Abstract
Osteoarthritis (OA) is the most common age-related rheumatic disease. Chondrocytes play a primary role in mediating cartilage destruction and extracellular matrix (ECM) breakdown, which are main features of the OA joint. Quantitative proteomics technologies are demonstrating a very interesting power for studying the molecular effects of some drugs currently used to treat OA patients, such as chondroitin sulfate (CS) and glucosamine (GlcN). In this work, we employed the iTRAQ (isobaric tags for relative and absolute quantitation) technique to assess the effect of CS and GlcN, both alone and in combination, in modifying cartilage ECM metabolism by the analysis of OA chondrocytes secretome. 186 different proteins secreted by the treated OA chondrocytes were identified. 36 of them presented statistically significant differences (p ≤ 0.05) between untreated and treated samples: 32 were increased and 4 decreased. The synergistic chondroprotective effect of CS and GlcN, firstly reported by our group at the intracellular level, is now demonstrated also at the extracellular level.
Similar content being viewed by others
Introduction
Osteoarthritis (OA) is the most common form of arthritis, mainly characterized by cartilage destruction. Despite the increasing number of OA patients, no cure for this disease has been found to date. The therapies currently available primarily address the handling of joint pain. The failure of conventional treatments (analgesics or non-steroidal anti-inflammatory drugs) to regenerate or slow the degeneration of damaged cartilage, combined with their frequent adverse side effects, may explain the increasing use of SYSADOA (SYmptomatic Slow-Acting Drugs for Osteoarthritis) therapies such as chondroitin sulfate (CS) and glucosamine (GlcN). Although several clinical trials have examined the structure-modifying effects of these drugs1,2,3,4,5,6, the outcomes of the treatment with a combination of glucosamine and chondroitin sulfate (Glu/CS) on knee OA progression are still under debate. The recent Glucosamine/Chondroitin Arthritis Intervention Trial (GAIT study) suggests that the combination of glucosamine and chondroitin sulfate may be effective in the subgroup of patients with moderate-to-severe knee pain7. In a more recent analysis by Pelletier et al., using data from participants enrolled in the progression cohort of the OAI, there was evidence of a beneficial effect of the Glu/CS at delaying knee OA structural progression: Participants who took Glu/CS had reduced loss of cartilage volume over 24 months in subregions assessed with qMRI, thus supporting a disease-modifying effect of Glu/CS that could not be identified by X-rays8. However, recent meta-analysis fuel the controversy surrounding the efficacy of these drugs in terms of pain and structure modifications, stimulating further investigations about the mechanistic effects of CS and GlcN9.
The effect of combined formulations of chondroitin and glucosamine has been extensively reported in several in vitro studies10,11,12,13,14. Chan and collaborators demonstrated that, in bovine cartilage explants, the combination of CS with glucosamine hydrochloride was slightly better than glucosamine alone in inhibiting both inflammatory and catabolic intermediates. However, the effects of the combined formulation on chondrocytes extracellular matrix (ECM) metabolism remain poorly understood and their action on factors involved in cartilage remodelling has never been investigated by proteomic tools.
Proteomics is being increasingly applied for the study of drug modes of action, side-effects and toxicity and it is also a valuable approach for the discovery of new drug targets. In OA research, our group exhibits a good track record employing quantitative proteomics technologies for anti-OA drug screening. In 2010, we published the first pharmacoproteomic study aimed to unravel the molecular mechanisms driven by CS alone or in combination with GlcN sulfate15, which was performed by a gel-based proteomic analysis of human articular chondrocytes (HACs) stimulated with IL-1β. In that work, a large number of target proteins of CS and GlcN were described, pointing out the different mechanisms of action of these drugs. Nevertheless, in most cases both molecules synergistically modified the chondrocyte proteome, showing a potent effect on oxidative stress and modulation of energy production and metabolic pathways. Furthermore, using that approach we could only evaluate the intracellular mechanisms modulated by CS and GlcN, which are the background for ulterior putative changes of ECM turnover. Once the utility of proteomics for analyzing the intracellular targets of these two drugs was proved, we decided to focus on the analysis of the subset of chondrocyte extracellular proteins that are essential for cartilage ECM synthesis and turnover processes. With this objective, a quantitative profile of the chondrocyte extracellular protein changes driven by CS both in normal and OA chondrocytes was recently obtained by the SILAC technique16,17. These works provided novel molecular evidences of CS properties and underlined the need of stricter regulations regarding CS quality control. Furthermore, for the first time, chondrocyte secretome emerged as an attractive starting point for the discovery of new OA drug targets (i.e. angiogenesis) and also for the identification of novel efficacy markers for monitoring different OA treatments.
In the present work, we analyze the synergic effect of glucosamine and chondroitin sulfate, addressing for the first time the study of chondrocytes secretome using a gel-free approach and employing the isobaric tags for relative and absolute quantitation (iTRAQ) methodology, in order to overcome the limitations of the classical electrophoresis-based methods (DIGE and SILAC). By these means, we have performed a shotgun proteomics experiment on OA HACs secretomes that pursued to evaluate the combined effect of CS and GlcN on cartilage ECM biology and to better characterize their mechanism of action.
Results
Secretome profiling of CS- and/or GlcN-treated HACs
Supernatants from OA HACs, treated with CS alone or in combination with GlcN, were collected after 48 hours of incubation for the proteomic analysis. Samples were concentrated by filtration, cleaned up by acetone precipitation and quantified. An aliquot of these samples was resolved by SDS-PAGE. As revealed by silver staining (Supplementary Figure S1), HAC supernatants display a medium complexity. Nevertheless, we decided to carry out a two-dimensional approach in order to achieve the greatest number of identified proteins. A schematic workflow of this work is depicted in Fig. 1. Firstly, equal amounts of proteins from the experimental conditions to be compared (treated or untreated with CS and/or GlcN) were digested with trypsin and then the correspondent tryptic peptides were labeled with four different iTRAQ tags. The resulting labeled peptides were combined and separated using reversed phase LC prior to MS analysis for the identification and relative quantification of the corresponding proteins. Biological (n = 3) and technical (n = 2) replicates were analyzed to increase the reliability of the iTRAQ technique for relative quantitation18. A total of 186 proteins could be identified in chondrocytes secretome after combining the results from all the experiments (false discovery rate at 1%) with two or more peptides with 95% confidence and total score ≥ 2 and quantified (Supplementary Table S1). As expected, many of the identified proteins were ECM components of mature cartilage or matrix regulating factors including proteases, protease inhibitors, growth factors and anti-inflammatory agents. Furthermore, the iTRAQ labeling allowed us to identify 9 unique peptides of collagen II (COL2A1), a specific cartilage marker that was not previously detected using the MALDI-MS approach. This might be due to the improved MALDI ionization of the peptides that is triggered by the iTRAQ method and also to the independence of this technique from newly protein synthesis rate. In fact, previous studies on chondrocytes using SILAC labeling failed to identify COL2A116,19,20, which can be attributed to the very low rate of type II collagen turnover. A higher number of COL2A1 peptides has been detected only in studies on articular cartilage (from mouse and human origin) using a different type of ionization source (electrospray)21,22,23. Considering the global effect of the pharmacological treatment in altering chondrocytes secretome profile, we found thirty-six proteins significantly modulated (pvalue ≤ 0.05) in OA treated cells when compared to untreated ones (basal condition): 32 were increased and 4 were decreased (Table 1). Among them, CS alone altered the expression of twenty-eight HACs secreted proteins, while GlcN alone modulated only twelve of these proteins. Data analysis resulted more informative when we compared the effect of the combined formulation with each compound separately (Table 2). We found 18 proteins upregulated and only one, VIM, downregulated when we analyzed GlcN alone or in combination with CS (Table 2A). Among them we found thrombospondin-1 (THBS1 or TSP1), a protein recently described by our group as potential new target for OA treatment16. GlcN alone is unable to alter THBS1 expression level, but when combined with CS a strong increase is observed (ratio = 3,281; pvalue = 0,0001). On the other hand, when we focused on CS alone or in combination with GlcN, only 3 proteins were found as significantly modulated: VIM and FN1 increased and TGFBI decreased (Table 2B).
Bioinformatic analysis of differentially expressed proteins
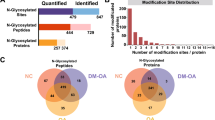
The STRING database was searched for protein interaction analyses in order to elucidate the effect of CS alone and in combination with GlcN. As shown in Figure 2, almost all (28) of the altered proteins interact with each other to constitute a big network. These proteins are involved in three main GO biological processes characteristic of connective tissue such as cell adhesion, cartilage development and ECM organization. Among them, proteins such as collagen VI, XII and tenascin showed increased release to the medium following all three treatments (Fig. 3A). The Pike tool was used to assign the cellular compartment of the identified proteins24. As shown in Fig. 3B, 60% of them are classically annotated as secreted proteins.
Protein-protein interaction network.
The STRING database was searched for protein interaction analyses in order to elucidate the effect of CS alone and in combination with GlcN. As shown in this Figure, almost all (28) of the altered proteins interact with each other to constitute a big network. These proteins are involved in three main GO biological processes: (A) cell adhesion, (B) cartilage development, (C) and ECM organization.
Data mining.
(A) Venn diagram depicting proteins modulated similarly and differently by CS-, GlcN- and CS + GlcN-treatment in OA HACs. Proteins in the green circle are modulated by CS, proteins in the violet circle are modulated by GlcN and proteins in the blue circle are modulated by the combined treatment. All proteins are upregulated except VIM, MSN, HSP90AB1 and PKM2. (B) Component pie charts indicating the cellular localization of those proteins identified in the HACs secretome, according to Gene Ontology annotation.
Verification of the modulation of THBS1 and TGFBI in NvsOA HACs
Taking into account previous proteomics results by our group16,20, we focused in particular on two proteins identified in this study: THBS1 and TGFBI. In our previous studies we could verify a significant modulation in the secretion of these proteins in IL1β-stimulated HACs. In the present work, Real Time-PCR assays demonstrated that THBS1 gene expression levels are decreased (ratio = 0,45; pvalue ≤ 0,05), while those of TGFBI are increased (ratio = 1,98; pvalue ≤ 0,05) in OA HACs compared to normal cells (Fig. 4). GlcN alone does not alter the expression of either THBS1 or TGFBI, whereas CS alone upregulates both genes (Table 1). Finally, CS + GlcN upregulates THBS1 compared to untreated cells (Table 1) and dowregulates TGFBI compared to CS-treated cells (Table 2B).
Verification of the modulation of TGFBI and THBS1 in NvsOA HACs by Real-Time PCR.
A significant increase (pvalue ≤ 0,05) in the gene expression of TGFBI (or BIGH3) and a decrease of THBS1 (or TSP1) were detected in OA (n = 7) HACs compared to normal (n = 6) cells. Results are expressed as the mean ± standard error.
Modulation of THBS1 by CS
In our previous studies we observed an increase of THBS1 or TSP1 (an angiogenesis inhibitor) driven by CS both in absence of IL1β stimulation, in OA chondrocytes17 and also in presence of this potent inflammatory cytokine in N cells16. In this case, as shown in Fig. 5, we detected a remarkable increase of thrombospondin 1 as a consequence of the cell treatment with CS alone (both at mRNA and protein level) and in combination with GlcN (only at protein level). Moreover, if we compared the effect of the combined formulation with that of GlcN alone, we observed a statistically significant increase in THBS1 protein expression level (Table 2A, Fig. 5B).
Thrombospondin-1 (THBS1 or TSP1) is increased by CS alone and in combination with GH.
Overexpression values of TSP1 were determined by real-time PCR (A) and Western blot analysis (B) of human articular chondrocytes from 3 OA donors. Results are expressed as mean ± SEM of 3 independent experiments. A representative image of Western blot is shown. *p < 0.05: chondroitin sulfate (CS)-treated group was significantly different from unstimulated group (CTL) both at mRNA and protein level, while the combination of CS + GH (glucosamine hydrochloride) was effective only at protein level. &p < 0.05: GH-treated group was significantly different from CS + GH group at protein level.
Discussion
We have performed a gel-free quantitative proteomics experiment for the analysis of secretomes (cell conditioned media) from CS and/or GlcN-treated OA HACs. This study has allowed us to generate a quantitative profile of chondrocyte extracellular protein changes driven by different CS formulations (simple and combined with GlcN). The strategy used is based on the differential labeling of peptides with iTRAQ reagents prior to their separation and analysis by multidimensional LC coupled to MS (Fig. 1). A previous analog study by our group described intracellular changes driven by CS and GlcN using a classical proteomic approach by 2DE15. 2DE is a powerful proteomic profiling technique for both protein identification and quantitation; however this traditional method showed some limitations in term of reproducibility. Furthermore, the 2DE platform fails to detect proteins with extreme pH values (greatly represented in cartilage by the high density and anionic nature of proteoglycans), high or low molecular weight, proteins present in low copy numbers and those with hydrophobic domains. In this sense, LC-MS/MS analysis overlaps these drawbacks, which are particularly important given the especial features of HACs, which synthesize and secrete a variety of highly anionic compounds (glycosaminoglycans) and a few abundant proteins (mainly collagens and proteoglycans) that hamper the performance of 2-DE-based approaches. Therefore, we recently developed an alternative method based on metabolic labeling (SILAC) for the quantitative analysis of chondrocytes proteome and secretome16,17,20 and also for the analysis of human bone marrow mesenchymal stem cells proteome during chondrogenic differentiation25. In this case, the main disadvantage is the limited number of conditions that can be compared simultaneously (usually two) and also the large culture time needed to obtain the fully labeled cell populations that are necessary for quantification. For all these reasons, LC-MS techniques have begun to exercise their dominance in the OA research field. Among these strategies, the use of iTRAQ protein tags significantly reduce sample-to-sample and time-point variation26, improves the ionization and subsequent analysis of peptides and finally allows the quantification of proteins in samples from different subjects, stages of disease or treatment conditions (up to 8) in a rapid and reproducible way.
The present study demonstrates the different effects of the simple and the combined administration of CS on OA HACs. CS alone increased the expression level of 24 proteins and decreased 4 (Tab. 1). Interestingly, the four decreased proteins are intracellular: two with a structural function (VIM, MSN), a glycolytic enzyme (PKM2) and a chaperone (HSP90B). Both vimentin and heat shock protein 90 beta are described in literature as OA-related proteins, as their protein expression levels are altered in OA chondrocytes27,28. Increased vimentin fragments were observed in a rat OA model29 and also in human OA cartilage30 and this correlates with a disrupted vimentin network. Here, we found that VIM is decreased by CS treatment (Table 1). Therefore, we hypothesize that CS could be effective in restoring a proper cytoskeleton network in OA-affected chondrocytes. On the other hand, a previous proteomic analysis performed by our group revealed an increase of the β subunit of the chaperone Hsp90 in diseased cells28. Many metabolic processes contributing to age-related changes in cartilage ECM are influenced by known roles of Hsp90β, such as COL2A1 and MMP-13 expression and NO synthesis31,32. Our result suggests that the well documented anabolic, anti-catabolic and anti-inflammatory properties of CS should be partially mediated by the Hsp90 inhibition observed in CS-treated chondrocytes10,11,12,33,34. However, further studies are needed to determine whether Hsp90β could serve as a therapeutic target of CS for reducing cartilage degradation in OA.
In OA HACs treated with GlcN alone, all of the modulated proteins were increased when compared to the untreated cells (Tab. 1). Generally, the increase observed is lower than the one observed with CS for the same proteins (except for ANXA5). Two proteins (CHI3L1 and PENK) were modulated only by GlcN alone or combined with CS and one was found to be positively modulated only by GlcN alone (LDHA). Interestingly, in our first pharamacoproteomic study15, all the proteins modulated by glucosamine sulfate (GS) related to energy production were decreased; while in the case of GlcN·HCl we found a slight increase (ratio = 1,888; pvalue = 0,0272) of this glycolytic enzyme. This difference could be determined by the different GlcN formulation employed, but probably also by the different cellular compartment analyzed.
Similar to the GAIT study7, many clinical trials tested CS together with glucosamine2,35,36. The results suggest that both components may enhance each other's efficacy. This synergistic effect was also proposed by various in vivo and in vitro studies10,11,12,13,37,38,39. As reviewed in recent works40,41,42, the mechanism of action of CS differs in several aspects from that of GlcN. In vivo and in vitro experiments have demonstrated that CS reaches the joint and distributes into the cartilage and subchondral layers43,44. However, being a large molecule, CS does not penetrate into the cells45 and so elicits its anti-inflammatory effect by engaging chondrocytes membrane receptors, e.g. CD44, TLR4 and ICAM1. In fact there is evidence that CS directly and/or indirectly modulates CD44 anti-inflammatory effects. CS engages CD44 and is internalized46,47. By binding to this receptor, CS could modulate transcriptional factors such as NF-κB thus blocking pro-inflammatory signaling pathways with down-regulation of target genes, such as ADAMTS, MMPs, IL-1β and iNOS48. Campo et al. had also demonstrated that CS could act on the toll-like receptor (TLR)-4 to inhibit the inflammatory cytokines, MyD88 and tumour necrosis factor (TNF) receptor associated factor (TRAF)-6, through the inhibition of nuclear factor (NF)-kB activation49. CS maintains the integrity of the cartilage ECM by two ways: reducing the expression of MMP1, MMP3, MMP13, ADAMTS1 and ADAMTS2, hence preventing the degradation of collagen, proteoglycans and aggrecan48; engaging integrins and increasing TGF-β1 expression that fosters the synthesis of hyaluronic acid and collagen II41. In addition, CS-containing proteoglycans play important roles in growth factor signaling in vivo, particularly during chondrogenesis50. Due to its highly negative charge, CS is able to interact electrostatically with positively charged growth factors such as TGFβ151. This ability to sequester growth factors should be exploited as drug delivery vehicles for controlled delivery and release, especially for repair of cartilaginous tissues52. On the other hand, GlcN penetrates into cells by means of glucose transporters (GLUTs). Once taken up by cells, exogenous GlcN is phosphorylated into GlcN-6-phosphate, which subsequently enters into the hexosamine biosynthetic pathway to generate UDP-N-acetylglucosamine (UDP-GlcNAc). UDP-GlcNAc is a substrate for the synthesis of proteoglycans, glycolipids and glycoproteins but also for protein acylation through O-linked GlcNAcylation (O-GlcNAc)53. Proteins can be modified reversibly at serine or threonine residues by attachment of a GlcNAc molecule. As suggested by Scotto D'Abusco et al. the effects of GlcN could derive, at least in part, from its capacity to O-GlcNAcylate proteins, primarily kinases (JNK, p38 and IKKα)54,55. In the case of chondrocytes treated with GlcN, this protein modification competes with phosphorylation by utilizing the same amino acidic sites and, as a consequence, GlcN reduces NF-κB nuclear translocation and abrogates the transcription of proteolytic and pro-inflammatory target genes. In our first pharmacoproteomic study we evaluated the potency of the use of CS in combination with GlcN15. These compounds produced different patterns of protein modification when tested alone or in combination. However, in most cases a synergistic effect was demonstrated when cells were exposed to both compounds, implying a potent effect on oxidative stress as indicated by the modulation of superoxide dismutase. Finally we can conclude that the differences in their mechanism of action could explain why the combination of CS and GlcN should be more effective than each individual drug supporting the use of the combined formulation. In the present study we focused on the subset of secreted proteins in order to identify putative novel biomarkers that would be easily detectable in the bloodstream of treated patients and therefore useful to discriminate responders and non-responders. The Venn diagram showed in Fig. 3A depicts the overlap of proteins modulated in OA chondrocytes by each treatment and is quite similar to that previously obtained in normal HACs stimulated with IL1β. In the case of CS, we observed a 62% of similarity with the combined treatment, while in the case of GlcN only a 33% was detected. A slight synergistic effect was noticed for some ECM components (ACAN, CHI3L1, COL5A1 and COL12A1). In other cases, a statistically significant modulation was seen only when CS and GlcN were employed together (COMP, FN1 and LUM).
As concluding remarks, our findings confirm in OA HACs the synergistic chondroprotective effect of chondroitin sulfate and glucosamine hydrochloride that was previously described by our group in normal cells. In fact, despite having employed in such studies different proteomic strategies based on 2DE, DIGE and SILAC, the modulation of several proteins (like VIM, PKM2, THBS1) in CS-treated chondrocytes has been observed also in this study (Table 3). Moreover, the iTRAQ approach exhibits the advantages for the relative quantification of HACs secreted proteins. This is especially useful to focus on cartilage ECM proteins, which have particular importance for their role in proper tissue maintenance. To our knowledge, this is the first time that COL2A1 is identified by MALDI-MS in chondrocytes secretome. If the presence of this protein into the conditioned medium represents new matrix synthesis, matrix degradation, or passive loss of components from the chondrocytes needs to be investigated. Furthermore, the subset of OA chondrocyte extracellular proteins has been successfully evaluated for the search of non-invasive OA biomarkers. In fact, the main goal of this study, in addition to focus on the evaluation of the combined formulation, is also to serve as novel source for OA biomarker discovery. Several proteins have emerged as putative candidate biomarkers and, hopefully, the negative correlation between THBS1 and TGFBI expression that we have encountered can be exploited in the next future for screening the presence of OA disease or monitoring therapeutic effectiveness in clinical samples. Especially THBS1, which is downregulated in OA chondrocytes and then upregulated after pharmacological treatment, could be a good standard for the outcome measures of clinical trials assisting data interpretation and enabling rigorous comparisons between different studies. However, further investigations on biological fluids are necessary to assess its biomarker usefulness.
Methods
Cartilage procurement and processing
Cartilage obtained from three OA patients (73, 78 and 84 years old) undergoing joint replacement was provided by the Tissue Bank and the Autopsy Service at CHU A Coruña for the pharmacoproteomic analysis. The study was approved by the local Ethics Committee. Articular chondrocytes were isolated from human cartilages as previously described15,56. Briefly, once cartilage surfaces were rinsed with saline, scalpels were used to cut parallel sections 5 mm apart, vertically from the cartilage surface onto the subchondral bone. These cartilage strips were then cut-off from the bone and the tissue was incubated with trypsin at 37°C for 10 min. After removing trypsin solution, the cartilage slices were treated for 12–16 h with type IV clostridial collagenase in DMEM with 10% FBS in order to release cartilage cells.
Chondrocytes culture and pharmacological treatment
Chondrocytes were recovered and cultured in DMEM supplemented with 100 U/mL penicillin, 100 mg/mL streptomycin, 1% glutamine and 10% FBS. Cells were seeded onto 100 mm culture plates for proteomic studies or 6-well plates for total RNA extraction. The cells were incubated at 37°C in a humidified gas mixture containing 5% CO2 balanced with air. Chondrocytes were used at weeks 2–3 in primary culture, after making them quiescent by incubation in a medium containing 0.5% FBS for 24 h. Finally, cells were cultured for 48 hours in serum free medium containing chondroitin sulfate (CS) and/or glucosamine hydrochloride (GlcN or GH). Both molecules were pharmacological grade and were provided by Bioiberica S.A. (Barcelona, Spain). CS was from bovine origin, with a CS content of 99.9% and a molecular weight of 15.12 kDa. Other characteristics (viscosity, sulfation sites, etc.) have been previously detailed elsewhere17,57. CS and GlcN concentrations (both 200 μg/mL) were optimized for the proteomic studies in accordance with previous results by our group and literature data15,20 where a very wide range of both glucosamine and chondroitin sulfate have been used on different cell types and tissues. These concentrations are also in accordance with those tested in the standardization step of our proteomic analysis (CS from 20 to 200 μg/ml and GlcN from 1 to 10 mM).
Processing of conditioned media for iTRAQ labeling
Conditioned media (CM) obtained from 3 different samples were analyzed independently. CM were collected, centrifuged and filtered using a 0.2 μm filter to ensure removal of any dead cells. Supernatant of each dish (6 mL) was concentrated to a final volume of 250 μl with Amicon ultrafiltration units (5 kDa MWCO, Millipore, Billerica, MA, USA) and then cleaned up by acetone precipitation. Protein pellets were dried in air and then resuspended in 25 μl Dissolution Buffer. Protein concentrations were determined by Bradford assay (Sigma-Aldrich, St. Louis, MO, USA). Equal amounts of chondrocyte secreted proteins (20 μg) from each condition were reduced, alkylated and digested with trypsin. Then iTRAQ labeling was performed according to the supplier's instructions (ABSciex, Foster City, CA, USA). The samples were labeled as follows: controls, 114; CS, 115; GH, 116; CS + GH, 117. iTRAQ-labeled peptides were mixed and desalted using reversed phase columns (Pierce C18 Spin Columns, Thermo Fisher Scientific, Rockford, IL, USA) prior to liquid chromatography coupled to mass spectrometry (LC-MS) analysis (Fig. 1).
LC-MS analysis
The peptide mixture was firstly separated by off-line reversed-phase liquid chromatography (RP-LC) at basic pH (pH = 10) to lower its complexity. The separation was performed on a HP 1200 system (Agilent Technologies, Santa Clara, CA, USA) employing a C18 reversed-phase column (Zorbax extend C18, 100 × 2.1 mm id, 3.5 μm, 300 Å; Agilent). The flow rate used was 0.2 mL/minute and the gradient was as in Suppl. Fig. S2. The chromatogram was produced using a UV Detector at 214 nm. Several fractions were pooled post-collection (FC203B fraction collector, Gilson, Middleton, WI, USA) based on the peak intensity of the UV trace, yielding a total of 26 samples per LC run. Each fraction was dried in a vacuum concentrator and stored at −20°C for the next step of analysis. The dried peptide fractions were dissolved in 0.1% trifluoroacetic acid (TFA) and 2% acetonitrile; 5 μL of this sample were injected onto a capillary trap column (0.5 × 2 mm, Michrom Bioresources, Auburn, CA, USA) at a flow rate of 15 μl/minute. Peptides were desalted for 10 minutes and loaded onto a C18 column (Integrafit C18, Proteopep™ II, 75 μm id, 10.2 cm, 5 μm, 300 Å; New Objective, Woburn, MA, USA) at a constant flow rate of 350 nl/minute to perform the separation. Then peptides were separated using linearly increasing concentration of acetonitrile in buffer B. The RP analytical column eluent was spotted onto a matrix-assisted laser desorption/ionization (MALDI) sample plate using the Sun Collect MALDI Spotter/Micro Collector (SunChrom Wissenschaftliche Geräte GmbH, Germany) and analyzed by a 4800 mass spectrometer (AB Sciex). After the screening of all LC-MALDI sample positions in MS positive reflector mode, the fragmentation of automatically selected precursors was performed to generate fragment ions that provided sequence information for the peptide and reporter ions. MS and MS/MS parameters have been detailed elsewhere20,26.
Data analysis
Protein identification and quantification were carried out using ProteinPilot™ software v.4.0 (ABSciex). Each MS/MS spectrum was searched in the Uniprot/Swissprot database (downloaded in May 2012) for Homo sapiens. Search parameters within ProteinPilot were set with trypsin cleavage specificity; methyl methanethiosulfate (MMTS) modified cysteine as fixed modifications; biological modification “ID focus” settings and a protein minimum confidence score of 95%. Thus, the identity of the protein from the analyzed peptide was confirmed and the ratios of the peak areas of iTRAQ reporter ions were used to compare the relative abundance of the protein identified in the sample. Only proteins identified with at least 95% confidence, or a Prot Score (protein confidence measure) of at least 1.3 were reported (Supplementary Table S1). Data were normalized for loading error by bias and the background correction was calculated using the Pro Group™ algorithm (ABSciex). To determine the cutoff value for significant fold changes, coefficient of variation and cumulative frequency were calculated for the common proteins employing the R statistical package58. Using this tool, we considered statistically significant only those changes with a p value ≤ 0.05 and a ratio ≥ 1.4 (or ≤0.7). The results obtained from ProteinPilot were exported to Microsoft Excel for further analyses.
Real-time PCR assays
Total RNA was isolated from OA and N HACs (5 × 105 per well) using Trizol Reagent (Invitrogen), following the manufacturer's instructions. cDNA was synthesized from 1 μg total RNA, using the Transcriptor First Strand cDNA Synthesis Kit (Roche Diagnostics, Basel, Switzerland) in accordance with the manufacturer's instructions and analyzed by quantitative real-time PCR. Quantitative real-time PCR assay was performed in the LightCycler 480 instrument (Roche) using 96-well plates. Primers for THBS1, TGFBI and the housekeeping genes, HPRT1 and RPLP0, were designed using the Universal Probe Library tool from the Roche website (http://www.roche-applied-science.com). Primer sequences were as follows: THBS1 forward, 5′-GCTGCACTGAGTGTCACTGTC-3′; THBS1 reverse, 5′-TCAGGAACTGTGGCATTGG-3′; TGFBI forward, 5′- CGAGTGCTGTCCTGGATATG-3′; TGFBI reverse, 5′- CCCAGGGTCTCGTAAAGGTT-3′; HPRT1 forward, 5′-TGACCTTGATTTATTTTGCATACC-3′; HPRT1 reverse, 5′-CGAGCAAGACGTTCAGTCCT-3′; RPLP0 forward, 5′-TCTACAACCCTGAAGTGCTTGAT-3′, PRPL0 reverse 5′-CAATCTGCAGACAGACACTGG-3′. The results were analyzed using the LightCycler 480 software release 1.5.0 (Roche).
Western blot analysis
Western blot analyses were performed utilizing standard procedures. Chondrocytes from 3 OA donors different from those selected for the proteomics strategy were used. Briefly, 20 μg of secreted proteins were loaded and resolved using 8% SDS-polyacrylamide gel electrophoresis (SDS-PAGE). The separated proteins were then transferred to polyvinylidene fluoride (PVDF) membranes (Immobilon P, Millipore Co., Bedford, MA, USA) by electro-blotting and probed with specific antibodies against THBS1 or TSP1 (Santa Cruz). Immunoreactive bands were detected by chemiluminescence using corresponding horseradish peroxidase (HRP)-conjugated secondary antibodies and enhanced chemiluminescence (ECL) detection reagents (GE Healthcare), then digitized using the LAS 3000 image analyzer. Equivalent loadings were verified by Ponceau Red (Sigma) staining after transference (data not shown). Quantitative changes in band intensities were evaluated using ImageQuant 5.2 software (GE Healthcare).
Statistical analysis
The statistical significance of the differences between mean values was determined using the two-tailed t-test, accepting p ≤ 0.05 to be significant. In the proteomic analysis, normalization tools and statistical package from ProteinPilot software were employed. Searches against a concatenated database containing both forward and reversed sequences allowed the false discovery rate (FDR) to be kept at 1%. Proteomics System Performance Evaluation Pipeline (PSPEP) software was used independently to calculate false discovery rates. Where appropriate, results are expressed as the mean ± standard error.
References
Kahan, A., Uebelhart, D., De Vathaire, F., Delmas, P. D. & Reginster, J. Y. Long-term effects of chondroitins 4 and 6 sulfate on knee osteoarthritis: the study on osteoarthritis progression prevention, a two-year, randomized, double-blind, placebo-controlled trial. Arthritis Rheum 60, 524–533 (2009).
Bruyere, O. & Reginster, J. Y. Glucosamine and chondroitin sulfate as therapeutic agents for knee and hip osteoarthritis. Drugs Aging 24, 573–580 (2007).
Pavelka, K. et al. Glucosamine sulfate use and delay of progression of knee osteoarthritis: a 3-year, randomized, placebo-controlled, double-blind study. Arch Intern Med 162, 2113–2123 (2002).
Reginster, J. Y. et al. Long-term effects of glucosamine sulphate on osteoarthritis progression: a randomised, placebo-controlled clinical trial. Lancet 357, 251–256 (2001).
Rovati, L. C., Girolami, F. & Persiani, S. Crystalline glucosamine sulfate in the management of knee osteoarthritis: efficacy, safety and pharmacokinetic properties. Ther Adv Musculoskelet Dis 4, 167–180 (2012).
Michel, B. A. et al. Chondroitins 4 and 6 sulfate in osteoarthritis of the knee: a randomized, controlled trial. Arthritis Rheum 52, 779–786 (2005).
Clegg, D. O. et al. Glucosamine, chondroitin sulfate and the two in combination for painful knee osteoarthritis. N Engl J Med 354, 795–808 (2006).
Martel-Pelletier, J. et al. First-line analysis of the effects of treatment on progression of structural changes in knee osteoarthritis over 24 months: data from the osteoarthritis initiative progression cohort. Ann Rheum Dis 2013-203906, 10.1136/annrheumdis-2013-203906 (2013).
Zhang, W. et al. OARSI recommendations for the management of hip and knee osteoarthritis: part III: Changes in evidence following systematic cumulative update of research published through January 2009. Osteoarthritis Cartilage 18, 476–499 (2010).
Chan, P. S., Caron, J. P. & Orth, M. W. Effect of glucosamine and chondroitin sulfate on regulation of gene expression of proteolytic enzymes and their inhibitors in interleukin-1-challenged bovine articular cartilage explants. Am J Vet Res 66, 1870–1876 (2005).
Chan, P. S., Caron, J. P., Rosa, G. J. & Orth, M. W. Glucosamine and chondroitin sulfate regulate gene expression and synthesis of nitric oxide and prostaglandin E(2) in articular cartilage explants. Osteoarthritis Cartilage 13, 387–394 (2005).
Chan, P. S., Caron, J. P. & Orth, M. W. Short-term gene expression changes in cartilage explants stimulated with interleukin beta plus glucosamine and chondroitin sulfate. J Rheumatol 33, 1329–1340 (2006).
Chan, P. S., Caron, J. P. & Orth, M. W. Effects of glucosamine and chondroitin sulfate on bovine cartilage explants under long-term culture conditions. Am J Vet Res 68, 709–715 (2007).
Tat, S. K. et al. Chondroitin and glucosamine sulfate in combination decrease the pro-resorptive properties of human osteoarthritis subchondral bone osteoblasts: a basic science study. Arthritis Res Ther 9, R117 (2007).
Calamia, V. et al. Pharmacoproteomic study of the effects of chondroitin and glucosamine sulfate on human articular chondrocytes. Arthritis Res Ther 12, R138 (2010).
Calamia, V. et al. Secretome analysis of chondroitin sulfate-treated chondrocytes reveals anti-angiogenic, anti-inflammatory and anti-catabolic properties. Arthritis Res Ther 14, R202 (2012).
Calamia, V. et al. Pharmacoproteomic study of three different chondroitin sulfate compounds on intracellular and extracellular human chondrocyte proteomes. Mol Cell Proteomics 11, M111.013417 (2012).
Gan, C. S., Chong, P. K., Pham, T. K. & Wright, P. C. Technical, experimental and biological variations in isobaric tags for relative and absolute quantitation (iTRAQ). J Proteome Res 6, 821–827 (2007).
Polacek, M., Bruun, J. A., Elvenes, J., Figenschau, Y. & Martinez, I. The secretory profiles of cultured human articular chondrocytes and mesenchymal stem cells: implications for autologous cell transplantation strategies. Cell Transplant 20, 1381–1393 (2011).
Calamia, V. et al. Metabolic labeling of chondrocytes for the quantitative analysis of the interleukin-1-beta-mediated modulation of their intracellular and extracellular proteomes. J Proteome Res 10, 3701–3711 (2011).
Wilson, R. et al. Comprehensive profiling of cartilage extracellular matrix formation and maturation using sequential extraction and label-free quantitative proteomics. Mol Cell Proteomics 9, 1296–1313 (2010).
Önnerfjord, P., Khabut, A., Reinholt, F. P., Svensson, O. & Heinegård, D. Quantitative proteomic analysis of eight cartilaginous tissues reveals characteristic differences as well as similarities between subgroups. J Biol Chem 287, 18913–18924 (2012).
Wilson, R. et al. Changes in the chondrocyte and extracellular matrix proteome during post-natal mouse cartilage development. Mol Cell Proteomics 11, M111.014159 (2012).
Medina-Aunon, J. A. et al. Protein Information and Knowledge Extractor: Discovering biological information from proteomics data. Proteomics 10, 3262–3271 (2010).
Rocha, B. et al. Metabolic labeling of human bone marrow mesenchymal stem cells for the quantitative analysis of their chondrogenic differentiation. J Proteome Res 11, 5350–5361 (2012).
Fernández-Puente, P. et al. Identification of a panel of novel serum osteoarthritis biomarkers. J Proteome Res 10, 5095–5101 (2011).
Ruiz-Romero, C. et al. Mitochondrial dysregulation of osteoarthritic human articular chondrocytes analyzed by proteomics: a decrease in mitochondrial superoxide dismutase points to a redox imbalance. Mol Cell Proteomics 8, 172–189 (2009).
Ruiz-Romero, C. et al. Proteomic analysis of human osteoarthritic chondrocytes reveals protein changes in stress and glycolysis. Proteomics 8, 495–507 (2008).
Capín-Gutiérrez, N., Talamás-Rohana, P., González-Robles, A., Lavalle-Montalvo, C. & Kourí, J. B. Cytoskeleton disruption in chondrocytes from a rat osteoarthrosic (OA) -induced model: its potential role in OA pathogenesis. Histol Histopathol 19, 1125–1132 (2004).
Lambrecht, S., Verbruggen, G., Verdonk, P. C., Elewaut, D. & Deforce, D. Differential proteome analysis of normal and osteoarthritic chondrocytes reveals distortion of vimentin network in osteoarthritis. Osteoarthritis Cartilage 16, 163–173 (2008).
Calamia, V., de Andrés, M. C., Oreiro, N., Ruiz-Romero, C. & Blanco, F. J. Hsp90β inhibition modulates nitric oxide production and nitric oxide-induced apoptosis in human chondrocytes. BMC Musculoskelet Disord 12, 237 (2011).
Boehm, A. K., Seth, M., Mayr, K. G. & Fortier, L. A. Hsp90 mediates insulin-like growth factor 1 and interleukin-1beta signaling in an age-dependent manner in equine articular chondrocytes. Arthritis Rheum 56, 2335–2343 (2007).
Bassleer, C. T., Combal, J. P., Bougaret, S. & Malaise, M. Effects of chondroitin sulfate and interleukin-1 beta on human articular chondrocytes cultivated in clusters. Osteoarthritis Cartilage 6, 196–204 (1998).
Imada, K. et al. Anti-arthritic action mechanisms of natural chondroitin sulfate in human articular chondrocytes and synovial fibroblasts. Biol Pharm Bull 33, 410–414 (2010).
Sawitzke, A. D. et al. Clinical efficacy and safety of glucosamine, chondroitin sulphate, their combination, celecoxib or placebo taken to treat osteoarthritis of the knee: 2-year results from GAIT. Ann Rheum Dis 69, 1459–1464 (2010).
Huskisson, E. C. Glucosamine and chondroitin for osteoarthritis. J Int Med Res 36, 1161–1179 (2008).
Lippiello, L., Woodward, J., Karpman, R. & Hammad, T. A. In vivo chondroprotection and metabolic synergy of glucosamine and chondroitin sulfate. Clin Orthop Relat Res, 229–240 (2000).
Lippiello, L. Glucosamine and chondroitin sulfate: biological response modifiers of chondrocytes under simulated conditions of joint stress. Osteoarthritis Cartilage 11, 335–342 (2003).
Orth, M. W., Peters, T. L. & Hawkins, J. N. Inhibition of articular cartilage degradation by glucosamine-HCl and chondroitin sulphate. Equine Vet J Suppl 224–229 (2002).
Henrotin, Y. & Lambert, C. Chondroitin and glucosamine in the management of osteoarthritis: an update. Curr Rheumatol Rep 15, 361 (2013).
du Souich, P. Absorption, distribution and mechanism of action of SYSADOAS. Pharmacol Ther (2014).
Henrotin, Y., Mathy, M., Sanchez, C. & Lambert, C. Chondroitin sulfate in the treatment of osteoarthritis: from in vitro studies to clinical recommendations. Ther Adv Musculoskelet Dis 2, 335–348 (2010).
Ronca, F., Palmieri, L., Panicucci, P. & Ronca, G. Anti-inflammatory activity of chondroitin sulfate. Osteoarthritis Cartilage 6 Suppl A, 14–21 (1998).
Sobal, G., Dorotka, R., Menzel, J. & Sinzinger, H. Uptake studies with chondrotropic 99mTc-chondroitin sulfate in articular cartilage. Implications for imaging osteoarthritis in the knee. Nucl Med Biol 40, 1013–1017 (2013).
Sobal, G., Menzel, J. & Sinzinger, H. Uptake of 99mTc-labeled chondroitin sulfate by chondrocytes and cartilage: a promising agent for imaging of cartilage degeneration. Nucl Med Biol 36, 65–71 (2009).
Lo, Y. L., Sung, K. H., Chiu, C. C. & Wang, L. F. Chemically conjugating polyethylenimine with chondroitin sulfate to promote CD44-mediated endocytosis for gene delivery. Mol Pharm 10, 664–676 (2013).
Fujimoto, T. et al. CD44 binds a chondroitin sulfate proteoglycan, aggrecan. Int Immunol 13, 359–366 (2001).
Legendre, F., Baugé, C., Roche, R., Saurel, A. S. & Pujol, J. P. Chondroitin sulfate modulation of matrix and inflammatory gene expression in IL-1beta-stimulated chondrocytes--study in hypoxic alginate bead cultures. Osteoarthritis Cartilage 16, 105–114 (2008).
Campo, G. M. et al. Glycosaminoglycans reduced inflammatory response by modulating toll-like receptor-4 in LPS-stimulated chondrocytes. Arch Biochem Biophys 491, 7–15 (2009).
DeLise, A. M., Fischer, L. & Tuan, R. S. Cellular interactions and signaling in cartilage development. Osteoarthritis Cartilage 8, 309–334 (2000).
Hintze, V. et al. Sulfated hyaluronan and chondroitin sulfate derivatives interact differently with human transforming growth factor-β1 (TGF-β1). Acta Biomater 8, 2144–2152 (2012).
Lim, J. J. & Temenoff, J. S. The effect of desulfation of chondroitin sulfate on interactions with positively charged growth factors and upregulation of cartilaginous markers in encapsulated MSCs. Biomaterials 34, 5007–5018 (2013).
Anderson, J. W., Nicolosi, R. J. & Borzelleca, J. F. Glucosamine effects in humans: a review of effects on glucose metabolism, side effects, safety considerations and efficacy. Food Chem Toxicol 43, 187–201 (2005).
d'Abusco, A. S. et al. Glucosamine affects intracellular signalling through inhibition of mitogen-activated protein kinase phosphorylation in human chondrocytes. Arthritis Res Ther 9, R104 (2007).
Scotto d'Abusco, A., Politi, L., Giordano, C. & Scandurra, R. A peptidyl-glucosamine derivative affects IKKalpha kinase activity in human chondrocytes. Arthritis Res Ther 12, R18 (2010).
Ruiz-Romero, C., López-Armada, M. J. & Blanco, F. J. Proteomic characterization of human normal articular chondrocytes: a novel tool for the study of osteoarthritis and other rheumatic diseases. Proteomics 5, 3048–3059 (2005).
Tat, S. K., Pelletier, J. P., Mineau, F., Duval, N. & Martel-Pelletier, J. Variable effects of 3 different chondroitin sulfate compounds on human osteoarthritic cartilage/chondrocytes: relevance of purity and production process. J Rheumatol 37, 656–664 (2010).
Jin, J. et al. Differential proteome profiling using iTRAQ in microalbuminuric and normoalbuminuric type 2 diabetic patients. Exp Diabetes Res 2012, 168602 (2012).
Acknowledgements
This work was supported in part through funding from the Fondo Investigación Sanitaria, Madrid, Spain (CIBER-CB06/01/0040; PI11/02397; PI12/00329; RETIC-RIER-RD12/0009/0018; and Proteo-Red/ISCIII); Ministerio Ciencia e Innovación PLE2009-0144, FEDER (European Community) and Xunta de Galicia: grant 10 PXIB 310153 PR and Red Gallega REDICENT. J. Mateos (CA11/00050) and P. Fernández-Puente (CA09/00458) are supported by Fondo Investigación Sanitaria-Spain. C. Ruiz-Romero is supported by the Miguel Servet program from Fondo Investigación Sanitaria-Spain (CP09/00114).
Author information
Authors and Affiliations
Contributions
V.C. performed the in vitro experiments, analyzed the data and wrote the manuscript. L.L., B.R. and C.F.C. helped to collect and process samples and participated in statistical data analysis. J.M. and P.F.P. carried out the LC-MS analysis. E.M. and J.V. provided CS and helped with the study design. C.R.R. participated in the study design, interpretation of the data and manuscript preparation. F.J.B. conceived and coordinated the project and revised the manuscript. All authors read and approved the final manuscript.
Ethics declarations
Competing interests
Eulàlia Montell is the Head of the Medical Area from Bioibérica, SA. Josep Vergés is Medical Director of Bioibérica, SA. Francisco J. Blanco received a grant from Bioibérica, SA to carry out this project. The authors declare no other competing interests.
Electronic supplementary material
Supplementary Information
Supplementary Information
Supplementary Information
Supplementary Table S2
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. The images in this article are included in the article's Creative Commons license, unless indicated otherwise in the image credit; if the image is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the image. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Calamia, V., Mateos, J., Fernández-Puente, P. et al. A pharmacoproteomic study confirms the synergistic effect of chondroitin sulfate and glucosamine. Sci Rep 4, 5069 (2014). https://doi.org/10.1038/srep05069
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep05069
This article is cited by
-
Hif-1α Knockdown Reduces Glycolytic Metabolism and Induces Cell Death of Human Synovial Fibroblasts Under Normoxic Conditions
Scientific Reports (2017)
-
Efficacy of glucosamine plus diacerein versus monotherapy of glucosamine: a double-blind, parallel randomized clinical trial
Arthritis Research & Therapy (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.