Abstract
Working memory (WM) capacity improvement is impacted by sleep and possibly by N-methyl-D-aspartate (NMDA) agonists such as D-cycloserine (DCS), which also affects procedural skill performance. However, the mechanisms behind these relationships are not well understood. In order to investigate the neural basis underlying relationships between WM skill learning and sleep, DCS and both sleep and DCS together, we evaluated training-retest performances in the n-back task among healthy subjects who were given either a placebo or DCS before the task training and then followed task training sessions either with wakefulness or sleep. DCS facilitated WM capacity enhancement only occurring after a period of wakefulness, rather than sleep, indicating that WM capacity enhancement is affected by a cellular heterogeneity in synaptic plasticity between time spent awake and time spent asleep. These findings may contribute to development, anti-aging processes and rehabilitation of higher cognition.
Similar content being viewed by others
Introduction
Working memory (WM) is regarded as a specific process by which a remembered stimulus is held “on-line” to guide behavior in the absence of external cues or prompts1,2,3. WM capacity, the maximum amount of information that can be retained in the WM, is an important factor influencing problem-solving and reasoning abilities4,5,6. The “n-back” task7,8,9,10 has been utilized to measure individuals’ WM capacity, as well as the neural basis of WM processes. Repetitive training facilitates improvements in WM capacity, an aspect of spatial WM performance associated with increased activities of relevant cortices, including the dorsolateral and medial prefrontal cortices (PFC) and the superior and inferior parietal cortices11. Moreover, improvement of WM capacity is achieved through the off-line process of neuroplasticity during sleep12. Significant improvements in WM capacity measured by a spatial n-back task were observed after subjects received a night of posttraining sleep, but not over a similar period of wakefulness; this result was seen regardless of whether time awake or time asleep occurred first and whether subjects were initially trained during morning, midday or evening12.
Although sleep plays a crucial role in the off-line development of various domains of skill learning13,14,15,16,17, delayed skill consolidation could also occur during periods of wakefulness18, suggesting that differences in delayed skill consolidation during sleep and wakefulness result from corresponding differences in neural substrate15,19,20. One of the key excitatory neurotransmitters is glutamate21,22,23,24. Activation of the N-methyl-D-aspartate (NMDA) glutamate receptor mediates a long-lasting increase in synaptic potentiation at the intracellular level25,26, which is thought to elicit synaptic plasticity and delayed skill consolidation27,28. Administration of NMDA receptor antagonists can prohibit long-term synaptic potentiation, thus preventing skill-learning practice from translating into successful skill acquisition in animals29. On the other hand, the administration of NMDA receptor agonists enhances skill-learning in animals30, including humans31. NMDA receptor-dependent glutamatergic neurotransmission contributes to the formation of long-term memory, not only within the hippocampus32 but also within the PFC33. Thus, it is likely that NMDA receptor agonists enhance WM capacity improvements via enhancing NMDA receptor-dependent synaptic plasticity in the PFC. An evidence suggesting that downregulation of NMDA receptors results in decreased spatial WM performance24 could also paradoxically support the notion.
In the current study, we explored delayed skill learning properties by using the n-back task12 to examine the effect of an NMDA partial agonist, D-cycloserine (DCS), on WM capacity improvement. DCS acts at the strychnine-insensitive glycine site of NMDA glutamate receptors. DCS is known to facilitate extinction of fear-conditioning in rats34,35,36 and humans37, as well as non-emotional skill learning31,38. Further, we also examined whether DCS interacted with sleep-dependent WM capacity improvement. We predicted that these data might help identify the distinct neural backgrounds underlying the differences between these skill consolidation processes; further, this information could be used for developing a technique facilitating improvements in overall human higher cognition.
Results
Psychomotor Performance
Results of the questionnaire about side effects showed that 2–3 subjects in each treatment group (Fig. 1, see Methods) reported drowsiness after administration of either DCS or the placebo; however, no significant drug-induced adversities were reported. At each training and retesting point, all subjects performed a psychomotor vigilance task (PVT), which is a measure of the psychomotor vigilance level39. Three-way ANOVA revealed that neither group (F1,52 = 0.38, p = 0.54) nor session (F1,52 = 0.70, p = 0.79) nor sex (F1,52 = 0.04, p = 0.84) significantly affected the simple response time (SRT) of the PVT in groups A and B; likewise, there was also no effect of the possible interaction terms (all F1,52 < 0.20, all p > 0.70). Four-way ANOVA also revealed that neither session (F1,100 = 0.04, p = 0.84) nor medication (F1,100 = 0.14, p = 0.71) nor inter-session schedule (F1,100 = 2.00, p = 0.16) nor sex (F1,100 = 2.07, p = 0.15) significantly affected the SRT of the PVT in groups C–F; likewise, there was also no effect of the possible interaction terms (all F1,100 < 2.50, all p > 0.12). Additionally, no subjects displayed any lapses during the PVT. These results suggest that subjects in groups A and B or C–F had similar psychomotor vigilance levels during each test session.
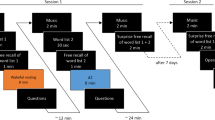
Experimental schedules for each of the 6 treatment groups.
Subjects were assigned to 3 pairs of randomized, blind, placebo-controlled, 2-arm experimental groups (A–F). Each group underwent a specific schedule consisting of an initial training session and a retest session. Subjects were administered encapsulated DCS (groups B, E and F) or a placebo (groups A, C and D) on an empty stomach 1.5 h prior to the training session. Subjects in groups A and B were placed on a diurnal experimental schedule, in which they were trained at 20:00 h and were then retested at 20:00 h the next day (e.g., 24 h later). Subjects in groups C–F were placed on a semidiurnal experimental schedule. Individuals in groups C and E were trained at 20:00 h and were retested at 08:00 h the following day (e.g., 12 h later) after a night of sleep. Individuals in groups D and F were trained at 08:00 h and were retested at 20:00 h after 12 h of wakefulness. All subjects performed spatial n-back WM tasks (n = 1–7) during each test session. All post-sleep retests were performed at least 1 h after awakening.
Sleep Length
Two-way ANOVA showed that neither group (F1,26 = 3.40, p = 0.08) nor sex (F1,26 = 0.24, p = 0.63) nor interaction of the two (F1,26 = 1.51, p = 0.23) had a significant effect on the amount of sleep received on pre-training (group A: 6.54 ± 0.13 h; group B: 7.16 ± 0.26 h). Three-way ANOVA showed that neither medication (F1,50 = 1.16, p = 0.29) nor inter-session schedule (F1,50 = 1.49, p = 0.23), sex (F1,50 = 2.28, p = 0.14) nor possible interactions among them (all F1,50 < 3.50, all p > 0.05) had a significant effect on the amount of sleep received in pre-training (group C: 6.64 ± 0.21 h; group D: 6.75 ± 0.24 h; group E: 6.57 ± 0.24 h; group F: 7.15 ± 0.16 h). Besides, two-way ANOVA showed that neither group (F1,26 = 0.03, p = 0.86; F1,26 = 1.01, p = 0.32) nor sex (F1,26 = 0.37, p = 0.55; F1,26 = 1.82, p = 0.19) nor interaction between them (F1,26 = 0.23, p = 0.88; F1,26 = 0.85, p = 0.77) had a significant effect on the amount of sleep received in post-training in groups A vs. B or C vs. E (Group A: 6.50 ± 0.21 h; Group B: 6.55 ± 0.22 h; Group C: 6.00 ± 0.19 h; Group E: 6.32 ± 0.21 h).
Initial Training Performance
Three-way ANOVA showed that n-back accuracy level was significantly impacted by training (F2,252 = 27.0, p < 0.0001), but not by medication (F1,252 = 0.41, p = 0.52) or sex (F1,252 = 2.27, p = 0.13); the possible interaction terms were also not significantly associated with accuracy level (all F < 0.50, p > 0.60; Fig. 2). Subsequent post-hoc tests showed that training significantly improved n-back accuracy level between the first and second trials (p < 0.0001) and between the first and third trials (p < 0.0001), but not between the second and third trials (p = 0.10). Although repetitive training of the n-back WM task maximized task performance almost by the end of the second trial, DCS administration had no effect throughout the training period. Moreover, it is indicated that there was no sex difference in the training performance of the n-back WM task.
Changes in working memory (WM) capacity during the training period.
Subjects were administered either a placebo (open circles with dotted line; groups A, C and D) or D-cycloserine (DCS; closed circles with continuous line; groups B, E and F). Subjects in both groups showed significant improvements in n-back accuracy levels across the 3 trials, but the rates of improvement were not related to medication. By the end of training, rates of improvement in both groups had nearly plateaued and accuracy levels in the 2 groups differed by only 0.06 ± 0.18 [mean ± standard error of the mean (SEM)]. The heights of the circles and error bars represent means and SEMs, respectively. Asterisks (**) indicate p < 0.0001.
Delayed Improvements in n-back Performance during Diurnal Experimental Period
A three-way ANOVA showed that, while session had a significant impact on n-back accuracy level (F1,52 = 22.8, p < 0.0001), medication (F1,52 = 1.99, p = 0.16)and sex (F1,52 = 0.004, p = 0.95) did not during the diurnal experimental period (groups A and B). However, there was a significant effect of the session × medication interaction term (F1,52 = 4.39, p = 0.041; Fig. 3A), while there were not any other interaction terms (all F1,52 < 1.0, all p > 0.45). Specifically, there was a significant difference in improvement in the n-back accuracy level between groups A and B (t28 = 3.21, p = 0.003; Fig. 3B). This indicates that although delayed improvements in n-back accuracy level were achieved in both groups, this process was significantly facilitated by DCS.
Changes in working memory (WM) capacity between and within testing sessions in experimental groups on the diurnal schedule (24-h interval between the testing sessions).
(A) The n-back accuracy level significantly improved between the training and retest periods in both groups (p < 0.0001). However, the significant session × medication interaction (p = 0.041) suggests that DCS administration facilitated the greater improvements observed in group B. Light and dark green bars represent n-back accuracy levels at the training and retest sessions, respectively. (B) Inter-session improvements in n-back accuracy level in groups A and B. The n-back accuracy level improved significantly more (p < 0.005, indicated by the asterisk) in group B, which received the DCS treatment, than in group A, which received the placebo treatment. The heights of the brown bars and error bars represent the mean and SEM, respectively.
Delayed Improvements in n-back Performance during Semidiurnal Experimental Period
A four-way ANOVA showed that n-back accuracy level was significantly affected by session (F1,100 = 8.82, p = 0.004), but not by medication (F1,100 = 1.48, p = 0.23), schedule (F1,100 = 0.02, p = 0.89), sex (F1,100 = 2.91, p = 0.091), or any of the possible interaction terms (all F1,100 < 2.0, all p > 0.10; Fig. 4A) during the semidiurnal experimental period (groups C–F). A two-way ANOVA revealed a significant effect of the medication × schedule interaction term (F1,54 = 4.75, p = 0.034) on improvement of n-back accuracy level, but non-significant effects of either medication (F1,54 = 0.42, p = 0.52) or schedule (F1,54 = 0.66, p = 0.42) alone (Fig. 4B). Subsequent post-hoc tests revealed trends toward significant differences between groups C and D (p = 0.038) and groups D and F (p = 0.046) in the improvement of n-back accuracy level. These findings suggest that DCS does not facilitate sleep-dependent skill consolidation, but, rather, skill consolidation during wakefulness.
Changes in working memory (WM) capacity between and within testing sessions in experimental groups on the semidiurnal schedule (12-h interval between testing sessions).
(A) WM capacity significantly improved (p < 0.005) between the training and retest sessions for groups C–F. Light and dark green bars represent n-back accuracy levels at the training and retest sessions, respectively. (B) Inter-session differences in n-back accuracy levels in groups C–F. In groups receiving the placebo (PLC) treatment (C, D), sleep seemed to facilitate improvement in accuracy more than wakefulness. However, improvements in n-back accuracy levels were similar in groups receiving the D-cycloserine (DCS) treatment, regardless of whether they followed training with a period of wakefulness (F) or sleep (E). Blue and yellow bars represent changes in n-back accuracy level during sleep and wake periods, respectively. The heights of the bars and error bars represent the mean and SEM, respectively. The crosses (†) indicate a trend toward significance (p < 0.05).
Discussion
First of all, any sex effects on vigilance levels, sleep lengths, WM performances, DCS effects and interactions between WM performance and DCS effect were not observed in the current study.
A definite improvement in WM capacity was observed within 2 trials during the training session; subjects had almost reached a performance plateau by the third n-back trial. Initial acquisition of WM skill performance was not facilitated by DCS. Onur et al. suggested that DCS does not facilitate immediate learning despite potentially accelerating hippocampal activity38. Thus, DCS may enhance the encoding process and accelerate delayed, rather than immediate, learning.
Medication and sleep quality did not significantly affect psychomotor vigilance levels in the different treatment groups; however, we did observe various group differences in the improvement of n-back accuracy levels across training-retest sessions. Differences in groups A (0.79%) and B (1.88%) in the improvement of n-back accuracy level clearly indicate that DCS facilitates the improvement of WM capacity during a 24-h post-training interval. Additionally, differences in accuracy improvements among groups C-F (C: 0.71%, D: 0.23%, E: 0.47%, F: 0.69%) suggest that DCS had higher efficacy when followed by wakefulness than when followed by sleep. Although there is no evidence that DCS affects sleep architecture, our results clearly indicate that WM capacity improvement facilitated by DCS was not achieved via sleep modulation.
A comparison of groups B and E does not immediately explain why the 24-h effect should emerge during the second 12 h of wakefulness, since DCS is probably no longer fully active during this period. We need to compare the results of the 2 experimental groups in which subjects first stayed awake and then slept during the diurnal (24 h) experimental schedule with DCS or placebo administration with those of the current study. These experimental groups would greatly establish our claims, however, we previously confirmed that overnight improvements in WM capacity were observed regardless of whether time awake or time asleep occurred first12. Taken together, these results suggest that DCS potentially affects the skill acquisition process, with delayed onset of action only occurring after a period of wakefulness, rather than sleep. The remaining question is whether the DCS interacts with sleep to have an impact on WM capacity. The results from groups C–F suggest that it does not. The largest improvement, observed after 24 h in group B, may result from simple integration of separate delayed improvements from the sleep-dependent skill consolidation process (robustly reflected in group C) and the DCS-facilitated skill consolidation process (robustly reflected in group F).
The other limitation remained that although DCS does not directly facilitate immediate learning of the WM skill, there is debate over whether DCS facilitates the consolidation process of the WM skill or merely facilitates delayed performance of the WM skill. Especially in semidiurnal experimental groups, DCS could act to even retest performances due to the long half-life of DCS40. If WM skill performance per se is facilitated by current enhancement of DCS binding activity of the NMDA receptor, initial training performances could be much enhanced and retest performances of the diurnal experimental groups could be less enhanced than retest performances of the semidiurnal experimental groups. Therefore, the current results suggest that DCS acts within the neuroplastic process during the delayed consolidation process that occurs in wakefulness.
Heterogenous neuroplastic processes seem to develop with WM capacity improvement during both sleep and wakefulness. During wakefulness, WM capacity improvement may have resulted from a delayed memory consolidation process driven by the cellular mechanism of long-term potentiation41,42,43, which could be facilitated by an NMDA agonist. However, during the sleep period, there may have been an additional delayed learning process dependent not on a given cellular long-term potentiation mechanism but on a novel mechanism by which neuroplasticity contributes to skill consolidation. A likely explanation is that sleep-dependent skill consolidation is generated via a reassembly of the cortical networks11,44 and may be independent of the synaptic-level consolidation process associated with NMDA receptor-dependent neuroplasticity. Changes in cortical activity have been observed in response to 5 weeks of WM training11. These include increases in activity in the middle frontal gyrus and superior and inferior parietal cortices, which may be consequences of the reorganization of reassembly activation patterns in the connections of both intracellular45 and intracortical46 levels. Delayed learning processes during sleep and wakefulness possibly share these roles in consolidating skill over an extended period of time. Although these neuronal reorganizations in 2 different levels may not be mutually exclusive44, our results suggest the neuronal reorganization of intracellular level predominantly occurs during wakefulness while that of the intracortical level predominantly occurs during sleep. Thus, DCS is able to enhance only the neuronal reorganization of intracellular level during wakefulness. Additionally, a previous study investigating motor skill improvement suggested that qualitatively different aspects of delayed learning resulted from intervals of sleep versus wakefulness47. A similar process may occur during WM capacity improvement.
MK-801 (dizocilpine), an NMDA glutamate receptor antagonist, has been shown to impair the consolidation of spatial WM skill learning across several days in animals29. On the other hand, another NMDA antagonist, amantadine, is not known to impair simple motor skill consolidation in humans48. However, when administered to human subjects, the NMDA antagonists caroverine and ketamine prevent delayed consolidation of visual procedural skill learning during sleep without affecting sleep architecture49. These findings seem to be restricted to each skill domain. However, when they are considered together with our current results, they suggest that the activity of the glutaminergic synapses during sleep and wakefulness could play complementary roles for skill consolidation; specifically, while consolidation of skill (including WM capacity) may occur predominantly during sleep, this process may not proceed during wakefulness until exposure to a glutaminergic receptor stimulant, such as the NMDA agonist DCS.
The prefrontal cortex is regarded as the central structure of WM processing21,24,50 and is known to play a crucial role in enhancing WM performance24,51. Incremental improvements in activities of the middle frontal gyrus and superior and inferior parietal cortices by repetitive WM training11 are less specific to various stimuli that drive cognitive performance52,53,54. Further, repetitive training on a spatial n-back task improves not only spatial n-back performance but also auditory n-back performance, enhancing the development of general fluid intelligence55. Given that WM capacity is an important factor in a wide range of cognitive abilities, including fluid intelligence55 and regulation of emotions56, it is likely that the administration of NMDA agonists with WM training could facilitate potential cognitive ability by boosting the available capacity of prefrontal learning57,58.
Although we instructed study participants to keep regular sleep-wake habits, it is possible that our results were confounded by differences in pre- or post-training sleep patterns or by potential circadian effects. However, both pre- and post-training sleep durations were similar across groups. Thus, we believe that our findings accurately reflect sleep- and wakefulness-related neural processes associated with skill learning and may therefore be helpful for developing techniques for strengthening the cognitive abilities of children59,60 and preventing specific cognitive decrements with aging61,62. NMDA agonists may be useful in the rehabilitation of patients with frontal dysfunctions, which appear to be closely related to general fluid intelligence63,64 and for preventing or treating posttraumatic stress disorder65. Before our results can be applied to achieving these goals, it will be important to further elucidate the neural mechanism of WM capacity development facilitated by NMDA agonists, at both the cellular and cortical network levels.
Methods
Participants
A total of 88 right-handed healthy subjects [21.3 ± 0.14 years old (mean age ± standard error of the mean); range: 20–25 years old; 40 females] participated in this study. Subjects had no previous history of drug or alcohol abuse or of neurological, psychiatric, or sleep disorders and maintained a constant sleep schedule validated by self-recorded sleep-logs. They were instructed to be drug-, alcohol- and caffeine-free for 24 h before and during the study period. Women in the follicular phase of their regular menstrual cycles were included in the study. All study procedures followed the guidelines outlined in the Declaration of Helsinki. The study protocol was approved by the Intramural Research Board of the National Center of Neurology and Psychiatry and all subjects provided written informed consent prior to participating in the study.
Experimental Design
Randomized, blind, placebo-controlled procedures were applied for diurnal and semidiurnal group partition tests (Fig. 1). Random allocation of subjects to 6 different groups (groups A–F) eliminated biases for age (F5,82 = 1.37, p = 0.24) and sex (χ2 = 2.35, p = 0.799). Nineteen subjects were initially recruited, but 2 women were omitted because they had irregular menstrual cycles. Subjects in groups A and B were assigned to a diurnal experimental schedule, which consisted of an initial training session and a retest session. Subjects in groups C–F were placed on semidiurnal experimental schedules, some of which (C, E) included a sleep period and some of which (D, F) did not. We examined the general effect of DCS on the improvement of WM capacity across 24 h by comparing groups A and B. Moreover, to examine whether DCS affects WM capacity by interacting with sleep, we compared groups C–F.
During each test session, subjects performed a spatial n-back WM task (n = 1–7). All post-sleep retests were performed at least 1 h after awakening to avoid the effect of sleep inertia66. Each subject had a sequence of task rehearsals (n = 0–2) prior to receiving medication. Medication (100 mg of either encapsulated DCS or a lactose placebo) was administered on an empty stomach 2 h prior to the training session. Subjects were not able to judge whether they received DCS or placebo. Given that the time course of the plasma concentration and the plasma half-life for DCS are within 1h and 8–12 h, respectively40, this timing ensured that subjects’ performances (including potential delayed learning) would be affected by the drug. DCS was administered to subjects in groups B (21.1 ± 0.34 years old; 8 females and 8 males), D (21.5 ± 0.43 years old; 4 females and 9 males) and F (21.0 ± 0.26 years old; 7 females and 9 males). Previous clinical studies have shown that the 100-mg dose used here facilitates the extinction of pathological fear memory in humans67,68,69. Subjects in groups A (21.8 ± 0.41 years old; 8 females and 6 males), C (20.7 ± 0.24 years old; 7 females and 7 males) and E (21.5 ± 0.34 years old; 6 females and 9 males) were given the lactose placebo.
The amount of pre-training sleep for each subject was estimated by the self-recorded sleep-log. The amount of overnight post-training sleep for each subject in experimental groups A, B, C and E was estimated with an ambulatory wrist activity recorder (Actiwatch-L, Mini-Mitter Co., Inc., Bend, OR, USA).
Working Memory Task
We utilized a spatial variant of the n-back WM task widely used to measure spatial WM with a sustained attention component7,8,9,10. The n-back WM task had 7 increasing levels of difficulty (n = 1–7). Four large dots presented in a single horizontal row were displayed on a computer screen, indicating the 4 possible places where a stimulus could appear12. The stimulus consisted of 1 of 4 dots changing color. Subjects were instructed to respond to the stimulus by using their right fingers to push 1 of 4 spatially corresponding buttons on a response box as quickly and as accurately as possible before the next stimulus appeared. Responses were to be made after a delay of n (load level) stimuli.
At each training or retest session, subjects performed 3 trials separated by 60,000 ms of inter-trial intervals. Each trial consisted of 7 load levels. The different load levels, which were shown before stimulation began, ran in a block of 20 + n stimuli each; thus, 20 responses were obtained at each load level. Each stimulus was displayed in a randomized order for 1500 ms with 500 ms of inter-stimulus interval; thus, each block lasted a total of 42,500–54,500 ms. Subjects completed all 7 load levels in ascending order of difficulty at 15,000 ms intervals in each trial and repeated this sequence 3 times (trials) during each session. Performance was evaluated using the average percentage of correct responses (accuracy) at each load level. The detection threshold for a given session was defined as the maximum n-back accuracy level at which the subject’s accuracy exceeded at least 80%. The maximum n-back accuracy level in the third trial was used to indicate the current WM capacity in each session.
At each training and retesting point, all subjects performed a psychomotor vigilance task (PVT), which is a measure of the psychomotor vigilance level39. The PVT involved pressing a button in response to the presentation of a stimulus (a red dot) on a computer screen. Several stimuli were randomly presented for 2000–10,000 s during a 5-min period, which resulted in a total of 30–45 responses. By measuring the simple response time (SRT), we could count the number of lapses (response time ≥ 500 ms), which were indicative of sleepiness, fatigue and drug-induced impairments. A subjective questionnaire was also utilized to determine whether and what type, of psychomotor side effects were caused by the DCS.
Statistics
Three-way factorial ANOVAs were applied to detect the effects of group (A–B), session (training-retest) and sex (women or men) on PVT performances. Four-way factorial ANOVA was also applied to assay for effects of session, medication (placebo or DCS), inter-session schedule (sleep vs. wakefulness) and sex on PVT performances of groups C–F. Two-way factorial ANOVA and three-way factorial ANOVA were applied to detect the effects of group and sex on amount of pre-training (groups A-B) sleep and pre-training (groups C–F) sleep, respectively. Two-way factorial ANOVAs were applied to detect the effects of group and sex on post-training (group A vs. B and group C vs. E) sleep.
To detect the effects of repetitive training (first to third blocks), medication and sex on the n-back accuracy level, we used three-way repeated measures ANOVA with Bonferroni post hoc tests. A three-way factorial ANOVA was used to measure the effects of DCS on delayed improvement of WM capacity across 24-h intervals; this 2 (groups) × 2 (sessions) × 2 (sexes) analysis allowed us to examine the impact of session (training vs. retest), medication and sex on the n-back accuracy level within groups A and B. An unpaired t-test was also applied to compare improvements in n-back accuracy level (retest minus initial training) in groups A and B.
We used a four-way factorial ANOVA to assay for effects of session, medication, inter-session schedule (sleep vs. wakefulness) and sex on the n-back accuracy level within groups C–F. This 4 (groups) × 2 (sessions) × 2 (schedules) × 2 (sexes) comparison allowed us to determine the impact of DCS on delayed improvement of WM capacity across 12-h intervals involving either sleep or wakefulness. Two-way factorial ANOVAs with Bonferroni’s post hoc tests were also applied to detect the effects of medication and schedule on the improvement of n-back accuracy level (retest minus initial training).
Results are shown as mean ± SEM. Significance was defined as p < 0.05 (adjusted to 0.0167 in the Bonferroni post hoc analysis).
References
Baddeley, A. D. & Hitch, G. J. Working memory: The psychology of learning and motivation. (Bower G. A., ed) pp 47–89. New York: Academic Press (1974).
Goldman-Rakic, P. S. The prefrontal landscape: implications of functional architecture for understanding human mentation and the central executive. Philos .Trans. R. Soc. Lond. B. Biol. Sci. 351, 1445–1453 (1996).
Owen, A. M., Evans, A. C. & Petrides, M. Evidence for a two-stage model of spatial working memory processing within the lateral frontal cortex: a positron emission tomography study. Cereb. Cortex 6, 31–38 (1996).
Fry, A. F. & Hale, S. Processing speed, working memory and fluid intelligence: evidence for a developmental cascade. Psychol. Sci. 7, 237–241 (1996).
Hale, S., Bronik, M. D. & Fry, A. F. Verbal and spatial working memory in school-age children: developmental differences in susceptibility to interference. Dev. Psychol. 33, 364–371 (1997).
Kyllonen, P. C. & Christal, R. E. Reasoning ability is (little more than) working memory capacity?!. Intelligence 14, 389–433 (1990).
Callicott, J. H. et al. Functional magnetic resonance imaging brain mapping in psychiatry: methodological issues illustrated in a study of working memory in schizophrenia. Neuropsychopharmacology 18, 186–196 (1998).
Callicott, J. H. et al. Physiological characteristics of capacity constraints in working memory as revealed by functional MRI. Cereb. Cortex 9, 20–26 (1999).
Gevins, A. & Cutillo, B. Spatiotemporal dynamics of component processes in human working memory. Electroencephalogr. Clin. Neurophysiol. 87, 128–143 (1993).
McEvoy, L. K., Smith, M. E. & Gevins, A. Dynamic cortical networks of verbal and spatial working memory: effects of memory load and task practice. Cereb. Cortex 8, 563–574 (1998).
Olesen, P. J., Westerberg, H. & Klingberg, T. Increased prefrontal and parietal activity after training of working memory. Nat. Neurosci. 7, 75–79 (2004).
Kuriyama, K., Mishima, K., Suzuki, H., Aritake, S. & Uchiyama, M. Sleep accelerates the improvement in working memory performance. J. Neurosci. 28, 10148–10150 (2008).
Karni, A., Tanne, D., Rubenstein, B. S., Askenasy, J. J. & Sagi, D. Dependence on REM sleep of overnight improvement of a perceptual skill. Science 265, 679–682 (1994).
Stickgold, R., James, L. & Hobson, J. A. Visual discrimination learning requires sleep after training. Nat. Neurosci. 3, 1237–1238 (2000).
Stickgold, R., Hobson, J. A., Fosse, R. & Fosse, M. Sleep, learning and dreams: off-line memory reprocessing. Science 294, 1052–1057 (2001).
Walker, M. P., Brakefield, T., Morgan, A., Hobson, J. A. & Stickgold, R. Practice with sleep makes perfect: sleep-dependent motor skill learning. Neuron 35, 205–211 (2002).
Walker, M. P., Brakefield, T., Hobson, J. A. & Stickgold, R. Dissociable stages of human memory consolidation and reconsolidation. Nature 425, 616–620 (2003).
Song, S., Howard, J. H. Jr. & Howard, D. V. Sleep does not benefit probabilistic motor sequence learning. J. Neurosci. 27, 12475–12483 (2007).
Smith, C. Sleep states and memory processes. Behav. Brain Res. 69, 137–145 (1995).
Walker, M. P. & Stickgold, R. Sleep-dependent learning and memory consolidation. Neuron 44, 121–133 (2004).
Seamans, J. K., Nogueira, L. & Lavin, A. Synaptic basis of persistent activity in prefrontal cortex in vivo and in organotypic cultures. Cereb. Cortex 13, 1242–1250 (2003).
Homayoun, H., Stefani, M. R., Adams, B. W., Tamagan, G. D. & Moghaddam, B. Functional interaction between NMDA and mGlu5 receptors: Effects on working memory, instrumental learning, motor behaviors and dopamine release. Neuropsychopharmacology 29, 1259–1269 (2004).
Zhao, M. G. et al. Roles of NMDA NR2B subtype receptor in prefrontal long-term potentiation and contextual fear memory. Neuron 47, 859–872 (2005).
Karlsgodt, K. H. et al. Reduced dysbindin expression mediates N-methyl-D-aspartate receptor hypofunction and impaired working memory performance. Biol. Psychiatry 69, 28–34 (2011).
Artola, A. & Singer, W. Long-term potentiation and NMDA receptors in rat visual cortex. Nature 330, 649–652 (1987).
Rumpel, S., Hatt, H. & Gottmann, K. Silent synapses in the developing rat visual cortex: evidence for postsynaptic expression of synaptic plasticity. J. Neurosci. 18, 8863–8874 (1998).
Miller, K. D., Chapman, B. & Stryker, M. P. Visual responses in adult cat visual cortex depend on N-methyl-D-aspartate receptors. Proc. Natl. Acad. Sci. U. S. A. 86, 5183–5187 (1989).
Kirkwood, A., Rioult, M. C. & Bear, M. F. Experience-dependent modification of synaptic plasticity in visual cortex. Nature 381, 526–528 (1996).
White, A. M. & Best, P. J. The effects of MK-801 on spatial working memory and within-session spatial learning. Pharmacol. Biochem. Behav. 59, 613–617 (1998).
Grzeda, E. & Wisniewska, R. J. Differentiations of the effect of NMDA on the spatial learning of rats with 4 and 12 week diabetes mellitus. Acta. Neurobiol. Exp. (Wars.) 68, 398–406 (2008).
Kuriyama, K., Honma, M., Koyama, S. & Kim, Y. D-cycloserine facilitates procedural learning but not declarative learning in healthy humans: a randomized controlled trial of the effect of D-cycloserine and valproic acid on overnight properties in the performance of non-emotional memory tasks. Neurobiol. Learn. Mem. 95, 505–509 (2011).
Herron, C. E., Lester, R. A., Coan, E. J. & Collingridge, G. L. Frequency-dependent involvement of NMDA receptors in the hippocampus: a novel synaptic mechanism. Nature 322, 265–268 (1986).
Barker, G. R. & Warburton, E. C. NMDA receptor plasticity in the perirhinal and prefrontal cortices is crucial for the acquisition of long-term object-in-place associative memory. J. Neurosci. 28, 2837–2844 (2008).
Walker, D. L., Ressler, K. J., Lu, K. T. & Davis, M. Facilitation of conditioned fear extinction by systemic administration or intra-amygdala infusions of D-cycloserine as assessed with fear-potentiated startle in rats. J. Neurosci. 22, 2343–2351 (2002).
Lee, J. L., Milton, A. L. & Everitt, B. J. Reconsolidation and extinction of conditioned fear: inhibition and potentiation. J. Neurosci. 26, 10051–10056 (2006).
Woods, A. M. & Bouton, M. E. D-cycloserine facilitates extinction but does not eliminate renewal of the conditioned emotional response. Behav. Neurosci. 120, 1159–1162 (2006).
Kuriyama, K., Honma, M., Soshi, T., Fujii, T. & Kim, Y. Effect of D-cycloserine and valproic acid on the extinction of reinstated fear-conditioned responses and habituation of fear conditioning in healthy humans: a randomized controlled trial. Psychopharmacology (Berl.) in press (2011).
Onur, O. A. et al. The N-methyl-D-aspartate receptor co-agonist D-cycloserine facilitates declarative learning and hippocampal activity in humans. Biol. Psychology 67, 1205–1211 (2010).
Corsi-Cabrera, M., Arce, C., Ramos, J., Lorenzo, I. & Guevara, M. A. Time course of reaction time and EEG while performing a vigilance task during total sleep deprivation. Sleep 19, 563–569 (1996).
Neir, K. G. S., Epstein, I. G., Baron, H. & Mulinos, M. G. Absorption, distribution and excretion of cycloserine in man. Antibiot. Annu. 3, 136–140 (1956).
Campbell, I. G., Guinan, M. J. & Horowitz, J. M. Sleep deprivation impairs long-term potentiation in rat hippocampal slices. J. Neurophysiol. 88, 1073–1076 (2002).
Guzman-Marin, R. et al. Suppression of hippocampal plasticity-related gene expression by sleep deprivation in rats. J. Physiol. 575, 807–819 (2006).
Tartar, J. L. et al. Hippocampal synaptic plasticity and spatial learning are impaired in a rat model of sleep fragmentation. Eur. J. Neurosci. 23, 2739–2748 (2006).
Marshall, L. & Born, J. The contribution of sleep to hippocampus-dependent memory consolidation. Trends Cogn. Sci. 11, 442–450 (2007).
Fujisawa, S., Amarasingham, A., Harrison, M. T. & Buzsáki, G. Behavior-dependent short-term assembly dynamics in the medial prefrontal cortex. Nat. Neurosci. 11, 823–833 (2008).
Garagnani, M. & Pulvermüller, F. From sounds to words: a neurocomputational model of adaptation, inhibition and memory processes in auditory change detection. Neuroimage 54, 170–181 (2011).
Kuriyama, K., Stickgold, R. & Walker, M. P. Sleep-dependent learning and motor-skill complexity. Learn. Mem. 11, 705–713 (2004).
Hadj,. Tahar, A., Blanchet, P. J. & Doyon, J. Effect of amantadine on motor memory consolidation in humans. Behav. Pharmacol. 16, 107–112 (2005).
Gais, S., Rasch, B., Wagner, U. & Born, J. Visual-procedural memory consolidation during sleep blocked by glutamatergic receptor antagonists. J. Neurosci. 28, 5513–5518 (2008).
McNab, F. & Klingberg, T. Prefrontal cortex and basal ganglia control access to working memory. Nat. Neurosci. 11, 103–107 (2008).
Jentsch, J. D., Trantham-Davidson, H., Jairl, C., Tinsley, M., Cannon, T. D. & Lavin, A. Dysbindin modulates prefrontal cortical glutamatergic circuits and working memory function in mice. Neuropsychopharmacology 34, 2601–2608 (2009).
Klingberg, T. Concurrent performance of two working memory tasks: potential mechanisms of interference. Cereb. Cortex 8, 593–601 (1998).
Duncan, J. & Owen, A. M. Common regions of the human frontal lobe recruited by diverse cognitive demands. Trends Neurosci. 23, 475–483 (2000).
Westerberg, H. & Klingberg, T. Changes in cortical activity after training of working memory: a single-subject analysis. Physiol. Behav. 92, 186–192 (2007).
Jaeggi, S. M., Buschkuehl, M., Jonides, J. & Perrig, W. J. Improving fluid intelligence with training on working memory. Proc. Natl. Acad. Sci. U. S. A. 105, 6829–6833 (2008).
Schmeichel, B. J., Volokhov, R. & Demaree, H. A. Working memory capacity and the self-regulation of emotional expression and experience. J. Pers. Soc. Psychol. 95, 1526–1540 (2008).
Colom, R., Jung, R. E. & Haier, R. J. General intelligence and memory span: evidence for a common neuroanatomic framework. Cogn. Neuropsychol. 24, 867–878 (2007).
Fukuda, K., Vogel, E., Mayr, U. & Awh, E. Quantity, not quality: The relationship between fluid intelligence and working memory capacity. Psychon. Bull. Rev. 17, 673–679 (2010).
Kuwajima, M. & Sawaguchi, T. Similar prefrontal cortical activities between general fluid intelligence and visuospatial working memory tasks in preschool children as revealed by optical topography. Exp. Brain Res. 206, 381–397 (2010).
Reed, J. A., Einstein, G., Hahn, E., Hooker, S. P., Gross, V. P. & Kravitz, J. Examining the impact of integrating physical activity on fluid intelligence and academic performance in an elementary school setting: a preliminary investigation. J. Phys. Act. Health 7, 343–351 (2010).
Daffner, K. R. et al. Mechanisms underlying age- and performance-related differences in working memory. J. Cogn. Neurosci. 23. 1298–1314 (2011).
Mattay, V. S. et al. Neurophysiological correlates of age-related changes in working memory capacity. Neurosci. Lett. 392, 32–37 (2006).
Woolgar, A. et al. Fluid intelligence loss linked to restricted regions of damage within frontal and parietal cortex. Proc. Natl. Acad. Sci. U. S. A. 107, 14899–14902 (2010).
Reuben, A., Brickman, A. M., Muraskin, J., Steffener, J. & Stern, Y. Hippocampal atrophy relates to fluid intelligence decline in the elderly. J. Int. Neuropsychol. Soc. 17, 56–61 (2011).
Schweizer, S. & Dalgleish, T. Emotional working memory capacity in posttraumatic stress disorder (PTSD). Behav. Res. Ther. 49, 498–504 (2011).
Scheer, F. A., Shea, T. J., Hilton, M. F. & Shea, S. A. An endogenous circadian rhythm in sleep inertia results in greatest cognitive impairment upon awakening during the biological night. J. Biol. Rhythms 23, 353–361 (2008).
Ressler, K. J. et al. Cognitive enhancers as adjuncts to psychotherapy. Use of D-cycloserine in phobic individuals to facilitate extinction of fear. Arch. Gen. Psychiatry 61, 1136–1144 (2004).
Kushner, M. G. et al. D-cycloserine augmented exposure therapy for obsessive-compulsive disorder. Biol. Psychiatry 62, 835–838 (2007).
Wilhelm, S. et al. Augmentation of behavior therapy with D-cycloserine for obsessive-compulsive disorder. Am. J. Psychiatry 165, 335–341 (2008).
Acknowledgements
This work was supported by grants from Grant-in-Aid for Scientific Research (# 21790235) from Ministry of Education, Sports, Science and Culture of Japan and Core Research for Evolutional Science and Technology program from the Japan Science and Technology Corporation.
Author information
Authors and Affiliations
Contributions
KK designed the study and wrote the main manuscript text. MH, MS, MH, TY and SK performed the experiments. YK contributed to random allocation of participants. KK, MH and SK carried out statistical analyses. All authors contributed to the final form.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareALike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Kuriyama, K., Honma, M., Shimazaki, M. et al. An N-methyl-d-aspartate receptor agonist facilitates sleep-independent synaptic plasticity associated with working memory capacity enhancement. Sci Rep 1, 127 (2011). https://doi.org/10.1038/srep00127
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep00127
This article is cited by
-
Psychostimulants and atomoxetine alter the electrophysiological activity of prefrontal cortex neurons, interaction with catecholamine and glutamate NMDA receptors
Psychopharmacology (2015)
-
Investigating dynamic structural and mechanical changes of neuroblastoma cells associated with glutamate-mediated neurodegeneration
Scientific Reports (2014)
-
Sleep-Dependent Declarative Memory Consolidation—Unaffected after Blocking NMDA or AMPA Receptors but Enhanced by NMDA Coagonist D-Cycloserine
Neuropsychopharmacology (2013)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.