Key Points
-
Identifies the commonest reasons for referral to a dental maxillofacial radiologist.
-
Reviews the commonest diagnoses made by the dental maxillofacial radiologist.
-
Evaluates the service, highlighting the demand for a referral service.
Abstract
The aim of this study was to determine the common reasons why a dental professional might request a second opinion on a dental radiograph from a Dental and Maxillofacial (DMF) radiologist. The study was a retrospective analysis of consecutive referrals for an opinion received by post or email by one DMF radiologist based in a UK dental hospital. The study period was from March 2009 to November 2015. Referrals came from a mixture of sources: mainly from general dental practitioners and specialists working in primary care, but with some referrals from hospital-based practitioners. An enormous range in diagnoses were made by the DMF radiologist, but the ten most frequent diagnostic categories contributed 57.5% of the total. Normal anatomy and anatomical variations in normal anatomy made up the largest category. Common dental disease was often diagnosed, but idiopathic osteosclerosis and maxillary antrum pathosis were both frequent reasons for seeking a second opinion. This service evaluation may assist in developing curricula for undergraduates and in designing continuing education courses. It also highlights a service that may avoid unnecessary referrals to hospital specialists but which currently is not commissioned by the NHS.
Similar content being viewed by others
Introduction
Radiography is one of the commonest special tests a general dental practitioner (GDP) can perform, with over 11 million dental x-ray examinations conducted in 2008/2009 in the UK.1 Compared to their medical colleagues, GDPs are required not only to justify the need for a particular type of radiograph but also to report on the images obtained. Although radiological interpretation is part of the undergraduate dental curriculum and, more recently, of the training given to hygienists and therapists, referrals are sometimes made by dental professionals to Dental and Maxillofacial (DMF) radiologists requesting a second opinion.
DMF radiology is a speciality recognised by the GDC with only 27 registrants on the specialists list.2 There is no current literature from the UK examining the reasons why dental professionals may refer for a second radiological opinion. One study, carried out in Canada, reviewed 430 referrals made to two DMF radiologists over a three-year period and found that approximately one quarter of referrals related to interpretation of variations in normal anatomy.3 This was followed in frequency by 'bone dysplasias', cysts and inflammatory diseases. Dental education and clinical practice in the UK, however, is likely to have some differences to the Canadian situation. Knowledge about the needs of UK dental professionals for specialist DMF radiological opinions could help with design of continuing professional development (CPD) courses and tailor the undergraduate curriculum which, in turn, have the potential to reduce future referrals and lessen the financial implications of this service to the National Health Service (NHS).
Consequently, the aim of this service evaluation was to determine the common reasons for a dental professional to request a second opinion on a dental radiograph from a DMF radiologist.
Materials and methods
This study was a retrospective analysis of consecutive referrals for radiological opinion, by letter or email, made to a registered specialist in DMF Radiology, who is a clinical academic (Honorary Consultant) at a UK dental hospital. Data were collected in reverse order of date of referral, starting at 6 November 2015 and ending at 17 March 2009. The end date was selected on the basis that records of referrals were not always available before that date and consecutive data collection thus became impossible.
Exclusion criteria for referrals included medico-legal work, non-patient radiological queries (principally about aspects of radiation protection or image quality) and overseas requests.
For each referral, one of the authors (MD) reviewed the referrer's communication and the reply made by the DMF radiologist. In the case of referrals by email, images were also available for review as attachments or embedded within the email body. For referrals by letter, images were not available for review as film radiographs or digital images on recordable media had been returned to the referrer at the time of providing the opinion.
The origin of the referral (general dental practice, specialist dental practice or hospital specialist) was recorded. The type of radiograph provided by the referrer and the diagnosis made by the DMF radiologist was also recorded. The additional parameters recorded included substandard quality of the radiograph supplied by the referrer and requests for a cone beam computed tomography (CBCT) scan that were judged not to be inconsistent with accepted referral criteria. Also recorded were recommendations made in the response by the DMF radiologist to undertake additional imaging (dental radiograph, CBCT) or referral to a specialist colleague for a second clinical opinion.
All data were collated on a Microsoft Excel worksheet. No data identifying either the patient or the referrer were recorded. Data analysis was limited to descriptive statistics.
As this study was classified as a service evaluation using the Health Research Authority Decision Tool (http://www.hra-decisiontools.org.uk/research/), it was judged not to require NHS ethical approval. This was confirmed by the Research Office of Central Manchester University Hospitals NHS Foundation Trust.
Results
In total, 871 separate requests for radiological opinions were collected, 713 of which had been made by post and the remaining 158 by email. The majority of these had originated from GDPs (n = 600; 68.9%). Referrals also originated from a wide range of other practitioners, with specialists in oral surgery or oral and maxillofacial surgery (n = 107; 12.3%) and orthodontists (n = 106; 12.2%) forming two substantial groups, followed by specialists in restorative dentistry or one of its sub-specialisms (n = 19; 2.2%) and community dental officers (n = 16; 1.8%). The remainder (n = 23; 2.6%) was made up of small numbers of other specialist and non-specialist groups.
The 871 referrals included 967 radiographs, of which periapical radiographs were the most common (49.6%), followed by dental panoramic radiographs (33.6%) and bitewing radiographs (6.9%). The remainder (9.9%) was made up of occlusal radiographs, images from cone beam CT and multislice CT scans, sialography and Magnetic Resonance Images. The more advanced imaging modalities came principally from oral surgeons and oral and maxillofacial surgeons.
Substandard image quality of at least one image for each case was reported in replies to 58 referrals (6.7%). In terms of advice on further imaging given to the referrer, a further radiograph was proposed by the DMF radiologist for 133 cases (15.3%) and a CBCT examination for 90 cases (10.3%). Within the 871 referrals there were 32 cases (3.7%) in which the request for a radiological opinion had included a request for a CBCT examination that was judged to be unnecessary by the DMF radiologist after viewing the radiograph(s). Onward referral to a specialist clinical colleague for management was advised by the DMF radiologist for 84 cases (9.6%).
The replies of the DMF radiologist to the referrers often included more than one diagnosis. Of the 871 referrals, 1,428 diagnoses were made, grouped into 112 separate categories. Of these, the ten most common diagnoses made up 57.5% of the total. This 'top ten' is shown in Table 1, of which the most frequent was 'normal anatomy or anatomical variations'. This encompassed a range of conditions (Table 2), but normal variation in trabecular bone pattern/large marrow space contributed more than a quarter of these (27.3%). If any diagnostic sub-category within 'normal anatomy or anatomical variations' occurred on fewer than five occasions, it was classified as 'other'. The 'other' category made up 25.3% of the total in this category and included the anterior nasal spine, the hyoid bone, anomalous pulp morphology, the inferior nasal concha and inferior alveolar canal variation, among others.
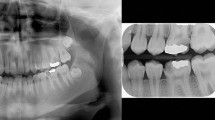
Figures 1,2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19 give examples of some radiographs for which an opinion was sought by referrers.
The referring dentist wanted to know whether the area of relative radiolucency periapical to 45, 46 and 47 region was cystic in nature. Note the lamina dura of the root apices are still identifiable on the associated teeth. Note also the multiple artefacts on the image from damage to the phosphor plate
The orthodontist noted a well-defined radiolucency with a lack of cortication at the right angle of the mandible. She felt that this was probably an air shadow but, as it was not symmetrical with the contralateral side, reassurance was sought. The air lies between the posterior aspect of the tongue and the soft palate
The dentist requested an opinion on the radiolucent area above and mesial to the tooth. The area of radiolucency is due to air in the right nostril, although the nasopalatine foramen contributes the ovoid radiolucency between the central incisor roots. Note the presence of a normal lamina dura around 11 where it overlies the radiolucency. Sclerosis of the pulp chamber and root canal in 11 has also occurred
The dentist asked whether the radiolucency over the upper premolars could be cystic, or whether it was a part of the antrum. The floor of the maxillary antrum forms the inferior edge of the radiolucency, but it continues distally across the roots of 25 and the molars. The distal aspect of the radiolucent area is formed by a septum in the antrum
The dentist was concerned about the radiolucency of the mandible below the roots of the molar tooth. The radiopaque line running obliquely across the radiograph close to 48 root apices is the mylohyoid ridge on the lingual aspect of the mandible. Beneath this line is the submandibular fossa. Note also the periapical inflammatory lesion on 48 distal root
The dentist recognised the foramen but requested an opinion because of drift the front teeth with development of a more prominent central diastema, but with no other clinical signs or symptoms. The report from the radiologist was that the foramen was within normal limits of size and that there was no radiologically apparent explanation for the drift of teeth
Discussion
This retrospective review of requests for second opinions on radiographs was limited to those received by one consultant DMF radiologist in one hospital, so gives a limited snapshot of what may be happening on a larger scale nationally. Nonetheless, referrals were received from over a wide part of the North West of England and sometimes from further afield. We did not attempt to identify any aspect of the referrers' training, such as dental school of qualification or continuing education, as this was not the focus of the service evaluation, but it would be of interest to try to relate aspects of education with the need for radiological opinions or particular diagnostic challenges.
One study is available against which ours can be compared, from Ontario in Canada.3 They found that referrers were predominantly GDPs, followed by oral surgeons and orthodontists, a pattern which was broadly the same in our study. We found fewer oral surgeons (12.3%), however, in our study than the 21.5% reported in the Canadian sample. This probably reflects the greater proportion of Canadian oral surgeons who are based in primary care, without easy access to a clinical radiologist's opinion, than is the case in the UK.4 In the Canadian study, panoramic radiographs were submitted alone or in combination with intraoral or other types of radiographs in 79.5% of cases. This proportion of panoramic radiographs is much greater than that seen in our study. Logically, it might be anticipated that there would be more requests for an opinion on panoramic radiographs than intraoral images because of the larger anatomical coverage. The reason why this was not the case in our study may be explicable by the relatively high frequency of use of panoramic radiographs in Canada compared with the UK. There is no accurate data on the number of dental practices, or dentists, with access to panoramic radiography equipment in either the UK or Ontario in Canada, but among dental practices using the services of Public Health England Dental X-ray Protection Service, about one third have their own panoramic equipment,5 while the figure is likely to be much higher than this in Ontario.4
Replies to referrers written by the DMF radiologist made a point of commenting on limitations in image quality in 6.7% of cases. This is likely to be an underestimate of the real frequency of poor image quality because a comment would only be made if artefacts or distortion significantly affected the confidence of the DMF radiologist in diagnosis. The frequency of faults on dental radiographs has been noted previously on several occasions.6,7 Although a switch to digital radiography has eliminated chemical processing errors, it does not eliminate errors in technique. Furthermore, with phosphor plate systems, damage to the plate surface inevitably occurs with use and several images in the study had severe artefacts of this kind (Figs 1, 13 and 15).
In a small proportion of referrals, where the dentist had included a request to perform a CBCT scan if needed, the request was judged to be unnecessary after the DMF radiologist had viewed the radiographs. Due to the higher radiation doses and financial costs, a basic principle of using CBCT is that it should be reserved for cases where conventional radiography is unable to provide the information required for diagnosis or treatment.8 Although it would be wrong to draw any solid conclusion regarding this finding, the result of the survey raises a possibility that without an opinion from a radiologist, unnecessary CBCT scans might be performed. There is a need for research to examine the criteria used by dentists when judging the need to perform CBCT examinations.
Our study revealed that a very wide range of diagnoses had been made for the referred cases, including cases with more than one diagnosis, for example, external root resorption in conjunction with chronic periapical periodontitis. It is notable that anatomy and anatomical variations were a particularly common diagnosis and, within this category, trabecular bone pattern variation or a large marrow space was the most frequent finding leading to a referral to the DMF radiologist. There is normal variation in the trabecular bone pattern in the jaws, both between and within individuals.9,10 The body of the mandible in particular, however, can contain large areas free of trabecular bone which in young people may contain bone marrow, although the radiological appearance will persist into adulthood.10 The term 'focal osteoporotic marrow defect' is sometimes used in textbooks.10 Osteoporosis is also associated with areas of sparse trabeculation in any area of the jaws.11 The way to distinguish between a marrow cavity and a large but asymptomatic pathological area is based upon the margins and the effects on adjacent structures. The commoner radiolucent pathoses in the jaws (chronic periapical inflammatory lesions and cysts) will tend to have well-defined and often corticated margins, although there are exceptions. With an area of sparse trabeculation that is normal variation, there are no effects on adjacent teeth or their lamina dura,10 nor on anatomical structures such as the inferior dental canal, inferior mandibular cortex or the maxillary antral floor. Figures 1 and 2 show examples of cases from the current study.
There were numerous other different diagnoses classified as variation in normal anatomy. This emphasises that normal radiological anatomy and the more common variations are important aspects of education for dentists. Examples of common causes of diagnostic uncertainty among referrers in this category are shown in Figures 3,4,5,6,7,8. Air in the mouth, nose, maxillary antra and pharynx may all be interpreted as potentially pathological findings. Some examples from the study are shown in Figures 3 to 5. This can be a particular problem on panoramic radiographs, where the lengthy exposure time can include movement of soft tissues of the palate and tongue that lead to asymmetry of the air shadows.10
Table 2 also includes the maxillary antrum. This may cause diagnostic uncertainty when its appearance is atypical, particularly at the floor of the antral cavity when there are loculations due to the presence of septa (Fig. 6). Maxillary antrum size is variable, with hypoplasia and hyperplasia both occurring.10 With the latter, pneumatisation of the alveolar bone is often seen and can cause diagnostic challenges (Fig. 7). Superimposition of the external (soft tissue) nose on intraoral radiographs of the maxillary incisors was recorded several times in this study (Fig. 8), often in the context of dental trauma and concern about possible root fracture. This phenomenon is only likely to occur with downward angled bisecting angle technique periapical radiographs and occlusal radiographs. The submandibular fossa was also recorded as a reason for dentists' referrals in the study. This is the anatomical depression on the lingual aspect of the body of the mandible below the molar regions. It is bounded superiorly by the mylohyoid line (or ridge) where the muscle of that name attaches to the mandible. The medio-lateral width of the mandible below this point is less than above it, so the mandible appears relatively radiolucent (Fig. 9). This radiolucency may be augmented by the frequent finding of sparse trabeculation/large marrow space in this region.
Examples of radiographs sent in for an opinion related to the nasopalatine foramen and the zygomatic process of the maxilla are shown in Figures 10 and 11, respectively.
Perhaps surprisingly, dental caries, periodontal bone loss and periapical inflammatory pathosis were relatively frequent diagnoses made relating to queries from the referring dentist. The reason was often equivocal imaging information, with an example being differentiation of distal caries on a lower second molar from cervical burnout. Another situation which occurred on several occasions was a request to report the caries on bitewing radiographs. Despite this being an everyday diagnostic task for a GDP, the implicit reason appeared to be a need for back-up in cases of an unexpected appearance of multiple new caries lesions in children or adolescents and where the GDP was preparing to inform the patient or parent about the need for a large number of restorations. In such situations the referring dentist was not demonstrating incompetence in radiological interpretation, but a need for reassurance and support.
One radiological abnormality which was regularly referred for diagnosis was idiopathic osteosclerosis, synonymous with enostosis or dense bone island, an entity that has been well-described by White & Pharoah.10 This was one of the most common diagnoses, in particular from referrals by orthodontists and oral surgeons as a chance incidental finding (Figs 12,13,14). There are no clinical signs or symptoms. Radiologically, it presents as a well-defined, localised, radiopacity, with either an irregular or sometimes a rounded radiopacity, often close to or in contact with the roots of teeth. There is no bony expansion or displacement of structures. In terms of differential diagnosis, there should be no peripheral radiolucency, such as might be seen with retained roots or odontomes. It is most commonly found in the mandibular molar and premolar regions, with a greater frequency in the mandible than the maxilla. The population prevalence is reported at a range from 2.3-9.7% in different ethnicities.12,13 Histologically, idiopathic osteosclerosis is an island of cortical bone in an area normally occupied by trabecular bone. No treatment or intervention is required. When closely related to teeth, the periodontal ligament space and lamina dura normally remain intact. In some cases, however, idiopathic osteosclerosis is associated with external root resorption of the associated tooth (Fig. 13).10 'Bony sclerosis' (Table 1) might have been combined with the idiopathic osteosclerosis category, but was characterised by a more diffuse or generalised increase in radiopacity with no apparent cause other than normal variation in trabecular pattern. Sclerosing osteitis (Fig. 15) due to chronic dental inflammation (periapical or periodontal) was included in the chronic periapical periodontitis category (Table 1).
Resorption of teeth was a diagnosis for a significant number of referrals. This included cases of internal resorption, inflammatory external resorption and replacement external resorption. In many cases in the study, referrers suggested the diagnosis and were only asking for confirmation of this. Root resorption has been thoroughly reviewed by Darcey and Qualtrough,14 but one aspect of resorption which is less well recognised is when it affects the crowns of unerupted teeth (Fig. 16). Patchy resorption of unerupted teeth is usually seen in older patients and it is the authors' impression that this is sometimes associated with atrophy of the pericoronal follicle. It seems to be age-related change rather than pathological in nature and, in the absence of any other pathosis, it does not require any treatment.
Inflammatory mucosal thickening and mucosal retention cysts of the maxillary antral lining made up 7.1% of the 'top ten' diagnoses (Table 1). Inflammatory mucosal thickening is an extremely common finding on asymptomatic patients, although it may not be visible on radiographs when present. Nonetheless, it can often be recognised on intraoral and panoramic radiographs as a band of radiopacity between the lamina dura of the floor of the maxillary antrum and the radiolucent air within it (Fig. 17).10 There are no immediate management implications if this finding is recognised, especially if the patient is asymptomatic. If the patient has symptoms of chronic sinusitis, then advice to see their general medical practitioner is appropriate.
Occasionally, however, inflammatory mucosal thickening arises on the sinus floor above teeth with periodontal disease or a tooth with periapical inflammatory pathosis. It is impossible to know in any specific case whether the dental pathosis causes the changes in the maxillary antrum or whether the findings are purely coincidental, but there is a clear association.15
Mucosal (or mucous) retention cysts, also known as 'retention pseudocysts', appear to be formed by blockage of secretory ducts of seromucous glands in the sinus mucosa, although other aetiologies have been suggested.9,10 Their characteristic radiographic appearance is of a well-defined, dome-shaped radiopacity, most commonly originating from the floor and extending towards the roof of the maxillary sinus, with usually no alteration of the antral outline (Fig. 18).9 It is the most common lesion in the maxillary sinus with its development probably associated with allergies, infection, trauma and humidity.10 No intervention is necessary and patients should be reviewed, with symptomatic treatment of sinusitis if required. According to White and Pharoah,10 the mucous retention cyst has no relationship with periapical dental disease. From the GDP's perspective, however, it is important to differentiate the mucous retention cyst from a radicular cyst (or other benign odontogenic lesion), growing from the maxillary alveolus into the maxillary antrum. In such cases, the bony floor of the maxillary antrum will be raised up to form a radiopaque margin to the mass (Fig. 19).
The study revealed a steady demand for this service, with evidence of an increase over the timescale of the study. The availability of DMF radiologists to provide such a service is not widely advertised, not least because of the uncertain workload implications and the impact on costs for the employing NHS Trusts. It should be noted that some dentists made repeated referrals for opinion, suggesting that once such a service was known to exist, the demand grew. In the past, opinions on radiographs have been provided as a courtesy to professional colleagues, with no charge made, but in the present climate of financial restraint in the NHS, this situation is unlikely to continue. Currently, NHS Commissioners do not contract with NHS Trusts for this service and consultants do not have allocated time in their job plans to deliver it. NHS Trust management may see a radiology reporting service for primary care practitioners as subsidising another organisation, certainly where the patient is being treated privately by the dentist, and charges may begin to be made. In our centre, a charge is now levied on referrers for reporting of radiographs and no service is offered for reporting of cone beam CT scans because of the much greater time commitment required and the difficulties in coping with multiple different types of viewing software.
On the other hand, for many of the cases included in this review, for example, in the context of interpretation of normal anatomical features, it was evident that the provision of a quick opinion on a radiograph from a specialist DMF radiologist avoided some patients being inappropriately referred to a hospital and the ensuing costs to the NHS and the patient. The DMF radiologist recommended only a small proportion of the cases (9.6%) in this review for referral to a specialist colleague, raising the possibility that unnecessary referrals may have been avoided. The cost benefits of a DMF radiologist service for dentists are unknown and would be worth further investigation. It remains to be seen whether NHS dental commissioners recognise a need for a second opinion reporting service when planning the commissioning of specialist services in dental and maxillofacial radiology. It must also be noted that with so few DMF radiology specialists in the UK, there may be limitations on what service could be delivered in practice.
Although a specialist second opinion service is one approach to improving the service to patients, improved education of clinicians is another option. The results of this study highlight some particular diagnostic challenges that warrant greater attention in curricula for undergraduate education and in continuing professional development. It should be remembered that 'Radiography and Radiation Protection' is highly recommended by the General Dental Council as part of verifiable CPD; although this is often assumed erroneously to be limited to safety aspects of X-ray use, radiological interpretation also comes under this umbrella and this service evaluation provides some evidence for topics to be included.
References
Hart D, Wall B F, Hillier M C, Shrimpton P C . Frequency and collective dose for medical and dental Xray examinations in the UK, 2008. Didcot: Health Protection Agency, 2010, HSECRCE012.
General Dental Council. Search the Registers. Available at: http://www.gdc-uk.org/Pages/SearchRegisters.aspx (accessed 9 September 2016).
Perschbacher S E, Pharoah M J, Leake J L, Lam E W, Lee L . A retrospective analysis of referral patterns for oral radiologic consultation over three years in Ontario, Canada. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010; 109: e86–91.
Personal communication. Susanne E. Perschbacher, Department of Oral Radiology, Faculty of Dentistry, University of Toronto, Toronto, O N, Canada. 23 August 2013.
Personal communication. John Holroyd, Dental X-ray Protection Services, Public Health England, Cookridge, Leeds, West Yorkshire, LS16 6RW, UK. 30 August 2016.
Chong B S, Miller J, Sidhu S . The quality of radiographs accompanying endodontic referrals to a health authority clinic. Br Dent J 2015; 219: 69–72.
Rushton V E, Horner K, Worthington H V . The quality of panoramic radiographs in a sample of general dental practices. Br Dent J 1999; 186: 630–633.
European Commission. Radiation Protection 172. Evidence Based Guidelines on Cone Beam CT for Dental and Maxillofacial Radiology. Luxembourg: Office for Official Publications of the European Communities, 2012. Available at: https://ec.europa.eu/energy/sites/ener/files/documents/172.pdf (accessed 9 September 2016).
Whaites E, Drage N . Essentials of radiography and radiology. 5th ed. Edinburgh: Churchill Livingstone Elsevier, 2013.
White S C, Pharoah M J . Oral radiology. Principles and interpretation. 7th ed. St. Louis: Elsevier, 2014.
Lindh C, Horner K, Jonasson G et al. The use of visual assessment of dental radiographs for identifying women at risk of having osteoporosis: the OSTEODENT project. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2008; 106: 285–293.
Halse A, Molven O . Idiopathic osteosclerosis of the jaws followed through a period of 20–27 years. Int Endod J 2002; 35: 747–751.
MacDonald-Jankowski D S . Idiopathic osteosclerosis in the jaws of Britons and of the Hong Kong Chinese: radiology and systematic review. Dentomaxillofac Radiol 1999; 28: 357–363.
Darcey J, Qualtrough A . Resorption: part 1. Pathology, classification and aetiology. Br Dent J 2013; 214: 439–451.
Shanbhag S, Karnik P, Shirke P, Shanbhag V . Association between periapical lesions and maxillary sinus mucosal thickening: a retrospective cone-beam computed tomographic study. J Endod 2013; 39: 853–857.
Acknowledgements
Many thanks to Susanne Perschbacher for providing information about her study in Ontario, Canada, and to John Holroyd (Dental X-ray Protection Services, Public Health England) for information related to panoramic radiography use.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Dave, M., Horner, K. Challenges in X-ray diagnosis: a review of referrals for specialist opinion. Br Dent J 222, 431–437 (2017). https://doi.org/10.1038/sj.bdj.2017.264
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2017.264
This article is cited by
-
The imaging role for diagnosis of idiopathic osteosclerosis: a retrospective approach based on records of 33,550 cases
Clinical Oral Investigations (2021)
-
Challenges in plain film radiographic diagnosis for the dental team
BDJ Team (2020)
-
Challenges in plain film radiographic diagnosis for the dental team: a review of the maxillary sinus
British Dental Journal (2020)
-
The use of localised CBCT to image inflammatory collateral cysts: a retrospective case series demonstrating clinical and radiographic features
European Archives of Paediatric Dentistry (2020)