Abstract
Decision-making regarding healthcare expenditure hinges heavily on an individual's health status and the certainty about the future. This study uses data on propensity of general health exam (GHE) spending to show that despite the debate on the necessity of GHE, its objective is clear—to obtain more information and certainty about one’s health so as to minimise future risks. Most studies on this topic, however, focus only on factors associated with GHE uptake and overlook the shifts in behaviours and attitudes regarding different levels of cost. To fill the gap, this study analyses a dataset of 2068 subjects collected from Hanoi (Vietnam) and its vicinities using the baseline-category logit method. We evaluate the sensitivity of Vietnamese healthcare consumers against two groups of factors (demographic and socioeconomic-cognitive) regarding payment for periodic GHE, which is not covered by insurance. Our study shows that uninsured, married and employed individuals are less sensitive to cost than their counterparts because they value the information in reducing future health uncertainty. The empirical results challenge the objections to periodic health screening by highlighting its utility. The relevance of behavioural economics is further highlighted through a look at the bounded rationality of healthcare consumers and private insurance companies in using and providing the service, respectively.
Similar content being viewed by others
Introduction
Attempts to dissect healthcare service expenditures as part of some behavioural trends are often obscured by the fact that individual behaviours occur under specific conditions and with private information and assessment. This study looks into the data of a specific healthcare spending: general health examinations (GHE). While it seems rational to regularly check one’s health to timely deal with the onset of an unexpected illness, the practice of periodic GHE is a rather modern phenomenon. The beginning of GHE could be traced back to the British physician Horace Dobell in 1861 when he sought a measure to monitor the health status of patients with tuberculosis (Dobell, 1961). Over the past two centuries, despite our intuition that regular health screenings could help prevent certain illnesses, studies have shown mixed results about their effects (Mehrotra and Prochazka, 2015; Ponka, 2014; Himmelstein and Phillips, 2016). The existing literature on the topic has also skewed toward Western practice of GHE, its limitations and benefits, and in turn, leaves an unfilled gap for research on this matter in developing countries such as Vietnam. This paper examines the case of Vietnam, an emerging economy where about 80% of its population of nearly 100 million have health insurance (Vietnam Plus, 2017). The analysis focuses on the sensitivity of Vietnamese healthcare consumers’ willing payments for GHE against two groups of factors, namely demographic and socioeconomic-cognitive, as this service is not covered by Vietnam’s health insurance (International Cooperation Department, 2017). Although the study is limited in its geographical scope, it nonetheless seeks to shed light on the behaviours of healthcare consumers in general when thinking about measures to minimise future risks.
Literature review
This section will look into the controversial nature of periodic GHE, the literature in developing countries and in Asia, the reason why Vietnam is chosen for the study, and the framework for identifying factors affecting consumer health behaviour.
On periodic GHE
Studies objecting to periodic GHE often point to (i) its high costs, (ii) the resulting wasted time and resources, (iii) its inconclusive support for reducing morbidity or mortality, and (iv) non-evidence-based approach (Kast et al., 2004; Merenstein, Daumit and Powe, 2006; Krogsbøll et al., 2012; Howard-Tripp (2011); Coffield et al., 2001; Thrall, 2009; Schäfer et al., 2012; Trogdon and Hylands, 2008; Yarnall et al., 2003). One of the most long-standing studies on routine general checkups is carried out in Canada where the practice has been discouraged and even abandoned since 1979 due to poor evidence on its effectiveness (Canadian Medical Association, 1979; MacMillan, MacMillan and Offord, 1993; Thombs, Lewin, and Tonelli, 2017).
Although it is worth noting that resources could be allocated to higher-quality medical services instead of the periodic GHE (Hayward et al., 1991; US Public Health Service (1994)), there are proven benefits to this kind of health screening. First, regular check-ups help facilitate patient-physician relationship, raising mutual trust and potentially contributing to positive health outcomes (Ponka, 2014; Kelley et al., 2014). Second, the service may assist marginalised groups that would otherwise miss out on regular health screening (Ponka, 2014). Third, it reduces patient anxiety and provides physicians with evidence-based preventive measures, such as early detection of risk factors and a more updated patient profile over time (Fletcher, 2007; Lin et al., 2011; Duerksen, Dubey and Iglar, 2012; Kermott et al., 2012). Another outcome often attributed to routine health check-ups is higher rates of cervical cancer screening, faecal occult blood testing, and cholesterol screening (Boulware et al., 2007), as well as new diagnoses that could have been missed or delayed (Himmelstein and Phillips, 2016).
Regular health screening in developing countries and Asia
In recent years research on periodic health screening has also emerged in developing countries and in Asia, with many studies analysing factors influencing consumer health behaviour. Participation in regular health exams among Brazilian women was linked to four factors, namely being younger than 40 years old, having higher educational level, having private health insurance and being married (Leal et al., 2005). Meanwhile, in Saudi Arabia where healthcare is free of charge, six factors were found to increase the likelihood of receiving periodic GHE, including high age, education, being married, daily consumption of fruits and vegetables, diagnoses of diabetes, and a clinic/hospital visit for injury/illness within the past two years (El Bcheraoui et al., 2015). A study on health screening behaviour among Singaporeans similarly named low education and income levels as two factors associated with low uptake of periodic GHE (Wong et al., 2015). The results were also confirmed in a study in South Korea, such that both demographic (gender, age) and socioeconomic attributes (education, income, health status, living habits) are strongly linked to the willingness to take a physical exam (Yeo and Jeong, 2012). In terms of occupation, Chinese civil servants and retired government officials were reported to have more frequent annual physical exams than farmers, especially the elderly, due to their better health knowledge (Sun et al., 2014). In South Korea, a recent study found workers at enterprises with more than 300 employees are more likely to participate in the national GHE than those at enterprises with fewer than 50 employees (Kang et al., 2017).
Another line of research in Asia looks for the impacts of a periodic checkup, such as improved healthcare utilisation in the short term in Japan (Ren, Okubo and Takahashi, 1994), increased surgical treatment for uterine fibroids in Chinese women (Wu, Yang and Zhou, 2010), higher hepatitis B vaccine uptake in Hong Kong (Chan et al., 2009), positive lifestyle changes in South Korea (Son et al., 2012; Yeo and Jeong, 2012), and higher likelihood of early treatment of some target diseases in Taiwan (Lin et al., 2011). For the large part, the literature of GHE in Asia seems to focus more on the effects of early examination toward a specific disease in a specific demographics, with cancer screening the most prevalent (Tang, Solomon, and McCracken, 2000; Yeoh, Chew, and Wang, 2006; Mehrotra, Zaslavsky and Ayanian, 2007; Domingo et al., 2008; Kim et al., 2011; Koo et al., 2012; Siew and Sunny, 2013).
Why Vietnam
It is important to point out that much of the literature on periodic health screening, whether in the West or Asia, has left out the cost of the medical service itself, with the exception of the service being free or covered by insurance in some cases (El Bcheraoui et al., 2015; Yeo and Jeong, 2012). Medical cost, as expected, may significantly determine people’s acceptance of periodic GHE (Oboler et al., 2002). This study for the first time seeks to evaluate the sensitivity to periodic GHE cost of a group of consumers, particularly Hanoi (Vietnam), continuing the line of recent studies such as (Vuong and Nguyen, 2015; Vuong, 2015; Vuong, 2016a; Vuong, 2016b).
Vietnam, which has a young population and a low GDP per capita of approximately US$2,000, offers a case study of human behaviour in the healthcare sector of a developing Asian country. Vietnamese health consumers are facing increasingly common issues–higher medical costs and widening income inequalities–that, in the worst case, could push them to the point of destitution (Vuong, 2015; UNDP Vietnam, 2016). This happened as a result of the health sector reforms in the 1980s. Before Vietnam changed from a centrally planned economic system to a market-oriented one, state subsidies played a major role in its health system, with healthcare services and drugs free of charge. The deregulation of the medical system has since brought about massive changes in healthcare delivery, access and financing (Chaudhuri and Roy, 2008). One of the significant changes to health financing is compulsory health insurance for all citizens from 2008 (Do, Oh and Lee, 2014), although the coverage has reached only 81.7% of the population as of 2017 (Vietnam Plus, 2017). Universal coverage is envisioned in the next few years. However, despite insurance coverage, the introduction of user fees at both public and private facilities has led to a sharp increase in out-of-pocket (OOP) expenses (Chaudhuri and Roy, 2008). A recent study shows that the OOP cost is still so high that the current insurance package, though reduces the vulnerability to high healthcare costs, needs reforms (Nguyen et al., 2012).
Research on Vietnamese healthcare, therefore, has mostly considered the rising OOP expenditure as a major barrier to quality healthcare (Chaudhuri and Roy, 2008; Vu et al., 2016; Van Minh et al., 2013; Nguyen et al., 2012), and left out the personal expenditure for periodic health examinations. This study arises from the need to assess the case in Vietnam as that might present a typical barrier to anticipatory care for health consumers in developing countries today. This research contributes to the literature by increasing understanding of some of the demographic and socioeconomic-cognitive factors that influence individuals to follow or not follow regular health screening guidelines.
Identifying factors affecting human health decisions
Given the controversial nature of periodic health check-up, it is important to take into account factors that could affect the behaviour and attitude of people in considering this service’s cost. With low income as a strong predictor for the low participation in GHE (Wong et al., 2015; Yeo and Jeong, 2012, Dryden et al., 2012; Kuo and Lai, 2013; Sun et al., 2014; Nakanishi, Tatara and Fujiwara, 1996; Wong et al., 2015), this study excludes the income factor from the scope of the investigation, instead focusing on two groups of factors that might influence with the level of willing payments for this service. The first is demographic: sex, marriage and job status; the second is socioeconomic and cognitive: health insurance, perception toward public health status, and hesitation to take GHE due to distrust in healthcare quality (see Table 1). Below is a brief review of the research on the correlation between these factors and periodic health attendance.
In terms of sex, the majority of studies over the years have shown females to be more inclined to take regular physical examinations than males (Nupponen, 1996; Jepson et al., 2000; Wall and Teeland, 2004; Lai and Kalyniak, 2005; Cherrington, Corbie-Smith and Pathman, 2007; Dryden et al., 2012). Two studies (Hsu and Gallinagh, 2001; Karwalajtys et al., 2005) were found to exhibit no difference in GHE uptake by sex (Dryden et al., 2012). Notably, periodic GHE has been shown to have an obvious, positive impact for female patients on detecting and dealing with breast cancer and uterine fibroids (Yeoh, Chew and Wang, 2006; Domingo et al., 2008; Wu, Yang and Zhou, 2010). Yet, despite widespread fear of cancer, on the health-seeking practices of Vietnamese people, studies have noted the lack of knowledge, as well as irregular check-ups among local women concerning breast and cervical cancer (Pham and McPhee, 1992; McPhee et al., 1997; Domingo et al., 2008).
In terms of marriage, married people are shown to have a higher likelihood of participating in annual physical check-ups, as seen in both developing and developed countries (Lai and Kalyniak, 2005; Leal et al., 2005; El-Haddad et al., 2015). Similarly, in an extensive review of over 17,000 published papers on general health checks, Dryden et al., (2012) found that marital status is associated with higher GHE participation rates, especially among men. The effect of marital status on health screening participation could be explained by a spouse’s attempt to monitor the other’s health and encourage healthy behaviour (El-Haddad et al., 2015; Engebretson, Mahoney and Walker, 2005).
As for job status and related factors, lower attendance of periodic health exam is linked to low incomes, low educational level, and unemployment (Hsu and Gallinagh, 2001; Culica et al., 2002; Wong et al., 2015; Yeo and Jeong, 2012; Dryden et al., 2012; Sun et al., 2014). This is true on an intuitive level as people of higher socioeconomic status are more likely to experience better health status (Kuo and Lai, 2013; Sun et al., 2014; Agborsangaya et al., 2012). By contrast, not only do those with lower incomes often have substandard habitat and unhealthy living habits but they also have restricted access to healthcare services, including periodic GHE (Tucker and Clegg, 2002; Kuo and Lai, 2013; Sun et al., 2014; Nakanishi, Tatara and Fujiwara, 1996). They are more susceptible to diseases and run the risk of astronomical treatment costs that could be worse in case of no insurance (Tucker and Clegg, 2002; Lu and Hsiao, 2003; Wilper et al. 2009).
Given that health insurance is seen as a proxy for healthcare access, it could be a predictor of having had a recent medical check-up (Naimi et al., 2006). Health insurance has been shown to improve the efficiency of healthcare services usages and was especially beneficial for the poor who have demand for screenings and treatment (Finkelstein, 2002; Ross and Mirowsky, 2000; Meer and Rosen, 2004). In Vietnam, national health insurance has been shown to have limited success in reducing medical expenses (Nguyen, 2012; Nguyen et al., 2012). Of the studies on periodic GHE in both developing and developed countries, health insurance coverage is related to a higher probability of using this service (Culica et al., 2002; Yeo and Jeong, 2012; Leal et al., 2005).
The two cognitive factors used in this study, namely perception toward public health status and hesitation to take GHE due to distrust in healthcare quality, are based on the understanding that mutual trust and communications could affect health outcomes (Glantz et al. 2008; Jepson et al., 2000). Problems in the health system could diminish such trust. A large-scale review of patient safety and care quality in developing countries in Southeast Asia found four major concerns, namely (i) patient infection risk, (ii) medications errors, (iii) maternal and perinatal care quality, and (iv) the overall healthcare quality (Harrison, Cohen and Walton, 2015). In Vietnam where healthcare services are being privatised, researchers have noted how many public hospitals are focusing on reaching revenues target rather than improving services (Minh (2011); Cong and Mai, 2014). A study on tuberculosis treatment and management in Vietnam highlights the distrust of patients and their families in the quality of healthcare delivery, such that the lower levels and status of the healthcare system are associated with low trust (Johansson and Winkvist, 2002). Vietnamese patients are known to frequently doubt their physicians’ advice, and thus, fail to follow through on the treatment (Vuong and Nguyen, 2015). Such distrust could hold people back from participating in periodic health screening. Here, because the doctors rely on a one-size-fits-all examination, the patients could feel as though their doctors are not genuinely interested in their views. This presents an asymmetrical relationship: the patients by default are in a vulnerable position where their trust can be abused by the doctors (Djulbegovic and Hozo, 2012). In the case of periodic GHE, Hammond, Matthews, and Corbie-Smith (2010) confirmed in a study among African American men that high medical distrust, plus traditional masculine norms, reduced the likelihood of using this service.
This study will take into account the crisscrossing influences of the above factors over another in the decisions regarding the cost of periodic GHE in Vietnam.
Method
Research questions
This study sets out to answer the following three research questions (RQ):
RQ1. Given that health insurance, though mandatory in Vietnam, does not cover periodic health screenings, what are the probabilities of insured and uninsured health consumers willing to pay for this service? And what price level is the deal breaker?
RQ2. Is there empirical evidence to support the view that (i) perception of public health, (ii) trust in healthcare quality, (iii) job and (iv) marriage status influence the willingness of paying for periodic health checks?
RQ3. Is the likelihood of paying determined by the need for information and certainty about one’s health status?
Study design and variables
A data team of Vuong and Associates collected a total of 2068 observations from September to October 2016 through a randomised survey at various clinics, schools, companies and households in Hanoi and the surrounding areas. The final dataset, with its data descriptor approved by Nature Research (Vuong, 2017a), was also deposited in the Open Science Framework (Vuong, 2017b) and Harvard’s Dataverse (Ho, 2018).
To answer RQ1-3, the study uses two types of variables, dependent and independent variables, as described in Table 1 in the Results section. The categorisation of the dependent variable “AffCost”, which stands for Affordable self-paid cost for a periodic GHE, was based on the per capita health expenditure in Vietnam, which rose from US$14 in 1995 to US$86 in 2012 (Pham, 2016; Hoang et al., 2015).
Statistical analysis
Raw data was entered into MS Excel and saved as CSV files. Data manipulation and categorical structuring with multi-way contingency data tables were executed using R 3.3.1. The categorical regression technique using BCL models, specified in (Agresti, 2013a), was used for analyses. All dependent and explanatory variables in this article are discrete variables consisting of multiple categories. The multinomial logistic regression model was applied to evaluate the impact of the response variable, as well as their tendencies to change when the predictors change.
Logistic regression was used here for two reasons: (i) the model is comprised of predetermined number of variables, thus showing each variable’s significance more clearly; and (ii) explanations for estimated coefficients in empirical calculations can be acquired directly. Moreover, the BCL model can provide all odds ratios simultaneously between baselines and other categories.
The general equation of the baseline-categorical logit model is:
n which \({\mathbf{x}}\) is the independent variable; and \(\pi _j\left( {\mathbf{x}} \right) = P\left( {Y = j|{\mathbf{x}}} \right)\) its probability. Thus \(\pi _j = P\left( {Y_{ij} = 1} \right)\) with Y being the dependent variable. In the logit model in consideration, the probability of an event is calculated as:
with \(\mathop {\sum}\nolimits_j {\pi _j\left( {\mathbf{x}} \right) = 1}\); \(\mathop {\sum}\nolimits_j {\alpha _j} = 0\); and \(\mathop {\sum}\nolimits_j {\beta _j} = 0\); in which \(n\) is the number of observations in the sample, \(j\) the categorical values of an observation \(i\), and \(h\) a row in basic matrix \({\mathbf{X}}_i\).
Estimated probabilities can be used to predict the possibilities of the person’s expenditure for a periodic GHE (low, medium, high) in certain conditions of such socio-economic and demographic variables (Vuong, 2015; Vuong, 2016a; Agresti, 2013b).
Estimated coefficients were computed through multi-variable logistic regression and were used to calculate empirical probabilities (Agresti, 2013b; Vuong, Napier and Tran, 2013; Vuong and Nguyen, 2017; Vuong, Nguyen and Vuong, 2017). The z-value and p-value indicate statistical significance of predictor variables in the models, with \(p < 0.05\) being the conventional level of statistical significance required for a positive result (Vuong, Napier and Tran, 2013).
Results
Descriptive statistics
During the data survey, one in six persons refused to be interviewed for questionnaires. There are more females than males in the sample (64.80% vs. 35.2%). Married individuals and those with stable jobs accounted for a higher proportion (57.35% and 54.30% respectively) among participants. Due to health insurance being compulsory, 82.21% reported to be insured.
As shown in Table 1, the majority of respondents have a positive attitude toward medical service quality: 73.21% of them do not have any hesitation toward GHE. Regarding respondents’ perceptions toward public health status, “bad” (problematic) is the most-received answer (36.22%), mostly with environmental pollution and hygiene and food safety issues cited as reasons. With respect to an acceptable charge for a periodic GHE participation, lower than VND2mn is the most favoured answer (86.32%).
Estimation probability of willing payments for GHE against socioeconomic and cognitive factors
Estimation
Employing logistic regression estimations with the dependent variable “AffCost” against three independent variables “HealthIns”, “HesitateTrustHq” and “CHPerc”, the results are reported in Table 2.
Table 2 shows that most estimated coefficients are statistically significant, implying correlations between the three socio-economic factors mentioned above and the acceptable cost of periodic GHE.
However, since not all of estimated coefficients are statistically significant, the goodness-of-fit test is used to ensure more solid conclusions. The estimated multi-way contingency table (Supplementary Table A in Supplementary file) shows that all fitted counts are larger than 5; coupled with a reasonable sample size, \(G^2 = 2{\sum} {{\mathrm{observed}}\left[ {\ln \left( {{\textstyle{{{\mathrm{observed}}} \over {{\mathrm{fitted}}}}}} \right)} \right]}\) is deduced to have an approximate χ2 distribution (Agresti, 2013a, b; Vuong, Nguyen and Vuong, 2017).
Considering the null hypothesis H0: \({\mathbf{\beta }}_i = {\mathbf{0}}\), P-value is computed as follows:
Although the P-value = 0.179 does not present a fantastic goodness-of-fit, when combining with 6 out of 8 highly significant coefficients, the specification is still reasonable well fitted for further consideration. That means the model, albeit imperfect, is still worthwhile for considering the following empirical observations.
Regression equations are constructed depicting relationships between the response variable and the predictor variables as follows:
Interpretations
One remarkable aspect revealed in the analysis was the subtle changes in the behaviour and attitude of Vietnamese healthcare consumers when the cost shifts from low to high even by a mere VND1mn (about US$45). Here we draw out some interesting patterns of behaviour.
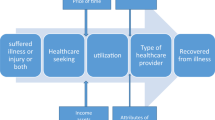
First, Fig. 1 summarises the changes in probabilities of customers’ willing payments when controlling the factors: health insurance, perception toward the state of public health, and hesitation due to mistrust in healthcare quality (Supplementary Table B). The results answer RQ1 by highlighting two points clearly. First, when the cost is high, the likelihood of paying for GHE is low (<24%), signalling that VND2mn might be the deal breaker. Second, insured individuals are more willing to pay for a periodic health check when the cost is low while the opposite is true for uninsured individuals, with the differences in probability ranging between 5 and 8 percentage points in both cases.
A diagram of decision-making by health consumers at different GHE price levels under two cases, with and without health insurance. A: Insured health consumers are more likely to pay for GHE when the cost is low. B: Uninsured health consumers, by contrast, are more inclined to pay for GHE even when the cost is high
This pattern of behaviour seems counterintuitive on the surface, yet, is in fact understandable given that Vietnamese national health insurance does not cover the cost for GHE but for clinical examination and treatment (International Cooperation Department, 2017). In this context, the insured are certain about being covered in case they have some health problems; hence, they tend to be more comfortable with paying at the low cost for a general health check-up. This certainty about having a guarantee for illness treatment later, however assuring it might feel, in no way reduces the risks of a health crisis. Thus, the attitude of insured people in this case shows a level of bounded rationality (Editorial, 2017). On the other hand, the uninsured tend to be more willing to pay for more expensive health screening likely because they are seeking information about their health status to minimise the risks concerning their future health.
While the result here reflects the behaviour of a specific region of Vietnam, this attitude, in closer examination, helps explain the rationality in the conventional practice of private insurance providers—inviting potential insurance buyers to take a GHE at designated places for free. In terms of information economics, such measure allows the insurance companies to gain information about their potential customer’s health and ensure profitability. This interpretation refutes the viewpoint that GHE has no value (Kast et al., 2004; Nupponen, 1996; Merenstein, Daumit and Powe, 2006).
In addition, as shown in Fig. 2, cognitive factors such as perception of public health and the distrust in healthcare service are both associated with the shifts in the willingness to pay for GHE. This result, addressing RQ2, is observed in both the insured and uninsured, although Fig. 2 presents only cases of the insured. Here, Fig. 2a shows the probabilities of high and medium spending increase with the trust in healthcare service quality, while it is the opposite for the low cost. For perception toward public health, Fig. 2b shows that the probability of low spending increases when the view shifts from “bad” to more favourable, while the probabilities of medium and high spending decrease. Details of probabilities could be viewed in Supplementary Information, with Supplementary Tables A and B and Supplementary Figs. A, B, C, D.
a Probabilities of willing payments for a GHE among insured people who hesitate to take GHE due to distrust in healthcare service quality. Three lines represent the level of willing payments: low, medium and high. “Yes” and “No” are the answers to whether the subject of this study hesitates to take GHE due to distrust in healthcare quality. b Probabilities of willing payments for a GHE among insured people with different perceptions of the state of public health. Three lines represent the level of willing payments: low, medium and high. “Bad” and “Other” are the answers to whether they have a negative or positive view
Estimating probability of willing payments for GHE against demographic factors
Estimation
The same logistic regression procedures are applied to figure out the correlations between periodic GHE willing payments and three demographic factors: gender, job status and marital status. Table 3 displays the estimation results of logistic regression model among these above variables.
Using the goodness-of-fit test, the fitted contingency table is computed and presented in Supplementary Table C (all supplementary tables and figures are provided in the file: Supplementary Information.pdf).
P-value is calculated as: Pr(χ2(8) < 18.6811) = 0.017 (<0.05), suggesting a satisfactory goodness-of-fit for the model. This inference reinforces the associations between the above-mentioned variables which were reported in Supplementary Table C.
In the same manner, Eq. 13 and Eq. 14 are formed based on Table 3:
Distributions of probabilities of periodic GHE willing payments conditional upon gender, marital status and health insurance are presented in Supplementary Table D.
Interpretations
Similar to socio-economic and cognitive variables, however which demographic variables are controlled, the probability of willingness to spend more than VND2mn, the high range, is significantly lower than that of low and medium ranges (high-cost group: 7.6% to 20.4%; low-medium cost: 31.4% to 55.3%). This observation confirms the sensitivity to cost of Vietnamese healthcare consumers, specifically at a price above VND2mn.
The findings, as illustrated in Fig. 3, also answer RQ2 by showing how the willingness to pay for GHE changes when job status and marital status are taken into account. When the cost is “low”, non-married and unemployed people are more inclined to spend on GHE than married ones (by as many as 10 percentage points). In contrast, for the high cost, married and employed people are more likely to pay than their counterparts; the probability is about twice the probability of the without job and marriage group (16.7% vs. 7.6% in case of females; 20.4% vs. 9.5% for males). The results provide further empirical support for the existing literature on the influence of marital status on participation in regular health screenings (Lai and Kalyniak, 2005; Leal et al., 2005; El-Haddad et al., 2015; Dryden et al., 2012).
A diagram of decision-making by male and female health consumers at different GHE price levels under two cases, with and without job and marriage. C: In the case of low-cost GHE, the probability of paying for the service is higher among people without job and marriage than those with job and marriage. D: By contrast, in the case of high-cost, the probability of paying for GHE among people without job and marriage is lower than among those with job and marriage
This tendency of the people with a stable job and marriage being more comfortable with spending higher for GHE could be explained by the fact that these demographic factors are often associated with risk aversion (Halek and Eisenhauer, 2001; Spivey, 2010; Meyer and Meyer, 2005; Cressy, 2000). Consequently, they might seek out ways to hedge against future uncertainty of income discontinuity due to health reasons by taking periodic physical examinations. However, it is also possible that people with a stable job have better income and they are more tolerant of higher medical cost.
Discussion
Limitations
This paper faces a number of limitations as follows. First, due to the nature of the random sample, the analysis was not able to control for equivalent sizes of subgroups of respondents. Therefore, the results, despite being empirically verified, should be interpreted with caution, with particular attention on the skewness toward a younger population. Second, as the dataset does not reflect the numerical level of households/individual income, the categorical value, albeit useful and successfully modelled, may be somewhat broad for a more useful explanation, such as computing threshold values. Third, the study could not generalise the results beyond the specific region examined here—which is Hanoi and its vicinities.
Finally, the fourth shortcoming of this study lies in the possibility of applying other models to explain the health decisions here. Like a large body of research on periodic health screening, the study uses logistic regression to evaluate the association between certain factors and GHE attendance, with the unique focus on consumers’ sensitivity to service cost. Other studies opt to apply health behaviour theories, such as the health belief model (Becker, 1974), to explain the health screening participation (Parsa et al., 2006; Shiloh, Vinter and Barak, 1997). Another potential method is to apply game theory to evaluate the relationships between healthcare consumers and providers or between patients and insurers. For instance, three models of game theory, namely the Prisoner’s Dilemma, the Assurance game, and the Centipede game, were used to analyse the two-way interaction in a medical consultation (Tarrant, Stokes, and Colman, 2004). Agee and Gates (2013) applies game theory to predict that a healthcare market may undergo a price inflation if providers set prices for services autonomously and in a non-cooperative manner. As such, when all parties act in cooperative way, the results are lower administrative costs and higher profit margins for the providers and the insurers (Agee and Gates, 2013).
Implications
Nonetheless, given the imperative of understanding issues regarding public health and exploring necessary conditions for bringing more practical preventive medicine measures to the populace, these limitations are considered acceptable for now and should be overcome in future studies. What this study offers are unique insights from a developing country on how the specific pricing of a preventive medical service, in relations to various factors, could influence the decision-making of consumers.
The behaviour of consumers in this survey underlines how people value information or certainty about one’s health status differently. Through the statistical analysis, the study shows that the likelihood of paying is indeed determined by the need for information and certainty (RQ3). In the three cases examined here, the uninsured, married, and employed all seek to stay updated on their physical conditions, and thus, are more willing to pay a higher price for a physical check-up. In economics terms, they are more risk averse than their counterparts due to the justifiable fears of future uncertainty. For example, in case of an unexpected illness, people in these groups will likely face a higher cost, whether that be an expensive hospital bill or disruption to the existing job and lifestyle. Along this line of behavioural economics (Editorial, 2017), the study also explores the connection through bounded rationality between the spending and providing behaviours of healthcare customers and private insurance companies. Here, both sides seek to gain information about health status that could help them lower future risks – either an unexpected sickness or a low profit from a costly medical bill. The rational behaviours of two independent parties who have different interests are harmonised through optimising the value of information. These insights present an often-underappreciated value of general health screening and clearly provides an evidence against the view that the practice is a waste of resources (Kast et al., 2004; Nupponen, 1996; Merenstein, Daumit and Powe, 2006; Krogsbøll et al., 2012; Howard-Tripp (2011); Coffield et al., 2001; Thrall, 2009).
The results, therefore, have certain implications for improving health outcomes. Healthcare providers should reconsider the pricing of GHE so as to encourage timely preventive medical practice, as well as to help reduce the out-of-pocket payment. On how pricing could carry certain meanings for consumers, the World Bank (2014) cited a study by Kremer and Glennerster (2011) which shows the willingness of people to adopt many health goods at a price of zero (or almost zero) and their complete hesitation when prices edge up above zero.
In the case of Vietnam, particularly the metropolis of Hanoi and its surrounding neighbourhood, because a general health check is not fully covered by insurance, any service that is priced at VND2mn or higher may be unaffordable for many people. This is understandable given the monthly income per capita in Vietnam’s urban region was VND4.37mn in 2016 (versus VND3.05mn across the country) (General Statistics Office of Vietnam Health (2018)), a level on par with other developing countries. Reducing the prices of routine health check-ups for Vietnamese consumers could encourage more people, especially the low-income, to take up the service.
For future research direction, it is important to empirically verify and measure influences of socio-economic and demographic factors on GHE in relations to plausible and implementable employment policies and trends of working environment. Moreover, results from different geographical regions are necessary for further research. Such a research attempt would require a significantly larger dataset reflecting different geographical, socio-economic and cultural traits.
Conclusion
The results in this study challenge the usual objections to periodic health screening by highlighting its utility through a number of sensitivity level analyses. In short, the first major finding here is the cost level that is highly sensitive to Vietnamese healthcare consumers. Based on the results, the majority of respondents became very reluctant to pay for a health service equal to or above VND2mn (about US$90).
The study also suggests some factors that could raise the spending willingness of healthcare consumers. Regarding demographic factors, the study confirms that people with different marital and job statuses diverge in their views on healthcare expenditure. Other studies have suggested job and marriage increase the probability of GHE participation (Lai and Kalyniak, 2005; Leal et al., 2005; El-Haddad et al., 2015; Sun et al., 2014; Culica et al., 2002), in this study, we show that stable jobs and marriage could raise the probabilities of higher spending for this service.
Regarding socioeconomic-cognitive factors, studies in the past have shown how the trust in healthcare quality and health insurance coverage could influence the uptake of GHE (Naimi et al., 2006; Culica et al., 2002; Yeo and Jeong, 2012; Leal et al., 2005), this study confirms the effect of these factors on consumers’ spending attitude. Here, distrust in healthcare quality and favourable perception toward public health status could both reduce the likelihood of spending for GHE at the medium or high range (>VND1mn or about US$45). Thus, in order to encourage frequent general health screenings, besides lowering prices, service providers and public health policymakers should seek to reduce consumers’ concerns about the healthcare quality and improve the image of public health status. More importantly, the statistical analysis shows that uninsured people, those without the certainty that they are covered when there are health problems, tend to be less sensitive to cost as they seek information to reduce the uncertainty about their future health risks. This has provided a clear value of periodic GHE—a means to obtain more information about one’s physical condition and thereby minimise future risks.
Finally, in the wake of any public health crisis, the results of this study suggest policymakers highlight the value of information—for instance, awareness of the disease, knowledge one’s physical conditions and the neighbourhood’s—through targeted ads campaigns. Understanding that people often make decisions in an instinctive or ‘heuristic’ manner is the key to improve the effectiveness of public health policies. There has been a similar suggestion in this regard, calling for public health to promote approaches that demand little or no effort as humans are effort minimisers (Hallsworth, 2017; Editorial, 2017). In addition, given that humans naturally crave situations with certainty, when targeting the more risk averse group, another suggestion is to emphasise the utility of a service instead of the perceived loss. Researchers have confirmed that presenting the information as gain-framed messages (“If you regularly examine your health, you will gain more information about your health and be more certain about your future”), rather than loss-framed messages (“If you do not regularly examine your health, you will lack the information about yourself and face more uncertainty later), is effective in nudging people to adopt preventive behaviours (World Bank, 2014). In any cases, what should always be encouraged is for both the patients and physicians to engage in shared and informed decision making.
Data availability
The description of how the datasets of this study were generated and processed could be found at (Vuong, 2017a). The complete datasets could be found in Open Science Framework: https://osf.io/afz2w/ and Harvard Dataverse: https://doi.org/10.7910/DVN/CWHOIC.
References
Agborsangaya CB, Lau D, Lahtinen M, Cooke T, Johnson JA (2012) Multimorbidity prevalence and patterns across socioeconomic determinants: a cross-sectional survey. BMC Public Health 12(1):201. https://doi.org/10.1186/1471-2458-12-201
Agee MD, Gates Z (2013) Lessons from game theory about healthcare system price inflation. Appl Health Econ Health Policy 11(1):45–51
Agresti A (2013a) Categorical data analysis, 3rd edn. Wiley, Hoboken, New Jersey
Agresti A (2013b) Modeling ordinal categorical data. http://www.stat.ufl.edu/~aa/ordinal/agresti_ordinal_tutorial.pdf Accessed 4 Feb 2018
Becker MH (1974) The health belief model and sick role behavior. Health Educ Monogr 2(4):409–419
Boulware LE, Marinopoulos S, Phillips KA, Hwang CW, Maynor K, Merenstein D, Wilson RF, Barnes GJ, Bass EB, Powe NR, Daumit GL (2007) Systematic review: the value of the periodic health evaluation. Ann Intern Med 146(4):289–300
Canadian Medical Association (1979) The periodic health examination. Canadian Task Force on the Periodic Health Examination. Can Med Assoc J 121(9):1193–1254
Chan OK, Suen SS, Lao TT, Leung VK, Yeung SW, Leung TY (2009) Determinants of hepatitis B vaccine uptake among pregnant Chinese women in Hong Kong. Int J Gynecol Obstet 106(3):232–235
Chaudhuri A, Roy K (2008) Changes in out-of-pocket payments for healthcare in Vietnam and its impact on equity in payments, 1992–2002. Health Policy 88(1):38–48
Cherrington A, Corbie-Smith G, Pathman DE (2007) Do adults who believe in periodic health examinations receive more clinical preventive services? Prev Med 45(4):282–289
Coffield AB, Maciosek MV, McGinnis JM, Harris JR, Caldwell MB, Teutsch SM, Haddix A (2001) Priorities among recommended clinical preventive services1. Am J Prev Med 21(1):1
Cong NT, Mai NT (2014) Service quality and its impact on patient satisfaction: an investigation in vietnamese public hospitals. J Emerging Econ Islamic Res 2(1), 1–13
Cressy R (2000) Credit rationing or entrepreneurial risk aversion? An alternative explanation for the Evans and Jovanovic finding. Econ Lett 66(2):235–240
Culica D, Rohrer J, Ward M, Hilsenrath P, Pomrehn P (2002) Medical checkups: who does not get them? Am J Public Health 92(1):88–91
Djulbegovic B, Hozo I (2012) When is it rational to participate in a clinical trial? a game theory approach incorporating trust, regret and guilt. BMC Med Res Methodol 12:85
Do N, Oh J, Lee JS (2014) Moving toward universal coverage of health insurance in Vietnam: barriers, facilitating factors, and lessons from Korea. J Korean Med Sci 29(7):919–925
Dobell H (1961) Lectures on the Germs and Vestiges of Disease: And on the Prevention of the Invasion and Fatality of Disease by Periodical Examinations; Delivered at the Royal Infirmary for Diseases of the Chest. John Churchill, London
Domingo EJ, Noviani R, Noor MR, Ngelangel CA, Limpaphayom KK, Van Thuan T, Louie KS, Quinn MA (2008) Epidemiology and prevention of cervical cancer in Indonesia, Malaysia, the Philippines, Thailand and Vietnam. Vaccine 26:M71–M79
Dryden R, Williams B, McCowan C, Themessl-Huber M (2012) What do we know about who does and does not attend general health checks? Findings from a narrative scoping review. BMC Public Health 12(1):723
Duerksen A, Dubey V, Iglar K (2012) Annual adult health checkup: update on the preventive care checklist form. Can Fam Physician 58:43–47
Editorial (2017) The rise of behavioural economics. Nat Human Behav 1:767. https://doi.org/10.1038/s41562-017-0252-9
El Bcheraoui C, Tuffaha M, Daoud F, AlMazroa MA, Al Saeedi M, Memish ZA, Basulaiman M, Al Rabeeah AA, Mokdad AH (2015) Low uptake of periodic health examinations in the Kingdom of Saudi Arabia, 2013. J Fam Med Prim Care 4(3):342
El‐Haddad B, Dong F, Kallail KJ, Hines RB, Ablah E (2015) Association of marital status and colorectal cancer screening participation in the USA. Colorectal Dis 17(5), O108–O114
Engebretson J, Mahoney JS, Walker G (2005) Participation in community health screenings: a qualitative evaluation. J Community Health Nurs 22(2):77–92
Finkelstein MM (2002) Preventive screening. What factors influence testing? Canadian Family Phys 48(9):1494–1501
Fletcher RH (2007) Review: periodic health examination increases delivery of some clinical preventive services and reduces patient worry. Ann Intern Med 12:118–118
General Statistics Office of Vietnam Health (n.d). Culture, Sport and Living Standard. https://www.gso.gov.vn/default_en.aspx?tabid=783 Accessed 4 Feb 2018
Glantz K, Rimer BK, Viswanath K (2008) The scope of health behavior and health education. In: Glanz K, Rimer BK, Viswanath K (eds) Health behavior and health education: theory, research, and practice, 4th edn. Jossey-Bass, San Francisco, p 3–22
Halek M, Eisenhauer JG (2001) Demography of risk aversion. J Risk Insur 68(1):1–24
Hallsworth M (2017) Rethinking public health using behavioural science. Nat Human Behav 1(9):612
Hammond WP, Matthews MD, Corbie-Smith G (2010) Psychosocial factors associated with routine health examination scheduling and receipt among African American men. J Natl Med Assoc 102(4):276
Harrison R, Cohen AW, Walton M (2015) Patient safety and quality of care in developing countries in Southeast Asia: a systematic literature review. Int J Qual Health Care 27(4):240–254
Hayward RS, Steinberg EP, Ford DE, Roizen MF, Roach KW (1991) Preventive care guidelines: 1991. Ann Intern Med 114(9):758–783
Himmelstein DU, Phillips RS (2016) Should we abandon routine visits? There is little evidence for or against. Ann Intern Med 164(7):498–499
Ho, MT (2018) Replication Data for: Healthcare consumers’ sensitivity to costs - a reflection on behavioural economics from an emerging market. Harvard Dataverse; https://doi.org/10.7910/DVN/CWHOIC
Hoang VM, Oh J, Tran TA, Tran TGH, Ha AD, Luu NH, Nguyen TKP (2015) Patterns of health expenditures and financial protections in Vietnam 1992-2012. J Korean Med Sci 30:S134–S138. https://doi.org/10.3346/jkms.2015.30.S2.S134. (Suppl 2)
Howard-Tripp Micheal (2011) Should we abandon the periodic health examination?: YES. Can Fam Physician 57(2):158–160
Hsu HY, Gallinagh R (2001) The relationships between health beliefs and utilization of free health examinations in older people living in a community setting in Taiwan. J Adv Nurs 35(6):864–873
International Cooperation Department (2017) Medical Benefit (Health Insurance). https://vss.gov.vn/english/thebenefits/Pages/medical-benefits.aspx Accessed 4 Feb 2018
Jepson R, Clegg A, Forbes C, Lewis R, Sowden A, Kleijnen J (2000) The determinants of screening uptake and interventions for increasing uptake: a systematic review. Health Technol Assess 4(14):i–vii
Johansson E, Winkvist A (2002) Trust and transparency in human encounters in tuberculosis control: lessons learned from Vietnam. Qual Health Res 12(4):473–491
Kang YJ, Park JH, Eom H, Choi B, Lee S, Lee JW, Myong JP (2017) Participation inequality in the National General Health Examination based on enterprise size. Ann Occup Environ Med 29(1):3
Kast D, Prochazka A, Miyoshi TJ, Bublitz C, Oboler SK, Fryer GE, Anderson RJ (2004) The annual physical examination: estimates from the National Ambulatory Care Medical Survey. J Gen Intern Med 19:214
Karwalajtys T, Kaczorowski J, Chambers LW, Levitt C, Dolovich L, McDonough B, Patterson C, Williams JE (2005) A randomized trial of mail vs. telephone invitation to a community-based cardiovascular health awareness program for older family practice patients [ISRCTN61739603]. BMC Fam Pract 6(1):35
Kelley JM, Kraft-Todd G, Schapira L, Kossowsky J, Riess H (2014) The influence of the patient-clinician relationship on healthcare outcomes: a systematic review and meta-analysis of randomized controlled trials. PLoS One 9:e94207
Kermott CA, Kuhl CS, Faubion SS, Johnson RE, Hensrud DD, Murad MH (2012) The diagnostic yield of the first episode of a periodic health evaluation: a descriptive epidemiology study. BMC Health Serv Res 2:137
Kim Y, Jun JK, Choi KS, Lee HY, Park EC (2011) Overview of the National Cancer screening programme and the cancer screening status in Korea. Asian Pac J Cancer Prev 12(3):725–730
Koo JH, Leong RW, Ching J, Yeoh KG, Wu DC, Murdani A, Cai Q, Chiu HM, Chong VH, Rerknimitr R, Goh KL (2012) Knowledge of, attitudes toward, and barriers to participation of colorectal cancer screening tests in the Asia-Pacific region: a multicenter study. Gastrointest Endosc 76(1):126–135
Kremer M, Glennerster R (2011) Improving Health in Developing Countries: Evidence from Randomized Evaluations. In: Thomas GM, Mark VP, Pedro PB (eds) Handbook of Health Economics. Elsevier, Amsterdam, p 201–315. Vol. 2
Krogsbøll LT, Jørgensen KJ, Grønhøj LC, Gøtzsche PC (2012) General health checks in adults for reducing morbidity and mortality from disease: cochrane systematic review and meta-analysis. BMJ 345:e7191
Kuo RN, Lai MS (2013) The influence of socio-economic status and multimorbidity patterns on healthcare costs: a six-year follow-up under a universal healthcare system. Int J Equity Health 12(1):69
Lai DW, Kalyniak S (2005) Use of annual physical examinations by aging Chinese Canadians. J Aging Health 17(5):573–591
Leal MD, Gama SG, Frias P, Szwarcwald CL (2005) Healthy lifestyles and access to periodic health exams among Brazilian women. Cad Saude Publica 21:S78–S88
Lin CC, Ko CY, Liu JP, Lee YL, Chie WC (2011) Nationwide periodic health examinations promote early treatment of hypertension, diabetes and hyperlipidemia in adults: experience from Taiwan. Public Health 125(4):187–195
Lu JFR, Hsiao WC (2003) Does universal health insurance make health care unaffordable? Lessons from Taiwan. Health Aff 22(3):77–88
MacMillan HL, MacMillan JH, Offord DR (1993) Periodic health examination, 1993 update: 1. Primary prevention of child maltreatment. The Canadian Task Force on the Periodic Health Examination. Can Med Assoc J 148(2):151
McPhee SJ, Bird JA, Davis T, Jenkins CN, Le B (1997) Barriers to breast and cervical cancer screening among Vietnamese-American women. Am J Prev Med 13(3):205–213
Meer J, Rosen HS (2004) Insurance and the utilization of medical services. Soc Sci Med 58(9):1623–1632
Mehrotra A, Prochazka A (2015) Improving value in health care—against the annual physical. New Engl J Med 373(16):1485–1487
Mehrotra A, Zaslavsky AM, Ayanian JZ (2007) Preventive health examinations and preventive gynecological examinations in the United States. Arch Intern Med 167(17):1876–1883
Merenstein D, Daumit GL, Powe NR (2006) Use and costs of nonrecommended tests during routine preventive health exams. Am J Prev Med 30(6):521–527
Meyer DJ, Meyer J (2005) Relative risk aversion: what do we know? J Risk Uncertain 31(3):243–262
Minh H (2011) Shunning Hippocrates-Privatization of healthcare breeds unethical medical practices at public hospitals. http://www.thanhniennews.com/2010/pages/20110416125458.aspx Accessed 10 Apr 2018
Naimi TS, Town M, Mokdad AH, Brewer RD (2006) Health care access among u.s. adults who drink alcohol excessively: missed opportunities for prevention. Prev Chronic Dis 3(2):A53
Nakanishi N, Tatara K, Fujiwara H (1996) Do preventive health services reduce eventual demand for medical care? Soc Sci Med 43(6):999–1005
Nguyen CV (2012) The impact of voluntary health insurance on health care utilization and out-of-pocket payments: New evidence for Vietnam. Health Econ 21(8):946–966
Nguyen KT, Khuat OTH, Ma S, Pham DC, Khuat GTH, Ruger JP (2012) Impact of health insurance on health care treatment and cost in Vietnam: a health capability approach to financial protection. Am J Public Health 102(8):1450–1461
Nupponen R (1996) Client views on periodic health examinations: opinions and personal experience. J Adv Nurs 23(3):521–527
Oboler SK, Prochazka AV, Gonzales R, Xu S, Anderson RJ (2002) Public expectations and attitudes for annual physical examinations and testing. Ann Intern Med 136(9):652–659
Parsa P, Kandiah M, Abdul Rahman H, Zulkefli NM (2006) Barriers for breast cancer screening among Asian women: a mini literature review. Asian Pac J Cancer Prev 7(4):509
Pham CT, McPhee SJ (1992) Knowledge, attitudes, and practices of breast and cervical cancer screening among Vietnamese women. J Cancer Educ 7(4):305–310
Pham LT (2016) Vietnam 2013 General Health Accounts and Disease Expenditures with Sub-Analysis of 2013 HIV/AIDS Expenditure. https://www.hfgproject.org/vietnam-2013-general-health-accounts-disease-expenditures-sub-analysis-2013-hivaids-expenditure/ Accessed 4 Feb 2018
Ponka D (2014) The periodic health examination in adults. Can Med Assoc J 186(16):1245–1245
Ren A, Okubo T, Takahashi K (1994) Comprehensive periodic health examination: impact on health care utilisation and costs in a working population in Japan. J Epidemiol Community Health 48(5):476–481
Ross CE, Mirowsky J (2000) Does medical insurance contribute to socioeconomic differentials in health? Milbank Q 78(2):291–321
Schäfer I, Hansen H, Schön G, Höfels S, Altiner A, Dahlhaus A, König HH (2012) The influence of age, gender and socio-economic status on multimorbidity patterns in primary care. First Results multicare cohort Study BMC Health Serv Res 12(1):89. https://doi.org/10.1186/1472-6963-12-89
Shiloh S, Vinter M, Barak M (1997) Correlates of health screening utilization: the roles of health beliefs and self-regulation motivation. Psychol Health 12(3):301–317
Siew CN, Sunny HW (2013) Colorectal cancer screening in Asia. Br Med Bull 105(1):29–42. https://doi.org/10.1093/bmb/lds040
Spivey C (2010) Desperation or desire? The role of risk aversion in marriage. Econ Inq 48(2):499–516
Son KY, Lee CM, Cho B, Lym YL, Oh SW, Chung W, Lee JS, Park D, Kim HS (2012) Effect of aditional brief counselling after periodic health examination on motivation for health behavior change. J Korean Med Sci 27(11):1285–1291
Sun X, Chen Y, Tong X, Feng Z, Wei L, Zhou D, Feng D (2014) The use of annual physical examinations among the elderly in rural China: a cross-sectional study. BMC Health Serv Res 14(1):16. https://doi.org/10.1186/1472-6963-14-16
Tang TS, Solomon LJ, McCracken LM (2000) Cultural barriers to mammography, clinical breast exam, and breast self-exam among Chinese-American women 60 and older. Prev Med 31(5):575–583
Tarrant C, Stokes T, Colman AM (2004) Models of the medical consultation: opportunities and limitations of a game theory perspective. BMJ Qual & Saf 13(6):461–466
Thombs BD, Lewin G, Tonelli M (2017) Implementing preventive health care recommendations in family medicine. Can Fam Physician 63(7):504–505
Thrall JH (2009) Drivers of health care costs: technology vs social, legal, and behavioral factors. J Am Coll Radiol 6(6):387–388
Trogdon JG, Hylands T (2008) Nationally representative medical costs of diabetes by time since diagnosis. Diabetes Care 31(12):2307–2311
Tucker LA, Clegg AG (2002) Differences in health care costs and utilization among adults with selected lifestyle-related risk factors. Am J Health Promot 16(4):225–233
UNDP Vietnam (2016) Growth that works for all: Viet Nam Human Development Report 2015 on Inclusive Growth. United Nations Development Programme
US Public Health Service (1994) The clinician’s handbook of preventive services: put prevention into practice. International Medical, Virginia
Van Minh H, Phuong NTK, Saksena P, James CD, Xu K (2013) Financial burden of household out-of pocket health expenditure in Viet Nam: findings from the National Living Standard Survey 2002–2010. Soc Sci Med 96:258–263
Vietnam Plus (2017) Health insurance covers 81.7 percent of Vietnam’s population. Vietnam Plus. https://en.vietnamplus.vn/health-insurance-covers-817-percent-of-vietnams-population/105228.vnp/ Accessed 6 Apr 2018
Vu DK, Hoang VM, Kim BG, Dao A, Le TT, Ng N (2016) Socioeconomic inequalities in catastrophic health expenditure and impoverishment associated with non-communicable diseases in urban Hanoi, Vietnam. Int J Equity Health 15(1):169
Vuong QH (2015) Be rich or don’t be sick: estimating Vietnamese patients’ risk of falling into destitution. Springerplus 4(1):529
Vuong QH (2016a) Data on Vietnamese patients’ behavior in using information sources, perceived data sufficiency and (non) optimal choice of healthcare provider. Data Brief 7:1687–1695
Vuong QH (2016b) Health communication, information technology and the public’s attitude toward periodic general health examinations. F1000Res 5:2935
Vuong QH (2017a) Survey data on Vietnamese propensity to attend periodic general health examinations. Sci Data 4:170142
Vuong QH (2017b) Vietnam general health examinations propensity survey 2016. Open Science Framework. https://doi.org/10.17605/OSF.IO/AFZ2W
Vuong QH, Nguyen H (2017) Patients’ contribution as a quid pro quo for community supports? Evidence from Vietnamese co-location clusters. Int J Bus Soc 18(1):189–210
Vuong QH, Nguyen TK (2015) Vietnamese patients’ choice of healthcare provider: in search of quality information. Int J Behav Healthc Res 5(3-4):184–212
Vuong QH, Napier NK, Tran TD (2013) A categorical data analysis on relationships between culture, creativity and business stage: the case of Vietnam. Int J Transit Innov Syst 3(1):4–24
Vuong QH, Nguyen H, Vuong TT (2017) Health insurance thresholds and policy implications: a Vietnamese medical survey in 2015. Biomed Res 28(6):2432–2438
Wall M, Teeland L (2004) Non-participants in a preventive health examination for cardiovascular disease: characteristics, reasons for non-participation, and willingness to participate in the future. Scand J Prim Health Care 22(4):248–251
Wilper AP, Woolhandler S, Lasser KE, McCormick D, Bor DH, Himmelstein DU (2009) Health insurance and mortality in US adults. Am J Public Health 99(12):2289–2295
Wong HZ, Lim WY, Ma SS, Chua LA, Heng DM (2015) Health Screening Behaviour among Singaporeans. Ann Acad Med 44:326–334
World Bank (2014) Health. In: World Development Report 2015: Mind, Society, and Behavior, Chapter 8. Washington, D.C.: World Bank Publications
Wu HY, Yang LL, Zhou S (2010) Impact of periodic health examination on surgical treatment for uterine fibroids in Beijing: a case-control study. BMC Health Serv Res 10(1):329. https://doi.org/10.1186/1472-6963-10-329
Yarnall KS, Pollak KI, Østbye T, Krause KM, Michener JL (2003) Primary care: is there enough time for prevention? Am J Public Health 93(4):635–641
Yeo JY, Jeong HS (2012) Determinants of health screening and its effects on health behaviors. Health Policy Manag 22(1):49–64
Yeoh KG, Chew L, Wang SC (2006) Cancer screening in Singapore, with particular reference to breast, cervical and colorectal cancer screening. J Med Screen 13(1):14–19
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Vuong, QH., Ho, TM., Nguyen, HK. et al. Healthcare consumers’ sensitivity to costs: a reflection on behavioural economics from an emerging market. Palgrave Commun 4, 70 (2018). https://doi.org/10.1057/s41599-018-0127-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1057/s41599-018-0127-3
This article is cited by
-
Does financial literacy influence preventive health check-up behavior in Japan? a cross-sectional study
BMC Public Health (2022)
-
Quality of health websites and their influence on perceived usefulness, trust and intention to use: an analysis from Thailand
Journal of Innovation and Entrepreneurship (2019)