA) in 50 μl of PBS, 24 hrs post-infection.
Mice were weighed daily and assessed for visual signs of clinical disease, including inactivity, ruffled fur, labored breathing and huddling behavior. Animals that had lost ≥15% of their original body weight were euthanized. Research was approved by the Monash University Animal Ethics Committee and studies were conducted in accordance with the approved guidelines. Levels of infectious virus in lung and nasal tissue homogenates were determined by standard plaque assay on MDCK cells.
Recovery and characterization of leukocytes in the airways of mice
BAL cells were obtained and analysed by flow cytometry as previously described23. For flow cytometric analysis, BAL cells were incubated with supernatants from hybridoma 2.4G2 to block Fc receptors, followed by staining with monoclonal antibodies to CD45, Ly6C, Ly6G, CD11c and I-Ab (BD Biosciences, USA). Leucocytes, neutrophils, airway macrophages (AM) and dendritic cells (DC) were identified as described previously23. Inflammatory macrophages (IM) were identified as Ly6G− Ly6C+. Living cells (propidium iodine negative) were analysed using a BD FACS Canto II flow cytometer (BD Biosciences, USA).
Detection of cytokines in mouse BAL fluids
Levels of cytokines in BAL fluid of mice were determined using Cytometric Bead Array (CBA) Mouse Inflammation or Flex Kits (BD Biosciences, USA). Levels of mouse IFNα were determined by sandwich ELISA using mouse monoclonal (clone F18, Thermo Scientific, USA) and rabbit polyclonal antibodies (PBL Interferon Source, USA). Levels of mouse IFNβ were determined by sandwich ELISA using mouse monoclonal (clone 7F-D3, Abcam, UK) and rabbit polyclonal antibodies (PBL Interferon Source, USA). Mouse IFNλ2 was quantified by ELISA (R&D Systems, USA).
Analysis of gene expression in mouse lung tissue
Lungs were excised from mice and immediately frozen in liquid nitrogen. Total RNA was extracted using TRIsure (Bioline, UK). RNA (1 μg) was DNase-treated (Promega, USA) and reverse-transcribed to cDNA using M-MLV reverse transcriptase (Promega, USA), according to the manufacturer's instructions. RT-PCR reactions were performed using SYBR Green (Invitrogen, USA) on an Applied Biosystems 7900HT Fast Real-Time PCR Machine. Gene expression was calculated relative to the housekeeping gene Gapdh. See Supplementary Table S2 for target genes and primer sequences.
Statistical analyses
For comparison of two sets of values, Student's t-test (two-tailed, two-sample equal variance) was used. When comparing ≥ three sets of values, data were analyzed by one-way ANOVA and Tukey's multiple comparison test.
References
Dulek, D. E. & Peebles, R. S., Jr Viruses and asthma. Biochim. Biophys. Acta. 1810, 1080–1090 (2011).
Singanayagam, A., Joshi, P. V., Mallia, P. & Johnston, S. L. Viruses exacerbating chronic pulmonary disease: the role of immune modulation. BMC Med. 10, 27 (2012).
Bergman, H., Livornese, L. L., Jr, Sambhara, S., Santoro, J. & Dessain, S. K. Patients Hospitalized with pH1N1 Influenza in an Academic Community Medical Center. Open Respir Med J. 5, 19–23 (2011).
Zarogoulidis, P. et al. Long-term respiratory follow-up of H1N1 infection. Virol J. 8, 319 (2011).
Nannini, L. J., Poole, P., Milan, S. J., Holmes, R. & Normansell, R. Combined corticosteroid and long-acting beta2-agonist in one inhaler versus placebo for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 11, CD003794 (2013).
White, P., Thornton, H., Pinnock, H., Georgopoulou, S. & Booth, H. P. Overtreatment of COPD with Inhaled Corticosteroids - Implications for Safety and Costs: Cross-Sectional Observational Study. PLoS One. 8, e75221 (2013).
McKeever, T., Harrison, T. W., Hubbard, R. & Shaw, D. Inhaled corticosteroids and the risk of pneumonia in people with asthma: a case-control study. Chest. 144, 1788–1794 (2013).
Suissa, S., Patenaude, V., Lapi, F. & Ernst, P. Inhaled corticosteroids in COPD and the risk of serious pneumonia. Thorax. 68, 1029–1036 (2013).
Ducharme, F. M. et al. Preemptive use of high-dose fluticasone for virus-induced wheezing in young children. N. Engl. J. Med. 360, 339–353 (2009).
Price, D., Yawn, B., Brusselle, G. & Rossi, A. Risk-to-benefit ratio of inhaled corticosteroids in patients with COPD. Prim Care Respir J. 22, 92–100 (2013).
Puhakka, T. et al. The common cold: effects of intranasal fluticasone propionate treatment. J. Allergy Clin. Immunol. 101, 726–731 (1998).
Gustafson, L. M., Proud, D., Hendley, J. O., Hayden, F. G. & Gwaltney, J. M., Jr Oral prednisone therapy in experimental rhinovirus infections. J. Allergy Clin. Immunol. 97, 1009–1014 (1996).
Skevaki, C. L. et al. Budesonide and formoterol inhibit inflammatory mediator production by bronchial epithelial cells infected with rhinovirus. Clin. Exp. Allergy. 39, 1700–1710 (2009).
Edwards, M. R., Haas, J., Panettieri, R. A., Jr, Johnson, M. & Johnston, S. L. Corticosteroids and beta2 agonists differentially regulate rhinovirus-induced interleukin-6 via distinct Cis-acting elements. J. Biol. Chem. 282, 15366–15375 (2007).
Van Ly, D. et al. Effects of beta(2) Agonists, Corticosteroids and Novel Therapies on Rhinovirus-Induced Cytokine Release and Rhinovirus Replication in Primary Airway Fibroblasts. J Allergy (Cairo). 2011, 457169 (2011).
Davies, J. M. et al. Budesonide and formoterol reduce early innate anti-viral immune responses in vitro. PLoS One. 6, e27898 (2011).
Edwards, M. R., Johnson, M. W. & Johnston, S. L. Combination therapy: Synergistic suppression of virus-induced chemokines in airway epithelial cells. Am. J. Respir. Cell Mol. Biol. 34, 616–624 (2006).
Bochkov, Y. A. et al. Budesonide and formoterol effects on rhinovirus replication and epithelial cell cytokine responses. Resp Res. 14, 98 (2013).
Wang, J. et al. Differentiated human alveolar type II cells secrete antiviral IL-29 (IFN-lambda 1) in response to influenza A infection. J. Immunol. 182, 1296–1304 (2009).
Schoggins, J. W. & Rice, C. M. Interferon-stimulated genes and their antiviral effector functions. Curr Opin Virol. 1, 519–525 (2011).
Thomas, B. J. et al. Transforming growth factor-beta enhances rhinovirus infection by diminishing early innate responses. Am. J. Respir. Cell Mol. Biol. 41, 339–347 (2009).
Tate, M. D., Schilter, H. C., Brooks, A. G. & Reading, P. C. Responses of mouse airway epithelial cells and alveolar macrophages to virulent and avirulent strains of influenza A virus. Viral Immunol. 24, 77–88 (2011).
Tate, M. D., Pickett, D. L., van Rooijen, N., Brooks, A. G. & Reading, P. C. Critical role of airway macrophages in modulating disease severity during influenza virus infection of mice. J. Virol. 84, 7569–7580 (2010).
Gern, J. E. et al. Rhinovirus enters but does not replicate inside monocytes and airway macrophages. J. Immunol. 156, 621–627 (1996).
Wark, P. A. et al. Asthmatic bronchial epithelial cells have a deficient innate immune response to infection with rhinovirus. J. Exp. Med. 201, 937–947 (2005).
Witte, K. et al. Despite IFN-lambda receptor expression, blood immune cells, but not keratinocytes or melanocytes, have an impaired response to type III interferons: implications for therapeutic applications of these cytokines. Genes Immun. 10, 702–714 (2009).
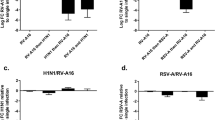
Singam, R. et al. Combined fluticasone propionate and salmeterol reduces RSV infection more effectively than either of them alone in allergen-sensitized mice. Virol J. 3, 32 (2006).
Chu, H. W., Campbell, J. A., Rino, J. G., Harbeck, R. J. & Martin, R. J. Inhaled fluticasone propionate reduces concentration of Mycoplasma pneumoniae, inflammation and bronchial hyperresponsiveness in lungs of mice. J. Infect. Dis. 189, 1119–1127 (2004).
Suzuki, T. et al. Effects of dexamethasone on rhinovirus infection in cultured human tracheal epithelial cells. Am J Physiol Lung Cell Mol Physiol. 278, L560–571 (2000).
Miller, E. K. et al. A mechanistic role for type III IFN-lambda1 in asthma exacerbations mediated by human rhinoviruses. Am. J. Respir. Crit. Care Med. 185, 508–516 (2012).
Schwantes, E. A. et al. Interferon gene expression in sputum cells correlates with the Asthma Index Score during virus-induced exacerbations. Clin. Exp. Allergy. 44, 813–821 (2014).
O'Byrne, P. M. et al. Risks of pneumonia in patients with asthma taking inhaled corticosteroids. Am. J. Respir. Crit. Care Med. 183, 589–595 (2011).
Reddel, H. K. et al. Effect of different asthma treatments on risk of cold-related exacerbations. Eur. Respir. J. 38, 584–593 (2011).
Contoli, M. et al. Role of deficient type III interferon-lambda production in asthma exacerbations. Nat. Med. 12, 1023–1026 (2006).
Edwards, M. R. et al. Impaired innate interferon induction in severe therapy resistant atopic asthmatic children. Mucosal Immunol. 6, 797–806 (2013).
Mallia, P. et al. Experimental rhinovirus infection as a human model of chronic obstructive pulmonary disease exacerbation. Am. J. Respir. Crit. Care Med. 183, 734–742 (2011).
Sykes, A. et al. TLR3, TLR4 and TLRs7-9 Induced Interferons Are Not Impaired in Airway and Blood Cells in Well Controlled Asthma. PLoS One. 8, e65921 (2013).
Sykes, A. et al. Rhinovirus-induced interferon production is not deficient in well controlled asthma. Thorax. 69, 240–246 (2014).
Bochkov, Y. A. et al. Rhinovirus-induced modulation of gene expression in bronchial epithelial cells from subjects with asthma. Mucosal Immunol. 3, 69–80 (2010).
McCullers, J. A. The co-pathogenesis of influenza viruses with bacteria in the lung. Nat Rev Microbiol. 12, 252–262 (2014).
Molyneaux, P. L. et al. Outgrowth of the bacterial airway microbiome after rhinovirus exacerbation of chronic obstructive pulmonary disease. Am. J. Respir. Crit. Care Med. 188, 1224–1231 (2013).
Grunberg, K. et al. Rhinovirus-induced airway inflammation in asthma: effect of treatment with inhaled corticosteroids before and during experimental infection. Am. J. Respir. Crit. Care Med. 164, 1816–1822 (2001).
de Kluijver, J. et al. Interleukin-1beta and interleukin-1ra levels in nasal lavages during experimental rhinovirus infection in asthmatic and non-asthmatic subjects. Clin. Exp. Allergy. 33, 1415–1418 (2003).
Djukanovic, R. et al. The Effect of Inhaled IFN-beta on Worsening of Asthma Symptoms Caused by Viral Infections. A Randomized Trial. Am. J. Respir. Crit. Care Med. 190, 145–154 (2014).
Levy, D. E., Marie, I. J. & Durbin, J. E. Induction and function of type I and III interferon in response to viral infection. Curr Opin Virol. 1, 476–486 (2011).
Donnelly, R. P., Dickensheets, H. & O'Brien, T. R. Interferon-lambda and therapy for chronic hepatitis C virus infection. Trends Immunol. 32, 443–450 (2011).
Acknowledgements
This work was supported by the Victorian State Government Operational Infrastructure Scheme. M.D. Tate and P.J. Hertzog were funded by National Health and Medical Research Council (NHMRC) of Australia Fellowships. B.J. Thomas was funded by Monash Lung & Sleep and Monash Lung & Sleep Institute.
Author information
Authors and Affiliations
Contributions
B.J.T. and M.D.T. designed, performed and analysed experiments. R.A.P. performed experiments. B.J.T., P.G.B., M.D.T. and P.J.H. conceived and contributed to the experimental design and wrote the paper.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Supplementary Information
Suppmentary Information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Thomas, B., Porritt, R., Hertzog, P. et al. Glucocorticosteroids enhance replication of respiratory viruses: effect of adjuvant interferon. Sci Rep 4, 7176 (2014). https://doi.org/10.1038/srep07176
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep07176
This article is cited by
-
Effects of treatment with corticosteroids on human rhinovirus-induced asthma exacerbations in pediatric inpatients: a prospective observational study
BMC Pulmonary Medicine (2023)
-
Gasdermin D promotes hyperinflammation and immunopathology during severe influenza A virus infection
Cell Death & Disease (2023)
-
Possible harm from glucocorticoid drugs misuse in the early phase of SARS-CoV-2 infection: a narrative review of the evidence
Internal and Emergency Medicine (2022)
-
COVID-19: IgG seroconversion under intensive glucocorticoid treatment in a high-risk patient with minimal change disease
Wiener klinische Wochenschrift (2021)
-
Risk factors for hospital-acquired influenza A and patient characteristics: a matched case-control study
BMC Infectious Diseases (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.