Key Points
-
Reviews the most common and serious medical conditions that are linked to erosive tooth wear.
-
Indicates that there is a clear benefit to patients from the dental team picking up on the early signs of these conditions, which may be very subtle and difficult to detect.
-
Suggests that the dental examination should include the possibility of detecting signs of GORD and eating disorders and if detected appropriate referral and liaison with medical professional instigated.
-
Discusses how such detection could protect the enamel from erosive wear and more importantly may even lead to saving the patient's life.
Abstract
There are many reasons why it is vital that dental professionals identify signs and symptoms that suggest that an individual's erosive tooth wear (ETW) may be linked to a broader medical problem than just poor diet. Primarily, spotting an underlying medical cause for ETW increases the likelihood that further deterioration in the individual's oral health will be prevented. However, perhaps more importantly, many of the medical conditions which are commonly related to ETW can have serious and even possibly fatal consequences if left untreated or not diagnosed. This paper reviews the nature of the most common and serious medical conditions related to ETW, such as gastro-oesophageal reflux disease (GORD), laryngo-pharyngeal reflux (LPR) and eating disorders. This article also covers the role of the dental team in the diagnoses, prevention and management of these conditions.
Similar content being viewed by others
Introduction
As a dental professional, there are many reasons why it is vital to pick up on signs and symptoms that suggest that an individual's erosive tooth wear (ETW) may be linked to a broader medical problem other than just poor diet. Primarily, spotting an underlying medical cause for ETW increases the likelihood that further deterioration in the individual's oral health will be prevented. However, perhaps more importantly, many of the medical conditions that are commonly related to ETW can have serious and even possibly fatal consequences if left untreated or not diagnosed: namely gastro-eosphageal reflux disease (due to its propensity to lead to premalignant changes in the oesophagus) and eating disorders (especially anorexia) which despite being uncommon, are the leading causes of mental health-related deaths, due to the effects of malnutrition and a result of suicide.
This paper will review the nature of the most common and serious medical conditions related to ETW and will discuss the role of the dental team in the diagnoses, prevention and management of these conditions.
Gastro-oesophageal reflux disease
Symptoms of gastro-oesophageal reflux disease (GORD) are very common and roughly 10% of the population seek medical help for the condition. The prevalence is probably much higher and it has been estimated that as many as 65% of the population suffer from the condition at some point in their lives.1 Gastro-oesophageal reflux (GOR) is a physiological phenomenon that occurs in the immediate period after eating (postprandial period). The bulk of the refluxate is cleared by peristalsis (coordinated contraction of oesophageal muscles) followed by neutralisation of any remaining acid by saliva. GORD is defined as 'a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications. It is normally classified as: two or more heartburn episodes per week and adversely affecting an individual's wellbeing.' This is often referred to as the 'Montreal definition of GORD'.2
The oesophagus is a hollow tube which controls the passage of food from the mouth to the stomach. At the lower end separating the oesophagus from the stomach is the lower oesophageal sphincter (LOS) and at the upper end is the upper oesophageal sphincter (UOS) separating the oesophagus from the mouth and pharynx/larynx. The LOS and UOS help stop regurgitated gastric contents into the oesophagus and the mouth and pulmonary system. The LOS allows some regurgitation of the gastric contents which is considered to be normal physiological GOR; however, transient relaxations of the sphincter, an incompetent sphincter or problems with the muscles of the oesophagus can result in GORD. In pathological GORD, the number of relaxations of the LOS and hence the number of times the refluxate enters the oesophagus is increased, and all the refluxate is not cleared from the oesophagus. In some instances the refluxate can travel further up past the UOS. This can result in pharyngeal/laryngeal symptoms as well as ETW of the teeth.3
Laryngo-pharyngeal reflux (LPR)
A related condition to GORD that may have more relevance to ETW is laryngo-pharyngeal reflux (LPR). The term is used for refluxate that travels above the UOS. While a small amount of acid above the LOS and into the oesophagus is within normal physiological limits as indicated above, no acid travelling above the UOS and into the pharyngeal/laryngeal areas is considered to be normal.4 LPR is of particular interest to the dental profession as any acid entering the mouth and resulting in ETW needs to have travelled passed the UOS. The presentation of LPR may be different to typical GORD and this should be considered in diagnosis of GORD/LPR-related ETW. Some individuals may suffer from LPR but have none of the typical GORD symptoms and diagnosis in this group of patients can be challenging (Table 1).5,6,7
Manifestations of GORD/LPR
Manifestations of GORD are many and can be classified into oesophageal (symptoms arising directly from the oesophagus) and extra-oesophageal (symptoms arising from structures other than the oesophagus (Table 2).7,8,9,10,11,12,13,14
Oesophageal manifestations
The most typical oesophageal symptoms of GORD are heartburn and regurgitation. Heartburn is defined as a burning/pain sensation along the length of the oesophagus that can be felt in the substernal area but can radiate upwards to the throat. Heartburn is very common and has been reported by 15–31% of the population at least once a month and 15% of those diagnosed with GORD on a daily basis.
Regurgitation is another commonly reported symptom which is defined as the movement of fluid into the pharynx/mouth. Regurgitation is different to vomiting in that it is an effortless and involuntary movement of gastric contents passed the UOS into the pharynx/mouth. The prevalence of regurgitation is slightly less that heartburn but still high in GORD patients. Other oesophageal manifestations include dysphagia (difficulty swallowing), belching and bloating. These symptoms are not as commonly reported.
Extra-oesophageal manifestations
The extra-oesophageal manifestations can be divided into various categories: cardiac, pulmonary, ear nose and throat (ENT) and oral
Non-cardiac chest pain (NCCP)
Non-cardiac chest pain (NCCP) is a symptom of GORD that can result in severe chest pain mimicking a heart problem and causing concern for the sufferer. The diagnosis can sometimes be challenging and cardiac assessments are sometimes carried out to exclude heart disease. This is a referred pain which occurs as a result of GORD.
Pulmonary manifestations
Pulmonary manifestations can result in a chronic cough or GOR- related asthma symptoms. Once the refluxate goes passed the UOS, it can enter the pulmonary system and result in aspiration and irritation of the pulmonary tissues. Pulmonary symptoms have been reported in some cases to be the only manifestations with none of the typical oesophageal symptoms being present.
Pharyngeal/laryngeal manifestations
Pharyngeal/laryngeal manifestations can present as chronic hoarseness, globus (feeling of a lump in the throat), pharyngitis, laryngitis and inflammation of the vocal cords.
Oral manifestations
Oral manifestations are present if acid enters the mouth and comes into contact with the teeth. ETW is a well-known manifestation of GORD and the prevalence of erosion in patients with GORD has been reported to be between 5 to 47%.14,15,16,17,18,19,20,21
Barrett's oesophagus and oesophageal adenocarcinoma
The oesophagus in health is lined by squamous epithelium. At the gastro-oesophageal junction this is replaced by columnar epithelium. A change in this normal epithelium within the oesophagus from squamous to columnar is referred to as Barrett's oesophagus (BO). This condition has been of great interest and is becoming increasingly so as it is premalignant, and can develop further into adenocarcinoma of the oesophagus in a small number of patients suffering with GORD. Although the condition affects older adults in the developed world, the incidence is increasing in patients less than 60 years of age. The true prevalence is unknown but it is estimated that 6% of patients with GORD symptoms have BO and the longer the symptoms have been present, the higher the risk. The severity of the symptoms is not necessarily indicative of a higher risk. Nocturnal reflux also seems to result in a higher risk. Assessment is by endoscopy and the condition is classified into long segment BO (greater than 3 cm) (LSBO) or short segment BO (less than 3 cm) (SSBO). LSBO has a greater risk of progressing to adenocarcinoma. Sufferers of BO have a 40-fold higher risk of developing oesophageal adenocarcinoma compared with the general population.22,23
Silent reflux
Presentation of GORD can be divided into three main categories: symptomatic (oesophageal mucosal breaks together with symptoms), non-erosive reflux disease (presence of symptoms but no oesophageal mucosal breaks), presence of oesophageal mucosal breaks but no symptoms (silent reflux). Patients suffering from silent reflux suffer from GORD but do not complain of any symptoms of GORD. Interestingly, ETW can be detected in some patients who suffer from silent reflux and can be the only sign of possible GORD.2,24
Traditional methods of diagnosis of GORD
The two main symptoms generally considered are heartburn and regurgitation. Traditionally GORD is treated by either taking over-the-counter medications, such as antacids, or, if more troublesome, in general practice by prescription medication.
In more severe cases and in those that do not respond to medications, an endoscopy is carried out that allows visual inspection of the oesophagus for oesophageal mucosal breaks, inflammation or ulceration, as well as changes in the oesophageal lining suggestive of Barrett's oesophagus. This is then followed by 24-hour ambulatory pH monitoring which has been the gold standard for diagnosis of GORD. The specificity and sensitivity of the 24-hour pH test is around 80% whereas for endoscopy it is much less.25
Recent developments in diagnosis of GORD/LPR
Wireless pH monitoring, where a capsule is placed at 5 cm above the LOS at the time of endoscopy, allows more reliable diagnosis as it is more comfortable, better tolerated by patients and allows pH measurements for periods up to 96 hours. One such system is called the Bravo capsule (Bravo, Given Imaging, Yoqeam, Israel), which uses radio-telemetric methods to detect acids.
The above methods are invasive. Ideally, non-invasive and simple methods of diagnosis would have many advantages. One such method being developed is by the use of biomarkers in saliva and sputum. One such biomarker is pepsin, a proteolytic enzyme that digests dietary proteins. Presence of pepsin in saliva and/or sputum could indicate the possibility of LPR. More work is needed to confirm the validation and accuracy of diagnosis by pepsin detection.6,26,27,28,29,30,31
Management of GORD
Traditional methods of management of GORD
Proton pump inhibitors (PPIs) are the first line of treatment of GORD symptoms and very effective in majority of patients. Other medications such as H2 receptor antagonists and over the counter antacids are also used in some cases. PPIs inhibit gastric reflux and hence improve reflux symptoms. Although very effective, there are side effects associated with their long-term use as well as a high cost to the NHS. Some of the reported side effects include gastrointestinal infections and hip fracture. There is also the problem of increased rebound gastric acid production which results in more severe symptoms once patients stop taking the medication and often results in them having to continue taking the medication. Anti-reflux surgery is also used in patients who do not respond to PPIs well or in patients who do not wish to take PPIs long term. Both methods are effective but there is of course some morbidity and in rare cases mortality associated with surgery.32,33,34
Non-pharmacological methods of management of GORD
Lifestyle modifications in mild cases or in conjunction with medication in more severe cases are effective and safe. They are generally more effective in the management of GORD and not so effective in LPR, which is more difficult to treat. The general advice given is also very useful for the dental team to provide to the patient and offers a non-invasive method of management for their symptoms. These include:
-
Eating smaller meals and avoiding eating large meals, in particular before sleeping
-
Decreasing alcohol consumption
-
Cessation of smoking
-
Reduction of weight
-
Management of stress.
Certain types of foods are also refluxogenic and should be limited, such as fatty foods, spicy foods, citrus fruit, coffee etc. Chewing gum has also been investigated as a useful method of control of symptoms and reduction of acid in the oesophagus. It is effective, harmless and beneficial in terms of oral health. Although some studies have investigated active ingredients in chewing gum to neutralise the acid, the main function of chewing gum is improvement in the salivary clearance and neutralisation. Chewing gum increases salivary flow rate and buffering capacity and increases the rate of swallowing. Clearance of acid from the oesophagus is via peristalsis and clearance of volume of the refluxate, which swallowing improves, followed by clearance and neutralisation by saliva.35
Differences in the presentation of GORD and LPR
Table 1 compares typical GORD with LRP. It is apparent that there are differences in the type of symptoms experienced, typical GORD showing the more typical oesophageal symptoms, such as heartburn and regurgitation; whereas with LPR the most commonly experienced symptoms are extra-oesophageal, such as hoarseness, a cough and globus. Pharyngeal pH measurement provides a more accurate diagnosis for LPR as the refluxate travels high up in the oesophagus and beyond the UOS. In terms of treatment, LPR is harder to treat successfully and a more aggressive treatment with PPIs is needed.
GORD/LPR and ETW
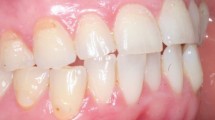
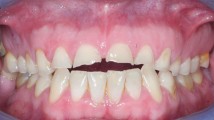
There is good evidence in the literature that GORD and ETW are related. Regurgitated or vomited stomach contents are highly acidic and repeated contact with the enamel and dentine results in ETW. The process is complicated and many factors influence the outcome. The duration of GORD; number and duration of episodes or reflux; whether the reflux happens during the day or at night (nocturnal reflux); how far up the refluxate travels and therefore how frequently it reaches the mouth; salivary flow rate and buffering capacity; and individual variations in saliva (and acquired enamel pellicle AEP); as well as management of the symptoms are all factors that influence the presence and severity of ETW. The most commonly affected surfaces of the teeth are the palatal surfaces of the upper anterior teeth and occlusal surfaces of molars (Figs 1 and 2), although this pattern can change depending on the direction of travel of the refluxate. As an example, in Figure 3 only one side is affected in a patient who had nocturnal reflux and had a habit of sleeping on the same side.18,36,37,38,39,40,41
The essential role of the dental team in diagnosis and management of GORD/LPR
The dental team have a fundamental role in diagnosis and management of GORD-related ETW. ETW in these patients is severe and there is often catastrophic destruction of many teeth. Management and treatment of the affected patients is complicated, prolonged and costly. Correct diagnosis, prevention and minimally invasive management at an early stage are fundamental to future success and providing patients with a good quality of life and maintenance of teeth for life. Once the diagnosis is confirmed control of acid reflux is the main approach to prevent further destruction of the teeth, together with strengthening and protection of the teeth. This can be achieved by various available fluoride-containing products, protection of the teeth with dentine bonding agents, fissure sealants or resin composite restorations. Often, in more complicated cases, there is a need for changes in the occlusion and the occlusal vertical dimension (OVD) and most of the teeth need to be restored. This is due to the dento-alveolar compensation associated with the wear process.42,43,44,45
The dental team, however, also has a fundamental role in detection and appropriate referrals so that a correct diagnosis can be made. As mentioned earlier, some patients who suffer with reflux disease do not have symptoms (silent refluxers) but they may suffer from ETW. The role of the dental team is not only to diagnose the ETW but also make appropriate referrals for possible diagnosis of GORD. Bearing in mind current methods of diagnosis and management of GORD, most of which are fairly invasive, and balancing that against conditions such as Barrett's oesophagus and oesophageal cancer, the decision to refer is not easy or straightforward.
Patients who clearly have symptoms of GORD/LPR and ETW should be informed about the condition and the need to see their general medical practitioner in the first instance. Those without any other symptoms other than ETW need to be managed and counselled more carefully to make the correct decision. A thorough history and examination taking all aetiological factors as well as a comprehensive history of all possible typical and atypical manifestations of GORD/LPR and ETW is essential. In future, more minimally invasive methods of diagnosis such as detection of biomarkers like pepsin and non-pharmacological management of GORD/LPR could improve the dilemma and decision making. There is no harm in providing the patients with preventive advice regarding ETW as well as possible GORD/LPR in terms of minimally invasive/non-pharmacological methods of management including the use of chewing gum in conjunction with close monitoring until such time that a referral may be appropriate.
Eating disorders
The dental team also have a fundamental role in the management of eating disorders. Firstly because of clear links between poor oral health (namely ETW) and eating disorders;46,47 also, secondly, because eating disorders are one of the leading causes of mental-health related deaths, whether due to the systemic effects of malnutrition or due to suicide.48 The dental team should be aware that the cardinal signs of an eating disorder are persistent abnormal behaviours designed to avoid food and food-related activities, resulting in impaired physical and psychosocial functions.49
The two eating disorders with the strongest links to poor oral health are anorexia nervosa and bulimia nervosa, these are closely related but distinct conditions, shown in Table 3. Individuals with anorexia relentlessly pursue 'thinness' and have a body weight which is lower than 85% of ideal body weight. In contrast, bulimia is characterised by binge eating episodes followed by behavioural responses aimed at avoiding body weight gain, such as purging and laxatives; however, body weight may be within or greater than normal limits.50
It has been estimated that in the UK, based on UK hospital admissions data from 2012 to 2013, there are currently over 725,000 people with an eating disorder in the UK, of whom approximately 90% are female.51 In addition the number of people being diagnosed and entering inpatient treatment for eating disorders in England alone has increased at an average rate of 7% year on year since 2009.51 This high prevalence and increasing incidence is even more worrying when one considers the average treatment and recovery cycle lasts 6 years at the end of which there is a 63% relapse rate, carrying a risk of fatal consequences to the individual and an overall cost to society of around £15 billion per annum.51 Therefore, as dentists our role of spotting the early subtle signs and making appropriate arrangements may be helpful in early identification which has a far better outlook for successful management.48
Anorexia nervosa
Patients suffering from this condition display an abnormal relationship with food which is driven by altered body image, despite being thin already. Anorexia has two clinical and overlapping subtypes: a restrictive type (that is, calorific intake restriction) and binge/purge type (that is, binge eating followed by purging aided by laxatives). The risk of developing any eating disorder is highest for young men and women between 13 and 17 years of age but females are diagnosed ten times more commonly than males.
The initial presentation is of gradual behavioural changes designed to limit high-calorie foods and later reliance on 'safe foods' without any calorific value. This manifests itself as missing meals or obsessively counting calories and the diagnosis of anorexia is made when less than 85% of target weight is reached. Depressive symptoms continue to perpetuate an altered body image distorting self-awareness despite obvious body changes to friends and family. Thus treatment of anorexia is multilevel and multidisciplinary, involving a combination of psychological therapy (such as tailored cognitive behavioural therapy) followed by supervised weight gain, mostly through outpatient care but compulsory in-patient care via sectioning may be required in extremis. Recently published NICE guidelines have clarified the optimal nature of the multidisciplinary care that may be required for individuals: most commonly a multi-disciplinary team provide a combination of outpatient hospital care, cognitive behavioural therapy, family therapy and, for the most severe cases, inpatient care which can be long term and compulsory depending on the level of severity.52
Bulimia nervosa
Bulimia nervosa involves cycles of binge eating an excessive amount of food followed by self-induced vomiting. The diagnosis is made when binge eating and vomiting occur more than twice a week for at least three months. The body weight for bulimics is generally within normal limits but if weight drops then anorexia becomes part of the condition. Reliable data for the prevalence of bulimia in the UK is difficult to find; however as with all eating disorders, women are much more likely to develop bulimia than men, although this is changing, with an increased incidence among men. The condition can occur at any age but on average, its onset is slightly later than anorexia, starting at around the age of 18 or 19.
Dental implications of eating disorders
The connection between poor oral health and eating disorders has been shown in several studies, with the key pathology being enamel damage from gastric juices entering the oral cavity leading to ETW; however, the lack of a healthy balanced diet can also lead to dental caries.53,54 Most commonly, the key presenting oral feature of an eating disorder is erosion of the palatal (lingual) surfaces of the maxillary anterior dentition.47
2017 NICE guidance on the recognition and treatment of eating disorders provides dentally focused recommendations for mitigating the impact of vomiting on oral health. Specifically, the guidance52 advised health professionals to encourage people with an eating disorder who are vomiting to:
-
Have regular dental and medical reviews
-
Avoid brushing teeth immediately after vomiting
-
Rinse with non-acid mouthwash after vomiting
-
Avoid highly acidic foods and drinks.
It is important to note that the NICE guidance also states that dietary counselling should only be offered as part of a multi-disciplinary approach; therefore, as dental professional it is probably most important to focus our advice regarding the timings of oral care routines (especially with regard to vomiting as stated above) and also to consider the role that normal salivary flow plays in protecting enamel from erosion. Rytömaa et al.55 reported decreased salivary flow rates in bulimics which was further corroborated by another study of 35 subjects with eating disorders which also reported decreased unstimulated salivary flow rate and reduced bicarbonate levels. Therefore, it is likely that the abnormal salivary protection may exacerbate the dental erosion but it is not easy to ameliorate this with clinically available methods despite the role of the saliva in erosion being an focus for ongoing research.18,37,56
Rumination
Rumination is a rare condition that can cause severe ETW, in a pattern of ETW presenting similarly to other eating disorders. Affected individuals consciously regurgitate ingested stomach contents and then swallow again. They repeatedly raise their intra-abdominal pressure after meals and regurgitation occurs when one of these compressions coincides with swallowing and the associated relaxation of the LOS. Rumination occurs commonly in people with learning difficulties but it can affect other members of the population as well.57 The pathophysiology of rumination is poorly understood and has been incompletely studied. It is generally considered to be a psychological disorder although it has also been suggested that patients might suffer from GORD. The pattern of dental erosion is similar to other intrinsic causes with the first signs developing on the palatal surfaces of the upper incisors.
Chronic alcoholism
Chronic alcoholism is a serious and complex condition with potentially life-threatening complications, and although difficult to precisely quantify the prevalence, up to 10% of the population are thought to drink over the recommended limits. Many alcoholics present with dental erosion related to regurgitated or refluxed stomach juice, although attrition due to bruxism has also been reported in alcoholics. Perhaps more significantly, alcohol increases the risk of oral cancer. The role of alcohol in ETW is two fold: primarily alcohol can result in gastritis and provoke gastroesophageal reflux, and secondly alcoholics are less likely to have a healthy balanced diet and tend to eat more acidic foods and drinks. In studies linking alcoholism to tooth wear, the palatal surfaces of the upper anterior teeth were the worst affected.46
Conclusions
This paper has reviewed the most common and serious medical conditions that are linked to erosive tooth wear. There is a clear benefit to patients from the dental team picking up on the early signs of these conditions, which may be very subtle and difficult to detect. The dental examination should include the possibility of detecting signs of GORD and eating disorders and if detected appropriate referral and liaison with medical professional instigated. This will have benefits in protecting the enamel from erosive wear and more importantly may even lead to saving the patient's life.
References
Dent J, El-Serag H, Wallander M A, Johansson S . Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 2005; 54: 710–717.
Vakil N, Van Zanten S, Kahrilas P, Dent J, Jones R . The Montreal definition and classification of gastroesophageal reflux disease: a global, evidence-based consensus paper. Z Gastroenterol 2007; 45: 1125–1140.
Meyer G, Austin R, Brady III C, Castell D . Muscle anatomy of the human esophagus. J Clin Gastroenterol 1986; 8: 131–134.
Demeester T R, Johnson L F, Joseph G J, Toscano M S, Hall A W, Skinner D B . Patterns of gastroesophageal reflux in health and disease. Annals of surgery. 1976; 184: 459.
Koufman J A, Aviv J E, Casiano R R, Shaw G Y . Laryngopharyngeal reflux: position statement of the committee on speech, voice, and swallowing disorders of the American Academy of Otolaryngology-Head and Neck Surgery. Otolaryngol Head Neck Surg 2002; 127: 32–35.
Koufman J A . Laryngopharyngeal reflux is different from classic gastroesophageal reflux disease. Ear Nose Throat J 2002; 81: 7.
Chandra A, Moazzez R, Bartlett D, Anggiansah A, Owen W . A review of the atypical manifestations of gastroesophageal reflux disease. Int J Clin Pract 2004; 58: 41–48.
Bennett J . Heartburn and gastro-oesophageal reflux. Br J Clin Pract 1990; 45: 273–277.
Irwin R S, French C L, Curley F J, Zawacki J K, Bennett F M . Chronic cough due to gastroesophageal reflux: clinical, diagnostic, and pathogenetic aspects. Chest 1993; 104: 1511–1517.
Chernow B, Johnson L F, Janowitz W R, Castell D O . Pulmonary aspiration as a consequence of gastroesophageal reflux. Dig Dis Sci 1979; 24: 839–844.
Irwin R S, Madison J M . Anatomical diagnostic protocol in evaluating chronic cough with specific reference to gastroesophageal reflux disease. Am J Med 2000; 108: 126–130.
Field S K . Gastroesophageal reflux and respiratory symptoms. Chest 1999; 116: 843.
Smit C F, van Leeuwen J A, Mathus-Vliegen L M et al. Gastropharyngeal and gastroesophageal reflux in globus and hoarseness. Arch Otolaryngol Head Neck Surg 2000; 126: 827–830.
Bartlett D, Evans D, Smith B . The relationship between gastro-oesophageal reflux disease and dental erosion. J Oral Rehabil 1996; 23: 289–297.
Meurman J H, Toskala J, Nuutinen P, Klemetti E . Oral and dental manifestations in gastroesophageal reflux disease. Oral Surg Oral Med Oral Pathol 1994; 78: 583–589.
Gudmundsson K, Kristleifsson G, Theodors A, Holbrook W P . Tooth erosion, gastroesophageal reflux, and salivary buffer capacity. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol 1995; 79: 185–189 Z.
Bartlett D, Evans D, Anggiansah A, Smith B . A study of the association between gastro-oesophageal reflux and palatal dental erosion. Br Dent J 1996; 181: 125–131.
Moazzez R, Bartlett D, Anggiansah A . Dental erosion, gastro-oesophageal reflux disease and saliva: how are they related? J Dent 2004; 32: 489–494.
Schroeder P L, Filler S J, Ramirez B, Lazarchik D A, Vaezi M F, Richter J E . Dental erosion and acid reflux disease. Ann Intern Med 1995; 122: 809–815.
O'Sullivan E A, Curzon M E, Roberts G J, Milla P J, Stringer M D . Gastroesophageal reflux in children and its relationship to erosion of primary and permanent teeth. Eur J Oral Sci 1998; 106: 765–769.
Gregory-Head B, Curtis D A . Erosion caused by gastroesophageal reflux: diagnostic considerations. J Prosthodont 1997; 6: 278–285.
Barrett N . Chronic peptic ulcer of the œophagus and œsophagitis. Br J Surg 1950; 38: 175–182.
Naini B V, Souza R F, Odze R D . Barrett's esophagus: a comprehensive and contemporary review for pathologists. Am J Surg Pathol 2016; 40: e45–e66.
Choi J Y, Jung H-K, Song E M, Shim K-N, Jung S-A . Determinants of symptoms in gastroesophageal reflux disease: nonerosive reflux disease, symptomatic, and silent erosive reflux disease. Eur J Gastroenterol Hepatol 2013; 25: 764–771.
Klauser A G, Heinrich C, Schindlbeck N E, Müller-Lissner S A . Is long-term esophageal pH monitoring of clinical value? Am J Gastroenterol 1989; 84: 362–366.
Blondeau K, Tack J . Usefulness of impedance testing in the management of GERD. Am J Gastroenterol 2009; 104: 2664–2666.
Sweis R, Fox M, Anggiansah A, Wong T . Prolonged, wireless pH-studies have a high diagnostic yield in patients with reflux symptoms and negative 24-h catheter-based pH-studies. Neurogastroenterol Motil 2011; 23: 419–426.
Dent J, Vakil N, Jones R, Bytzer P et al. Accuracy of the diagnosis of GORD by questionnaire, physicians and a trial of proton pump inhibitor treatment: the Diamond Study. Gut 2010; 59: 714–721.
Bardhan K D, Strugala V, Dettmar P W . Reflux revisited: advancing the role of pepsin. Int J Otolaryngol 2011; 646901.
Reulbach T R, Belafsky P C, Blalock P D, Koufman J A, Postma G N . Occult laryngeal pathology in a community-based cohort. Otolaryngol Head Neck Surg 2001; 124: 448–450.
Marshall R E, Anggiansah A, Owen W A, Manifold D K, Owen W J . The extent of duodenogastric reflux in gastro-oesophageal reflux disease. Eur J Gastroenterol Hepatol 2001; 13: 5–10.
Chapman D B, Rees C J, Lippert D, Sataloff R T, Wright S C . Adverse effects of long-term proton pump inhibitor use: a review for the otolaryngologist. J Voice 2011; 25: 236–240.
Dunbar K B, Agoston A T, Odze R D et al. Association of acute gastroesophageal reflux disease with esophageal histologic changes. JAMA 2016; 315: 2104–2112.
Lazarus B, Chen Y, Wilson F P et al. Proton pump inhibitor use and the risk of chronic kidney disease. JAMA Intern Med 2016; 176: 238–246.
Moazzez R, Bartlett D, Anggiansah A . The effect of chewing sugar-free gum on gastro-esophageal reflux. J Dent Res 2005; 84: 1062–1065.
Smoak B R, Koufman J A . Effects of gum chewing on pharyngeal and esophageal pH. Ann Otol Rhinol Laryngol 2001; 110: 1117–1119.
Carpenter G, Cotroneo E, Moazzez R et al. Composition of enamel pellicle from dental erosion patients. Caries Res 2014; 48: 361–367.
Wang G-R, Zhang H, Wang Z-G, Jiang G-S, Guo C-H . Relationship between dental erosion and respiratory symptoms in patients with gastro-oesophageal reflux disease. J Dent 2010; 38: 892–898.
Gregory-Head B L, Curtis D A, Kim L, Cello J . Evaluation of dental erosion in patients with gastroesophageal reflux disease. J Prosthetic Dent 2000; 83: 675–680.
Bartlett D, Evans D, Anggiansah A, Smith B . The role of the esophagus in dental erosion. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol 2000; 89: 312–315.
Marsicano J A, de Moura-Grec P G, Bonato R C, de Carvalho Sales-Peres M, Sales-Peres A, de Carvalho Sales-Peres S H . Gastroesophageal reflux, dental erosion, and halitosis in epidemiological surveys: a systematic review. Eur J Gastroenterol Hepatol 2013; 25: 135–141.
O'Toole S, Bartlett D, Moazzez R . Efficacy of sodium and stannous fluoride mouthrinses when used before single and multiple erosive challenges. Aus Dent J 2016; 61: 497–501.
O'Toole S, Mistry M, Mutahar M, Moazzez R, Bartlett D . Sequence of stannous and sodium fluoride solutions to prevent enamel erosion. J Dent 2015; 43: 1498–1503.
Dahl B L, Krogstad O, Karlsen K . An alternative treatment in cases with advanced localized attrition. J Oral Rehabil 1975; 2: 209–214.
Dahl B, Krogstad O . Long-term observations of an increased occlusal face height obtained by a combined orthodontic/prosthetic approach. J Oral Rehabil 1985; 12: 173–176.
Robb N, Smith B, Geidrys-Leeper E . The distribution of erosion in the dentitions of patients with eating disorders. Br Dent J 1995; 178: 171–175.
Milosevic A . Tooth surface loss: Eating disorders and the dentist. Br Dent J 1999; 186: 109–113.
Williamson D A, Martin C K, Stewart T . Psychological aspects of eating disorders. Best Pract Res Clin Gastroenterol 2004; 18: 1073–1088.
UK Government. Eating disorders: Types, causes, who's affected, treatment. NHS Choices Your health, your choices. Available online at http://www.nhs.uk/conditions/eating-disorders/pages/introduction.aspx (accessed Feb 2018).
Russell G . Bulimia nervosa: an ominous variant of anorexia nervosa. Psychol Med 1979; 9: 429–448.
PricewaterhouseCoopers. The costs of eating disorders: Social, health and economic impacts. Assessing the impact of eating disorders across the UK on behalf of BEAT. PricewaterhouseCoopers LLP, 2015.
National Institute for Health and Care Excellence. Eating disorders: recognition and treatment (NG69). 2017.
Scheutzel P . Etiology of dental erosion – intrinsic factors. Eur J Oral Sci 1996; 104: 178–190.
Hellström I . Oral complications in anorexia nervosa. Eur J Oral Sci 1977; 85: 71–86.
Rytomaa I, Jarvinen V, Kanerva R, Heinonen O P . Bulimia and tooth erosion. Acta Odontol Scand 1998; 56: 36–40.
Moazzez R V, Austin R S, Rojas-Serrano M et al. Comparison of the possible protective effect of the salivary pellicle of individuals with and without erosion. Caries Res 2014; 48: 57–62.
Gilmour A, Beckett H . The voluntary reflux phenomenon. Br Dent J 1993; 175: 368–372.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moazzez, R., Austin, R. Medical conditions and erosive tooth wear. Br Dent J 224, 326–332 (2018). https://doi.org/10.1038/sj.bdj.2018.166
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2018.166
This article is cited by
-
High serum ferritin levels are associated with a reduced periodontium in women with anorexia nervosa
Eating and Weight Disorders - Studies on Anorexia, Bulimia and Obesity (2020)
-
Effect of sucralfate against hydrochloric acid-induced dental erosion
Clinical Oral Investigations (2019)