Abstract
The aggregation of platelets on the plaque rupture site on the coronary artery is reported to cause both acute coronary syndromes (ACS) and acute myocardial infarction (AMI). While the inhibition of platelet aggregation by acetyl salicylic acid was reported to produce beneficial effects in ACS, it failed to do in AMI. The concentration of a stress induced protein (dermcidin isoform-2) was much higher in AMI than that in ACS. Incubation of normal platelet rich plasma (PRP) with dermcidin showed one high affinity (Kd = 40 nM) and one low affinity binding sites (Kd = 333 nM). When normal PRP was incubated with 0.4 μM dermcidin, the platelets became resistant to the inhibitory effect of aspirin similar to that in the case of AMI. Incubation of PRP from AMI with dermcidin antibody restored the sensitivity of the platelets to the aspirin effect. Incubation of AMI PRP pretreated with 15 μM aspirin, a stimulator of the NO synthesis, resulted in the increased production of NO in the platelets that removed the bound dermcidin by 40% from the high affinity binding sites of AMI platelets. When the same AMI PRP was retreated with 10 μM aspirin, the aggregation of platelets was completely inhibited by NO synthesis.
Similar content being viewed by others
Introduction
The aggregation of platelets by aggregating agents like ADP, l-epinephrine, collagen or thrombin is known to be an essential physiologic phenomenon in the life saving process of blood coagulation1. In contrast, excessive platelet aggregation particularly at the site of plaque rupture or fissuring on the wall of the major or medium size coronary artery is reported to result in the development of acute coronary syndrome (ACS) due to formation of thrombus (a micro aggregate of platelets embedded in fibrin mass) that led to the condition as a result of the blockade of the normal blood circulation in the heart musculature2. The blockade of normal blood circulation not only blocks the availability of the oxygenated blood but also interrupts the supply of water, nutrients and metal ions those are essential for the normal function of the heart. Although there are several platelets aggregating agents, as described above, can aggregate platelets, it has been reported that ADP induced platelet aggregation played a critically important role in the formation of the thrombus in ACS in humans3.
The excessive platelet aggregation is counteracted by several humoral inhibitors of platelets aggregation including prostacyclin4, insulin5, interferon α6 and estriol7 to achieve the systemic homoeostasis. In this context the pharmacological agents, acetyl salicylic acid (aspirin) is well known for its beneficial effect on the reduction of occurrence of ACS through its ability to inhibit platelet aggregation8. Although the aggregation of platelets on the arterial plaque rupture site may develop into ACS, the aggregation of platelets, sometime may also block the pericardial artery that might result in the cardiac cells death which appeared as dark patchy areas of infarcts developed due to the death of heart cells that ultimately could lead to acute myocardial infarction (AMI), which when massive, could result in the death of the victims9. Although >90% of the cases of AMI are the consequence of the development of the thrombus due to platelet aggregation10, severe anemia, coronary artery spasm are also known to cause AMI11.
It has been reported by many investigators that the use of aspirin, through its ability to inhibit platelet aggregation not only reduce the occurrence of death in ACS, but the compound has been reported to improve all acute syndromes associated with the condition8. Unfortunately, however, aspirin has been reported to fail to inhibit platelet aggregation in AMI12 and the use of aspirin in AMI is of little or no use in AMI13. Neither the mechanism of the resistance of the platelets to the inhibitory effect of aspirin in AMI nor the way to restore the sensitivity of the platelets to the aspirin effect that could be beneficial in AMI is currently available.
We have recently reported the appearance of a novel protein in the circulation of both ACS and AMI14. This protein has been determined to be a potent inducer of platelet aggregation and was identified to be dermcidin isoform-2 (dermcidin), a stress induced protein of Mr 11 Kda14. This protein was reported to be a powerful inhibitor of all known forms of nitric oxide syntheses (NOS). The role of protein which was found to be present >5 folds in AMI plasma than that in ACS and >40 folds than in normal plasma, was studied to determine its possible contribution in creating the resistance of platelets to the inhibitory effect of aspirin in AMI.
We also present a unique and simple way to resensitize the platelets in PRP from AMI subjects to the inhibitory effect of aspirin by the stimulation of NOS in the platelets.
Results
Effect of acetyl salicylic acid (aspirin) on the ADP and other platelet aggregating agents induced platelet aggregation in PRP from normal volunteers and from AMI subjects
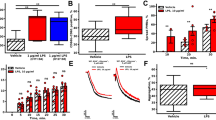
Preincubation of normal PRP with different concentrations of aspirin for 30 minutes at 37°C resulted in the maximal inhibition of platelets aggregation induced by 2 μM ADP at 80 μM of the inhibitor (fig. 1). In contrast, similar treatment of PRP from the AMI subjects with aspirin failed to inhibit the ADP induced platelet aggregation under identical condition (fig. 1). The use of aspirin for the inhibition of platelet aggregation in PRP from AMI subjects induced by either l-epinephrine (5 μM) or collagen (0.2 μg/ml) or thrombin (1 unit/ml) as aggregating agent instead of ADP also failed to produce the inhibitory effect of the compound.
The effect of aspirin on the inhibition of platelet aggregation in PRP from normal and AMI subjects induced by different platelet aggregating agents.
The PRP preparations were incubated with 80 μM aspirin for 30 minutes at 37°C. After incubation, aggregation of platelets was initiated by adding different aggregating agents as indicated. (A) = The aggregation of platelets induced by thrombin (1.0 Unit/ml) in PRP from AMI subjects treated with aspirin. (A1) = The effect of treatment of normal PRP with aspirin on the aggregation induced by thrombin. The upward increase of the transmission in both A and A1 was due to the clotting of the PRP induced by thrombin. (B) = The aggregation of platelets induced by ADP (2.0 μM) in PRP from AMI subjects treated with aspirin. (B1) = The effect of treatment of normal PRP with aspirin on the aggregation of platelets induced by ADP. (C) = The Aggregation of platelets induced by l-epinephrine (5.0 μM) in aspirin treated PRP from AMI subjects. (C1) = The effect of treatment of normal PRP with aspirin on the l-epinephrine induced platelet aggregation. (D) = The aggregation of platelets induced by collagen (2 μg/mL) in aspirin treated PRP from AMI subjects. (D1) = The effect of treatment of normal PRP with aspirin on the aggregation of platelets induced by collagen. Figures shown here are typical representatives of at least 20 sex and age matched normal volunteers and volunteers with AMI (n = 20, M = 10, F = 10).
The role of dermcidin in the development of resistance against the inhibitory effect of aspirin in the ADP induced platelet aggregation in normal PRP
To test this possibility the PRP from normal volunteers was incubated with 0.4 μM dermcidin (the concentration of dermcidin in AMI plasma was ≈0.4 μM, as described below) for 90 minutes at 37°C and the dermcidin treated PRP was subsequently used to determine the inhibition by aspirin of the ADP induced platelet aggregation. It was found that the treatment of normal PRP with dermcidin resulted in the development of résistance of the platelets to the inhibitory effect of aspirin (line A) when compared to control experiment where the normal PRP was incubated with 0.9% NaCl for 90 minutes at 37°C (line B) (Fig. 2).
The effect of incubation of normal PRP with 0.4 μM dermcidin on the aspirin treated platelet aggregation induced by ADP.
PRP was prepared from normal subjects as described in Methods and Materials. The PRP was next incubated with 0.4 μM dermcidin for 90 minutes at 37°C. After incubation, the dermcidin treated PRP was incubated with 80 μM aspirin at 37°C and aggregation of platelet was initiated by using 2.0 μM ADP. Similar results were also obtained by using other platelet aggregating agents including thrombin, l-epinephrine or collagen as described under Figure 1 (not shown in the figure). (A) = ADP induced platelet aggregation in the dermcidin treated normal PRP in presence of aspirin, (B) = ADP induced platelet aggregation in normal PRP not treated with dermcidin in presence of aspirin. The figure is a typical representative of at least 10 different experiments using blood samples from 10 different volunteers.
The concentrations of dermcidin in the plasma from normal volunteers and in the plasma of the subjects with AMI
As the PRP either from normal subjects or from the ACS subjects but not the PRP from AMI was found to be inhibited by aspirin in the ADP induced platelet aggregation, it was thought that the concentrations of dermcidin in the PRP samples might be related to the development of resistance to the inhibitory effect of aspirin. Determination of the plasma dermcidin concentrations demonstrated that while the dermcidin concentration in the normal plasma was 10 ± 3.6 nM, the dermcidin concentration in the cases of ACS as described before14 and AMI were 80 ± 4.5 nM and 400 ± 4.8 nM, (p < 0.001) respectively.
Scatchard plot analysis of the equilibrium binding of dermcidin to normal platelets
To determine whether the effect of dermcidin on the development of resistance to aspirin was mediated through the binding of the stress induced protein to the platelets, Scatchard plot analysis of the equilibrium binding of dermcidin to the normal platelets was carried out as described in the Material and Methods.
Scatchard plot of the equilibrium binding of dermcidin produced a curvilinear plot (Figure 3). The curvilinear nature of Scatchard plot suggested the presence of heterogeneous binding sites populations of dermcidin on the platelet surface i.e. one is high affinity-low capacity binding sites and another is low affinity-high capacity binding sites30. The analysis demonstrated the presence of one high affinity (Kd = 40 nM), with low capacity dermcidin binding sites (n = 128 × 103 molecules/platelet) and another low affinity (Kd = 333 nM) with high capacity binding sites (n = 189 × 103 molecules/platelet) in the normal platelet surface.
Scatchard plot of the equilibrium binding of electrophoretically purified dermcidin to the gel filtered platelets.
Gel filtered platelets were prepared from normal volunteers. The gel filtered platelets (3 × 108 platelets/mL) were incubated with 0.4 μM dermcidin for 90 minutes at 37°C. The unbound dermcidin was separated from the platelets bound dermcidin by using Millipore filtration as described in Methods and Materials. Platelets bound dermcidin was next released from the platelets by treated platelets with the 0.05% TritonX-100 and the dermcidin binding was quantitated by ELISA by using dermcidin antibody.
Effect of polyclonal antibody against dermcidin on the resistance of platelets from the AMI subjects in the inhibitory effect of aspirin
To determine the role of dermcidin further as the cause of resistance to the inhibitory effect of aspirin in platelets from the AMI subjects, the PRP from AMI subjects was incubated with dermcidin antibody for 90 minutes at 37°C. The dermcidin antibody treated PRP was subsequently challenged to the inhibitory effect of aspirin in the ADP induced platelet aggregation. It was found that the dermcidin antibody treated platelets from the AMI subjects yielded to the inhibitory effect of aspirin on the ADP induced platelet aggregation which was similar to that in the case of normal PRP (Figure 4, line B). Use of normal IgG at similar concentration had no effect on the aspirin induced inhibition on ADP due to platelets aggregation (Figure 4, line A).
Effect of incubation of PRP from AMI subjects with dermcidin antibody and the inhibitory effect of aspirin on the antibody treated platelet rich plasma.
(A) represents the PRP from AMI subjects was incubated with aspirin for 30 minutes at 37°C and aggregation of platelets was induced by ADP. (B) represents the PRP from same AMI patients treated with dermcidin antibody and subsequently treated with aspirin under identical condition like A. Figures shown here are typical representative of at least 10 experiments using PRP from 10 different AMI patients (n = 10, M = 5, F = 5).
The removal of the bound dermcidin from platelets from AMI subjects by the stimulation of NO in platelets
Dermcidin has been reported to be a potent inhibitor of nitric oxide syntheses (NOS) and the inhibition of NOS in platelets has been reported to aggregate normal platelets through the stimulation of thromboxane A2 synthesis even in the absence of the added ADP to PRP15.
As such, the effect of the stimulation of platelet's NOS on the expulsion of the platelet bound dermcidin and the consequent effect of the removal of dermcidin on the aspirin induced platelets aggregation in AMI platelets was studied.
It was found that aspirin at 15 μM was able to stimulate NO in platelets5,23 but did not inhibit platelet aggregation. On the other hand at that concentration aspirin was able to expel platelet bound dermcidin through NO from AMI PRP (figure 5). The use of 30 μUnit of insulin/mL to stimulate NO synthesis in platelets5, instead of aspirin, was also found to remove platelets bound dermcidin in PRP from AMI subjects (not shown in figure 5). The preincubation of AMI platelets in the PRP with NG-nitro-L-arginine methyl ester (L-NAME) (0.1 mM), an inhibitor of NOS16, resulted in the nullification of the effect of aspirin both in the increase of platelet NO level and in the removal of the bound dermcidin in AMI platelets (Figure 5). Furthermore, the use of NO solution (0.8 nM) in 0.9% NaCl in the place of either aspirin or insulin was also found to be able to remove the bound dermcidin from AMI platelets. On the other hand, addition of l-NAME (0.1 mM) to the PRP which itself failed to negate the removal of the platelet bound dermcidin. The absence of the effect of the l-NAME on removal of the bound dermcidin from the AMI platelets suggested that it was not the l-NAME itself that removed the bound protein from the AMI platelets. It was also found that the optimal concentration of aspirin for the removal of the dermcidin in PRP from AMI subjects was in the range of 14–15 μM. The use of higher concentration of aspirin >15 μM actually resulted not only the production of less NO in the AMI platelets, but also resulted in the removal of less amounts of the platelet bound dermcidin and at 333 μM aspirin (equivalent to 300 mg aspirin/70 kg body weight), removal of platelet bound dermcidin in the PRP from AMI subjects was decreased by ≈40% compared to that in the presence of 15 μM aspirin.
The effect of treatment of PRP from AMI subjects with 15 μM aspirin on the increase of NO and the removal bound dermcidin from the platelets.
Solid triangles ( ) represent the release of the bound dermcidin from AMI platelets treated with different concentration of aspirin as indicated. Solid squares (
) represent the release of the bound dermcidin from AMI platelets treated with different concentration of aspirin as indicated. Solid squares ( ) represent the synthesis of NO treated with different concentrations of aspirin as indicated. Solid circles (
) represent the synthesis of NO treated with different concentrations of aspirin as indicated. Solid circles ( ) represent the aspirin treated PRP from AMI with 0.1 mM NAME (an inhibitor of NO synthesis) on the release of dermcidin from the platelets. Coefficient of correlation (“r”) represents between increase of NO and release of dermcidin from AMI platelets from 0 μM to 30 μM aspirin was +0.967 and “two tailed p value” = 0.006. The figure shown is a typical representative of at least 10 different subjects with AMI.
) represent the aspirin treated PRP from AMI with 0.1 mM NAME (an inhibitor of NO synthesis) on the release of dermcidin from the platelets. Coefficient of correlation (“r”) represents between increase of NO and release of dermcidin from AMI platelets from 0 μM to 30 μM aspirin was +0.967 and “two tailed p value” = 0.006. The figure shown is a typical representative of at least 10 different subjects with AMI.
The effect of removal of the bound dermcidin from the platelets in the PRP from AMI subjects on the inhibitory effect of aspirin in the ADP induced platelet aggregation
When the PRP from the AMI subjects were preincubated with either aspirin (15 μM) for 30 min, or with insulin (30 μUnits/mL) for 2 hours or with 0.8 nM NO for 30 min at 37°C and the PRP was subsequently incubated with different concentrations of aspirin for 30 minutes at 37°C and the ADP induced platelet aggregation was initiated by using 2.0 μM ADP. It was found that the ADP induced aggregation of platelets was inhibited maximally at 10 μM aspirin in all cases (Figure 6). That contrasted the maximal inhibition of platelet aggregation in normal volunteers at 80 μM aspirin under identical conditions (Figure 1). In other word, the platelets from AMI subjects became 8 folds more sensitive to the inhibitory effect of aspirin compared to that of the normal platelets when the bound dermcidin was removed from the platelets from AMI subjects.
Effect of reexposure of PRP from the AMI subjects to 10 μM aspirin on the inhibition of ADP induced platelet aggregation in the PRP pre-treated with aspirin or insulin or NO in 0.9% NaCl.
The platelet rich plasma from the AMI subjects were incubated with either 15 μM aspirin for 30 minutes or 30 μUnit of insulin/mL for 2 hours or with 0.8 nM NO in 0.9% NaCl for 30 minutes at 37°C to remove the dermcidin bound to the platelets through the increase of platelet NO synthesis as described in the text. After incubation, the same PRP was treated with 10 μM aspirin for 30 minutes at 37°C and aggregation of the platelets was induced by using 2.0 μM ADP. (A) represents the aggregation of platelets in PRP from 3 different AMI subjects incubated with 80 μM aspirin for 30 minutes at 37°C followed by initiation of aggregation of the platelets using 2.0 μM ADP. A1 = The PRP from the same AMI subjects preincubated with 15 μM aspirin for 30 minutes at 37°C followed by treatment of the PRP with 10 μM aspirin for 30 minutes at 37°C. After incubation, the platelet aggregation was studied. A2 = The PRP from the same AMI subjects was incubated with insulin and after incubation platelet aggregation was studied by using 10 μM aspirin as described under A1. A3 = The PRP from the same AMI subjects was incubated with NO solution in 0.9% NaCl and after incubation the inhibition of platelet aggregation was studied by using 10 μM aspirin as described under A1.
The effect of preincubation of PRP from AMI subjects with aspirin, insulin or with NO in 0.9% NaCl solution on the binding characteristics of dermcidin to platelets in Scatchard plot
As the treatment of PRP from AMI subjects with aspirin, insulin or with NO in 0.9% NaCl solution all were found to restore the sensitivity of the platelets to the inhibitory effect of aspirin (figure 6), the effect of these agents on the binding characteristics of dermcidin to platelets from AMI was studied by Scatchard plot analysis (Fig. 7). It was found that the treatment of AMI platelets with the above mentioned agents decreased the binding sites (n) of dermcidin in the platelets in each case without changing the dissociation constant (Kd = 40 nM). It was found that the binding of dermcidin 128 × 103 molecules/platelet in the untreated AMI platelets decreased to 80 × 103 molecules/platelet and to 76 × 103 molecules/platelet and to 78 × 103 molecules/platelet dermcidin binding sites when the AMI platelets were treated with aspirin, insulin and NO solution respectively.
Scatchard plot of the equilibrium binding of dermcidin on platelets from AMI subjects in presence of aspirin, insulin or NO in 0.9% NaCl.
The solid squares ( ) represent the binding of dermcidin on platelets in control (normal) experiment. Hollow squares (
) represent the binding of dermcidin on platelets in control (normal) experiment. Hollow squares ( ) represent the binding of dermcidin in presence of 15 μM aspirin, solid triangles (
) represent the binding of dermcidin in presence of 15 μM aspirin, solid triangles ( ) represent the binding of dermcidin in presence of 30 μUnit/mL insulin and solid circles (
) represent the binding of dermcidin in presence of 30 μUnit/mL insulin and solid circles ( ) represent the binding of dermcidin in presence of 0.8 nM NO in 0.9% NaCl. In each case the binding of dermcidin to the platelets in presence of aspirin, insulin or NO was determined by ELISA as described in Method and Materials and the dissociation constant (Kd), the binding capacity (n = dermcidin binding sites/platelet) was determined. The Figure shown here is a typical representative of PRP from at least 6 different AMI subjects divided in 2 different groups with 3 AMI subjects in each group.
) represent the binding of dermcidin in presence of 0.8 nM NO in 0.9% NaCl. In each case the binding of dermcidin to the platelets in presence of aspirin, insulin or NO was determined by ELISA as described in Method and Materials and the dissociation constant (Kd), the binding capacity (n = dermcidin binding sites/platelet) was determined. The Figure shown here is a typical representative of PRP from at least 6 different AMI subjects divided in 2 different groups with 3 AMI subjects in each group.
Plasma concentration of insulin in AMI subjects
As the presence of 30 μUnits/mL insulin in the PRP from AMI subjects restored the sensitivity of those platelets to the inhibitory effect of aspirin. It was thought that the plasma insulin level in AMI could be insufficient to restore the inhibitory effect of aspirin in the absence of the added insulin to the PRP. When the plasma insulin level in the blood of AMI subjects was determined, it was found that the plasma insulin level was in the ranges from undetectable amount (near 0 to 5 μUnits/mL) by ELISA.
Discussion
Aspirin, through its ability to inhibit platelet aggregation by the inhibition of cyclooxygenase17 as well as by the stimulation of nitric oxide synthase24, is considered to be a corner stone in the therapeutic regimen both for the prevention and for the treatment of ACS that occurs due to the thrombus formation on the coronary artery. Although >90% of cases of AMI have been reported to be due to thrombosis10, aspirin is reported to fail to inhibit platelet aggregation in AMI and the use of aspirin in AMI is of little or no use13. And as such, it could be suggested that a third component in the circulation could be responsible for the resistance of platelets to the inhibitory effect of aspirin. We have reported before the appearance of a novel stress induced protein, identified to be dermcidin in the circulation in ACS14. Dermcidin was reported to be a potent inhibitor of all known forms of nitric oxide syntheses (NOS) and its systemic synthesis was determined to be due to the expression of dermcidin gene induced by environmental risk factors like tobacco extract or nicotine or alcohol or hypoxia18. As such, the appearance of dermcidin in the circulation of ACS was not a “metabolic expression” of the environmental stresses leading to the pathogenesis of the condition, but these environmental factors were actually capable of expressing the dermcidin gene in leucocytes, muscle, endothelial18 and in hepatic cells and in the whole animal19. The synthesis of dermcidin was reported to be suppressed by insulin or by aspirin through the cellular increase of NO level14. The inhibition of NO synthesis by dermcidin in platelets resulted in the increased binding of dermcidin on platelet surface “receptors” site (Figure 3) that could be removed by increasing NO levels in platelets (figure 5) possibly due to the mobilization of Ca2+ in platelets20. Dermcidin, a potent inhibitor of platelet NOS and a diabetogenic and hypertensive protein, was reported to be >40 folds more potent platelet aggregating agent than ADP through the inhibition of NO synthesis in platelet, that resulted in the increased thromboxane-A2 synthesis in platelets, leading to the aggregation of platelets14. In the context of dermcidin as a potent inhibitor of NOS, we have recently reported that the systemic NO level was found to be reduced to ≈0 pmol/ml plasma due to the inhibition of systemic NO by dermcidin that could have cause the anginal pain both in ACS and AMI21. It might be the suggested that the anginal pain in these conditions might be consequence of the systemic appearance of dermcidin in the circulation.
The inhibition of NOS by dermcidin in platelets was found to be related to the increased binding of dermcidin on the platelet surface leading to the failure of aspirin to inhibit platelet aggregation in AMI. The increase of platelet of NO level by aspirin, insulin or by NO itself resulted in the removal of the bound dermcidin from its high affinity binding sites on the platelet surface and as a result in the platelets from AMI subjects became more sensitive to inhibitory effect of aspirin by 8 folds (figure 6). As dermcidin is also present in the normal circulation14, it could be suggested that the presence of dermcidin in the normal plasma might have rendered the normal platelets partly resistant to the inhibitory effect of aspirin.
As described above when the PRP from the AMI subjects that was first incubated with 15 μM aspirin for 90 min (to remove the platelet bound dermcidin) followed by the treatment of the same PRP with 10 μM aspirin for 30 min resulted in the complete inhibition of platelet aggregation (figure 6). As such, it could be argued that if the total amounts of aspirin used in these experiments was 25 μM in the inhibition of platelet aggregation in the PRP from AMI, why then the use of 300 mg aspirin/70 kg body weight, the usual therapeutic dose of aspirin used in ACS failed to inhibit platelet aggregation in PRP from AMI subjects in the first place? However, as it has been described under Figure 5, the aspirin stimulated NO synthesis in AMI platelets had a biphasic effect in that the maximal synthesis of NO that was achieved at 15 μM of the compound and the use of higher doses of the compound actually resulted in the decreased production of NO and at 300 mg aspirin/70 kg body weight (equivalent to 333 μM aspirin) reduced the synthesis of NO by 70% with corresponding reduction removal of the platelet bound dermcidin by 40%.
In conclusion to our results suggested that was not due to the aspirin itself but due to the presence of dermcidin causing aspirin to fail to inhibit aggregation through the inhibition of NOS. The presence of dermcidin in AMI results to the pathological components in the pathophysiology of deadly AMI. This protein nullified the effect of aspirin induced inhibition of platelet aggregation through the synthesis of prostaglandin. Where NO produce from aspirin22, neutralizes the effect of dermcidin, as such the inhibition of aggregation of platelet by asprin has no effect in the inhibition of atherosclerosis, but inhibit the effect of dermcidin by the control of hypertension and hyperglycemia18.
The protein has a diagnostic significance because we have performed some preliminary experiments about the aggregation of AMI PRP in presence of aspirin. This data might indicate the AMI even in the absence of Troponin-I determination in plasma.
If these results from in-vitro study using PRP from the AMI subjects could be extended to the subjects affected by AMI, it might be suggested that the use of the 300 mg aspirin is not the optimal dose, in that it might actually not only create problem but also could be harmful, perhaps the chronic use of 14 mg bolus of aspirin/70 kg body weight and after 30 min another 9 mg bolus of aspirin/70 kg weight as described (figure 6) might be helpful in expulsion of platelet bound dermcidin to inhibit aggregation and may improve situation (fig. 6). In respect to dermcidin effect, our study relate in the basic science in the pathophysiology of AMI and the failure of aspirin to inhibit aggregation but not a peripheral clinical study.
Methods
Ethical Clearance
The research project, “Drmcidin isoform-2 induced nullification of the effect of acetyl salicylic acid in platelet aggregation in acute myocardial infarction” required nominal amount of blood (2 mL) from patients with AMI and ACS. The INSTITUTIONAL REVIEW BOARD, HUMAN & ANIMAL RESEARCH ETHICS COMMITTEE, SINHA INSTITUTE OF MEDICAL SCIENCE AND TECHNOLOGY, Kolkata, India approved the study on the condition that followed the approved Human Ethics Protocol strictly in accordance with 1964 Helsinki declaration and no deviation in the study was allowed without the prior written permission of the board.
AMI and ACS patient volunteers who participated in the study must be over ages of 43 to 62 years. No mentally retarded, pregnant women or prisoner took part in the study. All the volunteers signed an informed consent form prior to their participation in the study. It was ensured that the AMI and ACS patients had no other life-threatening infection. Care was taken to see that none of the volunteers were hospitalized for any condition within the last 6 months.
Patients with AMI and ACS were selected for the study only under the strict supervision of a cardiologist. Their complete blood picture was studied intensely and only those patients, who were willing to participate, were selected. Nominal amount of blood samples were drawn under the supervision of the attending physician and nurses. Seepage of blood after withdrawn, the blood was controlled by appropriate technique if any. Written consent was obtained from each of the patients. The committee inspected the progress and problems of the current investigation routinely.
The animal care and all experiments were performed in accordance with the guidelines approved by the Ethics Review Committee for Animal Experimentation at INSTITUTIONAL REVIEW BOARD, HUMAN & ANIMAL RESEARCH ETHICS COMMITTEE, SINHA INSTITUTE OF MEDICAL SCIENCE AND TECHNOLOGY, Kolkata, India. This study used healthy white New Zeland Rabbit after being examined by a certified veterinarian (according to animal protocol no 14 B of the institute). A standard diet and sterile water were given ad libitum. Care was taken to ensure that no animals were unnecessarily harmed or were subjected to pain during the study and the studies were performed only in the presence of a member belonging to the Animal Right Group.
Chemicals
Goat anti–rabbit immunoglobulin G-alkaline phosphatase, human IgG, l-epinephrine, collagen, thrombin and insulin were purchased from sigma Aldrich. Enzyme-linked immunosorbent assay (ELISA) Maxisorb plates were from Nunc, Roskilde, Denmark. Aspirin was obtained from Medica Zydus Healthcare. All other chemicals used were of analytical grade.
Selection of AMI patients
A total of 115 patients with chest pain lasting more than 120 min (n = 115; M = 92; F = 23) between the ages of 43 to 62 years, with characteristic chest pain of acute coronary syndrome (ACS) were admitted to the Intensive Coronary Care Unit of the Calcutta Medical College and Hospital, Calcutta. These subjects were further followed up for the occurrence of acute myocardial infarction as described below.
Exclusion Criteria
The patients with the history of diabetes mellitus or any life threatening infection were not included in the study. The subjects of ≥62 years old were also excluded. Also, as the pain due to pulmonary embolism, acute pericarditis, intestinal disorders, acute aortic dissection and other conditions that are known to simulate chest pain due to ACS, patients with these conditions and the patients with severe anemia, coronary spasms were also carefully excluded. None of those patients had received aspirin or were undergoing thrombolytic therapy or the subjects who had been hospitalized for any condition within the past 6 months were excluded from the study. None of the female subjects had ever received any contraceptive medications.
Diagnosis of AMI
Only those patients who were suspected to be affected with AMI were followed up by the electrocardiographic manifestation of both non-ST elevated myocardial infarction (nonSTEMI AMI, n = 68) and the patients with ST elevated myocardial infarction (STEMI AMI, n = 47) were included in these study. In those subjects where the either occurrence of non-STEMI or STEMI could not be ascertained definitely by electrocardiography were not included in the study.
The patients included in the study characteristically had developing Q wave AMI. All non Q wave MI patients were excluded.
The occurrence of AMI was confirmed by the determination of the plasma Troponin I within 24 h of the hospitalization.
Selection of normal volunteers
An equal numbers of normal volunteers (n = 115; M = 92; F = 23) of similar ages participated in the study. None of these volunteers had the history of diabetes mellitus, hypertension, cardiovascular or cerebrovascular condition. None had any life threatening infections. None of these volunteers had been hospitalized for any condition in the past 6 months. All selected volunteers were asked not to receive any medication including aspirin at least for 6 weeks before they were requested to donate blood samples. Blood samples were collected from AMI subjects before the initiation of any cardiovascular therapy for their condition.
Preparation of platelet-rich plasma
The platelet-rich plasma (PRP) from the blood samples from either AMI subjects or normal volunteers were prepared by centrifugation as described before22.
The platelet-free plasma (PFP) was prepared by centrifuging PRP at 10,000 g for 30 min as described before22.
Aggregation of platelets
Unless otherwise stated, the aggregation of platelets was studied by using optimal concentration of ADP (2.0 μM) in a platelet aggregometer as described before5.
Inhibition of platelet aggregation by acetyl salicylic acid (aspirin)
If not otherwise indicated, the inhibition of the ADP induced platelet aggregation was studied by incubating PRP with 80 μM aspirin for 30 minutes at 37°C before the aggregation of the platelets was initiated by adding 2.0 μM ADP to the PRP. As described in the results the use of aspirin as in the case of ADP induced platelet aggregation was found to fail to the inhibition of aggregation, use of other aggregating agents including either l-epinephrine, collagen, or thrombin for the aggregation of PRP of AMI subjects was also found to be resistant to the inhibitory effect of aspirin. For this reason the aggregation of platelet was routinely performed using only 2.0 μM ADP.
Preparation of aspirin solution
Aspirin (acetyl salicylic acid) was dissolved in deionised water. The pH was adjusted to 7.0 by adding 0.1 M NaHCO3 just before use and discarded after use.
Determination of nitric oxide
Nitric oxide (NO) was determined by methemoglobin method23 by determining the spectral changes of the absorption maxima at 575 and 630 nm in a Beckman Spectrophotometer Model DU as described before5. The concentration of NO was independently verified by using chemiluminescence method24.
Preparation of dermcidin
Dermcidin was prepared from the cell free plasma from the ACS patients by repeated electrophoresis on polyacrylamide gel first in the presence of sodium dodecyl sulphate (SDS), followed by the electrophoresis of the isolated protein in the absence of SDS25. The final preparation was dialyzed for 12 hours against 0.9% NaCl at 4°C as described in details before26.
Production of dermcidin antibody
The polyclonal antibody against dermcidin was raised in Newzeland rabbits by using eletrophoretically pure dermcidin as the antigen as described before27.
Enzyme linked immunosorbant assay (ELISA) for dermcidin and insulin
The details of the determination of dermcidin by ELISA have been described before28. The plasma insulin level was also determined by ELISA except that insulin antibody was the product of Santacruz Biotech.
Scatchard plot of the equilibrium binding of dermcidin to normal platelet suspension
Gel filtered platelets (GFP) suspension in Tyrod's buffer; pH 7.4 without Ca2+ was prepared by using sepharose 4 B column preequilibrated with the same buffer29. Typically, GFP (3 × 108 platelets/mL) in Tyrod's buffer was incubated with different concentrations of electrophoretically purified dermcidin for 90 min (optimal time required for the maximal binding of dermcidin to platelets determined in separate experiments). After incubation, 0.5 mL of incubation mixture was filtered over micro glass fibre membrane (GF/C, Sigma alrich) by using Millipore filtration unit as described before30. The use of GF/C membrane filtration allowed the platelets to remain adhered to the filter and the other constituents includig the incubation mixture including the free dermcidin passed through the filtrate under mild vacuum30,31. The membrane filter was washed with the 3 vol of the reaction buffer. After washing, the membrane filter was air dried and the bound dermcidin eluted from the filter by washing the filter with 1 vol of the buffer containing 0.05% TritonX-100. The filtrate was collected and dialysed against 0.9% NaCl for 12 hours at 4°C. The dialysed filtrate was used to determine the amount of dermcidin present in the filtrate by ELISA as described above.
Scatchard plot of the equilibrium binding characteristics to the platelets was constructed and the dissociation constant (Kd) and the dermcidin binding number (n) on the platelet surface was calculated as described below. Platelet number was determined by optical microscopy.
Statistical Analyses
The results shown are mean ± standard deviation (SD); the significance (p) of the results was determined by student's “t” test. The coefficient of correlation (“r”) was determined by Pearson test. The dissociation constant (Kd) and the number of the dermcidin binding sites (Bmax) in the Scatchard plot analyses were determined by (Graphpad Prism software) and Microsoft Office Excel.
References
Colman, R. W., Hirsh, J., Maeder, V. J. & Salzman, E. W. (eds) [594–605] Haemostasis and thrombosis. (J.B. Lippincott, Philadelphia, 1987).
Fuster, V., Badimon, J., Chesebro, J. H. & Fallon, J. T. Plaque rupture, Thrombosis and therapeutic implications. Haemostasis 26, 269–284 (1996).
Massberg, S., Schultz, C. & Gawaz, M. Role of platelets in the pathophysiology of acute coronary syndrome. Semin Vasc Med. 32, 147–162 Review (2003).
Whittle, B. J., Moncada, S. & Vane, J. R. Comparison of the effects of prostacyclin (PGI2), prostaglandin E1 and D2 on platelet aggregation in different species. Prostaglandins 16, 373–388 (1978).
Sinha, A. K., Bhattacharya, S., Acharya, K. & Mazumdar, S. Stimulation of nitric oxide synthesis and protective role of insulin in acute thrombosis in vivo. Life Sci. 65, 2687–2696 (1999).
Hoylaerts, M., Rijken, D. C., Lijnen, H. R. & Collen, D. Kinetics of the activation of plasminogen by human tissue plasminogenrin. J Biol Chem. 257, 2912–9 (1982).
Jana, P., Maiti, S., Ghosh, R., Ghosh, T. K. & Sinha, A. K. Estriol A stimulator of nitric oxide synthesis in platelets and its role as the powerful inhibitor of platelet aggregation. Cardiovascular Endocrinology 2, 50–54 (2013).
Pollack, C. V., Jr Emerging oral antiplatelet therapies for acute coronary syndromes. Hosp Pract. 38, 29–37 (1995).
Page, D. L., Caulfield, J. B., Kastor, J. A., DeSanctis, R. W. & Sanders, C. A. Myocardial changes associated with cardiogenic shock. N Engl J Med. 285, 133–7 (1971).
Carvalho de Sousa, J. et al. Factor VII hyperactivity in acute myocardial thrombosis. A relation to the coagulation activation. Thromb Res. 15, 51 165–73 (1988).
Maseri, A. et al. Coronary vasospasm as a possible cause of myocardial infarction. A conclusion derived from the study of “preinfarction” angina. N Engl J Med. 299, 1271–7 (1978).
Poulsen, T. S. et al. Prevalence of aspirin resistance in patients with an evolving acute myocardial infarction. Thromb Res. 119, 555–62 (2007).
Borna, C., Lazarowski, E., van Heusden, C., Ohlin, H. & Erlinge, D. Resistance to aspirin is increased by ST-elevation myocardial infarction and correlates with adenosine diphosphate levels. Thromb J. 26;3, 10 (2005).
Ghosh, R. et al. The appearance of dermcidin isoform 2, a novel platelet aggregating agent in the circulation in acute myocardial infarction that inhibits insulin synthesis and the restoration by acetyl salicylic acid of its effects. J Thromb Thrombolysis 31, 13–21 (2011).
Sinha, A. K., Rao, A. K., Willis, J. & Colman, R. W. Inhibition of thromboxane A2 synthesis in human platelets by coagulation factor Xa. Proc Natl Acad Sci. USA 80, 6086–90 (1983).
Kahn, N. N. et al. Nitric oxide: the “second messenger” of insulin. IUBMB Life. 49(5), 441–50 (2000).
Zhou, G., Marathe, G. K., Willard, B. & McIntyre, T. M. Intracellular erythrocyte platelet-activating factor acetylhydrolase I inactivates aspirin in blood. J Biol Chem. 286, 34820–9 (2011).
Ghosh, R., Bank, S., Bhattacharya, R., Khan, N. N. & Sinha, A. K. Neutralization by insulin of the hypertensive effect of dermcidin isoform 2: an environmentally induced diabetogenic and hypertensive protein. Cardiol Res Pract. (Epub) (2014).
Bank, S., Ghosh, R., Jana, P., Bhattacharya, S. & Sinha, A. K. The Diagnosis of High Altitude Illness by the Determination of Plasma Dermcidin Isoform 2 Levels by Enzyme Linked Immunosorbent Assay. Clin Lab. (Inpress) (2013).
Banerjee, D., Mazumder, S., Bhattacharya, S. & Sinha, A. K. The sex specific effects of extraneous testosterone on ADP induced platelet aggregation in platelet-rich plasma from male and female subjects. Int J Lab Haematol. (Epub) (2014).
Ghosh, R. et al. A Reduction of death rate due to acute myocardial infarction in subjects with cancers through systemic restoration of impaired nitric oxide. PloS One 9, e88639 (2014).
Chakraborty, K., Khan, G. A., Banerjee, P., Ray, U. & Sinha, A. K. Inhibition of human blood platelet aggregation and the stimulation of nitric oxide synthesis by aspirin. Platelets. 14, 421–7 (2003).
Karmohapatra, S. K., Chakraborty, K., Kahn, N. N. & Sinha, A. K. The role of nitric oxide in aspirin induced thrombolysis in vitro and the purification of aspirin activated nitric oxide synthase from human blood platelets. Am J Hematol. 82, 986–95 (2007).
Cox, R. D. & Frank, C. W. Determination of nitrate and nitrite in blood and urine by chemiluminescence. J Anal Toxicol. 6, 148–152 (1982).
Fazekas, de St., Groth, S., Webster, R. G. & Datyner, A. Two new staining procedures for quantitative estimation of proteins on electrophoretic strips. Biochim Biophys Acta. 71, 377–91 (1963).
Sarkar, M., Smith, A. E. & Pielak, G. J. Impact of reconstituted cytosol on protein stability. Proc Natl Acad Sci U S A. 110, 19342–7(2013).
Arquilla, E. R. & Stavitsky, A. B. The production and identification of antibodies to insulin and their use in assaying insulin. J Clin Invest. 35, 458–66 (1956).
Engvall, E. & Perlmann, P. Enzyme-linked immunosorbent assay, Elisa. 3. Quantitation of specific antibodies by enzyme-labeled anti-immunoglobulin in antigen-coated tubes. J Immunol. 109, 129–35 (1972).
Dutta-Roy, A. K. & Sinha, A. K. Purification and properties of prostaglandin E1/prostacyclin receptor of human blood platelets. J Biol Chem. 262, 12685–91 (1987).
Kahn, N. N. & Sinha, A. K. Stimulation of prostaglandin E1 binding to human blood platelet membrane by insulin and the activation of adenylate cyclase. J Biol Chem. 265, 4976–81 (1990).
Bhattacharjee, K. G., Bhattacharyya, M., Halder, U. C., Jana, P. & Sinha, A. K. The role of estrogen receptor status in neutrophils and maspin synthesis through nitric oxide production in human breast cancer. J Breast Cancer 15, 181–8 (2012).
Author information
Authors and Affiliations
Contributions
S.B. and A.K.S. designed the project and wrote the manuscript. S.B. and P.J. performed all experiments and prepared all the figures. S.B., S.M. and A.K.S. provided intellectual support and analysed data. S.G. and A.K.S. contributed reagents/samples. All authors reviewed manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Bank, S., Jana, P., Maiti, S. et al. Dermcidin isoform-2 induced nullification of the effect of acetyl salicylic acid in platelet aggregation in acute myocardial infarction. Sci Rep 4, 5804 (2014). https://doi.org/10.1038/srep05804
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep05804
This article is cited by
-
The role of Dermcidin isoform-2 in the occurrence and severity of Diabetes
Scientific Reports (2017)
-
Pentamethylquercetin (PMQ) reduces thrombus formation by inhibiting platelet function
Scientific Reports (2015)
-
The impaired synthesis of insulin and its inability to inhibit platelet aggregation in cerebrovascular accident
Metabolic Brain Disease (2015)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.