Key Points
-
Describes how electronic 3D images for use in clinical dentistry can be produced using both contact and non-contact methods.
-
Highlights how these images can be used in the different dental disciplines.
-
However the original is scanned, the output generated is composed of a discrete series of data points in 3D, which is used to recreate the final surface image.
Abstract
3D imaging has been widely used within various fields of dentistry to aid diagnosis, in treatment planning and appliance construction. Whereas traditionally this has involved the use of impression materials together with plaster or stone models, modern techniques are continually evolving which use virtual 3D images. These electronic virtual images are created using either contact or non-contact optical scanning techniques, but there are limitations, the most important of which is that any new virtual surface image is created from a series of discrete data points. It is not created from a continuous stream of data relating to the original object. This means that computer software has to be used to recreate a possible best fit, virtual surface from the data obtained. This paper describes the principles behind 3D scanning technology, the limitations of 3D imaging as well as current and possible uses of such imaging in clinical dentistry.
Similar content being viewed by others
Introduction
Within dentistry there has always been a requirement to record and manipulate three dimensional (3D) replicas of patients' tissues. To date this has predominantly been in the form of impressions and plaster or stone models. Whilst these have the advantage of dimensional accuracy, familiarity and ease of handling, they also possess a number of disadvantages, the principal ones being the time and the facilities required for fabrication, cataloguing, storage and retrieval. In recent years there have been developments in electronic 3D imaging that have led to an increasing use in dentistry, including restorative dentistry, orthodontics, and orthognathic and craniofacial surgery. It is easy to take such developments for granted and to automatically assume the images produced are accurate and reliable representations of the original. It is useful for the practising dentist to have an understanding of how such digital images are produced and indeed consider what we are actually looking at.
What are the principles behind 3D surface imaging?
3D surface scanners, as the name suggests, are devices that create a digital map of the surface of an object and collect data on its three dimensional shape and size. The raw data are usually obtained in the form of a point cloud, representing the 3D coordinates of the digitised surface. In practice there are two main categories of 3D surface scanners: contact and non-contact scanners. These will be described in turn.
Contact scanners
Many contact scanners are CMMs (co-ordinate measuring machines) which are mechanical systems designed to move a measuring probe over a surface and to determine the coordinates of the points comprising the surface. They have four main components: the measuring probe, the control or computing system, the machine which moves the probe and the measuring software. The mechanical measuring probe performs a linear or radial scan of the desired surface and, as it does so, the position of the stylus tip in the x, y and z planes is sampled at regular intervals. This gives rise to an array of data points, or a 'point cloud', representing points which lie on the object surface. An example of a contact probe scanner in use in dentistry is the Incise system (Fig. 1) (Renishaw, Wotton–under–Edge, UK), where the measuring probe has a ceramic shaft on the end of which is a ruby ball. This type of scanner can only usefully be used on hard surfaces such as dental stone, as a soft surface will either deform or wear when in contact with the probe. These scanners are used in the dental laboratory to obtain surface scans of tooth preparations. The 3D information is then used to mill alumina crown copings. Whilst contact probe scanning is very accurate, the scanning process is relatively slow when compared to non-contact optical systems.
Non-contact optical scanners
Many 3D laser scanners employ the principle of triangulation, familiar to most people from the fields of cartography and surveying, to obtain 3D surface images. A laser beam is incident on the surface of the object to be scanned and a camera-like device, such as a charge-coupled device (CCD) or position sensitive detector, is used to record the location of the point at which the laser beam strikes the object. Since the positions of both the laser and camera and the angle between them is known, the position of the surface can be calculated using simple triangulation. The measurement accuracy is mainly dependent on the accuracy of the image acquired from the object surface by the detector.1 However, beam reflection and stray light will affect the measurement accuracy, as will differences in the topography and finish of the object under investigation relative to the calibration surface. It is therefore important to calibrate the scanner on a surface with similar properties to the object to be scanned. Laser scans can either be created from a point which is progressively scanned over the object surface, or more rapidly by imaging the object with a series of laser lines or profiles. A potential problem can occur when a series of parallel laser lines progressively scan over an object surface. If there is a steep change in the object surface such as a void, as the first laser line passes into this void it may pass out of site of the detector or camera, which may then mistake the second laser line, yet to pass over the void, as the first line. Errors can then occur when the image is reconstructed by the computer software.
Photogrammetry, like laser scanning, also employs the principles of triangulation, but instead of a laser beam it uses a series of photographs of the object of interest. Variations on this method use aspects of photographic images such as defocus, shading and scaling which can help give an estimate of 3D shape and depth. The major drawback of this technique is that it is not possible to obtain the dense point clouds required for free-form surface modeling and accurate CAD surface reconstruction. Reconstruction of the acquired image can also be time consuming.
Interferometric techniques may use laser or white light. Interferometry uses the principle that waves will interact with one another causing interference. If waves are perfectly in phase they reinforce each other, but if they are perfectly out of phase (and of equal amplitude) they will cancel each other out. In interferometric shape measurement, light of different wavelengths (colours) is projected along a single beam onto a surface. The interference between the wavelengths depends on the distance between the source and the surface, thus fringes of dark and light are formed on the object which relate to the topography of the surface. In a sense, the interference fringes can be considered to be forming contours such as those seen on an Ordnance Survey map. The advantages of interferometry include high resolution, a long range, and they are also relatively insensitive to mechanical vibrations. Multiple variants have been developed.
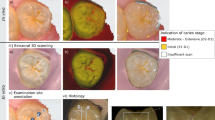
The Structured Light Method uses a well-characterised simple image which is projected onto the surface to be investigated. This image is often an array of black (dark) and white (bright) lines or a 'checkerboard' of black and white squares. Unless the surface is perfectly flat, the image will appear deformed. Therefore it will no longer look like an array of lines or squares but will take on a new appearance, which is a combination or superposition of the original image and the surface topography. The pattern images captured by the CCD camera are digitised and the phase distribution in the patterns is obtained by phase analysis techniques, such as Fourier transforms or phase stepping techniques.2 In other words, once the image is captured a computer algorithm is used to 'decode' the surface topography from the difference between the projected image and the original image. Figure 2 shows a sample process of the digital fringe projection technique.3 The main advantages of this method of 3D optical scanning are the high speed, low cost and high accuracy. It is used in the 3dMd facial imaging system.4 However, the technique is not without its problems as issues such as shading and surface holes or crevices will present problems with image projection and subsequent capture.
Digital fringe projection on a dental model35
The Moir fringe method is another projection technique. Here, light projected onto the surface of interest passes through a grating. The projected image is picked up by a camera after the light has passed back through an identical reference grating. The interference pattern created, in the form of lines on the object surface, can be used to create a 3D surface image, once again using triangulation techniques dependent on the position of the light and camera.
Converting the scanned image data into a format that can be used clinically
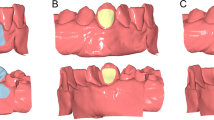
The raw data obtained from a 3D scanner is normally in the form of a point cloud, which represents the 3D coordinates in the x, y and z planes of the digitised surface (Fig. 3a). As the name suggests, this is a representation of each of the data points obtained from the image surface. The density of the point cloud and therefore how accurately it represents the imaged surface depends on numerous factors. These will include the capability of the particular scanner, both in terms of its hardware and software, how it is used by the operator and the time spent scanning. Missing data within the point cloud, for example as a result of an undercut, can pose problems when trying to accurately represent the original image surface. It is not difficult to see that the acquisition of the 3D data points to create a suitably dense point cloud, without missing data, can be a time consuming process and may require multiple scans from various different directions.
The production of the point cloud enables the observer, in this case a dentist, to explore and manipulate the virtual 3D image on the computer screen.5 However, although it might be relatively easy to visualise a tooth or teeth, as represented by the point cloud in one direction, when the same point cloud image is viewed from another direction it may not be as easy to visualise (Figs 3a–3b). In order to make the visualisation process more intuitive, computerised polygonisation of the point cloud is used to fabricate a virtual surface from the scan data.6 In this process the data points are linked to adjacent points within the cloud to make a polygon mesh. The polygon mesh usually being composed of triangles joining three adjacent data points within the cloud. The scanned object surface is therefore represented as a series of flat polygons, which in close up, although easier to view than the point cloud, might still make it difficult to visualise the surface. In addition it will also not replicate the original, relatively smooth surface of the scanned object. This will obviously depend to a large extent on the density of the point cloud. The greater the density, the more accurate and indeed the easier the surface visualisation will be.
The same model as Figure 3a viewed from a different angle where visualisation of the individual teeth within the point cloud is very difficult
Although software can create the polygon mesh from a single large scanned image, often the surface reconstruction process begins with the point cloud being divided into several features (eg molar, premolar, incisor, etc). A polygonised surface is created for each of these individual features. Once this has been done, each can be shaded and textured to give a realistic appearance and the individual scanned and processed components reassembled to create a final image. There are different types of shading that can be applied to such a rendered surface with examples being Gouraud and Phong shading.
It should be remembered that the final image – created by whatever technique – when made from a point cloud will have areas within it where there are no data concerning the scanned surface. This is because the data capture is not truly continuous, but is composed of discrete data points. Therefore, what we see in any final image may not be a true representation of the object surface.
The production of the polygon mesh and then the further post-processing surface rendering relies on a consistent set of point cloud data, without missing data points. If data points are missing then surface rendering is extremely difficult due to the algorithms usually defined within the rendering software. There are many types of such algorithms available.7 Figure 4 shows an example of surface polygonisation of half of a maxilla from the original point cloud.
Comparison of the polygonised surface on the left with the original point cloud data on the right35
An example of a software package which is capable of creating surfaces from point cloud data, and which is in common use in engineering, is Imageware.8 In addition to being able to accurately reconstruct complex 3D models, this software also enables detailed analysis of images, including measurement between feature points and areas. For example, it is possible to scan pre and post treatment upper study models of a patient and determine changes from one to the other, provided a stable reference landmark is available. One suggested reference is the medial aspect of the third palatal rugae. By superimposing two surface models, as in Figure 5, where the before treatment model in red is superimposed on the post treatment model in blue, a 3D surface to surface evaluation can be realised virtually. Once the images have been acquired and processed, point to point measurement of treatment changes then becomes relatively straightforward. Using the same principles, it is also possible to measure linear and volumetric changes in teeth as a result of tooth erosion.9 Although 3D imaging has applications within dental research, there are an increasing number of 3D imaging systems available with direct clinical applications and in various fields of dentistry.
Restorative dentistry
Within restorative dentistry, computer-aided design (CAD) and computer-aided manufacture (CAM) of indirect restorations became available approximately 20 years ago.10 Since this time, the rapid development of computer-based technology has provided increasingly sophisticated replication and digitisation of the complex topography of tooth structures. One of the criteria that must be fulfilled for any indirect restoration to be successful is an accurate fit to the tooth. This will be determined by the whole production process, but in particular the initial assessment of the surface topography of an object. In the case of a tooth, whether prepared or unprepared, it is composed of complex irregular geometric configurations that are unique in each case and where there is no exact reference form.11 Even with these potential problems there are several advanced dental CAD/CAM systems now available. These include systems which are capable of directly scanning within the mouth, namely:
-
Cerec 3 (Sirona, Bensheim, Germany). This system scans preparations intraorally using infrared irradiation. Alternatively models can be scanned in the laboratory. The marginal fit of crowns produced using this technique has been reported to be in the range of 60 to 100μm12,13
-
Hint-ELs® DentaCad System (Hint-ELS, Griesheim, Germany). This system is based on a visible light optical scanner
-
Lava (3M ESPE, Seefeld, Germany).Although already available as a laboratory based scanning system, it is soon to be introduced as an intra oral system based on a hand held wand using visible light. It can scan a single tooth up to a whole dental arch14
-
Cadent iTero. This system also uses visible light to scan single teeth or a whole dental arch.15
Other systems create scans from plaster or stone models of the mouth, usually in the dental laboratory and include:
-
Cercon Ceramics (DeguDent, Dentsply International Co., Germany). This system comprises a non-contact laser scanner
-
Everest (KaVO, Lake Zurich, IL, USA). This laboratory based system uses a visible light system with structured light projection
-
Incise (Renishaw, Gloucestershire, England). This is a contact probe system
-
Procera (Nobel Biocare, Göteborg, Sweden). This is also a contact probe system.
It can be seen that using these modern CAD/CAM systems, the geometry of the teeth, be it within the clinic or laboratory, can be digitised either using contact methods, such as coordinate measuring machines (CMMs) or non-contact methods (laser and optical scanners). For fixed prosthodontic treatment, laser, visible light or infrared scanners are used, predominantly in the clinical environment, for scanning the tooth preparation. Contact scanners are used exclusively in the laboratory setting, where the technician scans a die that has previously been cast in stone. An example of a contact probe scanner is the Renishaw Incise system, where a ruby ball contact probe scans the model surface in order to render a 3D computerised image. Using the data generated, a zirconia crown coping is then directly milled from a zirconia blank. An example of a non-contact optical method is the Cerec 3 system. In this case the tooth surface is directly scanned in the mouth using infrared radiation, which is reflected back from the tooth surface and detected by a charged couple device (CCD). Since the surfaces of enamel and dentine have differing degrees of reflectance with infrared light, the tooth is pre-treated with titanium dioxide powder prior to scanning. The 3D image is then used to mill ceramic restorations at the chairside.
CAD/CAM technology has a number of actual, or at least potential, advantages when compared to traditional indirect dentistry. These include:16
-
No impression taking or casting, thereby reducing the number of manufacturing steps, which may improve the dimensional accuracy of the final restoration
-
Direct chairside fabrication of various types of restoration in one appointment without the need for a provisional restoration. This not only improves the likely fit of a restoration, but also means the ever-present risk of loss or damage to a provisional restoration is removed
-
Reduced laboratory and chairside costs. However, there is the initial expenditure on the CAD/CAM equipment to consider, which may be very high.
Both contact and non-contact scanners can also be used to monitor and quantify tooth surface loss over time. For example, accurate impressions can be used to create stone models, which can then be scanned using a contact probe, laser or visible light. In this way surface loss due to attrition, abrasion or erosion can be quantified both linearly and volumetrically, provided there are stable reference points available.17,18
3D imaging in orthodontics
Within orthodontics, electronic 3D imaging has several potential and current applications. The most obvious is as a substitute for conventional plaster study models. These models are used not only for initial diagnosis, but also as a means of monitoring treatment progress, as a reference against which archwires can be fabricated, as a demonstration of quality of outcome and as a medico-legal record. In the latter case 3D records are likely to be acceptable to the court provided there is a suitable audit trail to show that such an image has not been tampered with/manipulated, although a legal precedent is perhaps yet to be set.
Digital study models are commercially available from several companies. One such company, OrthoCAD (Cadent, Fairview, NJ, USA) creates digital images of dental casts using an optical scanner. To obtain the images, the orthodontist sends alginate impressions and a wax bite to the OrthoCAD laboratory. These are then converted into 'plaster equivalents' for scanning and the scanned images are stored on the company's server for accessing by the orthodontist.19 They are useful for routine measurement of tooth size, overjet, overbite and for Bolton analyses. The accuracy of digital study models relative to conventional plaster models has been the subject of a previous investigation. Although digital models were not found to be as accurate as the plaster models for certain measurements, eg tooth size and overbite, the differences are thought probably to be insignificant during routine clinical use.20
Electronic 3D imaging can also be used for facilitating accurate bracket positioning, for wire bending and in appliance fabrication. Examples of the latter include the OrthoCAD iQ system, where conventional orthodontic brackets are positioned on the digital models, and positioners are fabricated to allow transfer of the brackets to the patient's mouth for indirect bonding. Ormco's Insignia™ system provides brackets with positioning jigs as well as custom made archwires. Here the digital images are created by a combined destructive process whereby patient models are sectioned into thin slices (typically 0.001' to 0.006' thick)21 and each slice is laser scanned to provide data to reconstruct a 3D image of the dental arch. A similar technique, but this time using non-destructive laser scanning, is used in the fabrication of the lingual Incognito™ appliance (TOP Service für Lingualtechnik, GmbH). Here, custom made lingual appliances are computer generated on the digital models and then engineered in wax, before finally being cast in gold alloy for placement in the mouth. The archwires to be used during treatment are also fabricated using the same electronic data to fit this customised appliance.22
Although digital models are created in the above techniques, they are still made by laser scanning models that have been cast from the patient's impressions. In the Suresmile technique (OraMetrix, Inc, Texas, USA), appliance and archwire fabrication uses either a direct optical scan of the mouth, which can take up to 45 minutes, or a scan of plaster models. The latter method has the advantage of saving clinical time, but it inevitably requires additional dental laboratory time. Newer systems are currently being developed that are likely to substantially reduce this scanning time, making routine digital image acquisition rather than conventional impression taking a reality.
There is currently a high demand for more aesthetic orthodontic appliances and to try to accommodate this, Align Technology (Santa Clara, CA, USA) reintroduced the concept of a series of transparent tooth positioners to treat malocclusion. Developed in the late 1990s, the process involves creating positioners using stereolithography, directly from digital images. These images are created by CT (computed tomography) X-ray scanning the dental impressions, which eliminates the need for creating plaster models for subsequent imaging. It has been reported that digital study models with a spatial resolution in the order of 45-50μm can be constructed using this CT scanned impression approach.23 However, the disadvantage of CT scanning is the expense of the equipment and the time taken to acquire the image.
Electronic 3D imaging of the face also has a role in orthodontics. The concept of using such 3D images in orthodontic diagnosis has been around for over 60 years. Thalmann-Degen24 and Burke and Beard25 used stereophotogrammetric technology to create contour maps of the face, not only to aid diagnosis, but also to record changes in facial morphology as a result of growth.26 3D facial imaging might be useful in orthodontics in monitoring the effects of treatments such as functional appliances and assessing the effects of extractions as part of orthodontic fixed appliance therapy.
Orthognathic and craniofacial surgery
Three-dimensional facial surface scanning has been used in orthognathic and craniofacial surgery to aid diagnosis, to help monitor the short and long term effects of surgery and to assist in facial reconstruction.27 The scanners are either laser-based, or stereophotogrammetric using structured light. In the latter instance two or more digital cameras are used to capture the images from which a 3D facial reconstruction is made, with the images being acquired in milliseconds and in full colour. An example of the latter is the 3dMDface™ System (3dMD, London, UK). The original laser systems used in facial imaging, as described by Moss,28 were slow at image acquisition, taking up to 20 seconds and with a reported accuracy of 0.5 mm. More recently systems such as the Konica-Minolta laser scanners, which are slit laser scanners rather than point lasers, are accurate to within 50 μm and have much shorter scan times of 0.3 seconds.
In diagnosis, such 3D facial imaging can be used to help simulate the effects of orthognathic surgery on facial aesthetics and thereby help in surgical planning, particularly in combination with x-ray CT scanning. However, some care needs to be exercised when using the 3D images, particularly when demonstrating to a patient the likely effects of any proposed surgery. It may unreasonably raise expectations as to the final surgical outcome. In this respect, it is best to accept that the 3D image is used to simulate rather than predict facial change.29 This arises not as a result of the 3D imaging technique, but because there is an inherent difficulty in being able to predict, with any degree of accuracy, the soft tissue changes as a result of surgically moving the underlying hard tissues.30,31
Since 3D scanning enables not only linear measures of outcome of orthognathic surgery to be determined, but also volumetric changes, it means that the effect of factors such as post operative period and differing pharmacological interventions on facial swelling following surgery can also be assessed.32,33
Where patients require facial reconstruction after tissue loss, as a result of trauma or malignancy, 3D scanning techniques can be used to map the area of deformity, mirror the area from the unaffected opposite side of the face and via rapid prototyping, recreate a facial prosthesis.34
Summary
It is easy to assume that high technology, high cost equipment will give a true and accurate representation of the original. Although hardware and software are improving all the time, it should be remembered this is not necessarily always the case. The data acquisition, however good and by whatever means, creates a discrete set of co-ordinates or data points and as such there will always be spaces between these points. Computer software, in the form of reverse engineering packages such as Imageware, will then attempt to create a virtual best fit surface to those data points and as such the surface created cannot be absolutely accurate. However, advances in technology are enabling 3D images to be captured with sufficient rapidity and precision that the clinical applications of such technology are surely set to increase further over the next few years.
References
Chen F, Brown G M, Song M . Overview of three-dimensional shape measurement using optical methods. Opt Eng 2000; 39: 10–22.
Yue H-M, Su X-Y, Liu Y-Z. Fourier transform profilometry based on composite structured light pattern. Opt Laser Technol 2007; 39: 1170–1175.
Zhang L, Alemzadeh K . A 3-dimensional vision system for dental applications, 29th Annual International Conference of the IEEE. Engineering in Medicine and Biology Society, 2007.
Schreiber W, Notni G . Theory and arrangements of self-calibrating whole-body three-dimensional measurement systems using fringe projection technique. Opt Eng 2000; 39: 159–169.
Kim L, Sukhatme G S, Desbrun M . A haptic-rendering technique based on hybrid surface representation. IEEE Comput Graph Appl 2004; 24: 66–75.
Stander B T, Hart J C . Guaranteeing the topology of an implicit surface polygonization for interactive modelling. Proceedings of the 24th annual conference on computer graphics and interactive techniques, 1987. pp 279–286.
Fabio R . From point cloud to surface: the modeling and visualization problem. International Archives of Photogrammetry, Remote Sensing and Spatial Information Sciences, Vol. XXXIV-5/W10. International Workshop on Visualization and Animation of Reality-based 3D Models. pp 24–28. Tarasp-Vulpera, Switzerland, February 2003.
Imageware. http://www.ugs.com/products/nx/imageware/
Mehl A, Gloger W, Kunzelmann K H, Hickel R . A new optical 3-D device for the detection of wear. J Dent Res 1997; 76: 1799–1807.
Williams A G, Rekow D . The Switzerland and Minnesota developments in CAD/CAM. J Dent Pract Adm 1987; 4: 50–55.
Persson A, Andersson M, Oden A, Sandborgh-Englund G. A three-dimensional evaluation of a laser scanner and a touch-probe scanner. J Prosthet Dent 2006; 95: 194–200.
Nakamura T, Dei N, Kojima T, Wakabayashi K . Marginal and internal fit of Cerec 3 CAD/CAM all-ceramic crowns. Int J Prosthodont 2003; 16: 244–248.
Tsitrou E A, Northeast S E, van Noort R. Evaluation of the marginal fit of three margin designs of resin composite crowns using CAD/CAM. J Dent 2006; 35: 68–73.
http://solutions.3m.com/wps/portal/3M/en_US/LavaCOS/3MESPE-LavaCOS/HowItWorks/
Palin W, Burke F J . Trends in indirect dentistry: 8. CAD/CAM technology. Dent Update 2005; 32: 566–572.
Bartlett D W, Blunt L, Smith B G . Measurement of tooth wear in patients with palatal erosion. Br Dent J 1997; 182: 179–184.
Heintze S D, Cavalleri A, Forjanic M, Zellweger G, Rousson V . A comparison of three different methods for the quantification of the in vitro wear of dental materials. Dent Mater 2006; 22: 1051–1062.
Joffe L . OrthoCAD: digital models for a digital era. J Orthod 2004; 31: 344–347.
Santoro M, Galkin S, Teredesai M, Nicolay O F, Cangialosi T J . Comparison of measurements made on digital and plaster models. Am J Orthod Dentofacial Orthop 2003; 124: 101–105.
Chisti M Z K, Benton P A . Teeth Viewing System. 2001 US Patent 313290.
Wiechmann D . Nesbit L. iBraces/Incognito Clinical Guide Version 2. Incognito by TOP-Service GmBH 2007.
Baumrind S, Carlson S, Beers A, Curry S L et al. Using three-dimensional imaging to assess treatment outcomes in orthodontics: a progress report from the University of the Pacific. Orthod Craniofac Res 2003; 6: 132–142.
Thalmaan Degen P . Die Stereophotogrammetrie ein diagnostisches Hilfsmitte in der Kieferorthopaedie. Doctoral Dissertation, University of Zurich, 1944.
Burke P H, Beard F H . Stereophotogrammetry of the face. A preliminary investigation into the accuracy of a simplified system evolved for contour mapping by photography. Am J Orthod 1967; 53: 769–782.
Burke P H . Serial stereophotogrammetric measurements of the soft tissues of the face. A case of a girl with mild facial asymmetry from 3 weeks to 10 years of age. Br Dent J 1983; 155: 373–379.
Kimoto K, Garrett N R . Evaluation of a 3-D digital photographic imaging system of the human face. J Oral Rehabil 2007; 34: 201–205.
Moss J P . Northcroft revisited. Br J Orthod 1989; 16: 155–167.
Smith J D, Thomas P M, Proffit W R . A comparison of current prediction imaging programs. Am J Orthod Dentofacial Orthop 2004; 125: 527–536.
Csaszar G R, Bruker-Csaszar B, Niederdellmann H . Prediction of soft tissue profiles in orthodontic surgery with the Dentofacial Planner. Int J Adult Orthodon Orthognath Surg 1999; 14: 285–290.
Eckhardt C E, Cunningham S J . How predictable is orthognathic surgery? Eur J Orthod 2004; 26: 303–309.
Day C J, Robert T . Three-dimensional assessment of the facial soft tissue changes that occur postoperatively in orthognathic patients. World J Orthod 2006; 7: 15–26.
Kau C H, Cronin A, Durning P, Zhurov A I et al. A new method for the 3D measurement of postoperative swelling following orthognathic surgery. Orthod Craniofac Res 2006; 9: 31–37.
Ciocca L, Scotti R . CAD-CAM generated ear cast by means of a laser scanner and rapid prototyping machine. J Prosthet Dent 2004; 92: 591–595.
Simonite T . Robot jaws to get a human bite. NewScienceTech website 2008 January 3. http://technology.newscientist.com/channel/tech/dn13133-robot-jaws-to-get-a-human-bite.html
Acknowledgements
The authors would like to thank Mr Rupert Hoppenbrouwers of the DDU for his advice in the preparation of this manuscript and Hovick Boughosyan for his help with the images.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed paper
Rights and permissions
About this article
Cite this article
Ireland, A., McNamara, C., Clover, M. et al. 3D surface imaging in dentistry – what we are looking at. Br Dent J 205, 387–392 (2008). https://doi.org/10.1038/sj.bdj.2008.845
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2008.845
This article is cited by
-
Removable orthodontic retainers: practical considerations
British Dental Journal (2021)
-
Accuracy of CAD/CAM-fabricated bite splints: milling vs 3D printing
Clinical Oral Investigations (2020)
-
Robotic-Assisted 3D Bio-printing for Repairing Bone and Cartilage Defects through a Minimally Invasive Approach
Scientific Reports (2019)
-
Validation of a new three-dimensional imaging system using comparative craniofacial anthropometry
Maxillofacial Plastic and Reconstructive Surgery (2017)
-
CAD/CAM-Technologien in der Zahnmedizin
Stomatologie (2015)