Key Points
-
Provides an understanding of the classification of microdontia.
-
Discusses the multidisciplinary treatment approach
-
Highlights the restorative treatment options available to treat microdontia
Abstract
Microdontia is a dental abnormality that will often present to the dental practitioner due to the aesthetic concerns of the patient. Treatment is therefore aimed at addressing the aesthetics issue of the patient and this can present a number of challenges which may require a multidisciplinary approach in its management. This article presents the restorative management of localised and generalised microdontia.
Similar content being viewed by others
Management of microdontia
Microdontia is a condition in which one or more teeth appear dimensionally smaller outside the usual limits of variation.1,2 This can pose primarily an aesthetic concern, with patients attending with complaints of having teeth which appear smaller in size or shape to the adjacent teeth or in comparison to others, and the presence of gaps between the teeth. Occasionally, the patient may present with functional difficulties such as food trapping associated with the microdont teeth and may also attend complaining of malocclusions associated with the microdontia such as impacted canines.
Microdontia can be classified into three types according to Shafer et al.:3
-
1
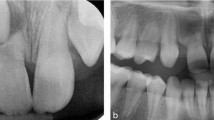
Single tooth microdontia – for example, maxillary 'peg-shaped' lateral (Fig. 1)
-
2
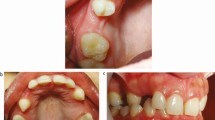
Relative generalised microdontia – the appearance of small teeth within large jaws (Fig. 2)
-
3
True generalised microdontia – is when all the teeth are smaller than normal.
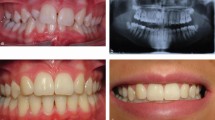
True generalised microdontia is rare, and has been reported in child patients receiving radiotherapy or chemotherapy treatment during tooth development (Fig. 3),4 pituitary dwarfism3 and Fanconi's anemia.5 It is also associated with a variety of syndromes including Gorlin-Chaudhry-Moss syndrome, Williams's syndrome, Ullrich-Turner syndrome, Rothmund-Thomson syndrome, Hallermann-Streiff and Orofaciodigital syndrome (type 3) and a variety of other syndromes.6
The most common teeth affected by microdontia are the maxillary lateral incisor and the third molars but it can affect any of the teeth (Fig. 4). The overall prevalence of peg-shaped maxillary permanent lateral incisors is around 1.8%.7 Maxillary peg-shaped laterals occur more frequently in women than men7 and is more common in patients suffering with Down's syndrome and patients with clefting of the lip and/or palate most frequently occurring on the cleft side.8 Microdontia has also been closely associated with hypodonita (Fig. 5).9,10,11
The cause of microdonita is related to the disturbance in the odontogenesis process. This complex process12 if disturbed can lead to abnormalities in tooth morphology, number and form and with this affect the function, form and aesthetics of the dentition. In the majority of patients microdontia is associated with a genetic basis and has been shown to run through families.13 It has also been identified in spontaneous or isolated cases, where no cause can be identified.14
Treatment options vary in the management of microdont teeth and are dependent on a number of factors but are heavily influenced by the severity of the condition and the patients presenting complaint. The patient presenting compliant, where possible, needs to be addressed and an appreciation of the patient's expectations needs to be evaluated at the planning stage of treatment to ascertain whether the treatment will meet the patient's expectations. If the treatment will not meet the expectations then this needs to be discussed and modified so that the patients can understand the limitations of the dental treatment. Diagnostic wax ups followed by mock ups in the patient's mouth can be a useful visual and diagnostic tool for the patient, clinician and technician and forms part of the informed consent process (Figures 6,7,8).
22 peg lateral with straight distal axial wall positioned distally to accommodate restorative treatment14
The type of treatment should be selected based on functional and aesthetic requirements and a thorough dental assessment is required which often includes an orthodontic assessment.
Treatment options for the comprehensive management of microdontia, which may also include hypodontia, vary but broadly include the following:
-
1
Orthodontic treatment – to idealise tooth position of the microdont tooth or teeth
-
2
Restorative treatment – using direct and indirect techniques on the microdont tooth or teeth
-
3
Joint orthodontics and restorative treatment
-
4
Extraction of the microdont tooth or teeth and orthodontics and tooth replacement if required
-
5
Extraction and tooth replacement
-
6
No treatment – which is unlikely to be acceptable.
Orthodontics
An orthodontic opinion should be sought which can either be the sole treatment in management of microdontia or to help accommodate the restorative treatment by idealising tooth position.15
Microdont lateral incisors have been associated with impacted upper canines16 so orthodontic treatment may have been carried out during childhood.
A Kesling set-up can be carried out as part of the orthodontic assessment to determine the effects of opening or closing the arch space for the microdont tooth/teeth on the overall malocclusion.14 It can also help visualise the proposed orthodontic and restorative end point17 and the aesthetics can be visualised and any potential compromises acknowledged early on in the treatment planning process.
Microdont teeth may be restoratively modified before, during, or immediately after, orthodontic tooth treatment.18 Restorative treatment is often left until after orthodontic treatment is completed, however microdont teeth can be built up to a more desirable size and shape with composite before orthodontic treatment begins – this will help facilitate bracket placement and helps the orthodontist place the tooth in the exact position to facilitate restorative treatment later (Fig. 9).19
It is vital, particularly towards the end of orthodontic treatment that the restorative dentist reviews the patient20 before debond to ensure orthodontic positioning of the crowns and roots of the teeth can accommodate the proposed restorative treatment. If this is not the case then further orthodontic treatment is required or the restorative treatment plan re-evaluated to accommodate the compromised tooth positioning.
Orthodontics can help accommodate restorative management by opening/closing the spacing and idealising tooth position in a mesio-distal, bucco-lingual and apical-coronal position.
Mesio-distal position
In the majority of cases the tooth is positioned in the middle of the space with equal spacing mesially and distally and is particularly true of teeth with parallel axial walls. Where one of the axial walls flare out it may be off benefit to orthodontically position the straightest axial wall fully in contact with the adjacent tooth (see Fig. 8).14 This will help with the aesthetics and will make the placement of the restoration easier. It will also reduce plaque accumulation by minimising the steepness of the emergence profile at the cervical margin of the tooth which can act as a plaque retentive factor.
However, care needs to be taken when restoratively increasing the mesio-distal width as it can lead to a tooth that appears wide and short and appears un-aesthetic – the restoration may need to also increase the length of the tooth to optimise the aesthetics and diagnostic wax ups can help in this regard. Conversely, one of the disadvantages of positioning a microdont centrally in the space may be the requirement to place both a mesial and distal restoration to close space. This would double the restorative maintenance need.
Apical-coronal position
Apical-coronal or 'vertical' positioning of the teeth can dictate the position of the gingival margin and the materials used to restore the teeth. The material being used to restore the microdont tooth or teeth needs to be considered, so that the tooth can be adequately positioned to accommodate the restoration where possible. When using porcelain such as a veneer, intruding the microdont tooth by 2mm apically will create space for the porcelain veneer with adequate thickness incisally to ensure structural integrity without the need for preparing the tooth. If a direct composite based restoration is being used then it may be advised to position the microdont tooth in occlusal contact so that there is reduced risk of fracture/chipping of the weaker composite based restoration14 if this is not attainable then providing at least 2 mm to accommodate the restoration is advised.
The gingival margin position will need to be considered so that it is in harmony with the adjacent teeth, particularly the contralateral tooth.14 There needs to be a balance between optimal incisal position and the desired gingival margin position.14
The apical-coronal position can also affect the occlusion and where possible single microdont teeth should have minimal or no contact in excursive movements as these teeth often have shorter roots and may be less adapted to occlusal load.
Labial-palatal position
The labial-palatal position will dictate the gingival margin as discussed previously, it may also help in providing adequate space to restore the microdont teeth. By placing the tooth slightly palatal, space can be created labially so that restorations can be placed with adequate thickness reducing the need for preparation or overcontoured/bulky restorations where preparation is avoided.
Restorative treatment
Restorative treatment options for microdont teeth include:
-
1
Direct restoration
-
2
Indirect restoration
-
3
Extraction and tooth replacement.
Direct restorations
Composite based restorations can be used as a reversible material to build-up and modify the morphology of the microdont tooth or teeth.21
Direct composite has been shown to be aesthetic, non-invasive, well-tolerated by pulpal tissue, minimally abrasive to opposing teeth and easy to repair and adjust, however, it is prone to staining/discolouration, accelerated wear rate of material in comparison to metal and ceramic based material, bulk fractures, complexity and challenging application with optimal moisture control required.22
Direct composite veneers can provide adequate aesthetics and studies have shown that both direct composite and porcelain can be just as aesthetic.23
When placing direct composite restorations it is recommended that the final labial contour is best placed in one increment to avoid voids24 as voids can attract staining and detract from the aesthetics. Multiple-layering composite systems can be used which come with a range of shades, opacities and translucencies that can provide very aesthetic results, however, getting proficient at using these multi-layering systems comes with experience and further training on specific hands-on courses may be recommended to assist with this (Figs 10,11,12,13).
Where possible the maximal coverage of the tooth should be used to increase the surface area for resin bonding and where possible no preparation or minimal preparation of the tooth to preserve tooth tissue and allow more predictable bonding to enamel is recommended. Pre-treatment of unprepared enamel with pumice will remove the pellicle and ensure a clean surface. This technique is particularly useful in children and young adults where growth has not fully completed; gingival maturity hasn't been achieved and avoids the risk of pulpal pathology in patients with larger pulps. Composite can also be added to, as apical movement of the gingivae occurs during gingival maturity. This restoration can be used as either an interim or definitive restoration and can be added to, removed and modified as required.
Indirect restoration
Veneers allow good aesthetics while being relatively conservative of tooth tissue in comparison to crowns (Fig. 14).25 Tooth removal is often required which can be destructive of reasonably sound tooth tissue,26 however, with microdont teeth preparation may not be needed and if it is this is often minimal – tooth preparation should be minimised to reduce the loss of enamel which is required to optimise the retention of the planned aesthetic restorations.27 Veneers can be either composite or porcelain, and both have proved to be aesthetic with high patient satisfaction.28,29
Ceramic veneers are useful with teeth that have lots of character, which composite can struggle to replicate.30 However, matching the aesthetics can be difficult to achieve.31
The advantages of adhesive ceramic restorations include, good aesthetics, good abrasion resistance, less susceptible to staining (in comparison to composite) and a higher level of gingival tolerance. The disadvantages include a brittle material that is prone to fracture unless applied in bulk, potentially abrasive to opposing teeth, difficult to repair and adjust, and expensive.22
Survival rates for porcelain veneers over periods of up to 16 years have been estimated to vary between 64% to 100%32 with common reasons for failure of veneers including ceramic fractures and large marginal defects.33
Indirect composite resin restorations offer two primary advantages over direct restorations, which include a reduced level of polymerisation shrinkage (as this is carried out in the laboratory) and the ability to add to the veneer after the initial curing phase.22 The advantages include; improved control in comparison to direct composite, the ability to add and repair intra-orally, reasonable aesthetics, less abrasive than indirect ceramic restorations, improved strength and wear resistance in comparison to direct composite. The disadvantages include, inferior marginal fit in comparison to metal and ceramic, expense, and the cementation line may require masking with direct materials.34 For patients with a thin tissue biotype and high lip line, veneers are at risk of aesthetic failure due to gingival recession (Fig. 15).33
Extraction, orthodontics and tooth replacement
Extraction of the microdont tooth/teeth is considered if there is a need for space or the long-term prognosis of the microdont tooth/teeth is poor, which includes teeth with small malformed crowns and lack of coronal tooth tissue to restore, short, thin roots, severely rotated teeth and teeth with associated dental anomalies such as amelogenesis imperfecta or dens in dente where the teeth are deemed unrestorable.
A thorough assessment of the microdont tooth or teeth is required which includes clinical and radiographic investigations and even a Kessling set or diagnostic wax up to visualise the effect of extracting the tooth or teeth.
The restorative management for the residual space of the microdont tooth/teeth is similar to the management if the tooth/teeth were missing due to hypodontia.
If the tooth is extracted or absent the options are either to:
-
1
Orthodontically close the space
-
2
Orthodontically open the space and tooth replacement
-
3
Accept spacing and tooth replacement
-
4
Leave the space unfilled.
The decision to open or close space depends on the number of teeth missing, the degree of crowding and the type of malocclusion.35
Where there is minimal spacing resulting from the extraction of the tooth/teeth it may not be an aesthetic concern to patients or they may be unwilling to accept necessary corrective orthodontic and restorative procedures and the spacing is left,36 however this is very uncommon and often the tooth would be left rather than be extracted.
Orthodontic space closure has the major advantage of avoiding a permanent restoration to replace the extracted tooth and with this a lifelong need for maintenance.35,36 The maxillary lateral incisor is the most common microdont and extraction and space closure to close the maxillary lateral space and substitute this with the canine and disguise this as a lateral incisor is an option. However, a decision to extract this tooth should be made carefully since it is often possible to restoratively improve the appearance of this tooth, when optimally positioned, as described previously in this article.37 Substituting the canine for the lateral incisor is restoratively and orthodontically challenging and the resulting aesthetics varies enormously. This is due to the canine being pointed, wider, longer and darker than the lateral incisor it replaces. It also in general has a gingival margin that is more apically positioned. By selective grinding the cusp tip and possible interproximal reduction, bleaching and using direct composite material a satisfactory result can be achieved.38,39,40
Opening the space is the preferred options when there is little or no crowding, especially where orthodontic treatment does not need to make use of the space and attempts could lead to undesirable aesthetic and orthodontic outcome. However, it commits the patient to the long term care and maintenance associated with restorative tooth replacement.35
The tooth replacement options, if the space is to be prosthetically restored, are:
-
Resin bonded bridge
-
Partial denture
-
Implant retained prosthesis
-
Conventional fixed prosthesis.
Spacing needs careful consideration to achieve an aesthetic result, the amount of spacing is dictated by the aesthetics and also what tooth replacement options are being considered. From an aesthetic perspective the space created is dictated by the dimensions of contralateral tooth so that symmetrical aesthetics are achieved when replacing the extracted microdont tooth. The tooth replacement options will also be dictated by the amount of space available to accommodate the tooth replacement options, this is particularly true of implant based restorations. As there is a close link between microdontia and hypodontia this patient group may present with multiple teeth of the permanent dentition missing and may have missing or retained deciduous teeth that often require replacement. The management of these patients necessitates careful joint multi-disciplinary planning with orthodontics, restorative and in some instances paediatrics and oral and maxillofacial specialties.
Implant-based prosthesis
An assessment should be carried out to see whether an implant-based solution is viable – where microdont teeth have been extracted there is a risk of a lack of bone volume to accommodate an implant and grafting techniques may be required to accommodate this. In addition, those with generalised hypodontia may have a lack of mesiodistal space between crowns and roots. An implant should be placed 1.5-2 mm from the adjacent teeth since placement too close to the adjacent tooth can cause resorption of the interproximal alveolar crest41 and with this leads to a lack of support for the interdental papilla42 leading to a poor aesthetic result. This must also be considered when evaluating the position of the roots of the adjacent teeth and where a lack of space exists, either orthodontic intervention is required to create the space or an implant-based solution is not viable (Figs 16 and 17).
The advantages of using implants are that it avoids using teeth as bridge abutments; they are also useful in patients with a spaced dentition where they can stand alone with spacing without the aesthetic compromise of closing the gap or creating a contact with abutment teeth when using bridgework. They are also useful where abutment teeth are unfavourable.35
Removable partial dentures (RPDs)
Removable partial dentures can be used where there are large numbers of teeth missing, however, for a single tooth or a small number of teeth that need replacing a partial denture isn't regarded as the first line tooth replacement option. It is often used as a temporary tooth replacement option or space maintainer. RPDs are often bulky with potential movement and are functionally and socially unacceptable to many patients as a definitive restoration as is their potential to harm the remaining teeth and periodontal tissues35 particularly in young patients.
Resin bonded bridge (RBBs)
Resin bonded bridges are a minimally invasive fixed prosthetic tooth replacement option and are very useful for anterior single tooth replacement particularly in young patients. They are particularly useful if spacing is unfavourable for dental implants. One of the challenges with metal winged RBBs is the greying effect or shine through the translucent enamel of the central incisor. Using the canines as the abutment teeth can help avoid this due to the reduction in translucency of this tooth or by using an all-ceramic RBB (Fig. 18).35
Conventional bridgework
Use of conventional bridgework is generally limited to the older patient, with heavily restored abutment teeth. In the younger patient the amount of tooth preparation and large pulp leads to a high risk of pulp exposure and subsequent periapical pathology. The reported survival of conventional bridgework is better than that of resin-bonded bridges.43 Failure will occur commonly as a result of recurrent caries and pulpal necrosis and can lead to the catastrophic loss of the abutment teeth leading to further tooth loss,44 and therefore cannot be condoned in a young patient with an unrestored dentition.
Conclusion
This article has shown that the restorative management of patients with microdontia can be challenging. It has emphasised the importance of orthodontics and the multidisciplinary team approach in the treatment of these patient to ensure an optimal outcome is achieved. The use of Kesling set up/diagnostic wax ups allows clinicians, patients and technical staff the ability to visualise the proposed end point of treatment and allows potential compilations or problems to be anticipated before embarking on treatment. Wherever possible, particularly in young patients conservative less invasive treatment is recommended and where restorative treatment is utilised the patient understands the need for lifelong care and maintenance of this restorative treatment.
References
Boyle PE . Kronfeld's Histopathology of the Teeth and their Surrounding Structures. 1st ed. pp 14. Philadelphia: Lea & Febiger, 1955.
Van Beek GC . Dental morphology. An illustrated guide. 2nd ed. pp 127. Woburn, MA: Butterworth-Heinemann, 1983.
Shafer W G, Hine M K, Levy B M . A Textbook of Oral Pathology. 1st ed. pp 26. Philadelphia: W B. Saunders Co, 1958.
Van der waal I, Van der kwast WAM . Oral pathology. Developmental anomalies and eruption disturbances and some acquired disorders of the teeth. 1st ed. pp 114. Chicago: Quintessence Publishing Co. Inc, 1988.
Opinya G N, Kaimenyi J T, Meme J S . Oral findings in Fanconi's anaemia: a case report. J Periodontol 1988; 59: 461–463.
Bargale SD, Kiran SD . Non-syndromic occurrence of true generalized microdontia with mandibular mesiodens- a rare case. Head Face Med 2011; 7: 19.
Hua F, He H, Ngan P, Bouzid W . Prevalence of peg-shaped permanent lateral incisors: a meta-analysis. Am J Orthod Dentofacial Ortho 2013; 144: 97–109.
Burke F J T, Shaw W C . Aesthetic tooth modifications for patients with cleft lip and palate. Br J Orthod 1992; 19: 311–317.
Hobkirk J A, Goodman J R, Jones S P . Presenting complaints and findings in a group of patients attending a hypodontia clinic. Br Dent J 1994; 177: 337–339.
Brook AH . A unifying aetiological explanation for anomalies of human tooth number and size. Arch Oral Biol 1984; 29: 373–378.
Brook AH . Variables and criteria in prevalence studies of dental anomalies of number, form and size. Community Dent Oral Epidemiol 1975; 3: 288–293.
Thesleff I . Genetic basis of tooth development and dental defects. Acta Odontol Scand 2000; 58: 191–194.
Arte S, Nieminen P, Apajalahti S, Haavikko K, Thesleff I, Pirinen S . Characteristics of incisor-premolar hypodontia in families. J Dent Res 2001; 80: 1445–1450.
Khan S, Gill D, Bassi S . Management of microdont maxillary lateral incisors. Dent Update 2014; 41: 867–874.
Bello A, Jarvis RH . A review of aesthetic alternatives for the restoration of anterior teeth. J Prosthet Dent 1997; 78: 437–440.
Brin I, Becker A, Shalhav M . Position of the maxillary permanent canine in relation to the anomalous or missing lateral incisors: a population study. Eur J Ortho 1986; 8: 12–16.
Fields HW . Orthodontic-restorative treatment for relative mandibular anterior excess toothsize problems. Am J Orthod 1981; 79: 176–183.
Harrison J E, Bowden D E . The Orthodontic/ Restorative interphase. Restorative procedures to aid orthodontic treatment. Br J Orthod 1992; 19: 143–152.
Durey K, Cook P, Chan M . The management of severe hypodontia. Part 1: Considerations and conventional restorative options. Br Dent J 2014; 216: 25–9.
Kulshrestha R . Interdisciplinary approach in the treatment of peg lateral incisors. J Orthod Endod 2016; 2: 1.
Asher C, Lewis D H . The integration of orthodontic and restorative procedures in cases with missing maxillary incisors. Br Dent J 1986; 160: 241–245.
Mehta S, Banerji S, Millar B, Suarez-Feito J . Current concepts on the management of tooth wear: Part 4. An overview of the restorative techniques and dental materials commonly applied for the management of tooth wear. Br Dent J 2012; 212: 169–171.
Nalbandian S, Millar B J . The effect of veneers on cosmetic improvement. Br Dent J 2009; 207: E3; discussion 72–73.
Robinson S, Nixon P J, Gahan M J, Chan M F . Techniques for restoring worn anterior teeth with direct composite resin. Dent Update 2008; 35: 551–558.
Patel M, McDonnell ST, Iram S, Chan M F . Amelogenesis imperfecta- lifelong management. Restorative management of the adult patient. Br Dent J 2013; 215: 449–57.
Nathwani N S, Kelleher M . Minimally destructive management of amelogenesis imperfecta and hypodontia with bleaching and bonding. Dent Update 2010; 37: 170–172: 175–176: 179.
Ferrari M, Patroni S, Balleri P . Measurement of enamel thickness in relation to reduction for etched laminate veneers. Int J Periodontics Restorative Dent 1992; 12: 407–413.
Nalbandian S, Millar B J . The effect of veneers on cosmetic improvement. Br Dent J 2009; 25: 207. (2): E3; discussion 72–3.
Meijering A C, Creugers N H, Roeters F J, Mulder J . Survival of three types of veneer restorations in a clinical trial: a 2.5-year interim evaluation. J Dent 1998; 26: 563–568.
Barber AJ, King PA . Management of the single discoloured tooth. Part 2: Restorative options. Dent Update 2014; 41: 194–6: 198–200: 202–4.
Christensen GJ . Restoring a single anterior tooth –Solutions to a dental dilemma. J Am Dent Assoc 2004; 135: 1725–1727.
Burke FJ . Survival rates for porcelain laminate veneers with special reference to the effect of preparation in dentin: a literature review. J Esthet Restor Dent 2012; 24: 257–265.
Peumans M, De Munck J, Fieuws S, Lambrechts P, Vanherle G, Van Meerbeek B . A prospective ten-year clinical trial of porcelain veneers. J Adhes Dent 2004; 6: 65–76.
Kilpatrick N, Mahoney E . Dental erosion: part 2. The management of dental erosion. NZ Dent J 2004; 100: 42–47.
Carter N E, Gillgrass T J, Hobson R S et al. The interdisciplinary management of hypodontia: orthodontics. Br Dent J 2003; 12: 361–366.
Jepson N J, Nohl F S, Carter N E et al. The interdisciplinary management of hypodontia: restorative dentistry. Br Dent J 2003; 22: 299–304.
Carter N E, Gillgrass T J, Hobson R S, Jepson N, Meechan J G, Nohl F S, Nunn J H . The interdisciplinary management of hypodontia: orthodontics. Br Dent J 2003; 194: 361–366.
Thordarson A, Zachrisson B U, Mjor I A . Remodelling of canines to the shape of lateral incisors by grinding: A long term evaluation. Am J Orthod Dentofacial Orthop 1991; 100: 123–132.
Millar B J, Taylor N G . Lateral thinking: the management of missing lateral incisors. Br Dent J 1995; 178: 99–106.
Sabri R . Management of missing lateral incisors. J Am Dent Ass 1999; 130: 80–84.
Thilander B, Odman J, Jemt T . Single implants in the upper incisor region and their relationship to the adjacent teeth. An 8 year follow up study. Clin Oral Implants Res 1999; 10: 346–355.
Jivraj S, Chee W . Treatment planning of implants in the aesthetic zone. Br Dent J 2006; 22: 201: 77–89.
Scurria M S, Bader J D, Shugars D A . Meta-analysis of fixed partial denture survival: Prostheses and abutments. J Prosthet Dent 1998; 79: 459–464.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Laverty, D., Thomas, M. The restorative management of microdontia. Br Dent J 221, 160–166 (2016). https://doi.org/10.1038/sj.bdj.2016.595
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2016.595
This article is cited by
-
Restorative dentistry clinical decision-making for hypodontia: peg and missing lateral incisor teeth
British Dental Journal (2023)