Key Points
-
Reports that 15.5% of patients changed dentist between 2003 and 2005.
-
Highlights that the proportion of patients changing dentist has increased steadily since 1993.
-
Reviews factors influencing patients changing dentist, such as patient age, charge paying status, dentist age and gender.
-
Explains that the patient's previous attendance pattern is also a factor when patients changing dentist.
Abstract
Aim
It is the aim of this paper to consider the factors associated with a patient's continuing attendance at a particular dentist's surgery.
Methods
A data set was established consisting of General Dental Services' (GDS) patients whose birthdays were included within a set of randomly selected dates, 20 in each possible year of birth. The data set was restricted to those patients aged 18 or older in 2003 who attended only one dentist in only one postcode area in 2003, and who also attended only one dentist in the same postcode area in 2005, and where the dentist attended in 2003 was also practising in the same postcode area in 2005. The patients were classified by age, gender and charge-paying status, and by whether they had attended a GDS dentist in 2002, and the dentists attended in 2003 were classified by age and gender. The proportion of patients changing dentists between 2003 and 2005 was calculated, together with standard error (se), for each combination of these factors. This was then replicated for each year from 1993–2002.
Results
Data for 323,382 patients were included in the analysis for 2003, these patients having not changed address during a two-year period, nor had their dentist changed location. The proportion of patients changing dentist over the period 2003 and 2005 was 15.5% (se 0.06 PCT). This has increased steadily since 1993, when the proportion was 12.4%.
Conclusions
Factors influencing whether a patient changes dentist include patient age and charge paying status, dentist age and gender, and the patient's previous attendance pattern.
Similar content being viewed by others
Introduction
Patient attendance
Information concerning the factors that influence a patient's choice of a particular dental practice and dentist are not well defined, but might be considered to include location, proximity to work or home, hours of opening, facilities, treatments offered and the dentist's reputation, manner and treatment effectiveness. However, information on the factors which encourage a given patient to continue attending a particular practice is scarce.
Results of work carried out in Australia using a postal questionnaire to 1,010 patients indicated that approximately one third of the 885 respondents reported attending a different dentist to that attended two years previously,1 with the proportion of patients changing dentist being greater among those not treated in the private sector. The majority had changed for reasons out of the immediate control of the dentist, but 15% had changed because they were unhappy with the treatment that they had received. The rate of failure to attend has recently been investigated, with the sending of a SMS text message having been shown to reduce the failure rate for outpatient dental appointments.2
Results of the Australian National Survey of Adult Oral Health in 2004–2006 indicated that dental attendance patterns were worse in terms of continuity in rural and remote locations.3 A follow up study to this work was carried out in order to identify the non-treatment costs associated with dental treatment from the perspective of the patient, with the results indicating that patient perception of the impact of travel costs and impact on family life were major drivers restricting access to dental services for people living in remote locations in New South Wales, Australia.4
Reasons for failing to attend for recall appointments have been investigated in rural India. On a database of 288 patients, 93 failed to return, citing lack of time as the most prevalent reason for non-attendance, but with males being more likely to attend for the recall appointment than female patients.5
Chronic illness may act as a barrier to dental attendance. In a cross-sectional postal questionnaire study in England, Baird and colleagues concluded that multiple sclerosis had a negative impact on perceived dental attendance.6
Attendance for a dental check-up was investigated by Batchelor in 2004,7 with the results indicating that the percentage of British adults who attended for a dental check-up within a 12-month period increased over the years 1991–2000. However, he also noted considerable variation in attendance by both age, with those aged between 46 and 55 years having the highest percentage of check-ups (75%), and by sex, with a higher proportion of females reporting having had a check-up under NHS arrangements than males, although no differences were found in the non-NHS sector.
It could be considered that patient loyalty is associated with satisfaction. Accordingly, a study examining patient satisfaction with ten dental practices in the UK, by Holt and McHugh, may be of relevance. These workers used questionnaires handed to patients.8 A total of 1003 questionnaires were returned by patients, with the most important factors with regard to patient satisfaction being 'care and attention' (rated as very important by 90% of respondents), followed by 'pain control/dentist puts you at ease/safety conscious' (all rated as very important by 79–82% of respondents) and 'explanation of treatment' which was rated as very important by 73% of respondents. Dentist's behaviour and personal skills may therefore be considered important in retention of patients. Patient satisfaction may also be considered to include a wide variety of factors, from ease of parking, location, friendliness of staff, and appearance of the surgery and the practice as a whole, but may also include satisfaction with treatment outcome. In this regard, it has been considered that unmet patient expectation with treatment outcome is a principal reason why patients resort to legal means in an attempt to receive compensation for treatment which has not met their expectation, with this occurring more and more frequently at the present time (KJ Lewis, Dental Director, Dental Protection Ltd, Personal Communication, October 2013).
Accordingly, while there is a reasonable amount of information in respect of factors influencing dental attendance, there is a paucity of information on factors which encourage or influence continuing attendance at a given dentist's practice. It is therefore the aim of this study to examine attendance patterns of patients at a given dentist with respect to the factors which lead to a patient not returning to that dentist, when neither patient nor dentist has changed address. This study uses a recently-developed, very large set of administrative patient data and tracks the attendances of patients with different dentists over three successive years.
Objectives
To establish the factors associated with a patient changing to a different dentist in the General Dental Services (GDS) in England and Wales, excluding patients who relocate or whose dentist ceases to practise in the same area.
Methods
The data
The source data9 consist of the attendance records of an age-stratified sample of GDS patients defined by 20 different dates of birth in each year of birth - generating over one million different patients in each year from 1991–2005. Each attendance record contains data about the patient, the dentist, the dates of the course of treatment and the post-code area of the dental practice where the treatment took place.
The sample
For the purpose of this study, the GDS data set for patients attending in 2003 was restricted to adult patients (aged 18 or over on 31st December 2002, that is, year of birth earlier than 1985) who attended only one dentist in only one postcode area in 2003, and who also attended only one dentist in the same postcode area in 2005, and where the dentist attended in 2003 was also practising in the same postcode area in 2005. The patients were classified by age, gender and charge-paying status, and by whether they had attended a GDS dentist in 2002, and the dentists attended in 2003 were classified by age and gender. The proportion of patients changing dentists between 2003 and 2005 was calculated, together with standard error (se), for each combination of these factors. This was then replicated for each year from 1993–2002.
Results
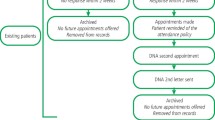
A total of 323,382 patients were included in the analysis for 2003. Figure 1 indicates that most of the patients excluded were either children in 2002 or they did not attend the GDS in 2005, although some of these patients could have been lost due to transfer to the Personal Dental Services initiative within the NHS at that time. The number of patients included in the analysis for 1993 was 431,855.
Of these 328,382 patients who attended in both 2003 and 2005, 15.5% (se 0.06 PCT) changed dentist. Figure 2 shows how this has increased steadily since 1993, when the proportion was 12.4% (se 0.05 PCT).
Figure 3 illustrates:
-
That non-payers were less likely than payers to return to the same dentist, irrespective of their attendance history or age (other than in the age group 70 years and over)
-
That patients who attended a different dentist in 2002 were the least likely to return to the same dentist, irrespective of age or payment status
-
That patients who did not attend any dentist in 2002 were less likely than those who had previously attended the 2003 dentist to return to that dentist, irrespective of age and payment status
-
The older the patient, the lower the proportion who changed dentist, irrespective of payment status and attendance history (except for patients aged 70 and over).
Figure 4 illustrates that:
-
With regard to dentist age, dentists under the age of 30 years are less likely to have a patient re-attending than dentists in other age groups, until dentist age group 55–60, and over 60 years, when patient re-attendance becomes less likely.
-
Patients who did not attend in 2002 were less likely to re-attend than those who had seen the same dentist in 2002, but in both cases the likelihood of changing dentist was related to the dentist's age.
-
Patients who attended another dentist in 2002 were the most likely to change dentist, and there was little relationship between this likelihood and the age of the dentist.
-
Charge-paying and non-charge-paying patients who attended the same dentist in 2002 (that is, had loyalty to that dentist) showed the lowest rates of changing dentist, whatever the age of the dentist.
Figure 5 indicates that:
-
In three dentist age groups patients were more likely to change dentist if that dentist was female. The groups were under 30, 30–34 and 40–44. Outside these ages, male and female dentists had similar proportions of patients changing dentist.
-
From ages 45–59, dentists had the highest rates of patient retention, with little difference between males and females.
The interaction between dentist age, patient age and charge-paying status is presented in Figure 6. This indicates that there is little interaction between the ages of patient and dentist and the patient's charge-paying status. Within each dentist age group there is a similar pattern of changing rates by patient age group and status.
In summary, the following factors were found to be significant:
-
Patient age: younger patients are more likely to change than older
-
Charge-paying status: charge-paying patients are less likely to change
-
Dentist age: patients of younger dentists are more likely to change
-
Dentist gender: patients of female dentists are more likely to change, with younger female dentists being more at risk of patient loss than male dentists
-
Patient history: new patients are more likely to change than those who attended the dentist in the previous year, particularly if they attended a different dentist in the previous year.
Discussion
With 25 million courses of treatment being linked over 15 years, the dataset used in this work is the largest ever to become available for work on dental treatment. This is the first publication related to the interrogation of this dataset. Because of the size of the dataset, not only can complex interactions be explored, but the robustness of resultant models and algorithms can be tested by replication. The new dataset, was released to the research community in August 2012 by the UK Data Service.9 While the method of payment to NHS dentists changed in April 2006 and data are no longer collected centrally at the individual tooth level, it may be considered that dentists have continued to carry out their work to the same high ethical and technical standards as were applied to the data in the data set. In this regard, there has been little fundamental change to the dental procedures or the materials used since 2006. In other words, the data may be considered valid at the current time and also until new technological advances are made and widely implemented.
The 2009 Adult Dental Health Survey of England, Wales, and Northern Ireland10 examined patient attendance patterns (but not re-attendance), with the results indicating that 61% of dentate adults stated that the usual reason for attendance at a dentist was for a regular check-up. A further 10% stated that they attended for an occasional check-up, while 27% stated that they only attended when 'having trouble'. In that regard, attendance patterns were associated with other aspects of oral health-related preventive behaviour, including frequency of tooth-brushing, use of additional dental hygiene products, plaque levels, presence of calculus and lower levels of anxiety, with regular attendance being associated with improved oral health-related preventive behaviour and lower levels and plaque and calculus.10 The present work may be considered to provide new information on the dentist and patient related factors which may affect patient re-attendance at a particular dentist.
Continuing care by the same dentist may be considered beneficial to the patient, as they will be known in the practice that they attend, their previous records and radiographs will be available, and thereby, their disease history and risk of further disease, and they are likely to receive fewer replacement restorations.11,12 It is also valued by dentists, for whom 'goodwill' is an important component in the valuation of a dental practice, and patient re-attendance will improve practice business. In this regard, in business terminology (and dental practices, while there to provide ethical treatment for patients, may still be considered small businesses), the term Customer Relationship Management (CRM) is increasingly designed, according to Wikipedia, 'as a customer-oriented feature with service response based on customer input, solutions to customers' requirements and communication that help customers solve their problems'.13 Accordingly, in CRM terms, apart from cases where patients or dentists move out of the area, what makes patients change dentist, or conversely, what makes dentists lose their patients? This study uses a massive set of administrative patient data (the largest ever developed for dental research) and tracks the attendances of patients with different dentists over three successive years in an attempt to answer this question.
As identified in the introduction, a paucity of papers has addressed the subject of patient loyalty. One paper is available which addresses this subject directly. In this, US practitioners' views on why patients change dentist were evaluated in 1986 using a short self-administered questionnaire.14 Useable replies were obtained from 619 general dentists, 96% of whom were men with the median number of years in practice being 21. Changing residence and changing job location were considered to be the most prevalent reasons for changing dentist (and these have been discounted in the present study). Dissatisfaction with the way they were handled, dissatisfaction with the quality of care and dissatisfaction with pain and anxiety control were the next most prevalent reasons presented by the responding dentists. This echoes the results of the survey by Holt and McHugh in the UK.8 Almost 30 years on, it may be considered that these will remain reasons why patients leave a particular dentist but the methodology of the present study is unable to assess these factors. However, examination of the figures indicates that two factors stand out as affecting patterns of retention of patients: charge-paying status and whether the patient is new to the dentist. In this regard, patients who previously attended a different dentist are particularly likely to change again.
Results of research on an earlier version of the large database used in the present study indicated that patients who were charge payers had restorations (be they direct placement fillings, crowns or bridges) which survived for longer periods of time than those patients who were exempt from charges.15 The reasons for this finding may be considered to be multifactorial, but may include differences in socio-economic status between the charge payers and those who did not pay charges and attendant differences in oral health behaviours and diet, notwithstanding the fact that patients who pay for treatment may value it more than those who do not pay. A similar factor could be at work here in the finding that patients who do not pay charges are less likely to re-attend the same dentist: it may be that a higher proportion of them simply do not regularly attend any dentist, so that re-attendance within the two-year period of the present study reflects urgent need rather than regular attendance. The timescale used in the present work to represent 'continuing care' was chosen because this was identified within the GDS as the maximum time interval for continuing attendance. However, the results may also give an important message for those who plan dental services. In this regard, Donaldson and co-workers concluded that 'overcoming barriers to regular dental attendance for low socio-economic groups may reduce oral health inequalities'.16
Dentists who are starting or re-starting their careers, or increasing their working hours, may have little choice as to which patients they see as they will be junior members of staff, and necessarily see proportionately more new patients who do not have an established attendance pattern or feel a need to present regularly at a dental surgery for a check-up. This may help to explain why younger dentists, and, in particular, female dentists of child-bearing age, have such high rates of patient loss. Other factors may also be at work. The young female dentist may have absences due to maternity leave and thereby find difficulty in establishing a long-term relationship with a patient. Similarly, young dentists, be they male or female, may be perceived as lacking experience by some patients. One wonders whether some grey hair and some wrinkles might improve patient confidence: the subject of another research project, perhaps?
The reasons why patient loyalty to a particular dentist is lower in younger patient age groups could be explained by the perceived higher mobility of such age groups, as they move in the search for fixed employment or to study. However, this perceived population mobility has been erased from the data set used in the present work, as only patients who were at a fixed address were included. However, this might include those who moved away to study or to find work, but who retained the family home as their address during a period when their actual living address was somewhat mobile. An alternative explanation could be the natural rebellion of youth-changing dentists as a change of fashion and statement of independence!
The reduced retention of patients by older male dentists of 55–60 years may also be considered worthy of comment and discussion. They may have the confidence-inspiring wrinkles, but they have poorer retention rates of patients than their male colleagues ten and twenty years younger. Might it be that this group are losing interest and that this has become apparent to their patients, or might it simply be that they have chosen to work fewer hours (or reduced their NHS hours) in the run up to retirement, with patients thereby finding it more difficult to obtain an appointment?
Let us return to the 2009 Adult Dental Health Survey. The results indicate that the majority of adults were positive about their last visit to the dentist, with 80% giving positive feedback.10 However, 20% of consultations were considered to be less than satisfactory, with the two most commonly reported concerns relating to 'not having been given enough time' and not being involved in 'decisions about dental care or treatment'. However, the survey was unable to identify the dentist factors which related to these perceived problems. Other factors, such as chair-side manner, may also play a role, and the charts presented in the present work may provide a benchmark against which dentists may rate their own performance or plan their strategies for the recruitment and retention of patients. Factors relating to the dental practice per se may also be of influence. In discussing the findings of the 2009 Adult Dental Survey, Hill and co-workers found that 85% of adults rated the practice that they had last attended as good or very good in terms of time to wait for a routine appointment.10 However, that leaves 15% of patients who are less than satisfied, and it may be this group who elect to change dentist. The dentist concerned may be among those who are or who have reduced their practising hours. The lack of availability of urgent appointments was also reported as a factor in which 13% of respondents expressed less than satisfaction, as too was the availability of evening and/or weekend appointments. These, along with the standard and quality of care provided, may be factors involved in the retention or non-retention of patients.
Other reasons for patients failing to return to a given dentist may be involved, such as the treatment carried out in the last course of treatment, for example, a surgical extraction. These would not affect the overall data presented here, but will, nevertheless, be the subject of further investigation.
Data are currently being collected on NHS dentistry by the Health and Social Care Information Centre (HSCIC),17 so it may be appropriate to examine factors in their most recent annual statistical report which may be considered of relevance to the present work. When the data post-2006 are examined, it is apparent that progressively fewer dentists own their own practice and there are not many new 'providing performers', that is, there are not many new providers who are also dentists. This may have implications for the provision of care and the retention of patients, because a major incentive to retaining patients is to be the owner of the practice, with all the financial implications thereof. This document17 advises that there are increasing numbers of female dentists, with the proportion rising to 46.1%, from 38.8% in 2006/07 (for detailed information see figure in HSCIC data). This increase is mainly in young dentists. This also is of relevance to the present work, given the poorer retention of patients by younger female dentists that we have identified, and the likelihood that some young female dentists will have interruptions in patient continuity as they go off on maternity leave.
Data at individual patient and course of treatment level (though not at tooth level) are still collected and available to the HSCIC, though not as yet to the wider community. The analysis which we have conducted over the period from 1991–2006 could therefore be repeated for the years from 2006 onwards, albeit at the level of dental performer or dental provider, rather than principal dentist.
Finally, the importance of the findings should not be underestimated in this era of increasing competition among dentists, notwithstanding the perceived surplus of dentists (as evidenced by the reduction in the number of UK dental students prescribed by the Department of Health in 2014). Every dental practice needs a regular patient base: it is hoped that this paper will help provide some pointers regarding how to achieve this.
Conclusions
Factors influencing whether a patient changes dentist include patient age and charge paying status, dentist age and gender, and the patient's previous attendance pattern.
References
Thomson W M, Stewart J F, Carter K D, Spencer A J . Patient mobility in Australian dentistry. Community Dent Health 1996; 13: 99–104.
Foley J, O'Neill M . Use of mobile telephone short message service (SMS) as a reminder: the effect on patient attendance. European Archives Paed Dent 2009; 10: 15–18.
Australian Institute of Health and Welfare. The national survey of adult oral health 2004–06: Australian capital territory. Dental and Statistics Research. 2008. Online information available at: http://blogs.adelaide.edu.au/arcpoh/2010/05/10/the-national-survey-of-adult-oral-health-state-and-territory-reports (accessed February 2015).
Curtis B, Evans R W, Sbaraini A, Schwartz E . Geographic location and indirect costs as a barrier to dental treatment: a patient perspective. Aust Dent J 2007; 52: 271–275.
George A C, Hoshing A, Joshi N V . A study of the reasons for irregular dental attendance at a private dental college in a rural setup. Indian J Dent Res 2007; 18: 78–81.
Baird W O, McGrother C, Abrams K R, Dugmore C, Jackson RJ . Factors that influence the dental attendance pattern and maintenance of oral health for people with multiple sclerosis. Br Dent J 2007; 202: E4.
Batchelor P A . Changes in self-reported attendance of British adults for dental check-ups between 1991 and 2000. Primary Dent Care 2004; 11: 125–130.
Holt V P, McHugh K . Factors influencing patient loyalty to dentist and dental practice. Br Dent J 1997; 183: 365–370.
Information Centre for Health and Social Care and NHS Business Services Authority. Longitudinal dental treatment, 1990–2006. 2012. Online information available at http://discover.ukdataservice.ac.uk/catalogue?sn=7024 (accessed February 2015).
Hill K B, Chadwick B, Freeman R, O'Sullivan I, Murray J J . Adult Dental Health Survey 2009: relationships between dental attendance patterns, oral health behaviour and the current barriers to dental care. Br Dent J 2013; 214: 25–32.
Lucarotti P S K, Holder R L, Burke F J T . Outcome of direct restorations placed within the General Dental Services in England and Wales (Part 1): variation by type of restoration and re-intervention. J Dent 2005; 33: 805–815.
Burke F J T, Lucarotti P S K . Ten-year outcome of crowns placed within the General Dental Services in England and Wales. J Dent 2009; 37: 12–24.
Wikipedia. Customer relationship management. Online information available at http://en.wikipedia.org/wiki/Customer_relationship_management (accessed February 2015).
O'Shea R M, Corah N L, Ayer W A . Why patients change dentists: practitioners views. J Amer Dent Assoc 1986; 112: 851–854.
Burke F J T, Lucarotti P S K, Holder R L . Outcome of direct restorations placed within the General Dental Services in England and Wales (Part 2): variation by patients' characteristics. J Dent 2005; 33: 817–826.
Donaldson A N, Everitt B, Newton T, Steele J, Sherriff M, Bower E . The effects of social class and dental attendance on oral health. J Dent Res 2008; 87: 60–64.
Health and Social Care Information Centre. NHS Dental Statistics.England, 2013-14. 2014. Online information available at http://www.hscic.gov.uk/catalogue/PUB14738 (accessed February 2015).
Acknowledgements
The authors acknowledge the support of the Economic and Social Data Service, the Health and Social Care Information Centre and the NHS Business Services Authority for collating and releasing this valuable data resource.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Lucarotti, P., Burke, F. Factors influencing patients' continuing attendance at a given dentist. Br Dent J 218, E13 (2015). https://doi.org/10.1038/sj.bdj.2015.230
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2015.230
This article is cited by
-
Are NHS dental practices socioeconomically distributed in Scotland, Wales and Northern Ireland?
British Dental Journal (2020)
-
Long-term validity and reliability of a patient survey instrument designed for general dental practice
British Dental Journal (2015)