Abstract
Gout is a common disease which mostly occurs after middle age, but more people nowadays develop it before the age of thirty. We investigated whether common dysfunction of ABCG2, a high-capacity urate transporter which regulates serum uric acid levels, causes early-onset gout. 705 Japanese male gout cases with onset age data and 1,887 male controls were genotyped and the ABCG2 functions which are estimated by its genotype combination were determined. The onset age was 6.5 years earlier with severe ABCG2 dysfunction than with normal ABCG2 function (P = 6.14 × 10−3). Patients with mild to severe ABCG2 dysfunction accounted for 88.2% of early-onset cases (twenties or younger). Severe ABCG2 dysfunction particularly increased the risk of early-onset gout (odds ratio 22.2, P = 4.66 × 10−6). Our finding that common dysfunction of ABCG2 is a major cause of early-onset gout will serve to improve earlier prevention and therapy for high-risk individuals.
Similar content being viewed by others
Introduction
Gout is a common disease which causes acute arthritis as a consequence of hyperuricemia1. Gout and hyperuricemia are reportedly associated with other common diseases1, such as hypertension2,3, coronary artery diseases4, cerebrovascular diseases5 and kidney diseases6. Although gout mostly occurs after middle age7, the number of patients experiencing its onset at a younger age is now increasing8,9. While gout with an earlier onset has a heritable component10, its common genetic causes are still unclear.
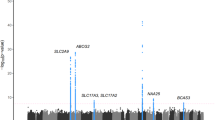
ATP-binding cassette (ABC) transporter, subfamily G, member 2 gene ABCG2/BCRP locates in a gout-susceptible locus (MIM 138900) on chromosome 4q11, which was earlier demonstrated by a genome-wide linkage study of gout11. Genome-wide association studies (GWAS) of serum uric acid (SUA) also identified several transporter genes including ABCG212,13,14. Recently, Woodward et al.15 and the present authors16 independently showed that ABCG2 regulates SUA as a urate transporter, which mediates urate excretion. We also showed that genotyping of only two dysfunctional variants, Q126X (rs72552713) and Q141K (rs2231142), is sufficient to estimate the severity of ABCG2 dysfunction; i.e. full function, 3/4 function (mild dysfunction), 1/2 function (moderate dysfunction) and ≤ 1/4 function (severe dysfunction). This dysfunction increases gout risk markedly, conferring an OR of more than 3.016. Furthermore, our human genetic analysis and animal model studies demonstrated that ABCG2 dysfunction plays an important role in the pathogenesis of hyperuricemia17. Because the dysfunctional ABCG2 genotype combinations are very common in gout/hyperuricemia patients15,16,18,19, ABCG2 dysfunction is a possible major cause of early-onset gout. In this study, we investigated the estimated ABCG2 function in 705 gout cases with onset age data and 1,887 controls to determine whether or not common dysfunction of ABCG2 causes early-onset gout.
Results
Onset age and ABCG2 function
Table 1 shows the genotype and estimated function of ABCG2 in 2,592 male Japanese (705 gout cases and 1,887 controls). Among them, in 705 gout cases, the less activity the ABCG2 function showed the younger the onset age of gout became (Fig. 1). The onset age of patients with severe ABCG2 dysfunction (≤ 1/4 function) was 6.5 years younger than those with full function. Cox regression analysis also showed that ABCG2 dysfunction significantly hastened the onset age (P = 6.14 × 10−3).
Association analysis of gout
The logistic regression analysis of ABCG2 dysfunction demonstrated the increased risk of gout in each dysfunctional group with 705 cases and 1,887 controls. The odds ratio (OR) was 2.74 (95% CI 2.21–3.39; P = 3.98 × 10−20) with mild dysfunction (3/4 function) and was markedly increased to 9.98 (95% CI 5.63–17.7; P = 3.62 × 10−15) with severe dysfunction (≤ 1/4 function) (Fig. 2).
Odds ratios for ABCG2 dysfunctions among gout patients in each onset age group.
Shown are the odds ratios (ORs) on a log10 scale of the gout risks for each onset age group and ABCG2 dysfunction. ORs and 95% confidence intervals (CIs) for each ABCG2 dysfunction were obtained by comparing with full function and adjusted for body mass index with logistic regression analysis. Circles and diamonds with horizontal lines indicate ORs with 95% CIs of each onset age groups. All ABCG2 dysfunction levels significantly increased the risk of gout (OR > 2.38) in all onset-age groups. Severe ABCG2 dysfunction especially increased the risk of early-onset gout, conferring an adjusted OR of 22.2.
The subsequent logistic regression analysis was performed to evaluate the association between ABCG2 dysfunction and early-onset gout (twenties or younger), as ABCG2 dysfunction accounted for as much as 88.2% of the early-onset gout cases. Compared with full function, severe ABCG2 dysfunction especially increased the risk of early-onset gout, conferring an adjusted OR of 22.2 (95% CI 5.89–83.7; P = 4.66 × 10−6). In addition, moderate and mild dysfunction of ABCG2 markedly increased the risk of early-onset gout, conferring an adjusted OR of 15.3 (95% CI 7.53–30.9; P = 4.08 × 10−14) and 6.47 (95% CI 3.31–12.7; P = 4.89 × 10−8), respectively (Supplementary Fig. S1). In fact, any dysfunction of ABCG2 significantly increased the risk of gout in all onset-age groups (Fig. 2).
Discussion
Our findings make it clear for the first time that any ABCG2 dysfunction causes early-onset gout. Dysfunctional ABCG2 accounts for approximately 90% of early-onset gout patients and accelerated early onset significantly in the present study. Moreover, the risk of early-onset gout is markedly increased by severe ABCG2 dysfunction, conferring an adjusted OR of 22.2. Thus, ABCG2 dysfunction is indeed a major cause of early-onset gout. To our knowledge, this is the first report on a common genetic cause of an early-onset gout that occurs in the twenties or earlier.
Generally, SUA levels in humans are higher than in most other mammals including mice, because humans lack the uric acid-degrading enzyme uricase20. Most uric acid mobilization is mediated by urate transporters in human kidneys. Therefore, human genetic studies have an advantage over rodent models in analyzing the urate transporters in humans. Indeed, in addition to ABCG2, our human genetic studies demonstrated that a urate transporter 1 (URAT1/SLC22A12) encodes renal urate reabsorption transporter and that its loss-of-function mutant causes renal hypouricemia type 1 (MIM 220150)21. After GWAS identified an association between SUA and glucose transporter 9 (GLUT9/SLC2A9) gene22, we also demonstrated that GLUT9 encodes another renal urate reabsorption transporter and is a causative gene for renal hypouricemia type 2 (MIM 612076)23.
Recent genetic studies also revealed that various genes have associations with common diseases, such as coronary artery diseases24,25,26, stroke27, diabetes mellitus26,28 and Alzheimer's disease29. The ORs to assess the risk of onset in these studies were, however, likely to fall in the 1.2 to 1.3 range or lower30. To date, there have been few genes to explain major genetic causes of common diseases. The same holds true for early-onset common diseases31,32. In the case of early-onset gout, the genetic causes have not been identified except for very rare Mendelian disorders33 such as hypoxanthine guanine phosphoribosyltransferase (HPRT) deficiency including Lesch-Nyhan syndrome (MIM 300322)34, phosphoribosylpyrophosphate synthetase (PRPS) superactivity (MIM 300661)35 and familial juvenile hyperuricemic nephropathy (FJHN [MIM 162000])36,37.
In the present study, Cox regression analysis of 705 gout patients revealed that ABCG2 dysfunction significantly decreases onset age (P = 6.14 × 10−3). The onset age was 6.5 years earlier with severe ABCG2 dysfunction. The gout risk is markedly increased in the younger generation having ABCG2 dysfunction. The ORs in the youngest onset-age group (onset age ≤ twenties) with severe, moderate and mild dysfunction were 22.2, 15.3 and 6.47, respectively (Fig. 2). These risks were considerably higher than those of all gout patients, conferring ORs of 9.98, 4.71 and 2.74, respectively (Fig. 2). Thus, ABCG2 dysfunction remarkably increases the risk of gout, especially for younger age-onset groups. In addition, mild to severe ABCG2 dysfunction was detected in up to 88.2% of early-onset gout patients, against 49.8% in controls. Our overall results clearly show that common dysfunction of ABCG2 is a major cause of early-onset gout.
Because early-onset gout will compromise patients' quality of life (QOL) for a long time and require huge life-long medical costs38, early screening for ABCG2 dysfunction and appropriate interventions will greatly benefit high-risk individuals. Moreover, risk assessment by genotyping of only two SNPs will provide a very cost-effective method for screening and personalized medicine including adequate prevention and effective therapy. Therefore, our findings will serve to improve the QOL of high-risk individuals and reduce health-care costs, which also promote public health and preventive medicine.
Methods
Study participants
All procedures were carried out in accordance with the standards of the institutional ethical committees involved in this project and the Declaration of Helsinki. Informed consent in writing was obtained from each subject participating in this study. Genotyping was performed in 2,592 male Japanese (705 gout cases and 1,887 controls). All cases were clinically diagnosed as primary gout according to the criteria established by the American College of Rheumatology39 at the gout clinics of either Jikei University Hospital (Tokyo, Japan) or Midorigaoka Hospital (Osaka, Japan). Patients with inherited metabolism disorders including Lesch-Nyhan syndrome were excluded beforehand and onset age data were available in all cases. As control, 1,887 individuals were assigned from Japanese male health examinees with normal SUA (≤ 7.0 mg/dl) and no gout history.
Genetic analysis
Genomic DNA was extracted from whole peripheral blood cells40. Genotyping of Q126X (rs72552713) and Q141K (rs2231142) in ABCG2 gene by high-resolution melting (HRM) analysis was performed with a LightCycler 480 (Roche Diagnostics)41. To confirm their genotypes, more than one hundred samples including all genotype combinations identified by HRM were subjected to direct sequencing. DNA sequencing analysis was performed with a 3130xl Genetic Analyzer (Applied Biosystems)23. ABCG2 genotype combinations were divided into four functional groups on the basis of the estimated ABCG2 transport functions16; i.e. full function, 3/4 function (mild dysfunction), 1/2 function (moderate dysfunction) and ≤ 1/4 function (severe dysfunction) as shown in Table 1.
Statistical analysis
For all calculations in the statistical analysis, the software SPSS v. 16.0J (IBM Japan Inc., Tokyo, Japan) and JMP 10.0.0 (SAS Institute Japan Inc., Tokyo, Japan) were used. Logistic regression analysis was performed to estimate adjusted genetic effects. Cox regression analysis was conducted to obtain adjusted P value for onset age. These regression analyses were corrected by body-mass index (BMI).
References
Feig, D. I., Kang, D. H. & Johnson, R. J. Uric acid and cardiovascular risk. N. Engl. J. Med. 359, 1811–1821 (2008).
Cannon, P. J., Stason, W. B., Demartini, F. E., Sommers, S. C. & Laragh, J. H. Hyperuricemia in primary and renal hypertension. N. Engl. J. Med. 275, 457–464 (1966).
Forman, J. P., Choi, H. & Curhan, G. C. Uric acid and insulin sensitivity and risk of incident hypertension. Arch. Intern. Med. 169, 155–162 (2009).
Tuttle, K. R., Short, R. A. & Johnson, R. J. Sex differences in uric acid and risk factors for coronary artery disease. Am. J. Cardiol. 87, 1411–1414 (2001).
Lin, Y. H. et al. Gouty arthritis in acute cerebrovascular disease. Cerebrovasc. Dis. 28, 391–396 (2009).
Talaat, K. M. & el-Sheikh, A. R. The effect of mild hyperuricemia on urinary transforming growth factor beta and the progression of chronic kidney disease. Am. J. Nephrol. 27, 435–440 (2007).
Doherty, M. New insights into the epidemiology of gout. Rheumatology (Oxford). 48 Suppl 2, ii2–ii8 (2009).
Tanaka, E. et al. Recent trend in the onset age of gouty arthritis in Japan [in Japanese]. Gout Nucleic Acid Metab 28, 7–11 (2004).
Yu, K. H. & Luo, S. F. Younger age of onset of gout in Taiwan. Rheumatology (Oxford). 42, 166–170 (2003).
Bleyer, A. J. & Hart, T. C. Genetic factors associated with gout and hyperuricemia. Adv Chronic Kidney Dis 13, 124–130 (2006).
Cheng, L. S. et al. Genomewide scan for gout in Taiwanese aborigines reveals linkage to chromosome 4q25. Am. J. Hum. Genet. 75, 498–503 (2004).
Dehghan, A. et al. Association of three genetic loci with uric acid concentration and risk of gout: a genome-wide association study. Lancet 372, 1953–1961 (2008).
Kolz, M. et al. Meta-analysis of 28,141 individuals identifies common variants within five new loci that influence uric acid concentrations. PLoS Genet. 5, e1000504 (2009).
Kamatani, Y. et al. Genome-wide association study of hematological and biochemical traits in a Japanese population. Nat. Genet. 42, 210–215 (2010).
Woodward, O. M. et al. Identification of a urate transporter, ABCG2, with a common functional polymorphism causing gout. Proc. Natl. Acad. Sci. U. S. A. 106, 10338–10342 (2009).
Matsuo, H. et al. Common defects of ABCG2, a high-capacity urate exporter, cause gout: a function-based genetic analysis in a Japanese population. Sci. Transl. Med. 1, 5ra11 (2009).
Ichida, K. et al. Decreased extra-renal urate excretion is a common cause of hyperuricemia. Nat. Commun. 3, 764 (2012).
Phipps-Green, A. J. et al. A strong role for the ABCG2 gene in susceptibility to gout in New Zealand Pacific Island and Caucasian, but not Maori, case and control sample sets. Hum. Mol. Genet. 19, 4813–4819 (2010).
Yamagishi, K. et al. The rs2231142 variant of the ABCG2 gene is associated with uric acid levels and gout among Japanese people. Rheumatology (Oxford). 49, 1461–1465 (2010).
Lee, C. C. et al. Generation of cDNA probes directed by amino acid sequence: cloning of urate oxidase. Science 239, 1288–1291 (1988).
Enomoto, A. et al. Molecular identification of a renal urate anion exchanger that regulates blood urate levels. Nature 417, 447–452 (2002).
Li, S. et al. The GLUT9 gene is associated with serum uric acid levels in Sardinia and Chianti cohorts. PLoS Genet. 3, e194 (2007).
Matsuo, H. et al. Mutations in glucose transporter 9 gene SLC2A9 cause renal hypouricemia. Am. J. Hum. Genet. 83, 744–751 (2008).
Connelly, J. J. et al. GATA2 is associated with familial early-onset coronary artery disease. PLoS Genet. 2, e139 (2006).
Samani, N. J. et al. Genomewide association analysis of coronary artery disease. N. Engl. J. Med. 357, 443–453 (2007).
Wellcome Trust Case Control Consortium. Genome-wide association study of 14,000 cases of seven common diseases and 3,000 shared controls. Nature 447, 661–678 (2007).
Ikram, M. A. et al. Genomewide association studies of stroke. N. Engl. J. Med. 360, 1718–1728 (2009).
Scott, L. J. et al. A genome-wide association study of type 2 diabetes in Finns detects multiple susceptibility variants. Science 316, 1341–1345 (2007).
Lambert, J. C. et al. Genome-wide association study identifies variants at CLU and CR1 associated with Alzheimer's disease. Nat. Genet. 41, 1094–1099 (2009).
Manolio, T. A., Brooks, L. D. & Collins, F. S. A HapMap harvest of insights into the genetics of common disease. J. Clin. Invest. 118, 1590–1605 (2008).
Kathiresan, S. et al. Genome-wide association of early-onset myocardial infarction with single nucleotide polymorphisms and copy number variants. Nat. Genet. 41, 334–341 (2009).
Khachaturian, A. S., Corcoran, C. D., Mayer, L. S., Zandi, P. P. & Breitner, J. C. Apolipoprotein E epsilon4 count affects age at onset of Alzheimer disease, but not lifetime susceptibility: The Cache County Study. Arch. Gen. Psychiatry 61, 518–524 (2004).
Zaka, R. & Williams, C. J. New developments in the epidemiology and genetics of gout. Curr. Rheumatol. Rep. 8, 215–223 (2006).
Torres, R. J. & Puig, J. G. Hypoxanthine-guanine phosophoribosyltransferase (HPRT) deficiency: Lesch-Nyhan syndrome. Orphanet J Rare Dis 2, 48 (2007).
Becker, M. A., Meyer, L. J., Wood, A. W. & Seegmiller, J. E. Purine overproduction in man associated with increased phosphoribosylpyrophosphate synthetase activity. Science 179, 1123–1126 (1973).
Hart, T. C. et al. Mutations of the UMOD gene are responsible for medullary cystic kidney disease 2 and familial juvenile hyperuricaemic nephropathy. J. Med. Genet. 39, 882–892 (2002).
Kamatani, N. et al. Localization of a gene for familial juvenile hyperuricemic nephropathy causing underexcretion-type gout to 16p12 by genome-wide linkage analysis of a large family. Arthritis Rheum. 43, 925–929 (2000).
Wu, E. Q. et al. Disease-related and all-cause health care costs of elderly patients with gout. J Manag Care Pharm 14, 164–175 (2008).
Wallace, S. L. et al. Preliminary criteria for the classification of the acute arthritis of primary gout. Arthritis Rheum. 20, 895–900 (1977).
Matsuo, H. et al. Familial paroxysmal dystonic choreoathetosis: clinical findings in a large Japanese family and genetic linkage to 2q. Arch. Neurol. 56, 721–726 (1999).
Margraf, R. L., Mao, R. & Wittwer, C. T. Rapid diagnosis of MEN2B using unlabeled probe melting analysis and the LightCycler 480 instrument. J Mol Diagn 10, 123–128 (2008).
Acknowledgements
We would like to thank all the patients and healthy volunteers involved in this study. We also thank J. Abe, K. Gotanda, Y. Morimoto, N. Katsuta, Y. Utsumi, S. Terashige, Y. Kato, H. Sasaki, Y. Takashima and H. Fujiwara, National Defense Medical College, Tokorozawa, Japan and T. Tamatsukuri, Jikei University School of Medicine, Tokyo, Japan for genetic analysis. This study was supported by grants from the Ministry of Education, Culture, Sports, Science and Technology of Japan (including the Grant-in-Aid for Scientific Research on Innovative Areas “Genome Science”), the Ministry of Health, Labor and Welfare of Japan, the Ministry of Defense of Japan, the Japan Society for the Promotion of Science, the Takeda Science Foundation, the AstraZeneca VRI Research Grant, the Kawano Masanori Memorial Foundation for Promotion of Pediatrics and the Gout Research Foundation of Japan.
Author information
Authors and Affiliations
Contributions
H.M., K.I., T.T., A.N., M.H., H.S., Y.K. and N.S. designed the experiment. H.M., K.I., A.N., T.H. and T.S. carried out patient analysis. H.M., K.I., A.N., Y.K., Y.T., K.Y., H.I., Y.O., C.O., S.S., M.S., T.C., H.O., K.N. and N.S. performed genetic analysis. H.M., A.N., M.N., A.H., K.W., A.M. and N.H. collected samples. H.N., T.N. and Y. S. performed statistical analysis. H.M., K.I., T.T., A.N. and N.S. wrote the paper. H.M., K.I., T.T. and A.N. contributed equally to this work.
Ethics declarations
Competing interests
H.M., K.I., T.T., T.N., H.S. and N.S. have a patent pending based on the work reported in this paper. The other authors declare no competing financial interests.
Electronic supplementary material
Supplementary Information
Supplementary Figure 1
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Matsuo, H., Ichida, K., Takada, T. et al. Common dysfunctional variants in ABCG2 are a major cause of early-onset gout. Sci Rep 3, 2014 (2013). https://doi.org/10.1038/srep02014
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep02014
This article is cited by
-
Evaluation of ABCG2-mediated extra-renal urate excretion in hemodialysis patients
Scientific Reports (2023)
-
Comparison Between Early-Onset and Common Gout: A Systematic Literature Review
Rheumatology and Therapy (2023)
-
The Hong Kong Society of Rheumatology consensus recommendations for the management of gout
Clinical Rheumatology (2023)
-
Emerging Urate-Lowering Drugs and Pharmacologic Treatment Strategies for Gout: A Narrative Review
Drugs (2023)
-
Relationship between CYP2C8, UGT1A1, and ABCG2 gene polymorphisms and the exposure, efficacy, and toxicity of eltrombopag in the treatment of refractory aplastic anemia
European Journal of Clinical Pharmacology (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.